Reviews of studies demonstrating an association between maternal depression and psychological problems in children have concluded by identifying a need for preventive interventions (Reference Downey and CoyneDowney & Coyne, 1990; Reference Goodman and GotlibGoodman & Gotlib, 1999). Both depression and childhood behaviour disorder have been associated with psychosocial adversity (Reference Ostler, Thompson and KinmonthOstler et al, 2001). Theoretical research consistently challenges simple linear causal models of the impact of maternal depression and raises the question of the bi-directionality with child behaviour problems (Reference DodgeDodge, 1990; Reference Rutter, Murray and CooperRutter, 1997). Effective interventions should therefore address both areas.
Few studies have focused on both mothers’ and children's problems (Reference Puckering, Rogers and MillsPuckering et al, 1994; Reference Gelfand, Teti and SeinerGelfand et al, 1996; Reference Cooper, Murray, Murray and CooperCooper & Murray, 1997; Reference Sanders and McFarlandSanders & McFarland, 2000); none used group interventions. The study reported here evaluated a cognitive–behavioural programme addressing maternal and child psychopathology, considering evidence of good outcome for cognitive therapy for depression (Reference Jacobson, Dobson and TruaxJacobson et al, 1996) and for parenting skills groups (Reference Webster-StrattonWebster-Stratton, 1991).
METHOD
This randomised, placebo-controlled trial compared three treatment groups: a cognitive–behavioural therapy (CBT) group for mothers with depression (the active treatment); a mothers’ support group (the placebo treatment); and no intervention. The following hypotheses were tested. The primary hypothesis was that children of mothers who received CBT would have significantly lower scores on the behavioural measures than children of mothers in the other two comparison groups at the end of treatment, and at 6-month and 1-year follow-up. The other hypotheses were that mothers who received CBT would have significantly lower scores on the measures of depression than mothers in the comparison groups at the same assessment points, and that mothers and children in both the CBT and mothers’ support group would have better outcomes than those receiving no treatment.
Overview
The study was an assessor-masked, randomised controlled trial using an epidemiological sample – that is, the sample was derived from the total population of mothers and children within a geographical area in which the children fell within a targeted age range. The study was not based upon a clinically referred sample. A community was screened to identify mother–child dyads where the mother and the child scored highly on standardised measures. Mothers identified as being clinically depressed from interview were randomly allocated to CBT, placebo contact (mother and toddler groups) or no treatment groups.
The project was conducted in the Wythenshawe, Withington and Burnage areas of south Manchester, UK, areas with high levels of socio-economic deprivation. The population is predominantly White and is composed of a high proportion of mothers with young children. Two large, centrally located modern health centres with child-friendly facilities were used. Ethical approval was obtained from South Manchester Ethics Committee. Consent for participation was obtained before screening and before trial entry.
Screening
All mothers with children aged between 2 years 6 months and 4 years (pre-school age) were identified using the Community Child Health Register and, subject to consent, were asked to complete the Beck Depression Inventory (BDI; Reference Beck, Ward and MendelsonBeck et al, 1961) and, by postal questionnaire, the Preschool Behaviour Checklist (PBCL; Reference Richman, Stevenson and GrahamRichman et al, 1982) or, by interview, the Behaviour Screening Questionnaire (BSQ; Reference Richman and GrahamRichman & Graham, 1971). Mothers were contacted first by post; those who did not respond were visited at home. Women were excluded if their child was not living with them, if their first language was not English, if they were suffering from a major psychiatric disorder other than depression, or if their child had a major developmental disability. Women who fulfilled the screening criteria both for depression (BDI score ≥15) and child problems (BSQ score ≥ 8) were entered into the study, using the multiple criterion screen methodology of Nicol et al (Reference Nicol, Stretch and Fundudis1993).
Sample size
In calculating the sample size, a moderately large effect size (0.6) was assumed on the primary outcome of child behaviour problems with the Child Behavior Checklist (CBCL; Reference Achenbach and EdelbrockAchenbach & Edelbrock, 1983). To have an 80% chance of detecting that size difference between the CBT and the control groups, using a two-tailed test, a sample of 45 per condition was required (significance level of 0.5).
Procedure
Randomisation to the three groups was concealed, and was performed by an independent statistician using sealed envelopes and stratified by gender of child. No blocking was used. Slowness in initial recruitment meant that an inadequate number of participants were available for three-way allocation at first randomisation. Because it was essential for the groups to start on time, the first randomisation was to the groups only – CBT or mother and toddler group – resulting in a smaller number being allocated to the ‘no treatment’ group (Fig. 1).

Fig. 1 Trial profile: recruitment, screening and random allocation (BDI, Beck Depression Inventory; BSQ, Behaviour Screening Questionnaire; MDD, major depressive disorder).
Assessment points
Assessments were made by research assistants masked to group allocation at the following time points: pre-intervention, immediately post-intervention, 6-month follow-up, and 12-month follow-up. Masking was maintained by separating the assessors administratively from the therapist and requesting participants not to discuss any details of treatment with them.
Measures
The primary outcome measures of the study were assessments of the behaviour problems of the children. Assessments of maternal depression were secondary outcomes. In choosing the primary measures of outcome, two issues were taken into account: first, the possibility that the mother's mental state would influence her rating of the child's behaviour; and second, the requirement that, as far as was possible, outcome measures were made masked to treatment status. These were resolved by obtaining child outcome measures from a number of sources (including direct observations), and by employing an independent assessor (the assistant clinical psychologist) kept masked to treatment status by exclusion from access to records and discussion regarding intervention.
Assessment of children
The mothers were asked to complete the CBCL – a well-validated checklist for parents’ reports of children's competencies and problems, yielding scores for internalising and externalising problems and a total score. This measure is in widespread research use, and norms are available for clinic-referred and non-referred populations (Reference Achenbach and EdelbrockAchenbach & Edelbrock, 1983). Mothers also completed the Eyberg Child Behaviour Inventory (ECBI; Reference Robinson, Eyberg and RossRobinson et al, 1980), a 36-item inventory of child conduct problem behaviours, standardised on children 2–7 years old and with acceptable validity and reliability. The ECBI is used frequently in evaluation of the effectiveness of parent training groups. In addition, a brief developmental assessment of the child investigated areas of vocabulary, verbal comprehension, digit recall and basic number skills, yielding scores for individual scales as well as overall IQ (British Ability Scales short form; Reference ElliottElliott, 1987), and a structured interview was used to obtain demographic details, family and psychosocial information, and details of the child's development.
For children attending nursery or school, teachers were asked to complete the teacher equivalent of the parent measures, the Preschool Behaviour Checklist (Reference McGuire and RichmanMcGuire & Richman, 1988) and CBCL. Small numbers attending nursery and a high attrition rate precluded further analysis of these measures.
Assessment of mothers
A standardised psychiatric interview, the Structured Clinical Interview for DSM–IV Non-Patient edition (SCID–NP; Reference Spitzer, Williams and GibbonSpitzer et al, 1994), was used to assess the adult participants’ mental state, with the Hamilton Rating Scale for Depression (HRSD; Reference HamiltonHamilton, 1967) for rating the severity of depressive symptoms. The participants also completed the BDI, an 18-item standardised self-report measure of clinical depression including suicidal risk which is in widespread research and clinical use in the UK (severity score range 0–63), and a self-report checklist of history and treatment of depression. The measures used at screening were repeated at the completion of treatment and at 6-month and 12-month follow-up.
Intervention
Women assessed as having a DSM–IV diagnosis of depression (American Psychiatric Association, 1994) and who accepted an offer of intervention were randomly allocated to one of the three groups. During the course of the intervention, group therapists used a strategy of assertive outreach to optimise attendance and minimise the numbers leaving the study. Transport was provided to all groups if required by participants. Follow-up contacts and telephone reminders were made prior to treatment sessions and after any missed sessions. The social aspects of the groups were emphasised to enhance adherence and participation.
Group 1 – cognitive–behavioural therapy
Group 1 (47 mother–child pairs) was assigned to receive CBT in the form of 16 group sessions. These sessions for 6–8 mother–child pairs were held weekly and were run by two clinical psychologists with support from two nursery nurses qualified in child care. Four experienced clinical psychologists qualified for a minimum of 5 years were involved in treatment.
The mothers’ group and the children's play sessions were separate and ran in parallel for 90 min. The mothers’ group applied:
-
(a) techniques in cognitive therapy for depression;
-
(b) a psycho-educational approach to understanding children's developmental needs;
-
(c) behavioural training in parenting skills, focusing on positive and child-centred methods of control;
-
(d) goal-setting in early sessions to promote focused change;
-
(e) task-setting for practice of skills outside the group.
The focus of cognitive therapy was on aspects of cognition and problem-solving that relate most directly to parenting, where possible. This included how depression could cause problems in parenting: for instance, effects of irritability on children's behaviour, and low mood leading to lack of confidence as a parent. There was a shift in focus as sessions progressed, with less time devoted to coping with depression and more to developing positive parenting skills (further information available from the author upon request). The parenting sessions included education about normal developmental problems and children's understanding, enhancing the mother–child relationship through child-centred play, dealing with negative behaviour (ignoring and time out), reinforcing positive behaviours, praise and attention. Mothers identified problems that they wished to work on and developed action plans, keeping a diary between sessions. Cognitive therapy sessions included education about depression from a cognitive perspective, development of a problem formulation for each woman, activity scheduling, problem-solving and cognitive restructuring.
Quality and fidelity of therapy was ensured by weekly supervision from one of three clinical psychologists experienced in CBT supervision.
Group 2 – mother and toddler groups
Group 2 (44 mother–child pairs) attended mother and toddler groups run by a health visitor together with an experienced clinical psychologist. These sessions were designed as an attention placebo and ran at the same frequency as the active treatment groups, using the same staffing ratio. They had the same facilities available and included informal, non-directed group discussion of problems raised by the mothers and separate play opportunities for the children. The format was similar to many community-based support groups for mothers with young children, but no advice was given on parenting or other problems.
Group 3 – no treatment
Group 3 (28 mother–child pairs) received no intervention, and these mothers and children were assessed by home visit only. Routine services were accessible as usual to these participants, and service uptake was recorded.
Analysis
Data were analysed using the Statistical Package for the Social Sciences version 10.1 for Windows. Analyses were conducted on an intention-to-treat basis – that is, all participants who had been randomised to a treatment group were included in the analyses irrespective of the actual treatment received. Parametric statistics were used throughout since all variables conformed to the assumptions underlying such analyses, including normality of distributions. Between-group differences on continuous measures for children and mothers were analysed through multivariate analyses of variance with repeated measures on the time factor. For assessing the outcomes over multiple time points (post-treatment, 6-month and 12-month follow-up) repeated-measures analysis of covariance (ANCOVA) was employed, again using pre-treatment scores as the covariate. To compare the effects within the treatment groups on the outcome measures before and after treatment, a series of paired-sample t-tests were used.
RESULTS
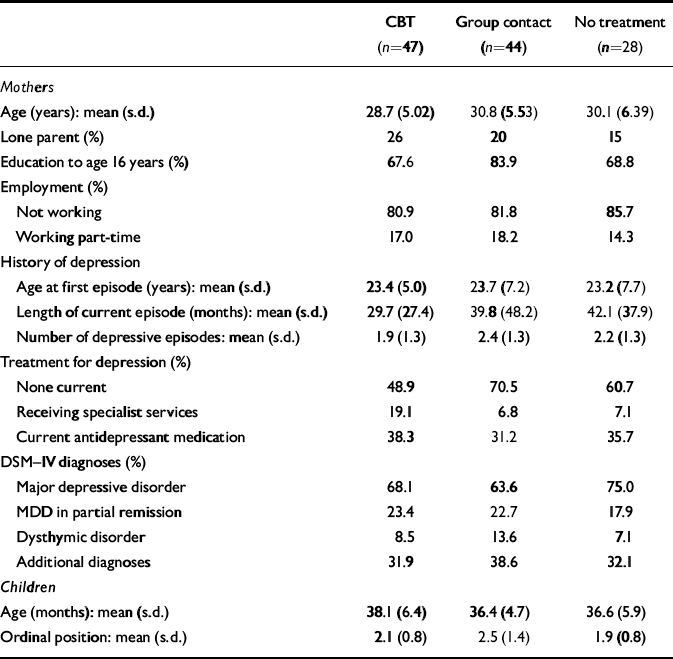
Characteristics of the study sample (n=119) are shown in Tables 1 and 2. None of the variables reported showed significant statistical difference between the three groups. It can be seen that participants represent a socially disadvantaged group, with mothers having recurrent or chronic histories of depression, often from adolescence.
Table 1 Sample characteristics (n=119)
| CBT (n=47) | Group contact (n=44) | No treatment (n=28) | |
|---|---|---|---|
| Mothers | |||
| Age (years): mean (s.d.) | 28.7 (5.02) | 30.8 (5.53) | 30.1 (6.39) |
| Lone parent (%) | 26 | 20 | 15 |
| Education to age 16 years (%) | 67.6 | 83.9 | 68.8 |
| Employment (%) | |||
| Not working | 80.9 | 81.8 | 85.7 |
| Working part-time | 17.0 | 18.2 | 14.3 |
| History of depression | |||
| Age at first episode (years): mean (s.d.) | 23.4 (5.0) | 23.7 (7.2) | 23.2 (7.7) |
| Length of current episode (months): mean (s.d.) | 29.7 (27.4) | 39.8 (48.2) | 42.1 (37.9) |
| Number of depressive episodes: mean (s.d.) | 1.9 (1.3) | 2.4 (1.3) | 2.2 (1.3) |
| Treatment for depression (%) | |||
| None current | 48.9 | 70.5 | 60.7 |
| Receiving specialist services | 19.1 | 6.8 | 7.1 |
| Current antidepressant medication | 38.3 | 31.2 | 35.7 |
| DSM—IV diagnoses (%) | |||
| Major depressive disorder | 68.1 | 63.6 | 75.0 |
| MDD in partial remission | 23.4 | 22.7 | 17.9 |
| Dysthymic disorder | 8.5 | 13.6 | 7.1 |
| Additional diagnoses | 31.9 | 38.6 | 32.1 |
| Children | |||
| Age (months): mean (s.d.) | 38.1 (6.4) | 36.4 (4.7) | 36.6 (5.9) |
| Ordinal position: mean (s.d.) | 2.1 (0.8) | 2.5 (1.4) | 1.9 (0.8) |
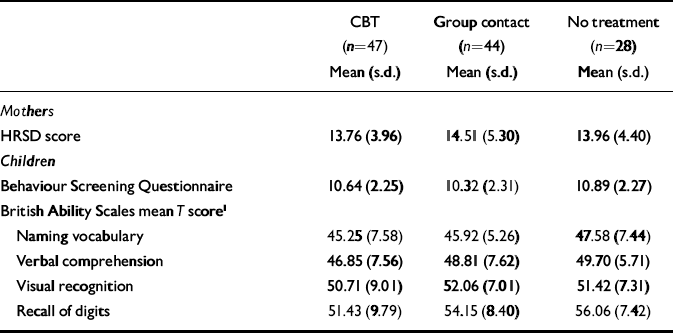
Table 2 Baseline scores on measures of depression, children's ability and behaviour (n=119)
| CBT (n=47) Mean (s.d.) | Group contact (n=44) Mean (s.d.) | No treatment (n=28) Mean (s.d.) | |
|---|---|---|---|
| Mothers | |||
| HRSD score | 13.76 (3.96) | 14.51 (5.30) | 13.96 (4.40) |
| Children | |||
| Behaviour Screening Questionnaire | 10.64 (2.25) | 10.32 (2.31) | 10.89 (2.27) |
| British Ability Scales mean T score1 | |||
| Naming vocabulary | 45.25 (7.58) | 45.92 (5.26) | 47.58 (7.44) |
| Verbal comprehension | 46.85 (7.56) | 48.81 (7.62) | 49.70 (5.71) |
| Visual recognition | 50.71 (9.01) | 52.06 (7.01) | 51.42 (7.31) |
| Recall of digits | 51.43 (9.79) | 54.15 (8.40) | 56.06 (7.42) |
Between-group analysis
Repeated-measures ANCOVA with pre-treatment scores as the covariate revealed no significant difference between the three groups at post-treatment assessment and follow-up on either the primary outcome measures of child problem or the secondary outcome measures of maternal depression (Tables 3 and 4). In an attempt to ascertain whether the two contact groups (groups 1 and 2) differed from group 3 (no treatment), these two groups were combined and compared with group 3. Again, repeated-measures ANCOVAs revealed no significant difference between the two contact groups combined and group 3 on any of the primary or secondary outcome measures.
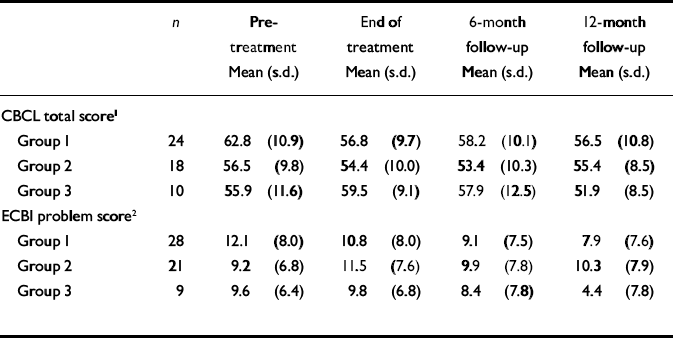
Table 3 Differences in child outcome measures between study group 1 (cognitive–behavioural therapy), group 2 (mother and toddler group) and group 3 (no treatment)
| n | Pretreatment Mean (s.d.) | End of treatment Mean (s.d.) | 6-month follow-up Mean (s.d.) | 12-month follow-up Mean (s.d.) | |
|---|---|---|---|---|---|
| CBCL total score1 | |||||
| Group 1 | 24 | 62.8 (10.9) | 56.8 (9.7) | 58.2 (10.1) | 56.5 (10.8) |
| Group 2 | 18 | 56.5 (9.8) | 54.4 (10.0) | 53.4 (10.3) | 55.4 (8.5) |
| Group 3 | 10 | 55.9 (11.6) | 59.5 (9.1) | 57.9 (12.5) | 51.9 (8.5) |
| ECBI problem score2 | |||||
| Group 1 | 28 | 12.1 (8.0) | 10.8 (8.0) | 9.1 (7.5) | 7.9 (7.6) |
| Group 2 | 21 | 9.2 (6.8) | 11.5 (7.6) | 9.9 (7.8) | 10.3 (7.9) |
| Group 3 | 9 | 9.6 (6.4) | 9.8 (6.8) | 8.4 (7.8) | 4.4 (7.8) |
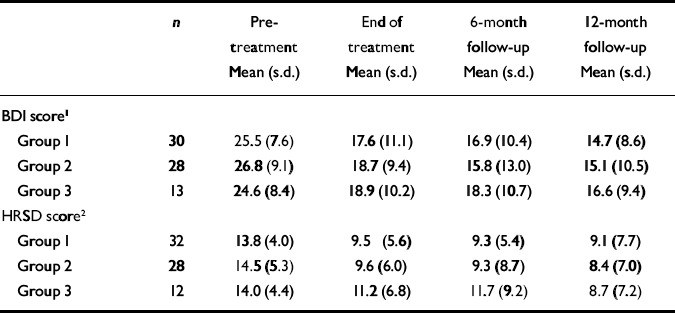
Table 4 Differences in maternal depression measures between study group 1 (cognitive–behavioural therapy), group 2 (mother and toddler group) and group 3 (no treatment)
| n | Pretreatment Mean (s.d.) | End of treatment Mean (s.d.) | 6-month follow-up Mean (s.d.) | 12-month follow-up Mean (s.d.) | |
|---|---|---|---|---|---|
| BDI score1 | |||||
| Group 1 | 30 | 25.5 (7.6) | 17.6 (11.1) | 16.9 (10.4) | 14.7 (8.6) |
| Group 2 | 28 | 26.8 (9.1) | 18.7 (9.4) | 15.8 (13.0) | 15.1 (10.5) |
| Group 3 | 13 | 24.6 (8.4) | 18.9 (10.2) | 18.3 (10.7) | 16.6 (9.4) |
| HRSD score2 | |||||
| Group 1 | 32 | 13.8 (4.0) | 9.5 (5.6) | 9.3 (5.4) | 9.1 (7.7) |
| Group 2 | 28 | 14.5 (5.3) | 9.6 (6.0) | 9.3 (8.7) | 8.4 (7.0) |
| Group 3 | 12 | 14.0 (4.4) | 11.2 (6.8) | 11.7 (9.2) | 8.7 (7.2) |
Within-group analysis
To determine whether there were any changes over treatment and at follow-up a series of post hoc within-group analyses were performed separately for each of the three treatment groups.
Primary outcome: child behaviour
There were significant differences in the primary outcome of child behaviour pre-test to post-test (t=3.54, d.f.=31, P < 0.001), pre-test to 6-month follow-up (t=2.95, d.f.=27, P=0.006) and to 12-month follow-up (t=2.98, d.f.=30, P=0.006) on CBCL total scores for the CBT group but not for the two control groups. The CBT group also displayed an improvement in ECBI problem scores from pre-test to 6-month follow-up (t=2.66, d.f.=31, P=0.01) and to 12-month follow-up (t=2.88, d.f.=33, P=0.007), whereas the two control groups did not.
Secondary outcome: maternal depression
Paired-sample t-tests were used to assess any differences in pre-intervention and post-intervention scores. At the end of the intervention, women's depression (as measured by the BDI) showed significant improvement in both group 1 (t=3.90, d.f.=34, P<0.001) and group 2 (t=2.30, d.f.=31, P<0.03). In contrast, there was no difference in the ‘no treatment’ group (t=1.58, d.f.=20, P=0.13). The improvement experienced by the two contact groups was maintained at the 12-month follow-up (group 1: t=4.41, d.f.=39, P<0.001; group 2: t=4.36, d.f.=30, P<0.001). The HRSD scores showed a similar pattern: group 1 had improved significantly after the intervention (t=5.18, d.f.=35, P<0.001), as had group 2 (t=4.23, d.f.=31, P<0.001). In contrast, the no treatment group did not improve on this measure. The improvements in groups 1 and 2 were maintained at 12-month follow-up (group 1: t=4.01, d.f.=39, P<0.001; group 2: t=3.67, d.f.=30, P=0.001).
DISCUSSION
This study used cognitive–behavioural group-based interventions to target both children's behaviour and maternal depression. It was based in a community setting, recruited from a population sample rather than from clinical referrals, and was closely linked to existing resources. An active treatment, a placebo treatment and a ‘no treatment’ control group were included. A wide range of outcome measures assessing both mother and child were applied, and assessments were made masked to treatment group allocation. There was a follow-up period of at least 1 year. The CBT and mother and toddler groups had high face validity for the mothers and also provided social support, and were integrated with established primary care services. This study attempted to address the general need for research on combined and pragmatic treatments which are clinically grounded (Reference Harrington, Peter and GreenHarrington et al, 2000).
There were important differences between this study and previous ones. The programme was targeted at severe and persistent maternal depression in women with children of pre-school age, in contrast to earlier studies which targeted either post-natal depression or less severe maternal depression. Additionally, the study overcame some methodological deficiencies of previous work by employing a design that controlled for the non-specific aspects of therapy (including social support), ensured masked and independent assessment of treatment outcomes, and had a sample drawn from an epidemiological cohort.
Outcome
The study did not demonstrate statistically significant differences between the three treatment groups on either the primary outcome of child behaviour or the secondary outcome of maternal depression. This was disappointing because there was a strong clinical impression and anecdotal feedback from the participants that the CBT groups were beneficial and well accepted. Thus, the principal analysis did not reveal significant group differences between the treatment groups.
Post hoc within-group analyses were promising. These indicated that the CBT group alone showed statistically significant improvement at the post-treatment assessment on the child behaviour measures. In addition, both the groups that involved contact (groups 1 and 2) showed significant improvements in maternal depression scores, which were maintained over the 12-month follow-up period, in contrast to women in the untreated control group, who did not improve. There are no clear group differences, although within-group analyses suggest that there are benefits for both child and mother from participation in CBT groups. The non-specific effects of mother and toddler groups may also reduce maternal depression although they have less effect on the problems of the child. These results must be treated with caution, and this study treated as a preliminary test of feasibility from which to generate further research, rather than as a definitive answer.
Recruitment and study design
The problems with slow recruitment at the beginning of the study meant that the non-intervention control group was restricted to 28 mother–child pairs, which reduced the power of the study to show statistically significant differences. A potential strength of the study was its use of an epidemiological cohort, using a community sample to avoid the selection and referral biases that dogged early studies of the impact of maternal depression (Reference Downey and CoyneDowney & Coyne, 1990). However, this methodology presented difficulties in conducting the study. Women who had not sought help were approached to attend groups; this was likely to have affected successful recruitment and might have resulted in inclusion of a smaller sample than would have been possible with recruitment from clinic attenders. Recruitment into therapy groups, which is conventionally expected to be about 50% with clinically referred populations, was 37% in this study. For testing study hypotheses this figure is problematic although clinically not unusual. Once recruited into the study, 39% of women completed a substantial number of sessions. It proved possible to design an attention placebo group sufficiently attractive to maintain similar attendance rates. Unfortunately, the level of attrition in the study was high, which means that the results need to be interpreted with caution.
The nature of the sample presented significant problems in assessing participants, as there were high levels of mobility and life crises. Encouraging attendance at follow-up assessments, particularly by participants who had not been offered intervention, proved difficult.
Clinical issues
Previous research has not used comparable populations or interventions, or targeted the problems of both mothers and children. The study suggests that the highly structured format of CBT was helpful, but completing the course in 16 weeks to adhere to the treatment manual was challenging to therapists. A key problem was persuading women to attend the groups consistently and regularly to protocol. Considerable effort was expended in attempting to achieve this, including arranging transport if required. Once attendance was established, retention was generally good but was sometimes interrupted by life events, most often episodes of difficulties with partners. For some women, a longer and more flexible intervention might have been more useful and in tune with their lifestyle.
In clinical practice, where referral increases the likelihood of successful engagement into groups, the treatment programme as it stands might be more effective than under research constraints. It appeared that the therapeutic approach was helpful to some mothers and their children. The group nature of the intervention was effective in promoting social support, to the extent that several of the groups continued to meet.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Clinical services should consider actively intervening to treat both maternal and child symptoms.
-
▪ Delivery of effective community-based programmes for mothers with depression presents challenges to therapists.
-
▪ Interventions with socially deprived populations, particularly those aimed at mothers with depression, need to consider active methods for engaging the targeted group, such as building effective working relationships over time, non-blaming approaches, home visiting, and methods that promote group support and cohesion.
LIMITATIONS
-
▪ Targeting women who had not sought help led to difficulties in recruitment and retention in the study.
-
▪ There was no clear significant difference between treatment groups. Significant changes were demonstrated over treatment, mainly in the cognitive–behavioural therapy group, but only in post hoc within-group analyses.
-
▪ The level of attrition in the study generally was high and only a third of eligible women attended the groups.
Acknowledgements
The study was funded by a National Health Service Research and Development. grant. We wish to acknowledge the following individuals who made an invaluable. contribution to the project: Maggie Manasse, health visitor; Linda Steen, consultant clinical psychologist; and Caitlin Jones and Gillian Fortune, research assistants. Group supervision was provided from within the research. team and by Dr Adrian Wells, senior lecturer at the Department of Clinical. Psychology, University of Manchester. Statistical support has been provided by. Dr Brian Faragher and Dr Julie Morris of the University of Manchester. Department of Medical Statistics.







eLetters
No eLetters have been published for this article.