Introduction
Approximately 136 million women give birth to a live or stillborn baby every year (World Health Organization, 2005) with 4.5 million of these births occurring in North America and 5.4 million in Europe (European Commission, 2011; UNdata, 2011). There is now substantial evidence that women can suffer from a range of psychological problems during this time. Postpartum depression is most widely recognized and affects between 10 and 15% of women (Gavin et al. Reference Gavin, Gaynes, Lohr, Meltzer-Brody, Gartlehner and Swinson2005). There is also evidence that women are more vulnerable to anxiety and adjustment disorders (Brockington, Reference Brockington2004; Wenzel et al. Reference Wenzel, Haugen, Jackson and Brendle2005; Brockington et al. Reference Brockington, Macdonald and Wainscott2006). Maternal mental health problems are usually higher in low- and middle-income countries – particularly women in socially and economically disadvantaged circumstances (Fisher et al. Reference Fisher, Cabral de Mello, Patel, Rahman, Tran, Holton and Holmes2011).
The causes of maternal mental health problems are multifactorial and include individual vulnerability factors, such as previous psychological problems, and psychosocial circumstances, such as socio-economic deprivation, intimate partner violence or other chronic stressors. In some instances the events of birth may also contribute to postpartum adjustment problems and mental health disorders. There is increasing evidence that some women develop post-traumatic stress disorder (PTSD) in response to events of birth (Ayers & Pickering, Reference Ayers and Pickering2001; Alcorn et al. Reference Alcorn, O'Donovan, Patrick, Creedy and Devilly2010). Reviews of this research suggest it affects 3.17% of women postpartum (Grekin & O'Hara, Reference Grekin and O'Hara2014). Unlike other postpartum psychopathology, this is therefore an area where there is clear potential to prevent or minimize postpartum PTSD by changing maternity and early postpartum care to improve women's experiences of birth. However, in order to do this we first need to identify the risk factors for birth-related PTSD.
Conceptual frameworks of the aetiology of postpartum PTSD draw together key vulnerability, risk and maintaining factors that are thought to be important in the development of birth-related PTSD (Ayers, Reference Ayers2004; van Son et al. Reference van Son, Verkerk, van der Hart, Komproe and Pop2005; Slade, Reference Slade2006). These usually draw on psychological approaches, such as the diathesis–stress model which explains health outcomes as an interaction between an individual's predispositional vulnerability and stressful experiences. In a previous paper, we used a diathesis–stress approach to propose a model of postpartum PTSD that incorporates vulnerability factors in pregnancy, risk factors during birth, and maintaining factors after birth in the onset and maintenance of PTSD (Ayers, Reference Ayers2004). Vulnerability factors in pregnancy were specified as previous psychological problems, a history of trauma or sexual abuse, anxiety and having a first baby (nulliparity). These vulnerability factors are proposed to interact with birth events to determine appraisal of birth as traumatic, and subsequent traumatic stress responses. Birth risk factors were specified as type of birth (as a broad indicator of level of intervention and complications), poor support, high levels of negative emotion, perceived threat, and dissociation. Postpartum factors that might maintain initial PTSD symptoms were specified as additional stress, maladaptive coping and poor support (Ayers, Reference Ayers2004).
Evidence broadly confirms the associations between the factors outlined above and postpartum PTSD (Wijma & Wijma, Reference Wijma, Söderquist and Wijma1997; Creedy et al. Reference Creedy, Shochet and Horsfall2000; Czarnocka & Slade, Reference Czarnocka and Slade2000; Söderquist et al. Reference Söderquist, Wijma and Wijma2002, Reference Söderquist, Wijma, Thorbert and Wijma2009; Cohen et al. Reference Cohen, Ansara, Schei, Stuckless and Stewart2004; Cigoli et al. Reference Cigoli, Gilli and Saita2006; Lev-Wiesel et al. Reference Lev-Wiesel, Chen, Daphna-Tekoah and Hod2009a ). Very few studies have looked at the interaction between vulnerability and risk factors. Those studies that have done so are consistent with the idea that trauma history interacts with birth intervention to increase risk of PTSD after birth (Ayers et al. Reference Ayers, Harris, Sawyer, Parfitt and Ford2009; Ford & Ayers, Reference Ford and Ayers2011). Likewise, support during birth can mediate the relationship between previous trauma and birth-related PTSD; as well as the relationship between birth intervention and postpartum PTSD (Ford & Ayers, Reference Ford and Ayers2011).
Overviews of factors associated with postpartum PTSD have been provided in various narrative reviews (Bailham & Joseph, Reference Bailham and Joseph2003; Ayers, Reference Ayers2004; Olde et al. Reference Olde, van Der Hart, Kleber and van Son2006; Andersen et al. Reference Andersen, Melvaer, Videbech, Lamont and Joergensen2012) and a meta-analysis (Grekin & O'Hara, Reference Grekin and O'Hara2014). The meta-analysis looked at risk factors for PTSD in postpartum women who reported PTSD in response to a range of traumatic stressors, including childbirth (Grekin & O'Hara, Reference Grekin and O'Hara2014). This reviewed 78 studies which reported prevalence and/or risk factors for PTSD and analysed risk factors for PTSD separately in community or high-risk samples. The authors concluded that the main factors associated with PTSD in community samples were birth experiences and postpartum depression. In high-risk samples the main factors were infant complications and postpartum depression. These results of this meta-analysis highlight the co-morbidity between postpartum PTSD and depression, and are broadly consistent with the vulnerability and risk factors outlined in the diathesis–stress model with the exception of parity, which was not found to moderate prevalence rates. However, this meta-analysis did not focus on birth-related PTSD and therefore understandably did not examine all the factors proposed to be important by models of birth-related PTSD, such as dissociation, postpartum stress and maladaptive coping. The most recent review of evidence focusing on birth-related PTSD was carried out by Andersen et al. (Reference Andersen, Melvaer, Videbech, Lamont and Joergensen2012) who concluded that subjective distress during labour and obstetric emergencies are the main risk factors for birth-related PTSD. Other risk factors included poor support during birth and complications with the baby. Vulnerability factors were a history of trauma or psychological problems in pregnancy (Andersen et al. Reference Andersen, Melvaer, Videbech, Lamont and Joergensen2012). Again, this is broadly consistent with the diathesis–stress model but no meta-analyses were conducted.
These reviews provide useful syntheses of research and promising evidence towards refining the diathesis–stress model of the aetiology of birth-related PTSD. The amount of evidence available means that meta-analyses are now possible and the meta-analysis by Grekin & O'Hara (Reference Grekin and O'Hara2014) provides a valuable overview of postpartum PTSD regardless of the trigger event. What is needed now is a more detailed meta-analysis of all the vulnerability and risk factors for birth-related PTSD proposed by the diathesis–stress model, and examination of a wider range of co-morbid symptoms. Methodological and sampling differences also need to be considered. This review and meta-analysis therefore has three aims. The first is to systematically review and identify the effect sizes for vulnerability and risk factors for birth-related PTSD symptoms and update the diathesis–stress model of birth-related PTSD. The second is to examine the association between birth-related PTSD and co-morbid symptoms. The third is to examine methodological and individual factors that might moderate these relationships. In doing so the review will identify the critical vulnerability and risk factors that put women at risk of developing birth-related PTSD symptoms, and therefore which women may need additional support and care during birth. The results will inform understanding and clinical practice by highlighting vulnerability factors to screen for in pregnancy; those elements of maternity services that can be targeted for most effective prevention; and which vulnerability or risk factors that perinatal psychology services may need to incorporate into assessment and treatment of birth-related PTSD.
Method
Selection of studies
A systematic search was conducted to identify studies of PTSD in women following childbirth. Computerized databases PsycINFO, PubMed, Scopus and Web of Science were searched up to March 2015 using terms related to PTSD (posttraumatic stress, post-traumatic stress, trauma*, PTSD) crossed with childbirth-related terms (birth, pregnancy, partum, postpartum, prenatal, postnatal, stillbirth, miscarriage, gestation, partus, labor). Additional studies (n = 40) were located through inspecting references and citations of key publications. Fig. 1 summarizes results of the search which yielded a preliminary database of 8044 papers. Of these, 6836 were excluded from the title as not relevant to childbirth. These were predominantly animal studies or occupational studies of work labour/labour. This left a database of 1208 papers of which examination of abstracts showed that 785 did not meet inclusion criteria, leaving 423 papers where the full text was examined to determine eligibility.
Flowchart of systematic search. PTSD, Post-traumatic stress disorder.
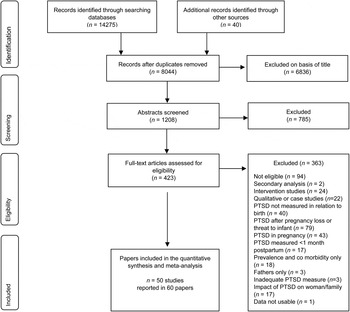
Inclusion and exclusion criteria
Inclusion criteria were that papers reported primary research that included a quantitative measure of birth-related PTSD taken at least 1 month after birth to exclude confounding with acute stress disorder. Research had to be with women 18 years of age or over, and published in English. Papers were excluded if they were qualitative or case studies, reviews or discussion papers, dissertations, conference abstracts, or only measured PTSD in pregnancy. Intervention studies were excluded unless they reported relationships between PTSD and risk factors prior to the intervention (n = 0). Control-comparison papers were excluded if the PTSD group was selected on the basis of non-standard cut-offs for subclinical symptoms. Studies on high-risk samples where all women had experienced pregnancy loss, stillbirth or severe complications with the baby (e.g. all preterm births or very low-birth-weight babies) were excluded to avoid potential confounding with traumatic bereavement or perceived threat to the baby rather than self. It is also possible that different factors are associated with the development of PTSD after loss of a baby (Daugirdaite et al. Reference Daugirdaite, van den Akker and Purewal2015).
Studies had to report the correlation coefficient r or odds ratio, or sufficient statistical information to compute these statistics. Authors of papers with unclear statistical information (n = 16) were contacted to request further information. Half these authors provided the data requested where available (n = 8)Footnote 1 Footnote †. Where data were not available these effects or the study were excluded (n = 1; Leeds & Hargreaves, Reference Leeds and Hargreaves2008). Longitudinal studies which measured PTSD at different time points were included and effect sizes taken from the shortest time between measurement of risk factors and PTSD. Thus concurrent and longitudinal relationships were included in the analyses and time between measures of risk and PTSD was examined as a potential moderator.
Variables coded
A number of variables were extracted for analysis. Detailed information on coding is given in online Supplementary File S1.
Sample characteristics extracted were: country of origin, clinical status of the sample, age, ethnicity, marital status, education and socio-economic status. Clinical status was classed as low risk, normal risk or high risk.
Methodological variables extracted were: methodological quality, design (cross-sectional or longitudinal), recruitment (antenatal or postnatal), sampling (via the Internet or community), sample size and time-frame of the effect size (i.e. months elapsed between the measure of risk and PTSD).
PTSD measures were coded for quality (0 to 3). Questionnaire measures that did not measure all symptoms of PTSD and included items that are not part of diagnostic criteria were scored 0; questionnaire measures of PTSD symptoms but not full diagnostic criteria scored 1; questionnaire measures of all diagnostic criteria scored 2; and clinical interviews scored 3.
Birth variables extracted included: objective birth experience, subjective birth experience, type of birth (operative or normal vaginal), length of labour (hours), pain, complications with the baby, presence of partner, dissociation during birth, and support from staff during birth. Subjective birth experience included: (i) overall ratings of birth experience; (ii) negative emotions and distress; and (iii) control and agency.
Vulnerability factors extracted were in four domains. The first domain was prior history and included history of traumatic events, PTSD, sexual abuse or psychological problems. The second domain was vulnerability due to poor mental health in pregnancy. These variables were depression in pregnancy, anxiety in pregnancy, fear of childbirth and counselling for problems associated with a previous pregnancy/birth. The third domain was pregnancy-related vulnerability which included: being primiparous, whether the pregnancy was planned, poor physical health in pregnancy, and problems in a previous pregnancy/birth. The final domain was psychosocial vulnerability which included coping and stress, and social support.
Co-morbid symptoms included depression, anxiety, general psychological health and physical health.
Potential moderators of clinical status of the sample, quality of PTSD measure, and time between measuring risk factors and PTSD were also extracted.
Methodological quality
Methodological quality of each study was assessed using a checklist based on Sawyer et al. (Reference Sawyer, Ayers and Field2010) and Andersen et al. (Reference Andersen, Melvaer, Videbech, Lamont and Joergensen2012). Nine criteria were assessed of: clear study aims; clear inclusion/exclusion criteria; method of data collection; measure of PTSD; sample representativeness; response rate; examination of bias in participants who did not take part or dropped out; prospective design; more than one postpartum data collection point (each rated from 0 to 3; total score 0–27). Most studies were of reasonable or good quality with 70% (n = 35/50) scoring over the mid-point of 14 or more (see Table 1).
Characteristics of studies included in the meta-analysis

PTSD, Post-traumatic stress disorder; Quality, Methodological Quality Score, possible scores: 0–27; NR, not reported in the study; MINI, MINI International Neuropsychiatric Interview; PDS, Posttraumatic Diagnostic Scale; PSS-SR, Post-Traumatic Stress Disorder Symptom Scale-Self Report; APTSD-Q, Adjusted Post-Traumatic Stress Disorder Questionnaire; IES, Impact of Event Scale (original version); PTSD-Q, Post-Traumatic Stress Disorder Questionnaire; DTS, Davidson Trauma Scale; IES-R, Impact of Event Scale (revised version); SRIP, Self-Rating Inventory for Posttraumatic Stress Disorder; PPQ, Perinatal PTSD Questionnaire; PCL, Posttraumatic Stress Disorder Checklist; PSS-I, Posttraumatic Stress Scale Interview; PCL-C, Posttraumatic Stress Disorder Checklist-Civilian Version; TES, Traumatic Event Scale; PTCS, Posttraumatic Childbirth Stress Inventory.
a Timing of PTSD measure.
b For longitudinal studies, time point(s) used for analysis.
c Time point not coded for analysis if range greater than 3 months.
Computation and analysis of effect sizes
The majority of effect sizes were reported as Pearson correlation coefficients, although some used odds ratios or rank correlations. Odds ratios were therefore converted to r and rank correlations were treated as equivalent to Pearson correlationsFootnote 2 . The effect size for all studies was therefore r. To ensure this approach did not influence results, we conducted analyses separately for r and odds ratios and they did not differ appreciably. A few studies reported correlation coefficients only for symptom subscales of PTSD. Therefore to guarantee the independence assumption among effect sizes the coefficients were averaged to produce a single effect size associated with overall PTSD.
In meta-analysis, there is a choice between fitting either fixed-effect or random-effect models (Hedges & Vevea, Reference Hedges and Vevea1998; Hunter & Schmidt, Reference Hunter and Schmidt2004; Borenstein et al. Reference Borenstein, Hedges, Higgins and Rothstein2010). Random-effects models are more usually recommended because it is likely that there is heterogeneity in the population effect sizes as a consequence of differences in, for example, study design and the measures used. However, Hedges & Vevea (Reference Hedges and Vevea1998) point out that it is not the presence of heterogeneity per se that should influence the choice of a fixed- or a random-effects model. Rather, the issue is which population we wish to make inferences to. In a fixed-effects model, inference is confined to the set of studies included in the analysis whereas in a random-effects model inference can be made to a broader population from which the studies included in the analysis may be considered a random sample. However, a random-effects model can be problematic when the number of studies is small because, in comparison with a fixed-effects model, the variability between population effect sizes is also estimated and, with limited numbers of studies, this estimate will be imprecise and can provide misleading results (Borenstein et al. Reference Borenstein, Hedges, Higgins and Rothstein2009). We therefore decided to use a fixed-effects model and confine inference to the set of study characteristics present in our sampleFootnote 3 . In analysing correlations, we use the Fisher z transformation for the analysis (Lipsey & Wilson, Reference Lipsey and Wilson2001) and an integral z-to-r transformation for converting our results back to the r metric (Hafdahl, Reference Hafdahl2009). Moderator analyses were also conducted using a fixed-effects general linear model on the z-transformed effect size. Analyses were carried out with the Metafor package in R (Viechtbauer, Reference Viechtbauer2010).
Results
Study characteristics
In all, 50 studies, reported in 60 papers, met inclusion criteria with a total of 21 429 participants. Studies included in the meta-analysis are listed in Table 1. Sample sizes of studies ranged from 40 to 3751 and studies were carried out in the UK (n = 12), the Netherlands (n = 7), Sweden (n = 6), USA (n = 4), Canada (n = 3), Israel (n = 3), Italy (n = 3), Australia (n = 2), France (n = 2), Iran (n = 2), Switzerland (n = 2), Austria (n = 1), Germany (n = 1), Norway (n = 1) and Nigeria (n = 1). Most studies were longitudinal (n = 36, 72%). Samples predominantly included white women (range 0 to 100%; mean 80.65% white) with a mean age of 30.41 (s.d. = 1.82) years. Women were mostly cohabiting or married (range 80 to 100%, mean 93.36%). On average, 32.76% of samples had university-level qualifications (range 7.6 to 68.5%). Most studies were on normal populations, with 10 (20%) on high-risk groups and three (6%) on low-risk groups. Samples were mixed in terms of parity (range 21 to 100% primiparous, mean 58.47%).
Vulnerability and risk factors for postpartum PTSD
The results of the meta-analyses are shown in Table 2 which gives the number of effects included (k), the effect size (r), and lower and upper confidence limits of the effect size. In this analysis, k is equivalent to the number of studies because only one effect was entered per study. Q e gives the residual heterogeneity so if it is significant it suggests the heterogeneity in effect sizes is greater than expected from sampling variation and there are likely to be moderators of the effect.
Meta-analysis of factors associated with postpartum PTSD (fixed-effects model)

PTSD, Post-traumatic stress disorder; k, number of effect sizes; CI, confidence interval; LL, lower confidence limit of the effect size; UL, upper confidence limit of the effect size; Q, heterogeneity statistic; df, degrees of freedom.
a When the study from Nigeria (Adewuya et al. Reference Adewuya, Ologun and Ibigbami2006) was removed effect sizes differed slightly for poor health/complications in pregnancy (k = 8, r = 0.23, 95% CI 0.20–0.26), control or agency in birth (k = 4, r = −0.35, CI −0.42 to −0.28) and education level (k = 5, r = −0.25, 95% CI −0.29 to −0.22).
b Medium effect sizes of ⩾ 0.3.
c Poor coping and stress were measured in pregnancy and after birth in different studies.
* p ⩽ 0.05.
Vulnerability factors during pregnancy that were most strongly associated with birth-related PTSD were depression in pregnancy (0.51), fear of childbirth (0.41), poor health or complications in pregnancy (0.38), a history of PTSD (0.39) or previous counselling for pregnancy or birth-related factors (0.32). Risk factors during birth most strongly associated with PTSD were subjective birth experience (0.59), operative birth (0.48), lack of support from staff during birth (−0.38) and dissociation (0.32). The effect of subjective birth experience was mostly due to negative emotions during birth (0.34) but lack of control or agency was also important (−0.23). After birth, PTSD symptoms were associated with depression (0.60) and poor coping and stress (0.30). PTSD was not associated with time since birth, although this is only based on two studies so should be interpreted with caution. Vulnerability and risk factors with the strongest effect sizes are summarized in Fig. 2.
Effect size (r) for factors with largest associations with postpartum post-traumatic stress disorder (PTSD).

One study in the meta-analysis was carried out in Nigeria (Adewuya et al. Reference Adewuya, Ologun and Ibigbami2006) which has a different social demographic and increased risk of maternal and infant morbidity compared with other studies. To check that this Nigerian study was not unduly influencing results it was removed and analyses repeated. When this study was removed effect sizes became smaller for poor health/complications in pregnancy [k = 8, r = 0.23, 95% confidence interval (CI) 0.20–0.26] but larger for control or agency in birth (k = 4, r = −0.35, 95% CI −0.42 to −0.28) and education level (k = 5, r = −0.25, 95% CI −0.29 to −0.22).
Moderator analyses
Moderator analyses examined whether methodological variables had an impact on the relationships between risk factors and PTSD. Moderators examined were clinical status of the sample, quality of PTSD measure, and time between measuring risk factors and PTSD. Results showed that the amount of time between measuring risk factors and postpartum PTSD significantly moderated many effects (see online Supplementary File S2). This means that the strength of the relationship between PTSD and some risk factors changed significantly over time, irrespective of whether this relationship was originally significant. Medium or large moderation effects of time since birth (i.e. greater than 0.3) showed that more time since birth reduced the effects of subjective birth experience (−0.37); but increased the effect of a history of sexual trauma (0.30). Clinical status of the sample moderated a few effects. Studies with high-risk samples, such as women who had pre-eclampsia or emergency caesarean sections, were more likely to find associations between PTSD and marital status (0.43), poor health/complications in pregnancy (0.55) and negative emotions in birth (0.32). These latter two are perhaps unsurprising as these factors are likely to be more prevalent in high-risk samples.
Measures of PTSD that used full diagnostic criteria were more likely to find effects between postpartum PTSD and poor health or complications in pregnancy. Conversely, measures that only looked at PTSD symptoms were more likely to find effects between PTSD and marital status (−0.43), previous counselling for pregnancy or birth-related factors (−0.59), stress and coping (−0.38), postpartum emotional health (−0.48) and marital status (−0.43).
Publication bias
Meta-analysis relies on the published literature so any biases in the selection of studies for publication will be reflected in the studies included in the meta-analysis. Tests of publication bias (see online Supplementary File S3) suggested that some effect sizes might be affected by publication bias, such as those for educational level, ethnicity, history of sexual trauma, type of birth, infant-related complications and depression after childbirth. However, trim-and-fill methods did not result in substantial changes to most effect sizes with only a few analyses where there was funnel plot asymmetry and where trim and fill was indicated. This suggests that the majority of findings are quite robust. The result of analyses where trim and fill was indicated was that the small effects between PTSD and age and planned pregnancy became non-significant; and the association between PTSD and socio-economic status, length of labour, and poor postpartum emotional health became significant.
Discussion
This meta-analysis aimed to quantify the key vulnerability and risk factors for postpartum PTSD, co-morbidity and potential moderators of these relationships. Results confirm that pre-birth and birth factors are important, and that PTSD is associated with poor coping and stress after birth and is highly co-morbid with depression in pregnancy and after birth. These results extend our understanding of postpartum PTSD in a number of ways. First, many of the risk factors identified are consistent with the diathesis–stress model (Ayers, Reference Ayers2004) and have been used to update this model as shown in Fig. 3. The revised model now includes factors identified as having the strongest associations with postpartum PTSD, as well as incorporating a pathway to indicate that vulnerability factors may make an impact on whether women with initial PTSD symptoms resolve their symptoms or develop chronic PTSD. The finding that previous counselling for pregnancy or birth-related factors is a risk factor is probably because this identifies women with previous traumatic birth and/or severe fear of childbirth. This has therefore been subsumed in the model as part of the broader category of fear of childbirth. The results of the meta-analysis therefore help refine our understanding of the aetiology of postpartum PTSD.
Revised diathesis–stress model of the aetiology of birth-related post-traumatic stress disorder (PTSD).

Second, this meta-analysis identifies factors that could be used for screening, prevention and treatment of birth-related PTSD. Women can be assessed during and after pregnancy for their level of risk. During pregnancy, women could be assessed for depression, fear of childbirth, poor health or complications, and a history of PTSD. If women score high on these factors steps could be taken to reduce the likelihood of them developing PTSD following childbirth. During birth, women who have operative births or show signs of dissociation could be flagged for postpartum follow-up to assess for PTSD. After birth, women could be asked about their subjective birth experiences. The exact nature that these assessments take and which steps are most effective in preventing or minimizing PTSD symptoms require further research. However, the results of this meta-analysis provide a preliminary basis on which to base screening, prevention or treatment.
The role of support during birth is important as a potential protective factor because it can be relatively easily addressed in maternity care. Perceived support during birth was associated with reduced PTSD and previous research suggests that perceived support is even more important for women with a history of trauma or those who have more intervention during birth (Ford & Ayers, Reference Ford and Ayers2011). General perceived support during and after pregnancy was also associated with reduced PTSD. However, it is not clear from this meta-analysis whether this association reflects a protective function of support or negative impact of poor support contributing to PTSD. There is evidence to substantiate both views. For example, a study of women's worst hotspots during birth (defined as peak emotional distress) found that over a third of hotspots were due to interpersonal factors such as feeling abandoned, being ignored and lacking support (Harris & Ayers, Reference Harris and Ayers2012). Similarly, in the PTSD literature there is evidence that interpersonal traumas where a person is perceived as the perpetrator are more likely to result in PTSD (Charuvastra & Cloitre, Reference Charuvastra and Cloitre2008). Conversely, there is evidence from experimental studies using birth stories that positive support may be critical in improving women's perceived control and reducing perceived trauma (Ford & Ayers, Reference Ford and Ayers2009). It is therefore important to look at ways that we can increase support for women during birth – particularly for vulnerable women – whilst at the same time reducing the incidence of poor support.
The results of this review therefore extend our knowledge of birth-related PTSD. However, a number of conceptual and methodological issues need to be considered before drawing conclusions. Conceptually childbirth differs from other traumatic events in that it is experienced as positive by many women and viewed positively by society. Childbirth also involves huge physiological changes that may affect women's responses. Normal postpartum symptoms such as sleep deprivation or increased vigilance may confound measurement of PTSD (Ayers et al. Reference Ayers, Wright and Ford2015). The baby might also act as a reminder of the birth – therein affecting symptoms of avoidance. Results from this meta-analysis may therefore not be generalizable to PTSD following other events. Despite this, many of the risk factors identified are similar to those found in meta-analyses of postpartum PTSD with a range of traumatic stressors (Grekin & O'Hara, Reference Grekin and O'Hara2014) and PTSD in non-obstetric samples (Brewin et al. Reference Brewin, Andrews and Valentine2000; Ozer et al. Reference Ozer, Best, Lipsey and Weiss2003). Childbirth also offers an accessible way to prospectively study responses to stressful and potentially traumatic events, as evidenced by the predominance of longitudinal studies in this review.
Moderator analyses (shown in online Supplementary File S2) suggest that some associations are influenced by type of sample, measurement and time since birth. High-risk samples and those using diagnostic interviews were more likely to find an association between poor health or complications in pregnancy and PTSD. This is probably because a few studies, such as the Nigerian study by Adewuya et al. (Reference Adewuya, Ologun and Ibigbami2006), were on high-risk samples (that are more likely to experience complications in pregnancy) and used diagnostic interviews to measure PTSD. Indeed, removing the Nigerian study from the bivariate analyses showed that the effect of complications in pregnancy reduced and the effects of control in birth increased. This suggests that there may be differences in some risk factors between low- and middle-income countries and high-income countries. This is plausible given different rates of maternal morbidity and mortality in these countries.
Moderator analyses of time since birth suggest that the association between birth factors and PTSD reduces over time, whereas the associations with pre-birth vulnerability, such as sexual trauma, and postpartum factors may increase over time. This is consistent with theories of PTSD which distinguish between factors associated with the onset and maintenance of PTSD (Ehlers & Clark, Reference Ehlers and Clark2000). However, these theories typically emphasize cognitive and coping factors that maintain PTSD, and there is evidence to support that these are important in postpartum PTSD (Ford et al. Reference Ford, Ayers and Bradley2010; Vossbeck-Elsebusch et al. Reference Vossbeck-Elsebusch, Freisfeld and Ehring2014). However, these moderator analyses suggest that pre-existing vulnerability and other postpartum factors may also be important in the resolution of postpartum PTSD.
Methodological issues with this review include that some analyses were based on small numbers of studies so results should be interpreted with caution. This is particularly the case for time since birth and sociodemographic variables so further research is needed examining these. Similarly, studies included in the meta-analysis used diverse measures of similar constructs which were difficult to combine. Therefore some agreement over which measures are most appropriate and valid to use in this population would be useful. Finally, we can only analyse and comment on the variables included in research. It is likely that there are variables that warrant further exploration which are not analysed here because of insufficient evidence. For example, cognitive appraisals after birth (Ford et al. Reference Ford, Ayers and Bradley2010; Vossbeck-Elsebusch et al. Reference Vossbeck-Elsebusch, Freisfeld and Ehring2014), anxiety sensitivity (Keogh et al. Reference Keogh, Ayers and Francis2002; Verreault et al. Reference Verreault, Da Costa, Marchand, Ireland, Banack, Dritsa and Khalifé2012) and insomnia (Garthus-Niegel et al. Reference Garthus-Niegel, von Soest, Vollrath and Eberhard-Gran2013) all appear promising but there was not enough evidence to include them in the meta-analysis. Future research should therefore consider other variables, such as these, which are not included in this review. Finally, little research is available from low- and middle-income countries so these findings may only be generalizable to American, European and Australasian populations.
Despite these caveats, it can be seen that this meta-analysis has a number of implications for clinical practice and research. This review identifies a number of vulnerability and risk factors for postpartum PTSD that can be used to inform our understanding of the aetiology of birth-related PTSD, as well as assessment, prevention and intervention. Although PTSD following birth is unique in some ways, results are broadly comparable with meta-analyses of risk factors for PTSD following other events, which suggests that results might be generalizable. Postpartum PTSD offers a useful paradigm to study responses to stressful and potentially traumatic events prospectively. Support during birth may be a particularly promising area for preventing PTSD and the same might be the case for postpartum support and care but more research is needed.
Supplementary material
For supplementary material accompanying this paper visit http://dx.doi.org/10.1017/S0033291715002706
Acknowledgements
We are very grateful to Caroline Childerley, Celine Chhoa, Michelle McKenner, Alexandra Thornton and Sarah Woodhouse for their help in carrying out this review.
Declaration of Interest
None.






