Early intervention in psychotic disorders has recently generated much interest, and a small number of studies have examined the possibility of detecting individuals in the prodromal stage, prior to the development of full psychosis. Yung et al (Reference Yung, McGorry and McFarlane1996) have pioneered the prodromal approach to prevention in their Personal Assessment and Crisis Evaluation (PACE) clinic, and have developed operational criteria to identify four subgroups at ultra-high risk of incipient psychosis: 40% of their high-risk sample developed psychosis over a 9-month period (Reference Yung, McGorry and McFarlaneYung et al, 1996). The identification of risk factors that yield such a high-risk group suggests the possibility of using preventive interventions. A trial by McGorry et al (Reference McGorry, Yung and Phillips2002) showed that specific pharmacotherapy and psychotherapy reduced the risk of early transition to psychosis in young people at ultra-high risk, in comparison with supportive therapy and case management, finding a reduction in progression to psychosis at end of treatment, although not at follow-up. However, the relative contribution of psychotherapy could not be determined since theirs was a combined treatment. They concluded that their findings demonstrated a delay in onset (i.e. a reduction in incidence). We aimed to determine whether psychological intervention could prevent transition to psychosis in help-seeking individuals at operationally defined high risk. We predicted that cognitive therapy would significantly reduce the transition rate, in comparison with treatment as usual. Secondary hypotheses were that cognitive therapy would significantly reduce the proportion of patients who needed to be prescribed antipsychotic medication, reduce the likelihood of meeting criteria for a DSM–IV (American Psychiatric Association, 1994) diagnosis of a psychotic disorder and reduce the severity of the presenting subclinical symptoms.
METHOD
Participants
Recruitment of participants was sought from a variety of sources, including primary care teams (general practitioners, practice nurses and psychological therapists), student counselling services, accident and emergency departments, specialist services (e.g. community drug and alcohol teams, child and adolescent psychiatry and adult psychiatry services) and voluntary sector agencies (such as carers’ organisations). In order to facilitate the referral process, a number of workshops were held for all of these organisations, and regular written reminders were provided. Individuals who met our criteria (based on the PACE criteria) were deemed to be at incipient risk of psychosis and were included in the study. Thirty-seven patients were randomised to receive cognitive therapy and 23 patients to monitoring.
Entry criteria
Specific state risk factors were operationally defined by the presence of either transient psychotic symptoms (termed ‘brief limited intermittent psychotic symptoms’ BLIPS) or attenuated (subclinical) psychotic symptoms, both of which were defined using an adaptation of the PACE duration and severity criteria (Reference Yung, McGorry and McFarlaneYung et al, 1996), based on the Positive and Negative Syndrome Scale (PANSS; Reference Kay and OplerKay & Opler, 1987) cut-off scores. Transient symptoms are those that score 4 or more on hallucinations, 4 or more on delusions or 5 or more on conceptual disorganisation, last less than 1 week and resolve without antipsychotic medication. Attenuated symptoms are those that score 3 on delusions, 2–3 on hallucinations, 3–4 on suspiciousness or 3–4 on conceptual disorganisation. Examination of the PANSS and the Brief Psychiatric Rating Scale (BPRS; Reference Ventura, Nuechterlein and SubotnikVentura et al, 2000) will confirm that these criteria are analogous to the PACE criteria.
Trait plus state risk factors are operationally defined by the presence of an atrisk mental state – defined for the purposes of this study as scoring for caseness on the General Health Questionnaire (GHQ; Reference Goldberg and HillierGoldberg & Hillier, 1979) and/or a recent deterioration in function of 30 points or more on the Global Assessment of Functioning (GAF; American Psychiatric Association, 1994) – plus either a family history, indicated by a first-degree relative with a history of any psychotic disorder, or a diagnosis of schizotypal personality disorder in the participant. This is analogous to the PACE criteria for their trait plus state risk group.
Potential participants below the age of 16 years or above the age of 36 years were considered to be outside the maximum risk period for psychosis and were excluded from the study. Current or past receipt of antipsychotic medication was an exclusion criterion.
Measures
The following measures were used to assess suitability for inclusion in the study and monitor outcomes. The PANSS is a clinician-administered, 30-item semi-structured interview consisting of 7 items assessing positive symptoms (e.g. hallucinations, delusions, conceptual disorganisation), 7 items assessing negative symptoms (e.g. blunted affect, passive/apathetic social avoidance) and 16 items assessing global psychopathology (e.g. depression, anxiety, lack of insight, guilt). All items are scored between 1 (not present) and 7 (severe). A number of studies have demonstrated the reliability and validity of this scale (Reference Kay, Opler and FiszbeinKay et al, 1988), which was used to assess both transient and attenuated symptoms, and was the primary outcome measure used for determining transition to psychosis. The Structured Clinical Interview for DSM–IV (SCID; American Psychiatric Association, 1994) was used to assess the presence of schizotypal personality disorder (only the relevant subsection was administered). The 28-item version of the General Health Questionnaire was used to assess general at-risk mental state, using a cut-off score of 5 or more to define psychiatric caseness. The Global Assessment of Functioning is a simple, 100-point measure of psychological, social and occupational ability designed to be concordant with DSM–IV, and was used to assess functioning. Additional psychological measures were administered at this baseline assessment and at monthly monitoring sessions in order to assess cognitive, personality and social factors, but these are not reported here.
The primary outcome measure was the rate of transition to psychosis, which was operationally defined based on the PACE criteria, using cut-off points on PANSS sub-scales (4 or more on hallucinations, 4 or more on delusions and 5 or more on conceptual disorganisation), the frequency of symptoms (at least several times a week) and their duration (more than 1 week). Secondary outcomes assumed to also represent transition to psychosis were:
-
(a) the prescription of antipsychotic medication from an independent medical practitioner;
-
(b) probable DSM–IV diagnosis from a consultant psychiatrist masked to treatment status (S.W.L.), rated using vignettes that were prepared from case notes and assessment records by the assessors.
These were considered to be valuable additional outcome measures, since some patients will not report psychotic experiences in an interview, but may be viewed as having psychosis by a clinician on the basis of behavioural indices. Scores on the PANSS over the 12 months were also analysed as a dimensional outcome measure of symptomatology.
Study design and intervention
The Early Detection and Intervention Evaluation (EDIE) trial was designed as a pragmatic, single-masked (rater), randomised controlled trial. Assessors were intended to be masked to the condition to which the patient was allocated; however, this proved difficult in practice because the participants often divulged information about their therapist, or used language that suggested they were receiving cognitive therapy. The only other treatment study reported with this population found similar difficulty in maintaining masking (Reference McGorry, Yung and PhillipsMcGorry et al, 2002), and this is a common difficulty in psychological intervention trials. Random assignment to the two conditions (monitoring only or cognitive therapy plus monitoring) was stratified by gender and genetic risk (whether the participant had a first-degree relative with a psychotic diagnosis), as these are known to be risk factors within the specified age range. A clerical worker who was independent of the study removed, at random, a slip detailing assignment from the appropriate one of four envelopes (male, family history; male no family history; female, family history; female, no family history) each of which had 25 therapy and 25 monitoring assignments. The sequence of randomisation was concealed until treatment had been allocated; the two groups were of unequal number by chance.
Recruitment and randomisation of participants occurred between 1 December 1999 and 1 April 2002. The randomised participants were monitored at monthly intervals (using the PANSS) for a period of 12 months following initial assessment (therefore monitoring alone consisted of 13 sessions, and was not intended as an attention control or placebo condition). Assessments were conducted by research assistants (L.W., A.K., J.G. and S.P.), and good interrater reliability was established using videotaped interviews.
The local research ethics committees of Salford and Trafford and North, South and Central Manchester (UK) approved the study. Potential participants who gave informed consent following the receipt of a detailed participant information sheet were assessed using the above measures in relation to the entry criteria. If they met these criteria, they were then given the other self-report indicators of risk.
The cognitive therapy intervention was limited to a maximum of 26 sessions over 6 months and followed the principles developed by Beck (Reference Beck1976). It was problem-oriented, time-limited and educational; it encouraged collaborative empiricism, used guided discovery and homework tasks, and was based on a written manual. It was based on the cognitive model most appropriate to the disorder that was prioritised on a problem list agreed between the therapist and the patient. Therefore, if a transient or an attenuated psychotic symptom was prioritised, the case conceptualisations (and subsequent treatment strategies) were based on Morrison's recent integrative model of hallucinations and delusions (Reference MorrisonMorrison, 2001). This model emphasises the culturally unacceptable interpretations that people with psychosis make for events, in addition to their responses to such events and their beliefs about themselves, other people and control strategies. The central feature of our approach to the prevention of psychosis involved normalising the interpretations that people make, helping them to generate and evaluate alternative explanations, decatastrophising their fears of impending madness and helping them test out such appraisals using behavioural experiments. However, if the problem prioritised was an anxiety disorder (such as panic, social phobia, obsessive–compulsive disorder or generalised anxiety) or depression, then the appropriate models were employed (Reference Beck, Rush and ShawBeck et al, 1979; Reference ClarkClark, 1986; Reference Clark, Wells, Heimberg and LiebowitzClark & Wells, 1995; Reference WellsWells, 1995; Reference Salkovskis, Forrester, Richards, Tarrier and WellsSalkovskis et al, 1998) and a general model of emotional dysfunction was also used (Reference Wells and MatthewsWells & Matthews, 1994). As these models have many cognitive, affective and behavioural processes and products in common, this helped to aid generalisation across problems and was extremely useful for patients with several presenting problems. A more detailed analysis of the treatment strategies can be found in our treatment manual (Reference French and MorrisonFrench & Morrison, 2004) and a case series with high-risk patients from this study is described elsewhere (Reference French, Morrison and WalfordFrench et al, 2003). All treatment and clinical supervision were provided by experienced cognitive therapists (P.F. and A.P.M.), with the exception of one case in which the patient was seen by a trainee clinical psychologist because of a gender preference.
Both monitoring and therapy conditions incorporated elements of case management in order to resolve crises regarding social issues and mental health risks. If a participant developed a full psychosis, urgent referral to a specialist clinical team outside the trial was effected and a record made of the treatment given. Medication was not prescribed as part of the trial protocol.
Statistical analysis
The Statistical Package for the Social Sciences (SPSS for Windows, version 10.1) was used for all statistical analysis. Comparison of the two groups was by intention to treat (with the exception of the two individuals who subsequently reported exclusion criteria). Missing data were recorded as missing, with the exception of transition status, which was conservatively assumed to be ‘no transition’ if this information was not obtainable. Most patients missed at least one monthly monitoring appointment. The median number of assessments attended was 7 for the monitoring group (interquartile range (IQR) 6) and 8 (IQR=7) for the therapy group. Some PANSS interviews were conducted over the telephone (a total of 21), which led to missing data for observational items on the negative and general sub-scales of the PANSS. The median number of telephone assessments was 0 (IQR=2, range=3) for the monitoring group and 0 (IQR=0, range=2) for cognitive therapy. If data were unavailable at a particular assessment occasion, then it was conservatively assumed (for both groups) that PANSS-defined transition had not occurred (medication details were obtained from medical records).
Logistic regression analyses were used to compare occurrence of transition to psychosis between the two groups while controlling for the effects of potential confounding variables (age, gender, family history of psychosis and initial PANSS positive scores); ‘number needed to treat’ statistics are also reported. Analysis of covariance was used to examine the effects of cognitive therapy on positive psychotic phenomena, since the mean and initial PANSS scores were shown to be normally distributed on the basis of visual inspection and consideration of skewness and kurtosis. Multiple regression analyses were performed on 12-month GHQ and GAF scores.
RESULTS
Participant flow and study sample
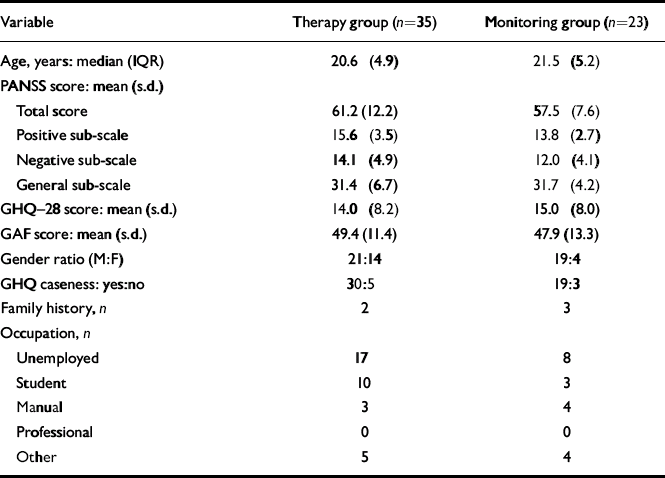
A total of 60 participants were randomised, 37 to the cognitive therapy group and 23 to the monitoring group (Fig. 1). Two patients were excluded from further analyses because, at the first post-randomisation assessment, they were assessed as meeting PANSS criteria for psychosis and also reported having concealed psychotic symptoms during their initial assessment (Reference Morrison, Bentall and FrenchMorrison et al, 2002). All other participants were questioned about this possibility, but none of them reported such psychosis at baseline. More than two-thirds of the final sample were men (n=40) and the mean age at entry was 22 years (s.d.=4.5, range 16–36). The routes into the study were as follows: 48 participants had attenuated psychotic symptoms, 6 transient psychotic symptoms and 4 were included on the basis of a family history and recent deterioration. The median number of sessions attended by participants allocated to cognitive therapy was 11 (IQR=13). The characteristics of the two groups at first assessment are presented in Table 1.

Fig. 1 Flow diagram for progress through phases of the Early Detection and Intervention Evaluation (EDIE) trial.
Table 1 Participant characteristics at baseline assessment
| Variable | Therapy group (n=35) | Monitoring group (n=23) |
|---|---|---|
| Age, years: median (IQR) | 20.6 (4.9) | 21.5 (5.2) |
| PANSS score: mean (s.d.) | ||
| Total score | 61.2 (12.2) | 57.5 (7.6) |
| Positive sub-scale | 15.6 (3.5) | 13.8 (2.7) |
| Negative sub-scale | 14.1 (4.9) | 12.0 (4.1) |
| General sub-scale | 31.4 (6.7) | 31.7 (4.2) |
| GHQ-28 score: mean (s.d.) | 14.0 (8.2) | 15.0 (8.0) |
| GAF score: mean (s.d.) | 49.4 (11.4) | 47.9 (13.3) |
| Gender ratio (M:F) | 21:14 | 19:4 |
| GHQ caseness: yes:no | 30:5 | 19:3 |
| Family history, n | 2 | 3 |
| Occupation, n | ||
| Unemployed | 17 | 8 |
| Student | 10 | 3 |
| Manual | 3 | 4 |
| Professional | 0 | 0 |
| Other | 5 | 4 |
Outcome measures
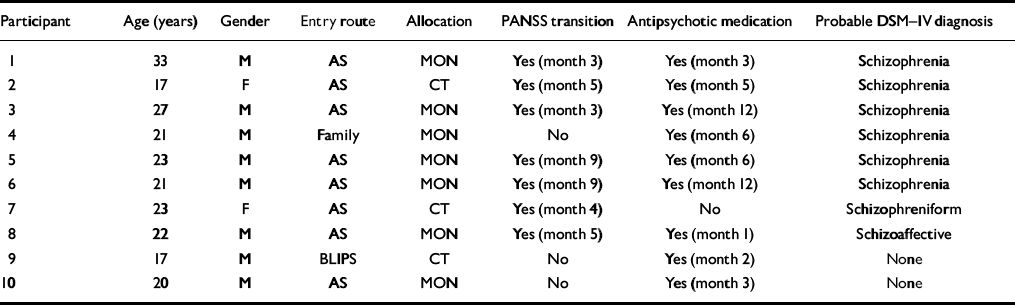
The proportion of patients making PANSS-defined transition to psychosis, receiving antipsychotic medication from an independent clinician and being rated as meeting criteria for a DSM–IV psychotic disorder are shown in Table 2, and details regarding entry route, age, gender, probable diagnosis and treatment status of the relevant participants are shown in Table 3.
Table 2 Outcome measures

| Treatment group | PANSS transition n (%) | Antipsychotic medication n (%) | DSM-IV psychosis diagnosis n (%) |
|---|---|---|---|
| Cognitive therapy | 2 (6) | 2 (6) | 2 (6) |
| Monitoring | 5 (22) | 7 (30) | 6 (26) |
Table 3 Details of participants classified as making transition or receiving antipsychotic medication
| Participant | Age (years) | Gender | Entry route | Allocation | PANSS transition | Antipsychotic medication | Probable DSM-IV diagnosis |
|---|---|---|---|---|---|---|---|
| 1 | 33 | M | AS | MON | Yes (month 3) | Yes (month 3) | Schizophrenia |
| 2 | 17 | F | AS | CT | Yes (month 5) | Yes (month 5) | Schizophrenia |
| 3 | 27 | M | AS | MON | Yes (month 3) | Yes (month 12) | Schizophrenia |
| 4 | 21 | M | Family | MON | No | Yes (month 6) | Schizophrenia |
| 5 | 23 | M | AS | MON | Yes (month 9) | Yes (month 6) | Schizophrenia |
| 6 | 21 | M | AS | MON | Yes (month 9) | Yes (month 12) | Schizophrenia |
| 7 | 23 | F | AS | CT | Yes (month 4) | No | Schizophreniform |
| 8 | 22 | M | AS | MON | Yes (month 5) | Yes (month 1) | Schizoaffective |
| 9 | 17 | M | BLIPS | CT | No | Yes (month 2) | None |
| 10 | 20 | M | AS | MON | No | Yes (month 3) | None |
Predictors of transition
All logistic regression analyses used gender and family history of psychosis as predictor variables, since randomisation was stratified using these. These analyses also used baseline PANSS positive sub-scale scores (since the groups differed at baseline) and age as predictor variables (as continuous variables). Treatment group was represented as a dichotomous variable in these analyses.
The primary logistic regression analysis was conducted using PANSS-defined transition as the dependent variable. The main effect of cognitive therapy was significant (odds ratio (OR) 0.04, 95% CI 0.01–0.71; P=0.028). This means that there is a 96% reduction in the odds of making a transition in the cognitive therapy group compared with those who received monitoring alone, after adjustment for age, gender, family history and baseline PANSS score. Summary statistics for the other variables are as follows: family history, OR=0.01, 95% CI 0–0.02, NS; age, OR=1.15, 95% CI 0.96–1.38, NS; gender, OR=4.59, 95% CI 0.42–50.48, NS; baseline PANSS positive score, OR=1.50, 95% 1.02–2.20, P=0.039. From the data in Table 2, the number needed to treat to prevent PANSS-defined transition is 6.
A secondary logistic regression was performed using prescription of antipsychotic medication as the dependent variable. The main effect of cognitive therapy was significant (OR=0.06, 95% CI 0.01–0.57; P=0.014). This means that there is a 94% reduction in the odds of making a transition in the cognitive therapy group compared with those who received monitoring alone, after adjustment for age, gender, family history and baseline PANSS score. Summary statistics for the other variables are as follows: family history, OR=1.28, 95% CI 0.10–16.00, NS; age, OR=0.99, 95% CI 0.83–1.20, NS; gender, OR=0.63, 95% CI 0.05–7.72; baseline PANSS positive score OR=1.31, 95% CI 0.94–1.83, NS. From the data in Table 2, the number needed to treat for preventing prescription of antipsychotic medication is 5. Another secondary logistic regression analysis was performed using a DSM–IV diagnosis of a psychotic disorder as the dependent variable. Again, the main effect of cognitive therapy was significant (OR=0.04, 95% CI 0.01–0.57; P=0.019). This means that there is a 96% reduction in the odds of making a transition in the cognitive therapy group compared with those who received monitoring alone, after adjustment for age, gender, family history and baseline PANSS score. Summary statistics for the other variables are as follows: family history, OR=2.18, 95% CI 0.16–29.12, NS; age, OR=1.11, 95% CI 0.94–1.31, NS; gender, OR=4.13, 95% CI 0.38–44.40; baseline PANSS positive score, OR=1.42, 95% CI 0.99–2.03, P=0.052. From the data in Table 2, the number needed to treat for preventing someone from meeting DSM–IV criteria for a psychotic disorder is 5.
Effect of therapy on psychotic experiences
In order to examine the effect of cognitive therapy on psychotic experiences over the monitoring period, an analysis of covariance was performed using mean PANSS positive symptom score over the 12 monitoring sessions as the dependent variable. Initial PANSS positive score was used as a covariate in the analysis. There was a significant effect of group on mean PANSS positive scores (F (1,48)=4.09, P=0.049), with cognitive therapy resulting in significantly fewer positive symptoms over time than treatment as usual. Baseline PANSS positive score was a significant covariate (F (1,48)=89.74, P=0.001).
Effects of therapy on functioning and distress
In order to examine the effect of cognitive therapy on functioning and distress, multiple regression analyses were performed using direct entry with 12-month GAF and GHQ scores as dependent variables. Each analysis included baseline score (GAF or GHQ), age, gender and cognitive therapy as predictor variables. The multiple regression analysis was not significant for either GHQ scores (F 4,24)=2.54, P=0.066, adjusted r 2=0.18) or GAF scores (F (4,23=2.54, P=0.067, adjusted r 2=0.19). However, it should be noted that there were many missing 12-month GAF and GHQ scores.
DISCUSSION
Summary of results
The identification of reliable operational criteria that predict a high risk of developing psychosis in the short term represents an important advance and raises the possibility of a preventive intervention. Our results suggest that a 6-month package of cognitive therapy is effective in reducing transition to psychosis over a 12-month period in a help-seeking, high-risk group. In addition, the high rate of consent to randomisation (95%) and the low withdrawal rate (14%) suggest that this is an acceptable intervention in this population (although the median number of sessions was low in comparison with the maximum available number, this reflected collaboratively agreed session contracts dependent on problem lists rather than engagement difficulties). This is, to our knowledge, the first study to suggest that cognitive therapy alone can prevent or delay progression to psychosis. Our findings complement the study of combined pharmacological therapy and psychotherapy (Reference McGorry, Yung and PhillipsMcGorry et al, 2002), which found a reduction in transition at the end of treatment but not at the 6-month follow-up; a double-masked, placebo-controlled trial of pharmacotherapy alone in the same population is due to report its findings soon (Reference McGlashan, Zipursky and PerkinsMcGlashan et al, 2003). It would also appear that cognitive therapy reduces the severity of subclinical psychotic experiences over a 12-month period, for which the individual had originally sought help. There was no evidence that the therapy improved functioning or distress (as measured by scores on the GAF and GHQ), although there was a large amount of missing data for these measures. The potential importance of prevention in this area is further highlighted by the apparent emergence of structural brain deficits in those high-risk participants who went on to develop psychosis (Reference Pantelis, Velakoulis and McGorryPantelis et al, 2003).
Why cognitive therapy?
There are several problems associated with using antipsychotic medication in an ultra-high-risk group. The risks associated with using pharmacological interventions with false-positive cases are considerable, adherence to antipsychotic medication regimens within this group is variable (Reference McGorry, Yung and PhillipsMcGorry et al, 2002) and the ethical position has caused some debate. In particular, it has been suggested (Reference Bentall and MorrisonBentall & Morrison, 2002) that use of antipsychotic medication is problematic because these drugs have harmful and stigmatising side-effects, their effect on the developing brain in adolescents is unknown, and because they target psychotic experiences, which may not be the priority for people at high risk. The ethics of using cognitive therapy with this client population may, therefore, be less controversial, especially as our patients are seeking help. We have argued (Reference Morrison, Bentall and FrenchMorrison et al, 2002) that such therapy may be well suited to the prevention of psychosis. Its efficacy as an adjunct to routine treatments has been demonstrated in acute psychosis (Reference Drury, Birchwood and CochraneDrury et al, 1996) and in cases of chronic, persistent psychotic symptoms (Reference Tarrier, Yusupoff and KinnerTarrier et al, 1998; Reference Sensky, Turkington and KingdonSensky et al, 2000), as well as in relapse prevention (Reference Gumley, O'Grady and McNayGumley et al, 2003) and emotional disorders (Reference Clark, Salkovskis and HackmannClark et al, 1994). Moreover, it is arguably less likely to result in distressing side-effects than medication. Our results suggest that a specific psychological intervention that is not usually associated with severe side-effects will be an effective and acceptable alternative to antipsychotic medication, particularly as a first line of treatment, for patients at ultra-high risk of developing psychosis. Indeed, McGorry et al (Reference McGorry, Yung and Phillips2002) suggested that their ‘general stance is that off-label use of even novel antipsychotic medications in such patients should not be first-line treatment’. It remains to be seen whether cognitive therapy truly prevents transition to psychosis, or merely provides a delay in onset (i.e. whether this effect would continue throughout a longer follow-up period).
Limitations and future directions
The fact that there was a significant effect of cognitive therapy on all psychosis-related outcome measures, both primary and secondary, suggests that these findings are likely to be robust. However, our study has methodological limitations. The sample size was small, and the 12-month transition rate overall of 12% (excluding the 2 individuals with psychosis at baseline) was lower than that of 26% in the PACE trial (Reference McGorry, Yung and PhillipsMcGorry et al, 2002), perhaps owing to lower non-consent rates in this trial. It proved impossible fully to maintain masking to treatment allocation for assessment of the primary outcome, as had also been the case in the previous trial in this population (Reference McGorry, Yung and PhillipsMcGorry et al, 2002). The method of randomisation, which resulted in uneven group sizes, was not ideal, but was unbiased, independent and pragmatic. The exclusion of two participants who, at the first post-randomisation assessment, reported having been psychotic at the time of the baseline assessment is another issue, as the study would not have achieved significant results had they been included in the analyses. However, it would seem reasonable to exclude such patients when they were unambiguously reporting that they were effectively unsuitable for inclusion for the trial at entry, so long as this occurred at a time prior to any treatment. There were also a number of participants lost to follow-up, and some participants did not have complete data-sets, owing to the highly mobile nature of this population. It should also be noted that both the monitoring and the therapy conditions included elements of case management, such as helping people network with appropriate services to address social problems such as housing and finances. It is also difficult to determine whether there is a specific beneficial effect of cognitive therapy or whether gains are attributable to non-specific effects of having a therapeutic relationship and regular contact with a mental health professional; however, as a pragmatic preliminary trial designed to discover whether an intervention worked at all, these results certainly support the further investigation of such therapy as a preventive intervention. Formal indices of treatment integrity were not assessed, although both therapists had close supervision and had specific post-qualification training in cognitive therapy.
Future research in this area should attempt to address such issues. This study measured psychotic experiences – rather than the distress and disability associated with them – as the primary outcome; it would be desirable to measure the latter in future studies, along with service-user-defined outcomes and the occurrence of non-psychotic disorders in this population. Future studies should also attempt to evaluate side-effects and acceptability of treatment in a more formal manner; for example, the risk of stigmatisation that exists with psychological interventions should be monitored. Further research of this kind should also include a 1-month baseline period with reassessment of eligibility, in order to exclude those concealing a psychotic disorder, and, ideally, a control condition that would deliver equivalent contact with a therapist in order to control for non-specific aspects (which might also help to maintain masking).
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Cognitive therapy appears to be a promising intervention for the indicated prevention of psychosis in a high-risk population.
-
▪ This therapy reduced the severity of psychotic phenomena over12 months in a high-risk population.
-
▪ Cognitive therapy for the prevention of psychosis appears to be an acceptable intervention that should avoid the distressing side-effects associated with medication.
LIMITATIONS
-
▪ The study had a relatively small sample size.
-
▪ It proved impossible fully to maintain masking to treatment allocation for assessment of the primary outcome.
-
▪ A number of participants were lost to follow-up and some had incomplete datasets, owing to the highly mobile nature of this population.
Acknowledgements
This research was supported by research grants from the North West NHS. Research and Development Executive and the Stanley Foundation. We thank Professor Graham Dunn for statistical advice, Dr Samantha E. Bowe for her help in providing cognitive therapy, and Uma Patel, Alice Knight, Marianne Kreutz, Sandra Neil and Shreeta Raja for their assistance with data collection and data entry.







eLetters
No eLetters have been published for this article.