Early environmental stresses have been recognized as important contributors to affective relapse (Reference Bryer, Nelson and MillerBryer et al, 1987; Reference Brown and AndersonBrown & Anderson, 1991; Reference Heim and NemeroffHeim & Nemeroff, 2001). The literature on severe childhood abuse has described its impact on depression and borderline personality disorder (Reference Brown and AndersonBrown & Anderson, 1991; Reference TrullTrull, 2001), but less attention has been focused on bipolar disorder. Childhood abuse has broadly been associated with complex forms of adult psychopathological disorder, including suicidality (reviewed by Reference Santa Mina and GallopSanta Mina & Gallop, 1998), substance misuse and dependence (Reference Dube, Anda and FelittiDube et al, 2001) and psychosis (Reference Hammersley, Dias and ToddHammersley et al, 2003). However, possible differences among subtypes of childhood abuse relative to clinical outcomes have been less well studied. We therefore sought to identify components of severe childhood abuse in a large group of patients with well-characterised bipolar disorder. Following recent observations by Leverich et al (Reference Leverich, McElroy and Suppes2002, Reference Leverich, Altshuler and Frye2003), we predicted that patients with histories of abuse would demonstrate more substance misuse comorbidity, past-year rapid cycling and lifetime suicide attempts. We further predicted that coexistent multiple forms of abuse would be associated with poorer clinical outcomes, and that severe physical or sexual abuse would be more prevalent among women than men in our sample.
METHOD
Study sample
The study group comprised 100 patients with bipolar disorder (95 out-patients and 5 in-patients) who were consecutively evaluated in the Bipolar Disorders Research Clinic of the New York Presbyterian Hospital. All were diagnosed with bipolar type I (n=73) or type II (n=27) disorder by means of the Structured Clinical Interview for DSM-IV (SCID-IV; Reference First, Spitzer and GibbonFirst et al, 1995), conducted by one of the authors (J.L.G.). Participants were enrolled over a period of about a year in the context of seeking evaluation and treatment for any phase of bipolar illness through an academic specialty centre. Treatment was given independently of the study protocol.
Study procedures
After giving written informed consent, all participants underwent SCID-IV assessments. The presence of childhood abuse was rated using the Childhood Trauma Questionnaire (CTQ), a 28-item self-report measure developed by Bernstein et al (Reference Bernstein, Fink and Handelsman1994). Individual component measures of childhood sexual abuse, physical abuse, physical neglect, emotional abuse and emotional neglect have been derived from this instrument, further subdivided along a continuum of severity ranging from ‘none’ through ‘mild’ and ‘moderate’ to ‘severe’. Categorical distinctions between the presence or absence of ‘severe’ forms of childhood abuse were conservatively used for dichotomous analyses.
Clinical status at the time of study entry was evaluated by one of the authors (J.L.G.) using standardised symptom severity indices, including the 17-item Hamilton Rating Scale for Depression (HRSD; Reference HamiltonHamilton, 1960) and the Young Mania Rating Scale (YMRS; Reference Young, Biggs and ZieglerYoung et al, 1978). Ratings on the HRSD and YMRS were made for the week preceding the assessment, in order to provide an estimate of current affective symptoms. Past-year rapid cycling and lifetime substance misuse or dependence were rated from the SCID-IV. Lifetime suicide attempts were assessed by one of the authors (J.L.G.) using a semi-structured interview developed by our group and used previously (Reference Michaelis, Goldberg and SingerMichaelis et al, 2003). The study protocol was approved by the institutional review boards of both the New York Presbyterian Hospital and Long Island University.
Statistical analyses
Statistical analyses were conducted using the Statistical Package for the Social Sciences, SPSS PC (version 11.5). Numbers are expressed as means and standard deviations. Group mean differences between continuous variables were analysed by t-tests; dichotomous variables were analysed by chi-squared tests. Logistic regression analyses were used to assess the strength of association between one or more continuous interval variables and a dichotomous dependent variable, from which odds ratios, 95% confidence intervals and Wald χ2 statistics were generated. In order to correct for multiple comparisons, a Bonferroni-corrected α level of P<0.005 (0.05/10) was used for the ten independent variables examined in Table 1. Otherwise, an α level of 0.05 was used throughout. All statistical tests were two-tailed.
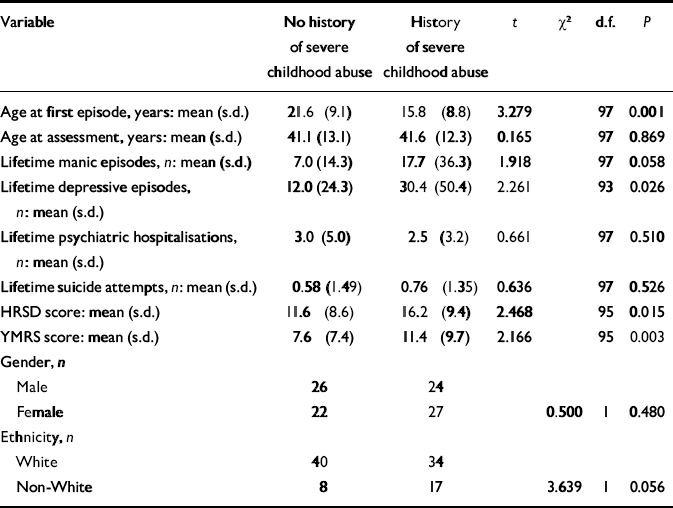
Table 1 Clinical features of patients with or without a history of severe childhood abuse
| Variable | No history of severe childhood abuse | History of severe childhood abuse | t | χ2 | d.f. | P |
|---|---|---|---|---|---|---|
| Age at first episode, years: mean (s.d.) | 21.6 (9.1) | 15.8 (8.8) | 3.279 | 97 | 0.001 | |
| Age at assessment, years: mean (s.d.) | 41.1 (13.1) | 41.6 (12.3) | 0.165 | 97 | 0.869 | |
| Lifetime manic episodes, n: mean (s.d.) | 7.0 (14.3) | 17.7 (36.3) | 1.918 | 97 | 0.058 | |
| Lifetime depressive episodes, n: mean (s.d.) | 12.0 (24.3) | 30.4 (50.4) | 2.261 | 93 | 0.026 | |
| Lifetime psychiatric hospitalisations, n: mean (s.d.) | 3.0 (5.0) | 2.5 (3.2) | 0.661 | 97 | 0.510 | |
| Lifetime suicide attempts, n: mean (s.d.) | 0.58 (1.49) | 0.76 (1.35) | 0.636 | 97 | 0.526 | |
| HRSD score: mean (s.d.) | 11.6 (8.6) | 16.2 (9.4) | 2.468 | 95 | 0.015 | |
| YMRS score: mean (s.d.) | 7.6 (7.4) | 11.4 (9.7) | 2.166 | 95 | 0.003 | |
| Gender, n | ||||||
| Male | 26 | 24 | ||||
| Female | 22 | 27 | 0.500 | 1 | 0.480 | |
| Ethnicity, n | ||||||
| White | 40 | 34 | ||||
| Non-White | 8 | 17 | 3.639 | 1 | 0.056 |
RESULTS
Complete CTQ data were available for 99 of the 100 study participants. Table 1 summarises the clinical and demographic features of the sample, categorised by the presence or absence of a history of any form of severe childhood abuse. For the total group the median age at first episode was 17.5 years, and only a small minority (16 of 99 patients; 16%) identified their first episode as occurring before age 10 years. Those who had a history of severe abuse had a significantly younger age at illness onset, as well as a higher severity level of current manic symptoms, than those without such a history. Near-significant relationships (after Bonferroni correction) were also observed between childhood abuse and current depressive symptoms severity as well as the mean lifetime number of depressive episodes.
Total HRSD and YMRS scores were independently assessed relative to a three-point minimisation/denial sub-scale of the CTQ, in order to estimate the extent to which participants might minimise or deny trauma histories relative to current affective symptoms. Modest but significant negative correlations were observed, suggesting that the denial or minimisation of trauma history items was negatively associated with levels of current depression (measured by HRSD scores; r=-0.259, P=0.011) or mania symptoms (measured by YMRS scores; r=-0.208, P=0.041).
No significant relationship was found between gender and overall severe childhood abuse histories, or abuse subtypes: emotional abuse (χ2=2.347, d.f.=1, P=0.126), emotional neglect (χ2=0.990, d.f.=1, P=0.320), physical abuse (χ2=0.003, d.f.=1, P=0.995), physical neglect (χ2=1.611, d.f.=1, P=0.204) or sexual abuse (χ2=0.624, d.f.=1, P=0.430).
Because type I and type II bipolar disorder may differ with regard to symptom intensity (Reference Vieta, Gastro and OteroVieta et al, 1997), we separately compared prevalence rates of severe childhood abuse subtypes between these two diagnostic groups. No significant difference was observed in any domains (childhood emotional abuse, χ2=0.018, d.f.=1, P=0.894; emotional neglect, χ2=0.026, d.f.=1, P=0.872; physical abuse, χ2=0.026, d.f.=1, P=0.872; physical neglect, χ2=0.011, d.f.=1, P=0.916; sexual abuse, χ2=0.716, d.f.=1, P=0.397) or in the mean total number of abuse subtypes for each of the two groups (t=0.466, d.f.=97, P=0.642). About half of the study group had experienced severe childhood abuse in at least one domain, most frequently emotional abuse. Within (non-mutually exclusive) subcategories of severe abuse, 37% reported emotional abuse, 24% physical abuse, 24% emotional neglect, 21% sexual abuse and 12% physical neglect. Two or more distinct forms of severe abuse were identified in 36 of the 99 participants (36%): of these, 16 had experienced two forms of severe abuse, an additional 10 three forms of severe abuse, 6 four forms of abuse and 4 all five forms of severe abuse. All the forms of abuse were significantly interrelated, with the strongest associations emerging between emotional abuse and physical abuse (r=0.74, P<0.001) and between emotional abuse and neglect (r=0.737, P<0.001).
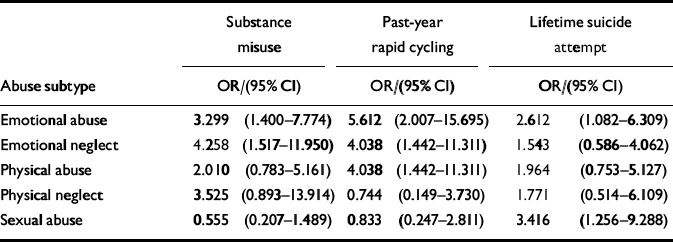
Table 2 presents individual odds ratios with corresponding 95% confidence intervals for each of the five abuse components relative to lifetime comorbid substance misuse or dependence, past-year rapid cycling and lifetime suicide attempts. These analyses indicated significant associations between comorbid substance misuse or dependence and severe emotional abuse or emotional neglect; past-year rapid cycling and severe emotional abuse, physical abuse or emotional neglect; and a lifetime suicide attempt with severe childhood emotional abuse or childhood sexual abuse. In light of previous research suggesting that suicide risk might be influenced by both sexual and physical abuse, we conducted an additional logistic regression analysis taking the presence or absence of lifetime suicide attempts as the dependent variable. A significant association was found with childhood sexual abuse (OR=3.327, 95% CI 1.027-10.412; Wald χ2=4.020, d.f.=1, P=0.045), but not with physical abuse (OR=1.163, 95% CI 0.340-3.975; Wald χ2=0.058, d.f.=1, P=0.810), physical neglect (OR=0.573, 95% CI 0.102-3.216; Wald χ2=0.401, d.f.=1, P=0.527), emotional abuse (OR=2.074 95% CI 0.626-6.876; Wald χ2=1.424, d.f.=1, P=0.233) or emotional neglect (OR=1.121, 95% CI 0.305-4.126; Wald χ2=0.030, d.f.=1, P=0.864).
Table 2 Individual odds ratios among severe childhood abuse subtypes and domains of adult outcome in bipolar disorder
| Substance misuse | Past-year rapid cycling | Lifetime suicide attempt | |
|---|---|---|---|
| Abuse subtype | OR/(95% CI) | OR/(95% CI) | OR/(95% CI) |
| Emotional abuse | 3.299 (1.400-7.774) | 5.612 (2.007-15.695) | 2.612 (1.082-6.309) |
| Emotional neglect | 4.258 (1.517-11.950) | 4.038 (1.442-11.311) | 1.543 (0.586-4.062) |
| Physical abuse | 2.010 (0.783-5.161) | 4.038 (1.442-11.311) | 1.964 (0.753-5.127) |
| Physical neglect | 3.525 (0.893-13.914) | 0.744 (0.149-3.730) | 1.771 (0.514-6.109) |
| Sexual abuse | 0.555 (0.207-1.489) | 0.833 (0.247-2.811) | 3.416 (1.256-9.288) |
Multiple forms of childhood abuse
To test the hypothesis that multiple forms of childhood abuse would be progressively associated with more complex forms of adult bipolar disorder, we undertook three separate logistic regression analyses to examine the number of forms of abuse (the independent variable) relative to the presence or absence of a lifetime suicide attempt; rapid cycling; and comorbid substance misuse or dependence (each as a respective dependent variable). Significant relationships were seen between an increasing number of childhood abuse forms and the presence of a lifetime suicide attempt (OR=1.466, 95% CI 1.095-1.964; Wald χ2=6.615, d.f.=1, P=0.010) and rapid cycling (OR=1.476, 95% CI 1.073-2.030; Wald χ2=5.730, d.f.=1, P=0.017). A marginally significant association was observed between the number of forms of abuse and the presence of comorbid substance misuse or dependence (OR=1.325, 95% CI 1.000-1.758; Wald χ2=3.809, d.f.=1, P=0.051).
DISCUSSION
Our results suggest that a history of severe childhood abuse is to be found in approximately half of adults with bipolar disorder, with multiple forms of having occurred in about a third. Distinct negative impacts on clinical outcome were associated with childhood physical, sexual or emotional abuse histories, with evidence suggesting more extensive suicidality, rapid cycling and possibly comorbid substance misuse associated with multiple forms of childhood abuse.
The observed prevalence of severe childhood abuse in about half of our adult patients with bipolar disorder is consistent with the 49% prevalence rate described within the Stanley Foundation Bipolar Network (Reference Leverich, McElroy and SuppesLeverich et al, 2002). These rates are only slightly higher than those previously reported from semi-structured interviews of patients with major depression (Reference Brodsky, Oquendo and EllisBrodsky et al, 2001) or community samples (Reference McHolm, MacMillan and JamiesonMcHolm et al, 2003), although lower rates (e.g. 20-30%) have been reported among general medical out-patients (Reference Dube, Anda and FelittiDube et al, 2001; Reference Edwards, Holden and FelittiEdwards et al, 2003). Also consistent with our findings are reports suggesting that multiple forms of childhood maltreatment often co-occur (Reference Cicchetti and RizleyCicchetti & Rizley, 1981) and may contribute additively or synergistically to more extensive psychopathology and suicidality seen in adulthood (Reference Dube, Anda and FelittiDube et al, 2001; Reference Read, Agar and Barker-ColloRead et al, 2001; Reference Edwards, Holden and FelittiEdwards et al, 2003).
Several factors could account for the high rates of childhood abuse among people with bipolar disorder. One issue involves intrinsic, developmental or familial factors that are especially deleterious for bipolar disorder, such as negative expressed emotion (Reference Miklowitz, Goldstein and NuechterleinMiklowitz et al, 1988). Factors that probably underlie the origins of childhood abuse are undoubtedly complex, although environments with high levels of expressed emotion could theoretically contribute to the potential for aggressive behaviours and verbal or emotional hostility. This may be an especially important consideration when prodromal features of severe psychopathological disorder become manifest in childhood, potentially evoking greater family distress (Reference Boye, Bentsen and UlsteinBoye et al, 2001). In addition, given the complex traits linked with the genetics of bipolar disorder (Reference Faraone and TsuangFaraone & Tsuang, 2003), it is also possible that aspects of parental psychopathology could represent a potential moderating factor in the expressivity of trait aggression in probands or parent-proband constellations.
Our study recruited people with bipolar disorder seeking treatment from an academic specialty centre, in contrast to those in the general population not seeking treatment, or those seen in more community-based treatment centres. In addition, earlier studies have suggested that patients more typically underreport abuse histories during clinical interviews as compared with self-report surveys (Reference Dill, Chu and GrobDill et al, 1991). The validity and reliability with which adult patients with bipolar disorder report histories of childhood abuse may also vary, given the known links between bipolar disorder and poor insight (Reference Ghaemi, Boiman and GoodwinGhaemi et al, 2000).
The relationship between affective symptoms and recall of childhood trauma also warrants discussion. Given recent concerns about the potential for patients to report factually inaccurate repressed memories of sexual abuse ‘recovered’ during psychotherapy (Reference BoakesBoakes, 1995; Royal College of Psychiatrists, 1997), caution is warranted in interpreting the validity of self-reported trauma. On the other hand, Goodman et al (Reference Goodman, Thompson and Weinfurt1999) observed good reliability in the longitudinal assessment of trauma histories among psychiatrically ill women.
In our study significant or near-significant associations were observed between current affective symptoms and self-reported childhood abuse. It is possible that the presence of current affective symptoms could influence the recall of adverse childhood experiences, as might be further suggested from the lack of denial or minimisation associated with either manic or depressive symptom severity. Indeed, the limitation posed by current depressive symptoms influencing retrospective recall has been noted previously in the trauma literature, in light of the high prevalence of persistent depressive symptoms among trauma survivors (Reference Bernet and SteinBernet & Stein, 1999). Moreover, attempts to obtain corroboration of retrospectively recalled childhood trauma histories in adult populations pose obvious impracticalities. This limitation of the current findings pertains to most (if not all) existing studies of bipolar disorder patient populations.
Although most other studies have subsumed physical, sexual and other forms of childhood abuse under one rubric, our study points to differences across abuse subtypes relative to illness complexity and course in bipolar disorder. The observed connection between suicidality and sexual (but not emotional or physical) abuse is consistent with prior observations in patients with this disorder (Reference Leverich, Altshuler and FryeLeverich et al, 2003). In addition, Brown et al (Reference Brown, Cohen and Johnson1999) found in a non-clinical sample of young adults that childhood sexual abuse conferred more than 8 times greater risk of repeated suicide attempts, whereas childhood neglect apparently had no moderating role. Physical abuse has previously been identified in connection with suicidal behaviour among psychiatric patients (Reference Silverman, Reinherz and GiaconiaSilverman et al, 1996), although existing studies have not systematically controlled for the potential overriding effects of sexual abuse relative to suicidal behaviour.
In our study the lack of an observed relationship between sexual, emotional or physical abuse and gender was surprising and contrary to previous findings in broad community-based samples (Reference Levitan, Parikh and LesageLevitan et al, 1998; Reference MacMillan, Fleming and StreinerMacMillan et al, 2001; Reference Edwards, Holden and FelittiEdwards et al, 2003) or clinical populations (Reference Gladstone, Parker and WilhelmGladstone et al, 1999). Data from the Stanley Foundation Bipolar Network similarly indicate no significant gender difference with regard to childhood physical abuse, although women were more likely than men to report childhood sexual abuse. Many - if not most - existing studies of childhood abuse in general focus on female samples, although a smaller body of research suggests that sexual and other forms of abuse may be more prevalent than many clinicians realise among male psychiatric outpatients (Reference Swett, Surrey and CohenSwett et al, 1990). Further studies are needed to clarify potential gender differences across childhood abuse subtypes in patients with bipolar disorder relative to other diagnostic groups.
The generalisability of our findings is limited to adult patients seen in an academic specialty centre for the treatment of bipolar illness; all the participants were evaluated in a dedicated research clinic, where diagnoses were established by standardised interviews conducted by trained and reliable raters. Although the diagnostic reliability of bipolar disorder (particularly bipolar II disorder) has been demonstrated when interviews are conducted by experienced clinicians (Reference Simpson, McMahon and McInnisSimpson et al, 2002), the same has not yet been demonstrated in general community samples, and remains a source of debate. Hence, replication of our findings in community-based treatment centres would help to establish the representativeness of the study results to the broader community of adults identified as having bipolar disorder.
The study data have a number of both clinical and theoretical implications. First, in light of the strikingly high prevalence of childhood abuse in our sample, coupled with its potential moderating role in suicide risk, it would seem prudent for clinicians to routinely evaluate histories of childhood trauma in patients with bipolar disorder. This point is underscored by similar observations by Read et al (Reference Read, Agar and Barker-Collo2001). In particular, because multiple forms of abuse during childhood appear to heighten the risk of suicide attempts in a graded fashion, consideration of the nature and extent of abuse may bear directly on gauging the risk of suicide attempts in patients with bipolar disorder, consonant with findings reported elsewhere (Reference Dube, Anda and FelittiDube et al, 2001; Reference Edwards, Holden and FelittiEdwards et al, 2003). The findings also suggest that the nature and extent of childhood abuse among men with this disorder may be higher and more comparable to that seen in women than has previously been identified. From a theoretical as well as a clinical standpoint, the nature, extent and magnitude of childhood abuse - particularly sexual and emotional abuse - have been hypothesised to contribute to cycle acceleration and illness complexity through mechanisms related to behavioural sensitisation (Reference Leverich, McElroy and SuppesLeverich et al, 2002). Although our findings are consistent with that model, additional preclinical evidence is required, to address this process more directly. Further investigations using prospective longitudinal designs are needed to affirm and extend these initial observations.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Self-reported severe childhood abuse may be evident in about half of adults with bipolar disorder and warrants routine clinical assessment.
-
▪ Childhood sexual abuse may increase the risk of suicide attempts in adults with bipolar disorder, warranting its assessment in routine screening for suicide risk factors.
-
▪ Multiple forms of severe childhood abuse may be associated with a progressive risk for suicide attempts and the development of rapid cycling in adult bipolar patients.
LIMITATIONS
-
▪ The retrospective recall of traumatic childhood events in this protocol requires replication using prospective, longitudinal assessments of children at risk of developing bipolar disorder.
-
▪ The presence of sub-threshold affective symptoms might have influenced patients' recall of past traumatic experiences.
-
▪ Because our sample was exclusively drawn from patients seen in a specialist centre, the generalisability of our results is limited.
Acknowledgements
The study was supported in part by NIMH K-23 Career Development Award. MH-01936 (J.F.G.), a NARSAD Young Investigator Award (J.F.G.) and by grants. from the American Foundation for Suicide Prevention (J.F.G.) and the Nancy. Pritzker Foundation (J.F.G.).





eLetters
No eLetters have been published for this article.