Women throughout the country are still admitted to psychiatric wards with mixed-gender living space. They should be able to expect their safety, privacy and dignity to be given a high priority by the trust and staff with whom they are in contact. However, sexual assault in psychiatric institutions is an issue of perennial concern (Reference GarthGarth, 1989; Reference TonksTonks, 1992; Reference Barlow and WolfsonBarlow & Wolfson, 1997). It is known that in psychiatric populations, childhood sexual abuse is associated with sexual and physical assault as an adult (Reference Lipschitz, Kaplan and SorkennLipschitz et al, 1996). A 1995 study showed that 33% of women in-patients had experienced unwanted sexual comments or molestation although the majority did not report their experiences to staff (Reference Thomas, Bartlett and MezeyThomas et al, 1995). This paper discusses the appropriate staff response to patients that do report assault.
Draft policies on preventing and responding to sexual assault on in-patient wards were published in 1993 (Reference SubotskySubotsky, 1993). This was followed in 1996 by a policy document from the Royal College of Psychiatrists on sexual abuse in psychiatric settings (Royal College of Psychiatrists, 1996). It recommends that a clear policy for dealing with allegations should be a prerequisite and that staff should be properly trained in implementing the policy. It also recommends that adequate procedures must be in place to ensure that incidents are not being ‘hushed up’ and observes that a regular review of staff attitudes is important. It notes that it may be easy to dismiss patients' complaints of sexual abuse or harassment, regarding them as delusions or exaggerated fears, and that the only way to minimise the occurrence of these acts in psychiatric settings is to deal with them appropriately. Local trust policy makes it clear that staff have a duty to report incidents ‘in-house’ and ensure that the service user is supported appropriately. Although both the College document and trust guidelines recommend staff training, neither specifies quantity, content or who should deliver it.
The NHS framework for mental health (Department of Health, 1999) acknowledges that while social and therapeutic activities will usually be mixed, there is an imperative both to ensure that single-gender day space is always provided and to achieve Patient's Charter standards for segregated sleeping and toilet facilities across the NHS. The NHS plan (Department of Health, 2000) recognises that mental health services are not always sensitive to the needs of women, and states that by 2004 there will be women-only day centres in every health authority.
This discussion paper examines how much of the advice in these documents has been translated into practice in one particular case series. It highlights the sensitive issues surrounding the management of sexual assault on in-patient units and argues that a consistent approach to all assaults needs to be taken. It also examines how staff dealt with allegations in a series of cases and discusses some of the pitfalls of a varied response.
Some of the current approaches to managing sexual assault are illustrated by the cases in Table 1. This gives details of six sexual assaults that were recorded in the medical notes of an urban psychiatric in-patient unit between October 1997 and May 1999. Four of the cases listed in Table 1 represent a subset of 177 cases collected when auditing the medical notes for a related project (Reference ColeCole, 2000) in which all the admission notes of women between 16 and 45 years old were scrutinised. This subset was examined with the aim of establishing whether there was consistency in management of allegations of sexual assault in the unit surveyed. Two further cases were identified for the periods between audit loops by a limited search of the incident forms, but there were difficulties accessing these data, which are discussed later.
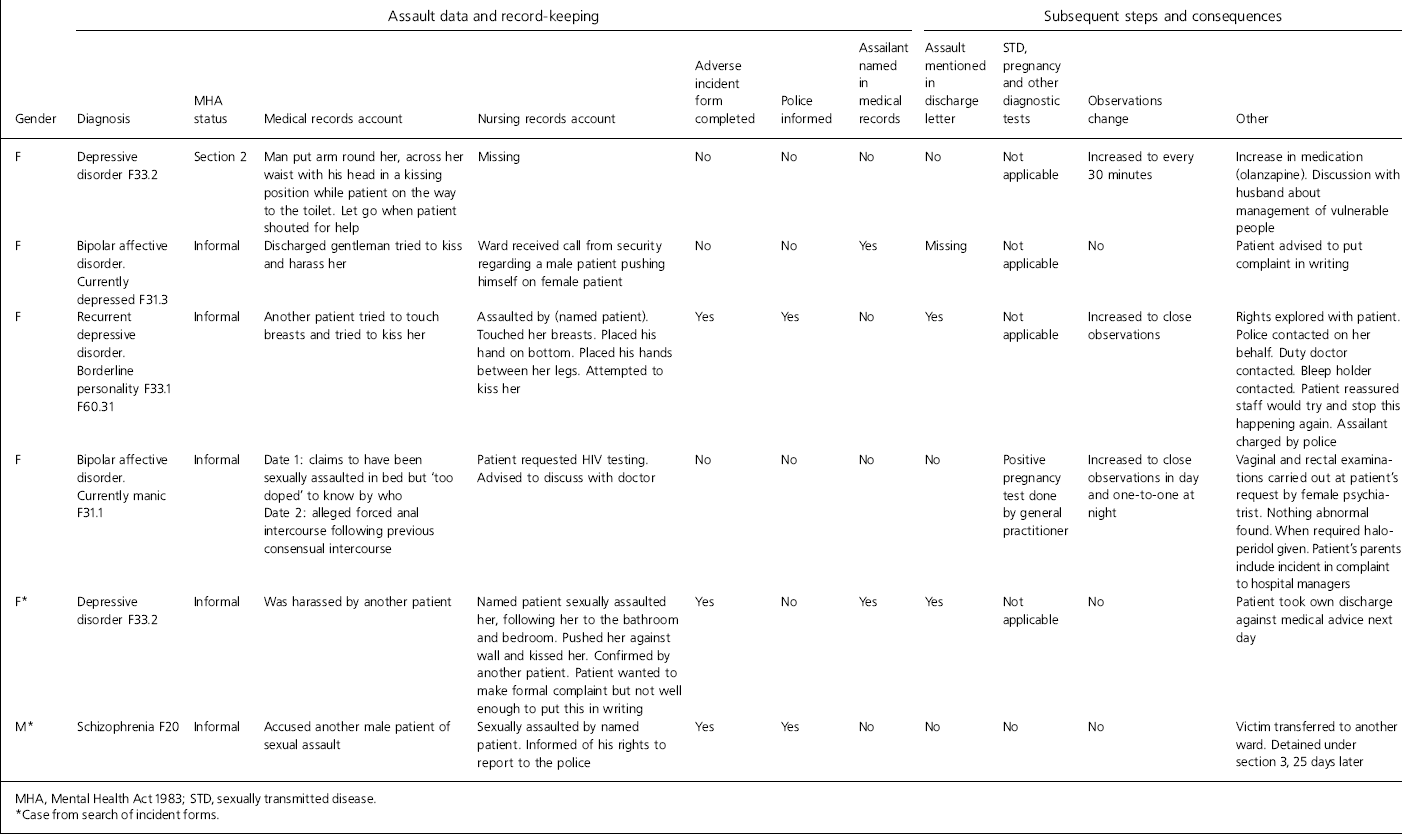
Table 1. A series of sexual assaults
| Assault data and record-keeping | Subsequent steps and consequences | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Gender | Diagnosis | MHA status | Medical records account | Nursing records account | Adverse incident form completed | Police informed | Assailant named in medical records | Assault mentioned in discharge letter | STD, pregnancy and other diagnostic tests | Observations change | Other |
| F | Depressive disorder F33.2 | Section 2 | Man put arm round her, across her waist with his head in a kissing position while patient on the way to the toilet. Let go when patient shouted for help | Missing | No | No | No | No | Not applicable | Increased to every 30 minutes | Increase in medication (olanzapine). Discussion with husband about management of vulnerable people |
| F | Bipolar affective disorder. Currently depressed F31.3 | Informal | Discharged gentleman tried to kiss and harass her | Ward received call from security regarding a male patient pushing himself on female patient | No | No | Yes | Missing | Not applicable | No | Patient advised to put complaint in writing |
| F | Recurrent depressive disorder. Borderline personality F33.1 F60.31 | Informal | Another patient tried to touch breasts and tried to kiss her | Assaulted by (named patient). Touched her breasts. Placed his hand on bottom. Placed his hands between her legs. Attempted to kiss her | Yes | Yes | No | Yes | Not applicable | Increased to close observations | Rights explored with patient. Police contacted on her behalf. Duty doctor contacted. Bleep holder contacted. Patient reassured staff would try and stop this happening again. Assailant charged by police |
| F | Bipolar affective disorder. Currently manic F31.1 | Informal | Date 1: claims to have been sexually assaulted in bed but ‘too doped’ to know by who Date 2: alleged forced anal intercourse following previous consensual intercourse | Patient requested HIV testing. Advised to discuss with doctor | No | No | No | No | Positive pregnancy test done by general practitioner | Increased to close observations in day and one-to-one at night | Vaginal and rectal examinations carried out at patient's request by female psychiatrist. Nothing abnormal found. When required haloperidol given. Patient's parents include incident in complaint to hospital managers |
| F* | Depressive disorder F33.2 | Informal | Was harassed by another patient | Named patient sexually assaulted her, following her to the bathroom and bedroom. Pushed her against wall and kissed her. Confirmed by another patient. Patient wanted to make formal complaint but not well enough to put this in writing | Yes | No | Yes | Yes | Not applicable | No | Patient took own discharge against medical advice next day |
| M* | Schizophrenia F20 | Informal | Accused another male patient of sexual assault | Sexually assaulted by named patient. Informed of his rights to report to the police | Yes | Yes | No | No | No | No | Victim transferred to another ward. Detained under section 3, 25 days later |
In each case, Table 1 records verbatim the entries in the medical and nursing notes concerning the assault. It also records what else was done, such as adverse incident reporting or communicating with the general practitioner (GP), and what practical steps were taken in the aftermath of the assault.
Inadequate recording of data
Data on the frequency and seriousness of assaults upon patients in their case were not available to managers in this trust. Adverse incident forms were not completed uniformly and a systems failure meant that none of those that had been completed before April 1999 could be retrieved from the computerised database. The hand-written forms were held in alphabetical order, based on patients' names not the nature of the incident. It is also of concern that if the alleged assailant remained unnamed in the medical and nursing records, multiple allegations could be made against the same assailant over different admissions, with only the memory of long-serving staff to make the connection between current and previous assaults. Furthermore, the data on victims assaulted during a previous admission are not easily accessible to medical or nursing staff on the wards unless they read the handwritten entries throughout the case notes.
The NHS plan has recommended a full reporting scheme for adverse events, with a single national database. If this is achieved, it should address some of the concerns that are raised by the quality of the data-recording reported here. However, in the above series, adverse incident forms were completed in only half of the cases that were recorded in the medical notes. Only two of these six alleged assaults were reported to the police and only two of the discharge letters to GPs mentioned the assault.
Reasons for inconsistency
It does not seem that the quality of the data-recording was related to the severity of the assault, either in terms of details written in nursing and medical records, completion of adverse incident forms or informing the GP or the police. Staff may become habituated to sexually aggressive behaviours by psychiatric patients, so that such behaviour does not evoke the same level of outrage as would be expected when perpetrated against a less stigmatised group of individuals (Reference Thomas, Bartlett and MezeyThomas et al, 1995).
Cases may be handled in a variety of ways in order to give a sensitive response to individual needs. However, variation may reflect staff attitudes towards the patient's mental state and whether staff regard the assailant or complainant as a ‘trouble maker’. Staff may often find it difficult to know when to consider the behaviour of mentally disturbed adults as criminal. Also, there may be a tendency to dismiss such allegations as attention-seeking, depending upon the history of the previous relationship between the staff member and the patient.
Staff may rightly feel ambivalent about police involvement, hoping to spare their patients the ordeal of legal scrutiny. This concurs with a Mind survey (Reference PedlarPedlar, 2000) in which three-quarters of the professionals questioned considered there was a problem with denial of access to the criminal justice system for people with mental health problems. This was particularly so in cases of rape and sexual assault.
Clinical consequences of inconsistency
The local trust policy on sexual assault states that the system in place should acknowledge the validity of the woman's experience. The use of increasing observations (although possibly intended as protective), coupled with increasing antipsychotic medication, is a particularly sensitive issue. It would be easy for the patient to misinterpret these actions as punitive, especially if procedural methods of demonstrating belief, such as completing an adverse incident form or discussing police involvement, are not performed at the same time. One patient, whose assault was witnessed by another, took her own discharge the next day and it may be that this decision was motivated by fear. Although she wished to make a complaint, it seems she was thwarted by her disturbed mental state and lack of someone to help her with this task.
Recommendations and limitations
The small number of cases in this series limits the generalisation of the conclusions about their management. The four cases found by examining case notes may be considered as representative, but they give no indication about management of alleged assaults that are not recorded in medical case notes. The two additional cases had already passed a threshold of sufficient concern to trigger completion of an incident form. However, the difficulty in collecting data on these cases, either across time or the whole patient group, highlights the ease with which assaults may be swept, if not under the carpet, then into the pages of handwritten continuation notes. National and local policies have not been put into practice in the management of these cases.
From consideration of this series, it is recommended that a minimum adequate response would be the completion of adverse incident forms; naming the alleged assailant in written records; mentioning the assault in the discharge summary and reporting to line managers. A specially designed incident form (above the requirements of the NHS plan), including time and description of the assault, and name of the alleged assailant and witnesses, could help clarify what is expected of staff in this situation. Without exception, this should be completed when there is an allegation of rape or sexual assault. Tick-boxes may be used to confirm that the relevant people had been contacted. Annual review of these forms may highlight weaknesses in layout or ward routine. Repeated allegations against the same person should be brought to the attention of those responsible for their care. This would enable rates and assault type to be monitored. The extent of the problem may then be assessed and protective interventions audited. Patients should feel safe on psychiatric wards, and any patient who has been frightened, injured or is at risk from infection or impregnation, should be encouraged to report the assault to the police. This would also relieve the staff from trying to ‘second guess’ the police response or themselves trying to assess the patient's credibility. An appropriate adult needs to be present for all interviews with those who are mentally disordered (Home Office, 1995). A patient's keyworker or social worker may do this. It is preferable that such workers have received appropriate training. The new Patient Advocacy and Liaison Service, due later this year, may be prepared to take on this role.
In 1995, City and Hackney Community NHS Trust opened a segregated ward for women with severe mental illness who would be vulnerable on a mixed-gender ward (Reference KohenKohen, 1999). The privacy and safety provided by the unit and the positive response from families and the community makes the case for more single-gender wards. It is a pilot project that may be repeated by other trusts. Meanwhile, both genders in mixed-gender wards should be cared for by staff who are vigilant for patients' safety and trained to avert assault proactively. Specific staff training upon recruitment, repeated at regular intervals, should lead staff to be confident about dealing with any assaults, and also ensure that the trust has information available to help prevent repetitions.
Declaration of interest
None.




eLetters
No eLetters have been published for this article.