Schizophrenia is a severe mental illness that is associated with high levels of emotional distress and poor social functioning. People with schizophrenia also have poor physical health. Reference Phelan, Stradins and Morrison1 In the UK and other high-income countries, life expectancy in people with schizophrenia is 20% lower than in others, and men with schizophrenia die, on average, 20 years earlier than those without this condition. Reference Wahlbeck, Westman, Nordentoft, Gissler and Laursen2 Although levels of suicide and other violent deaths are higher in people with schizophrenia, most of the increased mortality in this group is the result of higher levels of cardiovascular disease and other physical health problems. Reference Saha, Chant and McGrath3 Higher levels of cardiovascular disease in people with schizophrenia are partly explained by a higher prevalence of risk factors such as unemployment, smoking and alcohol misuse. Reference Samele, Patel, Boydell, Leese, Wessely and Murray4 Other risk factors for cardiovascular disease, including obesity and lack of exercise, are also more common in this group. Reference Osborn, Nazareth and King5 It seems likely that changes in glucose metabolism resulting from the use of some types of antipsychotic medication also contribute to higher levels of cardiovascular disease. Reference Rummel-Klugea, Komossaa, Schwarza, Hungera, Schmida and Lobosb6 There are also concerns about the quality of care that people with psychosis receive for their physical health. People with schizophrenia are less likely to receive proper treatment for cardiovascular disease. Reference Mitchell, Malone and Doebbeling7 Among people with diabetes who present to emergency medical services, those with comorbid schizophrenia are less likely to receive specialist treatment. Reference Sullivan, Han, Moore and Kotrla8 In the UK, premature mortality in people with schizophrenia has been called a national scandal Reference Thornicroft9 and efforts to improve physical healthcare for people with psychosis are a key component of current mental health policy. 10
The National Audit of Schizophrenia was commissioned by the Healthcare Quality Improvement Partnership as part of the National Clinical Audit and Patient Outcomes Programme to examine care received by people with schizophrenia. Monitoring and interventions for physical health formed a key component of the audit. 11 We conducted a secondary analysis of data from the audit to examine the extent to which the physical health of people with schizophrenia was monitored. We also examined the extent to which interventions for physical health problems were delivered and patients’ experience of the care they received for their physical health.
Method
The National Audit of Schizophrenia comprised a retrospective examination of clinical records and a cross-sectional survey of patients. 11 Data were collected between August and November 2011. The full audit was preceded by a pilot study that was used to test feasibility and refine methods for data collection and analysis.
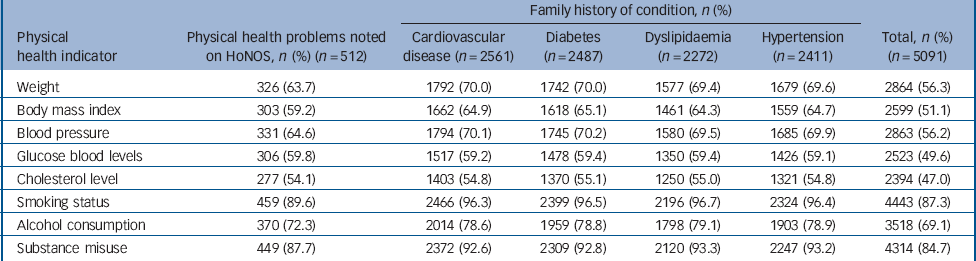
Table 1 Proportion of patients with documented evidence of assessment of physical health-related problems according to known history of physical health problems or family history of risk factors for cardiovascular disease
| Family history of condition, n (%) | ||||||
|---|---|---|---|---|---|---|
| Physical health indicator |
Physical health problems noted on HoNOS, n (%) (n = 512) |
Cardiovascular disease (n = 2561) |
Diabetes (n = 2487) |
Dyslipidaemia (n = 2272) |
Hypertension (n = 2411) |
Total, n (%) (n = 5091) |
| Weight | 326 (63.7) | 1792 (70.0) | 1742 (70.0) | 1577 (69.4) | 1679 (69.6) | 2864 (56.3) |
| Body mass index | 303 (59.2) | 1662 (64.9) | 1618 (65.1) | 1461 (64.3) | 1559 (64.7) | 2599 (51.1) |
| Blood pressure | 331 (64.6) | 1794 (70.1) | 1745 (70.2) | 1580 (69.5) | 1685 (69.9) | 2863 (56.2) |
| Glucose blood levels | 306 (59.8) | 1517 (59.2) | 1478 (59.4) | 1350 (59.4) | 1426 (59.1) | 2523 (49.6) |
| Cholesterol level | 277 (54.1) | 1403 (54.8) | 1370 (55.1) | 1250 (55.0) | 1321 (54.8) | 2394 (47.0) |
| Smoking status | 459 (89.6) | 2466 (96.3) | 2399 (96.5) | 2196 (96.7) | 2324 (96.4) | 4443 (87.3) |
| Alcohol consumption | 370 (72.3) | 2014 (78.6) | 1959 (78.8) | 1798 (79.1) | 1903 (78.9) | 3518 (69.1) |
| Substance misuse | 449 (87.7) | 2372 (92.6) | 2309 (92.8) | 2120 (93.3) | 2247 (93.2) | 4314 (84.7) |
HoNOS, Health of the Nation Outcome Scales.
Study sample
The study population were people in receipt of secondary care mental health services aged 18 years or over and who had a clinical diagnosis of schizophrenia or schizoaffective disorder. 11 We excluded those who were receiving in-patient treatment at the time of the audit and those who had been in contact with mental health services for less than a year. We aimed to collect data from all 64 mental health trusts and health boards in England and Wales. Service providers were helped to identify a random sample of patients who met the study inclusion criteria. Organisations were asked to select a random sample centrally from all those who met study inclusion criteria using an online randomisation tool (www.randomizer.org/form.htm). Organisations that were unable to generate a central list were asked to compile a sampling frame from case lists of individual community mental health teams. We asked organisations to tell us what method they used for selecting the sample. Of the 43 organisations that responded, 28 (65.1%) told us they generated it from a central list and the remainder relied partly or wholly on generating a sampling frame from case lists of local teams. 11 Audit data were submitted by each service provider via a secure online system. Unique usernames and passwords were provided to each participating service provider to ensure the data submitted were anonymous and confidential. Data entry errors were identified centrally and service providers were asked to check data against clinical records when possible errors were identified. Prior to final data analysis, all trusts were given copies of their local data to confirm that they were accurate.
During the pilot phase of the audit, it became clear that many trusts did not keep up-to-date records of physical health monitoring and that responsibility for monitoring the health of people with schizophrenia often lay with the patient’s primary care team. We therefore designed a template letter co-signed by representatives from the Royal College of General Practitioners to assist secondary care teams with collecting data held by the patients’ general practitioner. Providers of secondary care services used this letter to request information on physical health that was then combined with records kept by secondary care services.
Outcome measures
We assessed nine measures of physical health based on the recommendations included in the National Institute for Health and Care Excellence (NICE) clinical guidelines on schizophrenia: 12 weight, body mass index (BMI), blood pressure, tobacco use, alcohol use, substance misuse, blood glucose, blood lipids (total cholesterol and high-density lipoprotein) and history of cardiovascular disease, diabetes, hypertension or dyslipidaemia among family members. For each measure, the person extracting data was asked to indicate whether results had been recorded, whether there was reference to the measure being assessed but data not recorded, or whether there was no reference to the measure during the previous 12 months. They were then asked to note whether there was any record of interventions or referrals being made for the further assessment or treatment of physical health-related problems, including advice on smoking cessation, diet and exercise, substance misuse problems or interventions to treat hypertension, diabetes or dyslipidaemia. If there was no evidence of a test or intervention taking place, we assumed that it had not been done.
Basic demographic data on age, gender, ethnicity and length of contact with mental health services were also extracted. Data on past history of cardiovascular disease, diabetes, dyslipidaemia or other serious physical health problems were also extracted, together with data from the Health of the Nation Outcome Scales (HoNOS), 13 which asks the service to record whether the person has a physical illness that impairs their functioning on a five-point scale. We used a cut-off point of three or more, which corresponds to the person having a ‘physical health problem that imposes moderate to severe restrictions on activity’, to indicate their having a significant problem with their physical health.
The service user survey was based on the Carers’ and Users’ Expectations of Services, Reference Lelliott, Beevor, Hogman, Hyslop, Lathlean and Ward14 and included a question about whether the person thought they had received a physical health check-up during the previous 12 months, and whether those delivering physical healthcare had treated them with respect and taken their condition seriously.
Statistical analysis
The sample size was based on being able to detect differences in adherence with audit standards between different service providers. 11 Findings from the pilot study indicated that data on 73 patients per trust were needed to have 80% power to detect a 12% difference in adherence with standards between trusts at a 5% significance level. This level of difference was selected because it was judged to be clinically important. To take account of incomplete responses, we asked service providers to complete 100 audit forms. The sample size for the patient survey was based on being able to show a difference in the percentage of items that were rated zero for each trust compared with trusts as whole. A difference of 8% or more from the average of each trust was considered to be clinically important. To detect a difference of this magnitude required a sample of 50 completed questionnaires for each organisation. Results of the pilot study suggested that approximately a quarter of people who were sent the survey would respond and we therefore asked each trust to distribute 200 questionnaires.
All data were analysed using SPSS version 18 for Windows. The number and proportion of patients whose physical health was assessed and treated was calculated, together with 95% confidence limits. Factors associated with whether physical health was monitored, and whether people were offered an intervention for a health-related problem, were examined using binary logistic regression. We used complete-case analysis so that only participants who had data recorded for all variables were included in the analysis.
Results
Sixty (93.8%) of the 64 eligible trusts and health boards took part in the audit and returned data on physical health for 5091 patients (mean 84.9, range 17-134). Study patients had a mean age of 45 years (s.d. = 14, range 18-93), 3305 (64.9%) were male, and most (n = 3046, 59.8%) had been in contact with mental health services for over 10 years. Of the 4988 for whom ethnicity was stated, 3973 (79.7%) were White, 415 (8.3%) were Asian/British Asian, 431 (8.6%) were Black/Black British and 169 (3.4%) were mixed or from other minority ethnic communities. Data from the HoNOS were returned for 4778 patients. Of these, 512 (10.7%) had a physical health problem that imposed moderate to severe restrictions on activity.
Details of the assessment of physical health among the sample are presented in Table 1. A total of 2599 (51.1%, 95% CI 49.7-52.5) patients had documented evidence of their BMI being assessed during the previous 12 months, and 1102 (21.6%, 95% CI 20.5-22.7) had evidence of recording of all nine measures. The proportion of people having all nine items assessed in the previous 12 months varied across organisations from 5 to 65%.
Age and ethnicity did not affect the likelihood of aspects of physical health being recorded but, as seen in Table 1, physical health was more likely to have been assessed and documented in those who were recorded as having poor physical health on the HoNOS. Family history of cardiovascular disease, diabetes, hypertension or dyslipidaemia were recorded during the previous 12 months for 2648 patients (52%). Physical health was more likely to be monitored in those with family histories of risk factors for cardiovascular disease than in those without (weight was recorded in 70.0% of those with a family history of cardiovascular disease and 42.4% of those without, difference in proportions 27.6%, 95% CI 25.0-30.2, P<0.001). Nonetheless, for almost half of those with a family history of cardiovascular disease there was no evidence of their blood cholesterol being monitored in the last 12 months. Among the 2487 with a family history of diabetes, 1009 (40.6%) had no recorded evidence of their blood glucose level being assessed during the previous 12 months.
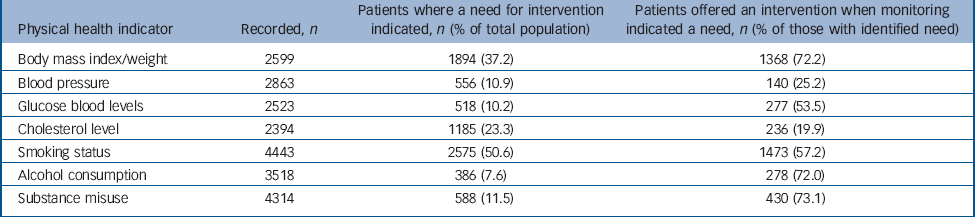
Table 2 Proportion of patients identified as needing intervention and proportion offered one, among 5091 people with schizophrenia
| Physical health indicator | Recorded, n | Patients where a need for intervention indicated, n (% of total population) |
Patients offered an intervention when monitoring indicated a need, n (% of those with identified need) |
|---|---|---|---|
| Body mass index/weight | 2599 | 1894 (37.2) | 1368 (72.2) |
| Blood pressure | 2863 | 556 (10.9) | 140 (25.2) |
| Glucose blood levels | 2523 | 518 (10.2) | 277 (53.5) |
| Cholesterol level | 2394 | 1185 (23.3) | 236 (19.9) |
| Smoking status | 4443 | 2575 (50.6) | 1473 (57.2) |
| Alcohol consumption | 3518 | 386 (7.6) | 278 (72.0) |
| Substance misuse | 4314 | 588 (11.5) | 430 (73.1) |
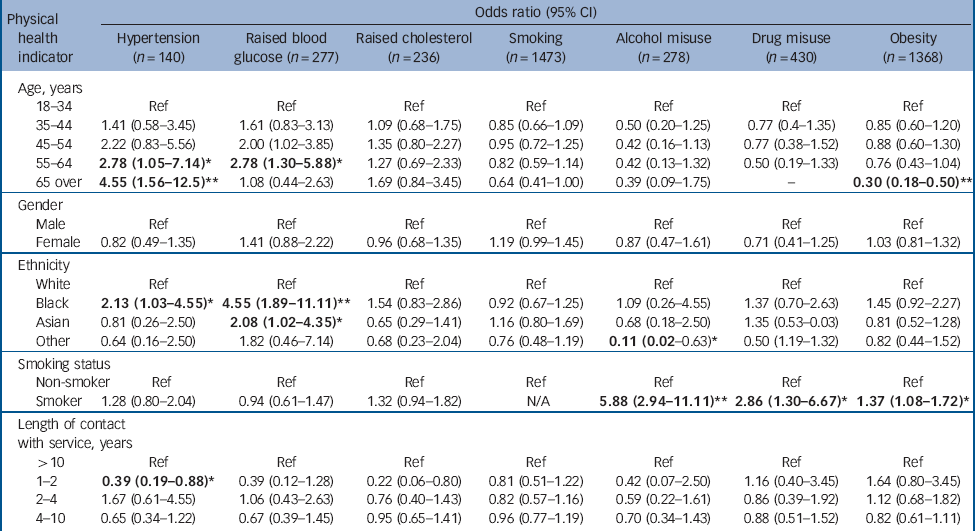
The proportion of those who had documented evidence of needing an intervention for a physical-health-related problem that were offered it during the previous 12 months are presented in Table 2. An intervention was most likely to have been offered to those with substance misuse problems (73.1%, 95% CI 69.5-76.7) and least likely for those with raised cholesterol (19.9%, 95% CI 17.6-22.2). Adjusted odds ratios for demographic and clinical factors associated with being offered interventions for physical health-related problems are presented in Table 3. Older adults with raised blood pressure were more likely to have been offered an intervention than younger adults with raised blood pressure, and smokers were more likely to be offered interventions for alcohol misuse, drug misuse and excessive weight than non-smokers.
A total of 2323 (19.4%) patients responded to the service user survey, a mean of 39 per trust (s.d. = 12). Of these, 1807 (77.8%, 95% CI 76.1-79.5) reported having had a physical health check-up during the previous 12 months, and 1906 (82.0%, 95% CI 80.4-83.6) stated that people who assessed and treated their physical health had offered them respect and taken their condition seriously.
Discussion
Data from this national audit of care received by people with schizophrenia and schizoaffective disorder show that the documented evidence of monitoring for physical health problems falls well below agreed standards. Only half the patients had documented evidence of their BMI being assessed during the 12 months prior to data collection and less than a quarter had evidence of all nine components of physical health being assessed during this period. Even among those with an established history of cardiovascular disease, over a third had no record of BMI assessment in the previous 12 months. Of those with documented evidence of risk factors for cardiovascular disease, many were not receiving appropriate treatment.
Although the majority of people who responded to the service user survey reported that they felt that their physical health was being taken seriously, most people with evidence of hypertension or dyslipidaemia had no record of being given appropriate treatment for these problems.
Strengths and weaknesses of the study
This is the largest study to date to examine the assessment and treatment of physical health among people with schizophrenia. By combining information from both primary and secondary care services we have obtained a comprehensive picture of the extent to which risk factors for premature mortality among people with schizophrenia are being monitored. Data were obtained from over 90% of all organisations in England and Wales that provide secondary care mental health services to people with schizophrenia. Previous studies have examined levels of assessment of physical health among smaller groups of people with psychosis, Reference Brown, Kim, Mitchell and Inskip15,Reference Manderbacka, Arffman, Sund, Haukka, Keskimäki and Wahlbeck16 but few have examined interventions offered to those who have identified problems and none have examined physical healthcare specifically among those with a past history of physical health problems.
Table 3 Adjusted odds ratios associated with being offered an intervention among those for whom this is indicated (adjusted for all other variables in the model)
| Physical health indicator |
Odds ratio (95% CI) | ||||||
|---|---|---|---|---|---|---|---|
| Hypertension (n = 140) |
Raised blood glucose (n = 277) |
Raised cholesterol (n = 236) |
Smoking (n = 1473) |
Alcohol misuse (n = 278) |
Drug misuse (n = 430) |
Obesity (n = 1368) |
|
| Age, years | |||||||
| 18-34 | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| 35-44 | 1.41 (0.58-3.45) | 1.61 (0.83-3.13) | 1.09 (0.68-1.75) | 0.85 (0.66-1.09) | 0.50 (0.20-1.25) | 0.77 (0.4-1.35) | 0.85 (0.60-1.20) |
| 45-54 | 2.22 (0.83-5.56) | 2.00 (1.02-3.85) | 1.35 (0.80-2.27) | 0.95 (0.72-1.25) | 0.42 (0.16-1.13) | 0.77 (0.38-1.52) | 0.88 (0.60-1.30) |
| 55-64 | 2.78 (1.05-7.14) Footnote * | 2.78 (1.30-5.88) Footnote * | 1.27 (0.69-2.33) | 0.82 (0.59-1.14) | 0.42 (0.13-1.32) | 0.50 (0.19-1.33) | 0.76 (0.43-1.04) |
| 65 over | 4.55 (1.56-12.5) Footnote ** | 1.08 (0.44-2.63) | 1.69 (0.84-3.45) | 0.64 (0.41-1.00) | 0.39 (0.09-1.75) | - | 0.30 (0.18-0.50) Footnote ** |
| Gender | |||||||
| Male | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Female | 0.82 (0.49-1.35) | 1.41 (0.88-2.22) | 0.96 (0.68-1.35) | 1.19 (0.99-1.45) | 0.87 (0.47-1.61) | 0.71 (0.41-1.25) | 1.03 (0.81-1.32) |
| Ethnicity | |||||||
| White | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Black | 2.13 (1.03-4.55) Footnote * | 4.55 (1.89-11.11) Footnote ** | 1.54 (0.83-2.86) | 0.92 (0.67-1.25) | 1.09 (0.26-4.55) | 1.37 (0.70-2.63) | 1.45 (0.92-2.27) |
| Asian | 0.81 (0.26-2.50) | 2.08 (1.02-4.35) Footnote * | 0.65 (0.29-1.41) | 1.16 (0.80-1.69) | 0.68 (0.18-2.50) | 1.35 (0.53-0.03) | 0.81 (0.52-1.28) |
| Other | 0.64 (0.16-2.50) | 1.82 (0.46-7.14) | 0.68 (0.23-2.04) | 0.76 (0.48-1.19) | 0.11 (0.02-0.63)Footnote * | 0.50 (1.19-1.32) | 0.82 (0.44-1.52) |
| Smoking status | |||||||
| Non-smoker | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| Smoker | 1.28 (0.80-2.04) | 0.94 (0.61-1.47) | 1.32 (0.94-1.82) | N/A | 5.88 (2.94-11.11) Footnote ** | 2.86 (1.30-6.67) Footnote * | 1.37 (1.08-1.72) Footnote * |
| Length of contact with service, years | |||||||
| >10 | Ref | Ref | Ref | Ref | Ref | Ref | Ref |
| 1-2 | 0.39 (0.19-0.88) Footnote * | 0.39 (0.12-1.28) | 0.22 (0.06-0.80) | 0.81 (0.51-1.22) | 0.42 (0.07-2.50) | 1.16 (0.40-3.45) | 1.64 (0.80-3.45) |
| 2-4 | 1.67 (0.61-4.55) | 1.06 (0.43-2.63) | 0.76 (0.40-1.43) | 0.82 (0.57-1.16) | 0.59 (0.22-1.61) | 0.86 (0.39-1.92) | 1.12 (0.68-1.82) |
| 4-10 | 0.65 (0.34-1.22) | 0.67 (0.39-1.45) | 0.95 (0.65-1.41) | 0.96 (0.77-1.19) | 0.70 (0.34-1.43) | 0.88 (0.51-1.52) | 0.82 (0.61-1.11) |
* P<0.05
** P<0.01 (results in bold are significant).
The data collected were from the patients’ clinical teams and case records. It is possible that some patients had some assessment of physical health without this being documented. Although it is also possible that response bias had an impact on the quality of data we collected, this was not to a degree that masked low levels of performance against standards of care for physical health monitoring of patients. Although most organisations were able to select a random sample of eligible patients from a centrally held database, a third had to rely partly or entirely on details of patients submitted by individual clinical teams. If information submitted by teams did not include all eligible patients, it would reduce the generalisability of the study findings.
The response rate to the service user survey was poor, with fewer than one in five people who were sent a questionnaire returning it. Data were obtained from patients about the help they received for physical health problems but not from carers. All the data we collected related to people using secondary care services. However, it is estimated that a third of people with schizophrenia are being treated entirely within primary care. Reference Reilly, Planner, Hann, Reeves, Nazareth and Lester17 We do not know how the monitoring of physical health for these patients compares with that for those who are in contact with secondary care services. Available evidence suggests that people with schizophrenia are less likely to have an appointment with practice nurses or take up offers of health promotion. Reference Reilly, Planner, Hann, Reeves, Nazareth and Lester17
Implications for patients, services and research
These results provide clear evidence of the scale of improvements that need to take place if internationally agreed standards are to be met. Reference De Hert, Dekker, Wood, Kahl, Holt and Moller18-20 The physical health of people with severe mental illness is an issue that should concern both primary and secondary care services. Although, in some parts of the country, local agreements have been reached about which service has responsibility for monitoring physical health at different stages of the care pathway, in many areas such agreements do not exist. Where local agreements do not exist, we propose that secondary care services should hold the responsibility for monitoring and treating the physical health problems of all in-patients, and for monitoring physical health in the community within 6 months of initiation of antipsychotic medication or major changes in the use of these drugs, and that primary care services take responsibility for assessing physical health at all other times.
There also needs to be greater consensus about what interventions should be provided to people who have problems identified through such monitoring. The recently published ‘Positive Cardiometabolic Health Resource’, Reference Lester, Shiers, Rafi, Cooper and Holt21 which was developed and endorsed by a wide range of professional bodies, goes some way to helping develop such a consensus. We believe that greater use of this and other decision-making aids can help improve the quality of physical healthcare that people with schizophrenia receive.
Patients and carers also have an important part to play in making sure that physical health needs are met. Organisations such as Rethink Mental Illness have worked with service providers to develop patient-held records that support people in playing an active role in the healthcare they receive. 22 At present it seems that most people with schizophrenia believe that their physical healthcare is being properly attended to, whereas the results of this audit show that it is not. Better information for patients about their physical health and greater dissemination and use of interventions such as patient-held records may also help to improve the standard of care that people receive.
Future research should explore barriers to delivering effective physical healthcare for people with schizophrenia. Hyland and colleagues found that nearly 40% of case managers believe that physical health needs are less important than the mental health of the patients they treat. Reference Hyland, Judd, Davidson, Jolley and Hocking23 Attitudes of patients and their tendency to ignore their own physical health are seen as barriers to improving physical health. Reference Dean, Todd, Morrow and Sheldon24,Reference Happell, Scott, Platania-Phung and Nankivell25 Nurses have described a ‘culture of low expectations’ and ‘troubling acceptance’ of patients’ poor physical health. Reference Happell, Scott, Platania-Phung and Nankivell25
Doubts have recently been raised about the value of annual health checks in the general population. Reference Krogsb⊘ll, J⊘rgensen, Juhl, Larsen and G⊘tzsche26 However, an acknowledged weakness of previous studies is that they may exclude a disproportionate number of people who are at greater risk of poor health outcomes - including people with severe mental illness. There is some evidence that changes to the way that services are delivered, especially those that strengthen links between primary and secondary care, can improve the assessment and quality of care that people receive, but the impact of these initiatives on physical health outcomes has not been properly tested. Reference Ohlsen, Peacock and Smith27-Reference McCormack, Wright, Dewar, Harvey and Ballantine29 There is also evidence that structured dietary advice and group-based exercise programmes can help people with psychosis achieve better physical health. Reference Daumit, Dickerson, Wang, Dalcin, Jerome and Anderson30,Reference Cimo, Stergiopoulos, Cheng, Bonato and Dewa31 Future research needs to examine the impact of such interventions on morbidity and mortality so that available resources can be used in the most effective way.
We conclude that the assessment and treatment of common physical health problems among people with schizophrenia in England and Wales currently falls well below acceptable standards. Mental health practitioners need to have the knowledge and skills to assess and treat problems associated with use of antipsychotic medication, and cooperation between primary and secondary care services needs to improve if premature mortality among people with schizophrenia is to be reduced.






eLetters
No eLetters have been published for this article.