‘No head injury is too trivial to ignore’ (Hippocrates, 460–377 bc, in Ingebrigsten (Reference Ingebrigsten1998))
Post-concussion syndrome has presented clinicians with controversy and intrigue for at least 130 years. Its symptoms, which often follow uncomplicated mild head injury (post-traumatic amnesia <1h, Glasgow Coma Scale score 13–15, loss of consciousness <15 min) and moderate head injury (post-traumatic amnesia 1–24 h, Glasgow Coma Scale score 9–12, loss of consciousness 15 min to 6 h), commonly include headache, dizziness, fatigue, poor memory, poor concentration, irritability, depression, sleep disturbance, frustration, restlessness, sensitivity to noise, blurred vision, double vision, photophobia, nausea and tinnitus (Reference KingKing, 1997). Debate and argument have always plagued this syndrome, but research over the past decade or so has helped to clarify some of the areas of dispute and some interventions have been developed and evaluated. What follows is an attempt to illuminate the syndrome in the light of these developments.
EPIDEMIOLOGY AND NATURAL RECOVERY
The number of people who sustain a mild head injury and experience subsequent post-concussion symptoms is very high. In Great Britain each year, 250–300 hospital admissions per 100 000 of the population involve head injury, of which only 8% are severe injuries and at least 75% are mild (Reference Jennett and MacmillanJennett & MacMillan, 1981). The number of mild head injuries that pass through accident and emergency departments without admission is 4–8 times this number. Many, if not the majority of those with mild head injury experience no discernible symptoms whatsoever, but at least half experience some post-concussion symptoms. Most recover completely within 3 months of injury, but around a third have some persisting symptoms beyond this time. Around 8% have significant symptoms at 1 year and in some cases these symptoms are possibly permanent (Reference BinderBinder, 1997). Quite clearly, mild head injury is not always a mild experience.
NEUROPSYCHOLOGICAL IMPAIRMENT
A consistent feature of post-concussion syndrome is the correlation between the severity of symptoms and the severity of neuropsychological impairments in speed of information processing. These impairments tend to improve in line with symptomatic recovery over 3 months following injury, and where symptoms do persist at 6 months these cognitive deficits also tend to remain (Reference Bohnen, Twijnstra and JollesBohnen et al, 1992). Verbal and visuospatial short-term and long-term impairments are also a consistent feature of the syndrome, and these, too, typically recover over 3 months following injury. These impairments do not, however, correlate well with the severity of symptomatic presentation. Measures of other cognitive domains (e.g. reaction time) have so far yielded only equivocal results.
EVIDENCE FOR ORGANIC FEATURES
The extent to which the syndrome is primarily of organic or psychological origin, at any given time following injury, is a debate that is often heated, and sometimes polemical. Evidence of organic and quasi-organic processes involved in at least some presentations of post-concussion syndrome includes the following:
-
(a) post-mortem studies demonstrating diffuse microscopic axonal injury after mild head injury in humans and animals (Reference OppenheimerOppenheimer, 1968);
-
(b) macroscopic brain lesions being evident in 8–10% of individuals who have had routine computed tomographic or magnetic resonance imaging (MRI) brain scans performed within the first few weeks of injury (Reference Sekino, Nakamura and YukiSekino et al, 1981; Reference Doezema, King and TanbergDoezema et al, 1991); these lesions predominate in frontal, temporal and deep white-matter areas, and although their existence does not correlate well with post-concussion syndrome symptoms, they too show substantial resolution over 3 months (Reference Levin, Williams and EisenbergLevin et al, 1992);
-
(c) cellular damage and metabolic abnormalities being found in frontal white matter in patients with mild head injury and normal MRI scan within the first few weeks of injury (Reference Garnett, Blamire and RajagopalanGarnett et al, 2000);
-
(d) abnormal intraparenchymal regional cerebral blood flow being found within the first few weeks of mild head injury (Reference Nedd, Sfakianakis and GanzNedd et al, 1993);
-
(e) subtle abnormalities on electroencephalographic and brain-stem evoked response measures being noted within 48 h of mild head injury (these, however, were unrelated to post-concussion symptoms or neuropsychological sequelae) (Reference Schoenhuber, Gentilini, Levin, Eisenberg and BentonSchoenhuber & Gentilini, 1989);
-
(f) abnormal regional cerebral blood flow and reduced glucose metabolism in anterior and posterior temporal areas being found in subgroups of patients with persistent and disabling post-concussion syndrome up to 5 years after injury (Reference Varney, Bushnell and NathanVarney et al, 1995).
Other evidence suggestive of organic factors includes the following: slower recovery with increased age (cut-off at around 40 years) (Reference BinderBinder, 1986); poorer outcome and a cumulative effect of previous and successive mild head injuries (Reference Gronwall and WrightsonGronwall & Wrightson, 1975); and poorer outcome with a history of alcohol or substance misuse (Reference LishmanLishman, 1988).
EVIDENCE FOR INVOLVEMENT OF PSYCHOLOGICAL PROCESSSES
Evidence for psychological features includes the following:
-
(a) there is worse outcome where there is pre-existing psychopathological disorder (Reference LishmanLishman, 1988);
-
(b) the best early predictors of persisting post-concussion symptoms are psychological factors;
-
(c) there are high rates of comorbidity of anxiety and depression symptoms with post-concussion symptoms and many of these symptoms are identical (Reference KingKing, 1997);
-
(d) stress exacerbates post-concussion syndrome;
-
(e) there is a higher prevalence of post-concussion syndrome in women, which is in line with a higher prevalence of psychopathological presentations in women (Reference KingKing, 1997);
-
(f) there is an association between severity of post-concussion symptoms or time off work after mild head injury and seeking compensation (Reference Binder and RohlingBinder & Rohling, 1996); it should be noted, however, that although twice as many patients seeking compensation have post-concussion symptoms compared with those who are not, few show significant improvement following settlement, even a year afterwards.
TREATMENT AND INTERVENTION
Papers describing post-concussion syndrome and its assessment vastly outweigh those investigating intervention and treatment. The majority of reported interventions are primarily psychological and have the central aim of minimising the vicious circle of stress and post-concussion symptoms becoming mutually exacerbating, through education, support and reassurance (Reference King, Crawford and WendenKing et al, 1997). Treatment typically involves:
-
(a) normalising post-concussion symptoms and emphasising their non-malignant nature;
-
(b) providing an optimistic prognosis and estimate of likely recovery time;
-
(c) explaining the nature of, and how to cope with, impairments of speed of information processing;
-
(d) describing how symptoms can be used as a ‘temperature gauge’ indicating when to increase or decrease demands and take breaks;
-
(e) facilitating graduated return to work and other premorbid activities when sufficient recovery has occurred;
-
(f) explaining the nature of, and how to minimise, the vicious circle of stress and post-concussion symptoms becoming mutually exacerbating.
There is good evidence from randomised controlled trials that early intervention within the first few weeks of mild head injury does significantly reduce post-concussion symptoms and limit the emergence of persisting problems (Reference Wade, King and WendenWade et al, 1998). A single hour-long assessment and treatment session is usually sufficient to achieve this effect, and there is some evidence that education plus reassurance has a superior outcome to education alone (Reference Alves, Macciocchi and BarthAlves et al, 1993). There is, however, no reliable evidence base for guiding the management of post-concussion syndrome when it persists, and there are virtually no systematic follow-ups of mild head injury and post-concussion beyond 1 year after injury. These areas need to be the focus of future research.
CONCLUSIONS
Mild organic dysfunction is not uncommon in the early days following mild head injury and during the subsequent few months. During this time psychological features can develop and/or pre-existing psychological vulnerabilities may be activated. The effectiveness of brief, early psychological intervention may predominantly stem from minimising the impact of unhelpful beliefs and behaviours surrounding the syndrome.
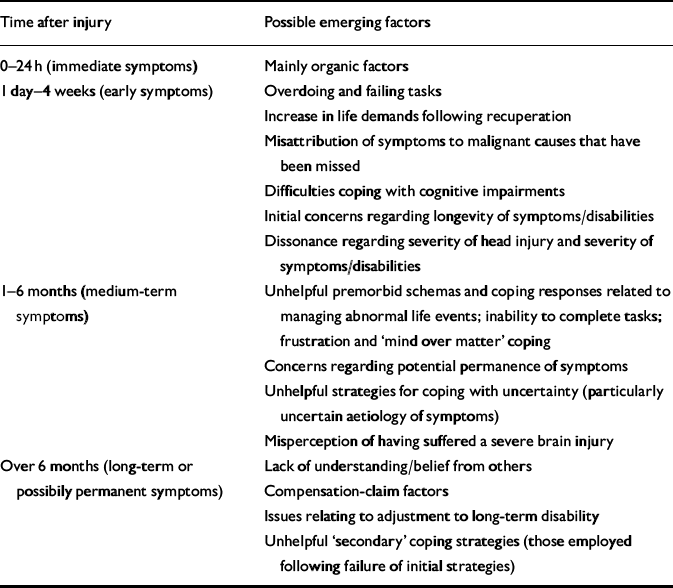
When post-concussion syndrome persists, psychological features will entirely account for the symptoms in some individuals, and organic or quasi-organic features will entirely account for the symptoms in others. Because the vast majority of patients with uncomplicated mild head injury will not receive extensive investigations it may be prematurely inferred that organic processes are not present, and therefore psychological processes must be the only, or predominant, cause of the syndrome. Conversely, in those without clear and conclusive evidence of psychopathological disorder it may be prematurely inferred that organic or quasi-organic processes are responsible. The vast majority of presentations of post-concussion syndrome, however, are unlikely to be at these extremes. Similar symptoms, but with different aetiological processes, will present in different cases and possibly within a single individual at different times following injury. It is quite possible that, at different times after injury, different ‘windows of vulnerability’ emerge which increase the role of psychological factors, for example when the patient begins to doubt the possibility of recovery or when issues surrounding compensation claims predominate (Table 1). In any given case the relative contribution of these processes will have to be gauged from both positive and negative evidence of organic and psychological features. This has to be done without losing sight of the complex interactional effects between these factors. It is therefore essential that patients with persisting and disabling post-concussion symptoms receive individualised formulations of their particular problems.
Table 1 ‘Windows of vulnerability’ in post-concussion syndrome
| Time after injury | Possible emerging factors |
|---|---|
| 0-24 h (immediate symptoms) | Mainly organic factors |
| 1 day-4 weeks (early symptoms) | Overdoing and failing tasks |
| Increase in life demands following recuperation | |
| Misattribution of symptoms to malignant causes that have been missed | |
| Difficulties coping with cognitive impairments | |
| Initial concerns regarding longevity of symptoms/disabilities | |
| Dissonance regarding severity of head injury and severity of symptoms/disabilities | |
| 1-6 months (medium-term symptoms) | Unhelpful premorbid schemas and coping responses related to managing abnormal life events; inability to complete tasks; frustration and ‘mind over matter’ coping |
| Concerns regarding potential permanence of symptoms | |
| Unhelpful strategies for coping with uncertainty (particularly uncertain aetiology of symptoms) | |
| Misperception of having suffered a severe brain injury | |
| Over 6 months (long-term or possibily permanent symptoms) | Lack of understanding/belief from others |
| Compensation-claim factors | |
| Issues relating to adjustment to long-term disability | |
| Unhelpful ‘secondary’ coping strategies (those employed following failure of initial strategies) |
DECLARATION OF INTEREST
None.




eLetters
No eLetters have been published for this article.