Victimisation rates among patients with a severe mental illness (SMI) are higher than in the general population. Reference Chapple, Chant, Nolan, Cardy, Whiteford and McGrath1–Reference Chapple, Chant, Nolan, Cardy, Whiteford and McGrath11 Recently, a Dutch study showed a 1-year prevalence of violent crimes of 25% among patients with SMI compared with 3% in the general population. Reference Kamperman, Henrichs, Bogaerts, Lesaffre, Wierdsma and Ghauharali4 Prevalence rates of non-violent crimes affect 30% of the SMI population against 8% of the general population. Reference Teplin, McClelland, Abram and Weiner10 Falling victim to a crime can be a highly stressful event. Studies have shown that the impact of stressful life events in patients with an SMI can be even more severe and may induce psychosis, relapse or post-traumatic stress disorder, or impair treatment outcomes. Reference Teplin, McClelland, Abram and Weiner10,Reference Maniglio12 People with SMI are more susceptible to victimisation because of the presence of certain risk factors. Reference Maniglio12,Reference Kelly and McKenna13 Several risk factors have been identified, but younger age, Reference Honkonen, Henriksson, Koivisto, Stengard and Salokangas3 unemployment, Reference Chapple, Chant, Nolan, Cardy, Whiteford and McGrath1,Reference Honkonen, Henriksson, Koivisto, Stengard and Salokangas3,Reference Schomerus, Heider, Angermeyer, Bebbington, Azorin and Brugha7 substance use/misuse and symptom severity are most consistently associated with victimisation. Reference Chapple, Chant, Nolan, Cardy, Whiteford and McGrath1,Reference Silver, Arseneault, Langley, Caspi and Moffitt8,Reference Fortugno, Katsakou, Bremner, Kiejna, Kjellin and Nawka14,Reference Walsh, Moran, Scott, McKenzie, Burns and Creed15 Past arrests, drugs and alcohol misuse are predictors of violent victimisation. Predictors of non-violent victimisation are better education, and more positive and negative symptoms, and also a history of arrests. Reference Schomerus, Heider, Angermeyer, Bebbington, Azorin and Brugha7
Predictors of violent victimisation in the general population are a younger age, gender (men are more at risk for physical assault and women are more vulnerable for sexual crimes), low socioeconomic status, past psychiatric status, previous victimisation, criminal activity and drug use. Reference Acierno, Resnick and Kilpatrick16,Reference Anderson17 Noteworthy, most victimisation in the general population is committed by someone close to the victim. Reference Wood and Edwards11 Most studies argue that patients who live in the community are more likely to be victims of violent and non-violent crimes, Reference Dean, Moran, Fahy, Tyrer, Leese and Creed2,Reference Honkonen, Henriksson, Koivisto, Stengard and Salokangas3,Reference Schomerus, Heider, Angermeyer, Bebbington, Azorin and Brugha7,Reference Maniglio12,Reference Walsh, Moran, Scott, McKenzie, Burns and Creed15 and this may be reflected in the increase in victimisation rates since the deinstitutionalisation of patients with SMI. Reference Kelly and McKenna13,Reference Short, Thomas, Luebbers, Mullen and Ogloff18 However, to our knowledge, no study has ever compared victimisation rates between types of care. Furthermore, we found little information about the perpetrators and how they relate to the victim. The aim of this study was to examine the 1-year prevalence of violent and non-violent victimisation among patients with SMI receiving treatment at mental healthcare institutions in Amsterdam (The Netherlands).
Victimisation rates of out-patients, patients in sheltered housing facilities and in-patients are compared with average victimisation rates in a weighed sample of the general population of Amsterdam and five surrounding towns. We examined the relationships between the perpetrator and the victims, and finally we looked at associations between victimisation and the clinical setting, sociodemographic risk factors, clinical characteristics and indices of substance use/misuse. Given the literature, we expected to find the highest rates of victimisation for out-patients with SMI. Younger unemployed patients with more severe psychopathology and comorbid substance use/misuse were expected to report more victimisation. This is the first study to examine the link between victimisation rates and types of care.
Method
Design
In this study, we studied victimisation experiences by comparing data from a longitudinal study and data from a cross-sectional study (comparison group). The same measure for victimisation (violent crimes, property crimes and vandalism), the primary outcome of interest, was used in both data-sets. The longitudinal study (2005–2011) looked at a survey sample of patients with SMI treated by the mental healthcare institutions Arkin and GGZ InGeest in Amsterdam (The Netherlands). Together, these mental healthcare institutions are involved in treating most patients with SMI residing in Amsterdam. The objective of this longitudinal study was to obtain information about quality of life, disease characteristics, general functioning, care needs, social network and inclusion in society, and victimisation. Reference Dekker, Theunissen, Van, Peen, Duurkoop and Kikkert19 This article is based on victimisation data obtained in 2011. The study was approved by the Dutch Association of Medical-Ethical Appraisal Committees (NVMETC) for mental health organisations. Details about the cross-sectional study are described in more detail in the ‘Comparison group’ section.
Population, inclusion and exclusion criteria
In The Netherlands, treatment for patients with SMI can be divided roughly into three levels of treatment intensity: (a) in-patient care facilities (long-stay psychiatric hospitals); (b) residential care in sheltered housing; and (c) flexible assertive community treatment for out-patients. In-patient care consists of a residential facility with permanent/semi-permanent care, where patients are closely monitored and receive assistance with their daily needs. Residential care in sheltered housing also consists of a residential care facility but with less psychiatric care and less monitoring of daily activities. Many of these facilities are group homes with shared living rooms and sanitation. Flexible assertive community treatment (FACT) is an integrated approach comprising psychological and psychiatric treatment, and supported employment for out-patients.
The target population consisted of patients aged 27–76 years with an SMI defined as a DSM-IV diagnosis 20 of schizophrenia (DSM code 295.xx), a psychotic disorder (DSM code 291.xx–293.xx, 295.xx, 297.xx, 298.xx), substance use disorder (DSM codes 303.xx–305.xx) or a severe mood or anxiety disorder (DSM codes 296.xx, 309.xx) and a history of continuous intensive mental healthcare during the previous 2 years. This group also included patients with a dual diagnosis. Dual diagnosis was defined as all Axis I disorders in conjunction with substance use disorders. 21 Further selection criteria for the target population were: adequate mastery of Dutch or English and residence in the Amsterdam district for at least 1 year. Exclusion criteria included being too ill to participate in the study, limited levels of understanding or impaired communication abilities.
Enrolment
For this study, 876 patients were randomly selected from outpatient treatment teams, sheltered housing facilities and in-patient care facilities. Of this sample, 553 (63%) did not participate in the study. Some patients refused to participate (26%), others did not participate for other, unspecified reasons (25%). Some patients had moved to other treatment facilities (9%), and in some cases the clinician considered participation too stressful (3%). In total, 323 (37%) patients were included in the study. In consultation with the psychiatrist, psychologist or psychiatric nurse, all patients were invited to a follow-up assessment 6 years later in 2011. Once patients had given written informed consent, the assessment was performed in a face-to-face interview. The interviews were conducted at the healthcare centre or, if preferred by the patient, at the patient's home. The interview took 1.5 h and patients received €15 for the interview. The interviews were conducted by one trained psychologist and a senior researcher.
Comparison group
We compared victimisation data of patients with SMI with victimisation data of the general population of Amsterdam and five surrounding towns obtained in the same year. The comparison group consisted of 10 865 representative participants, recruited by OIS, Research Information and Statistics, city of Amsterdam in 2011. Questionnaires were distributed via the internet or as paper copies, depending on participant preference. People were telephoned who did not complete the internet survey or they were visited at home, to finish the interview.
Measures
Victimisation was measured in both patients and the general population with the Dutch version of Integral Safety/Security Monitor (in Dutch: Integrale Veiligheidsmonitor, IVM section 4) 22 developed by the Dutch Ministry of the Interior and the Department of Justice. The IVM is the instrument used nationally by Statistics Netherlands (CBS) to measure victimisation on a large scale (almost 80 000 cases a year) and make geographical comparisons. It is a self-report instrument designed to measure factors such as neighbourhood livability, feelings of security and actual victimisation involving violent crimes, property crimes and vandalism in the past 12 months. Self-report questionnaires of victimisation tend to be more reliable than police reports because the latter tend to underreport victimisation. Reference Hiday, Swartz, Swanson, Borum and Wagner23 The IVM is an adequate instrument that provides consistent information. 22 All interviewers were extensively trained and received regular training updates. Victimisation was assessed on the basis of 14 different crimes allocated to three subscales: violent crimes (sexual crimes, threats and assaults), property crimes (burglary, theft of a bike, theft of a car, pickpocketing, or theft of other property) and vandalism (vandalism in general and vandalisation of a car). The three subscales were scored using a dichotomous yes/no format. Participants were asked whether they had ever experienced victimisation involving each specific crime. Even though these questions were asked to the patients, these data were not used for analysis. An example of a question about violent crime is: ‘Has anyone ever attacked you in the past 5 years, or mistreated you, by beating or kicking you, or by using a gun, a knife, a stick, scissors or another similar object?’
To reduce recall bias, participants were asked whether and how often they had been victimised in the previous 12 months and to state the month when the victimisation occurred. In the case of personal crimes, additional questions were asked about the perpetrator and the location of the most recent incident. In the original IVM, options for perpetrators are: partner, neighbour, former partner, colleagues, family members or other acquaintances. For the SMI group we added the category ‘housemate’, since some of our SMI group share accommodation in a care facility, and the category ‘friend’ based on the International Crime Victims Survey (ICVS). Reference van Dijk, Mayhew, van Kesteren, Aebi and Linde24
Psychopathology was measured with the Brief Psychiatric Rating Scale – Expanded (BPRS-E). Reference Ruggeri, Koeter, Schene, Bonetto, Vàzquez-Barquero and Becker25 The BPRS-E was originally designed by Overall and Gorham in 1962 to measure changes in psychopathology severity. Reference Andersen, Larsen, Schultz, Nielsen, Korner and Behnke26 It consists of 24 symptoms assessed on a scale from 1 to 7. Items are grouped into four subscales: positive symptoms, negative symptoms, depression and disorganisation. Reference Ruggeri, Koeter, Schene, Bonetto, Vàzquez-Barquero and Becker25 Items are scored on the basis of observations during the interview and patient self-reports. The BPRS-E tends to be a sensitive instrument and a good interrater reliability (r = 0.74, P<0.001) can be achieved with training and a standard interview procedure. Reference Andersen, Larsen, Schultz, Nielsen, Korner and Behnke26,Reference Overall and Rhoades27 Moreover, research has shown that the validity of the BPRS-E is higher than other measures of psychopathology. Reference Kopelowicz, Ventura, Liberman and Mintz28
Use of alcohol and drugs, substance dependence and misuse was assessed with the Measurements in the Addictions for Triage and Evaluation (MATE). Reference Schippers, Broekman, Buchholz, Koeter and Van Den Brink29 MATE assesses the use of psychoactive substances, history and current substance misuse and dependence on the basis of DSM-IV. Reference Schippers, Broekman and Buchholz30 It is a valid and reliable instrument for assessing individuals with addictions. The interrater reliability ranged between 0.75 and 0.92, and the interviewer reliability ranged between 0.34 and 0.73. Reference Schippers, Broekman, Buchholz, Koeter and Van Den Brink29 Patients' files were also consulted to identify patients with a DSM-IV diagnosis of substance misuse and dependence. Patients were registered with a dual diagnosis when MATE indicated both substance misuse and dependence or when a patient's files already contained such information.
Data analysis
Analyses were conducted using SPSS Statistics 17.0. Chi-squared analyses were used for categorical variables and ANOVA analyses were used to analyse continuous variables. We used the Kruskal–Wallis test when ANOVA assumptions were violated. Standardised residuals in chi-squared analyses were used to reject or to accept the null hypothesis. The null hypothesis was that there was no difference between the groups. A residual of more or less than +/−1.96 indicates that the number of cases in that cell is significantly larger than would be expected if the null hypothesis were true, with a significance level of 0.05. When standardised residuals did not exceed the positive or negative critical value, significances were rejected. For the comparison of our data and the data for the population of the Amsterdam district, we introduced weightings for gender, age, ethnicity and postal code. Risk ratios were calculated for every type of victimisation. The categorisation of type of care facility was based on the location for the interview. However, the IVM measures the prevalence of victimisation in the preceding year and so it is possible that individual patients may have been allocated to a different type of care facility in line with the situation when the actual victimisation event occurred. We therefore controlled for type of care facility when the victimisation event occurred and the type of facility at the time of the interview. The vandalism subscale was excluded from secondary analysis. This subscale is based on vandalism of (a) a car and (b) other objects such as a bicycle or a house. Since car ownership is relatively rare among our patients, vandalism rates were too low to justify further analysis.
Univariate logistic regression analyses were used to identify the association between sociodemographics, clinical variables, substance use/misuse and all crimes and violent crimes. Subsequently, two multivariate logistic regression analyses (BACKSTEP method) were used to examine predictors of violent and property crimes. This analysis was considered suitable since the outcome variable was categorical and predictor variables are both continuous and categorical. In these analyses, block one was defined as sociodemographics and clinical characteristics, block two as symptoms (BPRS-E) and block three as drugs misuse variables.
Results
Demographic information
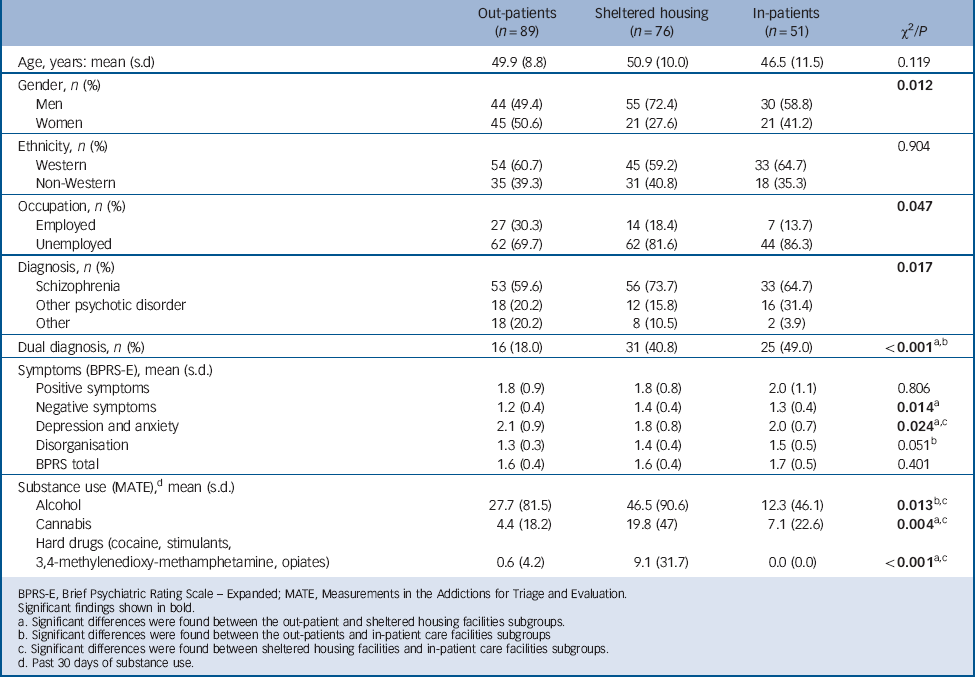
The 2005 baseline assessment included 323 patients in the SMI group. In 2011 we were able to follow up 216 patients from the original sample (66.9% follow-up rate). A total of 8 patients could not be traced, 29 died before the interview, 47 refused to be interviewed, 11 were unable to do the interview, 6 did not give consent, 1 had his patient file removed and 4 left the country. The data for one patient were incomplete. The patients had been receiving treatment for at least 7 years in 2011. Table 1 provides information about sociodemographics, care facilities, clinical characteristics and substance use/misuse by care facility.
Sociodemographics, care facilities, clinical characteristics and substance use (n = 216)
| Out-patients (n = 89) |
Sheltered
housing (n = 76) |
In-patients (n = 51) |
χ2/P | |
|---|---|---|---|---|
| Age, years: mean (s.d) | 49.9 (8.8) | 50.9 (10.0) | 46.5 (11.5) | 0.119 |
| Gender, n (%) | 0.012 | |||
| Men | 44 (49.4) | 55 (72.4) | 30 (58.8) | |
| Women | 45 (50.6) | 21 (27.6) | 21 (41.2) | |
| Ethnicity, n (%) | 0.904 | |||
| Western | 54 (60.7) | 45 (59.2) | 33 (64.7) | |
| Non-Western | 35 (39.3) | 31 (40.8) | 18 (35.3) | |
| Occupation, n (%) | 0.047 | |||
| Employed | 27 (30.3) | 14 (18.4) | 7 (13.7) | |
| Unemployed | 62 (69.7) | 62 (81.6) | 44 (86.3) | |
| Diagnosis, n (%) | 0.017 | |||
| Schizophrenia | 53 (59.6) | 56 (73.7) | 33 (64.7) | |
| Other psychotic disorder | 18 (20.2) | 12 (15.8) | 16 (31.4) | |
| Other | 18 (20.2) | 8 (10.5) | 2 (3.9) | |
| Dual diagnosis, n (%) | 16 (18.0) | 31 (40.8) | 25 (49.0) | <0.001 a,b |
| Symptoms (BPRS-E), mean (s.d.) | ||||
| Positive symptoms | 1.8 (0.9) | 1.8 (0.8) | 2.0 (1.1) | 0.806 |
| Negative symptoms | 1.2 (0.4) | 1.4 (0.4) | 1.3 (0.4) | 0.014 a |
| Depression and anxiety | 2.1 (0.9) | 1.8 (0.8) | 2.0 (0.7) | 0.024 a,c |
| Disorganisation | 1.3 (0.3) | 1.4 (0.4) | 1.5 (0.5) | 0.051 b |
| BPRS total | 1.6 (0.4) | 1.6 (0.4) | 1.7 (0.5) | 0.401 |
| Substance use (MATE), d mean (s.d.) | ||||
| Alcohol | 27.7 (81.5) | 46.5 (90.6) | 12.3 (46.1) | 0.013 b,c |
| Cannabis | 4.4 (18.2) | 19.8 (47) | 7.1 (22.6) | 0.004 a,c |
| Hard drugs (cocaine, stimulants, 3,4-methylenedioxy-methamphetamine, opiates) | 0.6 (4.2) | 9.1 (31.7) | 0.0 (0.0) | <0.001 a,c |
BPRS-E, Brief Psychiatric Rating Scale – Expanded; MATE, Measurements in the Addictions for Triage and Evaluation. Significant findings shown in bold.
a. Significant differences were found between the out-patient and sheltered housing facilities subgroups.
b. Significant differences were found between the out-patients and in-patient care facilities subgroups
c. Significant differences were found between sheltered housing facilities and in-patient care facilities subgroups.
d. Past 30 days of substance use.
As expected, there were some differences (P<0.05) between patients treated in the different care facilities in terms of sociodemographics, diagnosis, symptom severity and substance use. Chi-squared analyses showed differences for gender, employment and diagnosis by type of care facility. However, standardised residual values showed no significant discrepancies between subgroups. Out-patients were less likely to have a dual diagnosis than patients living in a sheltered housing facility or in-patients. Out-patients also reported fewer disorganisation symptoms than in-patients. Patients living in sheltered housing facilities reported more negative symptoms and drug use than out-patients, but fewer symptoms of depression and anxiety than out-patients and in-patients. Overall, in-patients use fewer substances than out-patients and patients living in a sheltered housing facility.
Victimisation of psychiatric patients by comparison with the general population
Table 2 lists the prevalence for victimisation in the preceding year broken down by type of care. In-patients reported higher rates of property crimes and a higher total sum score for all crimes than patients living in sheltered housing facilities. In-patients were also more likely to fall victim to property crimes than out-patients. Standardised residual values showed no discrepancies between the groups studied in terms of the correlation between type of care and the prevalence of violent victimisation (sexual crimes, threats, assaults). Vandalism tended to be spread evenly across all types of care facility (P = 0.204).
Comparison of prevalence of type of victimisation in patients with severe mental illness ((n = 216) and the population of the Amsterdam district a

| Out-patients (n = 89) |
Patients
in sheltered housing facilities (n = 76) |
In-patients (n = 51) |
Overall patients, % |
Population Amsterdam district (weighted), % |
Risk ratio |
|||||
|---|---|---|---|---|---|---|---|---|---|---|
| Type of victimisation | n | % | n | % | n | % | χ2 | |||
| All crimes | 37 | 41.6 | 21 | 27.6 | 29 | 56.9 | 0.004 b | 40.3 | 42.3 | 0.95 |
| Violent crimes | 20 | 22.5 | 12 | 15.8 | 18 | 35.3 | 0.037 | 22.7 | 8.5 | 2.7 |
| Sexual offences | 4 | 4.5 | 1 | 1.3 | 7 | 13.7 | 0.010 c | 5.6 | 1.4 | 4 |
| Threats | 14 | 15.7 | 9 | 11.8 | 7 | 13.7 | 0.771 | 13.9 | 6.6 | 2.1 |
| Assaults | 5 | 5.6 | 5 | 6.6 | 9 | 17.6 | 0.038 d | 8.8 | 1.9 | 4.6 |
| Property crimes | 14 | 15.7 | 10 | 13.2 | 24 | 47.1 | 0.000 b,d | 22.2 | 26.2 | 0.85 |
| Attempted burglary | 2 | 2.2 | 2 | 2.6 | 3 | 5.9 | 0.471 | 3.2 | 4.2 | 0.76 |
| Burglary | 0 | 0 | 3 | 3.9 | 10 | 19.6 | 0.000 c | 6.0 | 2.6 | 2.3 |
| Bicycle theft | 9 | 10.1 | 2 | 2.6 | 4 | 7.8 | 0.163 | 6.9 | 11.4 | 1.7 |
| Car theft and theft from car | 2 | 2.2 | 0 | 0 | 0 | 0 | 0.237 | 0 | 6.8 | 6.8 |
| Pickpocketing | 2 | 2.2 | 3 | 3.9 | 13 | 25.5 | 0.000 c | 8.3 | 4.0 | 2.1 |
| Robbery | 0 | 0 | 3 | 3.9 | 2 | 3.9 | 0.166 | 2.3 | 0.9 | 2.6 |
| Other theft | 2 | 2.2 | 4 | 5.3 | 5 | 9.8 | 0.147 | 5.1 | 5.6 | 0.91 |
| Vandalism | 10 | 11.2 | 7 | 9.2 | 10 | 19.6 | 0.204 | 12.5 | 23.1 | 1.8 |
a. Significant findings shown in bold.
b. Significant differences were found between the sheltered housing facilities and in-patient care facilities subgroups.
c. Expected cell count too low (<5) for accurate chi-square.
d. Significant differences were found between out-patients and in-patient care facilities.
When we compared the victimisation rates for the general population in the Amsterdam district with the SMI group, we found several notable results (Table 2). First, levels of total victimisation were similar in both groups. Second, the SMI group were 2.7 times more likely to be victims of violent crime. At the item level, we also found higher rates of violent victimisation. Sexual victimisation was four times as prevalent in the SMI group than in the general population; assaults were 4.6 times more likely and threats 2.1 times more likely. Third, these findings contrasted with the findings for the property crimes and vandalism subscales. The general population reported higher rates of non-violent crimes than the SMI group (the total rate of property crimes was 0.85 times higher; bicycle theft was 1.7 times higher, theft of/or from a car 6.8 times and vandalism 1.8 times higher). On the other hand, the SMI group reported a rate for theft from their homes that was 2.3 times higher, the rate for pickpocketing was 2.1 times higher, and the rate for robbery was 2.6 times higher than reported by the general population. There are also individuals who were victims of both violent and non-violent crimes (25.5% of the SMI group and 38.2% of the general population). In conclusion, the SMI group are more often victim of violent crimes, burglary, pickpocketing and robbery than the general population. Analyses showed that 83.7% of violent crimes and 81.3% of property crimes were at the same location as the interviews.
A frequency analysis shows that perpetrators of sexual offences in the SMI group were mostly housemates (41.7%), colleagues (8.3%), friends and former friends (8.3%), and other acquaintances (8.3%). Threats mostly came from housemates (36.7%), neighbours (26.7%) and other acquaintances (13.3%). Most assaults were perpetrated by housemates (21.1%), neighbours (15.8%), former partners (10.5%) or other acquaintances (10.5%). Perpetrators of sexual offences in the general population were mostly other acquaintances (13.9%) and neighbours (8.8%). Threats came most frequently from neighbours (19.5%) and other acquaintances (10.5%). Other acquaintances (15.7%) and neighbours (12%) were most often responsible for assaults in the general population. (Percentages of less than 8.3% are not detailed.) We then examined risk factors for violent and property crimes.
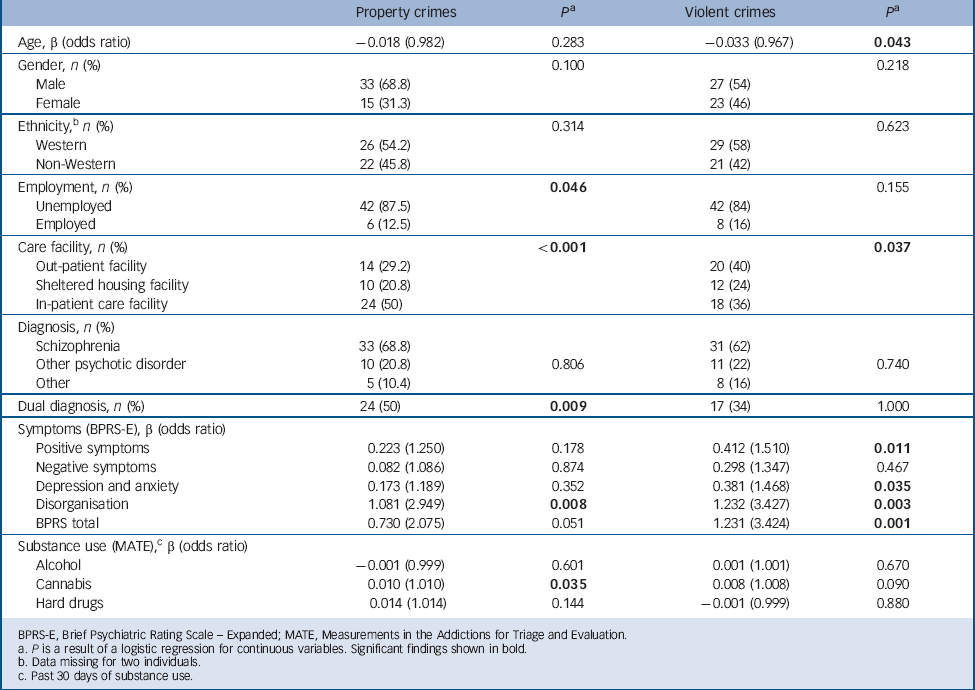
Table 3 lists the results of the univariate analysis for associations between violent and property crimes. Property crimes were associated more with being an in-patient, having a dual diagnosis, more severe symptoms of disorganisation and more severe cannabis use. A trend was found for the association between the BPRS-E total score and victimisation involving property crime. Standardised residual values showed no differences between the groups in terms of unemployment, employment and prevalence of property crimes. We found that younger people were more at risk of falling victim to violent crime. Gender was not related to victimisation risk. In an additional analysis we examined gender differences for each of the three violent crimes and found again no differences between men and woman. We also found that patients with more severe psychopathology, particularly positive symptoms, and symptoms of depression, anxiety and disorganisation were more often victims of violent crime. Finally, a trend was found for the association between cannabis use and victimisation involving violent crime. Standardised residual values showed no differences between the different groups in terms of the correlation between type of care and prevalence of violent victimisation.
Associations between sociodemographics, clinical characteristics and drugs with property and violent crimes (n = 216)
| Property crimes | P a | Violent crimes | P a | |
|---|---|---|---|---|
| Age, β (odds ratio) | −0.018 (0.982) | 0.283 | −0.033 (0.967) | 0.043 |
| Gender, n (%) | 0.100 | 0.218 | ||
| Male | 33 (68.8) | 27 (54) | ||
| Female | 15 (31.3) | 23 (46) | ||
| Ethnicity, b n (%) | 0.314 | 0.623 | ||
| Western | 26 (54.2) | 29 (58) | ||
| Non-Western | 22 (45.8) | 21 (42) | ||
| Employment, n (%) | 0.046 | 0.155 | ||
| Unemployed | 42 (87.5) | 42 (84) | ||
| Employed | 6 (12.5) | 8 (16) | ||
| Care facility, n (%) | < 0.001 | 0.037 | ||
| Out-patient facility | 14 (29.2) | 20 (40) | ||
| Sheltered housing facility | 10 (20.8) | 12 (24) | ||
| In-patient care facility | 24 (50) | 18 (36) | ||
| Diagnosis, n (%) | ||||
| Schizophrenia | 33 (68.8) | 31 (62) | ||
| Other psychotic disorder | 10 (20.8) | 0.806 | 11 (22) | 0.740 |
| Other | 5 (10.4) | 8 (16) | ||
| Dual diagnosis, n (%) | 24 (50) | 0.009 | 17 (34) | 1.000 |
| Symptoms (BPRS-E), β (odds ratio) | ||||
| Positive symptoms | 0.223 (1.250) | 0.178 | 0.412 (1.510) | 0.011 |
| Negative symptoms | 0.082 (1.086) | 0.874 | 0.298 (1.347) | 0.467 |
| Depression and anxiety | 0.173 (1.189) | 0.352 | 0.381 (1.468) | 0.035 |
| Disorganisation | 1.081 (2.949) | 0.008 | 1.232 (3.427) | 0.003 |
| BPRS total | 0.730 (2.075) | 0.051 | 1.231 (3.424) | 0.001 |
| Substance use (MATE), c β (odds ratio) | ||||
| Alcohol | −0.001 (0.999) | 0.601 | 0.001 (1.001) | 0.670 |
| Cannabis | 0.010 (1.010) | 0.035 | 0.008 (1.008) | 0.090 |
| Hard drugs | 0.014 (1.014) | 0.144 | −0.001 (0.999) | 0.880 |
BPRS-E, Brief Psychiatric Rating Scale - Expanded; MATE, Measurements in the Addictions for Triage and Evaluation.
a. P is a result of a logistic regression for continuous variables. Significant findings shown in bold.
b. Data missing for two individuals.
c. Past 30 days of substance use.
To further our understanding of prediction models for victimisation involving violent and property crimes, we performed a multivariable regression (BACKSTEP method). Table 4 shows the results of the regression analysis. The following variables for the victimisation model involving property crimes (model 1) were removed during the statistical analyses because they did not contribute to the fit: age, gender, ethnicity, employment, dual diagnosis, positive–negative symptoms and symptoms of depression and anxiety, the BPRS-E total score, alcohol and hard drugs misuse. The following variables for the victimisation model involving violent crimes (model 2) were removed during the statistical analyses for the same reason: gender, ethnicity, employment, care facility, diagnosis, dual diagnosis, positive–negative symptoms and symptoms of depression and anxiety, the BPRS-E total score and substance use/misuse. The strength of the models increased after eliminating these variables.
Results of multivariate logistic regression analyses (BACKSTEP method) for predictors of victimisation involving violent (model 1) and property (model 2) crimes (n = 216)

| B (s.e.) | P | Exp B (95% CI) | |
|---|---|---|---|
| Model 1: property crimes a | |||
| In-patients | 2.041 (0.508) | <0.001 | 7.695 (2.842–20.840) |
| Disorganisation | 0.824 (0.460) | 0.073 | 2.279 (0.925–5.614) |
| Cannabis | 0.013 (0.005) | 0.019 | 1.013 (1.002–1.024) |
| Constant | −3.512 (0.785) | <0.001 | 0.030 |
| Model 2: violent crimes b | |||
| Age | −0.049 (0.018) | 0.007 | 0.952 (0.919–0.987) |
| Disorganisation | 1.370 (0.424) | 0.001 | 3.936 (1.716–9.028) |
| Constant | −0.819 (0.963) | 0.395 | 0.441 |
a. Omnibus test, Step P = 0.063, Model P = <0.001; Hosmer-Lemeshow, P=0.856; Nagelkerke: R 2 = 0.215.
b. Omnibus test, Step P=0.434, Model P = <0.001; Hosmer-Lemeshow, P=0.154; Nagelkerke: R 2 = 0.127.
Goodness-of-fit for model 1 (P = 0.847) and model 2 (P = 0.154) indicates a proper fit of the models to the data. Risk factors for victimisation involving property crimes (model 1, P<0.001; χ2 = 1.510, d.f. = 4, R 2 = 0.215) included: in-patient care facilities, dual diagnosis, disorganisation and cannabis use. In-patients with a dual diagnosis, more severe cannabis use and more severe symptoms of disorganisation tend to report falling victim to property crimes. Risk factors for violent victimisation (model 2, P<0.001; χ2 = 11.927, d.f. = 8, R 2 = 0.127) included age and disorganisation. Younger patients with SMI with more severe symptoms of disorganisation tended to report falling victim to violent crime.
Discussion
Although the overall victimisation rate for our SMI group was similar to that for the general population, the SMI group were more likely to be victims of violent crime (22.7% as opposed to 8.5% in the general population). The SMI group were almost five times more likely to be a victim of assault than the general population, and four times more likely to be a victim of a sexual crime. In comparison, other studies report a wide range of victimisation prevalence rates. Reported prevalence rates in people with SMI for non-violent crimes range from 7.7% to 28%, and for violent crimes from 4.3% to 35%. Reference Maniglio12 If we focus, however, on studies with a similar design and population as this study, we find two with similar results. A Dutch study found a risk ratio of 4.6 for physical assaults and a risk ratio of 3.9 for sexual harassment or assault in out-patients with SMI compared with the general population. Reference Kamperman, Henrichs, Bogaerts, Lesaffre, Wierdsma and Ghauharali4 In a study among patients with SMI in the USA, 25.3% of the SMI group were the victim of a violent crime compared with 2.8% in the general population. Reference Teplin, McClelland, Abram and Weiner10
Contrary to our hypothesis we found that in-patients experienced the highest rates for all types of crimes (56.9%). This study worryingly highlighted that 35% of in-patients were victims of a violent crime, and 47.1% were victims of a property crime. These prevalence rates for violent and non-violent crimes affecting in-patients with SMI are higher than rates found in international studies with in-patients. Reference Sturup, Sorman, Lindqvist and Kristiansson9 Younger patients and patients with more symptoms of disorganisation also fell victim to violent crime more often. This is in accordance with other studies where age Reference Honkonen, Henriksson, Koivisto, Stengard and Salokangas3,Reference Latalova, Kamaradova and Prasko6,Reference Teplin, McClelland, Abram and Weiner10 and symptoms of disorganisation Reference Chapple, Chant, Nolan, Cardy, Whiteford and McGrath1 were identified as risk factors. Finally, the rates for victimisation involving property crime were highest in patients with more severe cannabis use and patients with symptoms of disorganisation. Of note, the SMI group were assaulted most often by someone they knew. This study was the first to compare the relationship between the risk of victimisation and the treatment facility.
Since psychopathology is associated with victimisation rates, it seemed fair to assume that elevated levels of victimisation affecting in-patients can be attributed to higher levels of psychopathology in this subgroup. However, we found no differences in psychopathology between in-patients and other patients measured with the BPRS-E. This means that the higher risk of victimisation in psychiatric hospitals is not linked to differences in psychopathology.
We realise that this is an observational study. There are myriad potential reasons explaining the susceptibility of in-patients to victimisation. One possible reason is that in-patients live close together, resulting in less privacy and more irritation towards each other, and this may result in conflicts and victimisation. Positive symptoms of psychosis and a lack of internal control also exacerbate the risk of the onset of violence. Reference Choe, Teplin and Abram31 However, a consideration of all the possible factors that may result in victimisation is beyond the scope of this study, even though the prevalence's found in this study are cause for concern.
It is notable that younger patients with SMI are more likely to fall victim to violent crime. This can be explained by the fact that younger people are more active in their daily lives than older people and therefore more exposed to dangerous situations. Reference Pettitt, Greenhead, Khalifeh, Drennan, Hart and Hogg32 Another possible explanation could be that younger patients may have fewer skills to cope with, or to avoid involvement in, a criminal event than older people, who have more life experience with victimisation.
Disorganisation as a risk factor for violent and property crime can also affect individuals' ability to assess risks and take steps to protect themselves. Disorganisation consists of several categories: disorganised thinking, disorganised behaviour and inappropriate affect. 33 Disorganised thinking is the inability to stay on track in conversations, jumping from one unrelated idea to another. A common example of disorganised behaviour is engaging in confrontations with others for no logical reason, and not acting appropriately in public. Difficulties with emotional expression can manifest themselves in absent or inappropriate emotional expression such as flat affect, inappropriate eye contact or acting boisterously during a serious event. 33 These disorganisational problems can affect an individual's ability to resolve conflicts or disputes with others adequately, or lead them to evoke aggressive or criminal behaviour in others.
The fact that cannabis use is a risk factor could be related to the perceptual alterations caused by cannabis use (including time distortion, and impaired short-term memory and attention). Long-term use may produce more subtle impairment in higher cognitive functions such as memory, attention and self-regulation, and the integration of complex information, which may impair motivational behaviour and social performance, Reference Gelder, López-Ibor and Anderasen34 rendering cannabis users susceptible to victimisation. Another explanation of the relationship between victimisation involving property crime and cannabis use can be found in the general association between drugs and high-risk social environments. However, since the use of cannabis is tolerated in The Netherlands by the authorities, this factor plays a much less significant role here and can be disregarded.
By contrast with several previous studies, we did not identify gender as a risk factor for sexual victimisation. In the general population, women are more likely to fall victim to sexual crimes, whereas men are more susceptible to overall and physical violence. Reference Khalifeh and Dean5 Although it is difficult to interpret our results, Khalifeh & Dean argue that the gender pattern for patients with SMI is conspicuously different. Reference Khalifeh and Dean5 They hypothesise that risk domains such as likely offenders, suitable targets and the absence of capable guardians are more common in men than women in the general population but equally represented in patients with SMI. Furthermore, people with SMI may have less distinct gender patterns because of the loss of certain social roles and the impact of illness on patterns of behaviour. Reference Khalifeh and Dean5
We found low rates of violent victimisation by family members/ex-partners, which is in contrast to findings of a systematic review by Oram et al who found higher rates. Reference Oram, Trevillion, Feder and Howard35 The low rates in our study can be explained by the fact that most patients with SMI in our sample have no partner and few family contacts. Most studies mentioned by Oram et al Reference Oram, Trevillion, Feder and Howard35 looked at patients with an intimate relationship, which makes it difficult to compare with our data.
Limitations
The current study has certain limitations. First and foremost, there was only a single measurement of victimisation and it should be pointed out that the current study is based on cross-sectional data. We are therefore not in a position to examine the causality of interrelations and we cannot state whether victimisation causes drug misuse, admission to hospital or the exacerbation of clinical symptoms, or vice versa. We also looked at only a limited number of potential determinants; we assume that other predictors of victimisation may exist which have not been included in this study, examples being previous victimisation, Reference Teplin, McClelland, Abram and Weiner10 conflictual relationships, Reference Choe, Teplin and Abram31 a post-traumatic stress disorder Reference Teplin, McClelland, Abram and Weiner10 and maladaptive coping strategies. Reference Hill36 Previous victimisation seems to affect behaviour in later crime-related events: patients are less motivated to report the criminal event to the police, Reference Buzawa, Hotaling and Byrne37 they are more likely to experience repeat victimisation Reference Teplin, McClelland, Abram and Weiner10 and they risk developing maladaptive coping strategies, Reference Hill36 which tend to worsen their feelings of well-being. Reference Dempsey38 Maladaptive coping strategies in victimised people include avoiding reminders of the incident and behavioural avoidance such as the use of drugs/alcohol, denial and self-deception, dissociation, obsession with the crime and self-harm. Reference Hill36 Furthermore, we did not examine the prevalence of emotional abuse. A large international epidemiological study suggests that emotional abuse is strongly associated with poor health outcomes. Reference Garcia-Moreno, Jansen, Ellsberg, Heise and Watts39 Second, mental impairment causing poor reality testing, judgement, social skills, planning and problem-solving often seen in people with SMI may affect their ability to calculate risks and take steps to protect themselves. Reference Teplin, McClelland, Abram and Weiner10
Third, the comparison of the victimisation involving property crimes affecting the SMI group and the general population is probably affected by the fact that only a few people in the SMI group own a car (5.6% of the SMI group as opposed to 74.5% in the general population; bicycle possession: 47.4% in the SMI group and 89.9% in the general population). Bicycle theft and car-related theft was found in 6.9% and 0% of the SMI group respectively, as opposed to 11.4% and 6.8% in the general population. The risk of bicycle theft or car-related theft is therefore very low for people with SMI. Other property crimes are clearly more common in patients with SMI than in the general population (examples being burglary, pickpocketing and robbery).
In addition, the symptomatology of the participants in this study may differ slightly from the general SMI population. Due to our sample selection procedure, in-patients were over-represented in our sample group (23.6%) by comparison with the general SMI population in Amsterdam (7%), and this may limit the generalisability of our findings. Second, only a few people in the SMI group in our study were severe substance misusers, and the analysis of subgroups who were substance-dependent was therefore not possible. Furthermore, we have no information about mental health problems in the comparison group. The comparison group is a random sample of the general population and is therefore likely to represent a normal distribution of mental health problems including SMI. In The Netherlands approximately 1.5% of the total population had an SMI. Reference Delespaul40 Although we were unable to control for these factors in our analysis, we do not anticipate this affecting our results because of the small proportion of people with SMI in the comparison group. Finally, our prevalence rate for victimisation could be an underestimate: patients included in this study receive treatment and are not homeless, which we know from the international literature is a risk factor for victimisation.
Recommendations
First of all, our study clearly indicates that all caregivers need to bear in mind that patients with SMI are at risk of victimisation. In addition, (a) prevention programmes are needed and (b) intervention programmes are needed for patients who are already being victimised. Professionals should be aware of signs of victimisation, they should provide patients with treatment and conduct risk assessments. Improving the detection of risk factors is the first step to improving services. Reference Teplin, McClelland, Abram and Weiner10 When professionals offer interventions they should screen patients in terms of age, substance use, type of treatment facility and symptoms of disorganisation.
In-patients and patients living in a sheltered housing facility may benefit from training in conflict management skills to improve skills relating to interaction with other patients. Out-patients may also be victimised less by the social environment if they receive training focused on victimisation. One example of such a programme is the SOS-training (Streetwise, Otherwise, Selfwise), a group-based intervention aimed at reducing vulnerability for victimisation in patients with SMI and co-occurring substance use disorder. The SOS-training consists of three modules focused on (a) ‘street skills’ such as awareness of (un)safe places, behaviour and people; (b) avoiding or resolving conflict with others; and (c) emotion regulation, anger management and coping. Reference Goudriaan, de Waal, Van, Malesevic, Neleman, Kikker, Callaghan, Oud, Bjørngaard, Nijman, Palmstierna and Almvik41
In conclusion, there is a need for evidence-based anti-victimisation intervention programmes to improve well-being. Although our study, like other studies in the past, has identified factors and patient characteristics that are linked to victimisation, future research should focus on the mechanisms underlying the victimisation of people with SMI. A clearer understanding of the existing explanatory factors could be obtained through prospective research over an extended period of time.
Funding
This research was supported by a grant from the Stichting tot Steun VCVGZ (ST13102.Me2) and NWO, The Netherlands Organisation for Scientific Research (432-09-805).
Acknowledgements
We would like to thank the patients and mental health workers for their participation in this study. We would also like to thank OIS, Research Information and Statistics, city of Amsterdam, The Netherlands for giving us access to their data for the general population of Amsterdam.






eLetters
No eLetters have been published for this article.