INTRODUCTION
A widespread increase in the number of reported cases of a novel influenza A virus (H1N1) prompted the World Health Organization (WHO) to announce a global influenza pandemic alert on 11 June 2009 [1]. As of 30 June 2009, over 100 countries have reported 70 893 confirmed cases (311 deaths) of H1N1 infection [2] and numbers continue to increase daily.
Despite the relatively low virulence and mildness of symptoms immediately associated with H1N1, people in different countries are encouraged to remain vigilant due to the uncertainty of the potential associated medical complications [Reference Fraser3]. In Hong Kong, the first confirmed case, a traveller from Mexico, was reported on 1 May 2009, leading to the closure and isolation of the Metropark Hotel and to the quarantine of 350 guests and staff from 1 to 8 May 2009 [4]. The number of confirmed cases then increased to 726 on 30 June 2009 [5].
Recent global outbreaks such as the SARS epidemic have focused attention on the importance of understanding community responses to emerging infectious diseases. SARS-related perceptions and behaviours changed dramatically during the early phase of the outbreak and the negative psychological effects of the outbreak persisted in the post-SARS period [Reference Lau6–Reference Wong8]. Similar studies of psychological responses to H5N1 in the general public have been conducted previously [Reference Lau9, Reference Lau10].
Two reports investigated community responses towards H1N1 in Hong Kong [Reference Lau11] and in the UK [Reference Rubin12] around the same time period (7–9 May and 8–12 May). The Hong Kong study documented high vigilance, which contrasted with observations of the European study. For instance, the prevalence of avoiding crowded places and washing hands more frequently were 54·9% and 73·6%, respectively, in Hong Kong, compared to 4·9% and 28·1% in Europe.
Since the Hong Kong government was committed to an initial policy of containment, their responses may have been more stringent and different from other countries including the USA and the UK, but were in line with those of mainland China. For instance, a 14-day class suspension was applied to a secondary school on 28 May 2009 when one pupil contracted the disease [13]. When the first non-imported case was reported on 10 June 2009 [14], all kindergartens, primary schools and special school classes in Hong Kong were suspended starting from 12 June 2009 until the subsequent school year [15]. Some general outpatient clinics were also converted to designated fever clinics. Although the UK also closed some schools for the same reason and had telephone triage and home visits for suspected cases, other measures were not in place.
This study investigated the changes in people's H1N1-related knowledge (e.g. misconceptions about modes of transmission), perceptions (e.g. risk perceptions, evaluation of governmental performance, and perceived clinical properties of H1N1), behaviours (e.g. the use of preventive measures and avoidance of visiting different places) and negative psychological responses (e.g. worry about contracting H1N1 and severe emotional disturbance) in the general population during the ‘pre-community-outbreak phase’ of the H1N1 epidemic in Hong Kong (1 May to 9 June 2009).
During the study period (7 May to 6 June 2009), all confirmed cases were either imported or related to imported cases. The three rounds of surveys were conducted from day 7 to day 9 (S1, 7–9 May, n=550), during which only one imported H1N1 case was detected in Hong Kong on 1 May; from day 14 to day 17 (S2, 14–17 May, n=201), when the number of imported H1N1 cases moderately increased to two on 14 May; and from day 35 to day 37 (S3, 4–6 June, n=248), when the number of imported cases sharply increased to 30 on 4 June. Thus the study period (7 May to 6 June) covered almost the entire ‘pre-community-outbreak phase’ of the local epidemic (1 May to 9 June 2009).
MATERIALS AND METHODS
Sampling and data collection
The study population comprised all Chinese Hong Kong adults aged between 18 and 60 years. Anonymous telephone surveys were conducted using a structured questionnaire which took about 20 min to complete. Random telephone numbers were selected from updated telephone directories. The last two digits of the selected number were randomized in order to include some unlisted numbers. Over 95% of households in Hong Kong have a landline telephone [16]. Interviews were conducted from 06:30 to 22:00 hours to avoid over-representation of non-working individuals. One participant was selected from each household contacted using the last-birthday rule. Verbal consent was obtained from respondents and the study was approved by the Chinese University of Hong Kong. A total of 1621 eligible respondents were identified and 999 completed the interview, giving a response rate of 61·6% (999/1621).
Measures
The items were modified from questionnaires used in some avian influenza [Reference Lau9, Reference Lau17, Reference Lau18] and SARS [Reference Lau10, Reference Lau19, Reference Lau20] studies. The baseline data of this study have been described elsewhere [Reference Lau11]. Sociodemographic data were recorded. The questions related to misconceptions and knowledge about modes of transmission, perceptions related to H1N1 (risk perceptions and perceived clinical properties), attitudes towards governmental measures (preparedness of the local health system, compliance to governmental policies and recommendations, and confidence in the government), practice and perceived efficacy of preventive measures (hand-washing, face mask use, and avoiding visiting different places) and negative psychological responses (worry about infection and severe emotional disturbance). The items are described in Tables 1–6.
Table 1. Background characteristics of the respondents
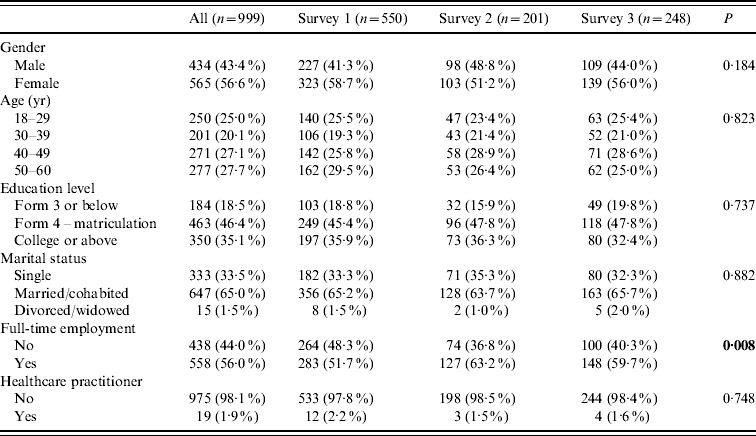
From the latest Hong Kong census data (http://www.censtatd.gov.hk/hong_kong_statistics/index_tc.jsp).
Gender: male (45·7%); Age: 18–29 (22·2%); 30–39 (25·0%); 40–49 (28·8%); 50–60 (24·0%); Education level: Form 3 or below (37·2%); Form 4 – matriculation (34·8%); College or above (28·0%); Martial status: single (32·4%); married (57·8%); divorced/widowed (9·8%).
In general, the sociodemographic characteristics were comparable across the three surveys.
Table 2. Knowledge of the mode of transmission and fatality of H1N1 influenza
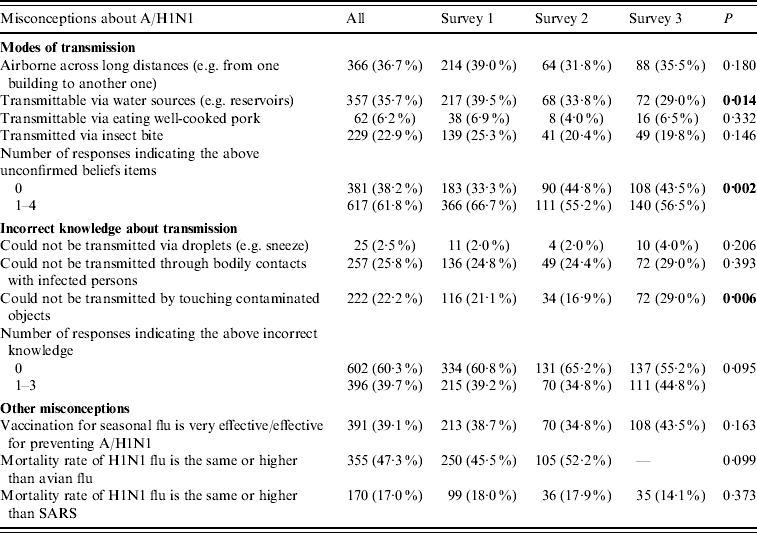
Table 3. Attitudes and related perceptions associated with the H1N1 epidemic
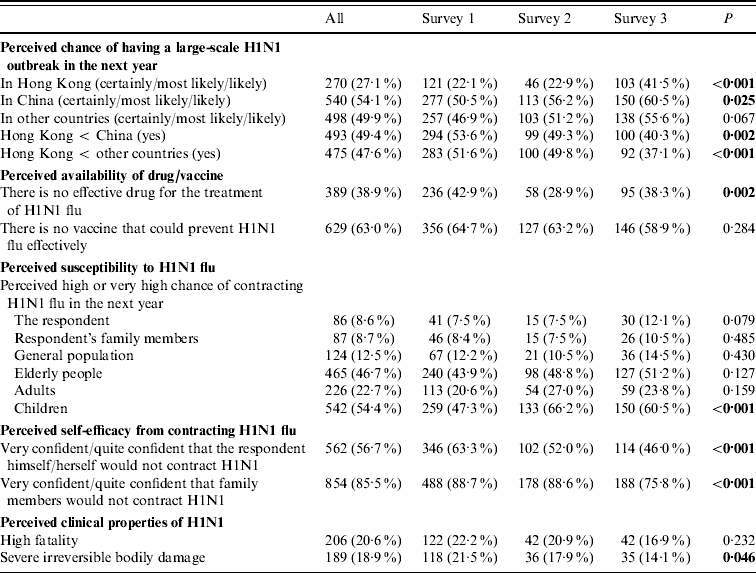
Table 4. Evaluations towards government preparation and recommendations

Table 5. Practices and perceived efficacy of preventive measures

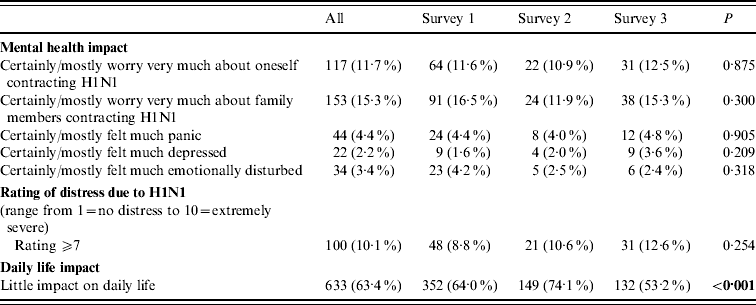
Table 6. Mental health impact of H1N1 influenza
Data analysis
The distribution of responses was tabulated for each of the three surveys. Differences across the three surveys were tested using the χ2 test. Correlations between variables have been analysed in another paper [Reference Lau21]. SPSS version 16.0 (SPSS Inc., USA) was used to analyse the data and P values <0·05 were considered significant.
RESULTS
Background characteristics
Variations in the distribution of gender, age, education levels and marital status were not significant across the three surveys. Employment status was the only parameter showing significant inter-survey differences. Distributions were comparable to those of the recent census data (see notes to Table 1). Of the respondents 56·6% were female, 54·8% were aged between 40 and 60 years, 56·0% were employed full time, and 35·1% had received post-secondary education.
Misconceptions about modes of transmission and fatality related to H1N1
Prevalent unconfirmed beliefs about H1N1 included: ‘H1N1 could be transmitted via airborne aerosols across long distances (from one building to another)’ (S1, 39·0%; S3, 35·5%); ‘via water sources (e.g. rivers or reservoirs)’ (S1, 39·5%; S3, 29·0%); ‘via insect bites’ (S1, 25·3%, S3, 19·8%); or ‘via eating well-cooked pork’ (S1, 6·9%, S3, 6·5%). Over 50% of all respondents possessed at least one of the above misconceptions, although the prevalence declined significantly over time (S1, 66·7%, S3, 56·5%; P<0·002, Table 2).
Very few people did not know that H1N1 could be transmitted via droplets (S1, 2·0%, S3, 4·0%; P>0·05). A sizable proportion did not know that H1N1 could be transmitted through having bodily contact with affected persons (S1, 24·8%, S3, 29·0%; P>0·05), or by touching contaminated objects (S1, 21·1%, S3, 29·0%; P<0·05, Table 2). Nearly 40% of all respondents answered at least one of the three questions incorrectly (S1, 39·2%, S3, 44·8%; P>0·05, Table 2).
Of all respondents, 39·1%, 47·3% and 17·0%, respectively, misunderstood that vaccination against seasonal influenza could prevent H1N1 effectively, that the fatality of H1N1 was the same or higher than that of human avian influenza, and that the fatality of H1N1 was the same or higher than that of SARS. Comparisons across time were not statistically significant (Table 2).
Perceptions related to the H1N1 epidemic
Risk perceptions
The prevalence of respondents anticipating a large-scale outbreak in Hong Kong (22·1–41·5%, P<0·001), in mainland China (50·5–60·5%, P<0·05) and in other countries (46·9–55·6%, P=0·067, Table 3) in the coming year all increased sharply across the three surveys. Over time, substantial but fewer respondents believed the chance of having an outbreak in Hong Kong in the next year was smaller than that in China (53·6–40·3%) or in other countries (51·6–37·1%, P<0·001, Table 3).
Respectively, 8·6%, 8·7% and 12·5% of all respondents perceived themselves, their family members and the general population as having high or very high chances of contracting H1N1 in the next year; similar figures with regard to adults and elderly people were 22·7% and 46·7%, respectively. Trends over time for the above-mentioned figures were not statistically significant (Table 3). Perceived susceptibility for children increased significantly over time (S1, 47·3%, S3, 60·5%; P<0·001, Table 3).
Perceived self-efficacy for HIN1 prevention among respondents declined over time. Fewer respondents were confident that they themselves (S1, 63·3%; S3, 46%; P<0·001) or their family members (S1, 88·7%; S3, 75·8%; P<0·001) would not contract H1N1 in the next year (Table 3).
Perceived clinical properties of H1N1
Around 21% of all respondents perceived H1N1 to be associated with high fatality. The comparison across surveys was not statistically significant (P>0·05, Table 3). Fewer respondents believed that H1N1 would result in severe irreversible body damage (S1, 21·5%, S3, 14·1%; P<0·05, Table 3). Around 39% and 63%, respectively, of all respondents believed there were currently no effective drugs or vaccines for treatment and prevention of H1N1 (Table 3).
Attitudes towards governmental measures
The majority of all respondents stated they would comply with quarantine measures, declare influenza symptoms to immigration control, or consult a doctor immediately in the case of influenza-like illness (ILI) symptoms. Trends over time were non-significant (90·8–98·1%, Table 4). Confidence in the government's ability to control a large-scale local H1N1 outbreak was high but declined slightly over time (S1, 80·5%; S3, 73·8%; P<0·05). The perception that vaccines, medications and personal protection equipment in Hong Kong were inadequate ranged from 30·1% to 41·1% (Table 4). The mean rating of governmental performance in dealing with H1N1 declined across the three surveys (from 7·3 in S1 to 6·7 in S3; P<0·001, Table 4).
Practices and perceived efficacy of preventive measures
Frequent hand-washing
In all three surveys, the majority of respondents (73·7%) washed their hands more frequently than prior to the identification of the first imported H1N1 case, with 91·1% washing their hands at least six times a day (P=0·89, Table 5). However, much fewer respondents believed frequent hand-washing to be very efficacious in preventing H1N1 (S1–S3, 35·6%, 27·9%, 21·4%, respectively; P<0·001, Table 5).
Using face masks in public venues
Fewer respondents would definitely or mostly wear a face mask regularly in public venues over time (S1, 23·8%; S3, 16·5%; P=0·068) and fewer perceived that such a measure was very efficacious in controlling H1N1 (S1, 35·6%; S3, 21·4%; P<0·001, Table 5). The prevalence of respondents wearing a face mask when suffering from ILI symptoms remained very high (S1, 89·6%; S3, 86·7%; P>0·05).
Avoid visiting different places
Fewer respondents avoided crowded places, going out, travelling to other countries or visiting hospitals over the survey periods (S1, 47·8–67·2%; S3, 35·9–59·7%; Table 5, P<0·05). Consistently, fewer respondents believed that avoiding crowded places is a very efficacious means of preventing the spread of H1N1 (S1, 23·6%; S3, 12·9%; P<0·01).
Distress
The prevalence of respondents who were very worried about themselves (11·7%) or their family members (15·3%) contracting H1N1 remained relatively low and stable over time (P>0·05, Table 6). Similar non-significant trends were observed in the prevalence of respondents who were very panicky, felt very depressed or felt very emotionally disturbed due to H1N1 (2·2–4·4%). Fewer respondents felt that H1N1 was having little impact on their daily life (S1, 64%; S3, 53·2%; P<0·001).
DISCUSSION
Misconceptions about modes of transmission of H1N1 were prevalent (e.g. 22·9% believed the virus could be transmitted through insect bites), although the prevalence of misconceptions decreased over time. Similar common misconceptions about modes of transmission relating to human avian influenza were reported in 2006 [Reference Lau10]. This finding may reflect difficulties in the effective transmission of knowledge about risk from emerging infectious diseases. Of particular importance is the lack of knowledge about transmission through contact with contaminated objects. Respondents underestimated the importance of this route, perceiving sneezing/coughing as the sole mode of transmission of H1N1. Educational strategies are important in clarifying this misconception.
There is also confusion in the minds of the public between avian flu and H1N1. A recent study showed that 43% of the Hong Kong general public mixed up the two infections and that about half believed H1N1 to have the same or higher fatality as avian influenza [Reference Lau17]. Other studies of avian influenza found that, as during the SARS epidemic, higher levels of perceived fatality are associated with higher levels of panic [Reference Lau18]. As 17% of the respondents of this study believed H1N1 to be associated with the same or higher fatality as SARS, it is likely that the public overestimated the fatality of H1N1 at the same time as underestimating the fatality of avian influenza. This is despite widespread dissemination of statistics and regular public announcements by the government [5] and media. As avian influenza and H1N1 may coexist in the near future, public education to distinguish between different types of respiratory infectious diseases and to clarify the mild nature of H1N1 would help support a response commensurate with evidence.
While some countries have treated H1N1 as a mild disease, the containment policy in Hong Kong led to stringent governmental measures, including quarantine and suspension of all primary schools and kindergartens on confirmation of community spread. The mitigation strategy has been implemented since 10 June 2009, with conversion of some general out-patient clinics into fever clinics. The costs are escalating, with more than one billion US$ allocated to purchase H1N1 vaccines once available. The proactive response by the government is in general supported by the community [Reference Lau11], although such measures may have a side-effect of creating an impression that H1N1 is a serious disease, which is apparently true as our data showed high perceived fatality and bodily damage being associated with H1N1.
Most (over 90%) of the public would comply with governmental recommendations for preventive measures, and 73·8% of the public in the third survey were confident in the government's ability to control a local large-scale outbreak, although levels of confidence and ratings towards the government had waned by small yet statistically significant margins. This could be because in the first survey the majority of respondents had expressed the view that Hong Kong would escape from having a local H1N1 outbreak. However, in reality, it turned out that the highly supported quarantine policy and interceptions at border checkpoints were unable to prevent community spread within Hong Kong.
Our study also highlighted the ongoing uncertainty among the public about the level of preparedness of the local health system in stocking enough vaccine, drugs and personal protection equipment. Such doubts may be related to the local experience of SARS. The government responded by allocating one billion US$ to purchase vaccines when they are available. It is important to monitor the level of public support for government policy in order to shape efforts for risk communication and disease control effectively.
Comparisons of results over time showed a shift of public knowledge and perception. As the number of confirmed cases increased from two to 30 within the 3 weeks of the study period, the public rightly perceived a greater chance of having a large-scale local outbreak in the next 12 months, with an increase from 22% to 42%, although many respondents still expected that the chance of an outbreak in Hong Kong would be lower than that in China or other countries. Over time, fewer respondents also believed that the disease would result in severe irreversible bodily damage. These changing perceptions followed the temporal pattern of the H1N1 epidemic and reflected greater understanding over time.
During this pre-community-outbreak phase, most people still did not perceive a high susceptibility of contracting the disease (7·5–12·1%). This may explain the relatively modest level of distress (<5% were panicking) which remained unchanged over the study period, despite the fact that about 21% of the respondents perceived H1N1 to be associated with very high fatality. It will be interesting to observe how such perceptions and inter-relationships change after the pre-community-outbreak phase of the local epidemic.
Over time, more respondents felt that H1N1 was having an impact on their daily lives, although the trend for avoiding visiting different places declined significantly. Avoiding going to different places may be seen as a preventive measure, but our figures show that only a diminishing minority perceived avoiding visiting crowded places as an efficacious means of H1N1 prevention. It seems that some people may avoid going out because of anxiety (12% worried about contracting H1N1), although they were uncertain about the efficacy for prevention. Avoidance of going out may harm the already troubled economy in Hong Kong. Some avian influenza studies in Hong Kong further showed that avoidance of visiting different places may be associated with distress [Reference Lau18], which is supported by the recent European H1N1 study [Reference Rubin12]. Our data therefore showed that H1N1 made a modest impact on life of the general public even during the pre-community-outbreak phase of the epidemic.
During the study period, the Hong Kong government gave specific guidance on health, e.g. frequent hand-washing, avoiding touching nose and eyes, wearing face masks in public areas, consulting a doctor immediately and avoiding travelling when suffering from ILI symptoms. However, the advice of wearing face masks regularly in public areas was not given by the government, although it was given during the SARS period. The prevalence of respondents reporting wearing masks regularly in public areas declined from 23·8% in S1 to 16·5% in S3 (P<0·05). Evidence of the effectiveness of wearing face masks is mixed and different governments have different policies [Reference Cowling22, 23]. However, the prevalence of wearing face masks when suffering from ILI symptoms was very high throughout the surveys. Wearing face masks to prevent spread of ILI to others may have become an established practice in Hong Kong.
The public response to advice on frequent hand-washing has also been heeded, possibly building on heightened awareness from the SARS experience. The government can hence turn emerging infectious diseases crises into opportunities for promoting hygiene.
However, over time, fewer people responded that hand-washing was very efficacious for H1N1 prevention, possibly signifying less impact of the health messages from the government as the numbers of reported cases increased despite very intensive publicity on education for frequent hand-washing. This response presents a greater challenge for the authorities responsible for controlling the disease.
This study has several limitations. First, the response rate was modest, although comparable to those of other relevant published studies [Reference Lau18, Reference Lau24, Reference Tang and Wong25]. However, the gender and age distributions were comparable to those of the census data [26]. Moreover, not all landlines were listed in the phone books (sampling frame) although no cost is involved in the listing. We randomized the last two digits of the selected phone number so that some unlisted numbers would be covered by the study.
Second, results were self-reported. Measurement errors (e.g. frequency of hand-washing) and social desirability bias may exist although the study was anonymous. Third, Hong Kong went through a unique SARS experience, and results may not be comparable with those of other countries.
In summary, this paper describes different aspects of community responsiveness and preparedness towards H1N1 in the initial pre-community-outbreak phase of a local epidemic. Misconceptions about modes of transmission and overestimation of fatality, although less prevalent, were still widespread. Anxiety and avoidance behaviours in the general public were modest but noticeable. While compliance with governmental recommendations for adoption of preventive measures remained high, there were still doubts about governmental preparedness. Throughout the pre-community-outbreak phase, the public continued to support governmental policies and actions, even though such measures were at variance with other countries in Europe and the USA.
While other countries have taken a more relaxed view of the spread within their communities, Hong Kong and China have been more hawkish – instituting strict border controls and enacting quarantine laws. Hong Kong respondents heed governmental recommendations on preventive measures whereas European respondents gave a muted response. As we are now facing a pandemic, international comparisons and global responses are very important as community responses in one country may affect the spread of the disease in other countries. Further analyses of global policies and responses are needed. This study represents one of the first steps towards that end.
Public attitudes towards the disease may become more tolerant – more people felt susceptible, yet more people perceived lesser harm and fewer avoided going out. Lower perceived efficacy of preventive measures is also of concern. Since different types of emerging infectious diseases may have become a continuum in the eyes of the general public, it is important to encourage the public to remain vigilant and follow government guidance as the pandemic unfolds and possibly changes in nature. The ongoing surveillance of public attitudes now in place in Hong Kong will provide information to guide policy-makers. The results of this initial series of surveillance studies indicate that continuous evidence-based public-health education is required at all stages of the pandemic, including its initial pre-community-outbreak stage.
ACKNOWLEDGEMENTS
The authors thank all participants of this study. Thanks are extended to Mr Nelson Yeung for help with the editing of the paper, Mr Tony Yung and Mr Johnson Lau for assistance in the preparation of the questionnaire, Ms. M. W. Chan, Mr Mason Lau, and Ms. Cheri Tong for coordination of the telephone survey, and all colleagues who served as telephone interviewers of this study. The study was supported by the Research Fund for the Control of Infectious Diseases from the Food and Health Bureau.
DECLARATION OF INTEREST
None.







