Dementia and depression are common psychiatric disorders in people over the age of 60 years. 1 At present, around 50 million people in the world are living with dementia, Reference Barnes and Yaffe2 and an estimated 30 million older adults are living with depression. Reference Beekman, Copeland and Prince3 They represent two of the world's biggest health problems and are increasingly a major public health challenge given that the world's population is ageing. Both disorders are associated with poorer overall health, social function and healthcare outcomes, and increased mortality. Reference Sampson, Blanchard, Jones, Tookman and King4–Reference Moussavi, Chatterji, Verdes, Tandon, Patel and Ustun7 However, these mental illnesses can be difficult to identify and often remain undetected, Reference Worrall and Moulton8–Reference Collerton, Davies, Jagger, Kingston, Bond and Eccles10 and possibly form barriers to care. Undetected dementia and depression levels vary among countries depending on social and cultural characteristics and health service provision. In the UK, O'Connor et al Reference O'Connor, Pollitt, Hyde, Brook, Reiss and Roth11 examined 208 patients aged over 75 years and observed that general practitioners (GPs) failed to identify 42% of those assessed as having dementia using the Cambridge Mental Disorders of the Elderly Examination. In Canada, Worrall & Moulton Reference Worrall and Moulton8 found that among 20 individuals with dementia (identified by the Canadian Mental Status Questionnaire) in rural community-dwelling residents aged >70 years, 15 patients (75%) were undetected in medical records. In Finland, Arve et al Reference Arve, Lauri, Lehtonen and Tilvis9 found that GPs failed to detect depression in 58% of 109 patients aged 70 years. A failure to detect dementia and depression can cause delays in starting treatment, leading to patient suffering, disability and worsening of the prognosis. Reference Licht-Strunk, Beekman, de and van Marwijk12,Reference Sternberg, Wolfson and Baumgarten13
Despite the high risk of non-detection of dementia and depression in older adults, related risk factors are not well known. Knowledge relating to levels of underdetection is mainly derived from studies undertaken in high-income countries, with consequential problems in generalising findings to low- and middle-income countries (LMICs) across the world. There are few studies examining undetected dementia and depression in older adults in LMICs, where the majority of dementia and depression occurs. Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14 Studying an older population in LMICs may offer internationally applicable insights into the level and determinants of undetected dementia and depression and aid earlier diagnosis. In this paper we examine data from a large-scale community-dwelling-based survey in China to explore determinants for undetected dementia and depression in older adults.
Method
The study population was derived from participants in a multicentre study of mental health in older adults in China; including a four-province study, Reference Chen, Wilson, Chen, Zhang, Qin and He15 an extended study in Hubei province and the Anhui cohort third-wave survey. Reference Chen, Hu, Wei, Ma, Liu and Copeland16 All were community-based household survey studies, with a common research protocol.
The four-province study
The methods of the four-province study have been fully described elsewhere. Reference Chen, Wilson, Chen, Zhang, Qin and He15 In brief, in 2008–2009 we selected one rural and one urban community from each of four provinces (Guangdong, Heilongjiang, Shanghai and Shanxi – four research centres) as the study fields, trying to recruit no fewer than 500 participants in each community. We employed a cluster randomised sampling method to choose residential communities from each of the four provinces; in Guandong, Jitang subdistrict in Huangpu district in Guangzhou city and Lianfeng village in Zhongshan county; in Heilongjiang, Dayou subdistrict in Daowai district in Harbin and four villages in Xianfeng township in Suihua; in Shanghai, a subdistrict (Xietu Road) in Xuhui district and two villages in Xingta township; in Shanxi, a subdistrict in Jinzhong and five villages in Zhuangzi township. The target population consisted of residents aged ≥60 years living in the area for at least 5 years. Ethical approval for the study was obtained from the Research Ethics Committee, University College London, UK, and from the Research Ethics Committee of Anhui Medical University and the local governments in China. Based on the residency list of the committees of the village and the district, we recruited a total of 4314 participants, with an overall response rate of 93.8%. Two researchers from each centre team were trained at the Anhui Medical University, where we had completed several surveys of mental illness in older people and had a skilled and experienced interview team. Reference Chen, Hu, Wei, Ma, Liu and Copeland16–Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 The trained researchers cascaded skills to local research teams and trained the interviewers. The local survey team from Guangzhou, Harbin and Shanxi Medical Universities and the School of Public Health of Fudan University interviewed the participants at home. Permission for interview and informed consent were obtained from each participant or, if that was not possible, from the closest responsible adult. In about 5% of the interviews, informed consent was impossible to elicit; in these cases, the nearest relative or carer was approached to provide assent to participation. The main interview included a general health and risk factors record, Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 the Geriatric Mental State (GMS) questionnaire Reference Chen, Hu, Qin, Xu and Copeland17 and other components of the 10/66 algorithm dementia research package. Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14,Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19 In the general health and risk-factors component we recorded details relating to socio-demography, social networks and support, and cardiovascular and other risk factors. Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 Socioeconomic variables included rural/urban domicile area, educational level, occupational class, and annual personal and family incomes. We asked participants (or their carers if the participant was unable to answer) whether they had received a doctor's diagnosis of heart disease (coronary or valve disease), angina, stroke, diabetes, Reference Chen, Song, Hu and Brunner20 chronic bronchitis, chronic kidney disease, cancer, overactive or underactive thyroid, dementia, depression, epilepsy, Parkinson's disease, etc. We measured systolic and diastolic blood pressure, height, weight and waist circumference for all participants according to standard procedures. Reference Chen and Tunstall-Pedoe21
The Hubei Study
In 2010–2011, we extended the project to include the Hubei province, using the same protocol as in the four-province study. Two researchers from the team at Hubei University of Medicine were trained at Anhui Medical University, capitalising on the experience of having undertaken several surveys of mental illness in older adults. Reference Chen, Hu, Wei, Ma, Liu and Copeland16–Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 We selected Maojian subdistrict in Shiyan city and Yanhe village in Wushan township of Wucheng county as the study field. In total, we recruited 1001 participants aged ≥60 years, and achieved a response rate of 91.8%.
Diagnosis of depression and dementia
Utilising the data from the interview, we documented all doctor-diagnosed cases of dementia and depression (defined as ‘detected cases’). The Geriatric Mental State – Automated Geriatric Examination for Computer Assisted Taxonomy (GMS-AGECAT) Reference Chen, Hu, Qin, Xu and Copeland17,Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18,Reference Copeland, Prince, Wilson, Dewey, Payne and Gurland22 and the 10/66 algorithms Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14,Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19 were used to diagnose depression and dementia in this population.
The GMS data were analysed by a computer program-assisted diagnosis, the AGECAT, to assess the principal mental disorders in the study participants. Reference Chen, Hu, Qin, Xu and Copeland17,Reference Copeland, Prince, Wilson, Dewey, Payne and Gurland22 The methods of the diagnosis have been fully described in previous publications. Reference Chen, Hu, Wei, Qin, McCracken and Copeland23,Reference Chen, Hu, Wei, Qin and Copeland24 The GMS-AGECAT depression diagnosis has been validated in China. Reference Chen, Hu, Qin, Xu and Copeland17,Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18
Individuals with dementia were identified using the 10/66 dementia algorithm, which has been widely used and validated in older adults with low educational levels in LMICs including in China. Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14,Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19 The 10/66 dementia diagnosis requires four inputs from the interview: the GMS-AGECAT diagnostic output, the Community Screening Instrument for Dementia (CSI-D) cognitive test score (COGSCORE), the CSI-D informant interview (RELSCORE) and the modified Consortium to Establish a Registry for Alzheimer's Disease (CERAD) ten-word list learning task with delayed recall. Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14,Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19 To save our research resources and to complete each interview within time, we designed a two-phase interview. In phase one, we completed the GMS, the CSI-D cognitive test and CERAD, as well as the general health and risk factors interview. Using three of the four constituent components of the 10/66 algorithm (i.e. data of GMS-AGECAT, the CSI-D cognitive test and CERAD interview), Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14,Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19,Reference Prince, Acosta, Chiu, Scazufca and Varghese25 we calculated a probability of possible dementia for each participant. In phase two, which started about 8 months (s.d. = 2) after phase one completion, we selected the top 15% of the population who had the highest probability of having ‘dementia’ as ‘probable cases’ and a random sample of 5% of the rest as ‘probable non-cases’ for subsequent interviews in each centre. The interview team completed the CSI-D informant interview for the selected participants. We used a cut-off point of probability derived from the full 10/66 algorithm to diagnose dementia, which has been validated in China. Reference Llibre Rodriguez, Ferri, Acosta, Guerra, Huang and Jacob14
The third-wave survey of the Anhui study
This was based on our Anhui follow-up study, the methods of which have been fully described. Reference Chen, Hu, Wei, Ma, Liu and Copeland16–Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18,Reference Chen, Hu, Wei, Qin, McCracken and Copeland23,Reference Chen, Hu, Wei, Qin and Copeland24 In brief, in 2001–2003 we examined a random sample of 3336 residents aged ≥60 years in the Yiming district of Hefei city and the Tangdian district of Yingshang county, Anhui province (wave 1) using the standard interview method of GMS-AGECAT. One year after the baseline investigation we re-examined 2608 cohort members (wave 2). Reference Chen, Hu, Wei, Qin, McCracken and Copeland23,Reference Chen, Hu, Wei, Qin and Copeland24 In 2007–2009 we carried out the third wave of the survey within the cohort. Using a similar protocol to that in the four-province study but differing slightly in the phase-two interview (including all 127 participants with phase one GMS-AGECAT dementia who had not completed the CSI-D cognitive test and the modified CERAD interview Reference Chen, Hu, Wei, Ma, Liu and Copeland16 ), we successfully interviewed 1757 participants with a response rate of 82.4% of surviving cohort members. Reference Chen, Hu, Wei, Ma, Liu and Copeland16
Statistical analysis
The SPSS statistical package (Windows version 16.0) was used for data analysis. Patients with undetected dementia and depression were defined as those who were diagnosed in the survey using the validated 10/66 algorithm and GMS-AGECAT but did not have doctor-diagnosed dementia or depression. Using adjusted logistic regression models we calculated odds ratios (ORs) and 95% CIs for undetected dementia and depression among patients in relation to baseline risk factors. In the model we adjusted for age, gender, activity of daily living (ADL) score and six-province geographic variable to reduce their confounding and cluster effects on the associations of undetected dementia and depression with each of the important determinants.
Results
Among 7072 participants, we diagnosed 359 (5.1%) as having dementia and 328 (4.6%) as having depression. There were 26 (0.7%) participants who had doctor-diagnosed dementia reported and 26 (0.8%) having doctor-diagnosed depression. The percentage of undetected dementia was 93.1 (95% CI 90.1–95.4) and of undetected depression was 92.5 (95% CI 89.2–95.0).
Tables 1, 2, 3 give the frequencies of risk factors for undetected dementia and depression. Both undetected disorders were associated with living in a rural area and low educational level and occupational class (Table 1). Undetected dementia was also associated with having ‘help available when needed’ (Table 2), and inversely, with a family history of mental illness, thyroid problems, hearing problems and low ADL (Table 3). Participants with undetected depression were more likely to be women, have low personal and family incomes (Table 1) and have more than three children (Table 2), whereas detected depression was related to having heart disease (Table 3). Neither undetected dementia nor undetected depression were significantly related to age, body mass index, alcohol drinking, marital status, living with family members, children/relatives visiting, having a religious belief, and other comorbidities (hypertension, angina, stroke, vision problem, chronic obstructive pulmonary disease, cancer, head injury) (data not shown).
In our adjustment analysis (Tables 1, 2, 3), we found similar associations to those in the univariate analysis. However, their statistical significances were changed; undetected dementia was no longer associated with having thyroid problems and hearing problems, while undetected depression was significantly related to fewer frequencies of visiting children/relatives.
Discussion
In this large-scale, community-based household survey in China we observed higher levels of undetected dementia and depression than has been reported in the West. Reference Arve, Lauri, Lehtonen and Tilvis9–Reference O'Connor, Pollitt, Hyde, Brook, Reiss and Roth11,Reference Eefsting, Boersma, Van den Brink and Van26,Reference Garrard, Rolnick, Nitz, Luepke, Jackson and Fischer27 Non-detection of both disorders was related to low socioeconomic status and some aspects of social networks. Patients with functional impairment and with family histories of mental illness were exposed to health examinations for detecting dementia, and having heart disease was associated with an increased chance of detecting depression.
Table 1 Numbers and percentages of undetected and detected dementia and depression, and odds ratios of undetection by basic characteristics and sociodemographic status in the six-province study of mental health in older adults, China
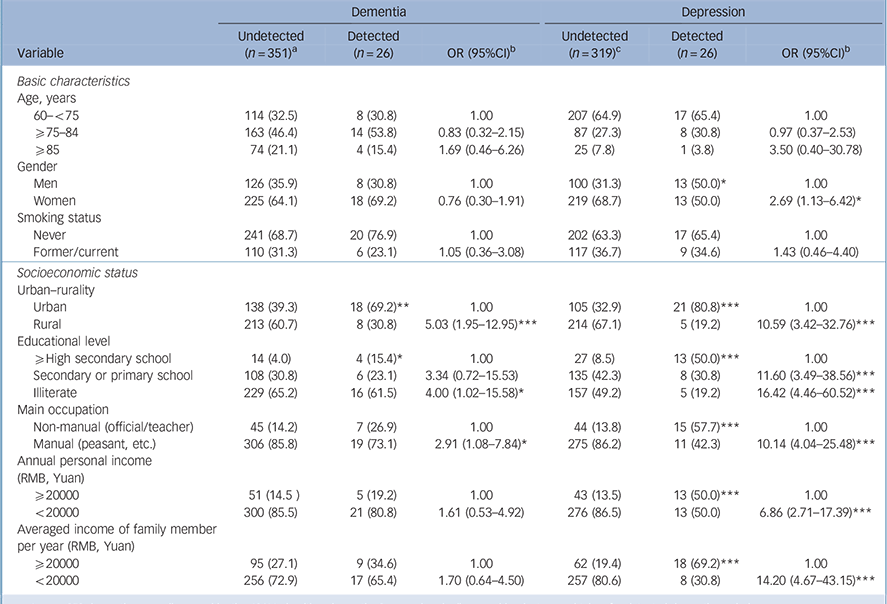
| Dementia | Depression | |||||
|---|---|---|---|---|---|---|
| Variable | Undetected (n = 351)Footnote a |
Detected (n = 26) |
OR (95%CI)Footnote b | Undetected (n = 319)Footnote c |
Detected (n = 26) |
OR (95%CI)Footnote b |
| Basic characteristics | ||||||
| Age, years | ||||||
| 60-<75 | 114 (32.5) | 8 (30.8) | 1.00 | 207 (64.9) | 17 (65.4) | 1.00 |
| ≥75-84 | 163 (46.4) | 14 (53.8) | 0.83 (0.32-2.15) | 87 (27.3) | 8 (30.8) | 0.97 (0.37-2.53) |
| ≥85 | 74 (21.1) | 4 (15.4) | 1.69 (0.46-6.26) | 25 (7.8) | 1 (3.8) | 3.50 (0.40-30.78) |
| Gender | ||||||
| Men | 126 (35.9) | 8 (30.8) | 1.00 | 100 (31.3) | 13 (50.0)Footnote * | 1.00 |
| Women | 225 (64.1) | 18 (69.2) | 0.76 (0.30-1.91) | 219 (68.7) | 13 (50.0) | 2.69 (1.13-6.42)Footnote * |
| Smoking status | ||||||
| Never | 241 (68.7) | 20 (76.9) | 1.00 | 202 (63.3) | 17 (65.4) | 1.00 |
| Former/current | 110 (31.3) | 6 (23.1) | 1.05 (0.36-3.08) | 117 (36.7) | 9 (34.6) | 1.43 (0.46-4.40) |
| Socioeconomic status | ||||||
| Urban-rurality | ||||||
| Urban | 138 (39.3) | 18 (69.2)Footnote ** | 1.00 | 105 (32.9) | 21 (80.8)Footnote *** | 1.00 |
| Rural | 213 (60.7) | 8 (30.8) | 5.03 (1.95-12.95)Footnote *** | 214 (67.1) | 5 (19.2) | 10.59 (3.42-32.76)Footnote *** |
| Educational level | ||||||
| ≥High secondary school | 14 (4.0) | 4 (15.4)Footnote * | 1.00 | 27 (8.5) | 13 (50.0)Footnote *** | 1.00 |
| Secondary or primary school | 108 (30.8) | 6 (23.1) | 3.34 (0.72-15.53) | 135 (42.3) | 8 (30.8) | 11.60 (3.49-38.56)Footnote *** |
| Illiterate | 229 (65.2) | 16 (61.5) | 4.00 (1.02-15.58)Footnote * | 157 (49.2) | 5 (19.2) | 16.42 (4.46-60.52)Footnote *** |
| Main occupation | ||||||
| Non-manual (official/teacher) | 45 (14.2) | 7 (26.9) | 1.00 | 44 (13.8) | 15 (57.7)Footnote *** | 1.00 |
| Manual (peasant, etc.) | 306 (85.8) | 19 (73.1) | 2.91 (1.08-7.84)Footnote * | 275 (86.2) | 11 (42.3) | 10.14 (4.04-25.48)Footnote *** |
| Annual personal income (RMB, Yuan) | ||||||
| ≥20000 | 51 (14.5) | 5 (19.2) | 1.00 | 43 (13.5) | 13 (50.0)Footnote *** | 1.00 |
| <20000 | 300 (85.5) | 21 (80.8) | 1.61 (0.53-4.92) | 276 (86.5) | 13 (50.0) | 6.86 (2.71-17.39)Footnote *** |
| Averaged income of family member per year (RMB, Yuan) | ||||||
| ≥20000 | 95 (27.1) | 9 (34.6) | 1.00 | 62 (19.4) | 18 (69.2)Footnote *** | 1.00 |
| <20000 | 256 (72.9) | 17 (65.4) | 1.70 (0.64-4.50) | 257 (80.6) | 8 (30.8) | 14.20 (4.67-43.15)Footnote *** |
a. Among 359 dementia cases diagnosed by the 10/66 algorithm dementia, 8 were already diagnosed by doctors and taken for detected dementia analysis.
b. Adjusted for age, gender, activity of daily living score and six-province geographic variable.
c. Among 328 depression cases diagnosed by the GMS-AGECAT depression, 9 were already diagnosed by doctors and taken for detected depression analysis.
* P≤0.05 but >0.01
** P≤0.01 but >0.001
*** P<0.001; P-values are for chi-squared test in the univariate analysis.
Strengths and weaknesses of the study
Our study has several strengths. First, our data provide some important evidence regarding the role of socioeconomic variables in influencing the detection of dementia and depression. Second, we included a relatively large number of participants from community-dwelling settings for this study and the response rate was high. The sample size enabled the exploration of a wide range of potentially important determinants likely to influence detection. Third, we used the 10/66 algorithm to diagnose dementia, which caters for low educational levels in detecting dementia. Reference Prince, de Rodriguez, Noriega, Lopez, Acosta and Albanese19,Reference Prince, Acosta, Chiu, Scazufca and Varghese25 However, our study also has some limitations. We defined medically diagnosed dementia or depression based on information obtained from participants or their carers, without accessing medical records. This methodology may underestimate rates of ‘doctor-diagnosed’ dementia and depression because participants may not recall having been given a diagnosis or may be reluctant to divulge the information. We anticipated that the involvement of carers is likely to have mitigated potential underreporting. However, we concede that more robust information would have been obtained through access to relevant medical records. The study was cross-sectional and the causal relationship between non-detection and correlative factors requires longitudinal cohort studies for confirmation. However, we have identified certain high-risk groups, such as those with a low educational level and occupational class, and living in a rural area, that may benefit from screening. Despite the fact the study population consisted of representative samples from each of six
Table 2 Numbers and percentages of undetected and detected dementia and depression, and odds ratio of undetection by social network and support in the six-province study of mental health in older adults, China

| Dementia | Depression | |||||
|---|---|---|---|---|---|---|
| Variable | Undetected (n = 351)Footnote a |
Detected (n = 26) |
OR (95%CI)Footnote b | Undetected (n = 319)Footnote c |
Detected (n = 26) |
OR (95%CI)Footnote b |
| Number of children | ||||||
| 0-3 | 106 (30.2) | 11 (42.3) | 1.00 | 144 (45.1) | 20 (76.9)Footnote ** | 1.00 |
| ≥4 | 245 (69.8) | 15 (57.7) | 1.23 (0.47-3.26) | 175 (54.9) | 6 (23.1) | 3.41 (1.20-9.70)Footnote * |
| How far to your closest relatives | ||||||
| Outside county/city or no relatives | 61 (17.4) | 8 (32.0) | 1.00 | 102 (32.0) | 11 (42.3) | 1.00 |
| Within same town or district | 290 (82.6) | 18 (68.0) | 1.36 (0.46-4.03) | 217 (68.0) | 15 (57.7) | 0.75 (0.28-2.04) |
| Frequency of visiting children/relatives | ||||||
| Daily | 73 (20.8) | 10 (38.5) | 1.00 | 66 (20.7) | 10 (38.5) | 1.00 |
| <Daily and ≥monthly | 153 (43.6) | 6 (23.1) | 2.53 (0.82-7.81) | 119 (37.3) | 7 (26.9) | 3.87 (1.26-11.91)Footnote * |
| <Monthly | 125 (35.6) | 10 (38.5) | 1.89 (0.70-5.09) | 134 (42.0) | 9 (34.6) | 4.30 (1.41-13.09)Footnote ** |
| Frequency of contacting and speaking to friends in village/community | ||||||
| Daily | 81 (23.1) | 5 (19.2) | 1.00 | 81 (25.4) | 8 (30.8) | 1.00 |
| <Daily and ≥monthly | 156 (44.4) | 7 (26.9) | 1.24 (0.36-4.21) | 129 (40.4) | 13 (50.0) | 0.87 (0.31-2.41) |
| <Monthly | 114 (32.5) | 14 (53.8) | 0.80 (0.25-2.57) | 109 (34.2) | 5 (19.2) | 3.10 (0.88-10.96) |
| Help available when needed | ||||||
| No | 14 (4.0) | 4 (15.4)Footnote * | 1.00 | 33 (10.3) | 3 (11.5) | 1.00 |
| Yes | 337 (96.0) | 22 (84.6) | 5.45 (1.36-21.78)Footnote * | 286 (89.7) | 23 (88.5) | 0.92 (0.24-3.47) |
a. Among 359 dementia cases diagnosed by the 10/66 algorithm dementia, 8 were already diagnosed by doctors and taken for detected dementia analysis.
b. Adjusted for age, gender, activity of daily living score and six-province geographic variable.
c. Among 328 depression cases diagnosed by the GMS-AGECAT depression, 9 were already diagnosed by doctors and taken for detected depression analysis.
* P≤0.05 but >0.01
** P≤0.01 but >0.001
*** P<0.001; P-values are for chi-squared test in the univariate analysis.
Table 3 Numbers and percentages of undetected and detected dementia and depression, and odds ratios of undetection by family mental illness histories and comorbidities in the six-province study of mental health in older adults, China

| Dementia | Depression | |||||
|---|---|---|---|---|---|---|
| Variable | Undetected (n = 351)Footnote a |
Detected (n = 26) |
OR (95%CI)Footnote b | Undetected (n = 319)Footnote c |
Detected (n = 26) |
OR (95%CI)Footnote b |
| Any blood-related relatives having mental illnessFootnote d | ||||||
| No | 348 (99.1) | 23 (88.5)Footnote ** | 1.00 | 305 (95.6) | 23 (88.5) | 1.00 |
| Yes | 3 (0.9) | 3 (11.5) | 0.04 (0.01-0.25)Footnote ** | 14 (4.4) | 3 (11.5) | 0.19 (0.04-1.01) |
| All types of heart disease | ||||||
| No | 319 (90.9) | 21 (80.8) | 1.00 | 255 (79.9) | 14 (45.5)Footnote ** | 1.00 |
| Yes | 32 (9.1) | 5 (19.2) | 0.55 (0.18-1.72) | 64 (20.1) | 12 (46.2) | 0.26 (0.11-0.66)Footnote ** |
| Stroke | ||||||
| No | 320 (89.6) | 21 (77.3) | 1.00 | 291 (91.2) | 24 (92.3) | 1.00 |
| Yes | 31 (10.4) | 5 (22.7) | 0.65 (0.19-2.20) | 28 (8.8) | 2 (7.7) | 0.98 (0.19-5.11) |
| Diabetes | ||||||
| No | 336 (95.7) | 24 (92.3) | 1.00 | 300 (94.0) | 22 (84.6) | 1.00 |
| Yes | 15 (4.3) | 2 (7.7) | 0.73 (0.14-3.84) | 19 (6.0) | 4 (15.4) | 0.37 (0.09-1.50) |
| Overactive or underactive thyroid | ||||||
| No | 336 (95.7) | 21 (80.8)Footnote ** | 1.00 | 296 (92.8) | 22 (84.6) | 1.00 |
| Yes | 15 (4.3) | 5 (19.2) | 0.33 (0.06-1.70) | 23 (7.2) | 4 (15.4) | 0.63 (0.15-2.67) |
| Hearing problems | ||||||
| No | 186 (53.0) | 8 (30.8)Footnote * | 1.00 | 207 (64.9) | 19 (73.1) | 1.00 |
| Yes | 165 (47.0) | 18 (69.2) | 0.52 (0.21-1.31) | 112 (35.1) | 7 (26.9) | 1.65 (0.62-4.39) |
| Activities of daily living, scoreFootnote e | ||||||
| 0 | 232 (66.1) | 9 (34.6)Footnote ** | 1.00 | 254 (79.6) | 22 (84.6) | 1.00 |
| 1-4 | 45 (12.8) | 5 (19.2) | 0.25 (0.10-0.62)Footnote ** | 23 (7.2) | 2 (7.7) | 1.30 (0.40-4.24) |
| 5-28 | 74 (21.1) | 12 (46.2) | 42 (13.2) | 2 (7.7) | ||
a. Among 359 dementia cases diagnosed by the 10/66 algorithm dementia, 8 were already diagnosed by doctors and taken for detected dementia analysis.
b. Adjusted for age, gender, activity of daily living score and six-province geographic variable.
c. Among 328 depression cases diagnosed by the GMS-AGECAT depression, 9 were already diagnosed by doctors and taken for detected depression analysis.
d. Including dementia, depression, schizophrenia and other psychiatric diseases.
e. The participant reported their level of difficulty in questions of the activities of daily living (ADL) scale. The valid response was ‘no difficulty alone’ (score 0), ‘manages alone with difficulty’ (score 1), ‘cannot do alone’ (score 2). The scale consists of 14 items: having a bath or all-over wash, washing hands and face, putting on shoes and stockings/socks, doing up buttons and zips, dressing yourself other than the above, getting to and using the WC, getting in and out of bed, feeding self, shaving (men) or doing hair (women), cutting your own toenails, getting up and down steps, getting around the house, going out of doors alone and taking medicine.
* P≤0.05 but >0.01
** P≤0.01 but >0.001
*** P<0.001; P-values are for chi-squared test in the univariate analysis
provinces and that they have comparable levels of economic development and modernisation to other provinces in China, caution should be exercised in generalising our findings to all of China's 169 million older inhabitants.
Comparison of our findings with those from other studies
There is evidence that in high-incomes countries about 60% of community-dwelling older adults with dementia or depression are not diagnosed. Reference Worrall and Moulton8–Reference Collerton, Davies, Jagger, Kingston, Bond and Eccles10,Reference Eefsting, Boersma, Van den Brink and Van26,Reference Valcour, Masaki, Curb and Blanchette28 Our study in China, which has the largest number of patients with dementia in the world, Reference Ferri, Prince, Brayne, Brodaty, Fratiglioni and Ganguli29 shows that the level of undetected dementia was much higher than has been seen in the studies undertaken in high-income countries. Reference Worrall and Moulton8,Reference Collerton, Davies, Jagger, Kingston, Bond and Eccles10,Reference O'Connor, Pollitt, Hyde, Brook, Reiss and Roth11,Reference Eefsting, Boersma, Van den Brink and Van26,Reference Valcour, Masaki, Curb and Blanchette28 A small study of 23 patients with dementia in Thailand Reference Jitapunkul, Chansirikanjana and Thamarpirat30 found a similar high level of undetected dementia (95.6%) to that in our study. The low level of dementia detection in Chinese older adults could be as a result of low socioeconomic status or reflect aspects of Chinese culture and traditions.
Previous studies in high-income countries have shown that more than half of older adults with depression are not diagnosed. Reference Collerton, Davies, Jagger, Kingston, Bond and Eccles10,Reference Garrard, Rolnick, Nitz, Luepke, Jackson and Fischer27 The current study demonstrated an extremely high level of underdetected depression, although the total risk of depression in Chinese older adults is lower than that in high-income countries. Reference Chen, Hu, Qin, Xu and Copeland17,Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 This high level of underdetection could be as a result of Chinese cultural aspects, such as the stigma associated with depression. Taken together with the figures of high undetection of depression in other countries, our study suggests that depression in older populations is poorly recognised and requires attention.
There are few studies that have examined factors influencing non-detection of dementia and depression in older adults. In the current study we found that increased risk of having undetected dementia and depression was strongly associated with low socioeconomic variables. In rural China, the average annual income (US$140–340) is two to five times lower than that in urban areas (US$412–652) Reference Woo, Kwok, Sze and Yuan31 and about 90% of older people are illiterate. Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 People living in rural areas mostly have no medical insurance, unlike those in urban China who have medical coverage provided by the government or their employers. Reference Woo, Kwok, Sze and Yuan31 The primary care system in rural areas is mainly made up of clinics staffed by less intensively trained medical personnel. Both lack of healthcare and low educational level in rural settings may thus explain further the relatively low detection rates of dementia and depression associated with low socioeconomic status. Previous studies in high-income countries did not show a significant association between low socioeconomic status and the risk of undetected dementia. Reference Sternberg, Wolfson and Baumgarten13,Reference Valcour, Masaki, Curb and Blanchette28 This could be at least partially a result of their small samples, better access to healthcare in these countries, or both.
A reduced risk of having undiagnosed dementia in relation to severe functional impairments was observed in high-income countries, Reference Sternberg, Wolfson and Baumgarten13 consistent with our finding of an association of detecting dementia with difficulties in ADL. Increased contact with healthcare services because of these impairments may lead to the detection of cognitive difficulties. Our data further showed that understanding family histories of mental illness would increase the chance of dementia, and probably depression being detected, even after allowing for socioeconomic status.
In the USA, Garrard et al Reference Garrard, Rolnick, Nitz, Luepke, Jackson and Fischer27 observed that men were more likely than women to have undiagnosed depression. However, in the current study we found that women were more likely to have undetected depression. This is consistent with female gender being a risk factor for depression Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 and could be linked to women in China having lower socioeconomic status. The increased risk of undetected depression in those having more than three children may also be because of low socioeconomic status, as having more children is associated with lower levels of education, occupational class, income, and living in rural areas, reducing the chance of detecting depression. Having heart disease may increase the chance of a hospital admission and diagnosing depression, and thus not surprisingly, it was inversely related to undetected depression in the community in this study.
Previous studies in high-income countries showed no associations between undetected dementia and social support. Reference Sternberg, Wolfson and Baumgarten13,Reference Callahan, Hendrie and Tierney32 Surprisingly, we found that increased risk of having undiagnosed dementia was associated with ‘help available when needed’. Unlike in high-income countries, most of older Chinese people live with their families and have a high level of social network support. Reference Chen, Wei, Hu, Qin, Copeland and Hemingway18 Traditionally, families take care of their frail and sick elders and around 90% of patients with dementia are looked after by their family. Reference O'Connor, Pollitt, Hyde, Brook, Reiss and Roth11,Reference Chiu and Zhang33 High levels of social support may disguise the disease and hinder detection, suggesting that identification may be enhanced through targeted screening in these circumstances. In contrast, other aspects of social support, such as visiting children/relatives, reduced the risk of undetected depression, suggesting the protective effects of social support on depression for early detection.
A variety of reasons have been suggested to explain the poor detection of dementia and depression and lack of utilisation of health services, for example interpreting symptoms as an acceptable part of the ageing process rather than as an illness. Reference Arve, Lauri, Lehtonen and Tilvis9,Reference Valcour, Masaki, Curb and Blanchette28 Previous studies have shown that the stigma attached to mental illness, Reference Marwaha and Livingston34–Reference Cheng, Lam, Chan, Law, Fung and Chan36 disillusionment with doctors, perceived exclusion from services, a lack of knowledge about mental illness and services Reference La, Ahuja, Bradbury, Phillips and Oyebode37 and different illness models Reference Marwaha and Livingston34 may account for decreased use of services by older people with dementia and depression. Older Asian people living in the West have been found to be reluctant to accept referral to mental health services and are less likely to receive secondary care for dementia. Reference Shah, Lindesay and Jagger38,Reference Livingston, Leavey, Kitchen, Manela, Sembhi and Katona39 According to data from our Chinese study and worldwide literature, we projected that globally about 35 million cases of dementia and 21 million cases of later-life depression are undiagnosed, meaning that large numbers of people are not receiving the care and services that they need. Reference Ferri, Prince, Brayne, Brodaty, Fratiglioni and Ganguli29 This estimate should urge governments to tackle the problem of undetected dementia and late-life depression immediately. Through public campaigns and education against stigma and discrimination towards dementia and depression, there should be increased awareness, detection and treatment of dementia and depression in older adults.
Implications
In this multicentre, community-based household survey we observed that there are extremely high rates of undetected dementia and depression in older adults in China. To our knowledge the current study is the first to investigate factors influencing undetected dementia and later-life depression, suggesting that both are significantly associated with low socioeconomic status. Some aspects of Chinese culture and tradition may also be related to underdetection of dementia and depression. Our findings imply that reducing the gap between low and high levels of socioeconomic status would increase detection of dementia and depression in older adults. The current economic improvement throughout China could provide the context for mental health campaigns and related education should be offered to target high-risk groups of people, including their carers. Mental health services for older adults should be developed, and providing primary care workers with appropriate skills has much to recommend it. This should be supported by attitudinal changes in the general population and professionals so that those who are demonstrably ill are recognised as such, and can be provided with the support that they, and their carers, might need.
Funding
This study was funded by research grants from Alzheimer's Research UK (Grant No. ART/PPG2007B/2) and the BUPA Foundation (Grants Nos. 45NOV06, and TBF-M09-05), UK.
Acknowledgements
The authors thank the participants and all who were involved in the surveys in the four-province and Hubei studies and in the Anhui study. Professor Martin Prince, a principle investigator of the 10/66 dementia research at Institute of Psychiatry, King's College London, helped the study by providing the 10/66 dementia diagnostic algorithm. Ms Qi Wang helped with data analysis. With support from the Strategic Research Development Fund at the University of Wolverhampton, D.Z. visited the UK to carry out 1 year of postdoctoral research on the Dementia Project.






eLetters
No eLetters have been published for this article.