Since its first description in 1974, Reference Dunner and Fieve1 rapid-cycling bipolar disorder has been shown to be present in about 12–24% of people with bipolar disorders at specialised mood disorder clinics in Western countries. Compared with non-rapid-cycling bipolar disorder, it is more common in females, associated with earlier age at onset, greater illness burden and relatively higher treatment resistance. Reference Bauer, Calabrese, Dunner, Post, Whybrow and Gyulai2–Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5 Nonetheless, a number of nosological and clinical issues about rapid-cycling bipolar disorder have remained unresolved. These include whether it is an iatrogenic condition, Reference Ghaemi6 an arbitrary entity in a dimensional framework of conceptualising episode frequency in bipolar disorder Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5,Reference Fisfalen, Schulze, DePaulo, DeGroot, Badner and McMahon7,Reference Schneck, Miklowitz, Miyahara, Araga, Wisniewski and Gyulai8 and, more generally, whether current knowledge about this disorder is biased by a higher probability of help-seeking that accompanies Western patients with severe rapid-cycling mood episodes.
There has been no community-based epidemiological study to clarify the above issues from a cross-national perspective. Reference Bauer, Beaulieu, Dunner, Lafer and Kupka3 This may be because it is difficult for lay interviewers to obtain precise data on the nuances of onset and offset of mood episodes in community samples using currently available structured diagnostic instruments. Another reason could be the need for a large representative sample to estimate the possibly very low prevalence of rapid-cycling bipolar disorder in the community. The World Mental Health version of the Composite International Diagnostic Interview (WMH–CIDI) Reference Kessler and Ustun9 allows us to create an epidemiological measure of rapid-cycling bipolar disorder that approximates the DSM–IV definition of the disorder. 10 This paper presents the first general population study of the prevalence and correlates of rapid-cycling bipolar disorder based on a large data-set from ten socioeconomically diverse countries of the World Mental Health Survey Initiative (www.hcp.med.harvard.edu/wmh/).
Method
Participants
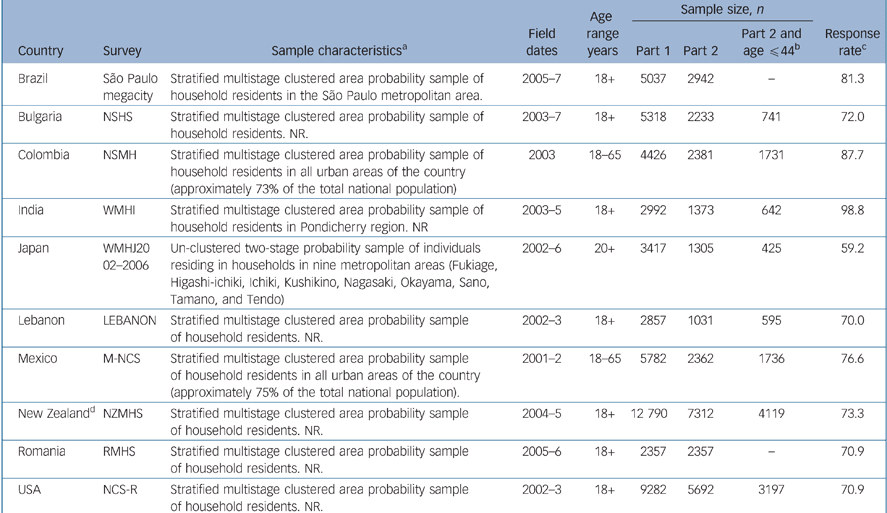
Ten surveys were carried out in the Americas (São Paulo metropolitan area in Brazil, Colombia, Mexico, USA), Europe (Bulgaria, Romania) and Asia (Pondicherry region in India, nine metropolitan areas in Japan, Lebanon, New Zealand). Except in Japan (unclustered two-stage probability sample), they were all based on stratified multistage clustered area probability samples. Interviews were carried out face to face by trained lay interviewers on household residents ages 18 and older (except ≥16 years in New Zealand and ≥20 years in Japan). Sample sizes ranged from 2357 (Romania) to 12 790 (New Zealand). Response rates ranged from 59.2% (Japan) to 98.8% (India), with an average of 74.4% (Table 1).
Table 1 World Mental Health sample characteristics
| Sample size, n | ||||||||
|---|---|---|---|---|---|---|---|---|
| Country | Survey | Sample characteristicsa | Field dates | Age range years | Part 1 | Part 2 | Part 2 and age ≤ 44b | Response ratec |
| Brazil | São Paulo megacity | Stratified multistage clustered area probability sample of household residents in the São Paulo metropolitan area. | 2005-7 | 18+ | 5037 | 2942 | — | 81.3 |
| Bulgaria | NSHS | Stratified multistage clustered area probability sample of household residents. NR. | 2003-7 | 18+ | 5318 | 2233 | 741 | 72.0 |
| Colombia | NSMH | Stratified multistage clustered area probability sample of household residents in all urban areas of the country (approximately 73% of the total national population) | 2003 | 18-65 | 4426 | 2381 | 1731 | 87.7 |
| India | WMHI | Stratified multistage clustered area probability sample of household residents in Pondicherry region. NR | 2003-5 | 18+ | 2992 | 1373 | 642 | 98.8 |
| Japan | WMHJ20 02-2006 | Un-clustered two-stage probability sample of individuals residing in households in nine metropolitan areas (Fukiage, Higashi-ichiki, Ichiki, Kushikino, Nagasaki, Okayama, Sano, Tamano, and Tendo) | 2002-6 | 20+ | 3417 | 1305 | 425 | 59.2 |
| Lebanon | LEBANON | Stratified multistage clustered area probability sample of household residents. NR. | 2002-3 | 18+ | 2857 | 1031 | 595 | 70.0 |
| Mexico | M-NCS | Stratified multistage clustered area probability sample of household residents in all urban areas of the country (approximately 75% of the total national population). | 2001-2 | 18-65 | 5782 | 2362 | 1736 | 76.6 |
| New Zealandd | NZMHS | Stratified multistage clustered area probability sample of household residents. NR. | 2004-5 | 18+ | 12 790 | 7312 | 4119 | 73.3 |
| Romania | RMHS | Stratified multistage clustered area probability sample of household residents. NR. | 2005-6 | 18+ | 2357 | 2357 | — | 70.9 |
| USA | NCS-R | Stratified multistage clustered area probability sample of household residents. NR. | 2002-3 | 18+ | 9282 | 5692 | 3197 | 70.9 |
Procedures
In each country, survey supervisors who were fluent in English and their local languages were trained by experienced CIDI trainers in the USA on the use of the survey instrument and procedures. They were also involved in translation of the instrument and training materials for interviewers in their survey sites according to the translation protocol of the World Health Organization. Reference Harkness, Pennell, Villar, Gebler, Aguilar-Gaxiola, Bilgen, Kessler and Üstün11 Surveys were carried out exclusively in the official languages of the countries. Individuals who could not speak these languages were excluded. Quality control protocols were standardised across countries to check on interviewers' reliability and specify data cleaning and coding procedures. The institutional review board of the organisation that coordinated the survey in each country approved and monitored compliance with procedures for obtaining informed consent and protecting participants.
Measures
All surveys used the World Mental Health Survey version of the WHO Composite International Diagnostic Interview (WMH–CIDI, version 3.0), a fully structured diagnostic interview composed of two parts to reduce participant burden and cost. Reference Kessler and Ustun9 Part one was for core diagnostic assessment of various mental disorders including major depressive disorder and bipolar disorders. Part two included additional information relevant to a wide range of survey objectives. All participants completed part one and those meeting criteria for any mental disorder and a probability sample of other participants were administered part two. Part two participants were weighted by the inverse of their probability of selection for part two of the interview to adjust for differential sampling. The WMH–CIDI field trials and later clinical calibration studies showed that all the disorders considered herein were assessed with acceptable reliability and validity. Reference Kessler and Ustun9 Specifically, concordance was high for bipolar disorder I (area under receiver operating characteristic curve (AUC) = 0.99, Cohen's kappa (κ) = 0.88) and acceptable for bipolar disorder II (AUC = 0.83, κ = 0.50) and any bipolar disorder (AUC = 0.93, κ = 0.69). Reference Kessler, Akiskal, Angst, Guyer, Hirschfeld and Merikangas12
Bipolar disorders
According to DSM–IV criteria, participants were classified as having lifetime bipolar disorder I if they ever had a manic episode, defined as a period of 7 days or more with elevated mood plus three other mania-related symptoms, or irritable mood plus four other mania-related symptoms and the mood disturbance resulted in marked impairment, the need for hospitalisation or psychotic features. To be classified as having lifetime bipolar disorder II, a participant had a major depressive episode and a hypomanic episode, defined as a period of 4 days or more with symptom number criteria similar to mania as above and associated with unequivocal change in functioning, but without any manic episode. The DSM–IV requirement that symptoms do not meet criteria for a mixed episode (criterion C for mania/hypomania and criterion B for major depressive episode) was not operationalised in making these diagnoses. Among participants with lifetime bipolar disorder I or II, those reporting major depressive episode or manic/hypomanic episode at anytime in the 12 months before interview were classified as having 12-month bipolar disorder. The corresponding number of manic/hypomanic episodes and major depressive episodes were assessed. Participants with at least four mood episodes of any combination within that year were classified as having 12-month rapid-cycling bipolar disorder. Three mutually exclusive groups: the 12-month rapid-cycling bipolar disorder (BPD-RC) group, the 12-month non-rapid cycling (12-month BPD-nonRC) group and the other lifetime non-rapid-cycling bipolar disorder group (lifetime BPD-nonRC) were compared in this study. The 12-month BPD-RC group was compared with the 12-month BPD-nonRC group to see how the rapid cycling phenomenon manifested in this recent group of people with bipolar disorder; it was also compared with the lifetime BPD-nonRC group to see how rapid-cycling bipolar disorder differs from general bipolar disorder without rapid cycling.
For those having episodes in the past 12 months we also assessed symptom severity and role impairment. Symptom severity for the most severe month was assessed with the self-report versions of the Young Mania Rating Scale (YMRS) for mania/hypomania Reference Young, Biggs, Ziegler and Meyer13 and the Quick Inventory of Depressive Symptoms (QIDS) for major depressive episode. Reference Rush, Trivedi, Ibrahim, Carmody, Arnow and Klein14 We divided severity of manic/hypomanic episode and major depressive episode into very severe (YMRS 25+; QIDS: 16+), moderate (YMRS 15–24; QIDS 11–15), mild (YMRS 9–14; QIDS 6–10) or clinically non-significant (YMRS 0–8; QIDS 0–5). Role impairment was assessed with the Sheehan Disability Scale (SDS). Reference Leon, Olfson, Portera, Farber and Sheehan15 This asked participants to focus on the month when the manic/hypomanic episode or major depressive episode was most severe and rate how much the condition interfered with home management, work, social life and close relationships using a visual analogue scale. Similar to a Likert scale, the impairment was scored from 1 to 10: none (0), mild (1–3), moderate (4–6), severe (7–9), very severe (10). Clinical features such as age at onset, course, longest lifetime episode, number of months in episode during previous years were asked for both manic/hypomanic episodes and major depressive episodes. Age at onset was assessed with retrospective self-report at syndrome level, as was course of illness by asking participants to estimate the number of years in which they had at least one episode. Annual persistence was defined as the number of years with depressive and/or manic/hypomanic episodes divided by number of years between age at onset and age at interview.
Other disorders
Assessment of other core DSM–IV disorders included anxiety disorders (generalised anxiety disorder, panic attack, panic disorder and/or agoraphobia, post-traumatic stress disorder, obsessive–compulsive disorder, specific phobia, social phobia and separation anxiety disorder), impulse–control disorders (attention-deficit hyperactivity disorder, oppositional dysfunction disorder, conduct disorder and intermittent explosive disorder) and substance use disorders (alcohol misuse and dependence, drug misuse and dependence). Organic exclusion rules and diagnostic hierarchy rules were used in making all diagnoses. Masked clinical reappraisal interviews using the non-patient version of the Structured Clinical Interview for DSM–IV (SCID) Reference First, Spitzer, Gibbon and Williams16 with a probability subsample of participants in the US National Comorbidity Survey Replication (NCS–R) found generally good concordance of CIDI/DSM–IV diagnoses of anxiety, mood and substance use disorders with independent clinical assessments. Reference Kessler, Abelson, Demler, Escobar, Gibbon and Guyer17–Reference Haro, Arbabzadeh-Bouchez, Brugha, de Girolamo, Guyer, Jin, Kessler and Üstün19 Clinical reappraisal interviews did not include the assessment of impulse–control disorder diagnoses.
Other measures
The following types of childhood adversities were asked with dichotomous questions in part two of the WMH–CIDI: loss of parents (parental death, parental divorce, other types of loss of contact with parents), adverse parental factors (mental disorder, substance use, criminal behaviour and violence), abuse (physical, sexual and neglect) and other (participants' serious physical illness and family poverty). We also considered the association of bipolar disorder with sociodemographic variables such as gender, age at interview (18–34, 35–49, 50–64, 65+), marital status at the time of interview (married, previously married, never married), education level compared with local country standard (low, low-average, high-average, high), employment status (working, student, homemaker, retired, other including those unemployed) and household income compared with local country standard (low, low-average, high-average, high). Concerning suicidality, we asked all part two participants (part one participants in New Zealand survey) whether they ever in their life seriously thought about committing suicide. If this was the case we asked the age when this first happened and then whether they ever made a suicide plan, a suicidal attempt and the age of their first occurrence. Finally, all part two participants were asked about 12-month and lifetime treatment of any problem concerning emotions, nerves or substance use. These treatment questions included treatment by psychiatrist, other mental health professional (psychologist, psychotherapist and psychiatric nurse), general medical provider, human services professional and complementary–alternative medical provider (e.g. acupuncturist, chiropractor, spiritual healer), receiving treatment specific to a major depressive episode and/or mania-hypomania, hospitalisation for major depressive episode and/or mania-hypomania, and use of indicated medications.
Statistical analysis
Most analyses were based on the weighted part one sample (n = 54 257). When some variables were only available for the part two sample (such as childhood adversities, suicidality, some sociodemographic variables like income), analyses were based on the part two subsample (n = 28 988). Additional weights were used to adjust for differential probabilities of selection within households, adjusted for non-response and matched the samples to population sociodemographic distributions. We compared the proportions and means for prevalence, persistence, severity and treatment among three subgroups (BPD-RC, 12-month BPD-nonRC, lifetime BPD-nonRC). Using logistic regression analysis, we studied predictors (childhood adversities) and correlates (sociodemographics, comorbid disorders) based on design-corrected variance–covariance matrices. For suicidality subsequent to the onset of bipolar disorder, we estimated first onset by using discrete time survival analysis with person-year treated as the unit of analysis. Because of the complex sampling design with weighting and clusters, standard errors of the above analysis were estimated using Taylor series linearisation method implemented by the SUDAAN software system, version 8.0.1 (Research Triangle Institute, North Carolina, USA, see www.rti.org/SUDAAN/) on UNIX, Solaris/SUN OS. The same set of analyses were done to compare between subgroups of bipolar I (BP-I-RC, 12-month BP-I-nonRC, lifetime BP-I-nonRC) and bipolar II disorder (BP-II-RC, 12-month BP-II-nonRC, lifetime BP-II-nonRC). However, these subgroup comparisons were deemed to be restricted because of small sample sizes. Statistical significance was evaluated using two-sided, 0.05 degree level.
Results
Prevalence, age at onset and other clinical characteristics
Lifetime prevalence estimates of any bipolar disorders, bipolar I and bipolar II disorder of the total pooled sample were 1.1%, 0.7% and 0.5% respectively. Most of the lifetime bipolar disorder occurred in the recent 12 months (12-month prevalence for any bipolar disorders 0.8%; bipolar I disorder 0.4%; bipolar II disorder 0.3%). The 12-month prevalence estimates of the BPD-RC, BP-I-RC and BP-II-RC groups were 0.3%, 0.2% and 0.1% respectively. Thus, roughly a third of participants with lifetime bipolar disorder and 4/10 of those with 12-month bipolar disorder met criteria for rapid cycling. There were cross-national variations in the lifetime prevalence estimates of any bipolar disorder (0.0–2.1%), bipolar I (0.0–1.0%) and bipolar II (0.0–1.1%) disorders and the 12-month prevalence estimates of rapid-cycling bipolar (0.0–0.7%) and non-rapid cycling bipolar disorders (0.0–0.7%). There was zero prevalence of rapid-cycling bipolar disorder in three sites, namely, Bulgaria, Japan and Pondicherry (online Table DS1).
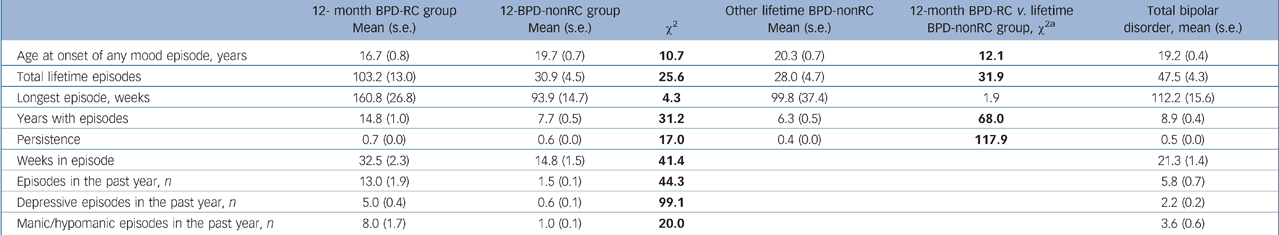
The BPD-RC group exhibited earlier age at onset of any mood episodes (16.7 years) than the 12-month BPD-nonRC group (19.7 years, χ2(1) = 10.7, P<0.01) and the other lifetime BPD-nonRC group (20.3 years, χ2(1) = 12.1, P<0.01) (Table 2). When manic/hypomanic episodes and major depressive episodes were examined separately, the BPD-RC group also showed earlier age at onset than the BPD-nonRC group (results not shown but available upon request). Compared with the 12-month BPD-nonRC group, the BPD-RC group showed more lifetime mood episodes (103.2 v. 30.9), more mood episodes in the year before interview (13 v. 1.5), a more extended longest lifetime episode (160.8 v. 93.9 weeks), more years in lifetime with any mood episode (14.8 v. 7.7 years), higher percentage of years after first onset of mood episode to have at least one episode (70% v. 60%) and more weeks with episode in the previous year (32.5 v. 14.8 weeks). These findings on more and longer episodes were similar when the BPD-RC group was compared with the other lifetime BPD-nonRC group (Table 2).
Table 2 Comparisons on age at onset and clinical characteristics of bipolar disorder (any) with those with the rapid-cycling bipolar disorder (BPD-RC group) and without rapid-cycling (v. 12-month BPD-nonRC group, and v. other lifetime BPD-nonRC group)
| 12- month BPD-RC group Mean (s.e.) | 12-BPD-nonRC group Mean (s.e.) | χ2 | Other lifetime BPD-nonRC Mean (s.e.) | 12-month BPD-RC v. lifetime BPD-nonRC group, χ2a | Total bipolar disorder, mean (s.e.) | |
|---|---|---|---|---|---|---|
| Age at onset of any mood episode, years | 16.7 (0.8) | 19.7 (0.7) | 10.7 | 20.3 (0.7) | 12.1 | 19.2 (0.4) |
| Total lifetime episodes | 103.2 (13.0) | 30.9 (4.5) | 25.6 | 28.0 (4.7) | 31.9 | 47.5 (4.3) |
| Longest episode, weeks | 160.8 (26.8) | 93.9 (14.7) | 4.3 | 99.8 (37.4) | 1.9 | 112.2 (15.6) |
| Years with episodes | 14.8 (1.0) | 7.7 (0.5) | 31.2 | 6.3 (0.5) | 68.0 | 8.9 (0.4) |
| Persistence | 0.7 (0.0) | 0.6 (0.0) | 17.0 | 0.4 (0.0) | 117.9 | 0.5 (0.0) |
| Weeks in episode | 32.5 (2.3) | 14.8 (1.5) | 41.4 | 21.3 (1.4) | ||
| Episodes in the past year, n | 13.0 (1.9) | 1.5 (0.1) | 44.3 | 5.8 (0.7) | ||
| Depressive episodes in the past year, n | 5.0 (0.4) | 0.6 (0.1) | 99.1 | 2.2 (0.2) | ||
| Manic/hypomanic episodes in the past year, n | 8.0 (1.7) | 1.0 (0.1) | 20.0 | 3.6 (0.6) |
Lifetime comorbidity and 12-month suicidality
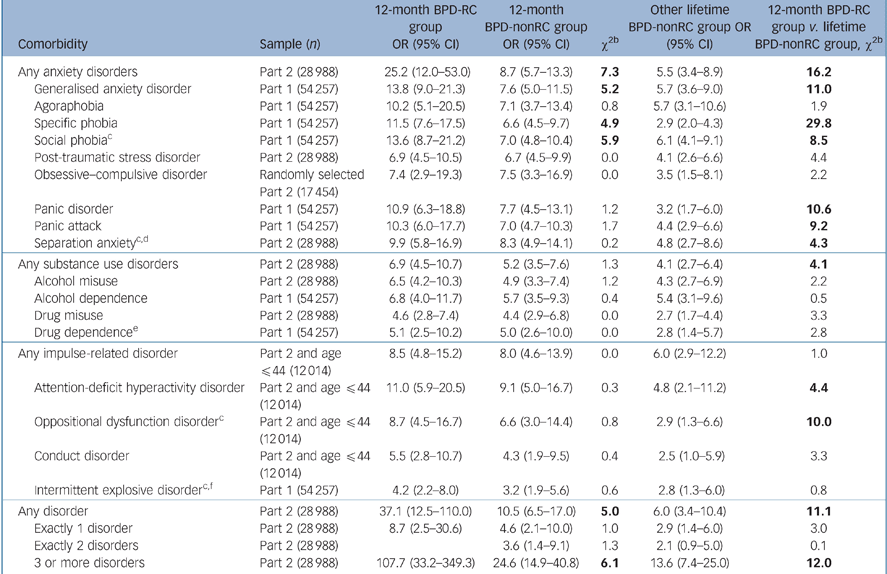
The BPD-RC group demonstrated even more comorbidity with lifetime anxiety disorders (odds ratio (OR) = 25.2, v. BPD-nonRC group, Wald χ2 = 7.3, P<0.01; v. other lifetime BPD-nonRC group, Wald χ2 = 16.2, P<0.01) than the 12-month BPD-nonRC group (OR = 8.7) and the other lifetime BPD-nonRC group (OR = 5.5). This difference in comorbidity was more obvious for generalised anxiety disorder, specific phobia and social phobia than other anxiety disorders, but it was still significant for panic disorder when compared with other lifetime BPD-nonRC groups (Table 3). Whereas the differences in odds ratios were not significant in the comparisons between the BPD-RC and the 12-month BPD-nonRC groups for other mental disorders, the BPD-RC group showed stronger comorbidity, relative to other lifetime BPD-nonRC group, with any substance use disorders as a group (OR = 6.9 v. 4.1, Wald χ2 = 4.1, P = 0.04), attention-deficit hyperactivity disorder (OR = 11.0 v. 4.8, Wald χ2 = 4.4, P = 0.04) and oppositional defiant disorder (OR = 8.7 v. 2.9, Wald χ2 = 10.0, P<0.01). For suicidality, although the BPD-RC, 12-month BPD-nonRC and other lifetime BPD-non RC groups all showed elevated odds ratio on predicting first onset of suicide ideation (ORs = 2.1–3.1), plan (ORs = 1.7–5.0) and attempt (ORs = 2.2–4.8) in previous years, the BPD-RC group did not show significantly higher likelihood than the other two groups (further details available upon request).
Table 3 Lifetime comorbidity of DSM–IV/CIDI bipolar disorder with and without rapid cycling (RC) (12-month BPD-RC group v. 12-month BPD-nonRC group, 12-month BPD-RC group v. lifetime BPD-nonRC group)a
| Comorbidity | Sample (n) | 12-month BPD-RC group OR (95% CI) | 12-month BPD-nonRC group OR (95% CI) | χ2b | Other lifetime BPD-nonRC group OR (95% CI) | 12-month BPD-RC group v. lifetime BPD-nonRC group, χ2b |
|---|---|---|---|---|---|---|
| Any anxiety disorders | Part 2 (28 988) | 25.2 (12.0-53.0) | 8.7 (5.7-13.3) | 7.3 | 5.5 (3.4-8.9) | 16.2 |
| Generalised anxiety disorder | Part 1 (54 257) | 13.8 (9.0-21.3) | 7.6 (5.0-11.5) | 5.2 | 5.7 (3.6-9.0) | 11.0 |
| Agoraphobia | Part 1 (54 257) | 10.2 (5.1-20.5) | 7.1 (3.7-13.4) | 0.8 | 5.7 (3.1-10.6) | 1.9 |
| Specific phobia | Part 1 (54 257) | 11.5 (7.6-17.5) | 6.6 (4.5-9.7) | 4.9 | 2.9 (2.0-4.3) | 29.8 |
| Social phobiac | Part 1 (54 257) | 13.6 (8.7-21.2) | 7.0 (4.8-10.4) | 5.9 | 6.1 (4.1-9.1) | 8.5 |
| Post-traumatic stress disorder | Part 2 (28 988) | 6.9 (4.5-10.5) | 6.7 (4.5-9.9) | 0.0 | 4.1 (2.6-6.6) | 4.4 |
| Obsessive—compulsive disorder | Randomly selected Part 2 (17 454) | 7.4 (2.9-19.3) | 7.5 (3.3-16.9) | 0.0 | 3.5 (1.5-8.1) | 2.2 |
| Panic disorder | Part 1 (54 257) | 10.9 (6.3-18.8) | 7.7 (4.5-13.1) | 1.2 | 3.2 (1.7-6.0) | 10.6 |
| Panic attack | Part 1 (54 257) | 10.3 (6.0-17.7) | 7.0 (4.7-10.3) | 1.7 | 4.4 (2.9-6.6) | 9.2 |
| Separation anxietyc,d | Part 2 (28 988) | 9.9 (5.8-16.9) | 8.3 (4.9-14.1) | 0.2 | 4.8 (2.7-8.6) | 4.3 |
| Any substance use disorders | Part 2 (28 988) | 6.9 (4.5-10.7) | 5.2 (3.5-7.6) | 1.3 | 4.1 (2.7-6.4) | 4.1 |
| Alcohol misuse | Part 2 (28 988) | 6.5 (4.2-10.3) | 4.9 (3.3-7.4) | 1.2 | 4.3 (2.7-6.9) | 2.2 |
| Alcohol dependence | Part 1 (54 257) | 6.8 (4.0-11.7) | 5.7 (3.5-9.3) | 0.4 | 5.4 (3.1-9.6) | 0.5 |
| Drug misuse | Part 2 (28 988) | 4.6 (2.8-7.4) | 4.4 (2.9-6.8) | 0.0 | 2.7 (1.7-4.4) | 3.3 |
| Drug dependencee | Part 1 (54 257) | 5.1 (2.5-10.2) | 5.0 (2.6-10.0) | 0.0 | 2.8 (1.4-5.7) | 2.8 |
| Any impulse-related disorder | Part 2 and age ≤ 44 (12 014) | 8.5 (4.8-15.2) | 8.0 (4.6-13.9) | 0.0 | 6.0 (2.9-12.2) | 1.0 |
| Attention-deficit hyperactivity disorder | Part 2 and age ≤ 44 (12 014) | 11.0 (5.9-20.5) | 9.1 (5.0-16.7) | 0.3 | 4.8 (2.1-11.2) | 4.4 |
| Oppositional dysfunction disorderc | Part 2 and age ≤ 44 (12 014) | 8.7 (4.5-16.7) | 6.6 (3.0-14.4) | 0.8 | 2.9 (1.3-6.6) | 10.0 |
| Conduct disorder | Part 2 and age ≤ 44 (12 014) | 5.5 (2.8-10.7) | 4.3 (1.9-9.5) | 0.4 | 2.5 (1.0-5.9) | 3.3 |
| Intermittent explosive disorderc,f | Part 1 (54 257) | 4.2 (2.2-8.0) | 3.2 (1.9-5.6) | 0.6 | 2.8 (1.3-6.0) | 0.8 |
| Any disorder | Part 2 (28 988) | 37.1 (12.5-110.0) | 10.5 (6.5-17.0) | 5.0 | 6.0 (3.4-10.4) | 11.1 |
| Exactly 1 disorder | Part 2 (28 988) | 8.7 (2.5-30.6) | 4.6 (2.1-10.0) | 1.0 | 2.9 (1.4-6.0) | 3.0 |
| Exactly 2 disorders | Part 2 (28 988) | 3.6 (1.4-9.1) | 1.3 | 2.1 (0.9-5.0) | 0.1 | |
| 3 or more disorders | Part 2 (28 988) | 107.7 (33.2-349.3) | 24.6 (14.9-40.8) | 6.1 | 13.6 (7.4-25.0) | 12.0 |
Symptom severity and role impairment
Although most participants in the BPD-RC group reported severe manic/hypomanic symptoms (63.2%), the proportion was not significantly higher than that of the BPD-nonRC group (54.1%, Wald χ2 = 0.1, P = 0.798). The proportion of those reporting severe depressive symptoms was also not significantly higher among the BPD-RC (80.3%) than the BPD-nonRC group (72.3%, Wald χ2 = 3.1, P = 0.077).
A higher proportion of participants in the BPD-RC than the BPD-nonRC group (86.9% v. 66.6%, Wald χ2 = 3.9, P = 0.05) showed severe role impairment from depressive episodes, but not manic/hypomanic episodes (66.3% v. 56.6%, Wald χ2 = 12, P = 0.28). Participants in the BPD-RC group also reported more days out of role owing to mania/hypomania (50.5 v. 20.6 days, Wald χ2 = 4.2, P = 0.04) and depression (81.6 v. 63.9 days, Wald χ2 = 0.1, P = 0.79), although the difference for the latter was not significant (detailed results available upon request).
Family and childhood predictors and sociodemographic correlates
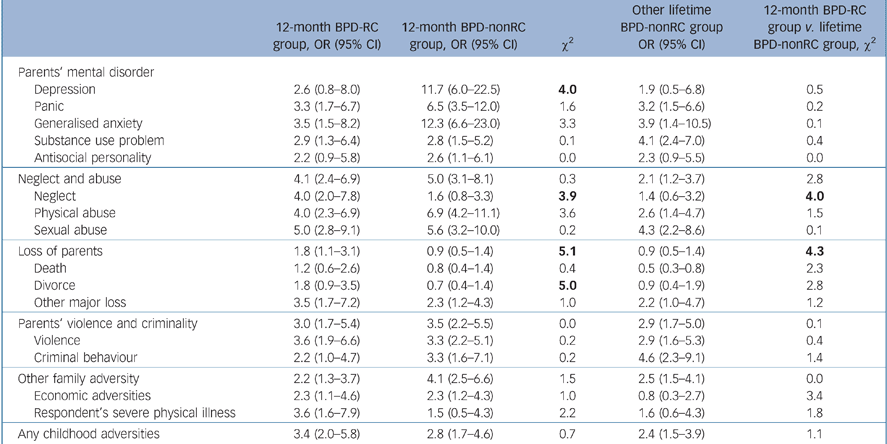
Parental depression was associated with elevated odds of bipolar disorder (ORs = 1.9–11.7), as were panic (ORs = 3.2–6.5), generalised anxiety (ORs = 3.5–12.3), substance use (ORs = 2.8–4.1) and antisocial personality (ORs = 2.2–2.6) disorders (Table 4). The difference between those with and without rapid cycling varied across the bipolar I and bipolar II disorder groups. The elevated risks were commonly larger for those with bipolar I disorder, with those in the BP-I-RC group showing even higher risks (ORs = 2.7–9.3) than those in other lifetime BP-I-nonRC group on parental psychopathology. For those with bipolar II disorder, the difference between the BP-II-RC group and other bipolar II disorder groups was not significant (detailed results for bipolar I and bipolar II disorders are available upon request).
Table 4 Family history and childhood adversity correlates of bipolar with and without rapid cycling (12-month BPD-RC group v. 12-month BPD-nonRC group, 12-month BPD-RC group v. lifetime BPD-nonRC group)a
| 12-month BPD-RC group, OR (95% CI) | 12-month BPD-nonRC group, OR (95% CI) | χ2 | Other lifetime BPD-nonRC group OR (95% CI) | 12-month BPD-RC group v. lifetime BPD-nonRC group, χ2 | |
|---|---|---|---|---|---|
| Parents' mental disorder | |||||
| Depression | 2.6 (0.8-8.0) | 11.7 (6.0-22.5) | 4.0 | 1.9 (0.5-6.8) | 0.5 |
| Panic | 3.3 (1.7-6.7) | 6.5 (3.5-12.0) | 1.6 | 3.2 (1.5-6.6) | 0.2 |
| Generalised anxiety | 3.5 (1.5-8.2) | 12.3 (6.6-23.0) | 3.3 | 3.9 (1.4-10.5) | 0.1 |
| Substance use problem | 2.9 (1.3-6.4) | 2.8 (1.5-5.2) | 0.1 | 4.1 (2.4-7.0) | 0.4 |
| Antisocial personality | 2.2 (0.9-5.8) | 2.6 (1.1-6.1) | 0.0 | 2.3 (0.9-5.5) | 0.0 |
| Neglect and abuse | 4.1 (2.4-6.9) | 5.0 (3.1-8.1) | 0.3 | 2.1 (1.2-3.7) | 2.8 |
| Neglect | 4.0 (2.0-7.8) | 1.6 (0.8-3.3) | 3.9 | 1.4 (0.6-3.2) | 4.0 |
| Physical abuse | 4.0 (2.3-6.9) | 6.9 (4.2-11.1) | 3.6 | 2.6 (1.4-4.7) | 1.5 |
| Sexual abuse | 5.0 (2.8-9.1) | 5.6 (3.2-10.0) | 0.2 | 4.3 (2.2-8.6) | 0.1 |
| Loss of parents | 1.8 (1.1-3.1) | 0.9 (0.5-1.4) | 5.1 | 0.9 (0.5-1.4) | 4.3 |
| Death | 1.2 (0.6-2.6) | 0.8 (0.4-1.4) | 0.4 | 0.5 (0.3-0.8) | 2.3 |
| Divorce | 1.8 (0.9-3.5) | 0.7 (0.4-1.4) | 5.0 | 0.9 (0.4-1.9) | 2.8 |
| Other major loss | 3.5 (1.7-7.2) | 2.3 (1.2-4.3) | 1.0 | 2.2 (1.0-4.7) | 1.2 |
| Parents' violence and criminality | 3.0 (1.7-5.4) | 3.5 (2.2-5.5) | 0.0 | 2.9 (1.7-5.0) | 0.1 |
| Violence | 3.6 (1.9-6.6) | 3.3 (2.2-5.1) | 0.2 | 2.9 (1.6-5.3) | 0.4 |
| Criminal behaviour | 2.2 (1.0-4.7) | 3.3 (1.6-7.1) | 0.2 | 4.6 (2.3-9.1) | 1.4 |
| Other family adversity | 2.2 (1.3-3.7) | 4.1 (2.5-6.6) | 1.5 | 2.5 (1.5-4.1) | 0.0 |
| Economic adversities | 2.3 (1.1-4.6) | 2.3 (1.2-4.3) | 1.0 | 0.8 (0.3-2.7) | 3.4 |
| Respondent's severe physical illness | 3.6 (1.6-7.9) | 1.5 (0.5-4.3) | 2.2 | 1.6 (0.6-4.3) | 1.8 |
| Any childhood adversities | 3.4 (2.0-5.8) | 2.8 (1.7-4.6) | 0.7 | 2.4 (1.5-3.9) | 1.1 |
For other childhood adversity predictors, the pattern of elevations was similar between the bipolar I and bipolar II disorder groups (Table 4). The overall results showed that neglect (ORs = 1.4–4.0), physical abuse (ORs = 2.6–6.9), sexual abuse (ORs = 4.3–5.6), other types of loss of contact with parents (ORs = 2.2–3.5), and parental violence and criminal behaviour (ORs = 2.9–3.5) were associated with bipolar disorder. Besides the findings that neglect and loss of parents in general were more elevated for those in the BPD-RC than in the BPD-nonRC group, there was no elevation for the BPD-RC group with other childhood adversities.
Examination of sociodemographic correlates including gender, marital status, education level, employment status and household income showed that younger age, lower education and other employment status (including being unemployed) were associated with bipolar disorder. However, gender was not associated with rapid-cycling bipolar disorder (Wald χ2 = 0.7, P = 0.402). Concerning the difference between the BPD-RC and BPD-nonRC groups, we only found a difference for marital status (Wald χ2 = 9.6, P = 0.01) in that rapid-cycling bipolar disorder was associated more with those previously married (OR = 1.9, Wald χ2 = 6.0, P = 0.05), but such an elevation did not exist for non-rapid-cycling bipolar disorder.
Treatment
More participants in the BPD-RC than the other BPD-nonRC group received lifetime mental health service not provided by psychiatrists (12-month BPD-RC 47.7% v. other lifetime BPD-nonRC group 32.8%, Wald χ2 = 5.8, P = 0.016) and lifetime general medical services (54.3% v. 43.2%, Wald χ2 = 3.9, P = 0.049). More of them also received lifetime treatment of major depressive episodes (67.1% v. 51.6%, Wald χ2 = 4.5, P = 0.033) but not mania/hypomania. These patterns were more prominent in the BP-I-RC than the BP-II-RC subgroups. A significantly larger portion of those in the BPD-RC group were prescribed some form of medication (55.3%) compared with those in the 12-month BPD-nonRC (30.3%) and other lifetime BPD-nonRC (32%) groups. Among those seeing psychiatrists, there was no significant difference between those with rapid-cycling bipolar disorder (52.8%) and those with other bipolar disorders (35.9% for the 12-month BPD-nonRC group, 31.6% for the lifetime BPD-nonRC group) on being prescribed mood stabilising or antipsychotic medications (details of separate distributions on treatment and medications for bipolar I and bipolar II disorders are available upon request).
Discussion
Methodological considerations
Interpretations of our findings must take account of the following issues. One fundamental issue is about the definition of rapid-cycling bipolar disorder. Clinical studies that adopted different definitions for rapid-cycling bipolar disorder captured different, although overlapping, patient groups. Reference Bauer, Beaulieu, Dunner, Lafer and Kupka3 Our finding of rapid-cycling bipolar disorder showing substantially more lifetime (103.2 v. 30.9) and 12-month (13 v. 1.5) mood episodes than non-rapid-cycling bipolar disorder suggested that the WHM–CIDI did not capture rapid-cycling bipolar disorder in the same way as clinicians diagnose using the DSM–IV. The DSM–IV requires 2 months of full or partial remission or switching of polarity in the counting of the offset of a mood episode. Partial remission is not defined and its determination during clinical interviews may be arbitrary. The WMH–CIDI did not directly assess time between episodes, although the offset of a major depressive episode was established by a respondent reporting ‘no longer have the problems for 2 weeks in a row’. The offset of a manic/hypomanic episode was not specifically defined. At this stage, there are no data to show whether a clinician's judgement of 2 months of full or partial remission of a depressive episode is more or less stringent than a respondent's self-report of 2 full weeks of wellness. Whereas 2 months of clinically assessed full or partial remission seem more stringent than the 2-week WMH–CIDI requirement, participants who were in partial remission for 2 months might continue to feel unwell and thus not endorse the CIDI remission question. This is because clinically judged remission (especially partial remission) might nonetheless be associated with significant subsyndromal self-reported mood, cognitive and functional disturbances among individuals with bipolar disorder. Reference Schneck, Miklowitz, Miyahara, Araga, Wisniewski and Gyulai8,Reference Judd, Akiskal, Schettler, Endicott, Leon and Solomon20,Reference Kaya, Aydemir and Selcuki21 Consequently, some participants might experience several clinical mood episodes as a longer continuous episode and reported them as such. This possibility was supported by prospective studies using daily mood ratings that showed that brief mood episodes were as frequent as full-duration DSM–IV-defined episodes. Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5 Since clinicians typically followed the DSM–IV categorical cut-off of four or more episodes and there is at present little difference in treatment given to people with different degrees of rapid cycling, they may not be inclined to count the exact number of milder episodes for the purpose of subtyping bipolar disorder as rapid cycling.
The WMH-CIDI cannot establish episode offset by using switching of polarity in a way that a clinician's interview can. Furthermore, it is by no means straightforward to examine ‘ultra-rapid’ and ‘ultradian cycling’ bipolar disorder or ‘truncated-episode’ rapid cycling (four or more episodes that last at least 1 day at full severity) in a community survey that employs lay interviewers. Reference Bauer, Beaulieu, Dunner, Lafer and Kupka3 To date, no community epidemiological interview instrument administered by lay interviewers has been clinically validated with reference to rapid-cycling bipolar disorder. Since the cardinal feature of rapid-cycling bipolar disorder is multiple annual episodes, rapid-cycling bipolar disorder generated by the WMH–CIDI provides a fair epidemiological proxy for a bipolar phenotype defined as DSM–IV rapid-cycling bipolar disorder. 10
Another limitation is that mixed episode was not assessed because, when defined according to the DSM–IV requirement for full mania/hypomania and full major depressive episode coexisting, 10 it is hard to operationalise in the WMH–CIDI. This omission could lead to double counting of mood episodes and thus overestimation of the number of mood episodes because DSM–IV mixed episodes should not be counted as manic/hypomanic or/and depressive episodes. Nonetheless, researchers have found that mixed episode as defined by the DSM–IV was rigid and rare. Reference Ghaemi6,Reference Akiskal, Hantouche, Bourgeois, Azorin, Sechter and Allilaire22,Reference Cassidy, Yatham, Berk and Grof23 This would suggest that any overestimation might be small. Retrospective recall could lead to bias in findings on persistence and clinical severity. No data are available on the accuracy of these reports. Besides, clinical severity was evaluated with reference to the most severe month in the previous 12 months. This single-month approach might minimise differences that could exist in the severity of participants' illness across the subsamples.
Community v. clinical findings
Using an identical methodology across the sites of study we showed that rapid-cycling bipolar disorder is a relatively rare condition in the community. There was cross-national variation in prevalence of both bipolar disorder and rapid-cycling bipolar disorder. The overall 12-month prevalence estimates of bipolar disorder (0.8%) and rapid-cycling bipolar disorder (0.3%) we found were lower than those found in the NCS-R study (1.4% and 0.7%). Reference Nierenberg, Akiskal, Angst, Hirschfeld, Merikangas and Petukhova24 This discrepancy is consistent with the repeated finding of higher prevalence of mood disorders in the USA than other WMH countries. It may reflect a genuinely higher level of bipolar disorder in the USA than non-US countries. Reference Post, Luckenbaugh, Leverich, Altshuler, Frye and Suppes25 Potential aetiological factors that vary across countries such as the prevalence of depression, frequency of antidepressant prescription, childhood adversity and thyroid dysfunction may contribute to this. Reference Azorin, Kaladjian, Adida, Hantouche, Hameg and Lancrenon26–Reference Kupka, Luckenbaugh, Post, Leverich and Nolen28
We confirmed the results of other well-documented clinical findings about rapid-cycling bipolar disorder and that it is common among those with bipolar disorder in the community. About a third of participants with lifetime bipolar disorder and 4/10 of those with 12-month bipolar disorder met criteria for 12-month rapid-cycling bipolar disorder. These proportions were higher than the prevalence of rapid cycling found among cases of bipolar disorder in major clinical studies such as the Collaborative Depression Study (CDS: 25.8%) Reference Coryell, Solomon, Turvey, Keller, Leon and Endicott29 and the EMBLEM study (17.3%; range of 2.2 to 23.0% across European countries). Reference Cruz, Vieta, Comes, Haro, Reed and Bertsch27 They were, however, comparable to those found in the NCS-R Reference Nierenberg, Akiskal, Angst, Hirschfeld, Merikangas and Petukhova24 and the Stanley Bipolar Network study (38.2%), which included ultra-rapid and ultradian-cycling bipolar disorder in the estimation of prevalence. Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5 Apart from methodological differences, the higher frequency we found could reflect the fact that rapid-cycling bipolar disorder identified in a community setting consisted of a wider spectrum of severity and other characteristics that might determine whether affected individuals would seek help from specialised mood centres. Nonetheless, the finding that 83.4% of those with rapid-cycling bipolar disorder had received lifetime treatment suggested that the illness was very impairing. Since psychiatrists were not most commonly involved in such treatment, rapid-cycling bipolar disorder in the community was not a primarily drug-induced condition as suggested in some clinical studies. Reference Cruz, Vieta, Comes, Haro, Reed and Bertsch27 Previous studies were inconsistent with regard to whether rapid cycling was more Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5 or less Reference Kupka, Luckenbaugh, Post, Leverich and Nolen28 common in bipolar I than bipolar II disorder. We did not find any difference.
Rapid-cycling bipolar disorder compared with non-rapid-cycling bipolar disorder exhibited several distinguishing characteristics indicating that it is a more severe form of bipolar disorder. Reference Bauer, Beaulieu, Dunner, Lafer and Kupka3,Reference Azorin, Kaladjian, Adida, Hantouche, Hameg and Lancrenon26,Reference Schneck, Miklowitz, Calabrese, Allen, Thomas and Wisniewski30 One is the greater frequency and persistence of episodes (Table 2). This confirmed prospective clinical studies indicating that the proportion of days depressed in the preceding year was significantly associated with shorter time to depressive recurrence. Reference Perlis, Ostacher, Patel, Marangell, Zhang and Wisniewski31 Other non-episode severity indicators of rapid-cycling bipolar disorder we found included higher comorbidity with other mental (especially anxiety) disorders, Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5,Reference Schneck, Miklowitz, Calabrese, Allen, Thomas and Wisniewski30,Reference MacKinnon, Zandi, Gershon, Nurnberger and DePaulo32 higher SDS impairment due to major depressive episodes and more days out of role due to mania/hypomania. That the overall severity of clinical symptoms and role impairment was greater with depression than mania/hypomania was consistent with other clinical studies. Reference Judd, Akiskal, Schettler, Endicott, Leon and Solomon20,Reference Coryell, Solomon, Turvey, Keller, Leon and Endicott29,Reference Judd, Akiskal, Schettler, Coryell, Endicott and Maser33,Reference Judd, Akiskal, Schettler, Endicott, Maser and Solomon34 The greater severity of rapid-cycling bipolar disorder was also shown by the higher frequency of receiving lifetime health services Reference Demyttenaere, Bruffaerts, Posada-Villa, Gasquet, Kovess and Lepine35 and its greater association with previously married status. One finding that was inconsistent with some previous studies of rapid-cycling bipolar disorder was about suicidality. Reference Azorin, Kaladjian, Adida, Hantouche, Hameg and Lancrenon26,Reference Cruz, Vieta, Comes, Haro, Reed and Bertsch27,Reference Coryell, Solomon, Turvey, Keller, Leon and Endicott29 Participants with 12-month rapid-cycling bipolar disorder did not exhibit significantly elevated risk of suicidality subsequent to the first onset of their disorder than participants with 12-month non-rapid-cycling bipolar disorder. This could reflect the lower severity of rapid-cycling bipolar disorder in community than those found in clinical studies. Our finding that more than half of participants with rapid-cycling bipolar disorder received 12-month health services not provided by psychiatrists would suggest that participants with rapid-cycling bipolar disorder in the community had less severe problems than those who attended specialised mood centres.
Regarding age at onset and sociodemographic profile, we confirmed the relatively consistent clinical finding that rapid-cycling bipolar disorder had younger age at onset no matter whether this was assessed with reference to mania/hypomania or major depressive episodes. Reference Azorin, Kaladjian, Adida, Hantouche, Hameg and Lancrenon26,Reference Coryell, Solomon, Turvey, Keller, Leon and Endicott29 That depressive episodes demonstrated an earlier age at onset than manic/hypomanic episodes in both rapid-cycling and non-rapid-cycling bipolar disorder is congruous with both historical and recent studies. Reference Schneck, Miklowitz, Calabrese, Allen, Thomas and Wisniewski30,Reference Alvarez Ariza, Mateos Alvarez and Berrios36,37 This convergence of community and clinical findings points to early age at onset as a risk factor for lifetime rapid-cycling bipolar disorder. By contrast, although most clinical studies indicated a female dominance in rapid-cycling bipolar disorder, Reference Cruz, Vieta, Comes, Haro, Reed and Bertsch27,Reference Schneck, Miklowitz, Calabrese, Allen, Thomas and Wisniewski30 we found that 12-month rapid-cycling bipolar disorder was not connected with gender. Psychosocial factors such as greater concerns about psychiatric stigma associated with help-seeking among males Reference Ojeda and Bergstresser38 and a greater tendency for females to translate distress into conscious recognition of an emotional illness Reference Kessler, Brown and Broman39 might both explain this discrepancy. It is worth noting that at least two studies also did not find rapid-cycling bipolar disorder to be associated with gender. Reference Tondo and Baldessarini40,Reference Shulman, Schaffer, Levitt, Herrmann, May, Akiskal, Lopez-Ibor and Sartorius41 Recent meta-analytic studies have concluded that the preponderance of females among people with BPD-RC was less marked than often suggested. Reference Kupka, Luckenbaugh, Post, Leverich and Nolen28
We examined a much wider range of childhood adversities and parental mental disorders than in previous clinical studies. Reference Leverich, McElroy, Suppes, Keck, Denicoff and Nolen42 The significant associations for childhood adversities found for both bipolar I and II disorders were expected. Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5,Reference Garno, Goldberg, Ramirez and Ritzler43 Although we found that both rapid-cycling and non-rapid-cycling bipolar disorder were associated with neglect and abuse, rapid-cycling bipolar disorder was more elevated than non-rapid-cycling bipolar disorder with childhood neglect and the difference was not significant for abuse. Our findings were more specific than previous studies in suggesting that although childhood abuse was associated with bipolar disorders, deprivational stress via neglect showed consistent association for rapid-cycling but not non-rapid-cycling bipolar disorder. Reference Post, Leverich, Xing and Weiss44 We are not aware of previous studies investigating the association of a range of parental mental disorders in childhood and bipolar disorder with and without rapid cycling in adults. That parental depression was less associated with rapid-cycling bipolar disorder than 12-month non-rapid-cycling bipolar disorder might indirectly support previous negative findings in genetic and family studies of people with rapid-cycling v. non-rapid-cycling bipolar disorder. Reference Bauer, Beaulieu, Dunner, Lafer and Kupka3 How different developmental adversities, their timing, quantity, repetitiveness and interactions with genetic factors and current stressors may mediate the onset and course of bipolar disorder remains to be elucidated in prospective studies.
Future research
One major obstacle to the community epidemiological study of rapid-cycling bipolar disorder is accurate assessment. There is a strong need to develop a refined fully-structured instrument that can validly assess such core characteristics as the onset and offset of episodes, partial v. complete remission, inter-episodic intervals and mixed episodes. Dimensional measures of these characteristics are desirable for resolving uncertainty about the optimal boundary distinctions for rapid-cycling bipolar disorder as rapid cycling may be a dimensional course specifier. Reference Kupka, Luckenbaugh, Post, Suppes, Altshuler and Keck5 The DSM–IV definition of rapid-cycling bipolar disorder by no means captures the spectrum of rapid cycling and mixed episodes, and their definitions may change as new research evidence and experts' consensus emerge. Reference Ghaemi6 When such a structured instrument is available, the validity of bipolar disorder subtypes beyond those defined in the DSM–IV and ICD–10 45 can then be examined critically from a longitudinal epidemiological perspective.
Acknowledgements
We thank the WMH staff for assistance with instrumentation, fieldwork and data analysis. A complete list of WMH publications can be found at www.hcp.med.harvard.edu/wmh/.







eLetters
No eLetters have been published for this article.