The past 20 years have seen much epidemiological research into depression and schizophrenia, but little such research into bipolar affective disorder (Reference GoodwinGoodwin, 2000). Furthermore, the few published studies have shown wide variations, ranging from 2.6 to 20.0 per 100 000 per year, in the incidence of bipolar affective disorder (Reference Lloyd and JonesLloyd & Jones, 2002). This variation may be due in part to methodological differences and to difficulties in studying a relatively rare condition that has a complex definition.
There is evidence to suggest that the incidence of bipolar affective disorder, like that of schizophrenia, may be greater in minority ethnic populations (Reference Leff, Fischer and BertelsenLeff et al, 1976; Reference Der and BebbingtonDer & Bebbington, 1987; Reference Van Os, Castle and TakeiVan Os et al, 1996). With the exception of the study by Leff et al (Reference Leff, Fischer and Bertelsen1976), that had a prospective arm, the cited studies had a predominantly retrospective case-note design, which relied upon information and classification recorded by the psychiatrist at initial contact. Defining and estimating the population at risk was also problematic in the majority of these studies, as before 1991 there was no nationally collected data source that estimated the African-Caribbean population. Therefore previous reported differences could have been due to bias in case definition and ascertainment, or errors in estimation of the population at risk.
In this study we used a prospective approach within well-defined catchment areas using operationalised diagnostic criteria to calculate the incidence of operationally defined bipolar affective disorder in three UK areas. We intended to investigate the relative occurrence of the disorder in men and women, and to compare the incidence in different ethnic groups, taking into account the age structure of these populations.
METHOD
The study Aetiology and Ethnicity of Schizophrenia and Other Psychoses (ÆSOP) is an epidemiological, case-control study investigating the causes of high rates of psychosis, including non-psychotic mania, in certain minority ethnic populations in the UK. Ethical approval for the ÆSOP study was obtained from the Nottingham, London and Bristol hospital local research ethics committees. As part of the ÆSOP study, we identified everyone aged 16-64 years living in Nottingham, south-east London or Bristol who made contact with mental health services because of a first episode of probable psychosis, non-psychotic mania or bipolar affective disorder. The search was deliberately broad to allow identification of all incident cases, and took place over 24 months in Nottingham and south-east London (September 1997 to August 1999) and the first nine months of this period in Bristol. Methods were based upon those used by the World Health Organization (WHO) Ten Country Study (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992) and investigations in our centres (Reference Leff, Fischer and BertelsenLeff et al, 1976; Reference Brewin, Cantwell and DalkinBrewin et al, 1997; Reference Harrison, Glazebrook and BrewinHarrison et al, 1997).
Population at risk
People aged 16-64 years were eligible if they lived in the geographical areas comprising the city of Nottingham, Lambeth and the southern two-thirds of Southwark in south-east London, and central Bristol. The sizes of the populations at risk were estimated from the 2001 census (National Statistics, 2002), which included raw data for ethnic minority groups. In the previous 1991 census (Office of Population Censuses and Surveys, 1992), there were significant albeit well-characterised problems in these data regarding the under-enumeration of young adults, particularly men, from some minority ethnic groups. The 2001 census has attempted to account for this under-enumeration in its ‘one number census’ protocol (Reference PereiraPereira, 2002), thereby negating the need for adjustment of the census data using under-enumeration correction figures.
Case ascertainment and assessment
We screened all those who presented for the first time to any psychiatric service (including adult community mental health teams, in-patient units, forensic services, learning disability services, adolescent mental health services and drug and alcohol units) because of psychotic phenomena, including those with possible negative syndrome schizophrenia and non-psychotic mania.
The ÆSOP study team regularly contacted all service bases that would have received primary care or other referrals to identify eligible participants, and reviewed all admissions with appropriate staff. Furthermore, a ‘leakage’ study based upon the methods used by Cooper et al (Reference Cooper, Goodhead and Craig1987) was undertaken after the survey period closed in order to maximise the proportion of true cases included. All relevant mental health information systems were interrogated in order to identify people with a psychotic diagnosis or non-psychotic mania, including drug-induced psychosis or schizotypal, schizoid or paranoid personality disorder. In addition, staff were provided with a list of cases from their area and asked to recall any patients not included. The charts of all potential participants thus identified in Nottingham and south-east London were scrutinised and everyone eligible for referral during the study was identified and asked if they would take part. In Bristol, ethical approval was not obtained for this aspect of the study, so the leakage study was not carried out there. An over-inclusive psychosis screening instrument (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992) was used to screen all the individuals identified in this case ascertainment procedure and identify those who were experiencing delusions, hallucinations, thought disorder, negative features of schizophrenia or features of the manic syndrome. Those who were experiencing any of these, regardless of putative cause, were included as cases in our study.
People who gave informed consent, including those identified in the leakage study, underwent extensive assessment using standardised instruments. These included the Schedule for Clinical Assessment in Neuropsychiatry (SCAN; World Health Organization, 1992), the Schedule for Assessment of Negative Symptoms (SANS; Reference AndreasenAndreasen, 1982), a modified Personal and Psychiatric History Schedule (PPHS; World Health Organization, 1992), which included collateral information from a relative or carer and a schedule developed for the study for the recording of socio-demographic data. In south-east London and Nottingham, if patients declined to be interviewed the SCAN interview was replaced with the accompanying Item Group Checklist (World Health Organization, 1992), based on material in the case notes and information from clinical staff. There was no ethnic group difference in the proportions of those who declined to be interviewed. In Bristol it was not possible to study detailed information in the case notes of patients who declined to take part in the study, owing to restrictions imposed by the local ethics committee. In these cases a member of the ÆSOP study team established broad diagnoses (no psychosis; non-affective psychosis; mania; psychotic depression) following discussion with the treating clinician at first contact.
Consensus diagnoses were made for each case by a group of clinicians from multicultural backgrounds, with experience in cross-cultural diagnoses, who were involved in the study. This included the researcher who conducted the original individual assessments. Clinical information was presented by the researcher to the diagnostic panel masked to the ethnicity of the patient concerned. Diagnostic codes were assigned in each case according to ICD-10 (World Health Organization, 1993) using all other information from the case notes, item ratings in SCAN and collateral histories.
Reliability of the diagnostic process
Reliability studies were conducted across all three centres for consensus diagnoses. The principal investigators in each centre produced independent ratings on 20 cases, which were chosen at random from the entire sample. Interrater reliability was established between raters, which gave kappa scores ranging from 0.6 to 0.8. Pre-study reliability was established for the SCAN interview, which involved the independent rating of videotaped patient interviews by all relevant researchers, who were trained in Nottingham as part of a World Health Organization-approved course.
Case definition and ethnicity categorisation in the numerator
Individuals who received a consensus ICD-10 diagnosis of manic episode with (F30.2) or without (F30.1) psychotic symptoms, including those who had experienced a previous non-psychotic depressive episode (F31.1, F31.2, F31.6), were defined as cases and ascribed a diagnosis of bipolar affective disorder for the purposes of this study. Participants were categorised into ethnic groupings according to a six-category classification of ethnicity (White; mixed; Asian; African-Caribbean and Black, any other background; Black African; any other), modified from the Office for National Statistics 11-category classification (National Statistics, 2003). The ‘mixed’ group is a new ethnic category introduced in the 2001 census that includes all individuals of mixed heritage. People of Indian, Pakistani and Bangladeshi descent were grouped together in the ‘Asian’ category, and similarly, people classified as Black, any other background were grouped with African-Caribbean individuals. We merged these groups for clarity of presentation, because their individual incidence rates were similar and to maximise our statistical power, although we acknowledge that they retain distinct cultural identities. Self-ascribed ethnic identity was collected within the socio-demographic interview and overrode all other data sources. Where this was not available, when the person had declined to be interviewed, other sources were used. The most useful was self-ascribed ethnicity collected clinically for the purpose of clinical care and management returns. Other sources were observer-rated ethnicity, place of birth and place of parents' birth; where there was ambiguity, a consensus rating was made by members of the ÆSOP study team. These methods have been previously used in epidemiological studies of psychosis, where they have been described in more detail (Reference Jablensky, Sartorius and ErnbergJablensky et al, 1992; Reference Cooper, Goodhead and CraigCooper et al, 1987; Reference Brewin, Cantwell and DalkinBrewin et al, 1997; Reference Harrison, Glazebrook and BrewinHarrison et al, 1997).
Population at risk
Estimates of the populations at risk were derived using the 2001 census of Great Britain, which included raw data for minority ethnic groups (National Statistics, 2002). People aged 16-64 years who were resident in one of the 32 Census Area Statistic wards comprising Lambeth and two-thirds of Southwark in south-east London, the 95 wards of the city of Nottingham, and 52 wards in central Bristol at the time of the census (29 April 2001) were included in the population at risk for the purposes of our analysis. Census Area Statistic wards were introduced in 1998 by the British government to supersede electoral wards for census enumeration.
The population figures were adjusted according to the length of the study period in each centre in order to obtain an appropriate denominator. Thus, the census population was doubled in south-east London and Nottingham (24-month study period), whereas in Bristol, where cases were recruited over a 9-month period, the census population was multiplied by 0.75.
Statistical analysis
Incidence rates for bipolar affective disorder were calculated, standardised for age and gender and stratified by gender and ethnicity across the three centres. The rates were adjusted for age and gender using the indirect method of standardisation (ISTDIZE; Reference StataStata, 2003) to the 2001 population of England and Wales. This is the preferred method of standardisation when rates are based upon small numbers in certain strata (Reference Breslow and DayBreslow & Day, 1987). Age was coded into five strata (16-19, 20-29, 30-39, 40-49 and 50-64 years), and two separate definitions of ethnicity were considered: White v. Black and minority ethnic groups, as adopted by the National Institute for Mental Health in England (2003), and the six-category classification of ethnicity described above.
RESULTS
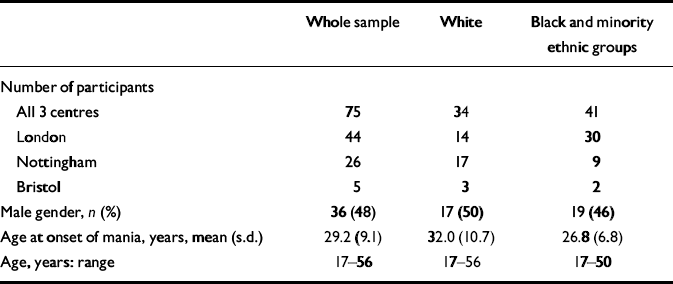
The calculated total population at risk (aged 16-64 years) was 1 631 462. In the combined south-east London, Nottingham and Bristol samples, 75 persons met ICD-10 criteria for their first episode of either mania with (F30.2) or without (F30.1) psychotic symptoms or bipolar affective disorder (F31). Although 11 people in Bristol passed the psychosis screen but refused to take part in the study, discussions with the treating clinician at first contact established that none of them had a diagnosis of bipolar affective disorder and thus they were not included in the analysis. Thirty-nine (52%) were women and 36 (48%) men. Twenty-five individuals (33%) out of the 75 had experienced a previous treated or untreated depressive episode, 3 (4%) had first-episode mania without psychotic symptoms and 47 (63%) had a diagnosis of first-episode mania with psychotic symptoms. Socio-demographic variables in White and Black and minority ethnic participants are shown in Table 1.
Table 1 Socio-demographic variables of the study sample: White and Black and minority ethnic groups
| Whole sample | White | Black and minority ethnic groups | |
|---|---|---|---|
| Number of participants | |||
| All 3 centres | 75 | 34 | 41 |
| London | 44 | 14 | 30 |
| Nottingham | 26 | 17 | 9 |
| Bristol | 5 | 3 | 2 |
| Male gender, n (%) | 36(48) | 17(50) | 19(46) |
| Age at onset of mania, years, mean (s.d.) | 29.2(9.1) | 32.0 (10.7) | 26.8 (6.8) |
| Age, years: range | 17-56 | 17-56 | 17-50 |
Incidence rates and rate ratios
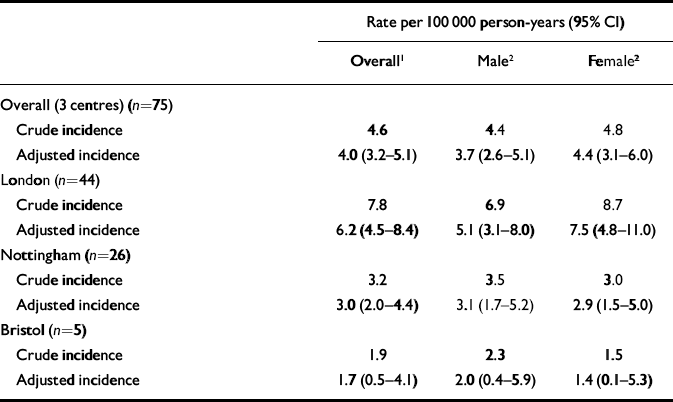
The standardised incidence rates for bipolar affective disorder in the south-east London, Nottingham and Bristol samples are given in Table 2. The age-standardised incidence rate of bipolar affective disorder in south-east London (6.2; 4.5-8.4) was more than double the rate in Nottingham (3.0, 95% CI 2.0-4.4) and Bristol (1.7, 95% CI 0.5-4.1). Overall, there was no significant difference in the incidence rate of the disorder between men and women (0.99, 95% CI 0.63-1.56), a consistent effect in each area.
Table 2 Incidence of bipolar affective disorder: rates by gender and centre1
| Rate per 100 000 person-years (95% CI) | |||
|---|---|---|---|
| Overall1 | Male2 | Female2 | |
| Overall (3 centres) (n=75) | |||
| Crude incidence | 4.6 | 4.4 | 4.8 |
| Adjusted incidence | 4.0 (3.2-5.1) | 3.7 (2.6-5.1) | 4.4 (3.1-6.0) |
| London (n=44) | |||
| Crude incidence | 7.8 | 6.9 | 8.7 |
| Adjusted incidence | 6.2(4.5-8.4) | 5.1 (3.1-8.0) | 7.5 (4.8-11.0) |
| Nottingham (n=26) | |||
| Crude incidence | 3.2 | 3.5 | 3.0 |
| Adjusted incidence | 3.0 (2.0-4.4) | 3.1 (1.7-5.2) | 2.9 (1.5-5.0) |
| Bristol (n=5) | |||
| Crude incidence | 1.9 | 2.3 | 1.5 |
| Adjusted incidence | 1.7 (0.5-4.1) | 2.0 (0.4-5.9) | 1.4 (0.1-5.3) |
The incidence rate for the combined Black and minority ethnic group (12.3, 95% CI 8.3-17.6) was significantly higher than that in the White group (2.3, 95% CI 1.6-3.2). African-Caribbean (18.2, 95% CI 10.8-28.8), Black African (11.9, 95% CI 5.9-21.3) and mixed ethnicity groups had particularly high overall incidence rates of bipolar affective disorder (12.7, 95% CI 4.6-27.8) compared with the White group (2.3, 95% CI 1.6-3.2).
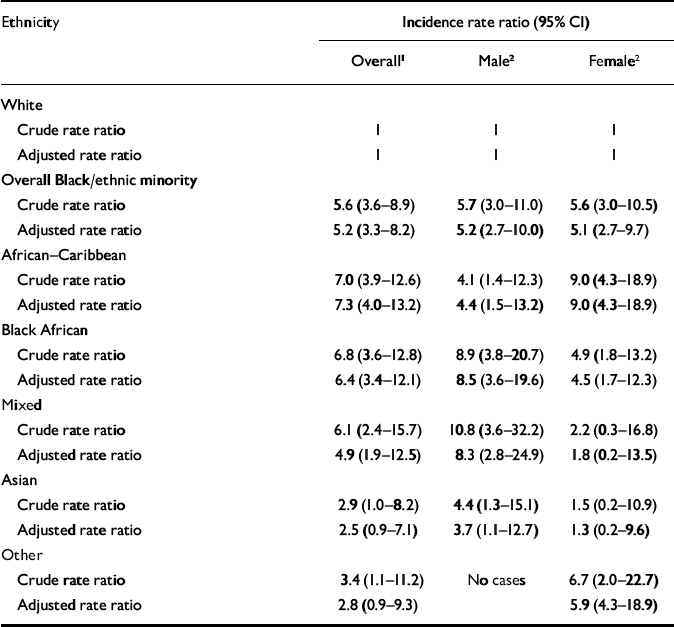
The corresponding rate ratios for the overall sample with 95% confidence intervals are given in Table 3. The incidence rate ratios were elevated in all the ethnic minority groups compared with the White group, but particularly so in the African-Caribbean (7.3, 95% CI 4.0-13.2), Black African (6.4, 95% CI 3.4-12.1) and mixed ethnicity (4.9, 95% CI 1.9-12.5) groups.
Table 3 Incidence rate ratios by ethnicity
| Ethnicity | Incidence rate ratio (95% CI) | ||
|---|---|---|---|
| Overall1 | Male2 | Female2 | |
| White | |||
| Crude rate ratio | 1 | 1 | 1 |
| Adjusted rate ratio | 1 | 1 | 1 |
| Overall Black/ethnic minority | |||
| Crude rate ratio | 5.6 (3.6-8.9) | 5.7 (3.0-11.0) | 5.6 (3.0-10.5) |
| Adjusted rate ratio | 5.2 (3.3-8.2) | 5.2 (2.7-10.0) | 5.1 (2.7-9.7) |
| African-Caribbean | |||
| Crude rate ratio | 7.0 (3.9-12.6) | 4.1 (1.4-12.3) | 9.0 (4.3-18.9) |
| Adjusted rate ratio | 7.3 (4.0-13.2) | 4.4 (1.5-13.2) | 9.0 (4.3-18.9) |
| Black African | |||
| Crude rate ratio | 6.8 (3.6-12.8) | 8.9 (3.8-20.7) | 4.9 (1.8-13.2) |
| Adjusted rate ratio | 6.4 (3.4-12.1) | 8.5 (3.6-19.6) | 4.5 (1.7-12.3) |
| Mixed | |||
| Crude rate ratio | 6.1 (2.4-15.7) | 10.8 (3.6-32.2) | 2.2 (0.3-16.8) |
| Adjusted rate ratio | 4.9 (1.9-12.5) | 8.3 (2.8-24.9) | 1.8 (0.2-13.5) |
| Asian | |||
| Crude rate ratio | 2.9 (1.0-8.2) | 4.4 (1.3-15.1) | 1.5 (0.2-10.9) |
| Adjusted rate ratio | 2.5 (0.9-7.1) | 3.7 (1.1-12.7) | 1.3 (0.2-9.6) |
| Other | |||
| Crude rate ratio | 3.4 (1.1-11.2) | No cases | 6.7 (2.0-22.7) |
| Adjusted rate ratio | 2.8 (0.9-9.3) | 5.9 (4.3-18.9) | |
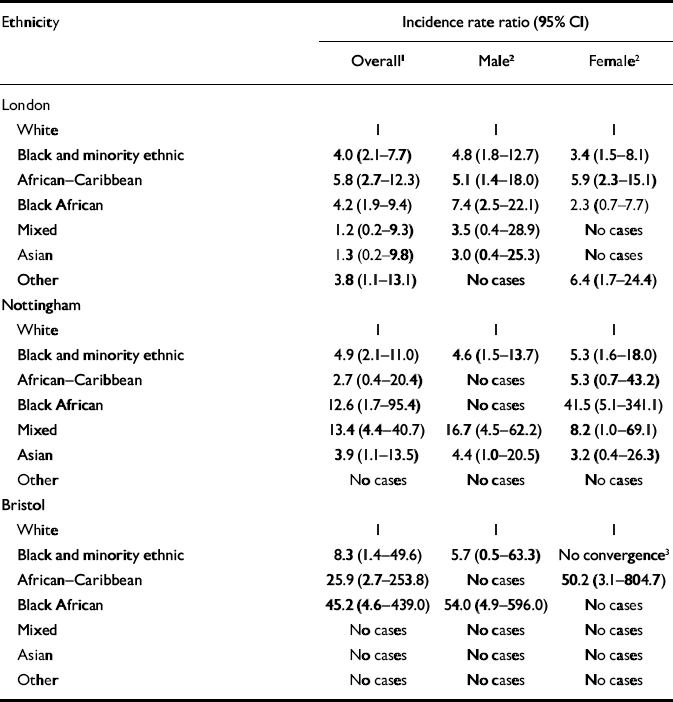
Table 4 displays the adjusted incidence rate ratios for bipolar affective disorder stratified by ethnicity and centre and shows increased incidence rate ratios for the disorder in certain Black and minority ethnic groups in Bristol and Nottingham compared with south-east London. The rate ratios were higher in Black African, Asian and mixed ethnicity groups in Nottingham, and in African-Caribbean and Black African groups in Bristol compared with south-east London. Incidence rates of bipolar affective disorder among the White population were somewhat higher in south-east London (3.0, 95% CI 1.7-5.1) than in Nottingham (2.2, 95% CI 1.3-3.5) and Bristol (1.1, 95% CI 0.2-3.3).
Table 4 Adjusted incidence rate ratios by ethnicity and centre
| Ethnicity | Incidence rate ratio (95% CI) | ||
|---|---|---|---|
| Overall1 | Male2 | Female2 | |
| London | |||
| White | I | I | I |
| Black and minority ethnic | 4.0 (2.1-7.7) | 4.8 (1.8-12.7) | 3.4 (1.5-8.1) |
| African-Caribbean | 5.8 (2.7-12.3) | 5.1 (1.4-18.0) | 5.9 (2.3-15.1) |
| Black African | 4.2 (1.9-9.4) | 7.4 (2.5-22.1) | 2.3 (0.7-7.7) |
| Mixed | 1.2 (0.2-9.3) | 3.5 (0.4-28.9) | No cases |
| Asian | 1.3 (0.2-9.8) | 3.0 (0.4-25.3) | No cases |
| Other | 3.8 (1.1-13.1) | No cases | 6.4 (1.7-24.4) |
| Nottingham | |||
| White | I | I | I |
| Black and minority ethnic | 4.9 (2.1-11.0) | 4.6 (1.5-13.7) | 5.3 (1.6-18.0) |
| African-Caribbean | 2.7 (0.4-20.4) | No cases | 5.3 (0.7-43.2) |
| Black African | 12.6 (1.7-95.4) | No cases | 41.5 (5.1-341.1) |
| Mixed | 13.4 (4.4-40.7) | 16.7 (4.5-62.2) | 8.2 (1.0-69.1) |
| Asian | 3.9 (1.1-13.5) | 4.4 (1.0-20.5) | 3.2 (0.4-26.3) |
| Other | No cases | No cases | No cases |
| Bristol | |||
| White | I | I | I |
| Black and minority ethnic | 8.3 (1.4-49.6) | 5.7 (0.5-63.3) | No convergence3 |
| African-Caribbean | 25.9 (2.7-253.8) | No cases | 50.2 (3.1-804.7) |
| Black African | 45.2 (4.6-439.0) | 54.0 (4.9-596.0) | No cases |
| Mixed | No cases | No cases | No cases |
| Asian | No cases | No cases | No cases |
| Other | No cases | No cases | No cases |
We calculated incidence rate ratios for Nottingham and Bristol using the south-east London incidence figures as a baseline and added an ethnicity stratum to the standardisation procedure in order to determine if the high rates in London might be related to differences in ethnic diversity. Our results suggested that ethnic variation probably accounts for some but not all of this difference, with incidence rate ratios (south-east London as baseline) for Nottingham and Bristol being 0.8 (95% CI 0.5-1.3) and 0.5 (95% CI 0.2-1.2) respectively after adjustment for ethnicity.
DISCUSSION
This study demonstrated a significantly higher incidence rate of bipolar affective disorder in south-east London than in Nottingham or Bristol. There was no significant difference in rates between men and women. Black and minority ethnic groups had significantly greater incidence rates of bipolar affective disorder than their White counterparts. This finding was apparent in all three areas and was particularly pronounced in certain minority ethnic groups in Nottingham and Bristol compared with south-east London.
Methodological issues
This study has a number of strengths. We employed a prospective design and used standardised assessments of psychopathology and operational diagnostic criteria. All three samples were collected from geographically defined catchment areas and relied upon direct estimates of the population at risk. The 2001 census data is temporally closest to the study period and included self-ascribed ethnicity and place of birth. The population data were pre-adjusted for under-enumeration. All first-contact patients rather than just first-admission patients were included, and attempts were made to identify any individuals missed by the referral and screening process through the leakage protocol.
A number of methodological issues merit attention. People who had never made contact with psychiatric services were not included in the study. It is therefore likely that we missed cases of bipolar spectrum disorder with brief or minor manic symptoms (bipolar II disorder), which are often managed in the community by general practitioners or possibly remain undiagnosed. Strictly, we have defined the administrative incidence of the more severe bipolar disorders. This will be closer to the true population incidence than would the administrative incidence of spectrum disorders where many subjects may not seek help. Differential use of health and psychiatric services by Black and minority ethnic populations compared with White people in our study might also have had an influence on our inception rates (Harrison, 1984). Cooper et al (Reference Cooper, Goodhead and Craig1987) have suggested that most patients in the UK with severe mental illness are eventually referred to psychiatric services, although among the mobile population of the inner-city areas this may result in presentation out of the geographical area where the illness first developed. However, if such cases are more likely to involve people from Black and minority ethnic groups, this would make our calculated rate ratios, if anything, slight underestimates.
Case definition is particularly problematic in research into bipolar affective disorder as it is difficult to establish the incidence of a disorder that can only be recognised at an unpredictable point in its course, i.e. when polarity changes. For the purposes of this study we accepted modern definitions, which assume bipolarity on the basis of a single episode of mania (Reference Goodwin and JamisonGoodwin & Jamison, 1990; Reference AngstAngst, 1998). Differences in illness presentation are therefore likely to result in failure to identify people presenting with initial depressive episodes who have not yet experienced their first manic episode. It is possible that initial presentation bias might account for some of the inflated risk of bipolar affective disorder in minority ethnic groups, as it has been suggested that Black African and African-Caribbean individuals with this disorder might present more frequently with initial manic episodes compared with their White British counterparts (Reference Kirov and MurrayKirov & Murray, 1999).
Comparison of findings with earlier studies
Our overall incidence figures for bipolar affective disorder are comparable with those reported in previous studies (Reference Spicer, Hare and SlaterSpicer et al, 1973; Reference Leff, Fischer and BertelsenLeff et al, 1976; Reference Daly, Webb and KaliszerDaly et al, 1995; Reference Veijola, Rasanen and IsohanniVeijola et al, 1996; Reference Rasanen, Tiihonen and HakkoRasanen et al, 1998). The first contact rate of bipolar affective disorder in Nottingham is similar to previous rates published by Brewin et al (Reference Brewin, Cantwell and Dalkin1997), whose study was conducted within approximately the same catchment area using a similar method. The latter study, however, found a considerable difference in rates between men and women, a finding not apparent in our sample. Indeed, in contrast to our study, a number of previous studies have reported an increased incidence of mania in women compared with men (Reference Spicer, Hare and SlaterSpicer et al, 1973; Reference Der and BebbingtonDer & Bebbington, 1987; Reference Daly, Webb and KaliszerDaly et al, 1995). However differences might be less apparent in these studies once sampling error is taken into account.
Interpretation of results across centres
Our results suggest that the increased incidence rates of bipolar affective disorder in south-east London compared with Nottingham and Bristol might be partly explained by the higher proportion of individuals from certain Black and minority ethnic backgrounds in this area compared with the other two centres. However, it is important to remember that numerous other factors distinguish the wards of Lambeth and Southwark from Nottingham and Bristol. Higher levels of deprivation, residential mobility and the social pressures of inner-city living together with factors relating to availability and resourcing of local services in south-east London may be of importance in influencing first-contact rates in this area. Incidence rates among the White population were also somewhat higher in south-east London, which accords with the latter hypothesis.
Interactions between bipolar affective disorder and ethnicity
The raised incidence of bipolar affective disorder in Black and minority ethnic groups in all three samples is in keeping with previous similar findings from the UK (Reference Leff, Fischer and BertelsenLeff et al, 1976; Reference Bebbington, Hurry and TennantBebbington et al, 1981; Reference Der and BebbingtonDer & Bebbington, 1987; Reference Van Os, Castle and TakeiVan Os et al, 1996). Leff et al (Reference Leff, Fischer and Bertelsen1976) reported high rates of mania and hypomania among the African-Caribbean population living in south-east London. This group showed significantly higher rates than the White group and more often displayed mixed manic and schizophrenic symptoms. Der & Bebbington (Reference Der and Bebbington1987) and Van Os et al (Reference Van Os, Castle and Takei1996) have confirmed these findings. Furthermore, we found higher rate ratios of bipolar affective disorder particularly in Black and minority ethnic groups in Nottingham and Bristol compared with south-east London. One possibility is that there might be an inverse relationship between the relative size of the ethnic population within a city and the risk of developing bipolar affective disorder; this finding has already been described for schizophrenia by Boydell et al (Reference Boydell, van Os and McKenzie2001), who reported a higher incidence of the latter disorder among members of ethnic minorities living in south-east London wards that had a lower percentage of ethnic minority inhabitants.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The incidence of bipolar affective disorder is greater in south-east London than in Nottingham and Bristol.
-
▪ The incidence is also increased in Black and minority ethnic groups compared with the White population.
-
▪ Greater public health initiatives and clinical resources need to be directed towards the care of patients from minority ethnic groups in the UK.
LIMITATIONS
-
▪ The study did not include people who never made contact with psychiatric services, and therefore cases of bipolar affective disorder with brief or minor manic symptoms are likely to have been missed.
-
▪ Initial presentation bias is problematic in all bipolar affective disorder research and might have affected our results.
-
▪ The study examined three predominantly urban areas and the findings may therefore not be generalisable to other areas in the UK.
Acknowledgements
We acknowledge the contributions of all the ÆSOP study team members. in the three centres on whose behalf the paper was written. We are grateful to. the Medical Research Council and the Stanley Foundation for financial. support.







eLetters
No eLetters have been published for this article.