CLINICIAN’S CAPSULE
What is known about this topic?
Evidence-based pediatric emergency care is variably applied across general and pediatric emergency departments.
What did this study ask?
What are the information-seeking patterns of pediatric emergency medicine network members?
What did this study find?
There remains a need to share successful methods of local dissemination and implementation across the network, and to leverage local professional champions such as clinical nurse liaisons.
Why does this study matter to clinicians?
Tailoring knowledge mobilization efforts to end-user priorities is essential to ensure impact and spread of outreach efforts.
INTRODUCTION
Use of the latest evidence is key to the delivery of high-quality care. In the field of emergency medicine, the scope of evidence is vast, and there is a well-cited disconnect between knowledge production and knowledge use.Reference Lang, Wyer and Haynes 1 The emergency department (ED) environment presents a number of unique challenges to sustained knowledge acquisition and sharing.Reference Curran and Abidi 2 Further challenges exist in community EDs where the staff is trained to meet the needs of the general population, are exposed to fewer pediatric cases, and have limited access to current and reliable resources, thus restricting exposure to new information and knowledge. The mixed-staffing model in many rural EDs, where intermittent coverage is provided by family physicians and other specialists, presents further challenges in knowledge sharing and upkeep. 3 In Canada, 85% of children seek care outside of pediatric centres where the vast majority of knowledge is produced. 4 It is estimated that as many as 40% do not receive treatments for which clear evidence exists, and one in five may receive treatments that are of no benefit or could even be harmful,Reference Knapp, Simon and Sharma 5 - Reference Freedman, Gouin and Bhatt 8 indicating a pervasive gap in the translation of the latest knowledge into practice.
Translating Emergency Knowledge for Kids (TREKK), a national network in pediatric emergency care, was established in 2011 to address these critical knowledge-to-practice gaps and accelerate the speed with which the latest evidence is shared and used in non-pediatric EDs. The TREKK network includes partnerships with 37 general EDs spanning nine provinces and one territory. Known as TREKK sites, each of these 37 institutions is partnered with its closest Pediatric Emergency Research Canada (PERC) site, within teaching or pediatric hospitals. The potential that networks have to address complex challenges is increasingly accepted in multiple disciplines.Reference Fitzgerald and Harvey 9 - Reference Borgatti and Foster 11 Health care professionals rely heavily on their social networks to find information and make clinical judgments.Reference Curran and Abidi 2 , Reference Scott, Albrecht and Given 12 - Reference Dawes and Sampson 14 Advantages of network coordination include enhanced learning, more efficient sharing and use of resources, increased capacity to address complex issues, reduced duplication, and rapid diffusion and reach 10 , Reference Provan and Kenis 15 ; however, measuring these impacts can be challenging. Social network analysis (SNA) uses network theory to understand patterns of interactionReference Wolfe 16 and presents a unique, but underused, opportunity to complement quantitative techniques with qualitative methods to gain insight into both network structures and processes.Reference Kelman, Luthe and Wyss 17 , Reference Williams and Shepherd 18
The purpose of this study was to build on the results of our two previous SNA measures to gain a more in-depth understanding of the network processes and context. The previous SNA measures provided important information on the overall structure of the TREKK network, including locating the knowledge brokers of the network and identifying a reduction in the number of disconnected sites between 2014 and 2015.Reference Klassen, Curran and Ripstein 19 Disconnected EDs were defined as those not connecting with a pediatric centre or other health institution for information seeking or advice. The specific aims of this qualitative study were to 1) determine patterns of knowledge sharing and connectivity among rural, urban, and community EDs; and 2) identify strategies and initiatives used to share knowledge in pediatric emergency medicine, including current barriers and opportunities.
METHODS
Sample
All health care professionals working in the EDs of TREKK sites were eligible to participate in this study. Sites were purposefully sampled to ensure representation from across Canada, with the aim of conducting at minimum two interviews per province. Informed by the results of previous quantitative SNAs conducted in 2014 and 2015, the sampling technique aimed to achieve representation from both connected and disconnected sites. Staff working in general EDs were invited to participate through their TREKK site representatives, who are senior clinicians and managers of their hospital sites and linking agents to the TREKK network.
Data collection
An interview guide was developed by the study team and piloted with three health care professionals (see Appendix). Data were collected through 22 individual semi-structured telephone interviews with health care professionals working in TREKK-affiliated general EDs between September and November 2016 ranging from 5 to 20 minutes in duration. Interviews were audio-recorded and were transcribed intelligent verbatim by an independent company. The interviewer reviewed transcripts to ensure accuracy and to remove any identifying information.
Data analysis
Interviews were analyzed by two members of the research team using content analysis.Reference Hsieh and Shannon 20 Each reviewer read through all interviews and independently open-coded 25% of the interview transcripts. Reviewers then compared and contrasted codes until an inter-coder agreement of >0.80 was achieved. Initial codes were established, and the remaining data were coded by both reviewers and managed using QDA Miner software. The reviewers employed analyst triangulation with the study team to develop themes and to ensure credibility and inter-coder agreement throughout the remaining analysis.
Ethical considerations
Approval was obtained from the University of Manitoba Health Research Ethics board (#H2016:249). Informed consent was obtained from all participants before commencing the interviews. Randomly generated codes were assigned to each name and location to protect participants’ privacy. Links between the name and code number are housed on a password-protected file and computer at the Children’s Hospital Research Institute of Manitoba.
RESULTS
The study population consisted of physicians (59%) and nurses (41%), representing 18 non-pediatric EDs. Participating ED sites were situated in both urban (68%) and rural/remote (32%) areas spanning 10 provinces and one territory of Canada. Slightly more males (n=12) than females (n=10) participated. Physician participants were more likely to be male (85%), and nurse participants were more likely to be female (91%). Participating sites were located between 2 and 1500 km from their nearest PERC site (average 215.94 km; standard deviation [SD]=364.56).
Major themes emerging from the analysis included: 1) patterns of knowledge acquisition and sharing; 2) barriers to obtaining pediatric information, training, or both; 3) opportunities to enhance capacity; and 4) benefits of affiliation with the TREKK network.
Theme 1 - Patterns of knowledge acquisition and sharing
Health care professionals working in general EDs reported using a range of pediatric information sources including guidelines, online resources, and colleagues and various means of accessing the information, including seeking advice from local or offsite pediatric experts, and attending pediatric-specific professional development opportunities. Guidelines and other online resources were frequent sources of information for both nurses and physicians. As a second line of information, participants reported talking to colleagues within their ED and local pediatricians. One of the initial objectives of TREKK was to increase connections between general and pediatric EDs. Contacting the nearest PERC site for information was consistently noted across all participants, particularly for unique cases or if uncertainty remained after consulting the latest guidelines. The PERC site was also used as a resource in instances in which health care professionals felt their colleagues’ practices were not in line with the latest evidence (Box 1; nurse 2109-MQ). Physicians reported engaging in more formalized methods of information seeking, including attending rounds or journal clubs and through telephone consults. Physicians working in rural areas described the overall culture in pediatrics as one that facilitated access to information (physician 2123-YA; 2422-XA). Alternatively, physicians in urban sites were more likely to report contacting the PERC site as a later step in the information-seeking process (physician 2275-JY). Nurses reported using more informal methods to seek information, such as talking to local physicians or contacting nurse educators at their nearest PERC site for the most up-to-date information.
Box 1 Participant quotes supporting key findings
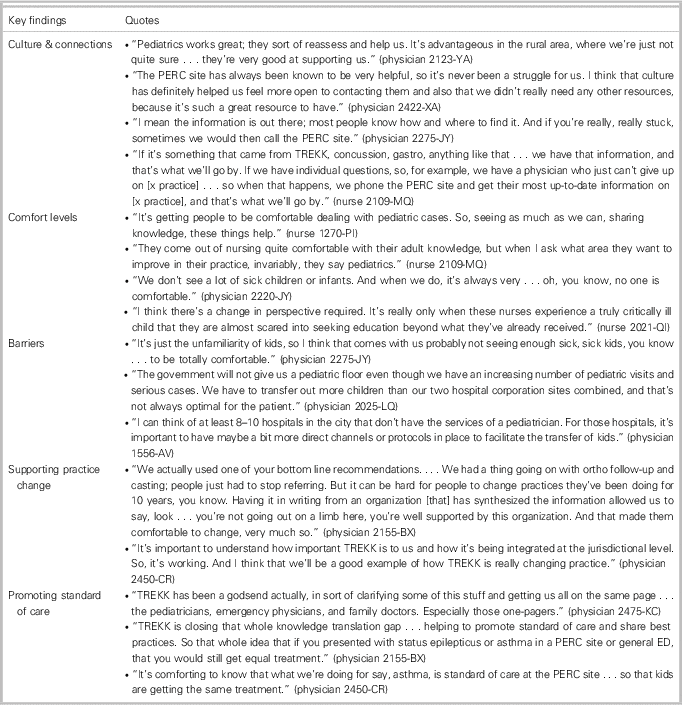
Achieving an adequate level of comfort with pediatric cases was critical for both physicians and nurses (nurse 1270-PI; 2109-MQ; physician 2220-JY). Professional development activities were highly valued across all demographics, serving to increase pediatric knowledge and comfort levels. Hands-on training through simulation scenarios, outreach education from the nearest PERC site, and sharing learnings with colleagues were the most frequently mentioned methods to increase comfort. Notably, an uptake in training often occurred following a critical or “scary” event (nurse 2021-QI).
Theme 2 - Barriers to obtaining pediatric information, training, or both
Participants reported organizational, personal, and system-level barriers to achieve the desired level of pediatric information and training. Barriers at the organizational level included challenges disseminating resources to staff, geographical barriers relating to patient transfers and attending professional development sessions, organizational resources (e.g., funding for professional development and staffing levels), low staff interest, and infrequent exposure to training opportunities. Participants reported personal barriers including time (e.g., competing clinical responsibilities), personal costs (e.g., paying out of pocket or using vacation days for training), and a low volume of children seen at their site (physician 2275-JY). At the systems level, policy level decisions were sometimes at odds with staff views and resulted in situations that were not always viewed as optimal for a patient (physician 2025-LQ; 1556-AV).
Theme 3 - Opportunities to enhance capacity
At the site level, enhancing the visibility of pediatric resources (e.g., through TREKK desktop icons) and having easy access to online pediatric protocols and resources facilitated information use. Pediatric liaison roles were key to the organization and provision of pediatric information and training, and, if absent, an inherent barrier. Reducing personal costs by facilitating reimbursement through nursing unions or recruitment and retention funds were noted as ways to enhance training attendance. At the systems level, embedding guidelines into local care systems, such as pediatric order sets and regional care maps and protocols, facilitated the use of best practices. Developing relationships early on, by promoting TREKK in medical school or by building sessions at the nearest pediatric site into orientation training, provided lasting connections to the children’s hospital and an instant link to an information source for pediatric emergency medicine. Of note, this strategy would be challenging for sites in rural and remote areas of Canada.
Participants identified opportunities to facilitate the dissemination and implementation of best evidence. Disseminating information to staff was often a challenge, suggesting a need to share successful methods of dissemination and implementation between TREKK sites. Nurses reported not having enough time to look online for information while delivering care, particularly in busy emergency settings. Embedding resources into local systems and providing easy access to resources at the point of care were suggested strategies to reduce barriers to information use. Some physicians reported using pediatric order sets for available conditions but noted a lack of them, especially for less common, more anxiety-provoking cases such as seizures. One physician suggested replicating successful initiatives from the adult field, including ongoing monitoring and evaluation of patient outcomes, transfer outcomes, and comparability to peer hospitals. Furthermore, one participant spoke of the need for better-developed protocols between institutions at the provincial or national level, particularly relating to criteria for transport.
Nurses often reported a “pull” (having to actively seek out needed information) versus “push” (tailored dissemination of knowledge and resources to those who need it) methodology for acquiring information, and both nurses and physicians expressed a desire for central coordination and promotion of events and practice changes. A prominent theme that emerged was the essential role of clinical nurse educators to facilitate training opportunities, as well as their potential to transform current efforts from a pull to a push methodology and to enhance connections between pediatric and general ED sites. In particular, nurse participants identified a shortage of available training opportunities and different training standards for those working within and outside of pediatric centres. Standardizing training requirements and reducing financial barriers to obtaining training in pediatrics was thought to be an essential step forward. “More contact, more simulation, more outreach education” was a common sentiment, suggesting that for comfort levels to increase, more frequent exposure is necessitated through the maintenance and enhancement of network connections.
Theme 4 - Benefits of affiliation with the TREKK network
Participants described numerous benefits of affiliation with the TREKK network. TREKK was commonly used by and promoted to other colleagues by nurse and pediatric educators. For nurses, hosting TREKK outreach education sessions established connections to pediatric experts and made obtaining pediatric information and training easier. Among nurses in the rural areas, TREKK was thought to enhance the availability of training events, and TREKK resources were used by other subspecialties in the community, such as primary care and respiratory therapy. Physicians working at multiple sites noted that their TREKK sites had stronger connections to their nearest PERC site, as compared with non-TREKK sites, and others noted that connections to their PERC site for education purposes emerged mainly as a result of TREKK. Network benefits were particularly strong for physicians working in rural areas, supporting local and jurisdictional practice change (physician 2155-BX; 2450-CR), promoting standard of care within emergency medicine and across other subspecialties (physician 2475-KC), and closing knowledge translation gaps, the umbrella term for the multiple activities involved in moving research into practice (physician 2155 BX; 2450-CR). As one physician noted, “being a TREKK site, we’re more aware of it, but I find others just aren’t aware,” suggesting a need to broaden network reach and to promote through multiple channels to ensure that all sites have equal access to pediatric knowledge and training opportunities.
DISCUSSION
TREKK is the only network in Canada dedicated to providing general ED professionals with current, evidence-based resources and training that is based on stakeholder and user identified prioritiesReference Scott, Albrecht and Given 12 and intended to improve the quality of pediatric emergency care. This study examined health care professionals’ information-seeking behaviours and identified ongoing challenges, network successes, and future opportunities for the TREKK network.
To fully comprehend the information seeking of health care professionals, it is important to understand their information needs first.Reference Davies and Harrison 21 At its inception, the main goals of TREKK were to determineReference Scott, Albrecht and Given 12 and address the knowledge needs of health care professionals working in general EDs by assembling existing evidence and developing usable educational tools through an iterative knowledge translation processReference Featherstone, Leggett and Knisley 22 to assist them in the access, adaptation, and implementation of new knowledge. The TREKK needs assessment identified a need to develop tools and interpersonal strategies to fulfill the knowledge needs and preferences of these health care professionals.Reference Curran and Abidi 2 In this study, use of resources including the TREKK bottom line recommendations, outreach education sessions, and talking to colleagues in pediatric EDs were common sources of information for both nurses and physicians, suggesting that the priorities and investments of TREKK were in line with the needs of end-users. Locating best-quality evidence throughout the mass of available information can be challenging,Reference Davies and Harrison 21 and evidence suggests that resources have to be quickly accessible to be practical at the bedside.Reference Sackett and Straus 23 Previous studies have reported a lack of guideline awareness as a barrier to their use in community settings.Reference Gilleland, McGugan, Brooks, Dobbins and Ploeg 24 To facilitate use, TREKK bottom line recommendations were reviewed at the regional level in some jurisdictions and embedded within local care maps and protocols. Other sites made frequent use of order sets, indicating a more direct strategy to enhance the use of TREKK products. Increasing content visibility and usability, through TREKK promotional materials, desktop icons and apps, and acceptability, and by promotion through local educators, were common strategies used to promote the use of best practice. Findings suggest that network resources and processes are being used as regional benchmarks across a number of sites, but there remain many EDs outside the network who stand to benefit from TREKK resources, which are publicly available.
A salient theme emerging from the data was a remaining level of health care provider discomfort with pediatric cases, suggesting a need for ongoing strategies to mitigate discomfort. This finding is consistent with existing research that supports an overall sense of unease with critical pediatric conditions in the community setting.Reference Gilleland, McGugan, Brooks, Dobbins and Ploeg 24 - Reference Falgiani, Kennedy and Jahnke 26 A desire for more frequent exposure to hands-on experiential learning has been previously reported in the community urgent care settingReference Scott, Albrecht and Given 12 , Reference Gilleland, McGugan, Brooks, Dobbins and Ploeg 24 and was reinforced in this study. Discomfort, both in dealing with pediatric cases and in seeking out advice from pediatric experts, was commonly discussed. At a practical level, this discomfort occurred because of infrequent experience with critically ill pediatric patients and was enhanced by exposure to pediatric information, resource sharing, training, and contact with pediatric experts. As network connections strengthened over time, health care professionals not only felt an increased comfort level to seek out clinical advice from PERC sites but also commonly shared knowledge gained through these encounters and other offsite training with colleagues in their local ED, amplifying the sharing of knowledge. These results demonstrate that network structure and processes minimized geographic boundaries and provided new opportunities to seek and disseminate knowledge.
The TREKK experience is consistent with the knowledge translation literature, which suggests that a multi-pronged active engagement strategy with research end-users is more likely to result in the uptake and use of knowledge.Reference Grol and Grimshaw 27 , Reference Lau, Stevenson and Ong 28 Elements that have been previously described to improve the effectiveness of knowledge translation interventions include increased exposure, access to and engagement with content experts, and tailoring interventions to the needs and contexts of end-users.Reference LaRocca, Yost, Dobbins, Ciliska and Butt 29 Successful knowledge translation requires understanding and attending to the multidimensional barriers and facilitators that influence knowledge-to-practice gaps.Reference Grol and Grimshaw 27 , Reference Grimshaw, Eccles, Lavis, Hill and Squires 30 However, barriers are dynamic, reinforcing the importance of evaluation over time to ensure that network strategies continue to be appropriate and relevant to end-users.Reference Lau, Stevenson and Ong 28
Implications
By gaining a better understanding of network processes from the perspective of front-line health care professionals, this study illuminates current information-seeking practices, a distinct culture in pediatric emergency medicine, and its potential impact on standardizing care across sites. This exploratory study highlights the need to strengthen current efforts through dedicated nurse liaison roles and to expand network reach to include additional sites and specialties such as family medicine. Although network structure and processes were associated with inherent benefits, ongoing challenges suggest a need for continued growth of TREKK activities and additional resources to enhance strategies to improve comfort with pediatric care in general ED settings.
LIMITATIONS
Our sampling technique aimed to enhance the external validity of our findings by sampling across a range of geographical areas, professions, and previously connected and disconnected sites. Despite our efforts, the majority of study participants held multiple roles, including those as educators or leaders, potentially weighting the results in favour of a more connected subset of health care professionals. It is critical to remember that our study was conducted within the TREKK network, a network in which health care professionals have access to more pediatric-specific resources and training opportunities. As a result, our findings may not have broad transferability to all general EDs without similar resources. Yet, the interview questions sought to identify challenges and opportunities in pediatric emergency medicine generally, rather than focus on network benefits. To further delineate the power of the network, future studies should replicate these interviews with staff working in general EDs outside the network. Future follow-up studies within the network have the potential to identify changes in the network structure and processes over time and to adapt knowledge mobilization efforts accordingly.
CONCLUSIONS
By gaining a better understanding of network processes from the perspective of front-line health care professionals, this study illuminates current information-seeking practices, a distinct culture in pediatric emergency medicine, and its potential impact on standardizing care across sites. It also highlights the need to strengthen current efforts through dedicated nurse liaison roles and to expand network reach to include additional sites and specialties. Our results reinforce the critical importance of ongoing network evaluation to ensure that network strategies continue to be appropriate and relevant to end-users.
Acknowledgements: The authors acknowledge the ongoing contributions of TREKK network members to network activities, including the Board of Directors, Knowledge Mobilization Advisory Committee, Parent Advisory Committees, PERC Representatives and Coordinators, TREKK Representatives, TREKK Steering Committee, and the TREKK Administrative Centre. LKC, LK, JC, and CL contributed to the study design, and LKC organized and conducted the interviews. LKC and GB analyzed the transcripts, and LKC, GB, and CL were involved in theme development and interpretation. LKC composed the manuscript, and TPK, LK, JC, CL, SS, LH, and MJ provided critical input to and revised the manuscript. All authors have read and approved the final manuscript.
Competing interests: None declared. TREKK is funded by the Government of Canada’s Networks of Centres of Excellence - Knowledge Mobilization initiative and gratefully acknowledges support from our host institution, the University of Manitoba, as well as support from the Children’s Hospital of Eastern Ontario Research Institute, Children’s Hospital Foundation of Manitoba, Children’s Hospital Research Institute of Manitoba, PERC, Research Manitoba, Stollery Children’s Hospital Foundation, University of Alberta, and the Women and Children’s Health Research Institute.
Appendix
Semi-structured interview guide
1. Tell me about your role in the ED. Do you work in any other EDs, health centres, wards, or clinics?
2. Where is your nearest children’s hospital? Is this your first point of contact for seeking guidance/updates/information on pediatric emergency medicine?
3. Broadly speaking, what factors do you see impacting your ability to seek pediatric emergency information or training?
4. Do you seek advice/information from anywhere else (other hospitals, institutions, or organizations)?
5. Can you think of any strategies/initiatives that could help your ED better connect to your nearest children’s hospital or tell me about any that have worked well to date?



