Introduction
Evidence suggests that analgesia is underutilized for acute abdominal painReference Ali, Chambers and Johnson 1 - Reference Herd, Babl and Gilhotra 5 , delayed in its administration,Reference Ali, Chambers and Johnson 1 - Reference Todd, Ducharme and Choiniere 3 and dosed insufficientlyReference Ali, Chambers and Johnson 1 , Reference Todd, Ducharme and Choiniere 3 in the emergency department (ED) setting. Compared to adults, children are at particular risk for suboptimal analgesia and have been found to receive analgesia less often.Reference Bauman and McManus 6 - Reference Brown, Klein and Lewis 8
Abdominal pain is the most frequent clinical feature of acute appendicitis,Reference Addiss, Shaffer and Fowler 9 , Reference Rasmussen and Hoffmann 10 which is the most common pediatric condition requiring urgent surgical intervention.Reference Sivit 11 In 2003, Kim and colleagues found that over one-third of pediatric emergency physicians (PEPs) were unlikely to provide analgesia before establishing a definitive diagnosis in children with acute abdominal pain.Reference Kim, Galustyan and Sato 12 Disapproval by surgeons was identified as the main barrier.Reference Kim, Galustyan and Sato 12 In the last decade, many studies have disputed the notion that providing analgesia is associated with an increased risk of diagnostic or management errors.Reference Manterola, Astudillo and Losada 13 - Reference Ranji, Goldman and Simel 15
The importance of providing optimal pain treatment has been echoed by several national and international policy statements. In addition to the mandate by the World Health Organization (WHO) that adequate pain treatment should be a fundamental human right,Reference Brennan, Carr and Cousins 16 the American Academy of Pediatrics (AAP) recently reaffirmed its position that adequate analgesia be provided for children.Reference Fein, Zempsky and Cravero 17 Moreover, untreated pain in childhood has been reported to lead to long-term negative outcomes such as anxiety, hyperesthesia, and needle phobia.Reference Taddio 18
Notwithstanding the above, few EDs have policies guiding pain management in patients with acute abdominal pain,Reference Ali, Chambers and Johnson 1 , Reference Villain, Wyen and Ganzera 19 and a 2012 study reported that analgesia is not provided to one-third of children with abdominal pain.Reference Thompson, Schuh and Gravel 20 It is thus imperative to explore reasons behind withholding analgesia, and, more speficially, the relationship of the practice of withholding analgesia with surgical consultation, in order to inform knowledge translation initiatives to improve care. The objectives of this study were to: (1) explore theoretical practice variation in the provision of analgesia to children with acute abdominal pain; (2) identify reasons for withholding analgesia; and (3) evaluate the relationship between providing analgesia and surgical consultation for physicians practicing in a Canadian pediatric ED setting.
Materials and Methods
Study design
A cross-sectional survey of PEPs was designed to test the hypothesis that there remains a reluctance to provide analgesia to children with acute abdominal pain and that this decision is related to surgical consultation.
Protocol
Potential participants were contacted from June to July 2014 through a database of PEPs administrated by Paediatric Emergency Research Canada (PERC). A modified Dillman’s Tailored Design Method for mail and internet surveys was used to optimize responses. 21 A pre-notification email was sent to physicians in the database on day 0, followed by electronic survey dissemination on days 3, 10, 17, 24, and 31. A paper-based survey copy was mailed to non-respondents on day 38. Members of the research team were blinded to the identity of electronic or paper-based participants. Surveys were administered using the SurveyMonkey platform (www.surveymonkey.com). Consent to participate was implied by completion of any portion of the electronic or paper-based survey. This study received approval from Western University’s Research Ethics Board.
Participants
The participants included consenting physicians within the PERC database as of March 2014. PERC is a network of health care providers whose primary clinical, administrative, and academic appointments are at EDs within tertiary care paediatric centres across Canada, and it includes physicians who consented to have their email addresses distributed for research purposes.
Instrument
The survey instrument included demographic questions, followed by three scenarios based on actual clinical cases of intussusception, renal colic, and appendicitis (see supplementary material). After each scenario, the participants were asked: (i) whether they would offer analgesia; (ii) whether they would obtain a surgical consultation; (iii) what their analgesic choices might be; and (iv) their reasons behind a decision not to offer analgesia (if applicable). Finally, the survey asked respondents to choose from a list of clinical conditions for which they would routinely provide analgesia and, using a 5-point Likert scale, rate the degree to which they believed that analgesia could mask important physical signs. Responses to all survey questions included multiple choice responses, Likert scale ratings, and free-text. Data were coded in duplicate by two co-investigators (AC,CD), and the survey was available in both English and French.
The survey was developed based on the approach outlined by Burns and colleaguesReference Burns, Duffett and Kho 22 using a focus group of four investigators (NP, RL, AC, CD). After a pre-testing phase, the survey was pilot tested among seven emergency physicians and two surgical residents who were asked to rate it for face validity, clarity, length, comprehensiveness, and bias.
Statistical analysis
Response rates, demographic variables, number of participants indicating they would or would not provide analgesia, reasons for not providing analgesia, and types of analgesia were summarized using means, frequencies, and percentages, as appropriate. The relationship between providing analgesia, obtaining a surgical consultation, and demographic variables were summarized using the Fisher exact or chi-square test, as appropriate. The primary outcome variable was the reported frequency of providing analgesia for each scenario. Secondary outcomes included the reasons for withholding analgesia, frequency of opioid use, and the relationship of opioid provision to surgical consultation for each scenario. Exploratory analyses included the exploration of the relationship between providing any analgesia and the following covariates, defined a priori: years of independent practice (greater than or less than 10), and type of training (pediatric emergency medicine (PEM) or other). Data were analyzed using SPSS (version 19, IBM SPSSTM, New York, NY). A p-value of <0.05 was considered statistically significant.
Results
Respondents
The survey was distributed to 200 physicians. One hundred thirty completed the electronic version and 19 completed the paper-based survey, resulting in an overall response rate of 74.5%. Respondents were permitted to skip questions and therefore the response rates were variable for each question. On average, there was a 10% increase in responses with each additional dissemination of the survey. All of the respondents worked at least one clinical shift per month. The demographic characteristics of the participants are provided in Table 1.
Table 1 Demographic features of study participants (n=149)

PEM=paediatric emergency medicine; FRCP=Fellow of the Royal College of Physicians; CCFP=Certification in the College of Family Physicians
Provision of analgesia
The characteristics of participants’ answers to questions pertaining to the provision of analgesia based on three scenarios are presented in Table 2. The proportions of any analgesic provision, for undifferentiated abdominal pain arising from intussusception, renal colic, and appendicitis, were 83.4%, 100%, and 92.1%, respectively, while 12.4%, 85.2%, and 58.6% of participants indicated they would provide intravenous opioids, respectively, for each case.
Table 2 Provision of analgesia by case

1 Participant could choose more than one answer.
IV=intravenous
In 35 responses, participants indicated they would not provide analgesia, and the most common reason (21/35, 60%) for this decision was a belief that pain was not sufficiently severe (Figure 1). In all 61 responses where respondents indicated they would obtain surgical consultation, they also indicated they would provide analgesia. There was no significant relationship between the provision of analgesia and type of training or years of practice (up to 10 versus greater than 10 years, Case 1: p=0.27; Case 3: p=0.72).

Figure 1 Self-reported reasons for withholding analgesia among participants who indicated they would not provide analgesia. (n=35)
Indications for analgesia
Table 3 provides results by etiology for the acute abdominal conditions for which participants indicated they would routinely provide analgesia. The most common was renal colic (138/149, 92.6%), followed by appendicitis (134/149, 89.9%).
Table 3 Reported routine analgesic provision by etiology (n=149)
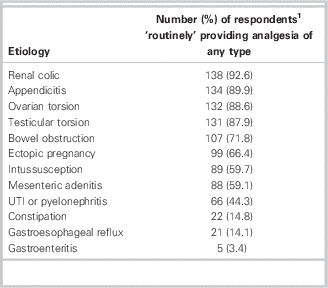
1 Respondents were permitted to choose more than one etiology
UTI=urinary tract infection
Most participants either disagreed (48/139, 34.5%) or strongly disagreed (85/139, 61.1%) that analgesia can mask physical findings enough to miss a diagnosis of appendicitis. Three of 139 participants (2.2%) agreed with this statement.
Discussion
The results of our scenario-based survey of Canadian PEPs’ self-reported rates of analgesia provision for acute abdominal pain are higher than rates reported approximately one decade ago.Reference Kim, Galustyan and Sato 12 , Reference Wolfe, Lein and Lenkoski 23 However, unwillingness to provide opioids for severe pain and concerns regarding analgesia obscuring a surgical diagnosis remain. Our results support the possibility that awareness has increased regarding the importance of providing analgesia to children with acute abdominal pain. Our findings are also consistent with a 2013 Canadian survey of PEPsReference Ali, Chambers and Johnson 24 that found only 4% of respondents stated they would withhold analgesia in the case of a child with suspected “surgical abdomen.” However, both the 2013 self-reported finding and our findings may be incongruent with directly observed practice. In a 2004 retrospective medical record review of 290 children referred to the surgical service with abdominal pain in a Canadian tertiary care centre, only 14% received analgesia.Reference Green, Kabani and Dostmohamed 25 More recently, a 2012 large Canadian multi-centre retrospective medical record review found that two-thirds of children with suspected appendicitis received analgesia.Reference Thompson, Schuh and Gravel 20 Other investigators have found that most survey respondents (64%) supported the concept of providing pre-diagnostic analgesia; however, almost 70% reported that pain treatment was rarely, if ever, given.Reference Zimmerman and Halpern 26 Wolfe and colleagues found that 75% of emergency physicians reported that patients received analgesia, but this contrasted with institutional audits revealing an actual administration rate of only 30%.Reference Wolfe, Lein and Lenkoski 23 A plausible explanation for our findings is social desirability bias, a well-described phenomenon in survey research.Reference Mindell, Coombs and Stamatakis 27 We sought to identify this bias by providing, as one of our three scenarios, a child with abdominal pain rated 4 out of 10. The fact that 23/145 (15.8%) of respondents indicated they would provide intravenous analgesia in a case of relatively mild abdominal pain suggests that social desirability bias may have played a role in participants’ responses. Another possible contributing factor for this difference between self-report and practice might be patient refusal of analgesia. Whatever the reasons, this discrepancy highlights the need for knowledge translation initiatives such as the development of evidence-based pain management policies across EDs.
Historically, the reluctance among clinicians to provide analgesia to patients with acute abdominal painReference Kim, Galustyan and Sato 12 , Reference Ayoade, Tade and Salami 28 , Reference Jawaid, Masood and Ayubi 29 was thought to be due to concerns of obscuring the diagnosis of appendicitis,Reference Falch, Vicente and Häberle 30 , Reference Nissman, Kaplan and Mann 31 leading to a delay in surgical management.Reference Armstrong 32 , Reference Vane 33 In a number of previous surveys of emergency physiciansReference Wolfe, Lein and Lenkoski 23 , Reference Ayoade, Tade and Salami 28 and surgeonsReference Villain, Wyen and Ganzera 19 , a large proportion of respondents chose not to provide analgesia until after surgical consultation. This practice has long impeded timely administration of analgesiaReference Mills, Shofer and Chen 34 or led to analgesia being withheld altogether.Reference Grundmann, Petersen and Lippert 35 In contrast, in all cases in our survey where participants sought surgical consultation, they indicated they would provide analgesia. Among cases where participants indicated they would withhold analgesia, only 5/35 (14%) indicated this was because they believed it would obscure a surgical condition. This shift in self-reported practice may reflect an increased acceptance that analgesia does not hinder the physical examination. Alternatively, it might suggest greater reliance on diagnostic imaging,Reference Sivit 11 , Reference Smink, Finkelstein and Garcia Peña 36 , Reference Neighbor, Baird and Kohn 37 compared to the physical examination.Reference Hashikawa, Burke and Pallin 38 Still, we believe that 14% remains unacceptably high; ample evidence currently supports the pre-diagnostic administration of analgesia.Reference Manterola, Astudillo and Losada 13 , Reference Poonai, Paskar and Konrad 14 , Reference Gallagher, Esses and Lee 39 - Reference Thomas and Silen 46 Furthermore, although the proportion of respondents withholding analgesia due to the belief it may mask a surgical diagnosis is significantly lower than reported in other studies, it still portends a delayed approach to providing analgesia in children with abdominal pain and emphasizes the need for wider knowledge translation.
Although the majority of respondents indicated they would provide analgesia in an appendicitis scenario (and AAP recommends to provide systemic opioids for severe painReference Fein, Zempsky and Cravero 40 ), less than two-thirds of survey respondents reported a willingness to provide intravenous opioids, despite a pain score of 8 out of 10. There are several possible explanations. First, despite ample evidence demonstrating opioids to be effective agents for pain associated with appendicitis,Reference Manterola, Astudillo and Losada 13 , Reference Poonai, Paskar and Konrad 14 , Reference Gallagher, Esses and Lee 39 , Reference Sharwood and Babl 41 concerns of adverse effects in children may still exist. Second, uncertainty of the diagnosis presented in the case scenario may have resulted in less willingness to provide opioids. Goldman and colleagues described this phenomenon, whereby morphine was given more commonly to children with a higher probability of appendicitis.Reference Goldman, Crum and Bromberg 4 Similarly, a significant number of respondents indicated they would provide immediate oral analgesia to patients who were vomiting or due for surgical consultation. This may reflect a reluctance to provide intravenous opioids as a first-line therapy.
Our findings highlight an important phenomenon regarding the reasons that physicians reportedly choose not to administer analgesia. All the scenarios in our survey depicted children with at least 4/10 abdominal pain. Among cases where respondents withheld analgesia, the most common reason cited was a belief that pain was not severe enough. This finding is incongruent with the WHO recommendationsReference Brennan, Carr and Cousins 16 that analgesia be routinely provided for children with pain scores of 4/10 or greater. These recommendations further advise that physicians base their decision to offer analgesia on the patient’s self-report of pain, rather than the clinician’s opinion of how much pain should exist for a particular clinical situation.Reference Brennan, Carr and Cousins 16
Assuming our results are more indicative of opinions rather than actual practice, our findings suggest that the change in reported practice of providing analgesia to children with acute abdominal pain has altered clinical opinion in favor of therapy. This may be due to increased awareness of the importance of appropriate pain management, improved understanding of analgesic effectiveness, or increased use of diagnostic imaging. More importantly, our findings suggest that in contrast to several decades ago, PEPs today may be willing to adopt such initiatives because, in general, they widely endorse providing analgesia. As a result, we feel future pain management policies should incorporate tools to help clinicians recognize and quantify pain in children and identify appropriate evidence-based therapies so that actual practice patterns can better reflect what is reported in surveys.
In addition to limitations inherent to any survey design, there are several additional limitations specific to our study that should be considered. Evidence suggests that pain score documentation in the ED is associated with increased use of analgesia.Reference Drendel, Brousseau and Gorelick 7 , Reference Kellogg, Fairbanks and O’Conn 47 Providing participants with a pain score may have thus artificially inflated their decision to provide analgesia. In addition, the PERC database included physicians who practiced primarily in a tertiary care setting. Increased familiarity with pediatric abdominal emergencies, more timely access to diagnostic imaging, and potentially greater awareness of current literature may have resulted in higher rates of reported analgesic provision. For these reasons, our findings may not be generalizable to community settings and general emergency physicians. In addition, our scenarios—based on actual cases of abdominal pain—were chosen because they varied in their diagnostic clarity. It has been shown that analgesia is more likely given in cases with a greater diagnostic certaintyReference Goldman, Crum and Bromberg 4 and there remains the possibility that the scenarios were sufficiently clear to the respondent such that this inflated reported rates of analgesic provision. Despite our favorable response rate of over 70%, up to 9/149 (6%) of respondents did not answer questions pertaining to the primary outcome. We do not feel that this constituted a threat to external validity or overall results of the study because the response options were comprehensive and open-ended and the number of non-respondents was relatively low. In keeping with good practice for clinician-led surveys,Reference Burns, Duffett and Kho 22 and the requirements of our ethics board, we did not force responses. Finally, the results of this survey did not evaluate PEPs’ actual practice regarding analgesic timing or dosing. These are all well-described components of suboptimal analgesia in childrenReference Ali, Chambers and Johnson 1 - Reference Herd, Babl and Gilhotra 5 and issues that could be explored in future work.
Conclusions
PEPs’ self-reported rates of providing analgesia for acute abdominal pain were higher than previously reported, and appeared unrelated to requests for surgical consultation. However, an unwillingness to provide opioid analgesia, belief that analgesia can obscure a surgical condition, and failure to take patient self-reported pain at face value remain, suggesting that the need exists for further knowledge translation efforts.
Competing Interests: Funding received from Department of Paediatrics Resident Research Grant, Western University, London, ON. No other competing interests declared.
Supplementary material
To view Supplementary material for this article, please visit http://dx.doi.org/doi:10.1017/cem.2015.112






