There is considerable evidence from animal studies that maternal antenatal stress can cause behavioural disturbances in the offspring. Experimentally induced antenatal stress increases disturbances in a range of behaviours in offspring, including decreased gender-typical behaviour and increased response to stress in rats (Reference ThompsonThompson, 1957; Reference Henry, Kabbaj and SimonHenry et al, 1994; Reference WeinstockWeinstock, 1997) and neuromoter delays, increased stress responses and shorter attention spans in non-human primates (Reference Schneider and CoeSchneider & Coe, 1993; Reference Clarke, Wittwer and AbbottClarke et al, 1994). One mechanism underlying this association in animal models is that the stress experienced by the mother has a direct influence on the development of the hypothalamic—pituitary—adrenal (HPA) axis in the foetus (Reference Henry, Kabbaj and SimonHenry et al, 1994; Reference Schneider, Moore and NelsonSchneider & Moore, 2000). The hypothesis that antenatal stress predisposes to behavioural disturbance in human offspring (Reference GloverGlover, 1997) was first suggested many years ago (Reference StottStott, 1973) but the few studies in this area are of small sample size, lack statistical control of confounding variables, rely on retrospective reports and fail to distinguish prenatal from postnatal stress (Reference StottStott, 1973; Reference McIntosh, Mulkins and DeanMcIntosh et al, 1995). The need for further research in humans is underscored by recent studies that might suggest possible mechanisms for this effect. Specifically, recent findings indicate that levels of maternal cortisol in pregnancy correlate with foetal cortisol (Reference Gitau, Cameron and FiskGitau et al, 1998) and that maternal anxiety during pregnancy is associated with increased uterine artery resistance (Reference Teixeira, Fisk and GloverTeixeira et al, 1999). The current study tests the hypothesis that maternal antenatal anxiety predicts behavioural/emotional problems in children.
METHOD
Sample and procedure
The study is based on the Avon Longitudinal Study of Parents and Children (ALSPAC), a longitudinal, prospective study of women, their partners, and an index child (Reference Golding, Pembrey and JonesGolding et al, 2001). The study design included all pregnant women living in the geographical area of Avon, UK, who were to deliver their baby between 1 April 1991 and 31 December 1992. It was estimated that 85-90% of the eligible population participated. The average age of the women at pregnancy was 28 years (range 14-46). Approximately 45% of the women were expecting their first child; 6% of the women had three or more children. All data were collected through postal questionnaires.
Data from at least one questionnaire assessment were available on 12 998 women. However, the total sample available for analysis was substantially lower for several reasons. First, data were collected during several assessments in the antenatal and postnatal period. The rate of attrition per questionnaire assessment was acceptable, in the range 5-15%, but the net effect was cumulative over the multiple assessments. Second, exclusion criteria were specified a priori to ensure our ability to evaluate the timing of antenatal stress on offspring outcome. We excluded those individuals who did not complete the antenatal questionnaires in the allotted time frame (for the first assessment, 6% of the total were excluded, the most obvious reason for this being that these pregnant mothers joined the study later in pregnancy; for the second assessment, the allotted time frame was defined as after 22 weeks and before 39 weeks, with 1% of the total excluded; a further 3% were excluded because the questionnaires were completed in overlapping time periods or in the reverse order), children from multiple births and children born before 33 weeks' gestation. The resulting sample size was 7448.
Maternal anxiety and depression were assessed on two occasions in the antenatal period (18 weeks' and 32 weeks' gestation) and at 8 weeks, 8 months, 21 months and 33 months postnatally. Data on covariates used in the analyses were assessed during pregnancy and shortly after birth. Data on children's behavioural/emotional problems were collected at 47 months.
Measures
Maternal anxiety was measured using the anxiety items from the Crown—Crisp index, a validated self-rating inventory (Reference Birtchnell, Evans and KennardBirtchnell et al, 1988; Reference Sutherland and CooperSutherland & Cooper, 1992). There is no well-established clinical cut-off for this measure; we therefore identified as anxious those mothers who scored in the top 15% (or as close as possible) at each assessment. In this sample, the internal consistencies exceeded 0.80. Maternal depression was assessed using the Edinburgh Postnatal Depression Scale (EPDS), a widely-used 10-item report questionnaire that has been shown to be valid in and outside of the postnatal period (Reference Cox, Holden and SagovskyCox et al, 1987; Reference Murray and CarothersMurray & Carothers, 1990). Internal consistencies exceeded 0.80. A cut-off of 13 was used because it predicts clinical depression based on diagnostic criteria (Reference Murray and CarothersMurray & Carothers, 1990).
Key obstetric factors that were likely to be directly or indirectly related to children's behavioural outcomes were included as covariates. Specific variables were gestational age, birthweight for gestational age (corrected for gender, parity and maternal age and weight), mode of delivery (Caesarean with and without labour, vaginal delivery), and first— or later-born status.
Self-reported smoking and alcohol consumption in early pregnancy were comparatively infrequent. For smoking, risk status was defined as any cigarette or other smoking defined in the 2 weeks prior to completion of the 18-week gestation questionnaire; for alcohol intake, risk status was defined as 1+ units/day in the first 3 months of pregnancy. None of the other measures of smoking and drinking at the later pregnancy assessment improved prediction once these earlier indicators were included in the models, and we therefore retained only the 18-week measures in the analyses.
To control for the possibility that antenatal anxiety was a response to a known or suspected problem with the foetus (which could also have led to behavioural disturbance), we asked whether the mother had concerns about the baby because of a test result in pregnancy. A risk score of 1 was given if the parent reported that she was ‘affected a lot’ or ‘fairly affected’ by the possibility of an abnormal test result; otherwise a score of 0 was assigned. Two indicators of socio-economic status, assessed during pregnancy, were included. A crowding scale, based on the ratio of the number of persons to the total number of rooms in the house, was used as a continuous variable. Maternal education was coded on a four-point scale, with the lowest score indicating minimal educational qualifications and the highest level indicating a university degree. Maternal age (in pregnancy) was included as a dichotomous variable, categorised as ≤20 years or ≥21 years, because preliminary analyses showed that only those children of young mothers were at increased risk for behavioural/emotional problems.
Behavioural adjustment in children at age 4 years was based on parent reports (Reference Goodman and ScottGoodman & Scott, 1999) using an adaptation of a previously widely used index of psychiatric symptoms in children (Reference Elander and RutterElander & Rutter 1996). This measure, which has three problem behaviour subscales (conduct problems, emotional problems, hyperactivity/inattention), has established links with clinical levels of disturbance (Reference Goodman and ScottGoodman & Scott, 1999). Internal consistencies of the scales ranged from 0.62 to 0.75. We identified children with difficulties based on statistically high scores, using a cut-off of 2 standard deviations (s.d.) above the mean. Cut-off scores were derived separately for males and females because of the gender differences in mean scores on these measures. Consequently, analyses were conducted separately for males and females.
Data analysis
The analytic aims were twofold. The first was to investigate whether antenatal anxiety is a risk for behavioural/emotional problems in children. We therefore examined whether antenatal anxiety predicts behavioural/emotional problems at age 4 years after controlling for key antenatal, obstetric and socio-demographic risks. In addition, to determine whether the antenatal risk for behavioural/emotional problems was specific to maternal antenatal anxiety or more generally to maternal mental health, we included in the analyses measures of ante— natal and postnatal depression (Reference Murray and CooperMurray & Cooper, 1997). The second aim was to examine whether there could be risks linked specifically to anxiety in the antenatal period. We therefore examined whether maternal antenatal anxiety predicted behavioural/emotional problems in children after controlling for multiple postnatal assessments of maternal anxiety. Throughout the analyses, we begin by reporting the findings for total behavioral/emotional problems and note if findings differ by specific behavioural problem sub-scale.
As expected, the large majority of children in this community sample did not exhibit clinically meaningful levels of psychopathology. Consequently, because we were interested in whether the findings were of clinical relevance, we initially report analyses using extreme scores using established cut-off scores (where available) or high scores defined statistically. We follow this approach with analyses of individual differences. As detailed below, the findings are substantively identical. The two approaches require somewhat different analytical methods, however. For analyses based on a dichotomous dependent variable, logistic regression was used and odds ratios (ORs) are reported as the index of association. When we examined the continuous measure of behavioural/emotional problems as the dependent variable, ordinary least-squares regression was used. In both kinds of analyses, a hierarchical approach was used in which the antenatal obstetric and psychosocial covariates were entered at step 1 and the measures of maternal anxiety and depression in pregnancy and the postnatal period were entered at step 2. The estimates reported in Tables 2 and 3 are from the final model, and indicate the effect of each variable controlling for the effects of all other variables in the model.
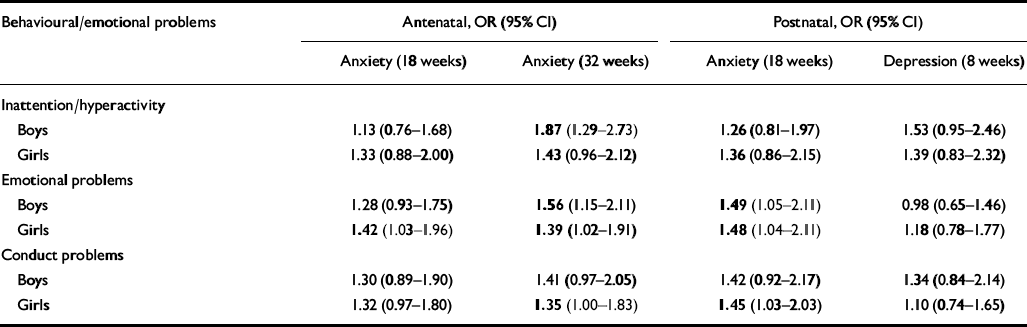
Table 1 Bivariate associations between antenatal anxiety at 18 and 32 weeks' gestation and children's behavioural/emotional problems at age 4 years
| Males | Females | |||
|---|---|---|---|---|
| 18 weeks | 32 weeks | 18 weeks | 32 weeks | |
| OR (95% CI) | OR (95% CI) | OR (95% CI) | OR (95% CI) | |
| Total problems | 2.43 (1.81-3.27) | 3.21 (2.42-4.27) | 2.82 (2.13-3.75) | 3.07 (2.34-4.03) |
| Inattention/hyperactivity | 1.84 (1.35-2.52) | 2.63 (1.96-3.53) | 1.96 (1.43-2.70) | 2.20 (1.63-2.97) |
| Emotional problems | 1.88 (1.47-2.40) | 1.91 (1.50-2.43) | 2.01 (1.56-2.58) | 1.99 (1.56-2.53) |
| Conduct problems | 2.11 (1.57-2.84) | 2.41 (1.80-3.22) | 2.06 (1.61-2.62) | 2.04 (1.62-2.58) |
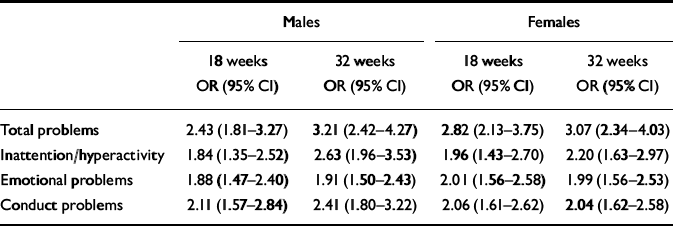
Table 2 Multivariate analysis of antenatal, obstetric and demographic predictors of age 4 total behavioural/emotional problems
| Males | Females | |||||||
|---|---|---|---|---|---|---|---|---|
| n | B | OR (95% CI) | Wald | n | B | OR (95% CI) | Wald | |
| Pregnancy/obstetric risks | ||||||||
| Birthweight: GA | 3853 | -1.70 | 0.18 (0.5-0.68) | 6.39* | 3595 | -0.87 | 0.42 (0.12-1.46) | 1.86 |
| Concerns about pregnancy | 0.49 | 0.03 | ||||||
| No | 3763 | 1.00 | 3503 | 1.00 | ||||
| Yes | 90 | 0.31 | 1.36 (0.58-3.22) | 92 | 0.07 | 1.08 (0.45-2.55) | ||
| Smoking | 3.47 | 1.29 | ||||||
| None | 3230 | 1.00 | 3047 | 1.00 | ||||
| Yes | 623 | 0.32 | 1.38 (0.98-1.93) | 548 | 0.20 | 1.21 (0.87-1.72) | ||
| Alcohol | 0.31 | 0.15 | ||||||
| <1 unit/day | 3786 | 1.00 | 3536 | 1.00 | ||||
| 1+ units/day | 67 | -0.30 | 0.74 (0.25-2.15) | 59 | 0.18 | 1.20 (0.48-2.97) | ||
| Psychosocial factors | ||||||||
| Crowding | 3853 | 0.07 | 1.06 (0.92-1.23) | 0.75 | 3595 | 0.14 | 1.15 (1.00-1.31) | 3.73 |
| Educational attainment | 11.14* | 16.73*** | ||||||
| CSE/Vocational | 932 | 1.00 | 828 | 1.00 | ||||
| ‘O’ level | 1394 | -0.10 | 0.90 (0.64-1.26) | 1298 | -0.26 | 0.77 (0.56-1.07) | ||
| ‘A’ level | 977 | -0.46 | 0.63 (0.41-0.97) | 915 | -0.45 | 0.64 (0.44-0.94) | ||
| University degree | 550 | -0.92 | 0.40 (0.21-0.74) | 554 | -1.26 | 0.28 (0.15-0.54) | ||
| Maternal age | 21.19*** | 5.05* | ||||||
| ⩽ 20 years | 148 | 1.00 | 141 | 1.00 | ||||
| ⩾ 21 years | 3705 | 1.11 | 3.04 (1.89-4.89) | 3454 | 0.58 | 1.78 (1.08-2.95) | ||
| Anxiety | ||||||||
| 18 weeks | 0.39 | 2.56 | ||||||
| No | 3283 | 1.00 | 3098 | 1.00 | ||||
| Yes | 570 | 0.12 | 1.13 (0.77-1.67) | 497 | 0.31 | 1.36 (0.93-1.98) | ||
| 32 weeks | 16.09*** | 11.84*** | ||||||
| No | 3250 | 1.00 | 3034 | 1.00 | ||||
| Yes | 603 | 0.76 | 2.14 (1.48-3.10) | 561 | 0.63 | 1.88 (1.31-2.69) | ||
| 8 weeks postnatal | 3.81 | 1.83 | ||||||
| No | 3300 | 1.00 | 3090 | 1.00 | ||||
| Yes | 553 | 0.43 | 1.54 (1.00-2.37) | 505 | 0.30 | 1.35 (0.88-2.07) | ||
| Depression | ||||||||
| Postnatal 8 weeks | 2.90 | 2.42 | ||||||
| No | 3504 | 1.00 | 3293 | 1.00 | ||||
| Yes | 349 | 0.40 | 1.49 (0.94-2.37) | 302 | 0.38 | 1.46 (0.91-2.34) | ||
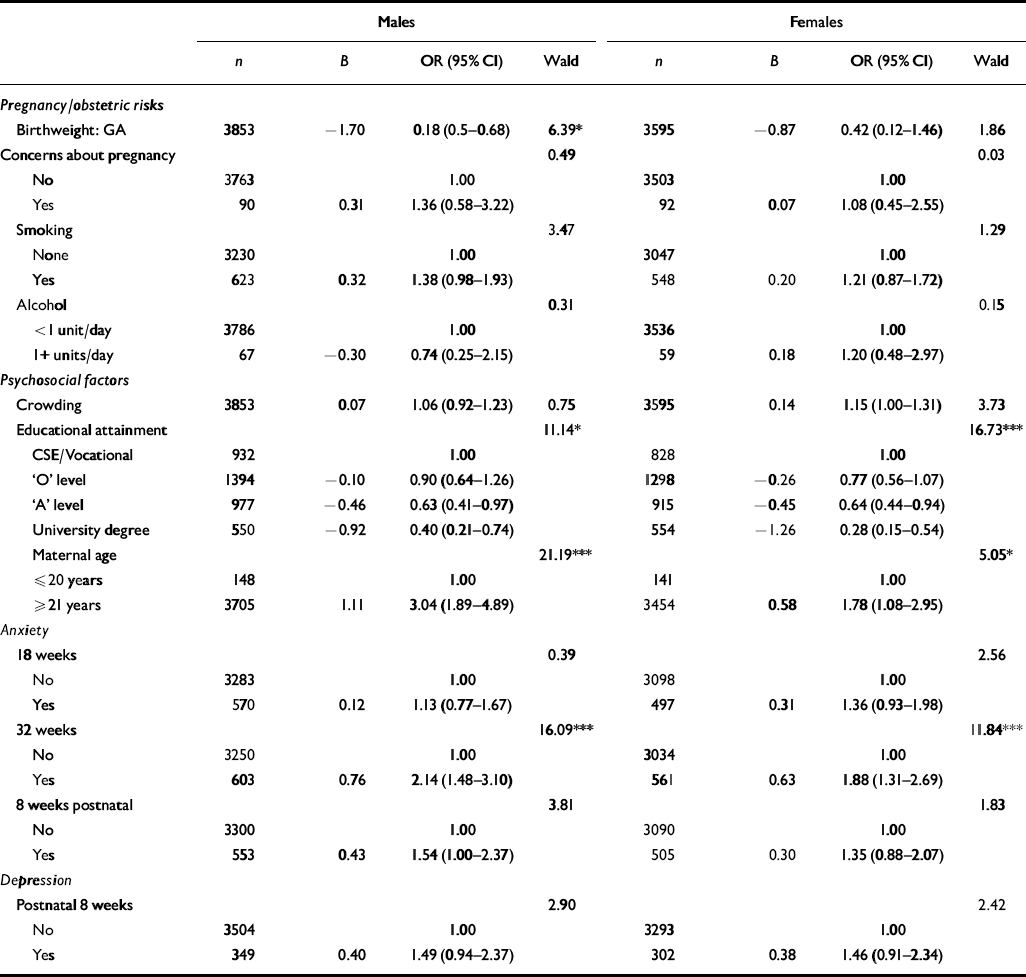
Table 3 Effects of antenatal and postnatal anxiety and postnatal depression on behavioural/emotional problems in children after covarying antenatal, obstetric and socio-demographic risks
| Behavioural/emotional problems | Antenatal, OR (95% CI) | Postnatal, OR (95% CI) | ||
|---|---|---|---|---|
| Anxiety (18 weeks) | Anxiety (32 weeks) | Anxiety (18 weeks) | Depression (8 weeks) | |
| Inattention/hyperactivity | ||||
| Boys | 1.13 (0.76-1.68) | 1.87(1.29-2.73) | 1.26 (0.81-1.97) | 1.53 (0.95-2.46) |
| Girls | 1.33 (0.88-2.00) | 1.43 (0.96-2.12) | 1.36 (0.86-2.15) | 1.39 (0.83-2.32) |
| Emotional problems | ||||
| Boys | 1.28 (0.93-1.75) | 1.56(1.15-2.11) | 1.49(1.05-2.11) | 0.98 (0.65-1.46) |
| Girls | 1.42(1.03-1.96) | 1.39(1.02-1.91) | 1.48(1.04-2.11) | 1.18 (0.78-1.77) |
| Conduct problems | ||||
| Boys | 1.30 (0.89-1.90) | 1.41 (0.97-2.05) | 1.42 (0.92-2.17) | 1.34 (0.84-2.14) |
| Girls | 1.32 (0.97-1.80) | 1.35(1.00-1.83) | 1.45(1.03-2.03) | 1.10 (0.74-1.65) |
RESULTS
Attrition was more likely in those with higher anxiety scores at the earlier assessments. For example, compared with women with complete data from early pregnancy through to the child's fourth birthday (n=7824), those women for whom data were available only at 18 weeks' gestation (n=508) scored, on average, approximately one-half point higher on the anxiety measure at the 18 weeks assessment (range 0-16; means 95% CI), respectively, 4.7 (4.6-4.8) and 5.4 (5.0-5.7). The disproportionate loss of families with elevated maternal anxiety could result in a diminished effect of antenatal anxiety to the extent that the connection between ante— natal anxiety and children's behavioural/emotional problems is evident only at the more extreme end of maternal psychopathology. Because of our interest in the timing of maternal anxiety and because we were concerned that those cases with missing data might be disproportionately likely to have high scores for a given assessment, we did not use any data substitution methods for missing maternal anxiety data. For similar reasons, we did not use any data substitution methods for missing behavioural outcome data for the child. Additionally, we were uncertain that respondents who did not provide data on some covariates (notably smoking and alcohol intake) would necessarily fall in the non-risk category (e.g. those who drank excessively might have refused to answer this question). Therefore, we used mean substitutions as a strategy for dealing with missing data only for continuous measures for which concerns about non-response bias were minimal (i.e. the ratio of birthweight to gestational age and crowding). The findings reported below are substantively identical when only cases with complete data are included, so we included the slightly more inclusive sample.
Preliminary analyses indicated that birthweight, gestational age and mode of delivery were not associated with the outcome measures once we controlled for birthweight for gestational age. Additionally, first and later pregnancies were combined because the effects of antenatal anxiety on offspring outcomes were substantively identical for first— and later-born children.
Maternal anxiety
All pairwise correlations between measures of maternal anxiety exceededr=0.50, and the magnitude was inversely associated with the time interval between assessments. The large sample size made it possible to identify specific groups with elevated anxiety only at particular times. Using the categorical distinction of a cut-off for high anxiety of the top 15%, 64.6% experienced no anxiety, 14.6% experienced elevated anxiety on one occasion only, 7.7% experienced elevated anxiety on two occasions, 5.2% experienced elevated anxiety on three occasions, 3.6% experienced elevated anxiety on four occasions, 2.7% experienced elevated anxiety on five occasions and 1.8% experienced elevated anxiety on all six occasions.
Bivariate associations between maternal anxiety and behavioural/emotional problems at age 4 years
The findings in Table 1 indicate that mothers who scored in the top 15% of the sample on anxiety at 18 or 32 weeks' gestation were generally 2-3 times more likely to have a child who scored more than 2 s.d. above the mean in behavioural/emotional problems.
Multivariate associations
The next set of analyses provides a stronger test of the effects of antenatal anxiety by including antenatal, obstetric and psychosocial covariates, together with postnatal assessments of anxiety and depression at 8 weeks. The results for total problems for boys and girls are shown in Table 2. The ORs in the models represent the effect of the variable controlling for the effects of other variables in the model. Mothers who experienced markedly elevated anxiety at 32 weeks' gestation were more than twice as likely to have children with markedly elevated behavioural/emotional problems at 4 years of age (OR 2.14 for boys and 1.88 for girls). The effects of antenatal anxiety were equally strong for boys and girls, although the prediction from other covariates differed slightly for boys and girls. No significant interactions between late antenatal anxiety and any of the covariates were detected. The findings for the specific symptom sub-scales are given in Table 3. Late antenatal anxiety significantly predicted later behavioural/emotional problems for four of the six outcomes.
Previous analyses indicated that the late antenatal anxiety effect was maintained after controlling for postnatal depression. As a test of the specific effects of anxiety in the antenatal period, we included in the model (from Table 2) the assessment of depression in the late antenatal period at 32 weeks' gestation. For neither boys nor girls was the significant effect of late antenatal anxiety reduced to non-significance when antenatal depression was included in the model predicting total problems.
Effects of postnatal anxiety
To determine whether or not the effect of antenatal anxiety could be distinguished from the cumulative effect of postnatal anxiety throughout the child's early years, we re-ran the models including maternal anxiety at 8, 21 and 33 months postnatally. Analyses indicated that, for both boys and girls, the composite measure of total problems remained significantly associated with late antenatal anxiety even when the effects of antenatal, obstetric and psychosocial covariates, as well as four measures of postnatal anxiety, were statistically controlled. In these models, the ORs for maternal anxiety at 32 weeks' gestation were 1.56 (95% CI 1.02-2.41) for boys and 1.51 (95% CI 1.01-2.27) for girls. In addition, for males, late antenatal anxiety was associated significantly with hyperactivity/inattention at 4 years of age, even after postnatal self-reports of anxiety at 8 weeks and 8, 21 and 33 months were included in the model (OR 1.85, 95% CI 1.22-2.81). Particularly notable is the finding that including maternal anxiety in the postnatal period had virtually no effect on the magnitude of antenatal prediction, and this is despite the fact that postnatal maternal anxiety also significantly predicted inattention/ hyperactivity at 4 years of age (only maternal anxiety at 21 months was statistically significant; OR 1.99, 95% CI 1.26-3.15).
Evaluating the robustness of the effect
A final series of analyses was carried out to demonstrate that these associations held across the range of individual differences rather than only at the extremes. When less extreme scores of behavioural/emotional problems were used in the models (based on a cut-off score of 1 s.d. above the mean) substantively similar results were obtained. For example, for the model predicting total problems that included all covariates plus postnatal assessments of anxiety through 33 months, the ORs were 1.39 (1.04-1.84) for boys and 1.53 (1.12-2.10) for girls. Furthermore, in the most conservative model that included the covariates plus postnatal assessments of anxiety through 33 months, the effect of late antenatal anxiety was significant in a regression analysis when we examined the continuous measure of maternal anxiety and the continuous measure of behavioural/emotional problems in children (for boys, β=0.07, P<0.05; for girls, β=0.06,P<0.05).
DISCUSSION
We found strong and significant links between antenatal anxiety and children's behavioural/emotional problems at age 4 years. Associations were found for a range of disturbances in children, and for both boys and girls. In most instances, the effects were maintained when antenatal, obstetric and socio-demographic risks were controlled for, together with a measure of anxiety and depression in the postnatal period. The most impressive finding was that elevated levels of anxiety in late pregnancy were associated with hyperactivity/inattention in boys, and total behavioural/emotional problems in both boys and girls, even when the effects of multiple postnatal reports of anxiety were controlled statistically. This suggests that the antenatal prediction is not mediated by a link between antenatal and postnatal anxiety or depression, but, as in the animal models, is due to a direct causal mechanism operating in the antenatal period.
Limitations
The prospective longitudinal design and the large community sample provided considerable power in assessing the connection between antenatal anxiety and later child outcomes, but some limitations should be noted. First, the selective attrition could mean that we are observing associations among the less severely distrubed individuals. However, it does not seem that the attrition would have fundamentally influenced the findings in a major way. That is because the association between antenatal anxiety and outcomes was not confined to the extreme ends of psychopathology, but was evident within the normal range of maternal anxiety and children's behaviour. Whether the obtained effects would have been larger if more of the psychologically distressed individuals remained in the study is a possibility that we are unable to test. A second consideration is that the data were based entirely on maternal report. This is inevitable in large-scale studies, but it does raise a methodological concern that the ratings of child behavioural/emotional problems were influenced by reporter bias. That is, anxious mothers might be more likely to over— (or mis-)report disturbance in their children. However, if reporter bias were operating, we would not expect to find adifferential prediction from the antenatal period, and certainly not when covarying multiple postnatal measures of maternal anxiety more proximal to the assessment of behavioural/emotional problems. Other sources of data on children's behavioural/emotional problems, notably teacher reports, were not available at 4 years. Concerns about maternal reports of children's behavioural/emotional problems must be balanced against the finding that the effect was obtained across the range of individual differences and that elevated scores do correspond to clinically documented psychopathology (Reference Goodman and ScottGoodman & Scott, 1999). Other explanations could also account for a transmission between maternal anxiety and child behavioural disturbance, most notably genetic mediation (Reference Rutter, Silberg and O'ConnorRutter et al, 1999). However, if genetic mediation were operating it would not be likely to explain why there is a specific connection between maternal antenatal anxiety and children's disturbance even when multiple postnatal assessments were covaried. Thus, the specific antenatal effect is noteworthy both in drawing direct parallels with previous animal research and in countering alternative explanations that the effect is due merely to reporter bias or genetic transmission.
Antenatal anxiety predicts behavioural/emotional problems
Several features of the association between antenatal anxiety and children's behavioural/emotional disturbance are of interest. First, the nature of the antenatal risk derived from anxiety/stress rather than from psychological disturbance more generally, indexed in our study by depression. This differential finding is especially important given that anxiety rather than depression is the analogue risk in animal studies and that depression and anxiety are invariably moderately to highly correlated. Postnatal depression, especially in the early weeks and months following birth, is a known risk factor for behavioural/emotional problems in children (Reference Murray and CooperMurray & Cooper, 1997). Therefore, the finding that the antenatal anxiety effect was maintained when postnatal depression was included indicates that the effect obtained is neither mediated through postnatal depression nor explained by general maternal distress. The apparent specificity of the antenatal anxiety effect is also inconsistent with a simple reporter bias as an alternative explanation of the findings.
Second, although there is some suggestion for specificity of risk associated with maternal antenatal mental health, it is far less clear whether the effects on children's behaviour are general or specific. Thus, the bivariate analyses showed that all three sub-scales were associated significantly with antenatal anxiety (Table 1), and this continued to be the case (albeit with two exceptions) when the covariates were included (Table 3). In the analysis that included multiple postnatal assessments of maternal anxiety, the prediction of total problems in both boys and girls from late antenatal anxiety remained significant; the only sub-scale that remained linked significantly with late antenatal anxiety was inattention/hyperactivity (in boys). It could be that the effects were strongest for the composite measure of total problems because this was the most reliable index of problems. The persistent effect on inattention/hyperactivity in boys parallels findings from animal research (Reference Schneider, Moore and NelsonSchneider & Moore, 2000).
Third, the results for total problems are consistent with developmental programming, or the notion that experiences in early life can persistently influence how the individual responds to later experiences (Reference Ladd, Owens and NemeroffLadd et al, 1996). This is the dominant model derived from the animal research findings, and is based on the finding that antenatal stress can permanently alter the developing HPA axis of the offspring. There are, as yet, few instances of developmental programming found in studies of human behavioural development, and further research on the mechanisms involved (e.g. HPA axis) is clearly needed. It is noteworthy that a model of foetal programming has gained considerable support in the cardiovascular research field (Reference BarkerBarker, 1995). Fourth, the connection between antenatal anxiety and children's behavioural/emotional problems was found after controlling for key antenatal and obstetric risks, including birthweight for gestational age. This is an important consideration given that maternal antenatal stress predicts poor obstetric outcome (Reference Hedegaard, Henriksen and SabroeHedegaard et al, 1993; Reference Lou, Hansen and NordentoftLou et al, 1994; Reference Copper, Goldenberg and DasCopper et al, 1996), which could have then increased the risk for behavioural/emotional problems in early childhood.
Finally, although all bivariate associations between antenatal anxiety and behavioural/emotional outcomes were substantial, the effect was partly, and in some cases completely, explained by co-occurring antenatal, obstetric or socio-demographic risks. Controlling for overlapping risks is a prerequisite in the effort to establish causal relationships. However, one side-effect is that we could have actually underestimated the ‘real’ effect insofar as statistically controlling for socio-demographic risk might also account for a substantial amount of stress and anxiety experienced by mothers; indeed, crowding, one of the covariates used in this study, was the stress imposed in early animal studies (Reference KeeleyKeeley, 1962). Similarly, by controlling for postnatal anxiety on multiple occasions we could have ‘over-controlled’ for the effects of antenatal anxiety.
Findings from experimental animal research point to the HPA axis as playing an important role in the connection between maternal antenatal stress and the adjustment of offspring (Reference Clarke, Wittwer and AbbottClarke et al, 1994; Reference Caldji, Diorio and MeaneyCaldji et al, 2000). Overactive or dysregulated HPA axis activity is implicated in much psychopathology in adults and children, especially depression and anxiety (Reference Chrousos and GoldChrousos & Gold, 1992). Whether this mechanism also explains the connections observed in this report requires further study.
This study shows a new and additional mode of transmission connecting maternal anxiety and children's behavioural/emotional problems. This should be considered together with other identified risks for psychopathology in children, such as psychosocial and genetic factors. These findings raise the possibility of benefit from an intervention programme targeted specifically at anxiety in pregnant women.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Anxiety in pregnancy could have long-term effects on children's behavioural/emotional problems.
-
• Long-term alterations in the stress response could be influenced by early, even antenatal, experience.
-
• Reducing maternal anxiety in pregnancy could have protective preventive effects for children.
LIMITATIONS
-
• Data on maternal anxiety and children's adjustment were based on self-report questionnaires.
-
• The effect sizes were small to modest, especially in analysis involving postnatal risks.
-
• The data do not allow us to determine what physiological mechanisms account for the observed associations.
Acknowledgements
The ALSPAC study is part of the World Health Organization-initiated European Longitudinal Study of Pregnancy and Childhood. We are extremely grateful to all of the mothers who participated and to the midwives for their cooperation and help in recruitment. The whole ALSPAC study team comprises interviewers, computer technicians, laboratory technicians, clerical workers, research scientists, volunteers and managers who continue to make the study possible.






eLetters
No eLetters have been published for this article.