In contrast to the legal position in relation to the provision of treatment for a physical disorder, the Mental Health Act 1983 in England and Wales attributes little significance to the patient's capacity to consent. It provides a legal framework for the detention in hospital of individuals with a mental disorder and for their treatment for that disorder, irrespective of their capacity to withhold consent. In only a few specific situations is the assessment of capacity required: continuation of treatment beyond 3 months in detained patients, electroconvulsive therapy, psychosurgery and implantation of sex hormones. Only in the last two situations is the absence of capacity or the absence of consent prohibitive of the provision of treatment (Reference Bartlett and SandlandBartlett & Sandland, 2003). Despite current debate about the place of mental capacity in mental health legislation, there is surprisingly little systematic research of the prevalence of capacity in clinical populations (Reference Szmukler and HollowaySzmukler & Holloway, 1998; Expert Committee, 1999; Reference Zigmond and HollandZigmond & Holland, 2000). One previous study described the proportion of patients lacking capacity (20%) in a sample of patients admitted for treatment to psychiatric or learning disability services, but this was limited by its small sample size (n=41) (Reference Bellhouse, Holland and ClareBellhouse et al, 2003). Other studies have compared the numbers of impaired patients in different diagnostic groups with each other and with normal controls for the components of treatment-related decisional capacity, but have not investigated global capacity judgements (Grisso & Appelbaum, Reference Grisso and Appelbaum1995a ,Reference Grisso and Appelbaum b ; Reference Grisso, Appelbaum and Hill-FotouhiGrisso et al, 1997; Reference Vollmann, Bauer and Danker-HopfeVollmann et al, 2003; Reference Palmer, Dunn and AppelbaumPalmer et al, 2004). The objectives of the current study were to determine the prevalence of psychiatric in-patients who lack capacity to make key decisions about their treatment and to establish whether mental incapacity is associated with specific demographic or clinical factors, in particular use of the Mental Health Act 1983, insight, perceived coercion, cognitive impairment and psychopathology.
METHOD
Participants
Consecutively admitted patients to three general adult psychiatric wards at the Maudsley Hospital, London, were approached for inclusion in this study over a 9-month period. These wards cover the catchment area of South Southwark, an inner-city deprived area, with an ethnically diverse population. The local research ethics committee approved the study and after complete description of the study to the participants, written informed consent was obtained. A total of 112 patients agreed to participate and all were interviewed within 9 days of admission (111 within 7 days of admission). Exclusion criteria included being unable to consent to taking part in research, being on no regular prescribed psychotropic medication or receiving medication for the sole purpose purpose of a medically assisted alcohol detoxification, and speaking no English.
Measurement of capacity
The MacArthur Competence Assessment Tool for Treatment (MacCAT–T) was administered to each patient (Reference Grisso, Appelbaum and Hill-FotouhiGrisso et al, 1997). It is a semi-structured interview that provides relevant treatment information for the patient and evaluates capacity in terms of its different components. As such it can detect impairment in four areas: the patient's understanding of the disorder and treatment-related information; appreciation of the significance of that information for the patient; the reasoning ability of the patient to compare their prescribed medication with an alternative treatment; and ability of the patient to express a choice between their recommended medication and an alternative treatment. The interview was modified slightly for our study and patients were given the option of ‘no treatment’ as the alternative to their prescribed or ‘recommended’ medication. This was to avoid confusion about the patient's current treatment and also to prevent potential problems in the relationship between the participant and the treating clinician.
Before each interview, relevant information about the patient's diagnosis, presenting symptoms and recommended treatment was obtained from the case notes and discussion with the clinical team. Where a patient was on more than one psychotropic medication, the interview focused on the medication that was judged to be the patient's main treatment. This information was disclosed to the patient during the MacCAT–T interview together with standardised information about the features, benefits and risks of the recommended treatment (based on UK Psychiatric Pharmacy Group Information leaflets; http://www.ukppg.org.uk) and of the no treatment option. After each interview the interviewer scored understanding, appreciation, reasoning and expression of choice according to MacCAT–T criteria and made a global judgement about the patient's capacity to make a treatment decision, based on information from both the MacCAT–T and a clinical interview with the patient. We used the England and Wales Draft Mental Incapacity Bill (Department for Constitutional Affairs, 2003) definition of mental incapacity in order to reach a binary (yes/no) decision.
Fifty-five patients in the present study were recruited initially for a study investigating the interrater reliability of capacity assessments (Reference Cairns, Maddock and BuchananCairns et al, 2005, this issue). These patients had been interviewed on two occasions by two separate interviewers and an excellent level of agreement for global capacity judgements was demonstrated for two separate interviews (kappa=0.82) and for the same interview, based on transcripts. One of the interviewers (R.C.) from the initial study continued to recruit patients for this study and therefore data she had collected from the first 55 patients were used for this study in preference to the data collected by the other interviewer. For the 57 cases seen only for this study, a consensus judgement was reached between the interviewer and a psychiatrist (M.H.) with an interest in mental capacity, when the judgement was felt to be difficult. In practice this amounted to eight interviews.
Other measures
Demographic and clinical information about each participant was collected from the case notes. In addition to the MacCAT–T, the Brief Psychiatric Rating Scale (BPRS) (Reference Ventura, Green and ShanerVentura et al, 1993), the Expanded Schedule for Assessment of Insight (SAI–E) (Reference Kemp, David and BlackwellKemp & David, 1997; Reference Sanz, Constable and Lopez-IborSanz et al, 1998), the Mini Mental State Examination (MMSE) (Reference Folstein, Folstein and McHughFolstein et al, 1975) and the Brief Perceived Coercion Scale (BPCS) (Reference Gardner, Hoge and BennettGardner et al, 1993) were completed for each patient. It was also noted whether the patient was documented as having delusional beliefs or experiencing auditory hallucinations at the time of admission.
The SAI–E is a semi-structured interview that measures three dimensions of insight (treatment compliance, recognition of illness, and relabelling of psychotic phenomena), as well as awareness of changes in mental functioning, of the need for treatment and of the psychosocial consequences of illness. It also includes a question on response to hypothetical contradiction. The BPCS is a sub-scale from the MacArthur Admission Experience Survey, ‘Short Form’, and asks patients to judge the degree of influence, control, choice and freedom they had about their admission to hospital.
Statistical analyses
Data analysis was performed using the Statistical Package for Social Sciences Version 11 (SPSS, 2001) and STATA (release 8.0; Stata Corporation, 2003). The prevalence figure for mental incapacity was calculated with 95% confidence intervals. Conventional bivariate methods were used to compare patients who were judged to lack capacity with those who were judged to have capacity. Logistic regression analysis was then performed to identify independent associations for incapacity. Each logistic regression model forced independent variables into a model in order to test specific hypotheses.
RESULTS
Participant characteristics
Out of 235 newly admitted patients, 189 were eligible for inclusion in the study and 112 (59.3%) agreed to take part. Out of the remaining 77, 64 (33.9%) refused to take part and 13 (6.9%) were eligible but not included because there was a high perceived risk of violence to the interviewer (9), the patient was discharged before being invited to participate (3), or the patient had absconded from the ward (1). Of the patients who were excluded, 17 were considered by medical or senior nursing staff to be too unwell to assent to taking part in research. Of these, 8 were mute and 9 had severe thought disorder or paranoid delusions. A further 24 excluded patients were on no regular prescribed medication and 5 spoke no English.
The interviewed group comprised 71 men and 41 women with a mean age of 37.2 years (s.d.=11.8). They were interviewed, on average, 3.3 days after admission. Diagnoses were made according to ICD–10 criteria (World Health Organization, 1993) by the treating clinical team and 62 participants (55.4%) had the following psychotic illnesses: schizophrenia (37), schizoaffective disorder (11) and other psychotic disorder (14). Twenty-one participants (18.8%) had a diagnosis of bipolar affective disorder, 25 (22.3%) had a diagnosis of depression and 4 (3.6%) had emotionally unstable personality disorder, borderline type. Thirty-six participants (32.1%) had been admitted under the Mental Health Act 1983 and the remaining 76 were voluntary.
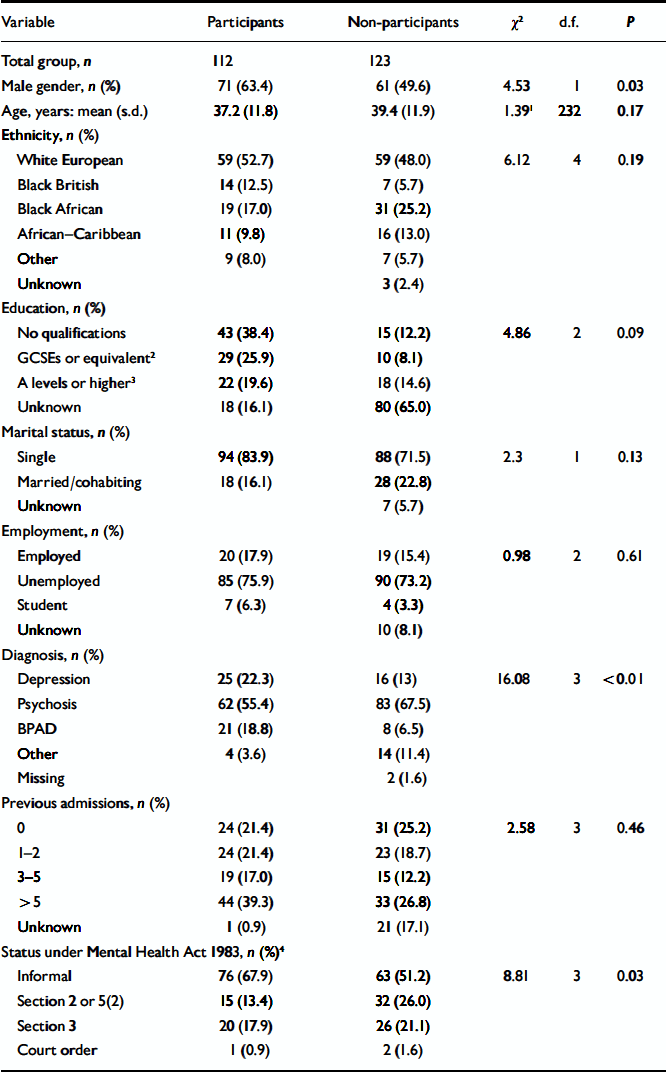
The interviewed group differed from the non-participants in terms of admission status, with higher proportions of the latter detained under the Mental Health Act 1983. A higher proportion of men agreed to take part than women and there were also differences in the distribution of psychiatric diagnoses between participants and non-participants. A comparison of the two groups is shown in Table 1.
Table 1 Comparison of participants and non-participants
| Variable | Participants | Non-participants | χ2 | d.f. | P |
|---|---|---|---|---|---|
| Total group, n | 112 | 123 | |||
| Male gender, n (%) | 71 (63.4) | 61 (49.6) | 4.53 | 1 | 0.03 |
| Age, years: mean (s.d.) Ethnicity, n (%) | 37.2 (11.8) | 39.4 (11.9) | 1.391 | 232 | 0.17 |
| White European | 59 (52.7) | 59 (48.0) | 6.12 | 4 | 0.19 |
| Black British | 14 (12.5) | 7 (5.7) | |||
| Black African | 19 (17.0) | 31 (25.2) | |||
| African—Caribbean | 11 (9.8) | 16 (13.0) | |||
| Other | 9 (8.0) | 7 (5.7) | |||
| Unknown | 3 (2.4) | ||||
| Education, n (%) | |||||
| No qualifications | 43 (38.4) | 15 (12.2) | 4.86 | 2 | 0.09 |
| GCSEs or equivalent2 | 29 (25.9) | 10 (8.1) | |||
| A levels or higher3 | 22 (19.6) | 18 (14.6) | |||
| Unknown | 18 (16.1) | 80 (65.0) | |||
| Marital status, n (%) | |||||
| Single | 94 (83.9) | 88 (71.5) | 2.3 | 1 | 0.13 |
| Married/cohabiting | 18 (16.1) | 28 (22.8) | |||
| Unknown | 7 (5.7) | ||||
| Employment, n (%) | |||||
| Employed | 20 (17.9) | 19 (15.4) | 0.98 | 2 | 0.61 |
| Unemployed | 85 (75.9) | 90 (73.2) | |||
| Student | 7 (6.3) | 4 (3.3) | |||
| Unknown | 10 (8.1) | ||||
| Diagnosis, n (%) | |||||
| Depression | 25 (22.3) | 16 (13) | 16.08 | 3 | <0.01 |
| Psychosis | 62 (55.4) | 83 (67.5) | |||
| BPAD | 21 (18.8) | 8 (6.5) | |||
| Other | 4 (3.6) | 14 (11.4) | |||
| Missing | 2 (1.6) | ||||
| Previous admissions, n (%) | |||||
| 0 | 24 (21.4) | 31 (25.2) | 2.58 | 3 | 0.46 |
| 1-2 | 24 (21.4) | 23 (18.7) | |||
| 3-5 | 19 (17.0) | 15 (12.2) | |||
| >5 | 44 (39.3) | 33 (26.8) | |||
| Unknown | 1 (0.9) | 21 (17.1) | |||
| Status under Mental Health Act 1983, n (%)4 | |||||
| Informal | 76 (67.9) | 63 (51.2) | 8.81 | 3 | 0.03 |
| Section 2 or 5(2) | 15 (13.4) | 32 (26.0) | |||
| Section 3 | 20 (17.9) | 26 (21.1) | |||
| Court order | 1 (0.9) | 2 (1.6) | |||
Ratings and predictors of incapacity
Of the participants, 49 (43.8%) (95% CI 34.6–54.0) lacked treatment-related decisional capacity, based on a judgement guided by the MacCAT–T and a clinical interview. The binary rating of capacity was based on the definition of ‘inability to make decisions’ proposed in the Draft Mental Incapacity Bill (England and Wales) (Department for Constitutional Affairs, 2003) (now the Mental Capacity Act 2005).
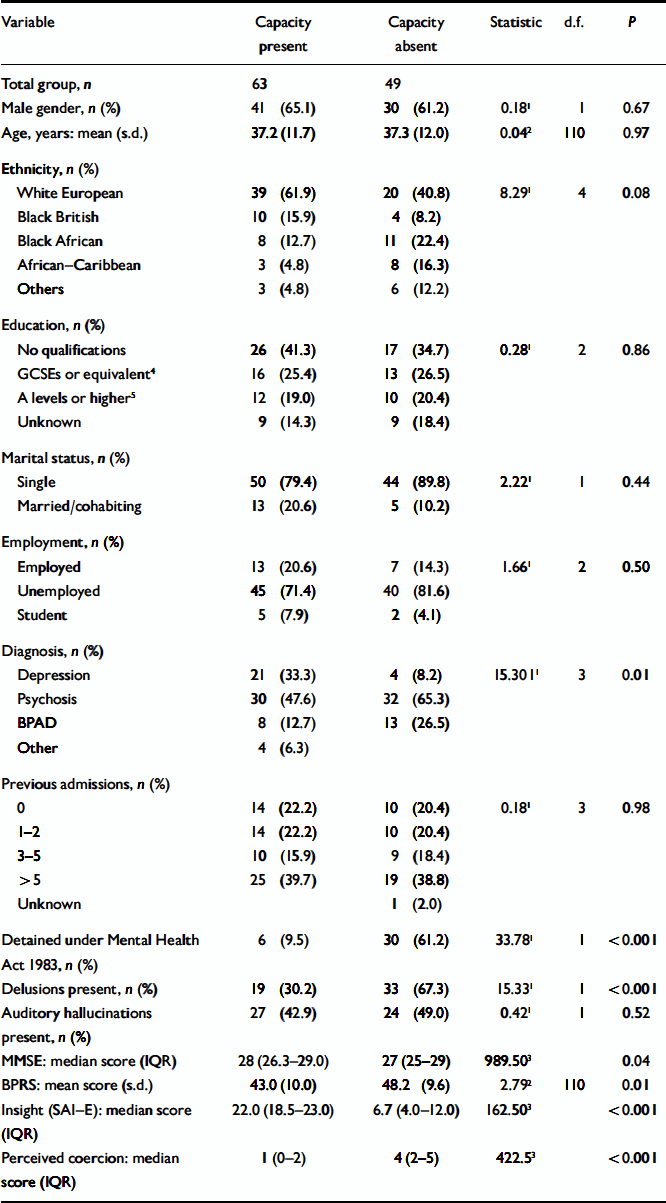
The socio-demographic and clinical characteristics of participants with and without mental capacity are shown in Table 2. Those lacking capacity were more likely to have a psychotic illness or bipolar affective disorder and to be Black African or African–Caribbean. They were also more likely to be detained under the Mental Health Act 1983, to experience delusions, to have higher scores on the BPRS and BPCS and to score significantly less on the MMSE and SAI–E. There were no statistically significant differences between the groups in terms of age, gender, educational level, marital status, employment status, number of previous admissions or whether the individuals experienced auditory hallucinations.
Table 2 Comparison of individuals with and without mental capacity to make a treatment decision
| Variable | Capacity present | Capacity absent | Statistic | d.f. | P |
|---|---|---|---|---|---|
| Total group, n | 63 | 49 | |||
| Male gender, n (%) | 41 (65.1) | 30 (61.2) | 0.181 | 1 | 0.67 |
| Age, years: mean (s.d.) | 37.2 (11.7) | 37.3 (12.0) | 0.042 | 110 | 0.97 |
| Ethnicity, n (%) | |||||
| White European | 39 (61.9) | 20 (40.8) | 8.291 | 4 | 0.08 |
| Black British | 10 (15.9) | 4 (8.2) | |||
| Black African | 8 (12.7) | 11 (22.4) | |||
| African—Caribbean | 3 (4.8) | 8 (16.3) | |||
| Others | 3 (4.8) | 6 (12.2) | |||
| Education, n (%) | |||||
| No qualifications | 26 (41.3) | 17 (34.7) | 0.281 | 2 | 0.86 |
| GCSEs or equivalent4 | 16 (25.4) | 13 (26.5) | |||
| A levels or higher5 | 12 (19.0) | 10 (20.4) | |||
| Unknown | 9 (14.3) | 9 (18.4) | |||
| Marital status, n (%) | |||||
| Single | 50 (79.4) | 44 (89.8) | 2.221 | 1 | 0.44 |
| Married/cohabiting | 13 (20.6) | 5 (10.2) | |||
| Employment, n (%) | |||||
| Employed | 13 (20.6) | 7 (14.3) | 1.661 | 2 | 0.50 |
| Unemployed | 45 (71.4) | 40 (81.6) | |||
| Student | 5 (7.9) | 2 (4.1) | |||
| Diagnosis, n (%) | |||||
| Depression | 21 (33.3) | 4 (8.2) | 15.3011 | 3 | 0.01 |
| Psychosis | 30 (47.6) | 32 (65.3) | |||
| BPAD | 8 (12.7) | 13 (26.5) | |||
| Other | 4 (6.3) | ||||
| Previous admissions, n (%) | |||||
| 0 | 14 (22.2) | 10 (20.4) | 0.181 | 3 | 0.98 |
| 1-2 | 14 (22.2) | 10 (20.4) | |||
| 3-5 | 10 (15.9) | 9 (18.4) | |||
| >5 | 25 (39.7) | 19 (38.8) | |||
| Unknown | 1 (2.0) | ||||
| Detained under Mental Health | 6 (9.5) | 30 (61.2) | 33.781 | 1 | <0.001 |
| Act 1983, n (%) | |||||
| Delusions present, n (%) | 19 (30.2) | 33 (67.3) | 15.331 | 1 | <0.001 |
| Auditory hallucinations present, n (%) | 27 (42.9) | 24 (49.0) | 0.421 | 1 | 0.52 |
| MMSE: median score (IQR) | 28 (26.3-29.0) | 27 (25-29) | 989.503 | 0.04 | |
| BPRS: mean score (s.d.) | 43.0 (10.0) | 48.2 (9.6) | 2.792 | 110 | 0.01 |
| Insight (SAI—E): median score (IQR) | 22.0 (18.5-23.0) | 6.7 (4.0-12.0) | 162.503 | <0.001 | |
| Perceived coercion: median score (IQR) | 1 (0-2) | 4 (2-5) | 422.53 | <0.001 |
Multivariable analyses
Because there was an apparent association (P=0.08) between Black and minority ethnic group and lack of capacity, we first explored whether this could be explained by diagnosis and/or country of birth (i.e. whether or not UK-born) using logistic regression analysis. The odds ratio for incapacity for all Black and minority ethnic groups as a single category was 2.36 (95% CI 1.10–5.05), but this became considerably smaller once diagnosis was controlled for (OR=1.59, 95% CI 0.68–3.68), and was eradicated when country of birth and diagnosis were controlled for simultaneously (OR=1.11, 95% CI 0.41–3.04). When different ethnic groups were considered, the overall significance of the effect was P=0.07 but this masked a strong, if imprecise, association between African–Caribbean ethnic group and lack of mental capacity (OR=9.75, 95% CI 1.07–89.2). This was reduced, although not eradicated, by controlling for diagnosis (OR=5.81, 95% CI 0.61–55.4). Country of birth was not controlled for in this analysis because of the large overlap in country of birth and ethnic group variables.
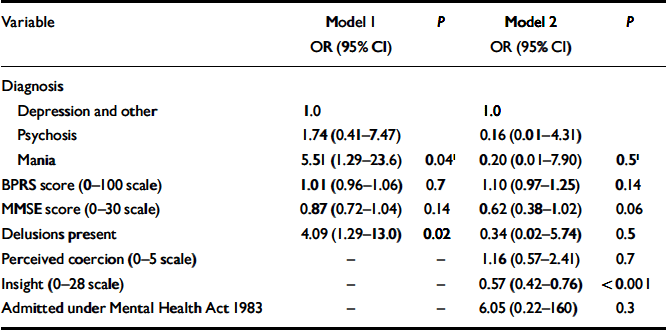
A second set of logistic regression analyses explored clinical variables. As there was considerable overlap between clinical variables (diagnosis, psychopathology such as experience of hallucinations and delusions, and scores on specific measures), we entered these variables into a logistic regression analysis shown in Table 3. In the first model, we entered diagnosis, presence of delusions, BPRS score and MMSE score. This model concentrated on the severity and type of psychopathology. Two variables were associated with incapacity – diagnosis (particularly mania or hypomania) and the presence of delusions. In the second model, which comprised diagnosis, presence of delusions, insight, perceived coercion, use of the Mental Health Act 1983, MMSE and BPRS scores, the only association which was statistically significant was insight. Those having higher insight scores were less likely to be rated as lacking capacity. There was a slighter non-significant association with MMSE, with those scoring higher being less likely to lack capacity. No other clinical variable was associated.
Table 3 Associations between psychopathology and lack of capacity
| Variable | Model 1 OR (95% CI) | P | Model 2 OR (95% CI) | P |
|---|---|---|---|---|
| Diagnosis | ||||
| Depression and other | 1.0 | 1.0 | ||
| Psychosis | 1.74 (0.41-7.47) | 0.16 (0.01-4.31) | ||
| Mania | 5.51 (1.29-23.6) | 0.041 | 0.20 (0.01-7.90) | 0.51 |
| BPRS score (0-100 scale) | 1.01 (0.96-1.06) | 0.7 | 1.10 (0.97-1.25) | 0.14 |
| MMSE score (0-30 scale) | 0.87 (0.72-1.04) | 0.14 | 0.62 (0.38-1.02) | 0.06 |
| Delusions present | 4.09 (1.29-13.0) | 0.02 | 0.34 (0.02-5.74) | 0.5 |
| Perceived coercion (0-5 scale) | — | — | 1.16 (0.57-2.41) | 0.7 |
| Insight (0-28 scale) | — | — | 0.57 (0.42-0.76) | <0.001 |
| Admitted under Mental Health Act 1983 | — | — | 6.05 (0.22-160) | 0.3 |
Out of the 63 patients who had capacity to make a treatment decision, 57 were admitted to hospital on a voluntary basis but 6 were detained under the Mental Health Act 1983. The only significant demographic or clinical differences between these two groups were that the detained patients had higher perceived coercion scores and the voluntarily admitted patients had unexpectedly higher scores of psychopathology on the BPRS. A comparison of these groups is shown in Table 4. Perceived coercion was also higher among patients who lacked mental capacity but were detained (mean score in those detained=4.0, s.d.=1.23 v. mean score for those not detained=2.4, s.d.=1.5; χ2=13.6; d.f.=5; P=0.02).
Table 4 Comparison of detained patients with capacity and voluntarily admitted patients with capacity

| Variable | Detained under Mental Health Act 1983 | Admitted voluntarily | Statistic | d.f. | P |
|---|---|---|---|---|---|
| Total group, n | 6 | 57 | |||
| Male gender, n (%) | 5 (83.3) | 36 (63.2) | 1 | 0.66 | |
| Age, years: mean (s.d.) | 34.7 (10.0) | 37.5 (11.9) | 0.552 | 61 | 0.58 |
| Ethnicity, n (%) | |||||
| White European | 1 (16.7) | 38 (66.7) | 7.983 | 4 | 0.09 |
| Black British | 2 (33.3) | 8 (14.0) | |||
| Black African | 2 (33.3) | 6 (10.5) | |||
| African—Caribbean | 1 (16.7) | 2 (3.5) | |||
| Others | 3 (5.3) | ||||
| Diagnosis, n (%) | |||||
| Depression | 21 (36.8) | 5.363 | 3 | 0.15 | |
| Psychosis | 4 (66.7) | 26 (45.6) | |||
| BPAD | 2 (33.3) | 6 (10.5) | |||
| Other | 5 (8.8) | ||||
| Previous admissions, n (%) | |||||
| 0 | 14 (24.6) | 2.023 | 3 | 0.57 | |
| 1-2 | 2 (33.3) | 12 (21.1) | |||
| 3-5 | 1 (16.7) | 9 (15.8) | |||
| >5 | 3 (50.0) | 22 (38.6) | |||
| Delusions present, n (%) | 3 (50.0) | 16 (28.0) | 1 | 0.36 | |
| Auditory hallucinations present, n (%) | 3 (50.0) | 24 (42.1) | 1 | 1.0 | |
| MMSE: median score (IQR) | 27 (25-29) | 28 (27-29) | 104.004 | 0.36 | |
| BPRS: mean score (s.d.) | 34.5 (12.9) | 43.9 (9.3) | 2.263 | 61 | 0.03 |
| Insight (SAI—E): median score (IQR) | 20.0 (14.7-23.3) | 22.0 (18.6-23.0) | 131.004 | 0.37 | |
| Perceived coercion: median score (IQR) | 5 (3-5) | 0 (0-2) | 20.04 | 0.001 |
DISCUSSION
This study suggests that lack of treatment-related decisional capacity is common, but by no means inevitable, among adult psychiatric patients who are unwell enough to require in-patient admission. Our reported prevalence of 43.8% relates closely to an estimated 40% of acutely ill medical patients who were found to lack capacity in a recent study by this group in the same geographical area (Reference Raymont, Bingley and BuchananRaymont et al, 2004). In a smaller study looking at treatment-related decisional capacity in psychiatric patients, only 20% of participants were judged to lack the capacity to consent to treatment (Reference Bellhouse, Holland and ClareBellhouse et al, 2003). Socio-demographic and clinical differences may partly explain this disparity: the present study was undertaken in a more deprived, ethnically diverse inner-city area, where a higher proportion of admissions are under the Mental Health Act 1983, than the previous study. The current estimate is likely to be conservative. Fifty-two per cent of the admitted patients were not included and, although there were few other differences between participants and non-participants, admission under the Mental Health Act 1983 and having a psychotic illness were both more common among the latter. Since we have shown that these two factors are associated with mental incapacity, it is almost certain that the true prevalence of incapacity is higher.
Factors associated with lack of capacity
The majority of patients (45 out of 49) who were judged incapable of making a treatment decision suffered from either a psychotic illness or bipolar affective disorder. We did not use a semi-structured diagnostic interview, and deliberately describe broad clinically derived diagnostic categories. The association was confirmed in regression analyses showing that mania and hypomania in particular were closely associated with incapacity, as was the experience of delusional beliefs. A similar pattern was described by Bellhouse et al (Reference Bellhouse, Holland and Clare2003) where all participants lacking capacity had a psychotic illness, although the authors made the important point that psychosis is not invariably associated with incapacity (six out of nine participants with schizophrenia had capacity to consent to treatment).
We found that Black and minority ethnic group was associated with lack of capacity, particularly in African–Caribbean participants. The effect of ethnicity may be due to several factors – most important being diagnosis. Very few (9%) individuals from Black and minority ethnic groups were hospitalised for unipolar depression, whereas this diagnosis was common in the White European group (41%). Another factor is country of birth. The group who were classified as Black British were no more likely to be categorised as lacking capacity than the White European group, suggesting that some of the effect of ethnicity may be due to different cultural understandings, such as differences in the use of language.
Predictors of capacity
A strong association was seen between lower insight scores and mental incapacity. Although the relationship between use of the Mental Health Act 1983 and insight is predictable (Reference McEvoy, Appelbaum and GellerMcEvoy et al, 1989; Reference David, Buchanan and ReedDavid et al, 1992), the relationship between mental capacity and insight has received little attention. Insight has at least three overlapping dimensions: awareness of illness, the ability to relabel unusual mental experiences as pathological, and treatment adherence (Reference DavidDavid, 1990). We suggest that there is conceptual overlap between insight and mental capacity and the respective components of each. For example, impairments in understanding, appreciation, reasoning or ability to express a choice would be reflected in one or more of the dimensions of insight. It also seems probable that the associations seen between mental incapacity and a diagnosis of psychosis or mania and with the experience of delusional beliefs are mediated through the effect of poor insight. Sanz et al (Reference Sanz, Constable and Lopez-Ibor1998) have previously shown that measures of insight relate strongly to the presence of delusions, grandiosity (inversely) and depression (positively).
Cognitive impairment has been shown to be an independent predictor of incapacity in general hospital in-patients (Reference Raymont, Bingley and BuchananRaymont et al, 2004). The results from the present study show an association between lower MMSE scores and mental incapacity that borders on statistical significance. The difference between these findings may be explained by the younger mean age of patients in this study (37.2 years) compared with a mean age of 64.2 years in the study looking at capacity in general hospital patients (Reference Raymont, Bingley and BuchananRaymont et al, 2004). Furthermore, the distribution of scores suggested a ceiling effect and hence insensitivity to potential differences. In a study of middle-aged and older out-patients with schizophrenia (mean age 50.2 years), the patients’ level of capacity (using MacCAT–T sub-scale scores) was strongly associated with cognitive test performance but not with severity of psychopathology (Reference Palmer, Dunn and AppelbaumPalmer et al, 2004). The authors suggest that their findings, although unexpected, are partly explained by the out-patient status (and therefore relative stability) of the participants and are consistent with the overall findings in functional outcome studies of schizophrenia that neuropsychological test performance tends to be a better predictor of everyday functioning than the severity of psychopathology alone (Reference GreenGreen, 1996; Reference Green, Kern and BraffGreen et al, 2000; Reference Evans, Heaton and PaulsenEvans et al, 2003). Severity of psychopathology, as measured by BPRS scores, was not closely associated with incapacity in this study although there was an association with the presence of delusions. A limitation of this study arises from using the MMSE as the sole measure of cognitive impairment: it is possible that as a result the potential association between this and incapacity may have been inadequately assessed.
Implications
We believe this study to be important because it is the first to use the MacCAT–T and a clinical interview to reach an overall judgement of capacity and describe the prevalence of mental incapacity in a consecutive sample of psychiatric patients. The consecutive sample design ensured that both voluntarily and involuntarily admitted patients with a range of psychiatric diagnoses were included. The sample was therefore reasonably representative of the heterogeneous mix of patients who require admission to a psychiatric in-patient unit. We are aware of one other study (Reference Bellhouse, Holland and ClareBellhouse et al, 2003) that was concerned with global capacity judgements in admissions to psychiatric or learning disability services but the numbers recruited for our study were larger (n=112 compared with n=41), conferring additional statistical power to our findings.
Coercion in psychiatry can be defined as any attempt to impose treatment against a patient's wishes (Reference BindmanBindman, 2004). Individuals lacking capacity were significantly more likely to be detained under the Mental Health Act 1983 and to have higher scores of perceived coercion than patients who had capacity to make treatment decisions. When the group of patients who lacked capacity was considered separately, the detained patients still experienced higher levels of coercion than voluntary patients who lacked capacity. The same pattern was seen in the group of patients with capacity (see Table 4). Unsurprisingly, involuntary admission to hospital is more closely associated with perceived coercion than the presence or absence of capacity.
Six participants with treatment-related decisional capacity had been detained under the Mental Health Act 1983. Proponents of capacity-based mental health legislation feel that the current Mental Health Act (1983) discriminates against these individuals by not respecting their wishes to refuse treatment in the way that legislation for physical illnesses allows. This group constituted 12.2% of those with treatment-related capacity and 5.4% of our sample as a whole. None was in their first admission and levels of psychopathology were not high. Further in-depth analysis of these patients’ journeys would be of value. Perhaps the Mental Health Act 1983 was used because of anticipated risks based on previous knowledge of the patients rather than their manifest levels of psychopathology.
The other notable group were the 19 voluntary patients who lacked capacity but were assenting (or ‘non-objecting’) to treatment and therefore fell into the ‘Bournewood gap’, so called because of the lack of legal safeguards in place for them ( R v. Bournewood Community and Mental Health NHS Trust, 1999). The Expert Committee's recommendation that capacity-based mental health legislation be introduced was not accepted by the government and is not reflected in the current Draft Mental Health Bill (Expert Committee, 1999). However, the Mental Capacity Act 2005, recently passed by parliament, provides a legal framework for the provision of treatment in the case of patients who lack capacity, and its implementation will make the assessment of mental capacity increasingly important in clinical practice. The degree of patient insight has a close relationship to capacity and the need for involuntary treatment. It remains possible that this construct, although no less complex than capacity, is more intuitive to mental health professionals and may provide a more reliable basis for coercive-treatment decisions.
Insight, ethnicity and capacity
This cross-sectional study has provided a ‘snapshot’ of incapacity among psychiatric in-patients. Our results suggest that insight has an important effect on capacity and this will be explored in more depth in future. The possible effect of ethnicity on capacity is also an important finding. Ethnicity is the most widely studied and important demographic variable in relation to the use of the Mental Health Act 1983, with higher proportions of Black than White patients being admitted to hospital on an involuntary basis (Reference Wall, Buchanan and FahyWall et al, 1999). Decisional capacity is a complex construct that is determined by the interaction of patient characteristics with contextual and environmental factors (Reference Palmer, Dunn and AppelbaumPalmer et al, 2004) and it is important that we try to improve our understanding of any potential ethnic biases that occur when it is assessed. Fluctuations and improvements in capacity should be studied and may lead to interventions to enhance decisional capacity.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ A small minority of patients with treatment-related decisional capacity were detained under the Mental Health Act 1983.
-
▪ The majority of patients judged incapable of making a treatment decision had poor insight and either a psychotic illness or bipolar affective disorder.
-
▪ Further research is required to validate and improve our understanding of the effect of ethnicity on mental capacity.
LIMITATIONS
-
▪ Fifty-two per cent of admittedpatients could not be included in the study; had they been, the prevalence of incapacity would probably have been higher.
-
▪ The study was based in an inner-London in-patient unit, which may limit the generalisability of the findings.
-
▪ The association between cognitive impairment and incapacity may have been inadequately assessed.







eLetters
No eLetters have been published for this article.