The 2007 amendments to the Mental Health Act 1983 introduced community treatment orders (CTOs) as part of supervised community treatment. Reference Woolley1 Although these are technically part of Section 17 leave, they effectively allow conditions to be placed on patients for treatment in the community. These conditions may include all aspects of medical and social care that are directly related to the patient’s mental health as long as they ‘ensure that the patient receives medical treatment for [his or her] mental disorder, prevent a risk of harm to the patient’s health or safety, [or] protect other people’ (p. 226). 2 The government’s declared aim was to update the Mental Health Act and propel it into the 21st century by realising that the majority of psychiatric treatment in England and Wales is now delivered in the community. The Act’s Code of Practice (Chapter 25) states that ‘the purpose of supervised community treatment is to allow suitable patients to be safely treated in the community rather than under detention in hospital, and to provide a way to help prevent relapse and any harm – to the patient or to others – that this might cause. It is intended to help patients maintain stable mental health outside hospital and to promote recovery’ (p. 220). 2 The ability to place conditions on patients at the time of discharge from hospital was designed to ‘address the specific problem of “revolving door” patients’. Reference Churchill, Owen, Singh and Hotopf3 In its own patient information leaflet the Department of Health states that CTOs are used if a treating clinician thinks that a patient is ‘well enough to leave hospital but is concerned that [the patient] may not continue with treatment, or may need to be admitted to hospital again at short notice for more treatment’. 4 It was hoped that such frequent readmissions could be avoided by compelling patients to be more cooperative, but at the same time allowing them to remain in the community. Other authors suggested there was a lack of evidence for such claims, and CTOs would not reduce ‘revolving door care’. Reference Kisely and Campbell5 In Scotland the purpose of a CTO is defined as ‘creating individual measures for the care and treatment of a patient who requires a degree of compulsion to accept these (Section 64(4))’. Reference Thomson6 Whereas it is still not possible to give people medication against their will in their own homes, the CTOs effectively allow compulsory community treatment. With the consent of the patient (the CTO does require a degree of cooperation) depot medication can be given in the patient’s own home.
Many countries (Germany, France, Belgium, Luxemburg, Portugal, Israel) have supervised discharge provisions or trial hospital leaves without formal CTOs. These trial leaves can be up to 6 months. In Spain, involuntary out-patient treatment is possible in some cities; this includes the use of covert medication, all of which need court permission. Reference Cañete-Nicolás, Hernández-Viadel, Bellido-Rodríguez, Lera-Calatayud, Asensio-Pascual and Pérez-Prieto7 In the USA, many federal states introduced CTOs in the late 20th century. However, these orders are usuallymadebyjudgesrather thanmental healthprofessionals, and the consequences of non-adherence to treatment vary markedly between the jurisdictions. Reference O'Reilly8 In Australia, Canada and New Zealand, CTOs exist as well. Reference Churchill, Owen, Singh and Hotopf3 They are usually authorised in connection with court hearings, a prior involuntary commitment is not always necessary. In Australia, it is possible to receive involuntary depot medication in the community without returning to hospital. Reference Cañete-Nicolás, Hernández-Viadel, Bellido-Rodríguez, Lera-Calatayud, Asensio-Pascual and Pérez-Prieto7
Community treatment orders fully came into effect throughout England and Wales in 2009 and have been very popular with treating teams and clinicians. 9 The number of people put on CTOs has significantly exceeded the Department of Health’s expectations and is higher than the previous use of Section 25. Reference Evans, Makala, Humphreys and Mohan10 The number is still rising, with a recent reported increase of 29% in the past year (2011). Reference O'Dowd11 However, there is a remarkable dearth of guidance for clinicians when it comes to defining CTO conditions. A recent audit in Wales 12 confirmed other studies, Reference Woolley1,Reference Manning, Molodynski, Rugkåsa, Dawson and Burns13 showing that there are not only vast regional differences but also a significant variety of conditions placed on patients. Since the Mental Health Act does not limit the type of condition that can be placed on patients other than asking for the least restrictive to achieve the aim, we see a wide range of conditions being used by clinicians and sanctioned by approved mental health professionals. The Welsh audit shows that 25% of conditions are not used to improve adherence but are measures to reduce risky behaviour. This may be a risk to the patient but it is more often about risk to others. In effect, those conditions are often similar to social behaviour orders trying to deal with the adverse or dangerous behaviours the patients have displayed in the course of their illness. The audit results across Wales are confirmed by our own local audit in North Wales, which shows very similar results.
The North Wales audit
The local audit expanded on the quantitative data collection with various factors emerging. A total of 50 CTOs showed fairly equal distribution between genders. The age range shows a wide distribution, suggesting the flexible application of CTOs. The majority of patients were single (76%, n = 38) and of White British ethnicity (96%, n = 48). This data are helpful in understanding the sociodemographic factors that emerge. The geographical data show that the CTOs are used more in urban settings. Variables used in the MINI (Mental illness Needs Index) were also collected. Reference Glover, Robin, Emami and Arabscheibani14 It is noteworthy that 82% (n = 41) of patients on a CTO did not have access to a car and 98% (n = 49) were permanently unable to work. Also, 100% were unemployed and 14% (n = 7) were living in a hostel. We expected that CTOs would be used in patients who have a history of multiple admissions. The data show that a peak occurs at six admissions but CTOs were also being used following just one admission. Only 18% (n =9) of patients had previously been on a Section 25. A total of 44% (n = 22) of patients with CTOs were treated by the assertive outreach team (AOT). This is a low figure if we assume that AOTs primarily treat so-called ‘revolving door patients’, the declared target group of patients for the use of CTOs. Regarding diagnosis, 66% (n = 33) of patients had schizophrenia and 18% (n = 9) schizoaffective disorder. The comorbid diagnosis of personality disorder was relatively low at 16% (n = 8), whereas the comorbid diagnosis of substance misuse was much higher at 40% (n = 20). This study is in keeping with the Epidemiologic Catchment Area (ECA) study that revealed a lifetime prevalence of 47% for substance misuse in patients with schizophrenia. Reference Regier, Farmer, Rae, Locke, Keith and Judd15 Despite the comorbid substance misuse rate of 40%, this is not reflected in the discretionary conditions that require only 18% of patients to refrain from illicit substances and 20% to attend drug counselling. This suggests a lack of a consistent approach in the generation of discretionary conditions.
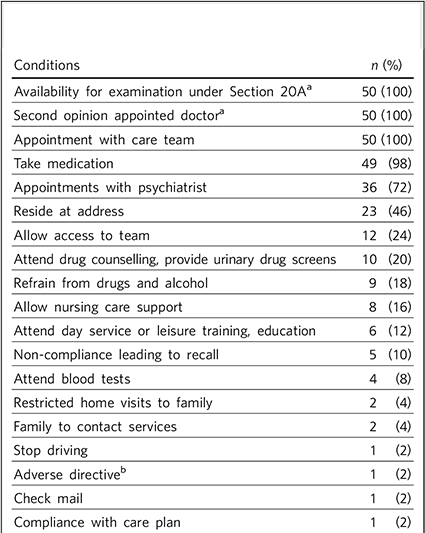
Community treatment orders play a part in medication adherence management strategies as 100% were on medication. Given that most patients had a diagnosis of schizophrenia or bipolar affective disorder, the high use of depot medication (n = 36, 72%) was unsurprising. Table 1 shows the conditions placed on patients in the CTOs audited.
Table 1 Conditions placed on patients in the community treatment order audited (n = 50)
| Conditions | n (%) |
|---|---|
| Availability for examination under Section 20A a | 50 (100) |
| Second opinion appointed doctor a | 50 (100) |
| Appointment with care team | 50 (100) |
| Take medication | 49 (98) |
| Appointments with psychiatrist | 36 (72) |
| Reside at address | 23 (46) |
| Allow access to team | 12 (24) |
| Attend drug counselling, provide urinary drug screens | 10 (20) |
| Refrain from drugs and alcohol | 9 (18) |
| Allow nursing care support | 8 (16) |
| Attend day service or leisure training, education | 6 (12) |
| Non-compliance leading to recall | 5 (10) |
| Attend blood tests | 4 (8) |
| Restricted home visits to family | 2 (4) |
| Family to contact services | 2 (4) |
| Stop driving | 1 (2) |
| Adverse directive b | 1 (2) |
| Check mail | 1 (2) |
| Compliance with care plan | 1 (2) |
a Mandatory condition.
b Term used by one consultant in the audit. It means a recall into a specific care plan once recalled.
The number of conditions that were changed at a later date (variation of conditions) was low at 6%, suggesting that the entire point of a CTO, is collaborative enforcement of care plans and conditions. This does raise the question of exactly how flexible a CTO is. Out of those patients currently on a CTO, the recall and revocation rates were similar at 34%. One may argue that it is less disruptive or traumatic for a patient to be asked to return to hospital rather than the process of a Mental Health Act assessment. The number of voluntary admissions while on a CTO was 8%. The combined recall and voluntary admission rate was 40%, questioning the effectiveness of CTOs. The rationale behind the conditions was not always clearly documented, exemplified by the use of invented terms such as ‘adverse directives’, attending blood tests or checking mail. Generic statements, for example ‘compliance with care plan’ are not specific and can be confusing for the patient.
The common themes to emerge are their use in order for patients to keep appointments with the care team and to cooperate with taking prescribed medication. To ‘reside at an address’ was detailed in 46% of cases. The actual presence of discretionary conditions raises the ethical issue of allowing structure and recovery versus a more paternalistic approach. Some practitioners may take an authoritarian attitude. The conditions ‘to stop driving’, ‘restricted home visits to family’ or allowing mail to be checked may be viewed as particularly authoritarian by patients. But also the conditions of attending education or taking medication regularly may be perceived as such by patients. This could even interfere with the therapeutic alliance. It remains unclear whether coercion to comply with conditions (created by others) under the threat of hospital readmission lead to the desired effect of better adherence and improved long-term prognosis. Complex patients who pose significant risk both to themselves and others, may have personality traits that require structure to achieve the optimal outcomes. This will in turn require specific identification of discretionary conditions, with a very low tolerance by the treating team to return the patient to hospital on breach of the conditions. This raises the difficulty of judging when a slight deviation from the care plan should result in a breach of the discretionary conditions and lead to a recall. Does the CTO form part of the care plan or does the care plan form part of the CTO? The Code of Practice for Wales does note that a patient may be recalled without an actual breach of the discretionary conditions if there is a deterioration of health that needs to be prevented. 16
It becomes increasingly clear that clinicians use the majority of CTOs in the intended way, to deal with adherence to treatment, but a sizeable minority of CTOs appear to address risk behaviour. Reference Malik and Hussein17,Reference Lepping18 In other words, the conditions are designed to manage and mitigate risk arising from behaviour rather than non-adherence. In the absence of convincing randomised controlled trial results looking at outcomes or the use of CTOs, it remains to be seen whether they are able to achieve the intended aim. The evidence to prove whether they are able to avoid repeat admissions is ambiguous, and even less is known about whether they can help to mitigate risk. The available evidence is primarily from other countries, particularly the USA and Australia, where treatment as usual, as well as the actual community legislation cannot easily be compared with CTOs in England and Wales. Reference Churchill, Owen, Singh and Hotopf3 However, given that many patients are put on CTOs without a history of recurrent admissions and evidently for risk management purposes, it is clear that clinicians use CTOs in two different ways. Interestingly, there have been three serious incidents that have arisen with patients while on a CTO in North Wales. Two of these incidents arose in situations where CTOs were primarily used to manage risk rather than deal with adherence issues.
Box 1 SMART framework

| To accept depot medication | To see care team | |
| Specific | To accept a (depot) antipsychotic medication every 2 weeks | To see keyworker 2 times per week. The content of the session will be specific to your needs, i.e. social or clinical |
| Measurable | The dose will be confirmed with you and specified in your care plan | Engagement will be noted |
| Achievable | Your mental health and the side-effects of the medication will be monitored by the community psychiatric nurse who administers the depot medication | Any difficulties will be discussed with the multidisciplinary team and practicable steps taken to enhance your recovery by effective participation with the care plan |
| Realistic | A fixed date, time and venue will be confirmed with you prior to the administration of the depot | A fixed date, time and venue will be confirmed with you prior to the appointments |
| Time framed | This treatment plan will be reviewed every 3 months in the out-patient clinic | This treatment plan will be reviewed every 3 months in the out-patient clinic |
The SMART framework
Community treatment order conditions as yet do not have a robust evidence base to guide the creation of discretionary conditions. We would like to suggest a simple set of goals (the SMART framework: Specific, Measurable, Achievable, Realistic, Time framed) that we hope will help clinicians to increase the robustness of the chosen conditions within the codes of practice of the Mental Health Act. We hope that our suggestions will help to ensure that any condition placed on a patient has a specific purpose, is reviewed regularly, and may help in focusing practitioners’ planning of medical treatment. We use medication and monitoring as examples as they were the two most common discretionary conditions that emerged from the audit (Box 1). It is hoped that the SMART framework can be applied to all potential discretionary conditions.
We believe that the SMART framework places a structure on the conditions and may be able to address adherence and risk in a format that is acceptable to the patient and ensures cooperation with the conditions in order to make the CTO a viable treatment option. The alternatives would either be extended Section 17 leave, guardianship or in-patient care waiting for absolute discharge.
Conclusions
There is good evidence to suggest that clinicians use CTOs much more than expected. They use the conditions placed on patients in order to (a) ensure adherence to treatment and (b) to mitigate risk. These are two very different purposes. It is so far unclear whether those two aims can realistically be achieved by using CTOs. They should clearly be examined separately in future research projects in order to guide their clinical use.
Acknowledgement
We would like to thank Rebecca Hoofe for her secretarial support.




eLetters
No eLetters have been published for this article.