Globally, great variation exists in estimates of exposure to violence in youth. Surveys in the USA have consistently observed high rates of violence and victimisation among urban adolescents, with some studies reporting rates ranging from 9% to 42% for experiencing and witnessing serious violence (American School Health Association, 1989; Centers for Disease Control and Prevention, 1992; Reference Schubiner, Scott and TzelepsisSchubiner et al, 1993). Violence exposure is linked to diverse mental health and behavioural sequelae, including depression, anxiety, post-traumatic stress, low self-esteem, self-destructive behaviour and aggression (Reference Fitzpatrick and BoldizarFitzpatrick & Boldizar, 1993; Reference Richters and MartinezRichters & Martinez, 1993; Reference Giaconia, Reinherz and SilvermanGiaconia et al, 1995). Gender may be an important determinant of later trauma-related distress in adolescents. Studies demonstrate higher rates of mood and anxiety symptoms in girls than in boys (Reference Pynoos, Goenjian and TashjianPynoos et al, 1993; Reference Green, Grace and VaryGreen et al, 1994). For example, in African Americans aged 7–18 years (Reference Fitzpatrick and BoldizarFitzpatrick & Boldizar, 1993), males were more likely than females to be victims of, and witnesses to, violent acts, but symptoms of post-traumatic stress disorder (PTSD) were more severe in victimised females.
Previous studies
Few surveys have described the extent of violence exposure and its associated psychological outcomes in African youth. A South African survey by Ward et al (Reference Ward, Flisher and Zissis2001) of 104 adolescents in four secondary schools in Cape Town found that the majority were exposed to at least one type of violent event either as a victim or a witness, and 6% were likely to meet criteria for PTSD. Symptoms of PTSD and depression were related to most types of violence exposure. In other cross-sectional studies of youth in rural and urban settings in South Africa, high rates of violence exposure, ranging from 67% to 95%, have been documented, with 8.4% to 40% of children less than 17 years of age fulfilling PTSD diagnostic criteria (Reference Ensink, Robertson and ZissisEnsink et al, 1997; Reference PeltzerPeltzer, 1999). A significant positive relationship has also been identified between the extent of exposure and the development of PTSD (Reference PeltzerPeltzer, 1998).
With these data underscoring the fact that adolescents are at high risk of becoming victims of violent crime, the purpose of our study was to compare trauma exposure and its sequelae, in particular rates of current full-symptom and partial-symptom PTSD, in adolescents in grade 10 at public and private schools in two African cities. The statistical differences of interest were type of trauma, gender and risk of PTSD in the context of setting. In a preliminary survey conducted at three secondary schools (n=307) in Cape Town (Reference Seedat, van Nood and VythilingumSeedat et al, 2000) we noted high rates of PTSD (12.1%), with girls reporting more trauma exposures and PTSD symptoms than boys. Given these preliminary findings and given the current high rates of criminal violence in South Africa (Victims of Crime Survey, 1998), we predicted that South African respondents, especially females, would endorse considerably higher rates of trauma and PTSD compared with Kenyan respondents.
METHOD
Participants
The sampling pool comprised grade 10 students from 18 schools in Cape Town (South Africa) and Nairobi (Kenya) who were surveyed during the 2000 school year. Seven public schools and two private urban schools were selected in each city to be representative of the ethnic and socio-economic make-up of the population. In total, 1140 South African students and 901 Kenyan students participated. Their mean age was 15.8 years (s.d.=0.98, range 14–22 years).
Procedure
The protocol was approved by the institutional review board (University of Stellenbosch) and the Departments of Education in Cape Town and Nairobi. Students and parents were notified in advance of the study. Participation was entirely voluntary and no student or parent opposed participation. All grade 10 students present on the day of the survey completed anonymous self-report questionnaires in English under the supervision of classroom teachers and research assistants (educated to master's level) during a 45–60 min classroom period at their schools.
Instruments
Demographics questionnaire
We devised a questionnaire to obtain demographic information on age, gender, ethnicity, composition of the home, parental marital status, parental occupation, family income and substance use.
Trauma Checklist
The Trauma Checklist, a list of DSM—IV qualifying traumas (e.g. being robbed or mugged, being physically hurt or attacked, being raped; American Psychiatric Association, 1994) was adapted from the Schedule for Affective Disorders and Schizophrenia for School-age Children — Present and Lifetime version (K—SADS—PL; Reference Kaufman, Birmaher and BrentKaufman et al, 1997). Respondents were also required to circle the most frightening or upsetting event that had ever happened to them.
Child PTSD Checklist
After ascertaining the event that was the most frightening or upsetting, the Child PTSD Checklist (further details available from the authors upon request) was administered. This is a 28-item structured interview developed to diagnose childhood and adolescent PTSD; no information about its psychometric properties has yet been published. For this survey, the Checklist was administered as a self-rated measure. The Child PTSD Checklist rates the presence in the past month of each of the 17 symptoms required for a DSM—IV diagnosis of PTSD, to assess current disorder. The scale uses a four-point Likert format, with 0 corresponding to ‘not at all’ and 3 to ‘all the time’. For the purpose of the study, respondents were asked to rate PTSD symptoms according to the most upsetting event endorsed on the Trauma Checklist. A conservative threshold score of 2 (‘most of the time’) was used to endorse the presence of a symptom. Partial-symptom PTSD was defined as having at least one symptom in each DSM—IV symptom criterion category (reexperiencing, avoidance, hyperarousal) (Reference Stein, Walker and HazenStein et al, 1997; Reference Marshall, Olfson and HellmanMarshall et al, 2001).
Life Events Questionnaire — Adolescent version
The Life Events Questionnaire — Adolescent version (LEQ—A; Reference Masten, Neeman and AndenasMasten et al, 1994), a 45-item measure of negative and positive life events, was used to measure non-PTSD events that can happen in the life of any adolescent or in any family. Respondents were required to indicate (‘yes’ or ‘no’) if an event had happened to them or their families in the past year. Discrete, negative life events included school failure and suspension, pregnancy, legal difficulties, and trouble with drugs or alcohol.
Beck Depression Inventory
The Beck Depression Inventory (BDI) is a widely used 21-item self-report measure of cognitive, affective, somatic and behavioural symptoms of depression with excellent psychometric properties (Reference Beck and SteerBeck & Steer, 1987). Each item consists of four statements rated from 0 to 3; high scores indicate more severe depression. In a school sample of adolescents who were screened with the BDI, a screening score of 16 produced 100% sensitivity and 93% specificity (Reference Barrera and Garrison-JonesBarrera & Garrison-Jones, 1988).
Statistical analysis
All data were analysed using the Statistical Package for the Social Sciences (version 10.0 for Windows). Demographic characteristics, exposure by trauma type, posttraumatic stress and depressive symptoms were assessed using frequency and descriptive statistics. Chi-squared tests (and odds ratios) for categorical variables and Student's t-tests for numeric variables were used to explore the relationship between country, gender, trauma exposure, PTSD and depression. Pearson's correlation statistics were used to correlate PTSD symptoms with BDI total scores. Fisher's exact tests were done in place of χ2 tests for independence when one or more cells in a 2×2 table had an expected count of less than 5. All tests were two-tailed and significance was set at P<0.05.
RESULTS
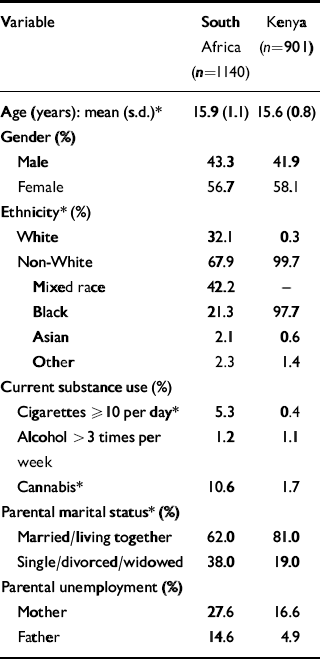
Table 1 compares the demographic characteristics of the South African and Kenyan respondents. There was a preponderance of girls in both groups. The majority of Kenyan respondents were Black whereas the majority of South African students were of mixed race (Coloured), representing the majority ethnic groups in Nairobi and Cape Town. In South Africa 38% of students had single, divorced or widowed parents, compared with 19% of Kenyan students.
Table 1 Demographic characteristics of the study group
| Variable | South Africa (n=1140) | Kenya (n=90 1) |
|---|---|---|
| Age (years): mean (s.d.)* | 15.9 (1.1) | 15.6 (0.8) |
| Gender (%) | ||
| Male | 43.3 | 41.9 |
| Female | 56.7 | 58.1 |
| Ethnicity* (%) | ||
| White | 32.1 | 0.3 |
| Non-White | 67.9 | 99.7 |
| Mixed race | 42.2 | – |
| Black | 21.3 | 97.7 |
| Asian | 2.1 | 0.6 |
| Other | 2.3 | 1.4 |
| Current substance use (%) | ||
| Cigarettes ≥ 10 per day* | 5.3 | 0.4 |
| Alcohol > 3 times per week | 1.2 | 1.1 |
| Cannabis* | 10.6 | 1.7 |
| Parental marital status* (%) | ||
| Married/living together | 62.0 | 81.0 |
| Single/divorced/widowed | 38.0 | 19.0 |
| Parental unemployment (%) | ||
| Mother | 27.6 | 16.6 |
| Father | 14.6 | 4.9 |
Pattern of trauma exposure
More than 80% of the 2041 respondents reported lifetime exposure to at least one DSM—IV trauma. The mean number of trauma exposures was 2.49 (s.d.=1.99, range 0–11). Results of comparisons by country were not statistically significant. For both groups the most common traumas were witnessing community violence (63%), being robbed or mugged (35%), and witnessing a family member being hurt or killed (33%). However, significantly more of those in the Kenyan group had witnessed violence, been physically hurt or beaten by a family member, or been sexually assaulted (Table 2).
Table 2 Trauma exposure type and diagnosis

| Common trauma type | Reported exposures | ||
|---|---|---|---|
| South Africa (n=1140) % (n) | Kenya (n=90 1) % (n) | P 1 | |
| Exposure to ≥ 1 trauma | 83 (943) | 85 (764) | NS |
| Exposure to ≥ 3 traumas | 44 (499) | 45 (406) | NS |
| Witnessing violence in the street, neighbourhood or school | 58 (660) | 69 (619) | < 0.00 1 |
| Being robbed or mugged | 34 (386) | 37 (331) | NS |
| Being in a bad accident | 26 (291) | 16 (140) | < 0.00 1 |
| Being in an earthquake, fire, flood or other natural distaster | 16 (184) | 16 (139) | NS |
| Seeing family members injured, beaten, hurt or killed | 33 (377) | 32 (286) | NS |
| Being beaten or physically hurt by a family member | 14 (161) | 27 (246) | < 0.00 1 |
| Being physically hurt or attacked by a non-family member | 18 (202) | 21 (188) | NS |
| Sexual assault | 14 (157) | 18 (161) | < 0.02 |
| PTSD diagnosis | |||
| Full symptom | 22 (253) | 5 (42) | < 0.00 1 |
| Partial symptom | 12 (136) | 8 (74) | < 0.0 1 |
Symptoms of PTSD
The most common PTSD symptoms (in descending order of frequency) were:
-
(a) avoidance of activities, places or people that aroused recollections of the trauma: South African group (SA) 33.3%, Kenyan group (Kenya) 53.2%;
-
(b) avoidance of thoughts, feelings or conversations associated with the trauma: SA 32.4%, Kenya 50.5%;
-
(c) irritability or outbursts of anger: SA 31.1%, Kenya 23.1%;
-
(d) intense psychological distress at exposure to traumatic reminders: SA 21.3%, Kenya 28.0%.
The South African students had higher scores across all the three symptom clusters of re-experiencing, avoidance and hyperarousal, and more PTSD symptoms, than Kenyan respondents: SA, 4.9 (s.d.=5.5) v. Kenya, 2.3 (s.d.=2.9); t=13.2, P<0.001. In the whole group, 14.5% (n=295) of adolescents met the symptom criteria for full PTSD, and an additional 10% (n=210) met symptom criteria for partial PTSD. Notably, 22% of South African adolescents had a full PTSD diagnosis compared with only 5% of Kenyan adolescents (P<0.001), and 12% met the symptom criteria for partial PTSD compared with 8% in the Kenyan group (P<0.01).
Relationship between trauma exposure and PTSD symptoms
Adolescents meeting the symptom criteria for full PTSD (PTSD-positive, n=295) endorsed more traumas on the Trauma Checklist than adolescents without PTSD (PTSD-negative, n=1748): 3.5 (s.d.=2.6) v. 2.3 (s.d.=1.8); t=-9.7, P<0.001)). These differences remained significant in the analysis by country: Kenya, PTSD-positive 2.9 (s.d.=2.1) v. PTSD-negative 2.4 (s.d.=1.7) mean exposures, t=-2.1, P<0.05; SA, PTSD-positive 3.6 (s.d.=2.7) v. PTSD-negative 2.2 (s.d.=1.9) mean exposures, t=-9.1, P<0.001; and by gender: males, PTSD-positive 3.7 (s.d.=2.6) v. PTSD-negative 2.5 (s.d.=1.9) mean exposures, t=-6.3, P<0.001; females, PTSD-positive 3.2 (s.d.=2.5) v. PTSD-negative 2.2 (s.d.=1.8) mean exposures, t=-6.3, P<0.001. Respondents with full PTSD were more likely to endorse a higher number of traumas (mean 3.7, s.d.=2.5) than those with partial-symptom PTSD (mean 2.9, s.d.=1.9) or no PTSD (mean 2.3, s.d.=1.8); F=58.9, P<0.001).
Gender and trauma exposure
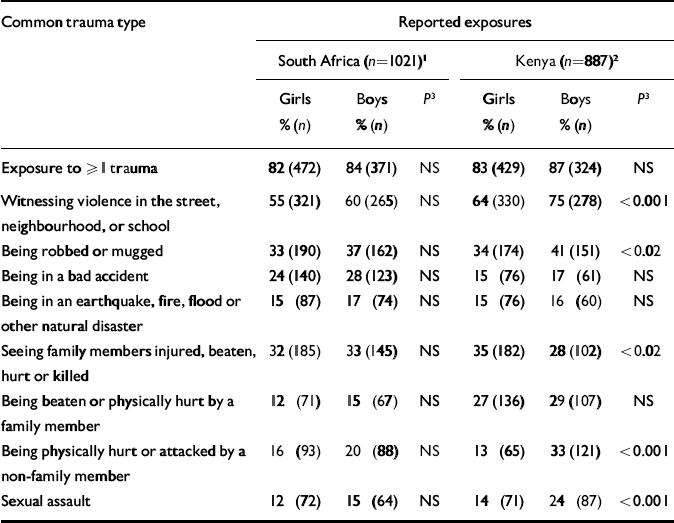
Boys had a higher mean number of trauma exposures than girls (2.7, s.d.=2.0 v. 2.3, s.d.=1.9; t=3.7, P<0.002). Boys were also significantly more likely than girls to have witnessed community violence (67% v. 60%; Fisher's exact text, P<0.001); to have been robbed or mugged (39% v. 33%; Fisher's exact test, P<0.03); to have been beaten by someone not a family member (26% v. 15%; Fisher's exact test, P<0.001); and to have been victims of sexual assault (19% v. 13%; Fisher's exact test, P<0.002); ‘sexual assault’ was operationalised in the survey as ‘any unwanted and forceful sexual experience that made you feel uncomfortable’. When responses for boys and girls were analysed by country, these differences remained significant in the Kenyan sample but not in the South African sample (Table 3).
Table 3 Trauma exposure analysed by gender
| Common trauma type | Reported exposures | |||||
|---|---|---|---|---|---|---|
| South Africa (n=1021)1 | Kenya (n=887)2 | |||||
| Girls % (n) | Boys % (n) | P 3 | Girls % (n) | Boys % (n) | P 3 | |
| Exposure to ≥ 1 trauma | 82 (472) | 84 (371) | NS | 83 (429) | 87 (324) | NS |
| Witnessing violence in the street, neighbourhood, or school | 55 (321) | 60 (265) | NS | 64 (330) | 75 (278) | < 0.00 1 |
| Being robbed or mugged | 33 (190) | 37 (162) | NS | 34 (174) | 41 (151) | < 0.02 |
| Being in a bad accident | 24 (140) | 28 (123) | NS | 15 (76) | 17 (61) | NS |
| Being in an earthquake, fire, flood or other natural disaster | 15 (87) | 17 (74) | NS | 15 (76) | 16 (60) | NS |
| Seeing family members injured, beaten, hurt or killed | 32 (185) | 33 (145) | NS | 35 (182) | 28 (102) | < 0.02 |
| Being beaten or physically hurt by a family member | 12 (71) | 15 (67) | NS | 27 (136) | 29 (107) | NS |
| Being physically hurt or attacked by a non-family member | 16 (93) | 20 (88) | NS | 13 (65) | 33 (121) | < 0.00 1 |
| Sexual assault | 12 (72) | 15 (64) | NS | 14 (71) | 24 (87) | < 0.00 1 |
Gender and PTSD symptoms
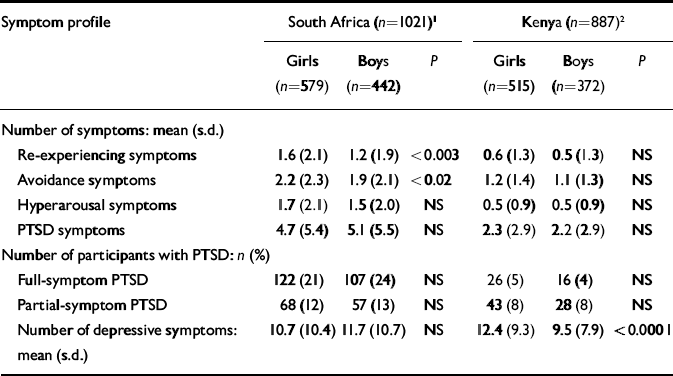
Boys and girls were equally likely to meet symptom criteria for full PTSD (χ2=0.96, P<0.18, n.s.) and partial PTSD (Fisher's exact test, P<0.07, n.s.), and PTSD symptom clusters (re-experiencing, avoidance and hyperarousal symptoms) also did not differ significantly by gender (Table 4).
Table 4 Symptoms of post-traumatic stress disorder and depression
| Symptom profile | South Africa (n=1021)1 | Kenya (n=887)2 | ||||
|---|---|---|---|---|---|---|
| Girls (n=579) | Boys (n=442) | P | Girls (n=515) | Boys (n=372) | P | |
| Number of symptoms: mean (s.d.) | ||||||
| Re-experiencing symptoms | 1.6 (2.1) | 1.2 (1.9) | <0.003 | 0.6 (1.3) | 0.5 (1.3) | NS |
| Avoidance symptoms | 2.2 (2.3) | 1.9 (2.1) | <0.02 | 1.2 (1.4) | 1.1 (1.3) | NS |
| Hyperarousal symptoms | 1.7 (2.1) | 1.5 (2.0) | NS | 0.5 (0.9) | 0.5 (0.9) | NS |
| PTSD symptoms | 4.7 (5.4) | 5.1 (5.5) | NS | 2.3 (2.9) | 2.2 (2.9) | NS |
| Number of participants with PTSD: n (%) | ||||||
| Full-symptom PTSD | 122 (21) | 107 (24) | NS | 26 (5) | 16 (4) | NS |
| Partial-symptom PTSD | 68 (12) | 57 (13) | NS | 43 (8) | 28 (8) | NS |
| Number of depressive symptoms: mean (s.d.) | 10.7 (10.4) | 11.7 (10.7) | NS | 12.4 (9.3) | 9.5 (7.9) | <0.0001 |
Lifetime trauma exposure, PTSD and ethnicity
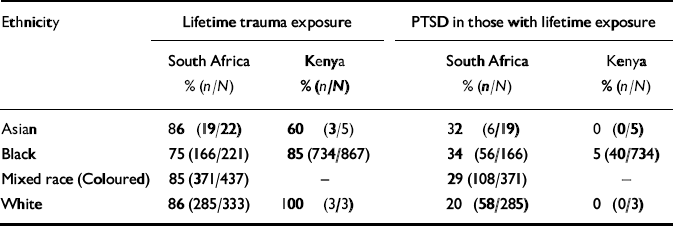
Table 5 shows lifetime trauma exposure rates and rates of PTSD across the major ethnic groups in the sample. Of those belonging to the majority ethnic group in the sample (mixed race) 85% reported exposure to trauma, with 25% of those exposed meeting criteria for a PTSD symptom diagnosis. In the Kenyan sample, 75% of the majority ethnic group (Black) endorsed trauma exposure, but only 5% met PTSD symptom criteria.
Table 5 Lifetime trauma exposure and post-traumatic stress disorder analysed1 by ethnic group
| Ethnicity | Lifetime trauma exposure | PTSD in those with lifetime exposure | ||
|---|---|---|---|---|
| South Africa % (n/N) | Kenya % (n/N) | South Africa % (n/N) | Kenya % (n/N) | |
| Asian | 86 (19/22) | 60 (3/5) | 32 (6/19) | 0 (0/5) |
| Black | 75 (166/221) | 85 (734/867) | 34 (56/166) | 5 (40/734) |
| Mixed race (Coloured) | 85 (371/437) | - | 29 (108/371) | - |
| White | 86 (285/333) | 100 (3/3) | 20 (58/285) | 0 (0/3) |
Trauma type and PTSD risk
Based on respondents' selection of the most frightening or upsetting event, the three traumas most likely to be associated with a PTSD symptom diagnosis were:
-
(a) sexual assault (χ2=38.9, P<0.001, odds ratio 2.5, 95% CI 1.8–3.3);
-
(b) physical assault by a family member (χ2=43.3, P<0.001, OR 2.3, 95% CI 1.8–2.9);
-
(c) serious accidents (χ2=33.5, P<0.001, OR 2.2, 95% CI 1.7–2.9).
The risk of PTSD following sexual assault was the same for girls (24% of sexually assaulted girls; Fisher's exact test, P<0.001, OR 2.3) as it was for boys (25% of sexually assaulted boys; Fisher's exact test, P<0.001, OR 2.3).
Regression analysis
All trauma exposures were then entered as independent variables into a stepwise regression equation to examine the relationship between type of trauma exposure and the risk for PTSD. The dependent variable was a PTSD full-symptom diagnosis. Traumas that constituted independent predictors for PTSD were:
-
(a) sexual assault (P<0.001, exp(B)=0.53, 95% CI 0.39–0.72);
-
(b) witnessing family members injured, beaten, hurt or killed (P<0.001, exp(B)=0.55, 95% CI 0.42–0.72);
-
(c) being in a bad accident (P<0.001, exp(B)=0.56, 95% CI 0.41–0.75);
-
(d) being robbed or mugged (P<0.04, exp(B)=0.74, 95% CI 0.56–0.98);
-
(e) being beaten or physically hurt by a family member (P<0.03, exp(B)=0.69, 95% CI 0.63–1.22);
-
(f) witnessing violence in the street, neighbourhood or school (P<0.02, exp(B)=1.47, 95% CI 1.09–1.97).
Physical attack by someone outside the family (P<0.432) and natural disaster (P<0.096) were not independently predictive of a PTSD symptom diagnosis.
Depression
For the sample as a whole, BDI scores were in the ‘mild’ range for depression (mean 11.5, s.d.=16.7). No significant difference was observed either for country (Kenya 12.2 (s.d.=23.2) v. SA 11.1 (s.d.=10.5)) or gender (males 10.8 (s.d.=9.7) v. females 11.4 (s.d.=10.0)). In the Kenyan group, but not in the South African group, girls reported more depressive symptoms and had significantly higher scores on the BDI than boys: females 12.4 (s.d.=9.3) v. males 9.5 (s.d.=7.9); t=-3.6, P<0.001 (see Table 4).
Correlation between PTSD and depression
The number of PTSD symptoms endorsed on the Child PTSD Checklist correlated significantly with total BDI scores (r=0.29, P<0.001). Statistical significance was retained in the analysis by country (Kenya, r=0.20, P<0.001; SA, r=0.52, P<0.001) and gender (males, r=0.48, P<0.001; females, r=0.51, P<0.001). Respondents with full-symptom PTSD also had higher mean BDI scores (mean 20.0, s.d.=11.4) than those with partial-symptom PTSD (mean 13.6, s.d.=9.6) and those with no PTSD (mean 9.4, s.d.=17.8; F=37.5, P<0.001).
Substance use
More South African adolescents than Kenyan adolescents reported smoking ten or more cigarettes a day (5.3% v. 0.4%, P<0.001) and using cannabis (10.6% v. 1.7%, P<0.001). In the sample as a whole, more boys than girls reported cannabis use (8.7% v. 4.6%, P<0.001). However, no significant gender difference was noted for cigarette or alcohol use. Use of these substances did not correlate significantly with PTSD symptoms.
Negative life events
South African respondents reported a higher number of past-year exposures to negative life events on the LEQ—A (mean 9.2, s.d.=5.2) than did the Kenyans (mean 8.3, s.d.=4.7; t=4.2, P<0.001); these events included doing much worse than expected in a test or examination and breaking up with a boyfriend/girlfriend. Negative life event exposure was not significantly associated with PTSD symptoms (total sample P=0.170, SA P=0.372, Kenya P=0.562). Further, adolescents who reported one or more traumas plus one or more negative life events were not more likely to meet PTSD symptom criteria (χ2=0.66, P=0.363).
DISCUSSION
PTSD and trauma
Of the whole study group, 14.5% (i.e. 14.8% of those exposed to ≥1 trauma; Table 2) fulfilled criteria for a full diagnosis of PTSD, and an additional 10.3% (i.e. 11.4% of those traumatised) fulfilled partial PTSD criteria. These rates are strikingly similar to rates previously documented in trauma samples. In a study by Giaconia et al (Reference Giaconia, Reinherz and Silverman1995), 14.5% of affected youths (6.3% of the total sample) met DSM—III—R criteria for PTSD (American Psychiatric Association, 1987), while Lipschitz et al (Reference Lipschitz, Rasmusson and Anyan2000) found that 14.4% and 11.6% of traumatised girls met DSM—IV symptom criteria for full and partial PTSD, respectively. Both countries had high rates of trauma exposure, with 83% of South African adolescents and 85% of Kenyan adolescents reporting at least one DSM—IV trauma in their lifetime, echoing the findings of other local (South African) and international studies (American School Health Association, 1989; Reference Giaconia, Reinherz and SilvermanGiaconia et al, 1995; Reference Ensink, Robertson and ZissisEnsink et al, 1997; Reference PeltzerPeltzer, 1999).
Differences between the South African and Kenyan groups
The most striking finding was the discrepancy in the rate of PTSD between South African and Kenyan adolescents in the context of equally high rates of trauma exposure (and even higher rates for specific types of trauma in the Kenyan sample). The lower rate of PTSD in Kenyan adolescents is difficult to explain. Our assessments did not measure the severity or chronicity of trauma exposure or past PTSD, variables that may contribute to PTSD risk. For example, differences in toxicity of exposure between the samples (much higher levels of exposure to violent crime in South African adolescents) may be operant here, accounting to some extent for the differences in PTSD rates.
Could cultural factors be responsible? Cultural differences in the way that concepts of ‘trauma’, trauma exposure and PTSD symptoms are operationalised and understood in different ethnic groups are known to exist. Our survey questionnaires were not culturally validated for the various ethnic groups in which they were used, and the likelihood of cultural response bias to questionnaire items cannot be excluded. Further, compared with the South African sample, in which the cultural contexts of the different communities were diverse, the ethnic composition of the Kenyan sample was relatively homogeneous (more than 97% of the Kenyan students were Black, compared with only a fifth of the South Africans).
Gender
In this study, boys had a higher mean number of trauma exposures and higher rates of exposure to certain types of assaultive violence (e.g. robbing or mugging, beating by a person other than a family member, sexual assault) compared with girls. Not all studies have noted gender differences in trauma exposure. Giaconia et al (Reference Giaconia, Reinherz and Silverman1995), in a community study of 18-year-olds, found that overall rates of trauma were the same for both boys and girls. Other studies have reported a greater incidence of trauma exposure in boys (Reference Breslau, Davis and AndreskiBreslau et al, 1991; Reference Vrana and LauterbachVrana & Lauterbach, 1994; Reference Schwab-Stone, Chen and GreenbergerSchwab-Stone et al, 1999). A surprising finding was the absence of a gender difference in the overall rate and presentation of PTSD. Several studies have demonstrated a much greater risk for PTSD (up to 6-fold) in females (Reference Breslau, Davis and AndreskiBreslau et al, 1991; Reference Green, Grace and VaryGreen et al, 1994; Reference Giaconia, Reinherz and SilvermanGiaconia et al, 1995). For example, Singer et al (Reference Singer, Anglin and Song1995) surveyed a diverse sample of high-school students (n=3735) selected from large-city, small-city and suburban schools, and reported that female gender was the strongest demographic predictor of trauma symptoms, including post-traumatic stress, depression, anxiety, anger, dissociation and total trauma symptoms. Our observations are consistent with those of Silva et al (Reference Silva, Alpert and Munoz2000) who, in a clinic sample of traumatised inner-city youths (n=59), found no significant difference in terms of the interaction of traumatic experience (including sexual abuse) and gender, and no difference in the mean number of PTSD symptoms. More than a fifth of these children met full criteria for PTSD, a third had partial symptoms and nearly half had no PTSD symptom.
Another unexpected finding was that, although boys and girls were equally likely to have experienced at least one lifetime trauma, more boys than girls endorsed sexual trauma. The risk of developing PTSD following sexual assault was the same for both genders (OR 2.3). Sexual assault, compared with all other traumas, was also associated with the highest risk of PTSD. This finding parallels that of other workers who have found a relatively higher risk for PTSD (up to 12-fold) following rape or sexual assault compared with other types of trauma (Reference Breslau, Davis and AndreskiBreslau et al, 1991; Reference Green, Grace and VaryGreen et al, 1994; Reference Giaconia, Reinherz and SilvermanGiaconia et al, 1995).
We found that depression, but not substance use, correlated with PTSD. Girls had higher depression scores than boys, consistent with previous work (Reference Lewinsohn, Hops and RobertsLewinsohn et al, 1993; Reference Schraedley, Gotlib and HaywardSchraedley et al, 1999). Further, respondents with more PTSD symptoms (i.e. those with full PTSD) tended to have more depressive symptoms than those with partial symptoms or no PTSD. In contrast, a recent study of children aged 7–14 years found no significant difference in comorbidity (e.g. major depressive disorder) or functional impairment between children with full or partial PTSD (Reference Carrion, Weems and RayCarrion et al, 2002).
Limitations
Several limitations of this study are worth mentioning. First, although we used a relatively high symptom threshold of ‘most of the time’ to establish PTSD criteria, diagnoses of current PTSD (full and partial) were based solely on symptom status and not on functional impairment. For partial PTSD, the presence of at least one symptom from each symptom category (criteria sets: re-experiencing; avoidance; and hyperarousal) was employed (Reference Stein, Walker and HazenStein et al, 1997; Reference Marshall, Olfson and HellmanMarshall et al, 2001). Second, as the age of onset and duration of PTSD were not documented, we were not able to establish symptom chronicity. Third, exposure to trauma was measured as a count of trauma types, rather than as the number of exposures or severity of exposure to a particular trauma. This might have contributed to the failure to detect significant differences between the samples, particularly as cumulative and toxic trauma exposure is associated with a higher PTSD risk. It does not, however, account for higher rates of PTSD in the South African students, despite higher rates of exposure in Kenyan youth to both sexual assault and physical assault by a family member, as these are traumas that are likely to be repeated. Further, these traumas were most likely to be associated with a PTSD full-symptom diagnosis. This discrepancy is one for which we do not have an adequate explanation. Finally, all questionnaires were administered in English (to be eligible participants had to be able to read and write English at tenth grade level), although English was not the home language of the majority of respondents.
In conclusion, replication across other ethnic and cultural settings in the African context is required to establish more clearly the nature and extent of trauma exposure and its psychological repercussions in African youth. Nevertheless, these findings share many similarities with studies undertaken in Western countries. They highlight the high rates of violence exposure and PTSD in both boys and girls and suggest a need for health care professionals to be more vigilant in screening for victimisation and trauma-related distress.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ High rates of full-symptom and partial-symptom post-traumatic stress disorder (PTSD) characterise African youth, mirroring findings in Western settings.
-
▪ Discrepant rates of PTSD between Kenyan and South African adolescents in the presence of comparable rates of trauma exposure suggest that other factors (e.g. differences in trauma toxicity, cultural variables) may be operant in contributing to risk.
-
▪ Boys in the sample endorsed more sexual traumas than girls. Compared with all other traumas, sexual assault was associated with the highest risk of PTSD.
LIMITATIONS
-
▪ Diagnosis of current PTSD (full and partial) was based on symptom status only and not on functional impairment.
-
▪ Survey questionnaires were not culturally validated.
-
▪ Exposure to trauma was measured as a count of types of trauma, not as the number of exposures or severity of exposures to a specific trauma. This might have contributed to the failure to detect significant differences between the groups.
Acknowledgements
The Kenyan portion of this survey was supported by the Chiromo Lane Medical. Center, and the South African portion was supported by the Medical Research. Council Unit on Anxiety and Stress Disorders. The authors wish to thank C. J. Hugo, J. van Kradenburg, D. Albers and J. Daniels for their assistance with. this survey.








eLetters
No eLetters have been published for this article.