A fundamental principle in antimicrobial stewardship is that of de-escalation, in which a broad-spectrum antibiotic is rapidly changed to an antibiotic with a narrower spectrum of activity once culture data allow.Reference Masterton1 The practice of de-escalation is supported by the Infectious Disease Society of America’s Antibiotic Stewardship Guidelines.Reference Barlam, Cosgrove and Abbo2 It offers not only an improvement in antibiotic resistance patterns but also a decrease in antibiotic-related adverse events and cost savings.Reference Teshome, Vouri, Hamptom, Kollef and Micek3–Reference Lee, Wang and Lee5 Despite recognition of the utility and safety of antibiotic de-escalation, this practice has been inconsistently applied.Reference Masterton1, Reference Madaras-Kelly, Jones and Remington6–Reference Shime, Satake and Fujita8 The electronic medical record offers new opportunities to facilitate de-escalation with best practice alerts (BPAs) prompting evidence-based clinical decisions.Reference Revolinski9, Reference Schulz, Osterby and Fox10 The impact of electronic alerts on antibiotic de-escalation, however, has not previously been examined.
The Mercy Health System Antimicrobial Stewardship Program instituted an automated antibiotic time-out alert within its electronic medical record in January 2017, independent of the current research study. This electronic prompt arises to the provider at 72 hours for all patients receiving broad-spectrum antibiotics and encourages de-escalation. Details of the alert are available in the supplementary materials. The current study sought to analyze the real-world impact of this alert on broad-spectrum antibiotic de-escalation.
Methods
A retrospective cohort study was performed within Mercy Hospital, St Louis, a 1,252-bed community teaching hospital in St Louis, Missouri. The primary outcome was defined as the proportion of patients in whom antibiotics were de-escalated at 72 hours in the year before the initiation of the antibiotic time-out alert (2016) and the year following (2017). Secondary outcomes included comparison of total antibiotic days, antibiotic cost per day, hospital length of stay, antibiotic-related adverse events, and in-hospital mortality between patients whose antibiotics were de-escalated and those who continued on broad-spectrum agents.
The pre-alert group was selected from existing reports of all antibiotics prescribed at Mercy Hospital, with random selection of 10 patients from each month in 2016 who had received broad-spectrum agents for ≥72 hours. The post-alert group was selected from reports of all hospitalized patients receiving an automated antibiotic time-out alert at 72 hours, with a random sampling of 10 patients for each month in 2017.
A manual review of the electronic medical record was performed to assess study eligibility and extract data points. Inclusion criteria included age ≥18 years, admitted to Mercy Hospital in the year 2016 (pre-alert group) or 2017 (post-alert group), and receiving broad-spectrum antibiotics for ≥72 hours. Exclusion criteria included antibiotics utilized for an infection diagnosed prior to hospitalization and hospitalization extending ≥20 days with utilization of 3 or more courses of antibiotics for multiple indications. De-escalation in such cases was difficult to define. Broad-spectrum antibiotics were defined to include those for which the alert had been built to fire, as described in the Supplementary Materials online.
Proportions of antibiotic de-escalation both before and after the initiation of the antibiotic time-out alert were analyzed. Patients were considered eligible for de-escalation if their antimicrobial cultures were either negative or were sensitive to a narrower-spectrum antibiotic. Any de-escalation was defined as discontinuation of any of the broad-spectrum antibiotics included in the alert. Optimal de-escalation was defined as cessation of all included broad-spectrum therapies.
The Pearson χ2 test was utilized to compare proportions of de-escalation between the 2 groups. P < .05 was defined as statistical significance, with use of the 95% confidence interval. A power of 0.79 was achieved for the primary outcome with the analyzed sample sizes and observed events rates as described below. The study was approved by the Mercy Hospital Institutional Review Board prior to its implementation.
Results
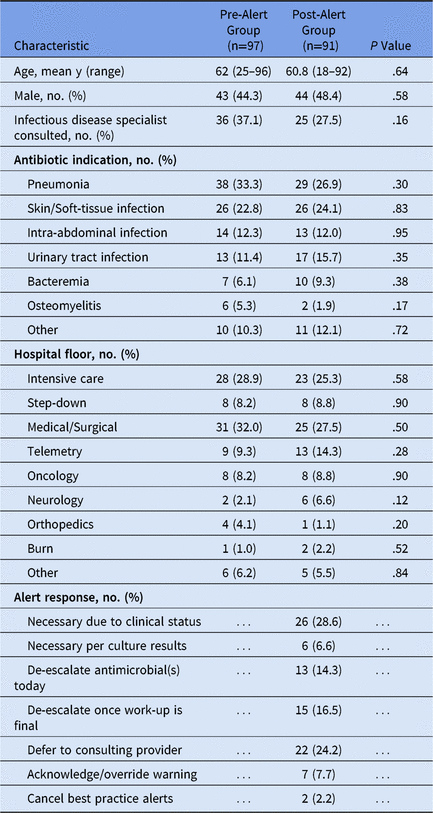
Of the 120 patients in the pre-alert group screened for eligibility, 113 were included for analysis. 1 patient was excluded for previously diagnosed infection and 6 patients were excluded for prolonged hospitalizations. Of these 113 patients, 97 (85.8%) were eligible for de-escalation by culture data. In the post-alert group, 107 of 120 screened patients were analyzed. 3 were excluded for having received <72 hours of broad-spectrum antibiotics, 1 was excluded for a previously diagnosed infection, and 9 were excluded for prolonged hospitalizations. Culture data culture data revealed that 91 of these 107 patients (85.0%) were eligible for de-escalation. Characteristics of study patients are included in Table 1.
Table 1. Patient Characteristics in the Pre-Alert and Post-Alert Groups
Primary outcomes demonstrated that, among eligible patients, 35.1% in the pre-alert group and 55.0% in the post-alert group had any of their broad-spectrum agents de-escalated (95% CI, −0.3491 to −0.0488; P =.0095). Optimal antibiotic de-escalation in the pre-alert group was 13.4% compared to 31.9% in the post-alert group (95% CI, −0.3126 to −0.0567; P = .0042) (Fig. 1). De-escalation proportions after the alert’s implementation were consistent over the course of the study period (see Supplementary Materials online).
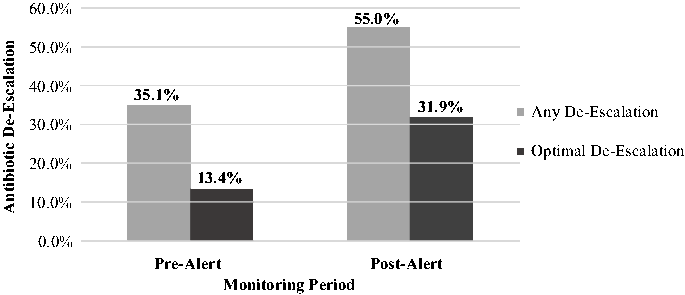
Fig. 1. Proportions of antibiotic de-escalation before and after implementation of an automated antibiotic time-out alert.
Among the secondary outcomes, patients whose antibiotics were de-escalated experienced the following: fewer total antibiotic days (6.9 vs 9.0 days; P = .002), shorter hospital lengths of stay (8.5 vs 11.5 days; P = .002), and fewer antibiotic-related adverse events, including any allergic reaction, Clostridium difficile infection, antibiotic-associated diarrhea as attributed by the provider, or any other reaction attributed by the provider to the antibiotic (11.9% vs 16.3%; P = .390) than their counterparts whose broad-spectrum agents were continued (see Supplementary Materials online). No difference in antibiotic cost per day of therapy ($34.51 vs $28.07; P = .266) or mortality (11.0% vs 11.0%; P = .976) between these groups was observed.
Discussion
De-escalation of broad-spectrum antibiotics is a cornerstone of antimicrobial stewardship efforts, yet this practice has been inconsistently applied.Reference Masterton1, Reference Madaras-Kelly, Jones and Remington6–Reference Shime, Satake and Fujita8 This observational study provides the first evidence that automated antibiotic time-out alerts are effective in improving antibiotic de-escalation.
One strength of this study was the analysis of not only any de-escalation but also optimal de-escalation, finding positive results in both groups. With this approach, we sought to more comprehensively analyze de-escalation practices by determining whether the antibiotics with the narrowest possible spectrums were being selected. The antibiotic time-out alert was also implemented within a large hospital system with a strong pre-existing antimicrobial stewardship program in place. Notably, hospital stewardship activities were otherwise nearly identical in the pre- and post-alert periods. The fact that de-escalation practices significantly improved in a hospital with an already strong stewardship culture points to the effectiveness of this additional measure. Additionally, the use of an electronic prompt helped to automate a portion of the stewardship efforts and to reduce this time burden on program personnel.
This study had several limitations. First, eligibility for antibiotic de-escalation was based solely on culture data rather than patient factors. Although this provided an objective basis to determine eligibility for de-escalation, it may have overlooked patient-specific factors such as severity of illness and immunocompromised status. Previous research, however, supports the use of antibiotic de-escalation even among critically ill patients.Reference Khasawneh, Mehmood and Zaaqoq11 Additionally, we acknowledge that alerts within the electronic medical record have the possibility of invoking “alert fatigue,” causing providers to become de-sensitized to the automated prompts over time. To minimize this effect, the alert was built to never fire for the same provider twice, to not fire for any subsequent providers if anyone selected “de-escalate antimicrobial(s) today,” and to fire only during daytime hours.
In conclusion, an automated antibiotic time-out alert within the electronic medical record may be an effective tool for encouraging de-escalation of broad-spectrum antibiotics. Further studies on the implementation of this modality are needed to better understand how it can optimally be applied to antibiotic stewardship efforts.
Acknowledgments
The authors thank Jason Redwine for his technological assistance in implementing the automated alert within the electronic medical record. Statistical planning and recommendations were performed by Dr Jimin Ding.
Financial support
No financial support was provided relevant to this article.
Conflicts of interest
All authors report no conflicts of interest relevant to this article.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/ice.2019.197



