More than 75% of people living with mental health problems in low- and middle-income countries (LAMI countries) do not receive treatment for mental health problems. Reference Demyttenaere, Bruffaerts, Posada-Villa, Gasquet, Kovess and Lepine1 In an effort to close this vast treatment gap new models of treatment provision have been developed that propose a collaborative approach to care delivery, also known as task-sharing. This entails that the bulk of direct mental health service delivery is conducted by front-line health workers, rather than restricted to the domain of mental health professionals. This approach is also advocated by the World Health Organization's (WHO's) Mental Health Global Action Programme (mhGAP), an initiative aimed to equip primary healthcare workers to provide mental healthcare. 2 Expanding the workforce and putting mental health services in place is crucial to close the treatment gap. However, this alone is inadequate without people with mental health problems actually making use of the services. Both availability and uptake of services are required to close the treatment gap. Thus, a major barrier for the scaling up of mental healthcare is the lack of awareness and demand for care. Reference Patel, Chowdhary, Rahman and Verdeli3 Low demand can be explained in part by non-detection or under-detection of mental health problems. Reference Halversen and Chan4 There are a number of barriers to detection methods that are effective in high-income countries including: first, low literacy rates preclude use of self-administered self-report tools such as the Patient Health Questionnaire; Reference Kroenke, Spitzer and Williams5 second, high levels of stigma and existing belief systems regarding mental health problems discourage endorsement of psychiatric labels; Reference Kohrt and Harper6 and third, self-report instruments of serious mental illness, such as schizophrenia, have failed to detect cases in some LAMI countries. Reference Shibre, Teferra, Morgan and Alem7,Reference Beyero, Alem, Kebede, Shibire, Desta and Deyessa8 Therefore, development of innovative methods for identification of people with mental illness are needed to address limited literacy, cultural stigma, and applicability across a range of common and serious mental disorders.
In response, community case-finding has been proposed to increase access to care in LAMI countries. Reference Shibre, Kebede, Alem, Negash, Kibreab and Fekadu9 Patel & Thornicroft Reference Patel and Thornicroft10 propose a two-staged case-finding procedure with probable cases being identified through community case-finding followed by a diagnostic interview by a trained health worker. In practice, active case-finding has played an important part in increasing demand for, and accessibility of, mental health services in Nigeria and India. Reference Patel, Chowdhary, Rahman and Verdeli3,Reference Cohen, Eaton, Radtke, George, Manual and De Silva11 Case detection by lay-workers may, especially in low-income settings, hold some population-level advantages, including greater population coverage. Reference Kagee, Tsai, Lund and Tomlinson12 Although proactive case finding has been used before, the current approach is, to the best of our knowledge, novel in a LAMI country setting, i.e. consisting of a structured approach using pictorial vignettes and an extensive development process emphasising compatibility with the sociocultural context. Also, to date, there has been limited evaluation of proactive case-finding strategies in LAMI country settings.
The current study will evaluate the accuracy of a newly developed procedure for proactive case finding by community informants in Nepal, with the aim of increasing help-seeking for mental healthcare. Proactive case-finding has been introduced as a strategy to increase help-seeking, as it aims to bridge the gap between people in need of mental healthcare with available services. It provides an alternative to systematic community screening that is associated with high financial and resource burden. The developed procedure is based on the premise that well-placed informants, who are intimately connected to people in the surrounding community, have good insight into its members' well-being. The hypothesis is that such a process of identification is best achieved through emblematic recognition, i.e. broadly matching of people they encounter in daily routine onto vignettes of mental health problems that have been made context-specific. This is the community version of a prototype-matching approach for clinicians, which has demonstrated comparable validity to more complex diagnostic algorithms based on dichotomous decisions on individual symptoms. Reference Westen13,Reference Westen, DeFife, Bradley and Hilsenroth14 This is an approach that proposes to examine a diagnostic prototype (short narrative description) taken as a whole and to gauge the extent to which a patient's symptom presentation matches the prototype. Reference Ortigo, Bradley, Westen, Millon, Krueger and Simonsen15 The developed procedure for proactive case-finding, which entails training of selected community members in the use of a structured tool (Community Informant Detection Tool, CIDT), is applied within a larger programme (Programme for Improving Mental Health Care, PRIME). PRIME aims to improve the coverage of treatment for priority mental disorders by implementing and evaluating a comprehensive mental healthcare package, integrated into primary healthcare in five LAMI countries (Nepal, India, South Africa, Ethiopia and Uganda). Reference Lund, Tomlinson, De Silva, Fekadu, Shidhaye and Jordans16 The care package includes the provision of psychosocial and pharmacological interventions by non-specialised primary health workers (following the WHO mhGAP Intervention Guide) 2 and community counsellors. The objective of the study is to evaluate how accurate the CIDT procedure is in identifying people with priority mental disorders.
Method
Setting
The research was conducted in Chitwan, a district in southern Nepal. Nepal is a low-income country, one of the poorest countries in Asia and is categorised by the World Bank as a fragile state. 17 The total population of the country is approximately 26.5 million (Central Bureau of Statistics, 2011, www.dataforall.org/dashboard/nepalcensus) with majority (86%) of the total population living in the rural areas. The country is passing through a transition following a 10-year intra-state conflict, between government forces and Maoists insurgents, which raged between 1996 and 2006 and claimed more than 13 000 lives. Previous studies have demonstrated the impact of political violence on psychosocial well-being and mental health in Nepal. Reference Tol, Kohrt, Jordans, Thapa, Pettigrew and Upadhaya18–Reference Kohrt, Jordans, Tol, Speckman, Maharjan and Worthman21 The conflict has further shattered an already weak healthcare system. The war formally ended in November 2006 with a comprehensive peace agreement between an alliance of political parties and the Maoists. The present situation is characterised by instability and political deadlock. It is against the backdrop of recent violence and ongoing poverty that PRIME was implemented in Nepal. In Nepal's healthcare system, there are sub-health posts that provide essential healthcare services and monitor community level healthcare activities; health posts that offer the same services with additional birthing centres, as well as the responsibility of monitoring the sub-health posts activities, and primary healthcare centres (PHCC) a higher level healthcare institution that serves as the first referral point for each electoral area. Currently, no mental health services are systematically available in primary healthcare. Reference Hanlon, Luitel, Kathree, Murhar, Shrivasta and Medhin22
Procedure
The CIDT procedure, as introduced above, was constructed following a process that encompassed several steps. This process can be summarised as follows. First, vignettes were developed for some priority disorders (depression, alcohol use disorder, psychoses, epilepsy and conduct disorder) by taking vignettes in WHO's mhGAP Intervention Guide 2 as a starting point. Subsequently, an inventory of local non-stigmatising idioms related to the vignette was made based on prior ethno-psychological research in Nepal. Reference Kohrt and Harper6 Selection of most relevant idioms was done through prioritisation by an expert panel of Nepali mental health professionals. The CIDT therefore does not use the diagnostic labels but Nepali descriptions that have found to be commonly acceptable and understandable for each of the vignettes. To facilitate the process of prompt recognition of people that potentially match the vignette, pictures were developed (see online Fig. DS1 for an example CIDT sheet). Pilot testing of the procedure was instrumental in identifying the most relevant groups of people to serve as community informants. The pilot testing, as well as formative research done for the overall PRIME initiative, Reference Jordans, Luitel, Tomlinson and Komproe23 demonstrated high levels of perceived acceptability for the proposed procedure among key stakeholders.
The CIDT procedure is used by community informants briefly trained in the essentials of public mental healthcare, the use of the procedure and the related ethical considerations. In their routine daily activities and tasks, the community informants aim to gauge the extent to which people in their direct vicinity match paragraph-long vignettes (aided with pictures) using a simple 5-point scale. If the community informant believes that a person in the community has significant features of the description (i.e. the person fits well with, or exemplifies, the description), then the informant answers two additional questions: one on whether the identified individual is perceived to have impaired daily functioning and a second question on whether the person would want support in dealing with these problems. In case of significant matching and a positive response to at least one of the additional questions, the community informant will encourage the person (possibly through their family) to seek help in the health facility where mental health services are being offered as part of PRIME, and where caseness can be confirmed by a trained health professional. No stigmatising diagnostic labels or psychiatric terminology is used, and encouragement for help-seeking is targeted to specific observable behaviours and/or signs of distress.
To evaluate the accuracy of the CIDT we assessed whether the people identified by the community informants were correctly detected according to a structured diagnostic assessment performed by a clinician. This was done by comparing CIDT results with results of a structured clinical assessment following the Composite International Diagnostic Interview (CIDI). Reference Kessler and Üstün24 CIDT results comprised of either ‘probable caseness’, which were respondents that met the criteria outlined above, or ‘probable non-caseness’ which are respondents that do not meet those criteria. The probable negative cases were identified by asking community informants to select people they felt confident of not matching the pictorial vignette. The group is included only for the purpose of this study (true negatives and false negatives are needed for standard analyses on psychometric properties). In keeping with the proposed real-life application of the tool, respondents were not screened systematically; rather it presents a selected sample of people proactively identified by the community informants as probable positives or negatives. The goal of the CIDT procedure is not for community informants to make a specific diagnosis, but rather to identify someone with any mental distress that would benefit from treatment. It is therefore intended as a proxy indicator for people with mental disorders. As a result, the comparisons at the heart of the study are not based on identification of specific disorders but take them as a composite concept (i.e. a possible case of any disorder).
The community informants that were part of the study included female community health volunteers (n = 8) and members of the local mother groups (n = 4), distributed over 6 wards. Members of mother groups do not require formal education, whereas female community health volunteers should minimally be literate and between 25 and 45 years of age. After receiving the 1-day training, they were asked to start using the CIDT forms. The training was provided by a health assistant, with years of experience in mental healthcare, who has been coordinating the training and implementation of the mental health services within the PRIME programme. The training consisted of minimal didactic teaching, and emphasised group discussion and practicing through role-plays. The community informants receive a small monthly allowance for their work (approximately US$2/month, paid as a flat rate as opposed to payment per identified case). All completed forms were handed over to a research assistant who subsequently arranged for the clinical assessment to happen with the identified person. When the forms were incomplete or unclearly completed the research assistants immediately contacted the community informant to clarify. Community members who were identified by the informants as potential cases were then approached by research assistants to request their permission to participate in the study. Participants were only included in the study, and clinical interviews were only conducted, after obtaining informed consent with signatures provided by literate participants and acknowledgement markings made by illiterate participants. Nepali psychosocial counsellors, with over 6 months of training and more than 5 years of experience in counselling in community settings, conducted the CIDI-structured clinical interviews and were masked to CIDT results at the time of the interview. Due to the shortage of mental health specialists in Nepal, psychosocial counsellors are the cadre of service providers with the most extensive skills-based clinical training other than psychiatrists who have limited availability to participate in research interviews given the overwhelming volume of clinical need. Psychosocial counsellors using structured clinical interviews have performed effectively in prior validation studies in Nepal. Reference Kohrt, Jordans, Tol, Luitel, Maharjan and Upadhaya25
The study was done in the area where pilot testing of the PRIME mental healthcare package was ongoing, which made referral to treatment possible. The treatment package included both psychotherapeutic and pharmacological interventions, and was offered in the nearby health facility. The PRIME programme and the CIDT procedure are endorsed by, and implemented in partnership with, the Ministry of Health and district level health authorities. Ethical approval was obtained from the Nepal Health Research Council and the Human Research Ethics Committee of the Faculty of Health Sciences, University of Cape Town (REC Ref: 412/2011). Data were collected in the period January to March 2013.
Instruments
In addition to the CIDT, we used different sections from the CIDI, notably the screens for psychosis, depression, alcohol use disorder, conduct disorder and oppositional defiant disorder. In addition, we used a 9-item screening questionnaire to detect epileptic seizures. Reference Placencia, Sander, Shorvon, Ellison and Cascante26 The Nepali-language CIDI has been validated in Nepal, (area under the curve any disorder = 0.85, area under the curve depression = 0.97). Reference Ghimire, Chardoul, Kessler, Axinn and Adhikari27 The psychosocial counsellors received a week of training in the Nepali CIDI including 6 h of observed administration and review of scoring. The training was conducted by an Australian psychologist with experience in conducting structured clinical interviews. Additional training and detailed review of videotaped interviews was provided by an expatriate psychologist (M.J.D.J) and an expatriate psychiatrist (B.A.K.) who are both fluent in Nepali.
Analyses
Using descriptive statistics the results from the CIDT and the clinical assessments were compared, and plotted as true or false positives and true or false negatives. Next, positive predictive value (PPV) and negative predictive value (NPV), positive and negative likelihood ratios were calculated. Analyses were done for the entire sample, as well as for children and adults separately. Primary analyses were done with caseness defined as identification or diagnosis of any disorder (see above). In addition, exploratory analyses were conducted for the disorders separately. Analyses were conducted using the Statistical Package for Social Sciences (SPSS version 19.0). 28
Results
The total sample consisted of 195 people. In total 210 people were identified by the community informants, of whom 5 people refused to participate and 10 people were unable to complete the interviews. See Table 1 for sociodemographic details of the sample for adults and children separately. In the combined sample, the average age was 32.21 years (s.d. = 15.47) and comprised of 59.5% female participants. Interrater reliability between the two counsellors based on independently conducted clinical interviews repeated with the same patient series was found to be good (intraclass correlation = 0.92; 95% CI 0.89–0.94). All of the study participants were identified by the community informants using the CIDT procedure, either as a probable positive (n = 110) or as a probable negative case (n = 85). After clinical assessments, 70 of the CIDT positive cases and 6 of the CIDT negative cases were found to meet criteria for a clinical diagnosis for one or more of the target disorders (i.e. true positives = 70, true negatives = 79). See Table 2 for a breakdown of the diagnoses (with the total diagnoses (101) exceeding the 76 individuals due to comorbidity).
TABLE 1 Sample characteristics

| Adults | Children | |
|---|---|---|
| n | 139 | 56 |
| Female, % | 61.2 | 55.4 |
| Age, years: mean (s.d.) | 39.37 (12.44) | 14.41 (1.90) |
| Caste, % | ||
| Brahmin/Chhetri | 51.0 | 44.6 |
| Dalit | 11.5 | 10.7 |
| Tharu | 23.7 | 32.1 |
| Janajati | 13.8 | 12.6 |
| Religion, % | ||
| Hindu | 95.7 | 87.5 |
| Christian | 3.6 | 7.1 |
| Buddhist | 0.7 | 5.4 |
| Education, % | ||
| Illiterate | 17.1 | 0 |
| Primary education | 30.6 | 15.1 |
| Secondary education | 34.2 | 75.5 |
| SLC pass | 6.3 | 0 |
| Intermediate | 11.7 | 9.4 |
s.d., standard deviation; SLC, School Leaving Certificate.
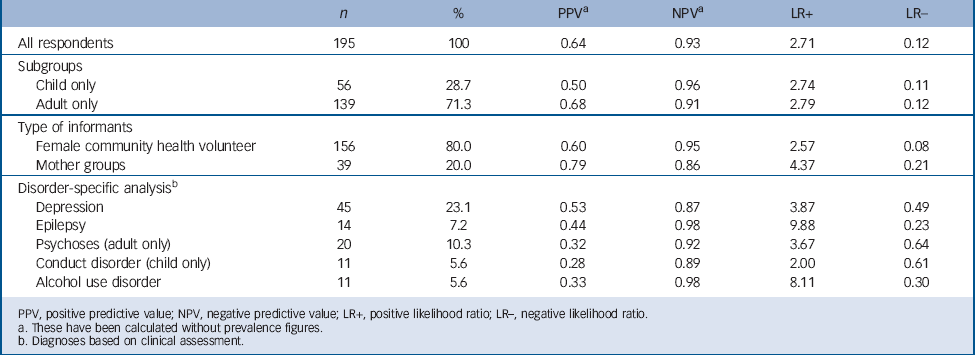
TABLE 2 Psychometric properties
| n | % | PPV a | NPV a | LR+ | LR− | |
|---|---|---|---|---|---|---|
| All respondents | 195 | 100 | 0.64 | 0.93 | 2.71 | 0.12 |
| Subgroups | ||||||
| Child only | 56 | 28.7 | 0.50 | 0.96 | 2.74 | 0.11 |
| Adult only | 139 | 71.3 | 0.68 | 0.91 | 2.79 | 0.12 |
| Type of informants | ||||||
| Female community health volunteer | 156 | 80.0 | 0.60 | 0.95 | 2.57 | 0.08 |
| Mother groups | 39 | 20.0 | 0.79 | 0.86 | 4.37 | 0.21 |
| Disorder-specific analysis b | ||||||
| Depression | 45 | 23.1 | 0.53 | 0.87 | 3.87 | 0.49 |
| Epilepsy | 14 | 7.2 | 0.44 | 0.98 | 9.88 | 0.23 |
| Psychoses (adult only) | 20 | 10.3 | 0.32 | 0.92 | 3.67 | 0.64 |
| Conduct disorder (child only) | 11 | 5.6 | 0.28 | 0.89 | 2.00 | 0.61 |
| Alcohol use disorder | 11 | 5.6 | 0.33 | 0.98 | 8.11 | 0.30 |
PPV, positive predictive value; NPV, negative predictive value; LR+, positive likelihood ratio; LR−, negative likelihood ratio.
a. These have been calculated without prevalence figures.
b. Diagnoses based on clinical assessment.
Table 2 further summarises the results of the analyses, including PPV (for the entire sample: 0.64), NPV (0.93), positive likelihood ratio (2.71) and negative likelihood ratio (0.12). The results for children and adults differ substantially only for the PPV (0.50 among children), due to the high number of false positives among the child sub-sample. When comparing the results between both types of community informants, we see differences on all indicators, with a far smaller proportion of false positives among the mother group participants. Finally, for explorative purposes we have included the analyses for the separate diagnostic clusters, indicating how well the separate disorder-specific vignettes of the CIDT detect those disorders.
We also analysed these results when varying the CIDT decision algorithm. Results changed only marginally when allocating positives based on matching symptoms only, or based on symptoms plus both additional criteria of functioning impairment and need for support – rather than matching of symptoms plus at least one of the two additional criteria (which is the original algorithm that was used in this study).
Discussion
Mental healthcare in LAMI countries is characterised by low resources, Reference Prince, Patel, Saxena, Maj, Maselko and Phillips29,30 which goes hand in hand with low demand for, and utilisation of, services. To fully capitalise on efforts to increase trained human resources and evidence-based treatments, an increase in demand and utilisation is imperative. Relying solely on self/family-referrals may risk missing out on a large group of clients that are simply not identified, yet need treatment. Use of self-report written screeners is not widely feasible given low literacy rates. A context-sensitive procedure of proactive case-findings, built on the notion of using non-stigmatising idioms and matching people on vignettes (aided with visual clues and two questions), has been piloted in rural Nepal to identify need for treatment and ultimately increase the demand for and utilisation of mental healthcare.
Community informants can assign caseness in the persons rated with pictorial vignettes with accuracy for the majority of persons rated. Given that real-life use of the CIDT only results in reporting positives, as opposed to a usual universal or community screening procedure that will result in both negatives and positives, the key indicator of accuracy of the CIDT are the PPV (i.e. the proportion of positive test results that are true positives) and the positive likelihood ratio (i.e. how much to increase the probability of disease if the test is positive), which were 0.64 and 2.71 respectively for all respondents and all disorders in this study.
With approximately two-thirds of the expected positives having a confirmed disorder, the community informants do well overall. By comparison many common standardised symptoms-based screening instruments have a similar (or lower) PPV Reference Boyd, Le and Somberg31 or positive likelihood ratio Reference Whooley, Avins and Browner32 – noted of course that these are generally disorder specific, and some also have higher values. This is quite surprising, given that the CIDT informants in our study do not have any formal training or even formal education in many instances. Although a promising strategy to identify cases that might have otherwise gone unnoticed, it does present with a risk for over-identification and additional burden for the health facilities, Reference Petersen, Ssebunnya, Bhana and Baillie33 but this burden is not necessarily higher than would be encountered with a standardised screening instrument. Overburdening providers is a serious concern with many health facilities already strained. At the same time, it is plausible that the ‘false positives’ do indeed require treatment but are just sub-threshold or have problems that were not assessed with the five CIDI disorders covered in the clinical interviews.
These promising results may be explained by the focus on a vignette-based structure, which like the prototype matching approach for clinicians, is a form that is more congruent with human (and clinical) cognitive processes than checking whether each of a series of symptoms is absent or present. Reference Westen13 The use of this approach in a community setting is quite new, and, to the best of our knowledge, a first in a low-income setting. In addition, incorporating locally salient manifestations of mental health problems through idioms of distress and drawings, may have contributed to good accuracy. This was also demonstrated in the cross-cultural construct validation of a brief screener for psychosocial distress for children in conflict affected settings. Reference Jordans, Komproe, Tol and de Jong34
To implement this proactive case finding strategy, it is important to know who the most adequate community informants might be. Formative research had already indicated that in Nepal female community health volunteers and mother group leaders would be most appropriate. The results further demonstrate that mother groups outperform female community health volunteers as the former have significantly lower false positives. From a perspective of potentially burdening the system, involving the mother's groups would lead to lower burden. This is an interesting finding given that female community health volunteers are currently an extension of the healthcare system in Nepal, and are excessively used for different task-shifting roles. Based on this finding it would actually be better to not add another task on this group of community health workers, but rather chose of group of people that is less taxed and may have better knowledge of the well-being of the community members.
For determining the overall accuracy of the CIDT, it is not necessary to see how well the procedure picks up on individual disorders. Yet, it is interesting to see that the depression module was most accurate among the five included disorders (in terms of PPV). This goes counter to the notion that depression and mood disorders generally are the more challenging to identify by lay people, Reference Shibre, Kebede, Alem, Negash, Kibreab and Fekadu9,Reference Lauber, Nordt, Falcato and Rössler35 and also contrary to the formative study into the feasibility of this approach. This is a promising result for a problem that is present so ubiquitously, but with near absence of treatment at present in rural Nepal. This would mean that the aim to increase demand for mental healthcare using the CIDT will not be limited to the more ‘visible’ disorders, such as schizophrenia or alcohol use disorder. It should be noted that the numbers for these subgroup analyses are very small, so this trend will need to be confirmed with a larger sample. An issue that should also be further considered when implementing this procedure is that it is less accurate in identifying children's mental health problems. This fits with common patterns of under-detection of children's problems. Reference Tyano, Fleishman, Remschmidt, Nurcombe, Belfer and Sartorius36 It is possible that this difficulty is especially pertinent for the conduct problems, and possibly less so for problems that are more clearly demarcated as pathological (i.e. severe mental retardation) by community members. Further development is needed to fine-tune the procedure towards children's mental health problems.
There are important potential downsides to this sort of case detection. Reference Kagee, Tsai, Lund and Tomlinson12 Community informants could potentially abuse their new role, however informal it is, and force people to seek treatment who may not be willing to do so. Individuals who are identified may experience stigma and discrimination, particularly if community informants are not bound by a clear code of confidentiality. The power dynamics of using this procedure is something that was addressed in the training and has been monitored throughout the pilot phase. It has not yet led to any such incidents, but this does not mean it will not, especially when the strategy is scaled up making intensive monitoring much harder. Also, possible downsides of a vignette-based approach are that its users may selectively recall certain features of the prototype, and that it allows for a lack of standardisation between users. Reference Maj37 It is important to emphasise that the proactive case finding strategy is not meant as a form of systematic community screening. If it were, population prevalence rates would need to be taken into consideration resulting in lower PPVs. Selection of respondents for this study was therefore pragmatic, reflecting the CIDT's intended real-life use. Although asking community informants to identify negatives they ‘felt confident’ about is congruent with the actual process of excluding cases when engaged in proactive case-finding; this identification may have had an effect on the NPV. A strength of the approach is the extensive development process that relied on available ethnographic study for selecting idioms of the vignettes and drawings, incorporating local stakeholder perspectives and fine-tuned a training package that balanced utilitarian and ethical concerns. This is important to emphasise, as potential replication of this approach without such preparation might impact the accuracy and introduce ethical or clinical risks.
Future research is needed to assess the actual effectiveness of the proactive case-finding procedure. Where the present study evaluated the accuracy, the next step is to evaluate whether the use of the CIDT also results in an increase in demand for, and uptake of, mental healthcare. Furthermore, more work is needed to make the procedure more sensitive to capture children's mental health problems in the future.
Implications
The procedure shows potential to identify the right people in need of treatment and the study suggests that it provides for a good surveillance procedure. About 64% of the people that the community informants identified as probable cases using the CIDT were actually positive cases based on clinical interviews and 93% of people that community informants were confident probable non-cases, were indeed found negative. It appears that the procedure does not need to exclusively rely on already overburdened community health volunteers. Given the selected use of proactive case finding, the procedure is not a substitute for systematic community screening. Actually, the CIDT may present a pragmatic alternative approach preferable to community screening.
The CIDT can be an important demand-side strategy to increase help-seeking for settings that are integrating mental health into primary healthcare. It can be used in conjunction with the training and implementation of WHO's mhGAP guidelines, and can be scaled up relatively easily to a national level. From a policy point of view this is important, given the commitment that so many countries have made towards this goal. 38 The use of the proactive case-finding may lead to significantly increased coverage of mental healthcare in a target area where mental health services are put in place, provided that the community informants are selected to represent a small geographical area (village or part of a village) where they are intimately connected and known. As stated above, the last part is at present still an assumption. Currently, research is planned to evaluate the effectiveness in facilitating referrals and reinforcing treatment-seeking behaviour.
Funding
This document is an output from the PRIME Research Programme Consortium, funded by the UK Department of International Development (DFID) for the benefit of LAMI countries. B.A.K. was supported by the National Institute of Mental Health U19 MH095687-01S1, South Asian Hub for Advocacy, Research & Education on Mental Health (SHARE). The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript. The authors had full control of all primary data. The views expressed in this publication do not necessarily reflect the views of the funders.
Acknowledgements
We thank the TPO Nepal Research team in Chitwan for their work on this study.





eLetters
No eLetters have been published for this article.