Introduction
Many people with health problems do not take up offers of treatment. For instance, after a heart attack a majority do not attend rehabilitation programmes despite the established benefits (e.g. Lane et al. Reference Lane, Carroll, Ring, Beevers and Lip2001). Health psychologists have emphasized that responses to a given condition, including adherence to treatment and overall outcomes, follow logically from people's perceptions of their problems (Leventhal et al. Reference Leventhal, Diefenbach and Leventhal1992). Cooper et al. (Reference Cooper, Lloyd, Weinman and Jackson1999), for example, found that patients who did not attend cardiac rehabilitation were less likely than attenders to believe that their condition was controllable and that their lifestyle might have contributed to their illness. The non-attending cardiac patients' beliefs about their condition did not fit with the treatment offered. In understanding responses to physical illnesses, key appraisals concern ideas about the cause, the length of time the problems will last, the severity of the consequences, and the degree of control (Weinman et al. Reference Weinman, Petrie, Moss-Morris and Horne1996; Hagger & Orbell, Reference Hagger and Orbell2003; Petrie et al. Reference Petrie, Jago and Devcich2007). This framework has now been successfully applied to understanding emotional adaptation and quality of life in severe mental health conditions such as psychosis (Lobban et al. Reference Lobban, Barrowclough and Jones2004; Watson et al. Reference Watson, Garety, Weinman, Dunn, Bebbington, Fowler, Freeman and Kuipers2006). In this report, we examine illness beliefs, specifically in relation to the successful take-up of psychological treatment for psychosis.
Meta-analyses lead to conclusions that cognitive behaviour therapy (CBT) can reduce the positive symptoms of psychosis (e.g. Zimmermann et al. Reference Zimmerman, Favrod, Trieu and Pomini2005; Wykes et al. Reference Wykes, Steel, Everitt and Tarrier2008; NICE, 2009), although the effect sizes in intention-to-treat (ITT) analyses of this first generation of therapies lie in the weak to moderate range. CBT for psychosis aims to give patients a better understanding and control of their experiences to reduce distress and increase functioning. It typically involves helping people understand the factors causing their difficulties, reviewing and testing unhelpful beliefs, and implementing more helpful coping techniques (e.g. Fowler et al. Reference Fowler, Garety and Kuipers1995).
However, not all clients will engage with CBT, and not all benefit from it. There have been few reports of the factors influencing the take-up of CBT for psychosis. Lack of ‘insight’, that is failure to endorse the view that a psychiatric illness is present, has been identified as affecting therapeutic alliance and completion of therapy (Álvarez-Jiménez et al. Reference Álvarez-Jiménez, Gleeson, Cotton, Wade, Gee, Pearce, Crisp, Spiliotacopoulos, Newman and McGorry2009; Wittorf et al. Reference Wittorf, Jakobi, Bechdolf, Muller, Sartory, Wagner, Wiedemann, Wolwer, Herrlich, Buchkremer and Klingberg2009; Barrowclough et al. Reference Barrowclough, Meier, Beardmore and Emsley2010). However, no study has examined patients' beliefs about their problems in detail, or considered the use of therapeutic strategies during the sessions. We therefore included the standard instrument for assessing illness representations, the Illness Perception Questionnaire (IPQ; Weinman et al. Reference Weinman, Petrie, Moss-Morris and Horne1996), in the pre-therapy baseline assessment for the Psychological Prevention of Relapse in Psychosis (PRP) Trial (Garety et al. Reference Garety, Fowler, Freeman, Bebbington, Dunn and Kuipers2008; Dunn et al. Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012), a large randomized controlled trial that compared CBT for psychosis with treatment as usual.
In this trial there was heterogeneity in take-up of therapy, and this determined outcome. Taken as a group, the ITT analysis for the PRP Trial showed that simply being randomly allocated to CBT resulted in very little benefit (Garety et al. Reference Garety, Fowler, Freeman, Bebbington, Dunn and Kuipers2008). However, only 41% of patients allocated to CBT had the more active types of therapeutic techniques. In a planned analysis that used structural equation modelling to estimate ITT effects for subgroups, we demonstrated that patients receiving full active therapy did extremely well, spending more months in remission and having less severe psychotic and affective symptoms than if they had not had CBT (Dunn et al. Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012). It is important to emphasize that the analysis demonstrated that this was not a group who were already likely to have good outcomes: it was the receipt of therapy that led to benefits. Comparing treated people who did and did not have full therapy revealed no differences, it was the comparison to the control group that identified benefits. However, there was a degree of symptomatic deterioration in the 38% of patients who were maintained in therapy but received only basic assessment and engagement components without progressing to active components of therapy (‘partial therapy’). The remaining 21% of patients received no therapy because they did not even attend sessions.
In this report we consider why individuals had different levels of therapy. It is a direct attempt to understand one aspect of the findings of Dunn et al. (Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012). We hypothesized that there would be differences in illness perceptions between those who went on to be fully engaged in therapy, those who did not engage with active therapeutic techniques, and those who did not attend sessions. Thus, people who benefit from CBT for psychosis would tend to have more psychologically orientated views of their problems. Specifically, we predicted that clients who engaged in full therapy and therefore derived symptomatic benefits would be those with psychological explanations for their difficulties and a belief that they could establish a degree of control over them. Finally, we examined the role of insight because of the earlier work indicating an effect on the therapy process (e.g. Barrowclough et al. Reference Barrowclough, Meier, Beardmore and Emsley2010).
Method
Participants
This report concerns the 92 PRP Trial participants who had completed the IPQ (Weinman et al. Reference Weinman, Petrie, Moss-Morris and Horne1996) at the pre-randomization baseline assessment, and were allocated to CBT and subsequently categorized using ratings of audiotapes by Dunn et al. (Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012) as having had ‘full therapy’, ‘partial therapy’ or ‘no therapy’. Therefore, the study explicitly uses the patient classifications carried out by Dunn et al. (Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012) to explain the take-up of therapy in the trial. Ten out of the 102 patients in the original report had not completed the IPQ.
The inclusion criteria for trial participants were: a current clinical diagnosis of non-affective psychosis in ICD-10 F20–29 (WHO, 1992) and DSM-IV (APA, 1994); age 18–65 years; a second or subsequent psychotic episode starting not more than 3 months before they agreed to enter the trial; and a rating of at least 4 (moderate severity) for at least one positive symptom on the Positive and Negative Syndrome Scale (PANSS; Kay, Reference Kay1991). Exclusion criteria comprised: a primary diagnosis of alcohol or substance dependence, organic syndrome or learning disability; spoken English inadequate for engaging in psychological therapy; and unstable residential arrangements such that the likelihood of being available for the duration of the trial was low. Participants provided informed consent under protocols approved by the appropriate ethics committees.
Treatment
CBT was delivered for 9 months, with a planned minimum of 12 sessions and a maximum of 20 sessions. The therapy was based upon the manual of Fowler et al. (Reference Fowler, Garety and Kuipers1995), amplified to include key aspects of relapse prevention highlighted in our cognitive model (Garety et al. Reference Garety, Kuipers, Fowler, Freeman and Bebbington2001). The mean number of sessions was 14.3 (s.d. = 7.8), each session lasting on average 1 h. Most of the participants received therapy from five lead trial therapists, all doctorate level or equivalent clinical psychologists employed full time on the trial. Additional cases were seen by therapists employed by local mental health services. These therapists were doctoral clinical psychologists and nurses with specialist training in CBT for psychosis. Details of recruitment, training and quality control are provided elsewhere (Garety et al. Reference Garety, Fowler, Freeman, Bebbington, Dunn and Kuipers2008).
Formal monitoring of therapy tapes was carried out throughout the trial. The Revised Cognitive Therapy for Psychosis Adherence Scale (R-CTPAS; Rollinson et al. Reference Rollinson, Smith, Steel, Jolley, Onwumere, Garety, Kuipers, Freeman, Bebbington, Dunn, Startup and Fowler2008) is a measure of fidelity that covers 21 cognitive therapy techniques for psychosis. Dunn et al. (Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012) used ratings from the R-CTPAS to create a classification for the therapy received by each person treated in the trial, and the current report aims to understand what led to a patient's particular classification. The classification was derived from factor analysis of the R-CTPAS, which generated two factors. The first, which was termed ‘partial therapy’, comprised engagement and assessment techniques, that is attempts to engage in therapeutic strategies; the ‘Columbo style’, which assesses the degree to which therapists promote guided discovery; and the collaborative assessment of psychotic experience and delusional beliefs. The second, termed ‘full therapy’, comprised active therapy techniques, that is relapse-prevention interventions; enhancing self-regulatory strategies; developing a personal model of relapse; developing a model of psychosis; work on reinterpreting the meaning of delusional beliefs and hallucinations; and schema work. For full or partial therapy to be considered present, at least one of the composite active intervention or engagement and assessment items needed to be unequivocally present across the course of therapy. Clients who received less than five therapy sessions formed a third, ‘no therapy’, group, as this number of sessions was regarded as too small for the delivery of effective CBT. Categorization of therapy was carried out by the therapists, who were unaware of the illness perception data. The latter were collected separately by research workers, before randomization to therapy. Thirty-eight participants had full therapy, 36 partial therapy and a further 18 had less than five sessions of therapy, thus falling into the no therapy group. It should be emphasized that partial therapy met the definition of highly competent cognitive therapy (in terms of the use of appropriate engagement and assessment skills), and was observed to be accompanied by attempts by the therapists to introduce and deliver the techniques of full therapy as well. Furthermore, the therapists had not simply classified the groups by their observed outcomes because there were no differences in the follow-up symptom measure scores between the full, partial or no therapy groups (Dunn et al. Reference Dunn, Fowler, Rollinson, Garety, Freeman, Kuipers, Smith, Steel, Onwumere, Jolley and Bebbington2012). The significant outcome results only emerged from the comparison with the appropriate patients in the control group (and therefore could not have been observed by the therapists).
Measures
The main measure reported here is the IPQ modified and validated for psychosis (Weinman et al. Reference Weinman, Petrie, Moss-Morris and Horne1996; Watson et al. Reference Watson, Garety, Weinman, Dunn, Bebbington, Fowler, Freeman and Kuipers2006). It was administered before trial randomization (and therefore before therapy). The IPQ assesses five main constructs: symptoms, causes, consequences, cure/control and timeline. For psychosis, the symptoms scale comprised six positive symptoms: (i) seeing images; (ii) feeling confused; (iii) hearing voices; (iv) having paranoid thoughts; (v) holding beliefs not shared by others; and (vi) feeling that one's mind is being controlled. For each item, the response format was 0–3, with a score of 0 representing ‘never’ and 3 representing ‘all the time’. Higher scores therefore indicate more symptoms. Eleven causes of psychosis are listed (e.g. ‘A germ or virus caused my current problems/illness’). The five-point scale for each putative cause was dichotomized into ‘agree’ (strongly agree, agree) and ‘not agree’ (neither agree nor disagree, disagree, strongly disagree); we were interested in whether a particular causal belief was present and not how strongly it was held. The consequences (e.g. ‘My current problems/illness have had major consequences on my life’), timeline (e.g. ‘My current problems/illness will last a long time’) and cure/control (e.g. ‘There is a lot which I can do to control my symptoms’) constructs were measured by seven, three and six items respectively. Each of these IPQ items was measured on a scale of 1–5, from strongly disagree to strongly agree. Higher scores represent greater perceived consequences, longer duration of problems and greater feelings of control. All questions were worded as referring to ‘problems/illness’ so that they could be completed by clients who did not believe that they had an illness.
Psychiatric symptoms were assessed with the PANSS (Kay, Reference Kay1991) and the Beck Depression Inventory (BDI; Beck et al. Reference Beck, Steer and Brown1996). Insight was measured using the ‘awareness of mental disorder’ item of the Scale to Assess Unawareness of Mental Disorder (Amador et al. Reference Amador, Strauss, Yale, Gorman and Endicott1993).
Statistical analysis
All analyses were conducted using SPSS 15.0 (2006). Group comparisons (no therapy, partial therapy, full therapy) for dichotomous variables were carried out using χ2 tests. Where there was an overall group effect, further comparisons of the groups were made. Group comparisons on the dimensional measures were carried out using analysis of variance (ANOVA) When the result of the ANOVA was significant, least significant post-hoc tests are reported. Finally, the ability of the IPQ to predict group membership was examined. A linear discriminant analysis was carried out, entering IPQ variables previously identified in the analysis as significant. All hypothesis testing was two-tailed.
Results
Demographic and clinical characteristics
Basic demographic and clinical information about the study participants is presented in Table 1. Participants tended to be male, unemployed, single and in their late thirties. The majority had a diagnosis of schizophrenia and had been admitted to psychiatric hospital on several occasions. The three therapy groups did not differ significantly in duration of illness (F 2,88 = 1.95, p = 0.149) or number of hospital admissions (F 2,85 = 0.53, p = 0.590). There were no differences between the groups in current levels of symptoms, whether assessed by the PANSS, BDI or by IPQ-Symptoms (see Table 3).
Demographic and basic clinical information

Values given as number or mean (standard deviation).
The perceived cause of problems
The groups differed significantly in their endorsement of three causes on the IPQ: state of mind, personality and pollution (Table 2). The full therapy group endorsed personality as a cause more than the partial therapy group [χ2(df = 1) = 5.89, p = 0.015] and the no therapy group [χ2(df = 1) = 3.88, p = 0.049]. The full therapy group endorsed state of mind as a cause more than the partial therapy group [χ2(df = 1) = 8.83, p = 0.003] but not significantly more than the no therapy group [χ2(df = 1) = 2.23, p = 0.135]. Those in the partial therapy group were more likely to endorse pollution as a cause compared with the full therapy group [χ2(df = 1) = 5.62, p = 0.018] and the no therapy group [χ2(df = 1) = 4.02, p = 0.045].
Illness Perception Questionnaire (IPQ) – causes

df, Degrees of freedom.
Perceived consequences, cure/control, timing and insight
The three groups did not significantly differ in their estimates of the consequences of their problems or in their degree of insight (Table 3). However, those in the no therapy group were significantly less likely to perceive their problems as long-lasting than both the partial therapy (p = 0.043) and the full therapy groups (p = 0.007). In addition, the partial therapy group scored significantly lower on the dimension of cure/control than the no therapy group (p = 0.012) and the full therapy group (p = 0.007).
IPQ dimensional scores, insight and psychiatric symptoms

IPQ, Illness Perception Questionnaire; PANSS, Positive and Negative Syndrome Scale; BDI, Beck Depression Inventory; s.d., standard deviation; df, degrees of freedom.
Predicting group membership
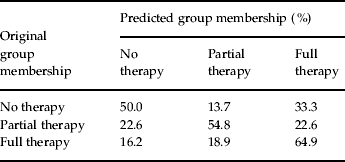
The five significant IPQ variables (state of mind, personality, pollution, cure/control, timing) were entered into a linear discriminant function analysis; 58.1% cases were classified correctly. Prediction of the full therapy group (64.9%) was higher than for the partial therapy (54.8%) and no therapy (50.0%) groups. Of note, those in the no therapy group were more likely to be misclassified as being in the full therapy group than in the partial therapy group (Table 4). A logistic discrimination analysis produced similar results.
Linear discriminant function analysis
Discussion
For clinicians practicing in the area, the variability in how CBT for psychosis proceeds is very clear. Some patients do not attend their appointments, in some instances regular attendance alone seems an achievement, and only in a proportion of cases does the collaboration lead to active adoption of new ways of thinking and behaving. In standard CBT for psychosis we know that only the latter instances lead to measurable benefit. This is the first study to examine patient characteristics that predict beneficial use of CBT for problems associated with psychosis. It is important to highlight that neither the level of symptoms nor the acknowledgement of the presence of a psychiatric illness (or ‘insight’) determined take-up of therapy; these standard psychiatric assessments did not illuminate response to psychological therapy. Instead, there were indications that the contributory factors may be what the person thought caused their problems, how long they thought the problem would last, and whether the degree of control they believed that they had seemed important. Illness representations predicted, to some extent, take-up of treatment, just as has been found for many other conditions (McAndrew et al. Reference McAndrew, Musumeci-Szabo, Mora, Vileikyte, Burns, Halm, Leventhal and Leventhal2008). Successful intervention is more likely when there is alignment between patients' ideas about their problems and the conceptual basis of the treatment approach.
The individuals who did not attend therapy typically thought that their problems would persist for less time than those who arrived for sessions. The non-attenders may have thought that there was less need for therapy, although it is of note that this was still a group with significant difficulties that had already required an average of four psychiatric admissions. Overoptimistic expectations of the duration of problems may be an important factor here. The non-attenders were also less likely to endorse psychological explanations of cause than those who had full therapy. Once clients were attending sessions, progress was facilitated if they believed they had more control over their problems, that their own psychological make-up contributed to the problems, and that unchangeable causal factors (e.g. pollution) were relatively unimportant. Indeed, the deterioration in the partial group may be accounted for by a clash between the underlying principles of therapy and the patients' ideas about their problems. Conversely, once a person was attending sessions, having psychological ideas about the cause of the problems and a sense that they could have control enabled full take-up of CBT. It seems that individuals could work with the therapists when they held the view that their ownbehaviour was important in contributing to the problems and that they could, to an extent, assert control. Of note, the non-attenders and the full therapy groups were more like each other than the partial therapy group. The non-attenders had a sense of control and some psychological explanations for their problems, but clearly they decided not to choose therapy as the way to help themselves.
Illness perceptions were only at best a moderate predictor of the groups. Our results do not mean that we can accurately predict who will derive most benefit from being offered CBT. Nor at this stage of the development of CBT for psychosis should that occur. The intervention itself is evolving, becoming more theoretically driven, targeted and problem focused (e.g. Trower et al. Reference Trower, Birchwood, Meaden, Byrne, Nelson and Ross2004; Freeman et al. Reference Freeman, Freeman and Garety2008; Foster et al. Reference Foster, Startup, Potts and Freeman2010; Freeman, Reference Freeman2011; Hepworth et al. Reference Hepworth, Startup and Freeman2011; Myers et al. Reference Myers, Startup and Freeman2011; Ross et al. Reference Ross, Freeman, Dunn and Garety2011). These findings indicate further that it is likely that techniques for encouraging more adaptive illness beliefs should be incorporated into therapy (e.g. Petrie et al. Reference Petrie, Cameron, Ellis, Buick and Weinman2002; McAndrew et al. Reference McAndrew, Musumeci-Szabo, Mora, Vileikyte, Burns, Halm, Leventhal and Leventhal2008). Thus, in the early stages of therapy the clinician might explicitly focus on, for example, beliefs about control. Such ideas may then be actively reviewed and tested. Clearly, other factors such as therapist attributes are likely to be important too. Work on treatment adherence has focused on beliefs about treatment as a key determinant (Horne & Weinman, Reference Horne and Weinman1999), showing the importance of the fit between beliefs about treatment and those about illness. Patients form their ideas about, and their response to, treatment (including adherence) in terms of their current illness model (Horne & Weinman, Reference Horne and Weinman2002; Llewellyn et al. Reference Llewellyn, Miners, Lee, Harrington and Weinman2003). Thus, future studies should include a measure of patients' beliefs about the treatment (Horne et al. Reference Horne, Weinman and Hankins1999).
Research on this topic is labour intensive and requires large samples to examine the different outcomes. Our study included 92 patients but still lacks statistical power, especially in the face of multiple statistical testing. Type 1 error may be seen in the results. Moreover, the classification rate of approximately 60% was determined from the same sample used in the derivation of the classification rule. This is likely to overestimate the success of prediction. A further weakness is that, in the assessment of illness representations, the causes were listed for the interviewees and there was no attempt to obtain respondent-generated responses. We therefore may not have been tapping the causes most pertinent to individuals. It would also be valuable to understand more about the origins of illness representations. Future studies should use the revised IPQ (Moss-Morris et al. Reference Moss-Morris, Weinman, Petrie, Horne, Cameron and Buick2002) because this separates beliefs about treatment control from personal control, and also allows investigators to assess additional illness-related beliefs, such as coherence and emotional impact.
In summary, the key clinical implication of the study is the potential informativeness of illness perceptions in the therapeutic context. These may provide an indicator of the potential progress of therapy, although replication of these findings for the psychological treatment of psychosis is clearly necessary. It is likely that encouraging and highlighting the degree to which patients have control will benefit them clinically and facilitate engagement with other therapeutic techniques. In the development of psychological approaches to psychosis, the study of illness perceptions and readiness to change may open a valuable area of future research.
Acknowledgements
This work was supported by a programme grant from the Wellcome Trust (No. 062452). D. Freeman is supported by a Medical Research Council (MRC) Senior Clinical Fellowship. P. Garety and E. Kuipers acknowledge support for their clinical sessions from the National Institute for Health Research Biomedical Research Center for Mental Health at the South London and Maudsley NHS Foundation Trust and the Institute of Psychiatry, King's College London.
Declaration of Interest
None.





