Studies of UK and US military personnel who have deployed to the recent conflicts in Iraq or Afghanistan have suggested that there are significant differences in mental health outcomes between personnel in the two militaries. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1-Reference Sundin, Fear, Iversen, Rona and Wessely6 Deployment to Iraq and Afghanistan has not been associated with post-traumatic stress disorder (PTSD) or common mental disorders for the majority of UK regular personnel, although an association between deploying in a combat role and PTSD has been demonstrated. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1 In contrast, US research has shown that deployment to Iraq and Afghanistan is consistently associated with higher rates of mental health problems in general and PTSD specifically. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Hoge, Terhakopian, Castro, Messer and Engel3 Research has also demonstrated an association between combat experiences and PTSD in the US military. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Smith, Ryan, Wingard, Slymen, Sallis and Kritz-Silverstein7,Reference Vasterling, Proctor, Friedman, Hoge, Heeren and King8 Overall, the prevalence of screening positive for PTSD has been reported to be higher in US compared with UK military personnel with the US typically reporting ranges between 9 and 20% and the UK reporting ranges between 3 and 7%. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1,Reference Hoge and Castro4-Reference Mulligan, Fear, Jones, Alvarez, Hull and Naumann12
Deployment to Iraq and Afghanistan is also associated with higher rates of alcohol misuse in UK and US personnel, but self-reported alcohol misuse tends to be greater in UK compared with US military personnel. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1,Reference Jacobson, Ryan, Hooper, Smith, Amoroso and Boyko13-Reference Wilk, Bliese, Kim, Thomas, McGurk and Hoge16 The prevalence of hazardous consumption of alcohol has been reported as 67% and 49% in UK male and female personnel respectively, compared with between 8 and 36% in US military personnel using similar measures. Reference Fear, Iversen, Meltzer, Workman, Hull and Greenberg17-Reference Meis, Barry, Kehle, Erbes and Polusny21 Deployment to Iraq and Afghanistan is also associated with aggressive behaviour, and similar prevalence of violent or aggressive behaviour has been reported in studies of UK (12.6%) and US personnel (11.2-18.4%) deployed to Iraq and Afghanistan. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Thomas, Wilk, Riviere, McGurk, Castro and Hoge10,Reference MacManus, Dean, Al Bakir, Iversen, Hull and Fahy22
Finally, deployments are associated with increased risk for reports of post-deployment somatic complaints often comorbid with psychological health symptoms. For example, 34.4% of US soldiers scoring positive for PTSD reported a high level of somatic complaints, compared with 5.2% for those who did not score positive for PTSD, with an overall prevalence of 12.0%. Reference Hoge, Terhakopian, Castro, Messer and Engel3 Similar prevalence has been reported in the UK military (12%), with a small association between deployments and increased risk for reports of post-deployment somatic complaints. Reference Hotopf, Hull, Fear, Browne, Horn and Iversen5
A number of reasons have been proposed for the differences between US and UK forces, including differences in levels of combat exposure, length of deployment, dwell time (the amount of time that service members spend in their home nation between deployments), time from returning from deployment to survey administration, level of anonymity of reporting, proportion of National Guard/reserve personnel, and differences in alcohol use among service members. Reference Sundin, Fear, Iversen, Rona and Wessely6,Reference Kok, Herrell, Thomas and Hoge23 However, there have been no direct comparisons to determine the specific reasons for the differences. A recent meta-analysis suggested that the principal reason for the differences in PTSD prevalence was because the majority of US studies have focused on combat infantry units, whereas UK studies have involved random samples of the entire deployed population. Reference Kok, Herrell, Thomas and Hoge23 Support personnel account for nearly two-thirds of all deployed service members, and there is strong evidence of a dose-response effect of greater combat frequency and intensity on the development of PTSD. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Kok, Herrell, Thomas and Hoge23,Reference Ikin, Sim, Creamer, Forbes, McKenzie and Kelsall24 Although the meta-analysis provided a useful way to group the large number of prevalence studies, there has not been an effort to combine data from different study samples, which would permit controlling for variables known to be associated with mental health outcomes. In our study we therefore combine data from comparable US and UK study samples. We compare the prevalence of post-deployment health outcomes, including PTSD, hazardous alcohol consumption, aggressive behaviour and multiple physical symptoms in UK and US military personnel who were deployed to Iraq in 2007-2008. We also examine whether demographic and military characteristics or combat exposures may explain differences between the post-deployment health outcomes observed in UK and US military personnel.
Method
Data were combined from one US and one UK study that assessed post-deployment mental health in military personnel who had deployed to Iraq. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1,Reference Adler, Britt, Castro, McGurk and Bliese25 The two data-sets were the only data-sets that US and UK investigators could identify, among a large number of studies, that were comparable in terms of deployment location, time period of deployment, survey items, timing of survey administration and level of confidentiality in the survey administration methods. Most US post-deployment prevalence studies have used anonymous survey methods, whereas most UK studies have required collection of personal identifiers for longitudinal tracking. Use of identifiers has been shown to influence willingness to report mental health concerns (compared with anonymous reporting). Reference Warner, Appenzeller, Grieger, Belenkiy, Breitbach and Parker26,Reference Fear, Seddon, Jones, Greenberg and Wessely27 The two data-sets used in this study both involved collection of identifiers to allow linkage with other data, and were thus not anonymous.
The US data were collected as part of a larger study on post-deployment transition. Reference Adler, Britt, Castro, McGurk and Bliese25 This study was approved by an institutional review board at the Walter Reed Army Institute of Research. In 2008, surveys were administered to US soldiers in an active component brigade combat team, 4 months after their return from a 15-month combat deployment to Iraq. Surveys were administered in large classrooms on a US army base in Germany. Participation was voluntary; 90.1% of potential participants provided informed consent and took part in the study. The survey was completed by 1658 soldiers but the final sample for the current study was 1591, excluding the few who had never deployed or had not deployed with the Brigade.
The UK data were collected as part of a longitudinal cohort study of the effect of deployment to Iraq or Afghanistan. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1 The study received ethics approval from the Ministry of Defence’s research ethics committee and King’s College Hospital local research ethics committee. The cohort started in 2004, with a further follow-up between 2007 and 2009 (n = 6427). At that time two new samples of individuals who had deployed to Afghanistan between April 2006 and April 2007 (n = 894) or who had joined the UK military since the cohort was first recruited in 2003 (n = 2663) were added to the cohort. It was the latter group who formed the sample frame for the current analyses (those who joined the study for the first time at the second phase of data collection and who had deployed to Iraq in 2007-2008 (n = 504)), to ensure a comparable sample frame with the US study. Participants were followed up on average a year after return from deployment.
The final analysis sample was limited to regular enlisted army male personnel, resulting in a total number of 1560 US soldiers and 313 UK soldiers who had deployed to Iraq in 2007-2008. There was considerable overlap between the UK and US questionnaires and variables that had been assessed with the same measure or that were comparable were identified (measures were similar because some of the authors had participated in an international technical panel in which they discussed using comparable approaches. The panel was sponsored through the Technical and Cooperation Program). Variables that were comparable but had used different response formats in the two studies were recoded to a similar response scale.
Measures
Comparable variables included sociodemographics and military characteristics: age at questionnaire completion, level of education, rank, marital status, years in service, total number of deployments to Iraq and Afghanistan and career intentions; combat experiences included 11 items taken from the Combat Experiences Scale, Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2 responses were coded based on whether an experience was endorsed as having happened at least once during the deployment.
The main outcomes included the 17-item National Center for PTSD Checklist (PCL) Reference Weathers, Litz, Herman, Huska and Keane28 to measure probable PTSD, and the 3-item Alcohol Use Disorders Identification Test - Consumption subscale (AUDIT-C) Reference Babor, Higgins-Biddle, Saunders and Monteiro29 to examine hazardous alcohol consumption. Two definitions of probable PTSD were examined, PCL-50 defined as a total score of 50 and above, and PCL-DSM-IV based on DSM-IV criteria, 30 which required that the participant scored moderate or above on one of the re-experiencing symptoms, three avoidance symptoms and two hyperarousal symptoms. Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Weathers, Litz, Herman, Huska and Keane28 In addition to examining probable PTSD, differences in PCL total score were examined with ordinary least squares (OLS) regression. This continuous PTSD outcome was used because of low levels of probable PTSD in the UK sample.
The majority of both the UK and the US samples scored above the standard cut-off of 4/5 on the AUDIT-C. Reference Babor, Higgins-Biddle, Saunders and Monteiro29 A receiver operating characteristics (ROC) analysis was carried out for the UK sample to assess the sensitivity and specificity of the AUDIT-C using the full AUDIT with a cut-off of 16 as the criterion for alcohol misuse. Reference Babor, Higgins-Biddle, Saunders and Monteiro29 The ROC analyses based on the total AUDIT-C scores indicated that a cut-off of 10 on the AUDIT-C resulted in the best sensitivity and specificity (78% and 80% respectively). The area under the curve (AUC) was 0.86 (95% CI 0.82-0.91). Therefore, a cut-off of 10 on the AUDIT-C was used for the multivariable analyses of alcohol misuse.
Other outcomes included a list of nine physical symptoms (such as stomach pain and headaches); the US items were drawn from the PHQ-15, Reference Kroenke, Spitzer and Williams31 and the UK items were taken from a checklist of 53 symptoms. Reference Hotopf, Hull, Fear, Browne, Horn and Iversen5,Reference Unwin, Blatchley, Coker, Ferry, Hotopf and Hull32 We used a case definition for multiple physical symptoms as two or more symptoms. Aggressive behaviour was assessed with four items that asked participants whether in the past month they ‘got angry with someone and yell or shout at them’, ‘got angry with someone and kicked or smashed something, slammed the door, punched the wall’, ‘threatened someone with physical violence’ or ‘got into a fight with someone and hit the person’. Reference Thomas, Wilk, Riviere, McGurk, Castro and Hoge10 For examining aggressive behaviour as an outcome we used the most specific item, ‘got into a fight with someone and hit the person’, as evidence of aggressive behaviour. Reference Thomas, Wilk, Riviere, McGurk, Castro and Hoge10
Analyses
All analyses were carried out in Stata 11.2 on Windows. The sociodemographic and military characteristics, combat experiences and outcome measures were compared between the UK and US samples. Proportions were calculated and statistical significance was assessed with Pearson’s χ2 statistic. Associations between cohort (UK or US) and dichotomous health outcomes were modelled using logistic regression analyses for PTSD, hazardous alcohol consumption, aggressive behaviour and multiple physical symptoms. We modelled the total score of the PCL using OLS regression and present the unadjusted and adjusted mean scores by cohort. The proportion of missing values was 7.4%. Complete cases analysis was used for each health outcome (PTSD outcomes n = 1747; alcohol misuse n = 1801; aggressive behaviour n = 1804; multiple physical symptoms n = 1810).
Analyses were stratified by combat exposure because there was a significant difference in the level of exposures between the US and the UK samples, and previous research has shown that those in combat roles and those with high levels of exposure are at greatest risk of health problems. The cut-off for the stratification variable was set at five or more combat experiences, this was the mean and median score for the US sample (the UK sample had a mean and median score of four combat exposures). The cut-off of five was chosen due to fewer cases of PTSD in the UK group with low-combat exposures when the cut-off was set at four or more experiences (n = 3). Results were comparable using both cut-offs with the exception for the adjusted comparison of PCL-DSM-IV with high levels of combat exposures, which became significant with a higher prevalence of PTSD in the US sample for the cut-off of four (odds ratio (OR) = 1.87, 95% CI 1.07-3.29).
In the adjusted analyses of aggressive behaviour, we entered hazardous alcohol use into the model as a covariate because of differences in hazardous alcohol use between the UK and US samples and the association between hazardous alcohol use and aggressive behaviour. Level of education was not included in the adjusted analyses due to a high association with rank (rho (ρ) = 0.66).
Results
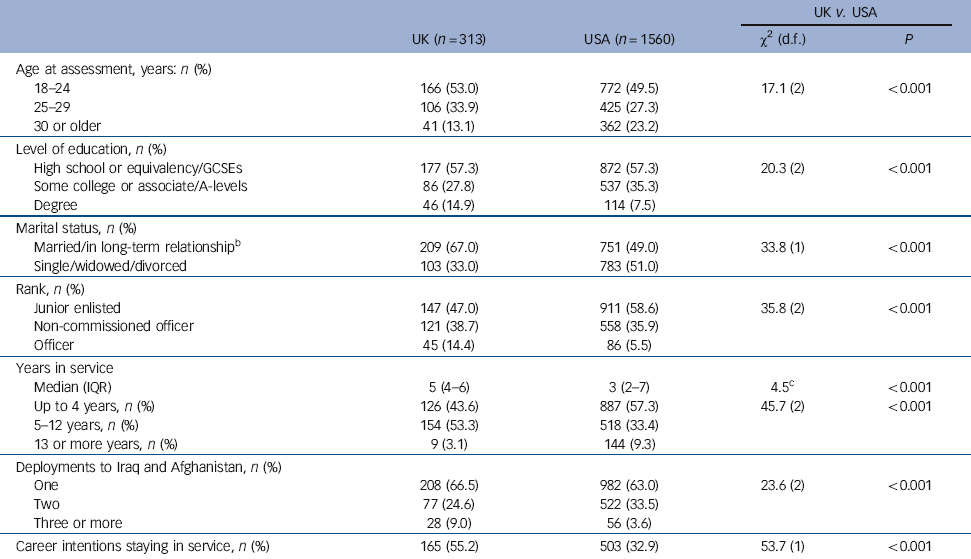
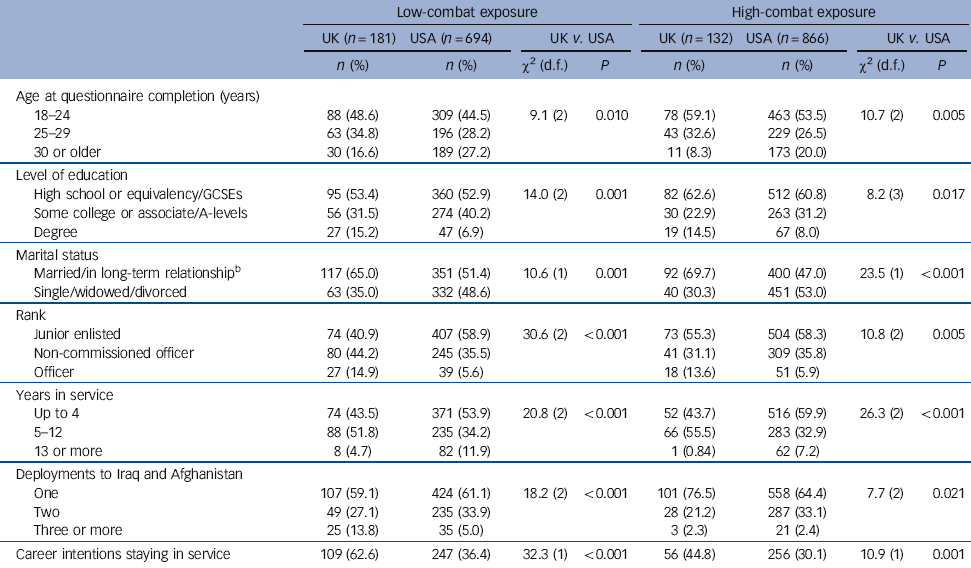
Compared with the UK sample, the US sample was older (although the majority of both samples were under 30 years of age), less likely to hold a degree, less likely to be married or in a long-term relationship (the response option being ‘in long term relationship’ was included in the UK, but not the US, questionnaire), less likely to be an officer and more likely to have served for less than 5 years or 13 or more years in the military, the UK sample was more likely to have served for 5-12 years (Table 1). The UK sample was also more likely to have deployed to Iraq and Afghanistan three or more times and to report having career intentions of staying in the military. Stratifying for level of combat exposure reversed the association between cohort and number of deployments to Iraq and Afghanistan in the high-combat exposure group, with the US sample more likely to have deployed twice. All other differences between the UK and US samples remained significant after stratifying for level of combat exposure (Table 2).
Table 1 Sociodemographic characteristics of the two samplesFootnote a
| UK v. USA | ||||
|---|---|---|---|---|
| UK (n = 313) | USA (n = 1560) | χ2 (d.f.) | P | |
| Age at assessment, years: n (%) | ||||
| 18-24 | 166 (53.0) | 772 (49.5) | 17.1 (2) | <0.001 |
| 25-29 | 106 (33.9) | 425 (27.3) | ||
| 30 or older | 41 (13.1) | 362 (23.2) | ||
| Level of education, n (%) | ||||
| High school or equivalency/GCSEs | 177 (57.3) | 872 (57.3) | 20.3 (2) | <0.001 |
| Some college or associate/A-levels | 86 (27.8) | 537 (35.3) | ||
| Degree | 46 (14.9) | 114 (7.5) | ||
| Marital status, n (%) | ||||
| Married/in long-term relationshipFootnote b | 209 (67.0) | 751 (49.0) | 33.8 (1) | <0.001 |
| Single/widowed/divorced | 103 (33.0) | 783 (51.0) | ||
| Rank, n (%) | ||||
| Junior enlisted | 147 (47.0) | 911 (58.6) | 35.8 (2) | <0.001 |
| Non-commissioned officer | 121 (38.7) | 558 (35.9) | ||
| Officer | 45 (14.4) | 86 (5.5) | ||
| Years in service | ||||
| Median (IQR) | 5 (4-6) | 3 (2-7) | 4.5Footnote c | <0.001 |
| Up to 4 years, n (%) | 126 (43.6) | 887 (57.3) | 45.7 (2) | <0.001 |
| 5-12 years, n (%) | 154 (53.3) | 518 (33.4) | ||
| 13 or more years, n (%) | 9 (3.1) | 144 (9.3) | ||
| Deployments to Iraq and Afghanistan, n (%) | ||||
| One | 208 (66.5) | 982 (63.0) | 23.6 (2) | <0.001 |
| Two | 77 (24.6) | 522 (33.5) | ||
| Three or more | 28 (9.0) | 56 (3.6) | ||
| Career intentions staying in service, n (%) | 165 (55.2) | 503 (32.9) | 53.7 (1) | <0.001 |
a. Numbers may not add up to total because of missing values.
b. The response option being ‘in long-term relationship’ was only asked in the UK questionnaire.
c. Wilcoxon rank-sum test for difference.
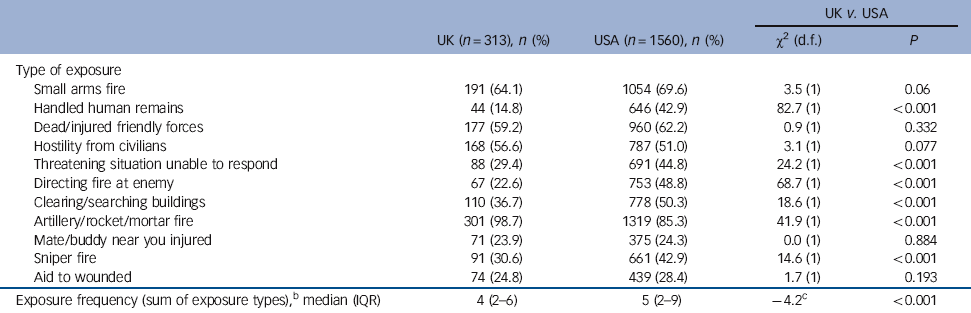
The US sample reported more combat exposures overall and were significantly more likely to report handling human remains, being in a threatening situation where they were unable to respond, directing fire at the enemy, clearing/searching buildings and encountering sniper fire than the UK sample (Table 3). In contrast, the UK sample was more likely to report indirect fire (artillery, mortar or rocket fire).
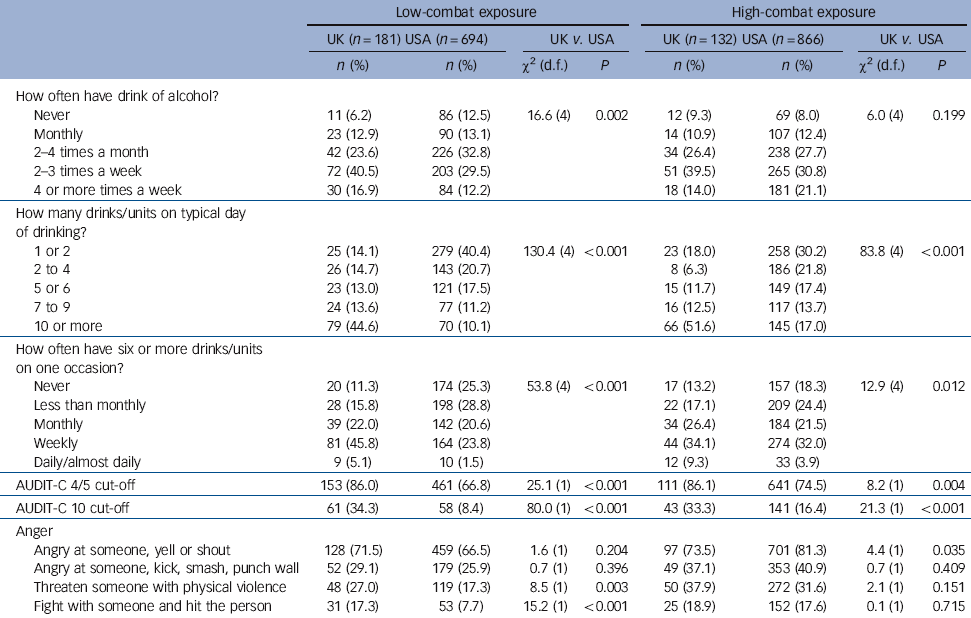
Comparison of unadjusted proportions of post-deployment health outcomes showed that the US sample had a higher prevalence of probable PTSD, based on the PCL-50 definition in the high-combat exposure group and a higher prevalence of PTSD based on the PCL-DSM-IV definition in both the low- and high-combat exposure groups (Table 4). The prevalence of hazardous alcohol use was higher in the UK compared with the US sample in both the low- and high-combat exposure groups (Table 5). There was a marked difference between the UK (52%) and US (17%) samples who reported drinking ten or more drinks/units on a typical day of drinking. There were differences between the UK and the US samples in aggressive behaviours, and among the low-combat exposure groups, the UK sample was more likely to report having threatened someone with violence or having had a fight and hitting a person (Table 5). Among the high-combat exposure groups the US sample was more likely to report yelling or shouting at someone, but other aggressive behaviours were comparable. There was no difference between the UK and US samples in multiple physical symptoms in either the low- or high-combat exposure groups (online Table DS1).
Table 2 Sociodemographics and family information, stratified by low- and high-combat exposureFootnote a
| Low-combat exposure | High-combat exposure | |||||||
|---|---|---|---|---|---|---|---|---|
| UK (n = 181) | USA (n = 694) | UK v. USA | UK (n = 132) | USA (n = 866) | UK v. USA | |||
| n (%) | n (%) | χ2 (d.f.) | P | n (%) | n (%) | χ2 (d.f.) | P | |
| Age at questionnaire completion (years) | ||||||||
| 18-24 | 88 (48.6) | 309 (44.5) | 9.1 (2) | 0.010 | 78 (59.1) | 463 (53.5) | 10.7 (2) | 0.005 |
| 25-29 | 63 (34.8) | 196 (28.2) | 43 (32.6) | 229 (26.5) | ||||
| 30 or older | 30 (16.6) | 189 (27.2) | 11 (8.3) | 173 (20.0) | ||||
| Level of education | ||||||||
| High school or equivalency/GCSEs | 95 (53.4) | 360 (52.9) | 14.0 (2) | 0.001 | 82 (62.6) | 512 (60.8) | 8.2 (3) | 0.017 |
| Some college or associate/A-levels | 56 (31.5) | 274 (40.2) | 30 (22.9) | 263 (31.2) | ||||
| Degree | 27 (15.2) | 47 (6.9) | 19 (14.5) | 67 (8.0) | ||||
| Marital status | ||||||||
| Married/in long-term relationshipFootnote b | 117 (65.0) | 351 (51.4) | 10.6 (1) | 0.001 | 92 (69.7) | 400 (47.0) | 23.5 (1) | <0.001 |
| Single/widowed/divorced | 63 (35.0) | 332 (48.6) | 40 (30.3) | 451 (53.0) | ||||
| Rank | ||||||||
| Junior enlisted | 74 (40.9) | 407 (58.9) | 30.6 (2) | <0.001 | 73 (55.3) | 504 (58.3) | 10.8 (2) | 0.005 |
| Non-commissioned officer | 80 (44.2) | 245 (35.5) | 41 (31.1) | 309 (35.8) | ||||
| Officer | 27 (14.9) | 39 (5.6) | 18 (13.6) | 51 (5.9) | ||||
| Years in service | ||||||||
| Up to 4 | 74 (43.5) | 371 (53.9) | 20.8 (2) | <0.001 | 52 (43.7) | 516 (59.9) | 26.3 (2) | <0.001 |
| 5-12 | 88 (51.8) | 235 (34.2) | 66 (55.5) | 283 (32.9) | ||||
| 13 or more | 8 (4.7) | 82 (11.9) | 1 (0.84) | 62 (7.2) | ||||
| Deployments to Iraq and Afghanistan | ||||||||
| One | 107 (59.1) | 424 (61.1) | 18.2 (2) | <0.001 | 101 (76.5) | 558 (64.4) | 7.7 (2) | 0.021 |
| Two | 49 (27.1) | 235 (33.9) | 28 (21.2) | 287 (33.1) | ||||
| Three or more | 25 (13.8) | 35 (5.0) | 3 (2.3) | 21 (2.4) | ||||
| Career intentions staying in service | 109 (62.6) | 247 (36.4) | 32.3 (1) | <0.001 | 56 (44.8) | 256 (30.1) | 10.9 (1) | 0.001 |
a. Numbers may not add up to total because of missing values.
b. The response option of being ‘in long-term relationship’ was only asked in the UK questionnaire.
The stratified analyses of health outcomes by high- and low-levels of combat exposure suggested that there were interaction effects between sample and combat exposure. There was a small but significant interaction term for sample and combat exposure for the OLS regression of PCL total score (regression coefficient 0.83, 95% CI 0.74-0.91) but the interaction term did not reach statistical significance for any other outcome (PCL-50: OR = 1.06, 95% CI 0.90-1.25; PCL-DSM-IV: OR = 0.99, 95% CI 0.35-2.75; hazardous alcohol misuse: OR = 1.09, 95% CI 0.99-1.19; aggressive behaviour: OR = 1.09, 95% CI 0.98-1.21; physical symptoms: OR = 1.05, 95% CI 0.94 -1.18).
Table 3 Combat exposuresFootnote a
| UK v. USA | ||||
|---|---|---|---|---|
| UK (n = 313), n (%) | USA (n = 1560), n (%) | χ2 (d.f.) | P | |
| Type of exposure | ||||
| Small arms fire | 191 (64.1) | 1054 (69.6) | 3.5 (1) | 0.06 |
| Handled human remains | 44 (14.8) | 646 (42.9) | 82.7 (1) | <0.001 |
| Dead/injured friendly forces | 177 (59.2) | 960 (62.2) | 0.9 (1) | 0.332 |
| Hostility from civilians | 168 (56.6) | 787 (51.0) | 3.1 (1) | 0.077 |
| Threatening situation unable to respond | 88 (29.4) | 691 (44.8) | 24.2 (1) | <0.001 |
| Directing fire at enemy | 67 (22.6) | 753 (48.8) | 68.7 (1) | <0.001 |
| Clearing/searching buildings | 110 (36.7) | 778 (50.3) | 18.6 (1) | <0.001 |
| Artillery/rocket/mortar fire | 301 (98.7) | 1319 (85.3) | 41.9 (1) | <0.001 |
| Mate/buddy near you injured | 71 (23.9) | 375 (24.3) | 0.0 (1) | 0.884 |
| Sniper fire | 91 (30.6) | 661 (42.9) | 14.6 (1) | <0.001 |
| Aid to wounded | 74 (24.8) | 439 (28.4) | 1.7 (1) | 0.193 |
| Exposure frequency (sum of exposure types),Footnote b median (IQR) | 4 (2-6) | 5 (2-9) | –4.2Footnote c | <0.001 |
a. Numbers may not add up to total because of missing values.
b. Combat exposure range: 0-11.
c. Wilcoxon rank-sum test for difference.
Adjustment for combat exposures appeared to account for the difference between the UK and US samples in prevalence of probable PTSD based on both the PCL-50 definition and PCL-DSM-IV. However, the confidence intervals for the comparisons on the PCL-DSM-IV definition only just included one, suggesting that a real difference might still be present (Table 6). There was a significant difference between the UK and US samples in the average PCL total score, with the US sample reporting greater mean scores in both the high- (UK adjusted mean: 26.9, 95% CI 26.1-27.8, US adjusted mean: 35.5, 95% CI 35.2-35.8) and low-combat exposure groups (UK adjusted mean: 22.9, 95% CI 22.4-23.4; US adjusted mean: 26.3, 95% CI 26.1-26.6); this difference remained significant after full adjustment. Combat exposure was the strongest independent predictor of PCL total score in all models, as measured by the standardised beta coefficients (data not shown). Officer rank was found to be a protective factor for the three PTSD outcomes in the high-combat exposure group (data not shown but available from the authors on request).
Table 4 Probable post-traumatic stress disorder (PTSD), stratified by low- and high-combat exposure

| Low-combat exposure | High-combat exposures | |||||||
|---|---|---|---|---|---|---|---|---|
| UK (n = 181) | USA (n = 694) | UK v. USA | UK (n = 132) | USA (n = 866) | UK v. USA | |||
| n (%) | n (%) | χ2 (d.f.) | P | n (%) | n (%) | χ2 (d.f.) | P | |
| PCL-50 cut-off, n (%) | 7 (3.9) | 24 (3.6) | 0.04 (1) | 0.838 | 13 (9.9) | 161 (19.4) | 7.0 (1) | 0.008 |
| PCL-DSM-IV, n (%) | 6 (3.4) | 56 (8.4) | 5.2 (1) | 0.022 | 15 (11.4) | 207 (25.0) | 11.9 (1) | 0.001 |
| PCL total score,Footnote a mean (95% CI) | 22.8 (21.4-24.2) | 26.4 (25.6-27.2) | –4.12 (846)Footnote b | <0.001 | 26.6 (24.4-28.7) | 35.7 (34.6-36.7) | –6.43 (959)Footnote b | <0.001 |
PCL, PTSD checklist.
a. Unadjusted for demographic differences between the two samples. Numbers may not add up to total because of missing values.
b. t-test for difference.
Table 5 Hazardous drinking and aggression outcomes, stratified by low- and high-combat exposureFootnote a
| Low-combat exposure | High-combat exposure | |||||||
|---|---|---|---|---|---|---|---|---|
| UK (n = 181) | USA (n = 694) | UK v. USA | UK (n = 132) | USA (n = 866) | UK v. USA | |||
| n (%) | n (%) | χ2 (d.f.) | P | n (%) | n (%) | χ2 (d.f.) | P | |
| How often have drink of alcohol? | ||||||||
| Never | 11 (6.2) | 86 (12.5) | 16.6 (4) | 0.002 | 12 (9.3) | 69 (8.0) | 6.0 (4) | 0.199 |
| Monthly | 23 (12.9) | 90 (13.1) | 14 (10.9) | 107 (12.4) | ||||
| 2-4 times a month | 42 (23.6) | 226 (32.8) | 34 (26.4) | 238 (27.7) | ||||
| 2-3 times a week | 72 (40.5) | 203 (29.5) | 51 (39.5) | 265 (30.8) | ||||
| 4 or more times a week | 30 (16.9) | 84 (12.2) | 18 (14.0) | 181 (21.1) | ||||
| How many drinks/units on typical day of drinking? | ||||||||
| 1 or 2 | 25 (14.1) | 279 (40.4) | 130.4 (4) | <0.001 | 23 (18.0) | 258 (30.2) | 83.8 (4) | <0.001 |
| 2 to 4 | 26 (14.7) | 143 (20.7) | 8 (6.3) | 186 (21.8) | ||||
| 5 or 6 | 23 (13.0) | 121 (17.5) | 15 (11.7) | 149 (17.4) | ||||
| 7 to 9 | 24 (13.6) | 77 (11.2) | 16 (12.5) | 117 (13.7) | ||||
| 10 or more | 79 (44.6) | 70 (10.1) | 66 (51.6) | 145 (17.0) | ||||
| How often have six or more drinks/units on one occasion? | ||||||||
| Never | 20 (11.3) | 174 (25.3) | 53.8 (4) | <0.001 | 17 (13.2) | 157 (18.3) | 12.9 (4) | 0.012 |
| Less than monthly | 28 (15.8) | 198 (28.8) | 22 (17.1) | 209 (24.4) | ||||
| Monthly | 39 (22.0) | 142 (20.6) | 34 (26.4) | 184 (21.5) | ||||
| Weekly | 81 (45.8) | 164 (23.8) | 44 (34.1) | 274 (32.0) | ||||
| Daily/almost daily | 9 (5.1) | 10 (1.5) | 12 (9.3) | 33 (3.9) | ||||
| AUDIT-C 4/5 cut-off | 153 (86.0) | 461 (66.8) | 25.1 (1) | <0.001 | 111 (86.1) | 641 (74.5) | 8.2 (1) | 0.004 |
| AUDIT-C 10 cut-off | 61 (34.3) | 58 (8.4) | 80.0 (1) | <0.001 | 43 (33.3) | 141 (16.4) | 21.3 (1) | <0.001 |
| Anger | ||||||||
| Angry at someone, yell or shout | 128 (71.5) | 459 (66.5) | 1.6 (1) | 0.204 | 97 (73.5) | 701 (81.3) | 4.4 (1) | 0.035 |
| Angry at someone, kick, smash, punch wall | 52 (29.1) | 179 (25.9) | 0.7 (1) | 0.396 | 49 (37.1) | 353 (40.9) | 0.7 (1) | 0.409 |
| Threaten someone with physical violence | 48 (27.0) | 119 (17.3) | 8.5 (1) | 0.003 | 50 (37.9) | 272 (31.6) | 2.1 (1) | 0.151 |
| Fight with someone and hit the person | 31 (17.3) | 53 (7.7) | 15.2 (1) | <0.001 | 25 (18.9) | 152 (17.6) | 0.1 (1) | 0.715 |
AUDIT, Alcohol Use Disorders Identification Test - Consumption subscale.
a. Unadjusted for demographic differences between the two samples. Numbers may not add up to total because of missing values.
The UK sample reported a significantly higher prevalence of hazardous alcohol use than the US sample, in both the low- and high-combat exposure groups, that remained significant after adjusting for combat exposures and sociodemographic and military characteristics.
The UK sample reported a higher prevalence of aggressive behaviour in the low-combat exposure group. This remained significant after adjustment for hazardous alcohol consumption, combat exposures and sociodemographics and military characteristics. There was no difference between the UK and US samples in aggressive behaviour in the high-combat exposure group. Hazardous alcohol consumption was also associated with aggressive behaviour, and combat exposure was associated with aggressive behaviour in the high-combat but not in the low-combat exposure group.
There was no difference between the UK and the US sample in multiple physical symptoms. Combat exposure was associated with multiple physical symptoms in the high-combat but not in the low-combat exposure group.
Discussion
Main findings
This is the first study to combine post-deployment survey data from independent studies of US and UK military personnel who deployed to Iraq. Differences in the level of combat exposure explain most of the differences in reported prevalence of PTSD, although a cohort effect in PCL total score remained significant independent of combat exposure, with the US sample reporting a greater PCL score. Although the prevalence of hazardous alcohol use was high in both US and UK participants, cohort differences in hazardous alcohol use and aggression remained significant after controlling for combat exposure and demographic variables, with the UK reporting higher levels of alcohol misuse.
Table 6 Logistic regression and ordinary least squares regression models of the association between cohort and combat exposure with the health outcomes, stratified by low- and high-combat exposureFootnote a
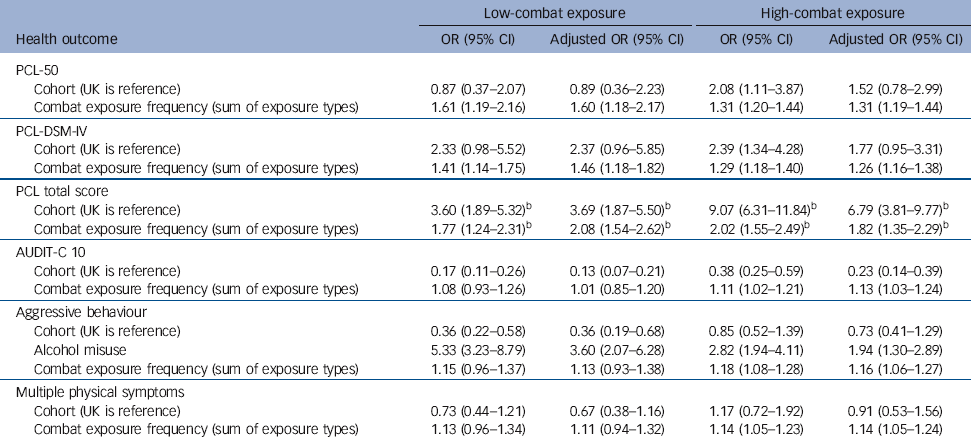
| Low-combat exposure | High-combat exposure | |||
|---|---|---|---|---|
| Health outcome | OR (95% CI) | Adjusted OR (95% CI) | OR (95% CI) | Adjusted OR (95% CI) |
| PCL-50 | ||||
| Cohort (UK is reference) | 0.87 (0.37-2.07) | 0.89 (0.36-2.23) | 2.08 (1.11-3.87) | 1.52 (0.78-2.99) |
| Combat exposure frequency (sum of exposure types) | 1.61 (1.19-2.16) | 1.60 (1.18-2.17) | 1.31 (1.20-1.44) | 1.31 (1.19-1.44) |
| PCL-DSM-IV | ||||
| Cohort (UK is reference) | 2.33 (0.98-5.52) | 2.37 (0.96-5.85) | 2.39 (1.34-4.28) | 1.77 (0.95-3.31) |
| Combat exposure frequency (sum of exposure types) | 1.41 (1.14-1.75) | 1.46 (1.18-1.82) | 1.29 (1.18-1.40) | 1.26 (1.16-1.38) |
| PCL total score | ||||
| Cohort (UK is reference) | 3.60 (1.89-5.32)Footnote b | 3.69 (1.87-5.50)Footnote b | 9.07 (6.31-11.84)Footnote b | 6.79 (3.81-9.77)Footnote b |
| Combat exposure frequency (sum of exposure types) | 1.77 (1.24-2.31)Footnote b | 2.08 (1.54-2.62)Footnote b | 2.02 (1.55-2.49)Footnote b | 1.82 (1.35-2.29)Footnote b |
| AUDIT-C 10 | ||||
| Cohort (UK is reference) | 0.17 (0.11-0.26) | 0.13 (0.07-0.21) | 0.38 (0.25-0.59) | 0.23 (0.14-0.39) |
| Combat exposure frequency (sum of exposure types) | 1.08 (0.93-1.26) | 1.01 (0.85-1.20) | 1.11 (1.02-1.21) | 1.13 (1.03-1.24) |
| Aggressive behaviour | ||||
| Cohort (UK is reference) | 0.36 (0.22-0.58) | 0.36 (0.19-0.68) | 0.85 (0.52-1.39) | 0.73 (0.41-1.29) |
| Alcohol misuse | 5.33 (3.23-8.79) | 3.60 (2.07-6.28) | 2.82 (1.94-4.11) | 1.94 (1.30-2.89) |
| Combat exposure frequency (sum of exposure types) | 1.15 (0.96-1.37) | 1.13 (0.93-1.38) | 1.18 (1.08-1.28) | 1.16 (1.06-1.27) |
| Multiple physical symptoms | ||||
| Cohort (UK is reference) | 0.73 (0.44-1.21) | 0.67 (0.38-1.16) | 1.17 (0.72-1.92) | 0.91 (0.53-1.56) |
| Combat exposure frequency (sum of exposure types) | 1.13 (0.96-1.34) | 1.11 (0.94-1.32) | 1.14 (1.05-1.23) | 1.14 (1.05-1.24) |
PCL, post-traumatic stress disorder (PTSD) Checklist; AUDIT-C, Alcohol Use Disorders Identification Test - Consumption subscale.
a. Adjusted odds ratio (OR) is adjusted for age, rank, years in service, marital status and total number of deployments to Iraq and Afghanistan.
b. Ordinary least squares regression coefficient (95% CI).
PTSD
Previous research on PTSD in personnel deployed to Iraq or Afghanistan has suggested that prevalence is greater in US military personnel than in UK personnel. Reference Sundin, Fear, Iversen, Rona and Wessely6 The prevalence of PTSD in UK studies of Iraq and Afghanistan deployed personnel have been reported to range between 3 and 7%, whereas US studies have reported higher prevalence, typically between 9 and 20%. Reference Richardson, Frueh and Acierno33,Reference Wells, Miller, Adler, Engel, Smith and Fairbank34 However, these studies did not compare prevalence directly after controlling for combat exposure or sociodemographic variables known to be associated with PTSD. The findings presented in this study are consistent with a recent meta-analysis that showed comparable results when studies involving combat infantry units were grouped separately from population-level studies involving both infantry and support units. Reference Kok, Herrell, Thomas and Hoge23
Hazardous alcohol use
Hazardous alcohol use is a concern for the armed forces in both the USA and UK, and research has shown that alcohol misuse in the US military has increased over the past decade, from 15% in 1988-1998 to 20% in 1998-2008. Reference Bray, Pemberton, Lane, Hourani, Mattiko and Babeu35 Studies have also found that deployment to Iraq and Afghanistan is associated with increased risk of hazardous alcohol use for both UK and US personnel. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1,Reference Hoge, Castro, Messer, McGurk, Cotting and Koffman2,Reference Browne, Iversen, Hull, Workman, Barker and Horn14,Reference Hawkins, Lapham, Kivlahan and Bradley36 The high prevalence of alcohol misuse found in this study is in line with previous research. Studies from the USA have generally reported lower prevalence and studies that have used the AUDIT-C report prevalence between 22 and 41%. Reference Hawkins, Lapham, Kivlahan and Bradley36-Reference Calhoun, Elter, Jones, Kudler and Straits-Troster38 Thus, our finding of a higher prevalence of hazardous alcohol use among UK military is supported by previous research, although this is the first study to directly compare the prevalence in UK and US military personnel deployed to Iraq. Research has also shown that alcohol misuse is more prevalent in the armed forces compared with the UK and US general population, although this is not a universal finding. Reference Fear, Iversen, Meltzer, Workman, Hull and Greenberg17,Reference Bray, Pemberton, Hourani, Witt, Olmsted and Brown39,Reference Ramchand, Miles, Schell, Jaycox, Marshall and Tanielian40 The higher prevalence of alcohol misuse in UK personnel may be partly explained by the differences in the approach to management of alcohol misuse in the two militaries. In the US, tolerance for alcohol-related incidents in military personnel has decreased over the years, and there is both active screening for alcohol-related problems on post-deployment surveys and a military-wide campaign to reduce alcohol-related behaviours. Any alcohol-related incident, such as driving or showing up at work under the influence, is grounds for immediate commander-directed counselling and potentially separation from service if the service member does not comply with treatment. Likewise, in the UK armed forces, ‘excessive’ consumption of alcohol is not tolerated and is considered incompatible with military service and serious misuse of alcohol may ultimately result in discharge from the service. However, there is no formal command-directed alcohol treatment programme and the UK armed forces are more likely to argue that moderate use of alcohol may be associated with some benefits, such as encouraging unit cohesion. Reference Browne, Iversen, Hull, Workman, Barker and Horn14 It is possible that differences in prevalence of hazardous alcohol use reflect different cultural attitudes towards reporting of alcohol use.
Aggressive behaviour
The difference in aggressive behaviour between UK and US personnel who reported low levels of combat exposures might be expected with the higher prevalence of hazardous alcohol use among the UK military. However, although hazardous alcohol use was associated with more aggressive behaviour, adjustment for hazardous alcohol use did not remove the association for more aggressive behaviour among the UK military. Our finding that there was no difference in aggressive behaviour between UK and US personnel who reported higher levels of combat exposures is likely to reflect the well-established link between high combat exposure and post-deployment aggression. Reference MacManus, Dean, Al Bakir, Iversen, Hull and Fahy22,Reference Wright, Foran, Wood, Eckford and McGurk41
Limitations
The principal limitation of this study is the reliance on self-report survey data and research has shown that combat exposure reports may be biased by PTSD symptom severity. Reference Brennen, Dybdahl and Kapidzic42-Reference Wessely, Unwin, Hotopf, Hull, Ismail and Nicolaou44 The studies used standardised validated measures to assess key health outcomes, including the PCL and the AUDIT-C, and used comparable questions on physical symptoms and aggressive behaviour. The study included active component military personnel deployed to the same country during a similar time frame, and used similar methods of non-anonymous confidential reporting, to further enhance comparability. The strict requirement to select comparable samples reduced sample size and thereby statistical power; nonetheless, the final sample of over 1800 respondents is reasonably powered to detect meaningful differences. Furthermore, the findings were comparable with those of a recent meta-analysis. Reference Kok, Herrell, Thomas and Hoge23 However, because of the small UK sample within this study and the low prevalence of PTSD in this population, it is possible that the study lacked power to detect a modest difference in PTSD prevalence. There was some indication of a higher adjusted prevalence of probable PTSD among the US military, based on the PCL with a DSM-IV definition, although this did not reach statistical significance. In contrast, the difference in PCL total score remained significant after adjusting for combat exposures and sociodemographics and military factors.
Another limitation of this study is the measure of combat exposures, and although we were able to adjust for a range of combat exposures on deployment we were not able to assess the severity or frequency of exposures. The samples included in this study were solely active duty personnel with recent deployments to Iraq. We were not able to adjust for the time from return from deployment to assessment and have therefore not considered time trends, such as the increase in rates of mental health problems that takes place in the months after deployment in US personnel, but seems to be less marked in UK personnel. Using a similar comparative strategy but in different sample frames might be a useful way of studying these apparent differences in a future study. We were also not able to examine childhood adversity, which is an important predictive factor that has consistently been shown to be associated with mental health problems. Nonetheless, we were able to take account of several covariates including combat experiences and a range of sociodemographic and military characteristics and adjustment for these accounted for differences in prevalence of PTSD.
Deployment to Iraq is associated with mental health problems among military personnel; including risk of PTSD, hazardous alcohol use and aggressive behaviour. Reference Fear, Jones, Murphy, Hull, Iversen and Coker1,Reference Thomas, Wilk, Riviere, McGurk, Castro and Hoge10,Reference Jakupcak, Conybeare, Phelps, Hunt, Holmes and Felker45-Reference Rona, Hooper, Jones, Iversen, Hull and Murphy47 Although unadjusted prevalence of PTSD tends to be higher among US military compared with UK military, adjusting for covariates may explain this difference. In particular, the high level of combat exposures reported in the US military accounted for most of the difference in prevalence of probable PTSD. We also found that prevalence of hazardous alcohol use differs between UK and US military, with higher prevalence among the UK military. In contrast to the difference in probable PTSD, adjusting for combat experiences and sociodemographic differences did not account for the disparate prevalence of hazardous alcohol consumption.
Implications
Overall, the results demonstrate that there are similarities as well as differences between the UK and US armed forces both in terms of deployment-related health outcomes and the risk factors associated with these outcomes. Recent US trials have demonstrated that post-deployment mental health training can reduce these negative outcomes and a UK training programme based on the US training model also found positive effects, although only for hazardous alcohol use. Reference Mulligan, Fear, Jones, Alvarez, Hull and Naumann12,Reference Adler, Bliese, McGurk, Hoge and Castro48,Reference Castro, Adler, McGurk and Bliese49 This shows that post-deployment mental health training can successfully target the key mental health problems associated with deployment in both nations. Such results underscore the feasibility of brief interventions to reduce the negative impact of deployment, and combat experiences in particular, on subsequent mental health adjustment, and suggest lessons learned from the UK and US are relevant to both nations.
Funding
J.S., N.T.F., N.G. and S.W. are based at King's College London, which receives funding from the UK Ministry of Defence. US funding for this work comes from the US Army's Military Operational Medicine Research Program.
Acknowledgements
This study was conducted under a cooperative research agreement between King’s College London and Walter Reed Army Institute of Research, US Army Medical Research and Materiel Command. We thank Colonel Carl Castro for his vision and support.









eLetters
No eLetters have been published for this article.