INTRODUCTION
Helicobacter pylori, a Gram-negative bacterium found on the luminal surface of the gastric epithelium, induces chronic inflammation of the underlying mucosa. The infection is usually contracted during childhood or adolescence [Reference Miendje Deyi1] and tends to persist lifelong unless treated. Its prevalence increases with older age and lower socioeconomic status and varies markedly around the world. H. pylori is responsible for the development of duodenal and/or gastric ulcers (reported to develop in 1–10% of infected patients) as well as a co-factor of gastric cancer (in 0·1–3%) and gastric mucosa-associated lymphoid-tissue lymphoma (in <0·01%) [Reference McColl2]. However, the majority of patients with H. pylori infection will not have any clinically significant complication.
A minority of patients with dyspepsia, infected with H. pylori, have an underlying ulcer disease [Reference Perri and Andriulli3]. It is essential to determine the H. pylori status with regard to adequate therapy. Two types of tests are available: invasive (endoscopic) tests and non-invasive (non-endoscopic) tests.
In our previous paper [Reference Miendje Deyi1], a large retrospective observational study was performed by extracting data from a laboratory database covering a third of Brussels and the surrounding population. The study included subjects attending several digestive endoscopy centres in Brussels during a 20-year period (1988–2007). The criterion for entry in the database was the initial screening of H. pylori infection by culture of gastric biopsy, performed at a central clinical microbiology laboratory. The higher prevalence in older age groups of immigrants or in children born to immigrant families compared to the population of Belgian origin is thought to reflect a cohort effect related to poorer living conditions of children in previous decades.
The same database was used to analyse the child population (aged <18 years at initial biopsy) whenever a subsequent endoscopy was recorded during the 20-year study period.
The main objectives are to describe:
-
• The risk of persistence of H. pylori after a first positive result.
-
• The risk of acquiring H. pylori colonization in subjects with an initial negative result.
-
• The risk of re-infection/relapse in subjects with successful ‘eradication’ treatment.
-
• The effect of age, gender, geographical origin, time period on the persistence, acquisition or re-infection/relapse risk of H. pylori colonization.
METHODS
Patients
The study group was derived from the initial database as published in our previous paper [Reference Miendje Deyi1] and restricted to paediatric patients (<18 years). Briefly, the source of data collection was the medical laboratory of Brugmann University Hospital in Brussels. Since 1984, the hospital has served as the H. pylori reference centre for a large number of institutions (3147/9175 hospital beds in Brussels) [Reference Taymans4]. Patients originated from several Belgian cities, with the majority (80%) from Brussels. Administrative (including geographical origin) and microbiological data were collected for each patient. The indication for gastrointestinal endoscopy included various gastrointestinal complaints not necessarily associated with H. pylori. Only patients with at least one interpretable result (either positive or negative) by H. pylori culture were included.
Data on the evolution of antibiotic treatment over this lengthy period have been published previously in 2001, 2007 and 2011 [Reference Bontems5–Reference Bontems7]. Before 1995, treatments were usually dual therapies [amoxicillin + (clarithromycin or metronidazole)], tailored to the antimicrobial susceptibility from the early 1990s. Proton pump inhibitors (omeprazole) were then added to the regimens before switching to sequential treatments gradually from 2007 [Reference Bontems7].
Biopsy specimens and H. pylori isolation
The Brussels laboratory receives gastric (antrum±fundus) biopsy specimens for culturing of H. pylori. Briefly, each biopsy specimen was ground in sterile distilled water. The final suspension was inoculated on in-house selective agar plates. The plates were then incubated for 3–7 days at 37°C under a humid, micro-aerobic atmosphere. The culturing was extended to 10 days if there was a known positive urea test. The typical growth of H. pylori was checked after 3 days and on a daily basis thereafter. Susceptibility testing was performed mainly using the disc diffusion method for several antibiotics including clarithromycin and metronidazole as described previously [Reference Miendje Deyi, Van Den Borre and Fontaine8, Reference Miendje Deyi9].
Statistical analysis
All data related to the patients (demography, H. pylori culture) were transferred from the laboratory information system to Excel 2000 (Microsoft, USA). The database was analysed with the Statistical Package for the Social Sciences version 18.0.1 (PASW Statistics, USA).
Differences of medians for continuous variables were analysed by Mann–Whitney U test. Differences of ⩾2 proportions for categorical variables were analysed, respectively, with Fisher's exact test and Pearson's χ 2 test.
Survival function: a database for survival analysis was constructed by aggregating all subjects monitored at least once after their initial screening biopsy.
Persistence rate was measured in subjects with an initial positive H. pylori result. Time to event was defined as the interval between initial biopsy and the timing of the first negative H. pylori culture. Subjects remaining positive were censored at their last positive H. pylori culture.
Acquisition and re-infection/relapse rates of H. pylori infection were measured, respectively, in subjects having an initial negative H. pylori result (acquisition) and in subjects initially infected after a first documented cure (re-infection/relapse). Time to event (diagnosis of H. pylori infection) was defined as the interval between initial biopsy (acquisition) or first cure (re-infection/relapse) and the timing of first subsequent positive H. pylori culture. Subjects remaining negative were censored at their last negative H. pylori culture.
Comparison of survival tables was performed with the Kaplan–Meier method and the P value was determined by log-rank test.
Cox regression analysis [Reference Kleinbaum and Klein10] with proportional hazards assumption was performed to measure the effect of variables on time-dependent risk of H. pylori infection in the three groups mentioned above (Persistence, Acquisition, and Re-infection/relapse).
All statistical tests were two-sided P values without correction for multiplicity of tests.
RESULTS
During the study period (Table 1), 4964 patients initially aged <18 years underwent an upper gastrointestinal endoscopy with gastric biopsy (antrum±fundus) and H. pylori culture. Median age was 7·9 years with an interquartile range of 3·3–12·0 years. Slightly more than a third (39·9%) of subjects were aged <6 years and a quarter (24·9%) were aged 12–17 years. Most patients (70·3%) were of non-European origin and sex ratio was close to unity. The data collection covered the period between January 1988 and December 2007, with a steady increase in the number of subjects during each 5-year period. Out of the initial group of 4964 patients, at least one subsequent upper gastrointestinal endoscopy with gastric biopsy and H. pylori culture was obtained in 922 subjects (18·6%). The majority (586/922, 65·6%) were examined twice while repeated biopsies with H. pylori culture reaching ⩾7 were performed for 25 patients.
Characteristics
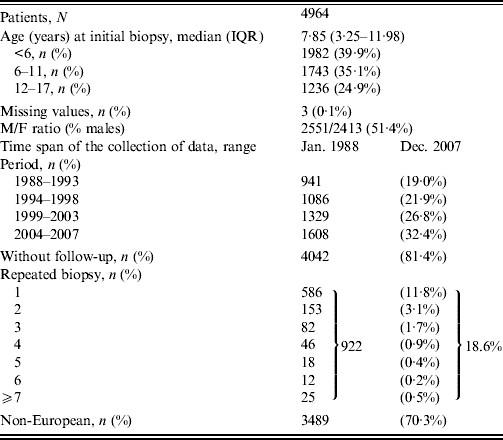
IQR, Interquartile range.
The comparison between the patients stratified according to their initial H. pylori status shows that patients initially non-infected were 3·7 years younger than those with an initial positive H. pylori culture (Table 2). The proportion of infected children increased with age (18·2% in children aged <6 years and 49·3% in adolescents aged 12–17 years) (P < 0·001). Girls were more often infected than boys (57% vs. 43%) (P < 0·001). The prevalence of H. pylori infection in the investigated children strongly decreased over the different time periods. Non-European origin was documented in 86·5% of children with an initial positive H. pylori result and in 60·7% of children with an initial negative result (P < 0·001). Antibiotic resistance was documented in 12·2% of cases for clarithromycin and in 20·9% of cases for metronidazole.
Baseline characteristics in 922 patients with repeated gastric biopsies and Helicobacter pylori culture
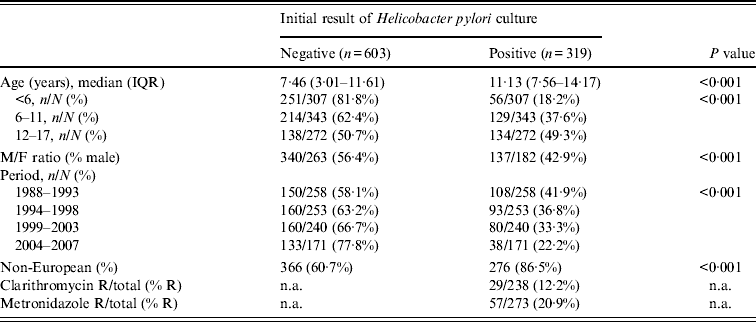
IQR, Interquartile range; n.a., not applicable.
R/total = ratio of number of antibiotic non-susceptible strains and total number of antibiograms.
% R = per cent non-susceptible.
The effect of four variables (age, gender, period, geographical origin) on the time course of H. pylori acquisition, persistence and re-infection/relapse during follow-up was analysed with Cox proportional hazards regression (Table 3). Non-European origin had a marked effect on the hazard of H. pylori acquisition (P < 0·001). None of the four variables had a significant effect on persistence rate after an initial positive biopsy. Female gender had a significant decreasing effect on the relapse/re-infection hazard rate (P = 0·028). Antibiotic resistance (clarithromycin and metronidazole) was also introduced in the multivariate analysis: neither had a significant effect on persistence or re-infection/relapse of H. pylori infection (data not shown).
Time-dependent multivariate analysis of Helicobacter pylori risk
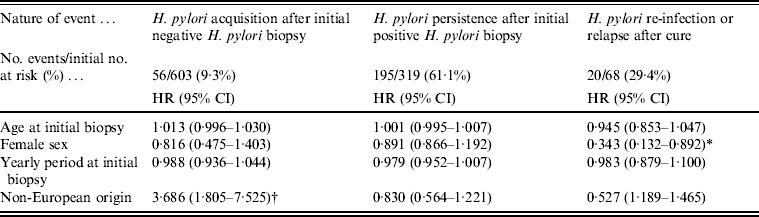
HR, Hazard ratio; CI, confidence interval.
† P < 0·001.
* P = 0·028.
Comparison of H. pylori antibiotic susceptibility profile at initial and last biopsy demonstrated a strong association of initial susceptibility with last susceptibility, with a pattern independent of geographical origin (European vs. non-European) (Table 4). In paired biopsy samples of the same subject, when initial biopsies contained non-susceptible H. pylori strains to clarithromycin or metronidazole, 83.3% and 82.0% of H. pylori obtained at last biopsy, respectively, were also non-susceptible to either antibiotic. By contrast, when initial biopsies contained susceptible H. pylori strains to either antibiotic, 10·2% strains for clarithromycin and 12·6% strains for metronidazole became non-susceptible at last biopsy. Within the 226 paired clarithromycin susceptibility tests, it can be calculated (by rearranging the numbers in last column of Table 4) that the number of non-susceptible H. pylori increased from 30 (13·3%) initial positive results to 48 (21·2%) last positive results (P = 5·08 × 10−4). In parallel, within the 223 paired metronidazole susceptibility tests, the number that were non-susceptible increased from 61 (27·3%) to 78 (35·0%) (P = 1·42 × 10−2).
Comparison of Helicobacter pylori non-susceptibility in paired samples at initial and at last biopsies in subjects stratified by geographical origin
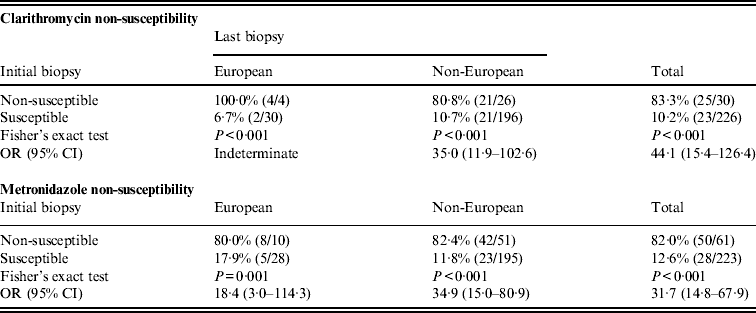
OR, Odds ratio; CI, confidence interval.
Percentages of susceptibility and of non-susceptibility to either antibiotic at initial biopsy did not differ in European children and in non-European children (P > 0·10).
In the group of 319 subjects initially positive for H. pylori and biopsied at least once subsequently, the risk of persistent H. pylori infection at 1 year after an initial positive biopsy was greater in the last period 1998–2007 (72·7%) than in the preceding period 1988–1997 (45·8%) (P = 1·96 × 10−3). The proportion of persistence decreased markedly to 16·5% at 10 years (Fig. 1), with the curves of both periods overlapping.
Comparison of Helicobacter pylori persistence in children (<18 years) according to the period of initial biopsy. Event = first negative H. pylori biopsy after an initial positive biopsy. n.a., Not available.

Of the 603 subjects initially free of H. pylori infection, 38·7% became infected within 12 years (Fig. 2, acquisition group). In 68 subjects with a documented cure of H. pylori infection, 48·6% relapsed within 5 years of follow-up (Fig. 2, re-infection/relapse) (P = 3·8 × 10−6).
Comparison of Helicobacter pylori acquisition in a cohort of 603 subjects with an initial negative biopsy and of H. pylori re-infection/relapse in a cohort of 68 subjects with an initial positive biopsy after documented cure. Event = first positive H. pylori biopsy after initial negative biopsy (acquisition) or after first documented cure (re-infection/relapse). n.a., Not available.

DISCUSSION
Persistence of H. pylori infection after an initial positive biopsy
In clinical practice, the term ‘eradication’ is used for negative H. pylori tests at least 4–8 weeks after treatment [Reference McColl2]. In fact, many studies document persistence of H. pylori infection in the follow-up of patients even after appropriate treatment [Reference Moya and Crissinger11–Reference Ryu16]. In our clinical team, the antibiotic protocol evolved according to successive guidelines, and remained based on a combination of amoxicillin+clarithromycin or metronidazole+omeprazole. The proportion of efficient treatment increased markedly in our last data, 81·9% being adequately treated as documented by a negative 13C breath test 8 weeks after treatment [Reference Bontems7]. Other large series show that over one third of patients do not eliminate their H. pylori infection with antibiotic treatment [Reference Oderda17].
The apparent greater risk of persistence of H. pylori infection in the present analysis during the more recent period (1998–2007 vs. 1988–1997) was, therefore, not an effect of decreased antibiotic efficacy, but probably resulted from a modification of patient selection. With the introduction of non-invasive testing such as the 13C-urea breath test [Reference Cadranel18], the indication of H. pylori culture on gastric biopsy is more restricted, with a better tailoring of patients in the recent period (1998–2007) vs. the preceding period (1988–1997). Our data should not be considered representative either of the general population or of the subpopulation infected by H. pylori, but only of the subgroup of subjects exposed to gastric biopsy and H. pylori culture in our Brussels series. Only a small percentage (18·6%) of subjects were monitored with repeated endoscopies after the first diagnosis of H. pylori and the majority of the initial cases were not followed up by this invasive technique. A non-invasive technique such as the 13C-urea breath test is preferred since its validation in the last decade of the 20th century.
Our patient group is representative of everyday clinical practice. H. pylori initially isolated at biopsy remained positive in many cases (18·1% as estimated by the 13C-urea breath test [Reference Bontems7]), and this persistence is confirmed in most cases when H. pylori culture on gastric biopsies are performed. Despite a clinical follow-up of patients according to current international guidelines, it appears that around a fifth of patients remain infected, at least after the first antibiotic therapy. More encouraging is when some of these subjects are re-evaluated later (i.e. after subsequent antibiotic therapies), the proportion of positive H. pylori cultures decreased markedly. The cumulative proportion of elimination of the pathogen as documented by gastric biopsy and H. pylori culture reached 84% at 10 years. Spontaneous cure of H. pylori infection – without antibiotic therapy – is rare.
Compared to the urea breath test and histology, our in-house culture method yielded 98% sensitivity and 100% specificity [Reference Miendje Deyi, Van Den Borre and Fontaine8] and, moreover, it was recently found to be equally efficient and more selective than two commercially available media [Reference Miendje Deyi9]. The performance of these diagnostic tests strongly supports the view that the data are expected to be similar whenever invasive or non-invasive tests are performed.
Acquisition and relapse rates of H. pylori infection
H. pylori infection is mainly acquired during childhood and adolescence. In our previous analysis [Reference Miendje Deyi1] based on initial results of H. pylori culture, an annual incidence of H. pylori of 15% per person-year was estimated in subjects of non-European origin in whom there was an indication for gastric biopsy and H. pylori culture. A fourfold lower incidence was calculated in subjects of European origin. The present data, based on follow-up (time 0 and subsequent H. pylori culture), show that an initial negative gastric biopsy does not predict a long-term absence of infection: 39% became H. pylori positive during a 10-year follow-up (Fig. 2). This result corresponds to ∼4% annual incidence rate of infection [Reference Miendje Deyi1], close to the incidence reported in a recent review [Reference Moya and Crissinger11]. The multivariate analysis shows that the risk of acquisition is 3·7 times greater in the population of non-European origin: this result confirms strongly the fourfold greater risk of H. pylori infection previously calculated in non-European subjects [1).
After a documented cure of infection, about half of the subjects relapsed within 5 years of follow-up. Again, due to type of selection of patients, the extrapolation of this percentage should be limited to the subjects for whom there was a clinical indication for biopsy and H. pylori culture. In these two groups, the pattern of acquisition or re-infection/relapse was similar in both periods (1988–1997 vs. 1998–2007), with no statistically significant difference (data not shown).
Effect of age, gender, time period, geographical origin
In our previous analysis, the risk of H. pylori-positive biopsy was associated with geographical origin (non-European origin – immigrants mainly from Maghreb in Brussels). The same association was observed in the present analysis: non-European origin had a significant effect on the acquisition rate of H. pylori infection. Besides this association, a decreased risk of re-infection/relapse in females was documented, with a modest P value (P = 0·028). Due to the multiplicity of association tests, this result requires further confirmation and should not be considered definitive.
Limitations of the study and new questions
Our analysis clearly belongs to descriptive epidemiology and, consequently, is limited to generation of a hypothesis not to allowing definitive conclusions. The analysis of data was based on a laboratory information system database: it is not possible to infer to what extent this population is representative of the entire group of patients infected with H. pylori. Clinical outcomes other than those linked to H. pylori infection clearly influence the recruitment in the database.
Nevertheless, the main message seems sufficiently strong to be accepted: if elimination of H. pylori by current treatment is the objective, eradication of this pathogen over the long term remains uncertain.
One of the long-term complications of H. pylori infection is gastric carcinoma [Reference Peeters19]. The elevated long-term recurrence of infection might explain the paradoxically low preventive effect of H. pylori elimination on gastric carcinoma [Reference Mazzoleni, Francesconi and Sander20]. Even if it is well established that antimicrobial therapy reduces markedly the recurrence of duodenal ulcer in H. pylori-positive subjects [Reference Hentschel21], our data suggest that repeated follow-up testing over the long term is indicated in order to detect the persistence or recurrence of the pathogen after several years. Non-invasive tests (13C-urea breath test and faecal antigen) allow easier regular repeated long-term follow-up of patients after a successful treatment of H. pylori. Furthermore, a multi-centre prospective study should be organized to confirm these results.
Our data cannot distinguish whether the infection is due to the persistence or recurrence of the initial strain, or to a re-infection with a different one. As there was an elevated risk association of antibiotic resistance in the first biopsy and in the last one, these data suggest strongly that a relapse occurred most of the time rather than a re-infection.
DECLARATION OF INTEREST
None.







