In spite of the fact that the UK was one of the first countries to develop specialist old age services, since the economic crisis and the restructuring of the National Health Service (NHS) the situation has started to change. There has been a drive to create ‘age inclusive’ mental health to address the needs of people regardless of their age. However, authoritative voices have expressed concern that an ageless service might well cause even more discrimination for elderly people if it is not designed to meet their specific needs. Reference Warner1 The Royal College of Psychiatrists, together with many other organisations concerned with the care of elderly people who are mentally ill, had asked the government for a halt in the implementation of ageless mental health services. Reference Bailey, Warner, Farrar, Dalton, Anderson and Burley2 In spite of this, by 2013 almost 11% of NHS trusts had already disbanded their old age psychiatry teams. Reference Warner3 In 2014 the President of the College wrote to the Minister of State for Care and Support warning of the dangers of treating 18- and 80-year-olds within the same team. 4
Even before the advent of ageless services there was no coherent policy to determine which services should look after older people with functional mental illness. Reference Green, Girling, Lough, Ng and Whitcher5 This lack of policy may relate to a lack of evidence. A survey of the needs of older people with enduring mental illness identified many unmet needs, Reference McNulty, Duncan, Semple, Jackson and Pelosi6 although there are clear problems in using a generic needs assessment tool in an elderly population. Reference Abdul-Hamid, Johnson, Thornicroft, Holloway and Silverman7 Jolley et al argued that there should be a needs assessment that takes in consideration local services and resources. Reference Jolley, Kosky and Holloway8 The current study reports a survey using a needs assessment schedule that was developed and validated on older people with functional mental illness. Reference Abdul-Hamid, Lewis-Cole, Holloway and Silverman9 In this study, we assessed the needs of an epidemiologically based sample of elderly people with functional mental illness in contact with old age psychiatry and general adult psychiatry services to explore which of the two services was better in meeting the needs of these patients.
Method
The aims of this study were: to undertake a needs assessment of all old people with enduring mental illness in contact with specialist mental health services (both general adult and old age psychiatry services) in a defined catchment area; and to compare the extent to which both services met the needs of this population. The study was carried out in Norwood, an ethnically diverse and socially deprived sector of the then Bethlem and Maudsley Trust catchment area in inner London. Two of the authors were the adult general and old age psychiatry consultants in this sector. The sampling frame of the study population included all patients aged 60 or over with functional mental illness who were in contact with the catchment area psychiatric services and who had the onset of their illness before the age of 60. Along with patients who were over 65 years of age, a ‘pre-elderly’ group of patients who were 60–65 years of age was included. Given the chronic and enduring nature of their illnesses this ‘pre-elderly’ group were highly likely to become ‘graduates’ of adult services within the succeeding 5 years. More than 300 medical notes of Norwood patients aged 60 or over were reviewed and 77 people with enduring mental illness were identified. The definition of ‘graduates’ used was that of Arie & Jolley: Reference Arie, Jolley, Levy and Post10 people with severe functional psychiatric disorders who graduate into old age. All patients with organic mental health problems or those with functional disorders who only came in contact with psychiatric services after the age of 65 were excluded. In total 64 out of the 77 patients identified were interviewed (3 were untraceable). Of these, 40 were in contact with the general adult psychiatry service and 34 were in contact with the old age psychiatry service. These patients and their psychiatric key workers were interviewed separately. Interviews were only started after securing ethical approval. The assessment package consisted of the following questionnaires: (a) Mini-Mental State examination; Reference Folstein, Folstein and McHugh11 (b) the Brief Psychiatric Rating Scale; Reference Ventura, Green, Shanter and Liberman12 (c) the Geriatric Depression Scale; Reference Yesavage, Brink, Rose, Lum, Huang and Adey13 (d) the Clifton Assessment Procedure for the Elderly (CAPE); Reference Pattie and Gilleard14 (e) the Elderly Psychiatric Needs Schedule (EPNS). Reference Abdul-Hamid, Lewis-Cole, Holloway and Silverman9
Statistical analysis included the following statistical methods: producing simple frequencies of study variables in the sample and hypothesis testing using bivariate analysis of crude rates (using the chi-squared test and t-test) generating significance tests in the form of P-values and confidence intervals.
Results
Demographic and clinical features
Not surprisingly the age groups of the general adult psychiatry group and old age psychiatry group were significantly different. Only 46% (n = 15) of the general adult psychiatry group were aged 65 years and over, whereas 97% (n = 39) of the old age psychiatry group were 65 years and over (χ2 = 25, P<0.00001). The general adult psychiatry group had an equal proportion of men and women, whereas the majority of the old age psychiatry sample (70%, n = 28) were women (the difference in gender was, however, not statistically significant between the two groups). The marital status of the two groups was similar. The ethnic origin of the sample reflected the age of the two groups and a cohort effect that reflects the changing demography of the sector as there were more White people in the old age psychiatry group (98% (n = 39) compared with 79% (n = 27) in the general adult psychiatry group). The difference was not statistically significant.
The main clinical diagnosis recorded in patients' hospital notes showed a higher proportion (not statistically significant) of people with schizophrenia among the general adult psychiatry group (56% (n = 19) compared with 28% (n = 11) in the old age psychiatry group) and a higher proportion (not statistically significant) of people with depression among the old age psychiatry sample (58% (n = 23) compared with 21% (n = 7) in the general adult psychiatry group).
Comparing needs
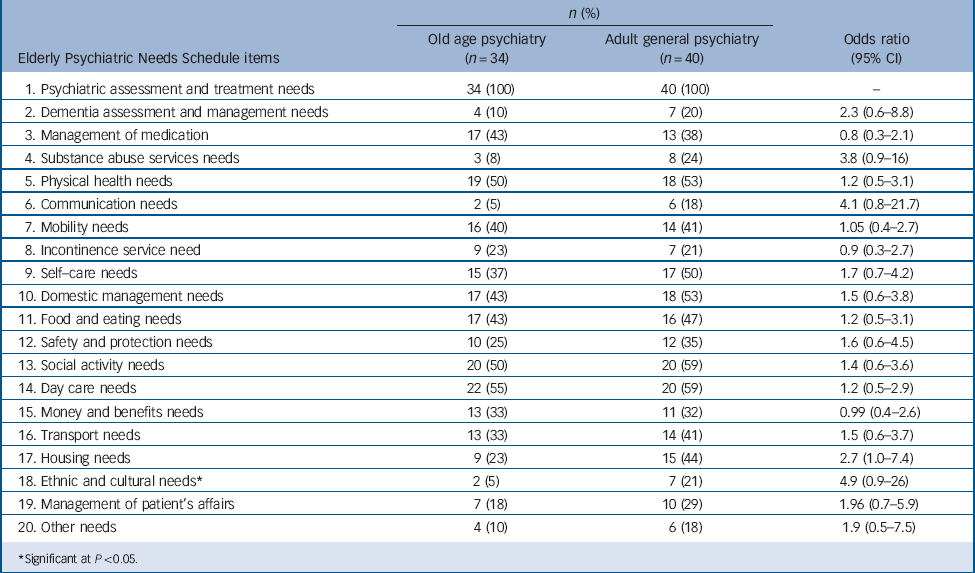
‘Total needs’ within the EPNS includes both met and unmet needs. It is a measure of disablement and is therefore potentially independent of service provision. Reference Wing15 Table 1 shows the distribution of these needs within the old age psychiatry and general adult psychiatry groups. In both groups 100% had a need for psychiatric assessment and treatment, which is reassuring since people should not be in contact with a psychiatric service if they do not have this need. More people in the general adult psychiatry group (21%, n = 7) needed dementia assessment compared with the old age psychiatry group (10%, n = 4), although this difference was not statistically significant. This might reflect the higher prevalence of schizophrenia in the general adult psychiatry group. A higher proportion of the general adult psychiatry group needed substance misuse services (24% (n = 8) compared with 8% (n = 3) in the old age psychiatry group) but this difference was not statistically significant.
TABLE 1 Comparison of total needs of the old people with enduring mental illness who are in contact with adult general adult and old age psychiatry
| n (%) | |||
|---|---|---|---|
| Elderly Psychiatric Needs Schedule items | Old age
psychiatry (n = 34) |
Adult general
psychiatry (n = 40) |
Odds ratio (95% CI) |
| 1. Psychiatric assessment and treatment needs | 34 (100) | 40 (100) | - |
| 2. Dementia assessment and management needs | 4 (10) | 7 (20) | 2.3 (0.6–8.8) |
| 3. Management of medication | 17 (43) | 13 (38) | 0.8 (0.3–2.1) |
| 4. Substance abuse services needs | 3 (8) | 8 (24) | 3.8 (0.9–16) |
| 5. Physical health needs | 19 (50) | 18 (53) | 1.2 (0.5–3.1) |
| 6. Communication needs | 2 (5) | 6 (18) | 4.1 (0.8–21.7) |
| 7. Mobility needs | 16 (40) | 14 (41) | 1.05 (0.4–2.7) |
| 8. Incontinence service need | 9 (23) | 7 (21) | 0.9 (0.3–2.7) |
| 9. Self–care needs | 15 (37) | 17 (50) | 1.7 (0.7–4.2) |
| 10. Domestic management needs | 17 (43) | 18 (53) | 1.5 (0.6–3.8) |
| 11. Food and eating needs | 17 (43) | 16 (47) | 1.2 (0.5–3.1) |
| 12. Safety and protection needs | 10 (25) | 12 (35) | 1.6 (0.6–4.5) |
| 13. Social activity needs | 20 (50) | 20 (59) | 1.4 (0.6–3.6) |
| 14. Day care needs | 22 (55) | 20 (59) | 1.2 (0.5–2.9) |
| 15. Money and benefits needs | 13 (33) | 11 (32) | 0.99 (0.4–2.6) |
| 16. Transport needs | 13 (33) | 14 (41) | 1.5 (0.6–3.7) |
| 17. Housing needs | 9 (23) | 15 (44) | 2.7 (1.0–7.4) |
| 18. Ethnic and cultural needs* | 2 (5) | 7 (21) | 4.9 (0.9–26) |
| 19. Management of patient's affairs | 7 (18) | 10 (29) | 1.96 (0.7–5.9) |
| 20. Other needs | 4 (10) | 6 (18) | 1.9 (0.5–7.5) |
* Significant at P<0.05.
The general adult psychiatry group had higher needs for most of the EPNS items but none of them reached statistical significance apart from ethnic and cultural needs (21% (n = 7) compared with only 5% (n = 2) in the old age psychiatry group). A calculation of the mean total needs in the two groups reflected the same pattern. The mean total needs for the general adult psychiatry group was 8.0 needs compared with 6.5 needs in the old age psychiatry group. There was a non-significant difference between mean total needs for the two groups (t = 1.2, P = 0.2).
Unmet needs
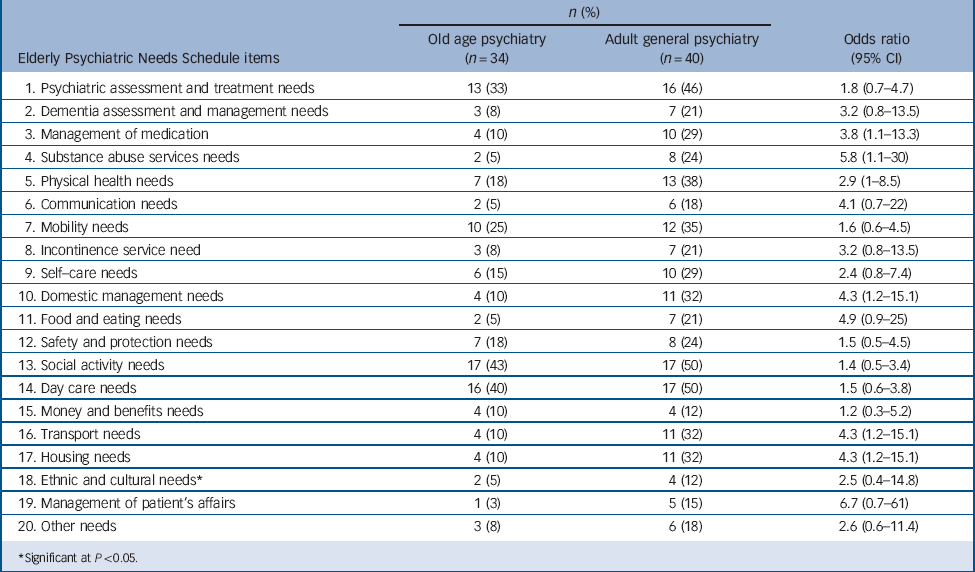
Table 2 shows the distribution of unmet needs in the old age psychiatry and general adult psychiatry groups. Unmet need was more common in the general adult psychiatry group across all 20 need domains and statistically significantly so in 6 domains. There were significantly higher unmet needs in the general adult psychiatry group on the management of medication (29% (n = 10) compared with 10% (n = 4) in the old age psychiatry group); substance misuse service needs (24% (n = 8) compared with 5% (n = 2) in the old age psychiatry group); physical health needs (38% (n = 13) compared with 18% (n = 7) in the old age psychiatry group); domestic management needs (32% (n = 11) compared with 10% (n = 4) in the old age psychiatry group); transport needs (32% (n = 11) compared with 10% (n = 4) in the old age psychiatry group); and housing needs (32% (n = 11) compared with 10% (n = 4) in the old age psychiatry group). The general adult psychiatry group had significantly more unmet needs than the old age psychiatry group (5.6 (s.d. = 6.4) v. 2.8 (s.d. = 3.4) t = 2.2, P = 0.03).
TABLE 2 Comparison of unmet needs of the old people with enduring mental illness who are in contact with adult general adult and old age psychiatry
| n % | |||
|---|---|---|---|
| Elderly Psychiatric Needs Schedule items | Old age
psychiatry (n = 34) |
Adult general
psychiatry (n = 40) |
Odds ratio (95% CI) |
| 1. Psychiatric assessment and treatment needs | 13 (33) | 16 (46) | 1.8 (0.7–4.7) |
| 2. Dementia assessment and management needs | 3 (8) | 7 (21) | 3.2 (0.8–13.5) |
| 3. Management of medication | 4 (10) | 10 (29) | 3.8 (1.1–13.3) |
| 4. Substance abuse services needs | 2 (5) | 8 (24) | 5.8 (1.1–30) |
| 5. Physical health needs | 7 (18) | 13 (38) | 2.9 (1–8.5) |
| 6. Communication needs | 2 (5) | 6 (18) | 4.1 (0.7–22) |
| 7. Mobility needs | 10 (25) | 12 (35) | 1.6 (0.6–4.5) |
| 8. Incontinence service need | 3 (8) | 7 (21) | 3.2 (0.8–13.5) |
| 9. Self–care needs | 6 (15) | 10 (29) | 2.4 (0.8–7.4) |
| 10. Domestic management needs | 4 (10) | 11 (32) | 4.3 (1.2–15.1) |
| 11. Food and eating needs | 2 (5) | 7 (21) | 4.9 (0.9–25) |
| 12. Safety and protection needs | 7 (18) | 8 (24) | 1.5 (0.5–4.5) |
| 13. Social activity needs | 17 (43) | 17 (50) | 1.4 (0.5–3.4) |
| 14. Day care needs | 16 (40) | 17 (50) | 1.5 (0.6–3.8) |
| 15. Money and benefits needs | 4 (10) | 4 (12) | 1.2 (0.3–5.2) |
| 16. Transport needs | 4 (10) | 11 (32) | 4.3 (1.2–15.1) |
| 17. Housing needs | 4 (10) | 11 (32) | 4.3 (1.2–15.1) |
| 18. Ethnic and cultural needs* | 2 (5) | 4 (12) | 2.5 (0.4–14.8) |
| 19. Management of patient's affairs | 1 (3) | 5 (15) | 6.7 (0.7–61) |
| 20. Other needs | 3 (8) | 6 (18) | 2.6 (0.6–11.4) |
* Significant at P<0.05.
Discussion
Historically the specialty of old age psychiatry has looked after patients who are frail and vulnerable. In addition to patients who have dementia of any age, the specialty manages patients with functional psychiatric disorders, physical illness and frailty, and also those with psychological and social difficulties associated with old age. Reference Warner3 The last two groups contain patients with functional problems who are traditionally known as ‘graduates’. These two groups are more likely to be looked after by general adult psychiatry under the new ageless services. Reference Warner1
Main findings
In this study we looked in detail at the needs of graduates at the interface between general adult psychiatry and old age psychiatry services. We found that old age psychiatry services were at the time of the study better able to meet the needs of graduates, which goes against the current trend towards ‘age-inclusive’ services. These patients are at risk of being overlooked in such ageless services, particularly when competing for resources with more disturbed younger patients.
The difference in age and diagnosis between the two groups reflects the nature of the interface between the two services and a cohort effect. Before the advent of ‘age-inclusive’ services it was usual for people with relapsing psychiatric disorder such as severe affective disorder to move to old age psychiatry services if they have a relapse after the age of 65 following a period out of contact with adult mental health services.
The ‘elderly graduates’ in contact with old age psychiatry in our study had significantly fewer unmet needs compared with those in contact with general adult psychiatry. This is in spite of the fact that total needs were not significantly different in the two groups. Tellingly the domains where unmet need was significantly more common in the general adult psychiatry group included management of medication, physical healthcare, domestic management, transport and housing. These were needs related to frailty that old age psychiatry services were more successful in addressing.
Limitations
This study reflects the work of the two services in a single innercity context. Feedback sessions for staff in the two services revealed the adult general psychiatry service was struggling with younger more disturbed patients who tend to divert time and resources away from older patients. There might be a need to repeat this study with a bigger sample that could include suburban and rural areas. The small sample also might have increased the risk of type II error, which also makes it necessary to recommend conducting further, and bigger, studies on this subject. Furthermore, the study is a cross-sectional assessment, which indicates the need for further follow-up studies in the field to make the finding more generalisable.
Implications
One of the main arguments that commissioners and local managers have put forward in support of the ageless services is that ‘there is no evidence to say that old age services are better’. Reference Warner1 In spite of the limitations of this paper it is safe to conclude that the assumption implicit in the construction of ‘ageless’ services, in that working-age adult teams caring for people with enduring mental health problems in later life might be better than old age psychiatry services, is not supported. Furthermore, those calling for ageless services need to look at the lessons from the past century's introduction of generic practice in social care. The 1968 Seebohm Report on Social Services aimed at replacing ‘a number of fragmented specialism with a confident generalism’. Reference Jones16 Thompson, writing almost four decades later, highlighted the complications of such an approach in the form of making the demand for services infinite, Reference Thompson17 needing a large undefined knowledge-base, Reference Thompson17 creating a large bureaucratic organisation Reference Thompson17 and resulting in a negative media and social image of the profession. Reference Thompson17 The ageless services might also cause resources and personnel to move from less popular services to more popular ones such as children services. Reference Cassel18 This paper is a small piece of evidence highlighting the risks to those patients with mental illness who are frail and elderly resulting from implementing ageless mental health services.





eLetters
No eLetters have been published for this article.