Introduction
Suicide is a significant contributor to decreased life expectancy in patients with schizophrenia (Ko et al., Reference Ko, Tsai, Chi, Su, Lee, Chen and Yang2018). Lifetime prevalence estimates are 50% for suicide attempt and 5% for completed suicide (Palmer, Pankratz, & Bostwick, Reference Palmer, Pankratz and Bostwick2005; Taipale, Lähteenvuo, Tanskanen, Mittendorfer-Rutz, & Tiihonen, Reference Taipale, Lähteenvuo, Tanskanen, Mittendorfer-Rutz and Tiihonen2021). Suicidal behavior in patients with schizophrenia is often directly linked to the symptoms of the disorder and typically occurs in the first decade after onset (Sher & Kahn, Reference Sher and Kahn2019). Certain symptoms of schizophrenia, such as delusions and hallucinations, as well as social isolation and illness awareness that leads to hopelessness, are associated with an increased risk of suicide (Hettige, Bani-Fatemi, Sakinofsky, & De Luca, Reference Hettige, Bani-Fatemi, Sakinofsky and De Luca2018; Kjelby et al., Reference Kjelby, Sinkeviciute, Gjestad, Kroken, Loberg, Jorgensen and Johnsen2015; Pjescic et al., Reference Pjescic, Nenadovic, Jasovic-Gasic, Trajkovic, Kostic and Ristic-Dimitrijevic2014). Comorbid depression, a history of suicide attempts, and alcohol or substance abuse also represent major risk factors for both suicidal ideation and behavior (Cassidy, Yang, Kapczinski, & Passos, Reference Cassidy, Yang, Kapczinski and Passos2018; Hawton, Sutton, Haw, Sinclair, & Deeks, Reference Hawton, Sutton, Haw, Sinclair and Deeks2005; Hor & Taylor, Reference Hor and Taylor2010; Popovic et al., Reference Popovic, Benabarre, Crespo, Goikolea, Gonzalez-Pinto, Gutierrez-Rojas and Vieta2014; Sher & Kahn, Reference Sher and Kahn2019).
Antipsychotic medication plays a pivotal role in the treatment of schizophrenia, effectively reducing hallucinations and delusions in the majority of patients (Dixon, Lehman, & Levine, Reference Dixon, Lehman and Levine1995; Zhu et al., Reference Zhu, Li, Huhn, Rothe, Krause, Bighelli and Leucht2017). Consequently, antipsychotics may contribute to a reduction in suicidality associated with these symptoms. A study conducted by Taipale et al. (Reference Taipale, Lähteenvuo, Tanskanen, Mittendorfer-Rutz and Tiihonen2021) found that all antipsychotic medications, and in particular clozapine, effectively reduced the suicide risk. Correspondingly, several studies show that lack of adherence to antipsychotic medication may increase the suicide risk (Forsman, Taipale, Masterman, Tiihonen, & Tanskanen, Reference Forsman, Taipale, Masterman, Tiihonen and Tanskanen2019; Haukka, Tiihonen, Harkanen, & Lonnqvist, Reference Haukka, Tiihonen, Harkanen and Lonnqvist2008; Pompili et al., Reference Pompili, Lester, Grispini, Innamorati, Calandro, Iliceto and Girardi2009). A large registry-based study by Tiihonen et al. (Reference Tiihonen, Wahlbeck, Lonnqvist, Klaukka, Ioannidis, Volavka and Haukka2006b) reported that compared to use of antipsychotic medications, non-use is associated with a 37-fold increase in suicide risk in patients with schizophrenia. On the flip side, antipsychotic drugs may elicit a spectrum of adverse effects, including akathisia (psychomotor restlessness). Previous studies have suggested that akathisia may contribute to an elevated risk of suicidality in individuals with schizophrenia (Bjarke et al., Reference Bjarke, Gjerde, Jørgensen, Kroken, Løberg and Johnsen2022; Seemuller et al., Reference Seemuller, Schennach, Mayr, Musil, Jager and Maier2012). However, it is important to note that despite some findings indicating increased suicide risk with antipsychotics, current literature strongly supports the notion that antipsychotic medications offer a robust protective effect for suicidality in patients with schizophrenia.
Adjunctive psychotropic drugs, in particular antidepressants and benzodiazepines, are commonly prescribed alongside antipsychotic drugs in the treatment of schizophrenia. A review conducted by Zink, Englisch, and Meyer-Lindenberg (Reference Zink, Englisch and Meyer-Lindenberg2010) reported that approximately 70% of individuals with schizophrenia received a combination of antipsychotics and other psychotropic drugs. Despite limited evidence for added beneficial effects (Gregory, Mallikarjun, & Upthegrove, Reference Gregory, Mallikarjun and Upthegrove2017), antidepressants are frequently co-prescribed for depressive or persistent negative symptoms, such as a lack of interest and initiative (Baandrup, Reference Baandrup2020; Ballon & Stroup, Reference Ballon and Stroup2013). Given that depression is a well-known risk factor for suicide, antidepressant treatment could offer a protective effect. However, demonstrating this connection has proven to be challenging, as there is conflicting evidence regarding the association between antidepressants and suicide risk (Dragioti et al., Reference Dragioti, Solmi, Favaro, Fusar-Poli, Dazzan, Thompson and Evangelou2019; Haukka et al., Reference Haukka, Tiihonen, Harkanen and Lonnqvist2008).
Benzodiazepines are commonly used in the acute treatment of psychosis, primarily to induce sleep or to alleviate anxiety and agitated behavior (Ballon & Stroup, Reference Ballon and Stroup2013). As both insomnia and anxiety are common in patients with schizophrenia and generally linked to an elevated risk of suicide (Garay, Samalin, Hameg, & Llorca, Reference Garay, Samalin, Hameg and Llorca2015; Miller, McEvoy, & McCall, Reference Miller, McEvoy and McCall2023), it may appear intuitive that short-term benzodiazepine use has a beneficial effect on suicide risk in patients with schizophrenia. However, the use of benzodiazepines comes with a range of adverse effects, including addiction and withdrawal symptoms, and several studies have indicated that benzodiazepine use is associated with an increased risk of suicide (Dodds, Reference Dodds2017; Tiihonen, Mittendorfer-Rutz, Torniainen, Alexanderson, & Tanskanen, Reference Tiihonen, Mittendorfer-Rutz, Torniainen, Alexanderson and Tanskanen2016; Tiihonen, Suokas, Suvisaari, Haukka, & Korhonen, Reference Tiihonen, Suokas, Suvisaari, Haukka and Korhonen2012). A review by Dodds (Reference Dodds2017) concluded that benzodiazepines appear to cause increased risk of attempted and completed suicide, potentially due to factors such as withdrawal symptoms, overdoses or heightened levels of aggression and impulsivity.
Taken together, suicidality represents a major concern in patients with schizophrenia. While previous studies have emphasized non-adherence to antipsychotic medication as a risk factor for suicide in patients with schizophrenia (Forsman et al., Reference Forsman, Taipale, Masterman, Tiihonen and Tanskanen2019; Haukka et al., Reference Haukka, Tiihonen, Harkanen and Lonnqvist2008), this study contributes with new knowledge regarding the impact of adjunctive medications on suicidality in this population. Non-adherence and concomitant psychotropic treatment are prevalent in clinical practice, but prospective studies investigating the effect of antipsychotic drugs, antidepressants, and benzodiazepines on suicidality in a real-life clinical setting are scarce. With a large cohort, a follow-up period of up to 10 years, and the possibility to take account for potentially confounding factors such as alcohol or substance abuse, depression, and aggression, the present study can provide a robust analysis of the association between suicidality and use of different psychotropic drugs. Accordingly, the aim of this study is to investigate how the use and non-use of psychotropic medications are associated with the risk of readmission with suicidal plans and attempted or completed suicide in patients with schizophrenia.
Material and methods
A major part of the material and methods has been outlined in three prior publications by Stromme et al. (Stromme et al. Reference Stromme, Mellesdal, Bartz-Johannesen, Kroken, Krogenes, Mehlum and Johnsen2021, Reference Stromme, Mellesdal, Bartz-Johannesen, Kroken, Krogenes, Mehlum and Johnsen2022b; Strømme, Bartz-Johannesen, Kroken, Mehlum, & Johnsen, Reference Strømme, Bartz-Johannesen, Kroken, Mehlum and Johnsen2022a), all stemming from the same study cohort, but are specified as follows:
Sample
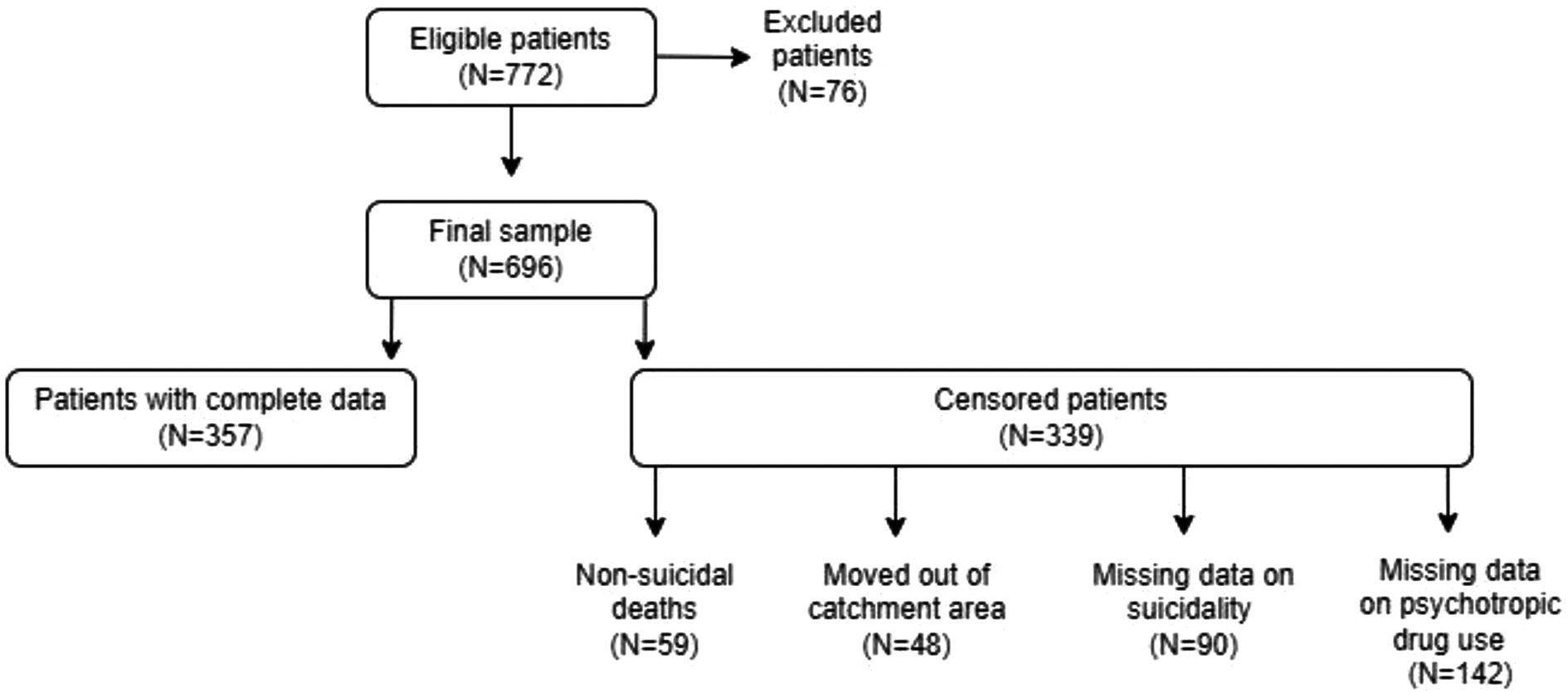
The study was carried out at the Division of Psychiatry, Haukeland University Hospital, Bergen, Norway. The hospital serves approximately 95% of individuals requiring acute psychiatric hospitalization in an area with a catchment population of about 400 000. All patients admitted consecutively to the psychiatric acute ward between 1 May 2005 and 15 June 2014, who met criteria for a discharge diagnosis of schizophrenia according to the ICD-10 (https://icd.who.int/browse10/2019/en) codes F 20.0–F 20.9, were considered eligible for inclusion. A total of 772 eligible patients were admitted over the span of 10 years (Fig. 1). Among them, 76 patients were excluded due to insufficient information regarding use of antipsychotic drugs post-discharge. Consequently, the final sample comprised 696 patients.
Flow of patients through the study.
Procedure
Patients diagnosed with schizophrenia were included upon their initial acute admission, hereby referred to as the ‘index admission,’ during the study. The follow-up started at discharge from the index admission. It ended either on the date of censoring (1 May 2015), at the date of an attempted or completed suicide, or at the date of the first acute psychiatric readmission with the presence of suicidal plans. As shown in Fig. 1, patients were censored if they died from other causes than suicide (n = 59, 8.5%), moved out of the hospital's catchment area (n = 48, 6.9%), had missing data about psychotropic drug use after discharge (n = 142, 20.4%), or suicidal behavior and ideation at time of readmission (n = 90, 12.9%).
The recording of drug prescriptions during the follow-up period was conducted retrospectively based on medical records. All available information from patients, their families, medical records, and, when accessible, serum-level measurements, was utilized to assess drug adherence. Data extraction was performed by M. F. S. and a research nurse, and any questions were logged and resolved within the research team. Ambiguity regarding medication use led to the censoring of the patient. In line with previous studies in the field (Mullins, Obeidat, Cuffel, Naradzay, & Loebel, Reference Mullins, Obeidat, Cuffel, Naradzay and Loebel2008; Sikka, Xia, & Aubert, Reference Sikka, Xia and Aubert2005), periods of non-use of medications lasting up to 2 weeks were not recorded as terminations if the medication was resumed thereafter. If information regarding medication use was unavailable, patients were censored after the last known day of information retrieval. Information regarding suicides and deaths from other causes was obtained by connecting the patients' 11-digit national identity number with data sourced from the Norwegian Cause of Death Registry (conducted 14 November 2016).
Variables
At every admission during the follow-up period, we recorded any suicidal ideation and suicide attempts preceding the admission. The level of depressive mood and of overactive, aggressive, disruptive, or agitated behavior was assessed using the first and seventh items of the Health of The Nation Outcome Scale (HoNOS) (Wing et al., Reference Wing, Beevor, Curtis, Park, Hadden and Burns1998), respectively. HoNOS is a clinician-rated instrument that measures psychiatric symptoms and behavior on a five-point scale ranging from ‘no problems’ to ‘severe to very severe problems’. The level of depressive mood and agitated behavior measured at index admission was applied in the analyses.
The Alcohol Use Scale (AUS) and Drug Use Scale (DUS) are one-item assessments conducted by clinicians to evaluate alcohol and drug use, respectively, the last 6 months prior to admission (Drake, Rosenberg, & Mueser, Reference Drake, Rosenberg and Mueser1996). Use is measured on a five-point scale ranging from ‘no problems’ to ‘extremely severe problems’ (Drake, Rosenberg, & Mueser, Reference Drake, Rosenberg and Mueser1996). AUS and DUS scores given at index admission were used in the analyses.
To capture periods with and without use of each psychotropic drug in individual patients, we used a dichotomous time-dependent variable that distinguished between ‘use’ and ‘no use’. The category ‘no use’ of psychotropic drugs encompassed both cases of patient non-adherence and instances where drug discontinuation was undertaken in collaboration with clinicians. Medications were classified according to the Anatomical Therapeutic Chemical (ATC) system. The included antipsychotic medications comprised amisulpride, aripiprazole, clozapine, flupentixol, haloperidol, olanzapine, paliperidone, perphenazine, pimozide, quetiapine, risperidone, sertindole, ziprasidone, and zuclopenthixol. The group of antidepressants included amitriptyline, bupropion, citalopram, clomipramine, doxepin, duloxetine, escitalopram, fluoxetine, fluvoxamine, mianserin, mirtazapine, moclobemide, nortriptyline, paroxetine, phenelzine, reboxetine, sertraline, trimipramine, and venlafaxine. The category of benzodiazepines included alprazolam, diazepam, flunitrazepam, nitrazepam, oxazepam, zolpidem, and zopiclone.
Statistics
The primary outcome of the two main analyses was (1) attempted or completed suicide, and (2) readmission with suicidal plans, respectively. Coincidences, such as timely intervention or insufficient means, often determine whether the patient survives a suicide attempt or not (Gvion & Levi-Belz, Reference Gvion and Levi-Belz2018). Accordingly, in this study we have opted to combine attempted and completed suicides as one primary outcome measure. This approach enhances the statistical power by increasing the number of outcomes.
Periods of use v. non-use of antipsychotics, antidepressants, and benzodiazepines in each patient were incorporated as time-dependent variables in Cox multiple regression analyses, aiming to investigate their associations with either (1) attempted or completed suicide, or (2) readmission with suicidal plans. In accordance with the pre-planned analysis plan, the multivariate models also adjusted for well-known confounders, including gender, age, depressive mood, agitated behavior, and excessive use of alcohol and illicit substances. To ensure the robustness of the results, both univariate and multivariate analyses were conducted.
The statistical software R version 4.0.2 (https://www.r-project.org/) and the ‘survival’ package were used for the statistical analyses. The assumption of Cox proportional hazards was validated using the cox.zph() function from the survival package.
Ethics
The study received an approval from the Norwegian Directorate of Health, the Norwegian Centre for Research Data, and from the Regional Committee for Medical Research Ethics (approval No. REK 46004). These authorities authorized the use of patient information without requiring informed consent. The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
Results
An overview of clinical and sociodemographic characteristics at baseline is presented in Table 1.
Baseline characteristics of the sample at index admission (n = 696)a
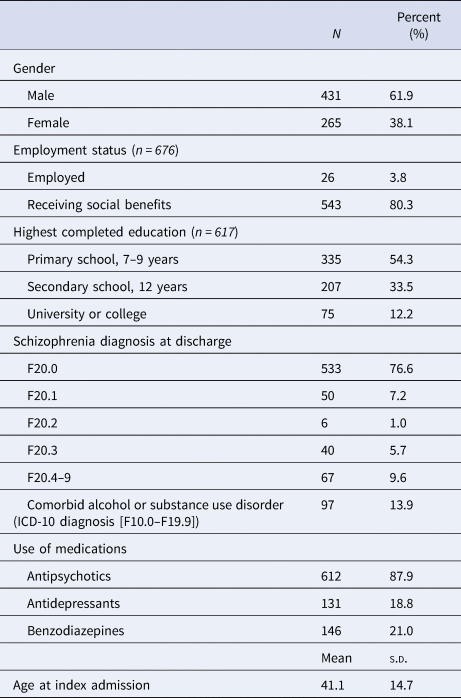
a If values are missing, the total n is presented.
N, Number; s.d., standard deviation.
Attempted or completed suicide
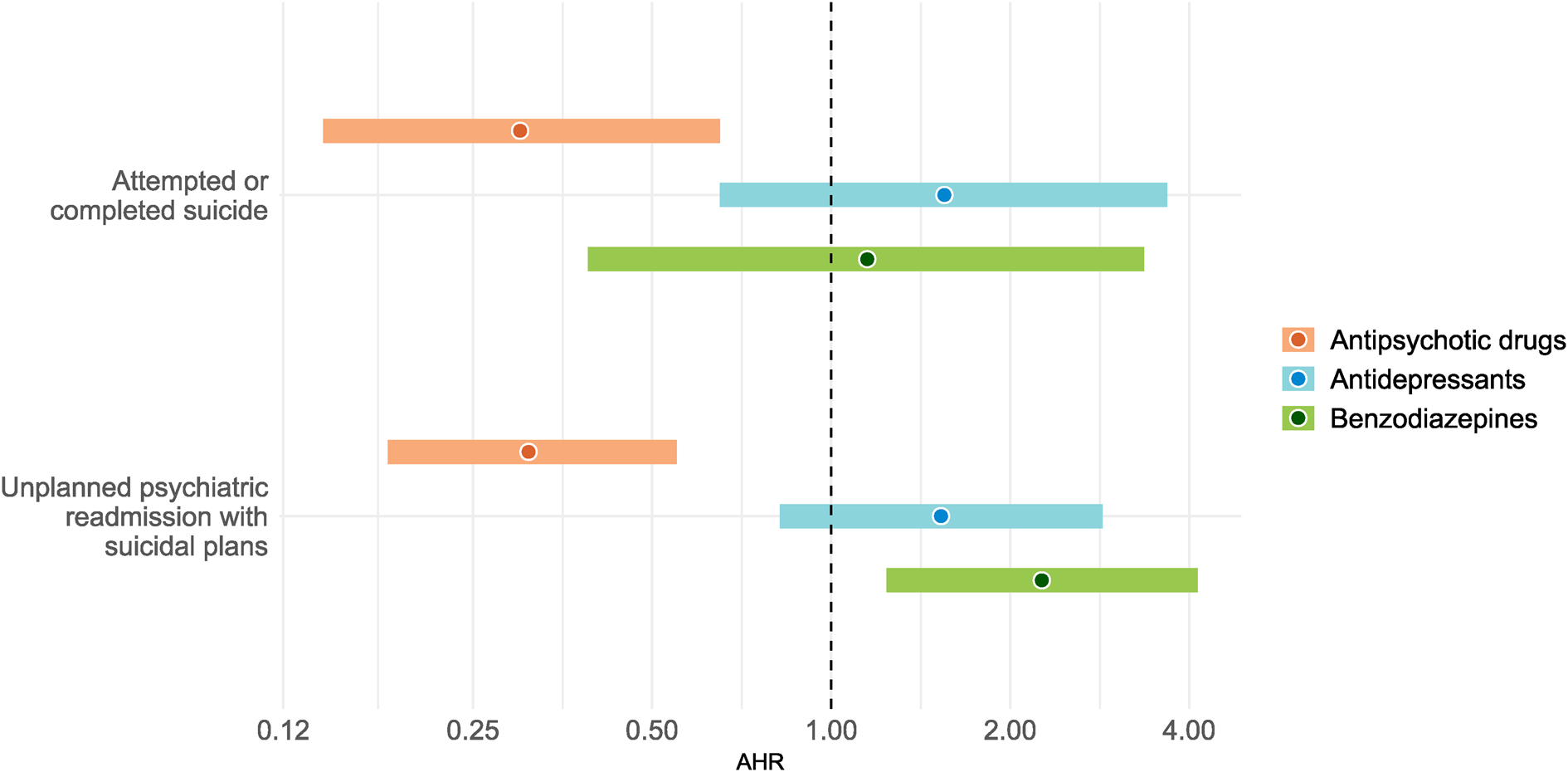
Throughout the follow-up period, a total of 23 (3.3%) patients attempted suicide, while 9 (1.3%) completed suicide. The mean (s.d.) and median durations in years until attempted or completed suicide were 1.7 (1.6) and 1.2, respectively. The key findings are shown in Fig. 2, while the comprehensive results of both the multivariate and univariate Cox analyses are provided in Table 2. In the multivariate analyses, there was a statistically significant negative association between the risk of attempted or completed suicide and the use of antipsychotic medications (adjusted hazard ratio [AHR] = 0.30, p < 0.01, CI 0.14–0.65). This indicates that, compared to periods of non-use, the use of antipsychotic drugs was associated with a 70% reduced risk of attempted or completed suicide. Age also exhibited a statistically significant negative association with the risk of attempted or completed suicide (AHR = 0.96, p = 0.01, CI 0.93–0.99), indicating a 4% decrease in risk per year. No significant associations were observed between the risk of attempted or completed suicide and gender, depressive mood, agitated behavior, excessive use of alcohol or illicit substances, or use of antidepressants or benzodiazepines.
Associations between psychotropic drug use and suicidality: adjusted hazard ratios (AHR) from Cox multiple regression models. The AHRs show the associations between the use of different psychotropic drugs and the risk of attempted or completed suicide, as well as unplanned psychiatric readmission with suicidal plans. Compared to non-use, use of antipsychotics was associated with 70% lower risk of attempted or completed suicide (AHR = 0.30, p < 0.01, CI 0.14–0.65) and 69% reduced risk of readmission with suicidal plans (AHR = 0.31, p < 0.01, CI 0.18–0.55). Use of prescribed benzodiazepines was associated with 126% increased risk of readmission with suicidal plans (AHR = 2.26, p = 0.1, CI 1.24–4.13). The results are presented on a log-transformed scale along the horizontal axis.
Risk factors of attempted or completed suicide (n = 696, whereof n = 32 attempted or completed suicide)
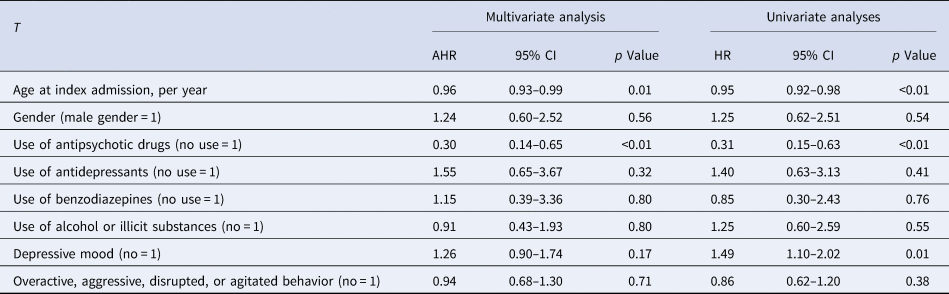
AHR, adjusted hazard ratio.
Readmission with suicidal plans
A total of 462 patients (66.4%) experienced at least one readmission during the follow-up period. Among these, 59 were readmitted with suicidal plans, with mean (s.d.) and median durations until readmission with suicidal plans being 2.3 (2.4) and 1.2 years, respectively.
The primary findings are displayed in Fig. 2, while the detailed outcomes of both the multivariate and univariate Cox analyses are outlined in Table 3. In the multivariate analyses, there were statistically significant negative associations between readmission with suicidal plans, and the use of antipsychotic medications (AHR = 0.31, p < 0.01, CI 0.18–0.55). This signifies that, compared to periods of non-use, the risk of readmission with suicidal plans was reduced by 69% for individuals utilizing antipsychotics. Additionally, positive associations were found between readmission with suicidal plans and the use of prescribed benzodiazepines (AHR = 2.26, p = 0.01, CI 1.24–4.13) and female gender (AHR = 1.75, p = 0.01, CI 1.04–2.95). This indicates that, compared to periods of non-use, use of prescribed benzodiazepines is associated with 126% increased risk. Moreover, female gender was associated with 75% increased risk of readmission with suicidal plans. No significant associations were observed between readmission with suicidal plans and age, depressive mood, agitated behavior, excessive use of alcohol or illicit substances, and use of antidepressants.
Risk factors of unplanned psychiatric readmission with suicidal plans (n = 696, whereof n = 59 were readmitted to a psychiatric acute ward with suicidal plans)
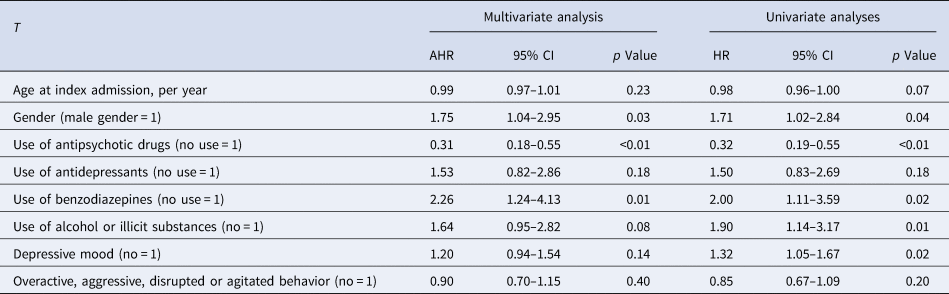
AHR, adjusted hazard ratio.
Discussion
In a cohort of 696 acutely admitted patients with schizophrenia, we found that use of antipsychotic drugs was associated with approximately 70% lower risk of attempted or completed suicide and of readmission with suicidal plans throughout the follow-up period. In contrast, the use of prescribed benzodiazepines was associated with 126% increased risk of readmission with suicidal plans.
Antipsychotic medication and suicidality
Our results demonstrate that, when compared to periods of non-use, use of antipsychotics was associated with 70 and 69% lower risk of attempted or completed suicide, and readmission with suicidal plans, respectively. This is in accordance with previous research, where non-adherence to antipsychotic drugs consistently emerges as a significant risk factor for suicidality in individuals with schizophrenia (Hassan et al., Reference Hassan, De Luca, Dai, Asmundo, Di Nunno, Monda and Villano2021; Hor & Taylor, Reference Hor and Taylor2010; Pompili et al., Reference Pompili, Amador, Girardi, Harkavy-Friedman, Harrow, Kaplan and Tatarelli2007; Taipale et al., Reference Taipale, Lähteenvuo, Tanskanen, Mittendorfer-Rutz and Tiihonen2021; Tiihonen et al., Reference Tiihonen, Wahlbeck, Lonnqvist, Klaukka, Ioannidis, Volavka and Haukka2006b). Active hallucinations and delusions are established risk factors for suicide in individuals with schizophrenia (Hor & Taylor, Reference Hor and Taylor2010). Moreover, insomnia has been proposed as a contributing factor to suicidal ideation, suicide attempts, and completed suicide within this group (Waite, Sheaves, Isham, Reeve, & Freeman, Reference Waite, Sheaves, Isham, Reeve and Freeman2020). Antipsychotic medication has demonstrated efficacy in reducing hallucinations and delusions in patients with schizophrenia (Sommer et al., Reference Sommer, Slotema, Daskalakis, Derks, Blom and van der Gaag2012), and antipsychotics can also enhance sleep (Monti, Torterolo, & Pandi Perumal, Reference Monti, Torterolo and Pandi Perumal2017). These properties may contribute to the protective effect of antipsychotics on suicidality.
Antidepressants and suicidality
We found no associations between the use of antidepressants and the risk of neither attempted or completed suicide, nor readmission with suicidal plans. While prior studies on combination therapy in patients with schizophrenia have indicated an impact of antidepressants on negative symptoms (Singh, Singh, Kar, & Chan, Reference Singh, Singh, Kar and Chan2010) and all-cause mortality (Haukka et al., Reference Haukka, Tiihonen, Harkanen and Lonnqvist2008; Lin, Yeh, & Pan, Reference Lin, Yeh and Pan2023), few studies have demonstrated a significant effect on suicidality (Reutfors et al., Reference Reutfors, Bahmanyar, Jönsson, Brandt, Bodén, Ekbom and Osby2013; Tiihonen et al., Reference Tiihonen, Lonnqvist, Wahlbeck, Klaukka, Tanskanen and Haukka2006a, Reference Tiihonen, Suokas, Suvisaari, Haukka and Korhonen2012). The evidence regarding the association between antidepressants and suicide risk is somewhat conflicting (Ballon & Stroup, Reference Ballon and Stroup2013; Dragioti et al., Reference Dragioti, Solmi, Favaro, Fusar-Poli, Dazzan, Thompson and Evangelou2019). Although some previous studies have suggested that antidepressants are associated with an increased short-term risk of suicidal acts in young people with psychiatric disorders (Hawkins et al., Reference Hawkins, Coryell, Leung, Parikh, Weston, Nestadt and El-Mallakh2021), the majority of studies, including comprehensive systematic reviews (Dragioti et al., Reference Dragioti, Solmi, Favaro, Fusar-Poli, Dazzan, Thompson and Evangelou2019), have concluded that antidepressants represent a safe treatment option for psychiatric disorders.
Benzodiazepines and suicidality
Our results revealed a significant association between the use of prescribed benzodiazepines and increased risk of readmission with suicidal plans, but not with increased risk of attempted or completed suicide in patients with schizophrenia. However, previous studies have identified associations with risk of attempted and completed suicide in this patient group (Dodds, Reference Dodds2017; Tiihonen et al., Reference Tiihonen, Suokas, Suvisaari, Haukka and Korhonen2012, Reference Tiihonen, Mittendorfer-Rutz, Torniainen, Alexanderson and Tanskanen2016). One potential explanation for the discrepancy between our results and previous studies may lie in the infrequency (n = 32) of attempted and completed suicides within our study cohort. We cannot exclude the possibility that this is a type 2 error, due to lack of statistical power. Moreover, confounding by indication is a well-known challenge in pharmacological cohort studies, as the use of medications is not randomized. Aggression and agitation not only represent risk factors for suicide (McGirr & Turecki, Reference McGirr and Turecki2008; Pompili et al., Reference Pompili, Lester, Grispini, Innamorati, Calandro, Iliceto and Girardi2009), but also serve as common rationales for the prescription of benzodiazepines in patients with schizophrenia (Dold et al., Reference Dold, Li, Tardy, Khorsand, Gillies and Leucht2012). Many prior studies on suicidality and benzodiazepines have failed to adjust for the patients' levels of aggression and agitation, and it is not surprising that these studies identify an association between benzodiazepine use and suicide risk. In our study, we addressed this concern by adjusting for the baseline levels of overactive, aggressive, disrupted, or agitated behavior. This adjustment might, at least partly, explain why our findings differ from those reported in previous studies.
Other findings
In line with other studies on suicidality in patients with schizophrenia (Hor & Taylor, Reference Hor and Taylor2010; Sher & Kahn, Reference Sher and Kahn2019), we found that younger age was independently associated with increased risk of attempted or completed suicide. Interestingly, our results did not reveal a significant association between age and the risk of readmission with suicidal plans, suggesting that while suicidal ideation spans across all age categories, the occurrence of actual suicides and suicide attempts is most prevalent among younger patients within a psychiatrically hospitalized cohort such as this. With regard to gender, a notable difference in suicidal behavior has been documented in previous literature, revealing a higher prevalence of females with non-fatal suicidal incidents and a predominance of males in completed suicides, commonly referred to as the ‘gender paradox of suicidal behaviour’, just as in the general population (Schrijvers, Bollen, & Sabbe, Reference Schrijvers, Bollen and Sabbe2012; Sher & Kahn, Reference Sher and Kahn2019). However, in patients with schizophrenia, previous research has indicated that the gender gap in completed suicides is notably less pronounced compared to the general population (Sher & Kahn, Reference Sher and Kahn2019). In line with this, our results showed that female gender was associated with an increased risk of being readmitted with suicidal plans. Moreover, no association was found between male gender and increased risk of attempted or completed suicide, perhaps because the primary outcome of the analyses included both attempted and completed suicides, not solely completed suicides.
Numerous studies have identified depression, agitated behavior, and abuse of alcohol and substances as potential risk factors for suicide in patients with schizophrenia (Hettige et al., Reference Hettige, Bani-Fatemi, Sakinofsky and De Luca2018; Hor & Taylor, Reference Hor and Taylor2010; McGirr & Turecki, Reference McGirr and Turecki2008; Sher & Kahn, Reference Sher and Kahn2019). In contrast, our results show no significant associations between the risk of attempted or completed suicide and either depressive mood, overactive, aggressive, disrupted, or agitated behavior, nor excessive use of alcohol or illicit substances. Similarly, no such associations were found between these factors and the risk of readmission with suicidal plans. This can possibly be attributed to the fact that our analyses relied solely on assessments of these factors at the initiation of the index admission. However, depression, agitation, and abuse of alcohol and substances are known to fluctuate over time, limiting the usefulness of one initial measurement.
Strengths and limitations
A key limitation of this study is its observational design, involving the non-randomized use of psychotropic drugs. This limits our ability to draw causal conclusions and raises the risk of confounding by indication. Confounding by indication occurs when clinical indications influence treatment decisions and are independent risk factors for the study outcome (Sendor & Stürmer, Reference Sendor and Stürmer2022). Benzodiazepines are commonly prescribed to patients with schizophrenia to manage agitation, aggression, or anxiety (Dold et al., Reference Dold, Li, Tardy, Khorsand, Gillies and Leucht2012), all of which are also risk factors for suicidality (McGirr & Turecki, Reference McGirr and Turecki2008; Pompili et al., Reference Pompili, Lester, Grispini, Innamorati, Calandro, Iliceto and Girardi2009). This confounding by indication may, at least partially, explain our observed association between benzodiazepine use and an increased risk of readmission with suicidal plans. Similarly, antipsychotic drugs are prescribed to manage psychosis (Tandon, Nasrallah, & Keshavan, Reference Tandon, Nasrallah and Keshavan2010). Since psychotic symptoms are well-known risk factors for suicidality, our finding of an association between antipsychotic use and a reduced risk of suicidality may actually be an underestimation. However, to address the issue of confounding by indication, we have accounted for well-known confounding variables in our analyses. Another possible approach to address this issue could involve excluding, for instance, the first 30 days of drug exposure. Unfortunately, conducting such an analysis was not feasible without compromising the statistical model used in this study.
Other limitations include the following: First, instances of suicidality that did not result in an acute psychiatric admission were not recorded. While the impact of incorporating such data into our analysis remains uncertain, it is likely that similar trends would persist, even among less severe manifestations of suicidality. Second, we lacked data regarding the doses of psychotropic medication used, and accordingly, we were unable to analyze the potential impact of varying doses on the risk of suicidality. Third, the term ‘non-use’ of antipsychotic drugs included both non-adherence and clinician-guided discontinuation. Given the assumption that discontinuation under a clinician may be associated with lower risk, our findings might have differed if we had exclusively examined this subset. However, recent studies have indicated that the mode of antipsychotic discontinuation is less important than previously believed (McCutcheon et al., Reference McCutcheon, Taylor, Rubio, Nour, Pillinger, Murray and Jauhar2023; Moncrieff et al., Reference Moncrieff, Crellin, Stansfeld, Cooper, Marston, Freemantle and Priebe2023). Fourth, data collection always includes subjective elements. However, we have addressed this by implementing defined algorithms in cases of doubt, ensuring a transparent and rigorous data collection process. Finally, statistical guidelines normally recommend 10 or more outcome events per predictor variable in Cox regression models (Vittinghoff & McCulloch, Reference Vittinghoff and McCulloch2007). Our multivariate analyses, with eight predictor variables each, yielded 4 and 7.4 outcomes per variable, respectively, and accordingly they fall short of the ideal threshold. Despite this statistical concern, the univariate analyses showed mainly the same results as the multivariate analyses. Thus, there is little reason to anticipate different outcomes with a reduced number of predictor variables in the multivariate analyses.
A major strength of this study is the large and unselected sample. Due to the study design and the authorization to include all patients discharged with a diagnosis of schizophrenia from a psychiatric acute unit, irrespective of consent, the sample includes even the most severely ill patients. Accordingly, the sample is highly representative for patients with schizophrenia admitted to a psychiatric acute ward. A less ill group with higher level of insight might, paradoxically, be at higher risk of suicide. Hence, it is possible that in a sample of less severely ill patients than ours, the associations between the use of psychotropic drugs and the risk of suicidality might be different from those found in our study. The time-dependent analyses, reflecting a real-life setting where patients use psychotropic medications intermittently, contribute further to high generalizability. In contrast, antipsychotic drug trials in general, and in particular randomized controlled trials, have faced criticism for their limited generalizability due to issues like selection bias, short trial durations, and small sample sizes (Leucht, Heres, Hamann, & Kane, Reference Leucht, Heres, Hamann and Kane2008). Moreover, the study has a long follow-up period of up to 10 years. Data on suicides were gathered from the Norwegian Cause of Death Registry and there is only one psychiatric acute ward in the catchment area, both contributing to complete follow-up data. The study also accounts for potentially confounding factors such as alcohol or substance abuse, depression, and aggression. As such, the study will probably provide a more robust and less biased analysis of the association between suicidality and the use of different psychotropic drugs in a population with sufficiently severe symptoms to require acute hospitalization.
Conclusion
In the present study, we have shown that adherence to antipsychotic medication is strongly associated with reduced risk of attempted or completed suicide in patients with schizophrenia. We also identified use of prescribed benzodiazepines as a significant risk factor for being readmitted with suicidal plans. Future research should aim to replicate these results in studies designed to identify causal associations. If confirmed as significant and causal, these findings should impact future treatment guidelines.
Acknowledgments
The authors express their gratitude to the research nurses and scientists in the Bergen Psychosis Research Group for their valuable contributions, which ensured the high quality of the data. Special thanks are extended to Marianne Krogenes for her contribution to the data extraction, and to the late Liv Solrunn Mellesdal for her invaluable contributions to this work, serving as the founder and principal investigator of SIPEA.
Funding statement
The study was funded by the Division of Psychiatry, Haukeland University Hospital, and received additional support in the form of research grants from the Western Norway Regional Health Authority (grant numbers: 911209/HV and 911671/HV). The funders were not involved in design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Competing interests
None.







