Up to a third of hospital consultants are estimated to experience psychiatric morbidity at any one time (Reference Graham and RamirezGraham & Ramirez, 1997; Reference Taylor, Graham and PottsTaylor et al, 2005). Poor mental health is clearly detrimental to doctors' lives, but less is known about the extent of its impact upon patient care. Harmful alcohol consumption, impaired clinical performance and planned early retirement detract from patient care. We have estimated the prevalence of these behaviours, identified demographic risk factors and explored the relationship between these behaviours and poor mental health.
METHOD
A confidential postal survey was sent to 1794 UK NHS hospital consultants in late 2002. The sample included all surgical oncologists, medical oncologists and clinical oncologists, a random sample of gastroenterologists (two in three) and a random sample of radiologists (one in five). Consultants were ascertained through the UK medical Royal Colleges and professional bodies to which they were affiliated. Sampling and ascertainment are described in detail elsewhere (Reference Taylor, Graham and PottsTaylor et al, 2005). Psychiatric morbidity was estimated using the General Health Questionnaire–12 (GHQ–12; Reference Goldberg and WilliamsGoldberg & Williams, 1988). Harmful alcohol consumption was screened using the World Health Organization's Alcohol Use Disorders Identification Test (AUDIT; Reference Saunders, Aasland and BaborSaunders et al, 1993). Impaired clinical performance was measured using a scale adapted from Firth-Cozens et al (1997), whereby the frequency that stress at work had caused irritability with colleagues, irritability with patients and reduction in standards of care (such as taking short cuts) was rated on four-point scale from ‘never to my knowledge’ to ‘at least weekly’. Early retirement was defined as intending to retire aged ≤55 years. Demographic measures included gender, age and marital status. Hierarchical logistic regression models were developed. Each univariately significant demographic variable was entered into a multivariate model (model 1) followed by the additional impact, if any, of poor mental health (GHQ score ≥4; model 2). Analysis of relationships with planned early retirement necessarily excluded consultants aged over 55. Individuals with missing data were excluded on a test-by-test basis. Missing data constituted less than 5% except AUDIT scores (9%) and intended retirement age (7%). All tests were two-tailed, using a 5% significance level, and all analysis was conducted using SPSS v.12.0.1 for Windows.
RESULTS
Questionnaires were returned by 1308 consultants (73%), of whom 19% (251) were women, 89% (1151) were married or cohabiting, 4% (52) were aged < 35 years, 41% (534) were aged 36–45, 36% (473) were aged 46–55 and 19% (242) aged > 55 years (Table DS1 in the data supplement to the online version of this paper).
In all, 32% of consultants (414) were estimated to have psychiatric morbidity (Table DS1 in the data supplement); 17% of consultants (207) reported consuming hazardous quantities of alcohol; 33% (432) reported that, at least monthly in the last 6 months, stress at work had caused them to be irritable with colleagues; 16% (212) reported being irritable with patients; 17% (221) had reduced their standards of care through, for example, taking short cuts or not following procedures; and 18% (176) planned to retire early.
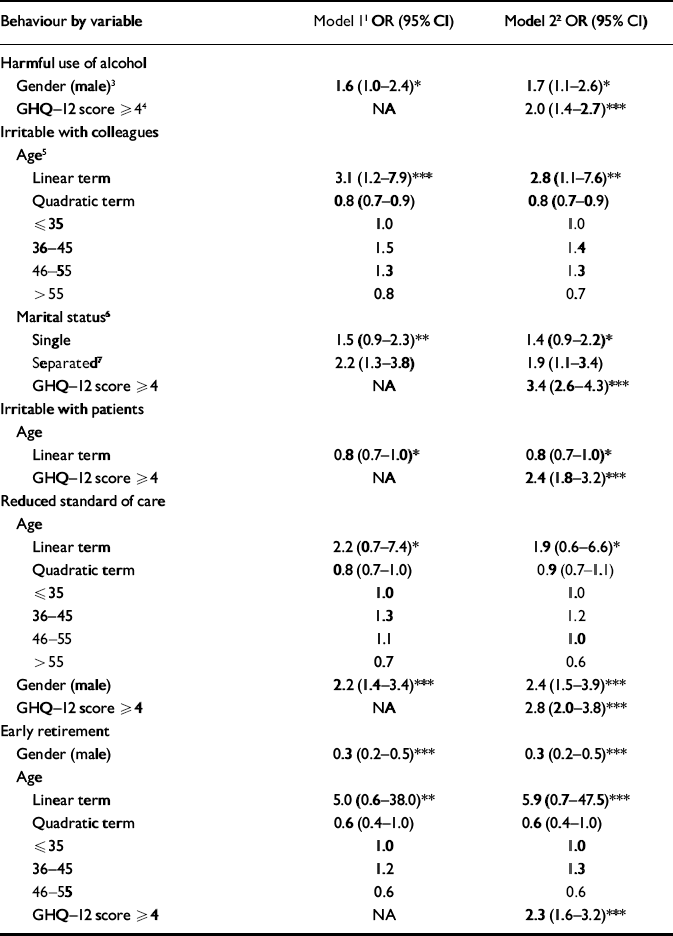
Male consultants were more likely to report harmful consumption of alcohol; consultants aged between 36 and 45 years (mid-aged) and those who were unmarried were more likely to report being irritable with colleagues; younger consultants were more likely to report being irritable with patients; male consultants and mid-aged consultants were more likely to report reducing their standards of care; and female consultants and mid-aged consultants were more likely to intend to retire early (Table 1: model 1). Poor mental health independently increased consultants' likelihood of reporting all of these behaviours (Table 1: model 2).
Table 1 Predictors of harmful alcohol use (score ≥8 for men, ≥7 for women on the Alcohol Use Disorders Identification Test), impaired performance at work (being irritable with colleagues or with patients, or reducing standards of care, at least monthly in the past 6 months) and intention to retire early (aged ≤55 years): logistic regression
| Behaviour by variable | Model 1 1 OR (95% CI) | Model 2 2 OR (95% CI) |
|---|---|---|
| Harmful use of alcohol | ||
| Gender (male) 3 | 1.6 (1.0–2.4) * | 1.7 (1.1–2.6) * |
| GHQ–12 score ≥4 4 | NA | 2.0 (1.4–2.7) *** |
| Irritable with colleagues | ||
| Age 5 | ||
| Linear term | 3.1 (1.2–7.9) *** | 2.8 (1.1–7.6) ** |
| Quadratic term | 0.8 (0.7–0.9) | 0.8 (0.7–0.9) |
| ≤35 | 1.0 | 1.0 |
| 36–45 | 1.5 | 1.4 |
| 46–55 | 1.3 | 1.3 |
| > 55 | 0.8 | 0.7 |
| Marital status 6 | ||
| Single | 1.5 (0.9–2.3) ** | 1.4 (0.9–2.2) * |
| Separated7 | 2.2 (1.3–3.8) | 1.9 (1.1–3.4) |
| GHQ–12 score ≥ 4 | NA | 3.4 (2.6–4.3) *** |
| Irritable with patients | ||
| Age | ||
| Linear term | 0.8 (0.7–1.0) * | 0.8 (0.7–1.0) * |
| GHQ–12 score ≥ 4 | NA | 2.4 (1.8–3.2) *** |
| Reduced standard of care | ||
| Age | ||
| Linear term | 2.2 (0.7–7.4) * | 1.9 (0.6–6.6) * |
| Quadratic term | 0.8 (0.7–1.0) | 0.9 (0.7–1.1) |
| ≤ 35 | 1.0 | 1.0 |
| 36–45 | 1.3 | 1.2 |
| 46–55 | 1.1 | 1.0 |
| > 55 | 0.7 | 0.6 |
| Gender (male) | 2.2 (1.4–3.4) *** | 2.4 (1.5–3.9) *** |
| GHQ–12 score ≥ 4 | NA | 2.8 (2.0–3.8) *** |
| Early retirement | ||
| Gender (male) | 0.3 (0.2–0.5) *** | 0.3 (0.2–0.5) *** |
| Age | ||
| Linear term | 5.0 (0.6–38.0) ** | 5.9 (0.7–47.5) *** |
| Quadratic term | 0.6 (0.4–1.0) | 0.6 (0.4–1.0) |
| ≤ 35 | 1.0 | 1.0 |
| 36–45 | 1.2 | 1.3 |
| 46–55 | 0.6 | 0.6 |
| GHQ–12 score ≥ 4 | NA | 2.3 (1.6–3.2) *** |
NA, not applicable
* P < 0.05
** P < 0.01
*** P < 0.001
1. Model 1: demographic predictors only
2. Model 2: impact of psychiatric morbidity, assessed as General Health Questionnaire (GHQ–12) score ≥4
3. Female consultants were the reference category for gender
4. GHQ–12 score < 4 was the reference category for GHQ–12
5. Effect of age modelled using a quadratic function to describe an inverse-U-shaped relationship. Resultant odds ratios for each age category are also given, using < 35 as the reference
6. Married/cohabiting consultants were the reference category for marital status
DISCUSSION
These findings suggest that hospital consultants with poor mental health are substantially more likely to report harmful consumption of alcohol, being irritable with patients, being irritable with colleagues, reducing their standards of care at work and/or planning to retire early. In addition, we have shown that male and mid-aged consultants are particularly at risk.
Our study included a large national cohort of consultants from five specialties. Despite the sensitive nature of the survey questions, the response rate was high, giving us confidence that the sample is representative. The cross-sectional design limits interpretation of causality, and assessments of mental health and consultant behaviours relied upon self-report measures. However, both the GHQ–12 and the AUDIT have been shown to be reliable and valid screening tools.
To our knowledge, this is the first study to examine the relationship between the mental health of hospital consultants and behaviours that detract from patient care.
Our finding that male consultants were more at risk of harmful alcohol consumption is consistent with findings from general population surveys. Perhaps more surprising is the increased risk of impaired clinical performance and planned early retirement at mid-age. Consultants appear to be particularly vulnerable at this phase in their career (e.g. Reference Spickard, Gabbe and ChristensenSpickard et al, 2002), which may be due to the fact that the honeymoon period of achieving consultant status is over but retirement is far from sight. They will have accumulated all of the responsibility and associated pressures, and are also more likely to have high demands on their time from home, with many having young families.
This study adds to the growing literature which highlights the critical importance to patients, as well as to doctors, of identifying approaches that protect consultants' mental health and support them to practice medicine safely throughout their careers.
Acknowledgements
We thank the consultants who took part in the survey, Royal Colleges of Physicians and Radiologists, British Society for Gastroenterology and British Association of Surgical Oncologists for their support.
This study was jointly funded by the Charitable Foundation of Guy's and St Thomas' Hospitals (London, UK) and Cancer Research UK.




eLetters
No eLetters have been published for this article.