CLINICIAN'S CAPSULE
What is known about the topic?
Substance and opioid use are common among emergency department (ED) patients, and ED-based interventions are effective; however, optimal targeting is unclear.
What did this study ask?
Among ED patients with substance and opioid use, are frequent ED use and degree of frequent use associated with mortality?
What did this study find?
Frequent users with substance use and extremely frequent users with substance and opioid use had higher mortality than non-frequent users.
Why does this study matter to clinicians?
Clinicians should flag frequent users electronically and explore and address their unmet needs, because multiple visits are missed prevention opportunities.
INTRODUCTION
Substance and opioid use are common among emergency department (ED) patients,Reference Sanjuan, Rice and Witkiewitz1–Reference Wu, Swartz and Wu3 especially among frequent ED users.Reference Urbanoski, Cheng, Rehm and Kurdyak4–Reference Curran, Sullivan and Williams7 In the current opioid epidemic, frequent ED presentation is increasingly being recognized as a harbinger of poor patient outcome; patients often make frequent ED visits prior to near-fatal overdose events.Reference Otterstatter8, Reference Hasegawa, Brown, Tsugawa and Camargo9 These ED visits are often missed opportunities to intervene. If frequent ED use could identify patients with substance and opioid use who are at risk of dying, a visit flagging system could enable practitioners to initiate ED-based brief interventions known to be effective, to engage patients with necessary follow-up care (e.g., addictions services), and ultimately to prevent mortality.Reference Crawford, Patton and Touquet10–Reference D'Onofrio and Degutis12 Although frequent ED users have a higher mortality than non-frequent users in general,Reference Moe, Kirkland and Ospina13 they are heterogeneous,Reference Doupe, Palatnick and Day6, Reference LaCalle and Rabin14, Reference Moe, Bailey and Oland15 and this risk has not been elaborated among patients with substance use. Additionally, frequent users likely differ by degree, that is, those at the extremes of frequent use (e.g., ≥ 16 visits/year) likely have different characteristics and outcomes than those with moderately high use (e.g., 5–15 visits/year). For instance, psychiatric comorbidities and non-urgent presentations are more common among patients with ≥ 18 annual visits; however, whether a “dose-response” relationship exists for mortality remains unclear.Reference Doupe, Palatnick and Day6, Reference Ruger, Richter, Spitznagel and Lewis16 Despite important prevention implications, to date, no system-level study has evaluated whether frequent ED use is associated with all-cause mortality in patients with substance and opioid use.
The objective was primarily to determine among ED patients with substance or opioid use whether frequent ED use in the previous 12 months was independently associated with mortality compared with non-frequent ED use, and, secondarily, whether mortality differed by degree of frequent use. We hypothesized that frequent use would be associated with mortality in ED patients presenting with substance or opioid use-related concerns.
METHODS
Study design and setting
This is a population-based, cohort study obtained from linked electronic ED visit and mortality databases evaluating patients who presented between April 1, 2012, and March 31, 2013. The study adheres to the RECORD reporting guidelines.Reference Benchimol, Smeeth and Guttmann17 The study setting is Alberta, Canada, with a population of over 4 million served by more than 100 EDs.
Data sources
The ED visit data were drawn from the National Ambulatory Care Reporting System administrative database containing all provincial ED visits.18 This database contains patient demographic information (i.e., personal health number, age, sex, postal code) and ED visit information (i.e., arrival mode, visit date, visit time, Canadian Triage and Acuity Scale level [CTAS]19), in-ED care (i.e., provider details, procedures), and outcome (International Classification of Diseases and Related Health Problems-10 diagnostic codes, disposition date, time, and destination). The CTAS categorizes patient presentations based on severity. This ranges from resuscitation (Level 1) requiring immediate physician assessment, to non-urgent (Level 5) with a suggested time to physician within 2 hours.Reference Lee, Oh and Peck20 Previous studies have validated the scale's ability to accurately predict patient outcomes and resource utilization, and have demonstrated high inter-rater reliability.Reference Lee, Oh and Peck20–Reference Beveridge, Ducharme and Janes22
The Canadian Institute of Health Information performs annual quality checks on National Ambulatory Care Reporting System data to ensure its accuracy.23 For the years of data analysed, incomplete ED record-level data were negligible (0.03% to 0.5%), and Albertan ED submissions met the most complete reporting standard (Level 3).24–26 Additionally, Alberta has independent validation processes for its electronic ambulatory care data.27 Furthermore, external validation studies have found 98% agreement for encounter and demographic data and 87% agreement for diagnostic coding.28
Mortality for all Alberta residents is captured within the Vital Statistics Registry, which records death date and demographic information.29 Vital statistics data were collected until the final study date, December 31, 2014.
The final database for this study was created by linking the National Ambulatory Care Reporting System and vital statistics registries using postal code, birthdate, and sex. The data for this study were obtained by the Alberta Health Services Data Integration Management and Reporting Service.30
Study population
The study included all adult patients (≥ 18 years old at time of index visit) who presented to an Albertan ED at least once during the study year (April 1, 2012, to March 31, 2013) for a substance use-related concern. Visits were classified as being related to substance use if an a priori group of diagnostic codes was listed as the primary or secondary diagnoses. Additional fields were excluded to limit misclassification from coding failure. The primary definition consisted of ICD-10 codes within the category, “Mental and behavioural disorders due to psychoactive substance use” (F10-F19), based on a previously published algorithm.31 Two additional sensitivity analyses were conducted using alternative ICD-10 code-based substance use definitions: firstly, a more comprehensive definition including additional selected codes within the category, “Poisoning by drugs, medicaments and biological substances” (T36-T50), and, secondly, a definition including all F10-F19 codes except those pertaining to the use of tobacco (F17).
A separate analysis of opioid use-related ED visits was performed because we hypothesized that the analysis of 2012–2013 data may provide important insight into the growth of the current public health issue. These were defined as visits with a primary or secondary ICD-10 diagnosis within the category, “Mental and behavioural disorders due to use of opioids” (F11) or certain codes within the category, “Poisoning by narcotics and psychodysleptics” (T40), consistent with the definition used by Alberta Health Services.32
In the entire database, 101 visits attributing to 14 unique patient identifiers had an index visit that occurred after the recorded death date. These visits were deleted as presumed erroneous entries; they represented 0.4% (101/24,880) of the study database.
Definition of frequent ED use
Patients were defined as frequent ED users if they had made ≥ 5 ED visits for any reason in the 12 months prior to the index visit (i.e., first visit within the study year). Non-frequent users had made ≤ 4 visits. The threshold of ≥ 5 visits corresponded to the 95th percentile of annual visits made by adult patients in Alberta, as suggested in previous studies.Reference Moe, Bailey and Oland15 An additional sensitivity analysis defined frequent ED use based on the number of substance use-related visits (rather than visits for any reason).
To assess whether mortality risk differed by degree, the frequent use definition was subcategorized into four groups: 5–10, 11–15, 16–20, and > 20 visits. Patients within the categories 16–20 and > 20 visits/year were considered to have extremely frequent ED use.
Key outcome measures
The primary endpoint was survival at 90 days following the index visit. Secondary endpoints were survival at 30 days, 365 days, and 2 years. Deaths were recorded over the entire study period from the index visit until December 31, 2014.
Statistical methods
Unadjusted mortality for frequent and non-frequent users was assessed using log-rank tests. Adjusted mortality was assessed using multivariable Cox proportional hazards regression and is reported as hazard ratios (HRs).
Age, sex, and postal-code-derived income33–Reference Thomas, Eberly, Davey Smith and Neaton35 were included in the model as important potential confounders. Income was dichotomized as above or below the median income for the cohort. Missing income data (n = 1032) were included as a separate category. Additional sensitivity analyses were performed to account for missing data by excluding missing entries and excluding income entirely as a covariate. All analyses were performed using SAS 9.4 (SAS Institute Inc., Cary, NC) and used a two-tailed p < 0.05.
Power calculation
Estimating that our frequent user population comprised 20% of our total cohort, 298 mortality events were necessary to detect an HR of 1.5 for mortality among frequent users compared with non-frequent users, with 80% power and an α = 0.05 two-tailed level of significance.
Ethical considerations
The study received ethics approval from the University of Alberta (Pro00058053_AME3), and administrative approval and a data sharing agreement from Alberta Health Services. Investigators accessed data after de-identification from a secure research server.
RESULTS
Characteristics of study subjects
Visit and patient characteristics
A total of 16,389 patients accounted for 24,880 substance use visits during the study year. Frequent users comprised 3,209 (19.6%) patients and 9,719 (39.1%) visits. Within the study year, 1,787 patients made 2,241 visits for opioid use. Among patients with opioid use, 481 (26.9%) frequent users accounted for 821 (36.6%) visits.
Baseline patient and visit characteristics are presented in Table 1. Among patients with substance and opioid use, frequent users were older, lower income, and more often resided rurally than non-frequent users. Furthermore, visits by frequent users were lower acuity (proportionally fewer triage level 1 or 2 visits) and were hospitalized less often.
Table 1. Patient characteristics of frequent and non-frequent ED users among patients with substance and opioid use
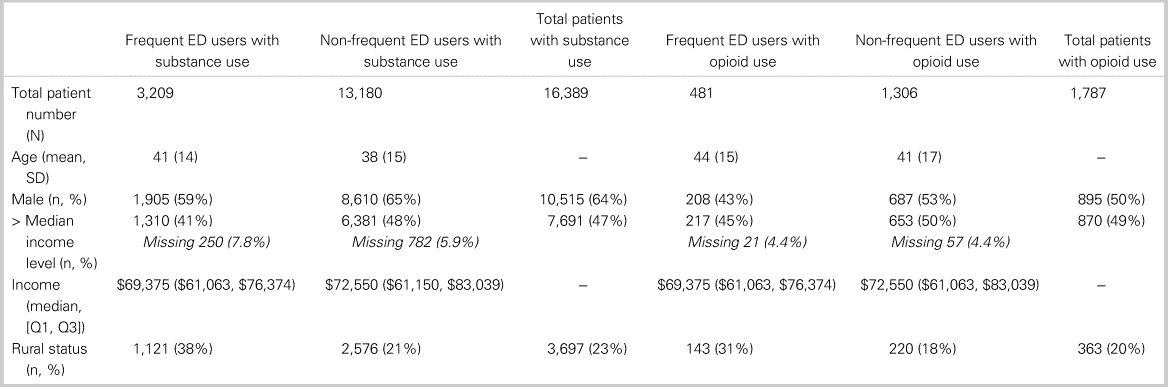
Main results
Unadjusted mortality
Table 2 reports unadjusted mortality estimates. Overall mortality was low in all groups, and 364 total mortality events (92 among frequent users and 272 among non-frequent users) were observed within the substance use cohort. Among substance use patients, no mortality difference was identified for frequent users compared with non-frequent users at 90 days or at 30 days. Mortality was higher for frequent users compared with non-frequent users at 365 days (2.3%, 95% confidence interval [CI]: 1.8, 2.8 versus 1.6%, 95% CI: 1.4, 1.8) and at 2 years (2.9%, 95% CI: 2.3, 3.4 versus 2.0%, 95% CI: 1.8, 2.3).
Table 2. Visit characteristics of frequent and non-frequent ED users among patients with substance and opioid use
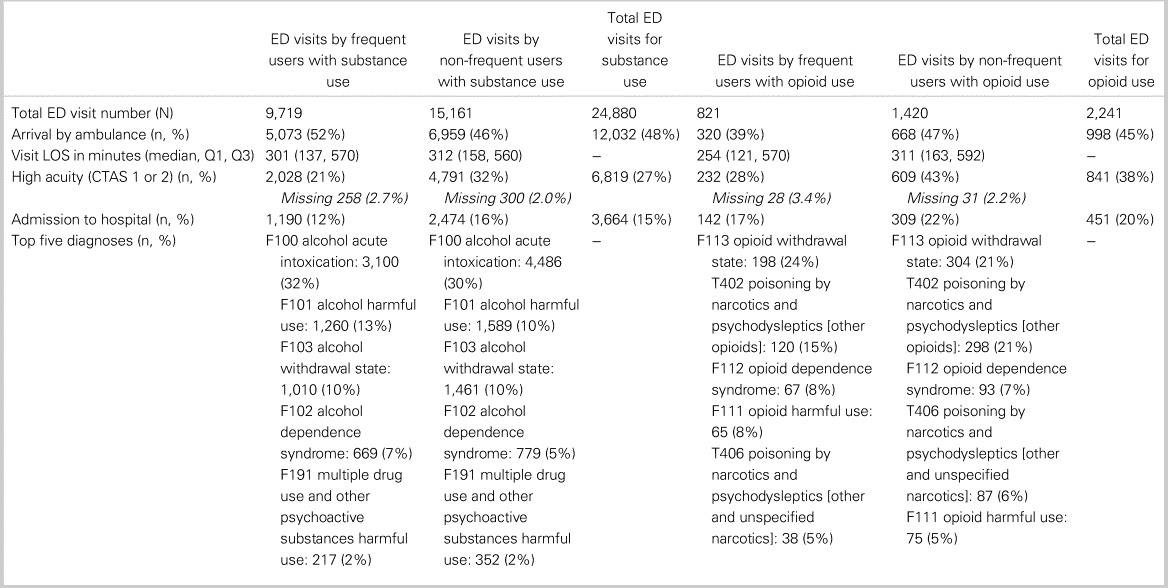
LOS = length of stay
Among patients with opioid use, there was no significant difference between frequent users and non-frequent users for mortality at 90 days, 30 days, 365 days, or 2 years.
Adjusted mortality
Table 3 presents the results of multivariable regression analyses. Frequent use was not significantly associated with 90-day mortality for patients with substance use; however, it was significantly associated with mortality at 365 days (HR 1.36 [95% CI: 1.04, 1.77]) and 2 years (HR 1.32 [95% CI: 1.04, 1.67]) when controlling for age, sex, and income. For patients with opioid use, frequent use was not associated with mortality at 90 days, 30 days, 365 days, or 2 years.
Table 3. Unadjusted mortality estimates for frequent and non-frequent ED users
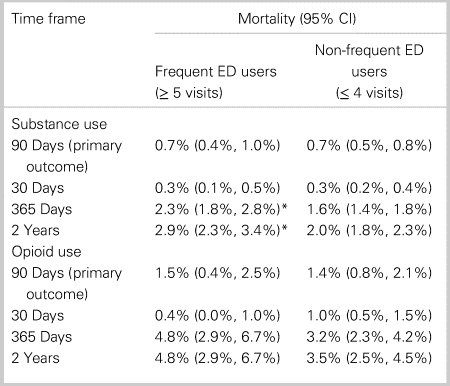
*Significant at p < 0.05
By degree (5–10, 11–15, 16–20, and > 20 visits), frequent use was significantly associated with mortality for patients with substance use and > 20 visits/year at 365 days (HR 1.88 [95% CI: 1.03, 3.44]) and at 2 years (HR 1.89 [95% CI: 1.10, 3.22]) (Table 4). Frequent use was significantly associated with mortality for patients with opioid use and 16–20 visits/year at 365 days (HR 3.62 [95% CI: 1.12, 11.66]) and at 2 years (HR 3.37 [95% CI: 1.05, 10.81]). These results remained consistent over the multiple sensitivity analyses.
Table 4. Adjusted mortality estimates by degree of frequent ED use
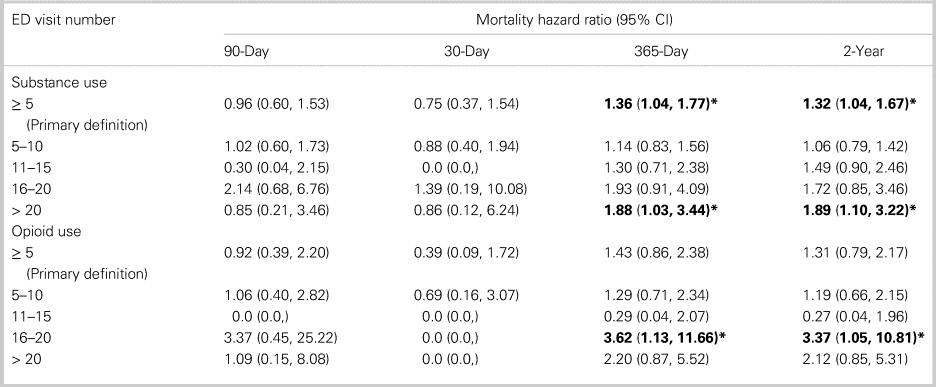
*Significant at p < 0.05
DISCUSSION
Among ED patients with substance use identified from valid province-wide, population-based administrative data, frequent users were more likely to die at 365 days and at 2 years than non-frequent users, but not at 30 and 90 days, when controlling for age, sex, and income. Despite low overall mortality, these results support the hypothesis that frequent ED presentation is correlated with risk of dying among patients with substance use, generally, but not opioid use alone.
Our results suggest that frequent ED users with substance use are high-risk patients; this is likely related to specific complications (e.g., overdose, infections) but also probably reflects poor overall health, chronic illness, and low socioeconomic status.Reference LaCalle and Rabin14, Reference Sun, Burstin and Brennan36, Reference Khan, Glazier, Moineddin and Schull37 Urbanoski et al.Reference Urbanoski, Cheng, Rehm and Kurdyak4 (2018) found that frequent ED users with psychiatric conditions died more often if they had comorbid substance use. Our study expands on this finding by suggesting that, among all patients with substance use, frequent ED use is associated with long-term mortality. Our study furthermore builds on previous work that has correlated overdose with frequent ED presentationReference Hasegawa, Brown, Tsugawa and Camargo9, Reference Brady, DiMaggio and Keyes38 by suggesting that risk extends to all-cause mortality.
Our analysis provides a signal that mortality risk may differ by degree of frequent use (e.g., patients with ≥ 16 visits compared with those with 5–15 visits). Subcategorized by degree (5–10, 11–15, 16–20, and > 20 visits), higher mortality was only seen for extremely frequent users with substance use (> 20 visits) and opioid use (16–20 visits). This finding is unexpected given that previous studies have not demonstrated that extreme frequent users have higher mortality and, in fact, they make lower acuity visits.Reference Doupe, Palatnick and Day6, Reference Ruger, Richter, Spitznagel and Lewis16 Our results support the importance of recognizing frequent users’ heterogeneity. Risk factors and outcomes should be explored within specific clinical subgroups. Additionally, our results suggest that recurrent low acuity visits should not distract from the long-term mortality risk among patients with substance use.
Our results also showed that frequent users with substance use made lower acuity visits and were admitted less often, which is somewhat paradoxical given their increased mortality risk. One possible explanation is that practitioner bias may enter into triage classifications. Another explanation is that medical complications of substance use (e.g., cellulitis, falls) are rapidly diagnosed and treated.Reference Kerr, Wood and Grafstein39 Finally, many of these patients would likely have medical and psychosocial needs (which may potentially be inadequately addressed by existing services) that would necessitate high healthcare service use overall, of which frequent ED utilization is one aspect.Reference Byrne, Murphy and Plunkett40 Whatever the cause, it is possible that these multiple minor ED visits indicate ongoing high-risk behaviours that increased frequent users’ overall long-term mortality. In retrospect, these minor events represent missed prevention opportunities and highlight the need for screening.
Limitations
This study has several limitations. Firstly, our diagnostic code-based definitions have not been validated. Nonetheless, they are aligned with current standards,31, 32 and our results remained consistent in multiple sensitivity analyses exploring a range of definitions. Secondly, the algorithm used to link the National Ambulatory Care Reporting System and Vital Statistics databases was not validated. Nonetheless, it is expected to be robust due to the requirement of three matching pieces of demographic information. It did not achieve a perfect match; however, erroneous entries represented a very small number of visits relative to the entire database (0.4%) and are unlikely to have affected results. Thirdly, there is a small possibility of losses to follow-up (e.g., patients not properly identified at death or who moved out of the province). Overall, censored data are likely minimal given the comprehensive provincial database and previously low documented rates of inter-provincial healthcare claims (approximately 2% for Alberta and Canada).41 Fourthly, our ability to control for potential confounders was limited by information available in the National Ambulatory Care Reporting System database. We were unable to adjust for comorbidities, end-of-life status or receipt of palliative/hospice care, patient complexity, homelessness or aboriginal status, which are not reliably recorded. Our inability to control for comorbidities in this analysis is a study limitation. In particular, it is possible that frequent ED use is associated with psychiatric comorbidities or chronic medical conditions, and that adequately controlling for these factors may help explain the difference in mortality observed between groups. Frequent ED presentations are, however, important considerations in their own right, because they are an easily measurable indicator that allows preventive intervention to be initiated; our study provides justification for more detailed analyses of potential underlying drivers of increased mortality among frequent ED users with substance use. Fifthly, our analysis is limited by missing data, particularly for income. In spite of this, our results remained consistent over multiple sensitivity analyses dealing with the missing income variable. Finally, despite the low overall mortality rates observed among all groups studied, given the importance of the outcome (mortality) and the public health crisis that exists, we argue that this small difference has the potential to have an important impact across Canada (assuming similar provincial event rates). This analysis of 2012–2013 data is an important precursor of what has likely become an increasingly significant issue in the context of the current burgeoning opioid epidemic and ongoing societal issues of alcohol and other substance-related disorders. Evidence shows that numbers of substance and opioid use-related ED visits continue to climb.42 Therefore, the small mortality difference that we detected at a population level likely translates to many individual lives at stake. Our results provide an important reference point and set the stage for current analyses by highlighting an important signal of risk among extremely frequent ED users presenting with substance and opioid use. This association likely has become stronger and merits repeat evaluation using data collected since 2012–2013.
CONCLUSIONS
This study suggests that, among patients with substance use, generally, but not opioid use alone, frequent ED use is associated with a higher risk for long-term (365-day and 2-year) but not short-term (90- and 30-day) mortality compared with non-frequent ED users. Our analysis appears to signal that extremely frequent ED use is associated with mortality among patients with substance use (> 20 visits) and opioid use (16–20 visits). This finding may be generalizable across Canada; for instance, in British Columbia, at the epicentre of the current opioid epidemic, similar evidence is emerging.Reference Otterstatter8 Extremely frequent users might benefit from targeted prevention, such as by flagging them using existing electronic visit tracking systems already operational in many EDs. Additionally, educating clinicians about exploring patient needs and reasons for frequent presentation will facilitate identification of appropriate interventions. Future research should link ED data to additional databases to better adjust for patient complexity and should assess the effectiveness of targeted interventions for frequent ED users with substance and opioid use.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2019.15.
Acknowledgements
The authors acknowledge the support of the Emergency Strategic Clinical Network of Alberta Health Services (AHS) for access to the health data.
Financial support
Author JM's research is currently supported by the University of British Columbia Department of Emergency Medicine and the Vancouver Acute Emergency Physicians’ Association. At the time of the study, author BHR's research was supported by a Tier I Canada Research Chair in Evidence-based Emergency Medicine funded by the Canadian Institutes of Health Research (CIHR) through the Government of Canada. He is currently supported by the CIHR as the Scientific Director of the Institute of Circulatory and Respiratory Health (ICRH). At the time of the study, author SJ's research was supported by the Emergency Strategic Clinical Network of AHS. The funders take no responsibility for the content or interpretation of these data.
Presentations
A related abstract was presented as a poster presentation at the Canadian Association of Emergency Physicians Conference in May 2018.





