For an individual who has engaged in self-harm, the risk of dying by suicide is significantly higher than for the general population (Reference Hawton and FaggHawton & Fagg, 1988; Reference SakinofskySakinofsky, 2000; Reference Owens, Horrocks and HouseOwens et al, 2002), especially during the first 12 months following self-harm (Reference Hawton, Zahl and WeatherallHawton et al, 2003b ). Consequently, the identification of risk factors for suicide in these patients is important for clinicians conducting assessments and planning after-care. The level of suicidal intent at the time of self-harm – that is, the degree to which the individual wished to die – has been investigated as a potential risk factor. However, follow-up studies of people treated for self-harm have produced inconsistent results concerning the relationship between suicidal intent and future suicidal behaviour (e.g. Pierce, Reference Pierce1981, Reference Pierce1984; Reference Beck and SteerBeck & Steer, 1989; Reference Hjelmeland, Stiles and Bille-BraheHjelmeland et al, 1998; Reference Scocco, Marietta and ToniettoScocco et al, 2000; Reference Nimeus, Alsen and Traskman-BendzNiméus et al, 2002) and a range of demographic and clinical factors (e.g. Reference Dyer and KreitmanDyer & Kreitman, 1984; Reference Hamdi, Amin and MattarHamdi et al, 1991; Reference Hjelmeland, Nordvik and Bille-BraheHjelmeland et al, 2000). As suicidal intent is often routinely measured in clinical practice, it is essential that the value of this procedure can be verified. Using a long-term monitoring system for self-harm, we have examined the characteristics associated with suicidal intent and the relationship of intent to both repetition of self-harm and eventual suicide.
METHOD
Study population
Patients were identified through the Oxford Monitoring System for Attempted Suicide (Reference Hawton, Harriss and HallHawton et al, 2003a ). All individuals who present to the general hospital following an episode of self-harm are identified either through assessment by members of the hospital psychiatric service, or (for non-assessed patients) by scrutiny of records of presentations to the accident and emergency department. It has been established that this system produces comprehensive data (Reference Sellar, Goldacre and HawtonSellar et al, 1990), and that the findings are comparable with those from other areas in the UK (e.g. Reference Platt, Hawton and KreitmanPlatt et al, 1988).
The definition of self-harm Footnote 1 comprises intentional self-injury or self-poisoning, irrespective of motivation (Reference Hawton, Harriss and HallHawton et al, 2003a ). Self-poisoning is defined as the intentional self-administration of more than the prescribed dose of any drug, and includes poisoning with non-ingestible substances, overdoses of ‘recreational drugs’ and severe alcohol intoxication where clinical staff consider such cases to be acts of self-harm. Self-injury is defined as any injury that has been intentionally self-inflicted.
For all patients assessed by the general hospital psychiatric service, a clinician completes a standardised form that records demographic and clinical information. Since 1 January 1993 the Suicide Intent Scale (SIS; Reference Beck, Schuyler and HermanBeck et al, 1974) has also been completed at the time of assessment whenever possible. All assessed patients aged 15 years or over, who presented to the general hospital following self-harm between 1 January 1993 and 31 December 2000 and for whom the SIS had been completed on at least one presentation, were included in the initial examination of the characteristics associated with suicidal intent. To allow a substantial follow-up period, only patients who presented to the general hospital before 1 January 1998 were included in the follow-up part of this study, which investigated the association between suicidal intent and both repetition of self-harm and eventual suicide.
Suicide Intent Scale
The SIS is a 15-item questionnaire designed to assess the severity of suicidal intention associated with an episode of self-harm (Reference Beck, Schuyler and HermanBeck et al, 1974). Each item scores 0–2, giving a total score range of 0–30. The questionnaire is divided into two sections: the first 8 items constitute the ‘circumstances’ section (part 1) and are concerned with the objective circumstances of the act of self-harm; the remaining 7 items, the ‘self-report’ section (part 2), are based on patients’ own reconstruction of their feelings and thoughts at the time of the act. Scores for each of these sections were considered separately in the analysis, as well as the total SIS score.
To examine the relationship between suicidal intent and patient characteristics, total SIS scores were divided into two categories – ‘low’ and ‘high’ – by taking the median score for each gender as the point of division. Scores on the circumstances and self-report sections were also assigned to ‘low’ and ‘high’ categories using the same principle. For patients who presented on more than one occasion during the study period, the SIS score from the first episode was used in the initial analysis. Scores for subsequent episodes were included in the examination of changes in suicidal intent preceding suicide. We investigated suicidal intent in relation to a range of demographic and clinical variables: age, marital status, employment status, drug misuse, alcohol misuse (defined as chronic alcoholism with physical symptoms, alcohol dependence or excessive drinking), lonely living conditions (living alone, in an institution, in lodgings or in a hostel), previous self-harm (irrespective of whether or not this resulted in a general hospital referral), physical illness, method of self-harm, further repetition of self-harm and eventual suicide.
Repetition of self-harm
Further episodes of self-harm that resulted in another presentation to the general hospital in Oxford were included in the analysis of repetition of self-harm. Episodes that did not result in hospital presentation, or resulted in presentation to another hospital, were not included.
Suicide
Deaths from suicide that occurred up to 31 December 2000 were identified for patients who presented between 1 January 1993 and 31 December 1997, through the submission of demographic information (name, gender and date of birth) to the Office for National Statistics for England and Wales, the Central Services Agency in Northern Ireland and the General Register Office for Scotland. Tracing revealed whether a patient was alive or dead at 31 December 2000. Patients who could not be traced were excluded from the follow-up analyses. All deaths that received a coroner's verdict of suicide (ICD–9 codes E950–E959), undetermined cause (E980–E989) or accidental poisoning (E850–E869) (World Health Organization, 1978) were combined to form the suicide category for the purposes of this study, as it has been shown that the overall mortality from suicide is underestimated if the ‘suicide’ verdict alone is used (Reference Charlton, Kelly and DunnellCharlton et al, 1992).
Statistical analyses
Chi-squared, Mann–Whitney U, Kruskal–Wallis and Wilcoxon signed rank tests, Spearman's rank correlation and forward stepwise logistic regression analyses were used to examine the data. The analyses were conducted using the Statistical Package for the Social Sciences version 10 for Windows (SPSS Inc., 2000).
RESULTS
Between 1 January 1993 and 31 December 2000 a total of 6494 persons (2727 males and 3767 females) presented following 10 690 episodes of self-harm. Psychosocial assessment was conducted for 7767 (72.7%) of these episodes. An SIS score was available for 5855 (75.4%) of the assessed episodes, which involved 4415 persons (1784 males, 2631 females). These 4415 persons were included in the analysis of suicidal intent and patient characteristics. To provide a sufficient follow-up period for investigation of repetition of self-harm and eventual suicide, only the 2719 patients (1136 males, 1583 females) presenting between 1 January 1993 and 31 December 1997 were included in the follow-up analysis. Follow-up information was available for 2489 of these patients, with a mean follow-up time of 5.2 years (range 2 days to 8 years).
To determine whether the patients for whom the SIS had been completed were a representative sample, all assessed patients with an SIS score were compared with all assessed patients without a score for gender, age and method of self-harm. A marginally greater proportion of those with an SIS score were female (59.6% v. 54.7%; χ2=7.94, P<0.01), under 35 years old (67.3% v. 63.9%; χ2=4.10, P<0.05) and had self-poisoned (89.7% v. 84.9%, χ2=16.89, P<0.0005).
Suicide Intent Scale scores
Suicide Intent Scale scores are shown in Table 1. The median total SIS score for all patients was 9 (interquartile range 5–14). Males scored significantly higher on the SIS than females, both overall and for each of the two parts of the SIS. Scores on the two parts of the SIS correlated moderately well with each other (Spearman's r 0.63, P<0.0005).
Table 1 Suicide Intent Scale part and total scores

| SIS score | Whole sample (n=4415) | Males (n=1784) | Females (n=2631) | Mann-Whitney Z | P |
|---|---|---|---|---|---|
| Total | |||||
| Mean (s.d.) | 9.8 (6.4) | 10.6 (6.6) | 9.2 (6.2) | ||
| Median (IQR) | 9 (5-14) | 10 (5-15) | 8 (4-13) | 6.64 | <0.0005 |
| Part 1 | |||||
| Mean (s.d.) | 4.1 (3.1) | 4.3 (3.2) | 3.9 (3.0) | ||
| Median (IQR) | 3 (2-6) | 4 (2-6) | 3 (2-6) | 4.79 | <0.0005 |
| Part 2 | |||||
| Mean (s.d.) | 5.7 (3.9) | 6.2 (4.0) | 5.3 (3.8) | ||
| Median (IQR) | 6 (2-9) | 6 (3-9) | 5 (2-8) | 7.27 | <0.0005 |
Suicidal intent and method of self-harm
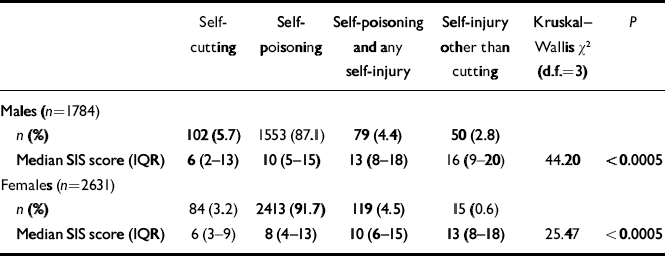
Median SIS scores for patients harming themselves by self-poisoning, self-cutting, other methods of self-injury, and both self-injury and self-poisoning together are presented in Table 2. For both males and females, SIS scores were lowest among patients who engaged in self-cutting, and highest among those who used other methods of self-injury (e.g. jumping from a height or in front of a vehicle, hanging, gunshot).
Table 2 Suicide Intent Scale scores categorised by method of self-harm and gender
| Self-cutting | Self-poisoning | Self-poisoning and any self-injury | Self-injury other than cutting | Kruskal-Wallis χ2 (d.f.=3) | P | |
|---|---|---|---|---|---|---|
| Males (n=1784) | ||||||
| n (%) | 102 (5.7) | 1553 (87.1) | 79 (4.4) | 50 (2.8) | ||
| Median SIS score (IQR) | 6 (2-13) | 10 (5-15) | 13 (8-18) | 16 (9-20) | 44.20 | <0.0005 |
| Females (n=2631) | ||||||
| n (%) | 84 (3.2) | 2413 (91.7) | 119 (4.5) | 15 (0.6) | ||
| Median SIS score (IQR) | 6 (3-9) | 8 (4-13) | 10 (6-15) | 13 (8-18) | 25.47 | <0.0005 |
Patient characteristics and suicidal intent
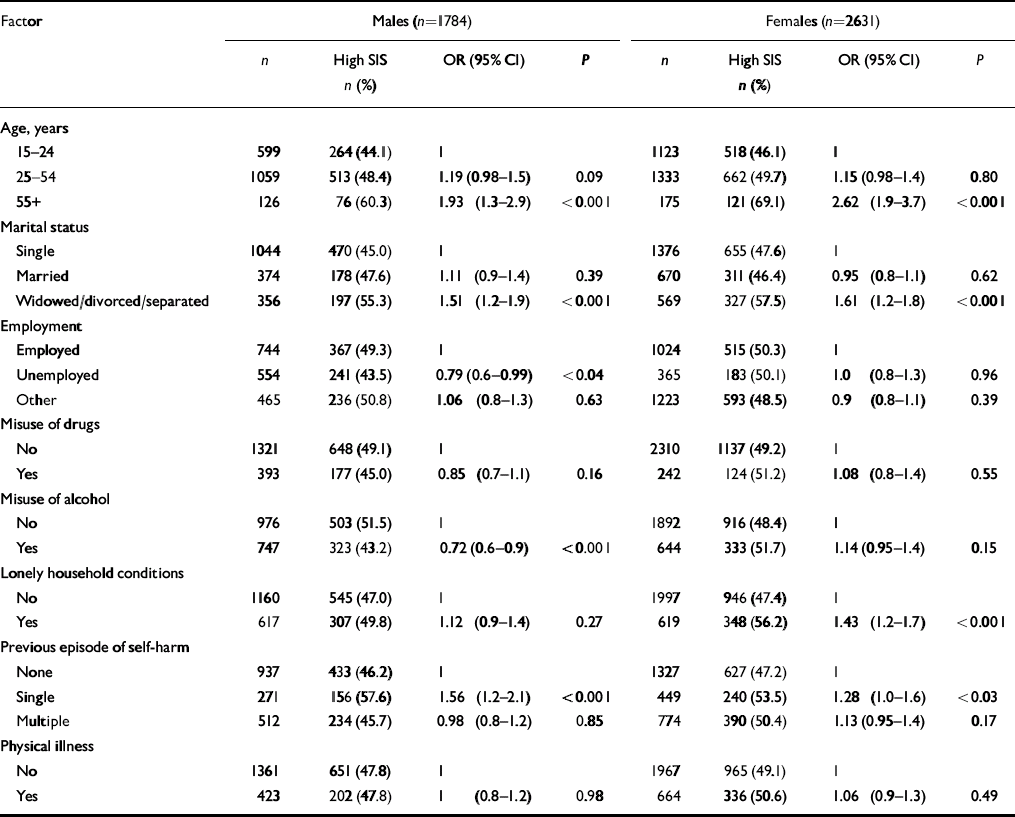
The relationships between SIS scores (high v. low) and demographic and clinical patient characteristics were examined separately for men and women (Table 3). Univariate analyses showed that high suicidal intent was associated with increasing age in both genders. Among males, patients aged 55 years or over had almost twice the odds of having high suicide intent scores compared with those aged 15–24 years (OR=1.93, 95% CI 1.3–2.9), and among females this ratio was even greater (OR=2.62, 95% CI 1.9–3.7). High SIS scores in males were additionally associated with being widowed, divorced or separated, being employed and having a single previous episode of self-harm. Low scores were associated with alcohol misuse. Among females, high SIS scores were again associated with being widowed, divorced or separated, having a single previous episode of self-harm and also with living in lonely household conditions.
Table 3 Factors associated with high Suicide Intent Scale scores
| Factor | Males (n=1784) | Females (n=2631) | ||||||
|---|---|---|---|---|---|---|---|---|
| n | High SIS n (%) | OR (95% CI) | P | n | High SIS n (%) | OR (95% CI) | P | |
| Age, years | ||||||||
| 15-24 | 599 | 264 (44.1) | 1 | 1123 | 518 (46.1) | 1 | ||
| 25-54 | 1059 | 513 (48.4) | 1.19 (0.98-1.5) | 0.09 | 1333 | 662 (49.7) | 1.15 (0.98-1.4) | 0.80 |
| 55+ | 126 | 76 (60.3) | 1.93 (1.3-2.9) | <0.001 | 175 | 121 (69.1) | 2.62 (1.9-3.7) | <0.001 |
| Marital status | ||||||||
| Single | 1044 | 470 (45.0) | 1 | 1376 | 655 (47.6) | 1 | ||
| Married | 374 | 178 (47.6) | 1.11 (0.9-1.4) | 0.39 | 670 | 311 (46.4) | 0.95 (0.8-1.1) | 0.62 |
| Widowed/divorced/separated | 356 | 197 (55.3) | 1.51 (1.2-1.9) | <0.001 | 569 | 327 (57.5) | 1.61 (1.2-1.8) | <0.001 |
| Employment | ||||||||
| Employed | 744 | 367 (49.3) | 1 | 1024 | 515 (50.3) | 1 | ||
| Unemployed | 554 | 241 (43.5) | 0.79 (0.6-0.99) | <0.04 | 365 | 183 (50.1) | 1.0 (0.8-1.3) | 0.96 |
| Other | 465 | 236 (50.8) | 1.06 (0.8-1.3) | 0.63 | 1223 | 593 (48.5) | 0.9 (0.8-1.1) | 0.39 |
| Misuse of drugs | ||||||||
| No | 1321 | 648 (49.1) | 1 | 2310 | 1137 (49.2) | 1 | ||
| Yes | 393 | 177 (45.0) | 0.85 (0.7-1.1) | 0.16 | 242 | 124 (51.2) | 1.08 (0.8-1.4) | 0.55 |
| Misuse of alcohol | ||||||||
| No | 976 | 503 (51.5) | 1 | 1892 | 916 (48.4) | 1 | ||
| Yes | 747 | 323 (43.2) | 0.72 (0.6-0.9) | <0.001 | 644 | 333 (51.7) | 1.14 (0.95-1.4) | 0.15 |
| Lonely household conditions | ||||||||
| No | 1160 | 545 (47.0) | 1 | 1997 | 946 (47.4) | 1 | ||
| Yes | 617 | 307 (49.8) | 1.12 (0.9-1.4) | 0.27 | 619 | 348 (56.2) | 1.43 (1.2-1.7) | <0.001 |
| Previous episode of self-harm | ||||||||
| None | 937 | 433 (46.2) | 1 | 1327 | 627 (47.2) | 1 | ||
| Single | 271 | 156 (57.6) | 1.56 (1.2-2.1) | <0.001 | 449 | 240 (53.5) | 1.28 (1.0-1.6) | <0.03 |
| Multiple | 512 | 234 (45.7) | 0.98 (0.8-1.2) | 0.85 | 774 | 390 (50.4) | 1.13 (0.95-1.4) | 0.17 |
| Physical illness | ||||||||
| No | 1361 | 651 (47.8) | 1 | 1967 | 965 (49.1) | 1 | ||
| Yes | 423 | 202 (47.8) | 1 (0.8-1.2) | 0.98 | 664 | 336 (50.6) | 1.06 (0.9-1.3) | 0.49 |
To determine which of these factors were independently and most strongly related to suicidal intent, the variables examined in the univariate analyses were entered into a forward stepwise conditional logistic regression model as the independent factors, with intent score (high or low) as the dependent variable. Given the different patterns of results for men and women at the univariate stage of the analysis, a separate model was constructed for each gender.
Among male patients, age over 55 years, being widowed, divorced or separated, having a single previous episode of self-harm and absence of alcohol misuse were all independently associated with high suicidal intent scores (Table 4). Among females, high suicidal intent was associated with being over 55 years old, being widowed, divorced or separated, having a single previous episode of self-harm and living in lonely household conditions.
Table 4 Multivariate logistic regression for factors associated with high Suicide Intent Scale scores

| Males (n=1662) | Females (n=2522) | |||||
|---|---|---|---|---|---|---|
| OR | (95% CI) | P | OR | (95% CI) | P | |
| Age, years | ||||||
| 55+ | 1.79 | (1.2-2.7) | 0.006 | 2.08 | (1.4-3.0) | 0.001 |
| Marital status | ||||||
| Widowed/divorced/separated | 1.40 | (1.1-1.8) | 0.01 | 1.31 | (1.1-1.6) | 0.01 |
| Previous self-harm | ||||||
| Single previous episode | 1.62 | (1.2-2.1) | 0.001 | 1.30 | (1.0-1.6) | 0.02 |
| Alcohol misuse | ||||||
| No | 1.49 | (1.2-2.1) | 0.001 | |||
| Lonely living conditions | ||||||
| Yes | 1.35 | (1.1-1.6) | 0.002 | |||
Suicidal intent and repetition of self-harm
Initial analysis of all patients showed no difference between the proportions of high-scoring and low-scoring patients (15.4% v. 17.7%) who engaged in another episode of self-harm within 12 months of the index episode (χ2=2.42, P=0.1). However, when male and female patients were examined separately, a contrasting pattern of association between repetition of self-harm and SIS scores emerged. Among male patients, 12.4% of those with high SIS scores harmed themselves again within 12 months, whereas 22.3% of those with low SIS scores had one or more further episodes (χ2=18.26, P<0.0001). The same pattern was observed in the male patient group when repetition of self-harm within 3 years of the index episode was examined. Among females, patients with high scores (17.4%) were more likely than those with low scores (14.2%) to engage in self-harm again within 1 year, although this difference was not statistically significant. When repetition of self-harm during the 3 years following the index episode was considered, this difference was found to be greater, and significant: 29.5% (high) v. 20.6% (low); χ2=5.84, P<0.02.
Suicidal intent and suicide
Of the patients for whom follow-up information was available, 30 males (2.9%) and 24 females (1.7%) died by suicide. Of these patients, 19 males (63%) and 19 females (79%) had high SIS scores at their index episode. Associations between SIS scores and suicide are shown in Table 5.
Table 5 Association of Suicide Intent Scale scores at index episode with outcome of suicide or non-suicide

| Suicide | Non-suicide | Mann-Whitney Z | P | |
|---|---|---|---|---|
| Whole sample | ||||
| n | 54 | 2435 | ||
| Median SIS score (IQR) | 15 (10-21) | 9 (5-14) | 4.78 | <0.001 |
| Males | ||||
| n | 30 | 1019 | ||
| Median SIS score (IQR) | 13 (10-18) | 10 (5-15) | 2.37 | <0.02 |
| Females | ||||
| n | 24 | 1416 | ||
| Median SIS score (IQR) | 17 (10-22) | 8 (4-13) | 4.18 | <0.001 |
Suicidal intent recorded at the index episode was significantly higher in both male and female patients who later died by suicide than for those who did not (males, Mann–Whitney z=2.37, P<0.02; females, z=4.18, P<0.001). The difference in SIS scores between suicides and non-suicides was notably greater within the female patient group than in the males.
The SIS scores of those who died by suicide and those who did not were examined within three age groups: 15–24 years, 25–54 years and 55+ years. With the exception of men in the oldest group, none of whom died by suicide, within every group the proportion of patients with high SIS scores was greater among those who died by suicide. However, because of the small numbers, these differences were not significant.
Following Pierce (Reference Pierce1984), changes in SIS scores were calculated for the 508 patients who had more than one episode of self-harm with an associated SIS score. Intent scores rose for 239 of these patients. Follow-up information was available for 222 of these ‘rising repeaters’ and for 249 of the ‘non-rising repeaters’. In the ‘rising repeaters’ group, 7 died by suicide, yielding a suicide rate of 3.2%. The suicide rate among the ‘repeaters’ whose SIS scores did not rise was 2.0% (5/249). This difference was not significant.
Although 29 of the 54 patients who died by suicide had two or more episodes of self-harm during the study period, only 12 had more than one associated SIS score. The SIS scores in these 12 cases were used to examine changes in intent scores preceding suicide. SIS scores at the last episode of self-harm during the follow-up period (median 15) appeared to be greater than index episode scores (median 12). This rise in SIS scores was accounted for by changes in the scores of the seven ‘rising repeater’ suicide cases; the scores of the other five suicides decreased or remained the same. Non-parametric analysis revealed that this change in suicidal intent scores over time was not significant (Wilcoxon signed rank test z=1.33, P=0.18).
The relationship between each of the two sections of the SIS and eventual suicide was also examined. Males with high scores on part 1 of the SIS at their index episode were significantly more likely to die by suicide than those with low scores on part 1 (4.4% v. 1.78%; χ2=6.53, P<0.02). Males with high scores on part 2 of the SIS at their index episode were also more likely to die by suicide (3.7%) than those with low scores (2.2%), but this difference did not reach significance (χ2=2.16, P=0.41). Among female patients, those with high scores on part 1 at their index episode were again significantly more likely to die by suicide than those with low scores on part 1 (2.5% v. 0.7%; χ2=8.97, P<0.005). Females with high scores on part 2 at their index episode were more likely to die by suicide (2.3%) than those with low scores (1.0%), but this difference also did not reach significance (χ2=3.46, P=0.06).
Time between index episode and suicide
Of the patients who died by suicide and had high SIS scores at their index episode of self-harm, 42.1% died within 12 months of the index episode. In contrast, of those who recorded low SIS scores at the index episode and who later died by suicide, 12.5% died within 12 months (χ2=4.44, P<0.04). This difference was found among both males (42.1% with high SIS scores and 18.2% with low SIS scores died within 12 months) and females (42.1% v. 10.0%), although owing to the small number of suicides neither difference reached statistical significance.
DISCUSSION
Using a large sample of self-harm patients, followed up for an average of over 5 years, we have shown that suicidal intent at the time of self-harm is associated with risk of subsequent suicide, especially within the first year after an episode. The absence of any association between suicide intent scores and eventual suicide that has been reported by some researchers (Reference Nimeus, Traskman-Bendz and AlsenNiméus et al, 1997; Reference Hjelmeland, Stiles and Bille-BraheHjelmeland et al, 1998; Reference Scocco, Marietta and ToniettoScocco et al, 2000) may be due to smaller sample sizes, shorter follow-up periods or different inclusion criteria. These factors vary greatly across studies of suicidal intent, which may account for some of the diversity in their findings. Our results support the findings of studies by Pierce (Reference Pierce1981) and Niméus et al (Reference Nimeus, Alsen and Traskman-Bendz2002), both of which concluded that high suicidal intent scores at the time of self-harm are associated with an elevated risk of eventual suicide.
Methodological issues
There are some limitations to our study. It was not possible to include all the self-harm patients who presented to the general hospital during the study period, as some people did not receive an assessment, and the SIS was not completed for all of those who were assessed. Additionally, some patients who repeated their self-harm did not have an SIS score for repeat episodes, thereby limiting the number of ‘repeater’ cases that could be included in the analysis of changes in intent scores over time. Although complete follow-up information was obtainable for a large proportion of the sample, for some patients this information was not available or covered a limited period only.
To allow a sufficient follow-up period, deaths by suicide were only identified for patients who presented during the first 5 years of the study. The patients who were categorised as having died from suicide included those whose deaths were officially recorded as suicides, open verdicts or accidental poisonings. This approach, which has been used in previous studies (e.g. Reference Charlton, Kelly and DunnellCharlton et al, 1992), ensures as complete an identification of suicides as possible. Although few deaths will be misidentified through this procedure, some suicides might be missed owing to misclassification under other categories.
The classification of ‘high’ and ‘low’ suicide intent categories was based upon median scores within each gender. Although this is perhaps the most straight-forward principle to adopt, it provides two broad categories that between them cover a range of scores that might be better classified as ‘middle’ rather than ‘high’ or ‘low’. In consideration of this, we repeated the analysis of the categorised SIS scores using a higher cut-off point of 12, which assigned the top 25% (approximately) of SIS scores to the ‘high’ category. The pattern of results was for the most part the same as that obtained in the original analysis. The only exceptions were found in the associations between high SIS scores and both ‘single previous episode of self-harm’ and repetition of self-harm within 3 years among female patients, which, despite displaying the same trends as observed in the original analysis, no longer reached statistical significance.
Suicidal intent and suicide
The risk of suicide among self-harm patients is highest within the first year following the episode of self-harm (Reference Hawton and FaggHawton & Fagg, 1988; Reference Owens, Horrocks and HouseOwens et al, 2002; Reference Hawton, Zahl and WeatherallHawton et al, 2003b ). Patients in this study who died by suicide and had high SIS scores were significantly more likely to die within 12 months of their index episode than those with low SIS scores, replicating the findings of Niméus et al (Reference Nimeus, Alsen and Traskman-Bendz2002). Measurement of suicidal intent may therefore be particularly useful in the assessment of short-term suicide risk.
Unlike Pierce (Reference Pierce1984), we did not find an increased risk of suicide among patients whose suicide intent scores increased with repeated episodes of self-harm. Pierce originally compared his ‘rising repeaters’ with the remainder of his sample of 500 patients; in our study, the ‘rising repeaters’ were compared, perhaps more appropriately, with the other ‘repeaters’ whose intent scores did not rise. Further comparison of the ‘rising repeaters’ group with all the other patients in the sample also showed no difference in rates of suicide.
Additionally, among patients who repeated self-harm and died by suicide, suicidal intent scores at the last episode in the study period were not significantly greater than intent scores at their index episodes. Pierce (Reference Pierce1981) reported that the mean scores for the penultimate episodes of patients who died by suicide and had repeatedly presented following self-harm (n=4) was especially high, in comparison with the rest of his sample. As Pierce did not report the mean score for the index episodes of these four patients, it is not possible to establish whether their scores were consistently high over repeated episodes of self-harm, or whether they increased over time. Our results suggest that a high level of suicidal intent at any single episode of self-harm is a better predictor of eventual suicide than change in intent over time.
It is desirable in clinical practice to use as brief a measuring instrument as possible in the assessment of self-harm patients. The ‘circumstances’ section of the SIS is regarded as a more reliable measure of suicidal intent than the ‘self-report’ section, as the items in the latter section are more vulnerable to distortion by the patient, who might wish to enhance the social desirability of the act or exaggerate the wish to die. The results of our study support this theory: the relationship between scores on the ‘circumstances’ section of the SIS and eventual suicide was substantially stronger than that between suicide and ‘self-report’ scores, for both men and women. However, a verbally expressed wish to die at the time of the episode of self-harm has also been associated with subsequent suicide (Reference HjelmelandHjelmeland, 1996). For measuring suicidal intent in order to inform suicide risk assessment, the ‘circumstances’ section of the SIS along with a question from the ‘self-report’ section regarding the wish to die may be sufficient.
Suicidal intent and gender
Suicidal intent scores of male patients were higher than those of female patients, both overall and for each of the ‘circumstances’ and ‘self-report’ sections of the SIS. Although several previous smaller studies have found no gender difference in intent scores (Reference Dyer and KreitmanDyer & Kreitman, 1984; Reference Nimeus, Alsen and Traskman-BendzNiméus et al, 2002), others have found higher scores among male patients (Reference Hjelmeland, Nordvik and Bille-BraheHjelmeland et al, 2000; Reference Haw, Hawton and HoustonHaw et al, 2003). Hjelmeland et al (Reference Hjelmeland, Nordvik and Bille-Brahe2000) argued that the gender difference observed in their study was due to their large sample rendering a negligible difference statistically significant, and was therefore of no theoretical or practical significance. The difference in intent scores of the male and female patients in our study is considerably larger, and highly significant. In addition, the gender differences found throughout the rest of the analyses suggest that there are real differences between men and women who harm themselves, with respect to suicidal intent. Most notably, we found a stronger relationship between intent scores and suicide among women than men. Almost four-fifths of the women who went on to die by suicide, and almost two-thirds of the men, had high SIS scores at their index episode. Intent scores of both genders were higher among those who died by suicide than among those who did not, but this difference was markedly greater within the female patient group.
Suicidal intent and age
The association of suicide intent scores with increasing age found in previous studies (Reference Dyer and KreitmanDyer & Kreitman, 1984; Reference Nimeus, Alsen and Traskman-BendzNiméus et al, 2002) was confirmed by our findings. Niméus et al (Reference Nimeus, Alsen and Traskman-Bendz2002) reported that suicide intent scores were higher in those who died by suicide than in the non-suicide group only among patients over 55 years old. Intent scores of those who died by suicide within all age groups of both genders in our study were higher than those of the non-suicide group, with the exception of men over 55 years old. Although older men are generally at high risk of suicide (Reference Hawton, Zahl and WeatherallHawton et al, 2003b ), no suicides occurred in this patient group between 1993 and 1997. Because of the smaller number of suicides in some of the age groups, differences in intent scores were not significant.
Factors associated with high suicidal intent
Logistic regression analysis showed that high suicidal intent scores among male patients were associated with being over 55 years old, being widowed, divorced or separated, having a single previous episode of self-harm and an absence of alcohol misuse. Among the female patients, high SIS scores were associated with being over 55 years old, being widowed, divorced or separated, having a single previous episode of self-harm and living in lonely household conditions. With the exception of absence of alcohol misuse in males, these characteristics are all known risk factors associated with eventual suicide following self-harm (Reference Hawton and CatalanHawton & Catalan, 1987; Reference SakinofskySakinofsky, 2000), and thus support the associations between suicidal intent and suicide found in this study. The finding relating to alcohol might be due to the relatively broad definition of alcohol misuse, which included excessive drinking as well as alcohol dependence and chronic alcoholism.
Suicidal intent and lethality
Suicide intent scores have been shown to be related to the potential lethality of the method of self-harm (Reference Hamdi, Amin and MattarHamdi et al, 1991; Reference Haw, Hawton and HoustonHaw et al, 2003). Although no measure of lethality was used in our study, the suicide intent scores of patients using different methods of self-harm support these findings. The highest intent scores were recorded for patients who injured themselves using methods other than self-cutting, which are more likely to be lethal. Patients who engaged in self-cutting had the lowest intent scores. This behaviour is rarely suicidal in nature, and more often used for affect regulation or self-punishment (Reference ShearerShearer, 1994).
Suicidal intent and repetition of self-harm
The Suicide Intent Scale was not originally designed to predict repetition of self-harm. The majority of studies that have investigated the relationship between intent scores and repetition have done so retrospectively, and have not considered male and female patient groups separately. Hjelmeland et al (Reference Hjelmeland, Stiles and Bille-Brahe1998) reported that low suicide intent scores predicted repetition of self-harm within 12 months of the index episodes of 552 patients, using a logistic regression model in which gender was not a significant factor; however, the difference between mean SIS scores in male ‘repeaters’ and ‘non-repeaters’ (11.6 v. 14.7) was notably greater than that between female ‘repeaters’ (12.0) and ‘non-repeaters’ (13.1) (Reference Hjelmeland, Stiles and Bille-BraheHjelmeland et al, 1998). No associated statistical analysis of these proportions for each gender was reported. When mean SIS scores in our study were similarly examined, the pattern of association with repetition within 12 months was found to be comparable (males: ‘repeaters’ group mean SIS score 8.8, ‘non-repeaters’ group 10.8; females: ‘repeaters’ group mean SIS score 9.5, ‘non-repeaters’ group 9.4).
It is possible that previous findings of either no relationship between repetition of self-harm and SIS scores, or of an association between low SIS scores and repetition, have been confounded by examining data from both genders together, or by the relative brevity of follow-up periods. We have identified contrasting patterns of association between repetition of self-harm and SIS scores within male and female patients. A strong association between low suicide intent scores and repetition of self-harm was found among male patients, and a weaker association between high SIS scores and repetition was found in female patients, which reached statistical significance at 3 years’ follow-up. It is evident that suicide intent scores cannot be used reliably to assess risk of repetition of self-harm, and that future studies investigating the relationship between suicidal intent and repetition of self-harm should address gender differences.
Clinical implications
Accurate prediction of suicide following self-harm will always be restricted by the low rate of suicide and by the low specificity of predictive factors, including measures of suicidal intent. However, the findings of this study confirm that the measurement of suicidal intent is valuable in the evaluation of future suicide risk. It is likely to be most beneficial when considered in conjunction with other known risk factors (Reference Hawton and CatalanHawton & Catalan, 1987; Reference SakinofskySakinofsky, 2000). Use of the ‘circumstances’ section of the Suicide Intent Scale, along with a question concerning the patient's wish to die, may be sufficient in clinical practice. Suicide intent scores appear to be especially useful in the assessment of short-term suicide risk.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ The measurement of suicidal intent is valuable in the evaluation of future suicide risk among self-harm patients.
-
▪ Suicide intent scores appear to be especially useful in the assessment of short-term suicide risk.
-
▪ Use of the ‘circumstances’ section of the Suicide Intent Scale, along with a question concerning the patient's wish to die, may be sufficient in clinical practice.
LIMITATIONS
-
▪ It was not possible to include all self-harm patients presenting to the general hospital during the study period.
-
▪ Follow-up information was not available for all patients in the study sample.
-
▪ Some suicides might have been missed owing to their classification as other types of death.
Acknowledgements
The authors thank the staff of the Office for National Statistics for. England and Wales, the General Register Office for Scotland, and the Central. Services Agency in Northern Ireland for their assistance with this project. Staff at the Department of Psychological Medicine at the John Radcliffe. Hospital in Oxford, and Elizabeth Bale and Alison Bond, assisted with the. collection of patient information used in this study. The Oxford Monitoring. System is funded by the Department of Health. The mortality follow-up study. was funded by a grant from the National Health Science Executive for England. K.H. is also supported by Oxfordshire Mental Healthcare Trust.







eLetters
No eLetters have been published for this article.