Introduction
Respiratory distress often results from conditions such as congestive heart failure (CHF), chronic obstructive pulmonary disease (COPD), asthma exacerbation, and pneumonia. 1 Patients experiencing respiratory distress represent a common presentation for Emergency Medical Services (EMS) providers; EMS personnel play a critical role in decisions related to triage, transport, and initial management of patients with respiratory distress. Non-invasive positive pressure ventilation (NIV) has been shown to improve outcomes in patients with acute pulmonary edema and other forms of respiratory distress. Previous studies suggest that interventions in the prehospital setting can reduce mortality among patients with respiratory distress.Reference Prekker, Feemster and Hough 2 - Reference Kallio, Kuisma, Alaspaa and Rosenberg 6
Advanced Life Support (ALS) providers have adopted continuous positive airway pressure (CPAP), but there have been theoretical concerns about the safety of Basic Life Support (BLS) providers using CPAP. In this report, ALS is defined as Paramedic level-of-care and BLS is defined as basic Emergency Medical Technician (EMT) level-of-care. Critics argue that BLS providers have not been trained to have the critical thinking skills to determine when the use of CPAP is appropriate, nor have they been trained in the tools and skills to adequately monitor CPAP patients. However, a strong argument in favor of CPAP use by BLS providers is that the BLS providers have no other treatment options available for a patient in respiratory distress unless the patient loses consciousness and requires manual ventilation with bag valve mask. Another compelling argument is that patients may benefit from earlier application of CPAP by BLS providers.Reference Wesley 7
A July 2014 National Association of State EMS Officials (Falls Church, Virginia USA) survey of states within the United States showed that 14 states reported using CPAP at the BLS level. 8 The National EMS Information System (NEMSIS; Salt Lake City, Utah USA) was queried to find additional evidence of state usage, and it was determined that 25 out of 50 reporting states and territories are using CPAP at the BLS level. 9 There has previously been evaluation of the application of CPAP by Primary Care Paramedics in Canada who possess levels of training and certification similar to Advanced EMTs in the United States.Reference Cheskes, Thomson and Turner 10 Despite the increased usage and adoption of BLS CPAP around the country, there is a gap in the literature for use of CPAP by Basic EMTs.
In Delaware (USA), BLS providers often arrive on-scene before ALS providers. While CPAP had been used by the three county ALS agencies throughout the state since the late 1990s, CPAP was not previously considered within the scope of practice of state BLS agencies. On average, BLS is on-scene four minutes before ALS for “Respiratory Distress” calls 60% of the time throughout the state. The purpose of this study was to determine whether BLS providers can appropriately identify patients who would benefit from CPAP, apply the device, and monitor the patients prior to ALS arrival.
Methods
Study Design and Setting
This study was a retrospective, observational study using quality assurance data collected from October 2009 through December 2012 throughout the Delaware BLS CPAP pilot program. The study was approved by expedited review from the Christiana Care Health System (Newark, Delaware USA) Institutional Review Board with a waiver of consent. The State of Delaware has a total population of approximately 900,000 and a total square mileage of 1,982. The state is comprised of three counties with different population densities. A total of 72 prehospital BLS agencies exist throughout the state. Delaware BLS providers receive their state certification from the Delaware State Fire Prevention Commission (DSFPC; Dover, Delaware USA), and most in-state training is provided by the Delaware State Fire School (DSFS; Dover, Delaware USA). State EMS medical direction is provided by the Delaware Office of Emergency Medical Services (OEMS; New Castle, Delaware USA) utilizing board-certified emergency medicine physicians. There are nine receiving emergency departments (EDs) within the state and two receiving EDs in neighboring states.
In 2009, the Delaware OEMS and the DSFPC approved a pilot protocol to allow BLS providers to utilize CPAP for patients in respiratory distress. A total of 12 companies throughout the state (four per county) were chosen for participation in the BLS CPAP pilot program. A training program was developed and approved by both the OEMS and DSFS. The training consisted of a 4-hour program, with two hours of presentation and lecture followed by a 2-hour “hands-on” didactic training session. The trainees were evaluated and coached to correct deficiencies during the didactic training sessions. Approved equipment consisted of Food and Drug Administration (FDA; Silver Spring, Maryland USA)-approved, flow-driven CPAP devices and manometer to determine effective CPAP pressure provided to the patient. All participating BLS agencies utilized the Boussignac oxygen-driven CPAP devices (Vygon; Ecouen, France).Reference Templier, Dolveck, Baer, Chauvin and Fletcher 11 A goal pressure of 7.5 cm H2O was chosen for consistency throughout the pilot as a pressure that could be both safe and efficacious.
The pilot protocol called for CPAP to be initiated by BLS providers for patients recognized to be in respiratory distress and/or impending respiratory failure with a history of CHF, asthma, and/or COPD, and who demonstrated spontaneous respirations and a patent, self-maintained airway. The use of BLS CPAP with inclusion and exclusion criteria and monitoring parameters was added to the state BLS standing orders and protocols as a pilot protocol (Table 1). The protocol was initiated by BLS only if they were on-scene prior to ALS arrival. Vital sign inclusion criteria included at least three out of five of the following: tachypnea, tachycardia, hypertension, hypoxia, and verbal impairment. Exclusions to CPAP were: circumstances in which endotracheal intubation or surgical airway were preferred or necessary to secure a patent airway; circumstances in which the patient did not improve or deteriorate despite CPAP; and patients with respiratory distress due to trauma. Patients with suspected non-cardiogenic pulmonary edema due to narcotic abuse/near-drowning could receive CPAP administration by BLS with online medical control approval. Although ALS was still indicated to assist with patient care, a BLS provider continuously monitored any patient for whom CPAP was initiated by BLS. The BLS providers were trained to recognize worsening respiratory failure or declining mental status despite CPAP and to react accordingly by providing bag valve mask ventilation and advanced airway management by ALS during transport.
Table 1 Vital Signs Inclusion Criteria

Data Collection and Analysis
A data collection form was developed and approved by the OEMS and DSFS to be completed for each CPAP use initiated by BLS throughout the pilot period. The form included the agency name, provider name, incident number, Medical Priority Dispatch code, chief complaint, CPAP manufacturer utilized, indication for CPAP (pulse oximetry [spO2] less than 92%, respiratory rate [RR] greater than 24, or cyanosis), contraindications (if applicable), and result of CPAP (spO2 greater than 92%, reduced RR, improved color, or improved mental status). The form also included an independent evaluation by an advanced provider (physician, nurse, respiratory therapist, or paramedic) regarding the CPAP application. The advanced practitioner review included whether CPAP was indicated, applied correctly, appropriately monitored, and whether respiratory status was appropriately managed with comment section. The independent provider then determined if the patient’s outcome was subjectively improved, unchanged, or worsened and signed the form. All CPAP data collection forms were then faxed to the OEMS for review as part of the Quality Assurance (QA) for the pilot program. Patient Care Reports were analyzed to review BLS CPAP application and to obtain Glasgow Coma Score (GCS) and heart rate (HR). The McNemar’s and t-tests were used to determine statistical differences between monitoring parameters before and after CPAP application.
Results
A total of 74 patients had CPAP applied and monitored by BLS during the study period. The three most common chief complaints included difficulty breathing (36.5%; n=27), shortness of breath (31.1%; n=23), and respiratory distress (6.8%; n=5). The majority of study participants were white (83.8%) and approximately one-half were female (44.6%). The age of participants ranged from 10 to 97 years with a median age of 70 years (inter-quartile range: 59.5-83.5).
For all 74 patients (100.0%), CPAP was correctly indicated and applied; CPAP was appropriately monitored for almost all patients (98.6%; 71/72), with two patients having unknown CPAP monitoring status. Respiratory status also was appropriately managed in almost all patients (98.6%; 72/73), with one patient having unknown respiratory management status.
Of the 74 patients, BLS team members indicated overall improvement in the patient’s status after CPAP administration for the overwhelming majority (89.2%; 66/74), whereas 6.8% were unchanged (5/74) and only 4.1% (3/74) experienced a worsened status. Improvement in mental status was reported for 20.3% (15/74) of patients.
The BLS CPAP administration statistically significantly reduced the proportion of patients with spO2 values<92%, a RR>24 breaths per minute, and who were cyanotic (Table 2). Overall, there was an 84% reduction in the proportion of patients with poor spO2 values, a 55% reduction in those experiencing poor RRs, and a 58% reduction in cyanosis.
Table 2 Proportion of 74 Individuals with Each Condition Before and After CPAP Administration
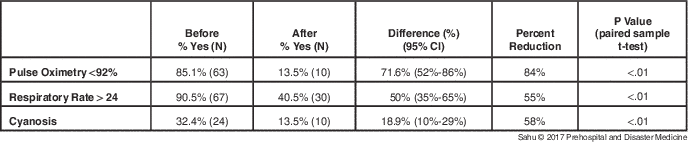
Abbreviation: CPAP, continuous positive airway pressure.
Finally, differences before and after BLS CPAP administration by BLS for three continuous metrics, GCS, HR, and spO2, were examined. All three metrics displayed improvement after CPAP administration (Table 3). Comparing pre-CPAP and post-CPAP values, there was a statistically significant decrease in HR (mean difference [MD]: -10.9; 95% CI, -3.2 to -18.6; P<.01) and a statistically significant increase in spO2 levels (MD: 17.8; 95% CI, 14.2-21.5; P<.01).
Table 3 Means and Standard Deviations for 74 Individuals Before and After CPAP Administration

Abbreviation: CPAP, continuous positive airway pressure.
Discussion
The pilot study of BLS utilizing CPAP for patients in respiratory distress revealed several important findings. First, BLS providers who received additional training in the use of CPAP were able to recognize patients presenting with acute respiratory distress who would benefit from CPAP and to apply CPAP correctly 100% of the time. Patient respiratory status and CPAP were monitored properly by these BLS providers in 98.6% of cases. When BLS arrived prior to ALS and applied CPAP, the majority (89.2%) of patients improved while only 4.1% of patients were observed to have a worsening overall clinical status. It is unknown if the proportion of patients that worsened is different than with ALS-applied CPAP, and further study is needed. The chart review of two patients with “unknown” CPAP monitoring status and one patient with “unknown” respiratory management status indicate that the advanced provider who reviewed the case did not complete the CPAP data collection form. The protocol did not exclude pediatric patients, and there was one CPAP application for a 10-year-old child with a history of intubation for asthma who presented in severe respiratory distress, after consultation with online medical direction. The widespread application in pediatric patients would need to be studied in more depth. Patients receiving CPAP applied by BLS demonstrated overall improvement in spO2 and mental status, with reductions in RR, cyanosis, and HR. Further studies would be needed to determine if there is a downstream morbidity benefit to application of CPAP by BLS.
Although roughly one-half of US states and territories report using some form of CPAP by BLS, 9 there is a paucity of literature in the United States that review the safety and efficacy of BLS administering CPAP. Patients must be recognized as presenting in respiratory distress with a self-maintained airway and appropriate mental status in order to benefit from NIV. Trauma patients with respiratory distress, patients suffering from psychiatric emergencies, unresponsive patients, and patients presenting with spontaneous pneumothoraces generally represent contraindications to the use of NIV, and no cases of BLS administering CPAP to patients with any of these contraindications were found. In the pilot study, BLS providers were able to determine patients in whom the use of CPAP was indicated, to apply CPAP correctly, and to appropriately monitor the status of these patients.
The majority of patients improved after CPAP administration. These results address one of the most common arguments against BLS utilizing CPAP: the lack of a skill set to identify appropriate patients, to apply CPAP, and to monitor its effect. This pilot study demonstrates that BLS providers, with appropriate training, QA processes, and medical direction oversight, possess the critical thinking skills to identify appropriate CPAP candidates and the necessary skills and tools to adequately monitor patients receiving CPAP. The safe application of CPAP by BLS providers could mean earlier application and adoption of this procedure.
This study encompasses different EMS operation models, geographic locations, and populations. The BLS agencies involved in this study are a mixture of volunteer and paid agencies. This distinction is important due to perceived differences in training requirements among volunteer versus paid units. 12 Also, the geographic settings of the three counties in which the 12 BLS CPAP pilot agencies were implemented span the rural, suburban, and urban settings with different population densities. These geographic differences translate to different systems of care.Reference Patterson, Freeman, Moore and Slifkin 13 Given the diverse population densities among the BLS agencies utilizing CPAP in this pilot, the success of this study could be generalized to other BLS agencies throughout the nation. Delaware has a long history of being a microcosm of the nation with its heterogeneous demographics and geographic variations which allow the results to be generalized to the greater context of BLS care in the United States. 14
Limitations
Limitations of this study include the fact that in this two-tiered EMS system, there is generally ALS intercept for respiratory distress calls. Patients whose respiratory status or mental status declined despite the use of CPAP by BLS were able to be managed by both BLS and ALS providers. Additionally, a total of only 74 patients were captured during the pilot protocol period among the 12 BLS agencies participating in the study. While this number is not expansive, the overall benefit to patients receiving CPAP by BLS among varying geographic and BLS agency climates was significant. Also, a comparison was not made between the BLS CPAP pilot patients and a group of patients presenting with respiratory distress who were initially evaluated by BLS agencies without CPAP. The goal of this study was not to evaluate the efficacy of CPAP in the prehospital setting; the purpose was rather to study the feasibility of trained BLS providers to safely and effectively determine the need for CPAP, to administer CPAP, and to monitor patients receiving CPAP. Lastly, a subjective assessment of patients who received CPAP administered by BLS was included. These assessments were performed by an advanced provider (physician, nurse, respiratory therapist, or paramedic) regarding the CPAP application after independently evaluating the patient. The advanced provider determined if the patient’s outcome was subjectively improved, unchanged, or worsened. Cyanosis also was measured subjectively by BLS providers based on standard EMT curriculum training and could vary between providers, which limits its accuracy as a measurement standard. While the nature of a subjective assessment can be considered a limitation, the other metrics used to measure the success of CPAP administration by BLS were felt to support the overall improvement of patients receiving CPAP.
Future Studies
Further studies may address BLS use without subsequent ALS intercept. The timing of earlier intervention by BLS should be assessed to determine if there are ultimate patient outcome benefits. Expanding the BLS scope of practice to include carrying and providing bronchodilator therapy in addition to CPAP may also improve prehospital BLS care for patients in respiratory distress. Additional studies also may assess the use of intermediate levels of EMT providers in the United States for CPAP application. Further studies also may be directed toward examining downstream hospital morbidity and mortality data as well as cost-of-care benefits from earlier application of CPAP by BLS. Expanding the limitations of BLS scope of practice to include CPAP can enable EMS systems to play a greater role in the context of public health through evidenced-based advances. 15
Conclusion
Continuous positive airway pressure can be safely used by BLS providers with appropriate training, QA processes, and medical direction oversight. Patients treated with CPAP by BLS providers were observed to have improvements in their clinical status and vital signs. Further studies may be needed to determine longer term effects on patients and EMS systems from the use of CPAP administered by BLS providers.
Acknowledgements
The authors acknowledge Brian Levine, MD; Jason Nomura, MD; and Barbara Davis, RN, Department of Emergency Medicine, Christiana Care Health System, who helped with manuscript review and submission; the staff of the Delaware Office of Emergency Medical Services, who helped with protocol implementation and data collection; the Delaware State Fire School, who helped with training; and all of the Delaware EMS providers, who helped by caring for and transporting these patients, and with data collection.





