Introduction
Burnout is a pervasive, international problem affecting the healthcare workforce, characterized by emotional exhaustion, depersonalization, and decreased professional effectiveness. In a 2017 survey of 14,000 physicians, 51% endorsed clinically elevated symptoms of burnout, reflecting a significant increase from 40% in 2013 (Peckham and Grisham, Reference Peckham and Grisham2017). The highest rates of burnout reported are among emergency medicine and primary care providers (Shanafelt et al., Reference Shanafelt, Hasan, Dyrbye, Sinsky, Satele, Sloan and West2015). Drivers of burnout include increased bureaucratic tasks, overall workload, poor life–work balance, lack of flexibility, autonomy, and control, misalignment of individual and organizational values, lack of social support/community at work, and loss of meaning in work (Balch et al., Reference Balch, Freischlag and Shanafelt2009; Shanafelt et al., Reference Shanafelt, Boone, Tan, Dyrbye, Sotile, Satele, West, Sloan and Oreskovich2012; Peckham and Grisham, Reference Peckham and Grisham2017; West et al., Reference West, Dyrbye and Shanafelt2018).
Personal, organizational, and societal consequences of burnout are significant. Physician burnout is associated with increased levels of anxiety, depression, and substance use. Female physicians commit suicide at about 2.3 times the rate of the general population and male physicians about 1.4 times (Shanafelt, Reference Shanafelt2009). Physical burnout also reduces patient access to care. Burnout is one of the strongest predictors of intent to reduce clinical work hours and leave current position (West et al., Reference West, Dyrbye, Rabatin, Call, Davidson, Multari, Romanski, Hellyer, Sloan and Shanafelt2014), and nearly 20% of physicians reported an intent to reduce their clinical hours in the next year. The losses in patient services related to work cutback and early retirement have been estimated to be at least CAN$213 million (Dewa et al., Reference Dewa, Loong, Bonato, Thanh and Jacobs2014). Further, cross-sectional studies have linked physician burnout with suboptimal patient care practices (Williams et al., Reference Williams, Manwell, Konrad and Linzer2007, Klein et al., Reference Klein, Grosse, Blum and von dem Knesebeck2010), a doubled risk of medical error (Shanafelt et al., Reference Shanafelt, Balch, Bechamps, Russell, Dyrbye, Satele, Collicott, Novotny, Sloan and Freischlag2010), and a 17% increase in the odds of being named in a medical malpractice suit (Balch et al., Reference Balch, Oreskovich, Dyrbye, Colaiano, Satele, Sloan and Shanafelt2011, West et al., Reference West, Dyrbye and Shanafelt2018).
Combating burnout is a two-fold process that involves both individually focused and structural or organizational-directed solutions (West et al., Reference West, Dyrbye and Shanafelt2018). Organizational-directed interventions that foster communication between members of the healthcare team and cultivate a sense of team cohesion and job control tend to be the most effective in reducing burnout (Regehr et al., Reference Regehr, Glancy, Pitts and Leblanc2014; Ruotsalainen et al., Reference Ruotsalainen, Verbeek, Mariné and Serra2016; West et al., Reference West, Dyrbye, Erwin and Shanafelt2016; Panagioti et al., Reference Panagioti, Panagopoulou, Bower, Lewith, Kontopantelis, Chew-Graham, Dawson, van Marwijk, Geraghty and Esmail2017). Individual approaches, such as mindfulness and resilience interventions, have been shown to decrease perceived stress, increase resilience to stressful work environments, and enhance work engagement (Ruotsalainen et al., Reference Ruotsalainen, Verbeek, Mariné and Serra2016). Self-compassion is also pertinent to healthcare providers, as it is positively associated with resilience among medical residents and inversely associated with burnout among healthcare providers (Gilbert, Reference Gilbert2010; Feldman and Kuyken, Reference Feldman and Kuyken2011; Hofmann et al., Reference Hofmann, Grossman and Hinton2011; Olson et al., Reference Olson, Kemper and Mahan2015). Self-compassion involves being touched by one’s own suffering, generating the desire to alleviate one’s suffering, and treating oneself with understanding and concern (Neff, Reference Neff2003, Neff et al., Reference Neff, Hsieh and Dejitterat2005). Furthermore, increased self-compassion has been reported as a promising method of increasing resilience (Pidgeon et al., Reference Pidgeon, Ford and Klaassen2014).
Research must now address delivery models of mindfulness-based resilience trainings that enhance feasibility for onsite delivery, consider cultural considerations specific to primary care, and utilize team processes that are integral to primary care. Therefore, Mindfulness-based Wellness and Resilience (MBWR) was developed by the authors. MBWR was designed to be a brief, cost-effective, evidenced-based, and replicable curriculum to enhance mindfulness, resilience, and self-compassion among intact interdisciplinary primary care teams (IPCTs). MBWR is unique in that, it is delivered onsite among interdisciplinary teams with the aim to assist hospitals, medical centers, and training institutions in promoting health, well-being, and community among staff, ultimately, enhancing the quality of care they provide. The primary objectives of this trial were to (1) evaluate feasibility of recruitment and retention to a novel training program MBWR and (2) assess acceptability of MBWR training among IPCTs. The secondary objective was to determine the perceived effects of MBWR among IPCTs. To achieve these aims, we conducted a mixed-method, wait-list controlled trial.
Method
Participants
Recruitment and data collection occurred in a safety-net primary care center in the Pacific Northwest that serves predominately poor, uninsured, and underserved populations. As defined, primary care orientates toward family and community care and handles a wide array of patients and diseases states. Services include preventive care, physical examinations, and management of common, acute medical conditions. In addition, primary care provides care for chronic diseases and conditions, including diabetes, cardiovascular disease, mental health, and other long-term conditions. To be included in the study, individuals had to (1) be employed by the medical center; (2) be a member of an IPCT, including medical doctor, nurse, nurse practitioner, behavioral health consultant, physician assistant, medical assistant, or team assistant; (3) be willing to attend five of the eight sessions; (4) consent to complete baseline, post-, and 3-month follow-up MBWR measures; and (5) be fluent in English. Individuals were excluded if they endorsed active suicidality or psychosis, or attended a previous pilot study of MBWR. All participants provided written informed consent via a process approved by Institutional Review Board of Pacific University.
Procedures
Two researchers attended primary care team meetings to inform 45 employees of the purpose of the study, the eligibility requirements, and exclusion criteria, and receive written informed consent from interested and eligible individuals. Researchers were experts in the fields of mindfulness and resilience for high stress populations. Expected recruitment was 80% of staff informed of the training at the medical center (n = 36). A battery of measures was collected on a secure web-based survey system and administered at three time points: baseline, immediately following the 8-week intervention period, and at 3-month follow-up. Following baseline assessments, IPCTs were assigned to either MBWR or waitlist control group (WL) in a 1:1 ratio. Due to the naturalistic study design, groups were allocated to treatment arm based on scheduling and clinic space availability. Participants were not blind to the groups. WL participants received the training after 3-month follow-up measures were complete.
Intervention
MBWR, grounded in the evidence-based mindfulness practices of Mindfulness-Based Stress Reduction (Kabat-Zinn et al., Reference Kabat-Zinn, Lipworth and Burney1985) and the Mindful Practice curriculum (Epstein et al., Reference Epstein, Quill, Krasner and Mcdonald2007), was developed by the authors and designed to increase resilience, mindfulness, and self-compassion among IPCTs. IPCTs typically consist of 7–14 members and include two to three physicians, and physician assistants, nurses and nurse practitioners, medical assistants, social workers, pharmacists, and community coordinators whom all work with the same panel of patients. Eight 60-minute weekly sessions were delivered onsite directly following weekly team meetings. Weekly sessions included “formal” mindfulness practices, or time set aside to engage in mindfulness practices such as body scan, mindful breathing, sitting meditation, loving-kindness, and mindful-movement. They also included “informal” mindfulness practices that are intended as way to intentionally apply the skills and qualities fostered in formal practice to daily living. Specific informal practices were developed for the primary care setting and used prior to entering an examination room, during patient–provider communication, professional consultation, or team meetings. For example, a provider may incorporate pausing before entering an examination room, to intentionally scan their body, breath, and mind states before walking into room. Class discussions explored how to integrate informal practices into the workday and create the structure and consistency needed to develop and maintain new skillful responses to stress and adversity in the workplace. Brief didactics on mindfulness, resilience, and relevant research were presented weekly. The primary interventionist was a doctoral student in clinical psychology and had extensive experience facilitating mindfulness-based interventions (MBIs) training in primary care settings. MBWR was provided to the active control group only. Following the completion of the 3-month follow-up assessments, the WL control groups received the intervention.
Measures
Primary outcomes
Feasibility. Feasibility was assessed by number of participants recruited, percent of MBWR treatment completer, and attrition rate during the 8-week intervention. Recruitment of at least 80% of those screened and deemed eligible to participate was used to indicate feasibility. Similar to previous MBSR studies (Moss et al., Reference Moss, Reibel, Greeson, Thapar, Bubb, Salmon and Newberg2014), treatment completer was defined as attending at least five out of eight sessions. An attrition rate equivalent or smaller than those reported in past MBI studies with healthcare providers (20%) was used to indicate MBWR feasibility (Shapiro et al., Reference Shapiro, Astin, Bishop and Cordova2005).
Acceptability. Acceptability was measured by four items on a Likert-type scale (0–6): (1) How much did you enjoy this course? (2) How important was this course? (3) Would you recommend this course to colleague(s)? and (4) Would you participate in follow-up sessions?
Secondary outcomes: perceived effects
Qualitative measures
Focus groups were conducted one week after the MBWR training to assess perceived effects of MBWR. The facilitator of the MBWR sessions conducted the two focus groups, one for each team that participated in MBWR. Approximately 7–10 questions were asked in each group (Table 1). Mindful inquiry, recognized as a valid qualitative interview process (Bentz and Shapiro, Reference Bentz and Shapiro1998), was employed to understand the participants’ first-person perspectives on how they experienced the training and its effects. Inquiry is a process in which a facilitator engages participants in a collaborative and interactive verbal exploration of their experiences and observations. This interview approach permitted discussion and allowed for data to enter the interview that was not directly sought, thus allowing participants to provide information they believe was important and relevant to them. Audio recordings of the focus groups were transcribed verbatim. To reduce the threat of social desirability bias, prior to the focus groups, electronic anonymous surveys with the same open-ended questions asked during the focus groups were sent to participants (Nederhof, Reference Nederhof1985).
Table 1. Focus group questions

Quantitative measures: The following self-report outcome measures were collected at baseline, post, and 3-month follow-up assessment points.
The Brief Resilience Scale (Smith et al., Reference Smith, Dalen, Wiggins, Tooley, Christopher and Bernard2008) is a 6-item measure designed to assess the ability to bounce back or recover from stress. Higher scores indicate greater resilience. At baseline, the BRS demonstrated good internal consistency (α = 0.83).
The Five Facet Mindfulness Questionnaire-Short Form (Bohlmeijer et al., Reference Bohlmeijer, Peter, Fledderus, Veehof and Baer2011) is a 25-item measure of dispositional or trait mindfulness based on the 39-item Five Facet Mindfulness Questionnaire (Baer et al., Reference Baer, Smith, Hopkins, Krietemeyer and Toney2006). Higher scores for each facet indicate more of the trait. Due to previous reports of poor psychometrics, the Describing and Observing Facets were not assessed (Baer et al., Reference Baer, Smith, Lykins, Button, Krietemeyer, Sauer, Walsh, Duggan and Williams2008; Christopher et al., Reference Christopher, Woodrich and Tiernan2014). At baseline, the three facets of the FFMQ-SF (Acting with Awareness, Nonjudging of Inner Experience, and Nonreactivity to Inner Experience) demonstrated good-to-excellent internal consistency (α’s ranging from .75 to .91).
The Self-Compassion Scale-Short Form (SCS-SF) (Raes et al., Reference Raes, Pommier, Neff and van Gucht2011) is a 12-item measure that assesses three facets of self-compassion (self-kindness, mindfulness, common humanity) and their respective opposites (self-judgment, over-identification, isolation). Higher scores indicate greater self-compassion. At baseline, the SCS-SF demonstrated good internal consistency (α = .86).
Sample size
As this was a feasibility study, a sample size calculation was not conducted. Instead, we followed the recommendations of Julious (Reference Julious2005), who suggested a minimum sample size of 12 subjects per treatment arm.
Data analysis
Primary outcomes
Frequency reports analyzed feasibility and acceptability data and were performed using IBM SPSS version 22 (SPSS, Reference Spss2013).
Secondary outcomes
Qualitative
Prior to analysis, focus group transcripts were de-identified to ensure confidentiality and limit analytical bias among researchers. Qualitative data were analyzed using a conventional content analysis. This method systematically examines material and obtains a condensed description of content (Hsieh and Shannon, Reference Hsieh and Shannon2005). The first author independently reviewed the focus group transcripts in their entirety to get an overall sense of the data. Next, each transcript was individually re-read to identify recurring words, phrases, or concepts and the first author and a research associate independently developed preliminary codes (open coding). The two researchers discussed their independently developed codes, resolved differences, and devised a final coding scheme. The final coding scheme was then applied to both the transcripts by the two independent coders. Once all transcripts had been coded, the first author examined all data within a particular code. Codes were then sorted into categories based on how different codes are related and linked. These emergent categories were used to organize and group codes into meaningful cluster. Some codes were combined during this process, whereas others were split into subcategories. Definitions for categories were developed (Coffey and Atkinson, Reference Coffey and Atkinson1996, Hsieh and Shannon, Reference Hsieh and Shannon2005, Patton, Reference Patton2005). Transcripts were then reanalyzed to search for disconfirming data. A similar, yet independent, process was completed for the online surveys.
Quantitative
Means and standard deviation were calculated for each variable (resilience, mindfulness, and self-compassion) at the three time points. Analyses of between-group effects of mindfulness, resilience, and self-compassion were tested individually using a multilevel linear modeling (MLM) approach with restricted maximum likelihood estimation (REML), performed using IBM SPSS version 22 (SPSS, Reference Spss2013). Statistical significance for all parameter estimates were set at p < .05, two tailed. Effect sizes were calculated using Cohen’s d (Cohen, Reference Cohen1992).
Results
Preliminary analyses: feasibility and acceptability
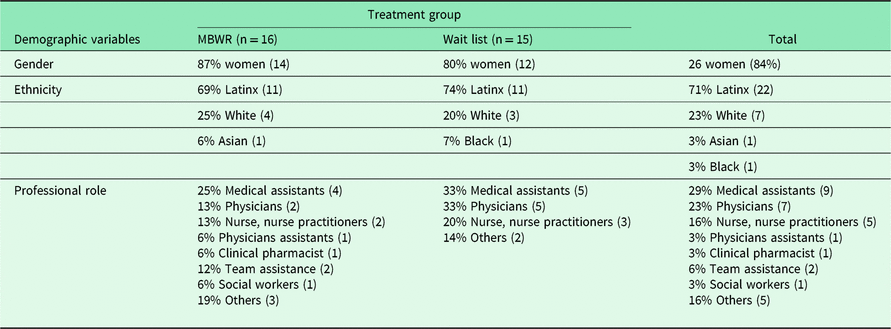
Of 45 primary care team members screened, six individuals did not meet study eligibility because they were unable to attend at least five of the eight classes. This was due to maternity leave (n = 1), scheduling conflicts due to clinical rotations (n = 4), or pending resignation (n = 1). One individual declined to participate due to a religious conflict with mindfulness meditation. Thirty-eight individuals enrolled in the study and completed baseline assessments (84%). Due to unexpected structural changes in the clinic, at the beginning of the study, seven participants (six medical assistants and one registered nurse) were required to switch teams. To reduce the threat of contamination, their data were removed. The eligible study sample numbered 31 participants. Two teams (n = 9, n = 7) completed MBWR and two teams were in a WL control (n = 7, n = 8). Of the 31 participants, 84% identified as female; 71% identified as Mexican, Latinx, or Puerto Rican, 20% as White, 6% as Asian, and 3% as Black. Medical assistants comprised 29% of the sample, primary care physicians comprised 23%, nurse or nurse practitioners 23%, team assistants 6%, physician’s assistants 3%, resident pharmacists 3%, social workers 3%, and other 10% (community resource officers, interns; see Table 2).
Table 2. Demographics and professional roles by group
All MBWR participants were completers (ie, attended at least five out of eight sessions) and total class attendance was 88%. Six participants attended all eight sessions, eight participants attended seven sessions, one participant attended six sessions, and two participants attended five sessions. Reasons for missing a class included being off-shift, attending an off-site training, or responding to a medical crisis or labor and delivery. Online surveys revealed participant ratings of the MBWR course: 87% of participants reported extremely or very much enjoying the course, 82% rated the course as extremely or very important, 100% would recommend the course to a colleague, 100% reported they would attend follow-up or booster sessions, and 100% reported the instructor was extremely or very knowledgeable.
Secondary outcome: perceived effects
Qualitative
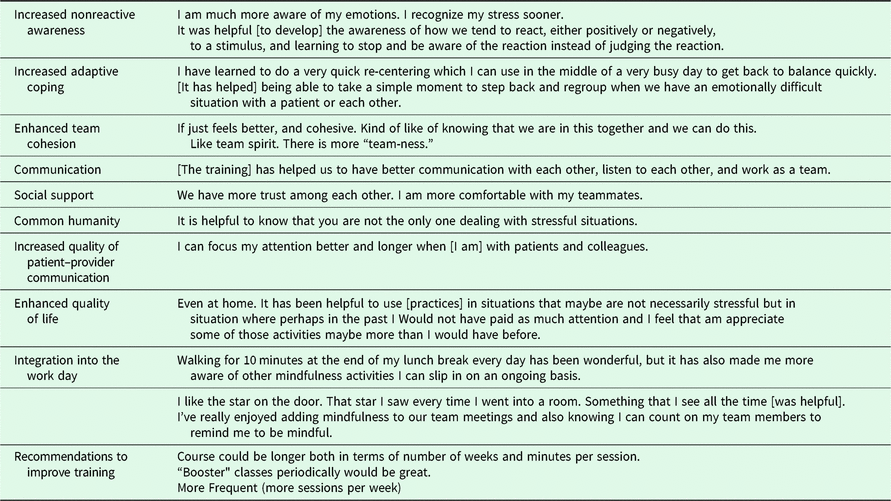
Analysis of the focus groups and open-ended survey questions from MBWR participants revealed seven themes: (1) increased nonreactive awareness, (2) improved adaptive coping, (3) enhanced team cohesion, (4) enhanced quality of patient–provider communication, (5) increased quality of life, (6) participants’ perceived importance of integrating informal mindfulness practices into the workday; and (7) participants’ recommendations for longer and more frequent sessions. Each of the themes and subthemes, with illustrative participant quotes, are displayed in Table 3.
Table 3. Final qualitative coding scheme
Quantitative
Due to the nature of the study and the small sample size, analyses focused on direction and magnitude of mean change from baseline to post-course in variables of resilience, mindfulness, and self-compassion, although results of significant tests are also provided (Table 4). To assess intervention effects, we estimated MLM separately for each outcome variable, using REML. Past meditation experience and expectancy of treatment effectiveness were included as covariates in the models. At baseline, there were significant differences between MBWR and WL in resilience (P = .006) and mindfulness non-reactivity of internal experience (P = .02). To account for these differences, for each of these dependent variables, the pre-MBWR variable was entered into the respective model as a covariate, and MLM analyses of co-variance were performed (Tabachnick and Fidell, Reference Tabachnick and Fidell2007).
Table 4. Means, standard deviations, and change in outcome variables for MBWR and wait-list control groups at baseline, post-MBWR, and 3-month follow-up
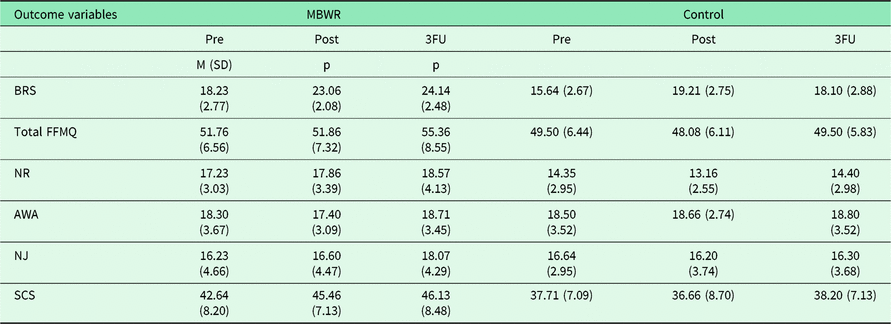
Note: 3FU = 3-month follow-up; BRS = Brief Resilience Scale; Total FFMQ = Three Facets (Act with Awareness, Non-Judgmental Awareness, and Nonreactivity) of Five Facets Mindfulness Questionnaire; NR = Nonreactivity of Inner Experiences Facet of FFMQ; AWA = Act with Awareness Facet of the FFMQ; NJ = Nonjudgmental Awareness Facet of the FFMQ; SCS = Self Compassion Scale – Short Form.
Discussion
MBWR was developed by the authors to be a brief, cost effective, evidenced-based, and replicable curriculum that is delivered onsite for IPCTs. MBWR is designed to assist hospitals, medical centers, and training institutions in promoting health, well-being, and community among staff, ultimately, enhancing the quality of care they provide. The primary aim of this study was to assess feasibility and acceptability of novel intervention, MBWR. All criteria for recruitment and retention were met and participants endorsed high levels of satisfaction and recommendations to colleagues. Results indicate that MBWR may be a feasible and acceptable method to integrate mindfulness and resilience into the primary care setting. This study offers several unique contributions to the literature. First, to our knowledge, this is the first study to examine a mindfulness-based intervention enriched with resilience that is delivered to IPCTs in the natural workday environment. Second, MBWR was implemented in a safety-net medical center, designed to reduce health disparities that disproportionately affect racial and ethnic minority groups, and poor and uninsured individuals. These centers report higher rates of burnout and turnover among healthcare workers than in non-safety-net center (Werner et al., Reference Werner, Goldman and Dudley2008). Further, MBWR participants reported increased quality of care, described as enhanced focus and less reactivity when interacting with patients. These preliminary findings suggest that MBWR training for providers may have secondary benefits for the marginalized communities they serve. Finally, 68% of the sample identify as Latinx, a population greatly underrepresented in the mindfulness and resilience literature. Results suggest that MBWR was feasible and acceptable for these participants of Latinx heritage.
The study also revealed a potential limitation of this delivery model, as seven participants were required to switch teams during the study, moving from the control group to the intervention group (or vice versa). This unforeseen reduction in sample size may have reduced the ability to see true differences between the groups. Researchers will need to engage in careful consideration and thoughtful planning when developing future studies using this delivery method in the primary care setting as to reduce threat of contamination.
Secondary objectives were to determine the perceived effects of MBWR among medical providers who attended the training. Qualitative analyses of focus groups and online survey were conducted to achieve this aim. Participants of MBWR described (1) enhanced self-awareness, (2) increased self-regulation skills, and (3) increased team cohesion, congruent with the three essential aims of resilience-promoting programs (Epstein and Krasner, Reference Epstein and Krasner2013). Existing literature suggests that to enhance resilience in the face of stressful work conditions, medical providers must be able to recognize when they are adversely affected by stress, cultivate skillful responses to the stressors, and self-regulate their cognitive, emotional, somatic, and behavioral reactions to the stressors (Shapiro et al., Reference Shapiro, Astin, Bishop and Cordova2005; Wolever et al., Reference Wolever, Bobinet, Mccabe, Mackenzie, Fekete, Kusnick and Baime2012; Epstein and Krasner, Reference Epstein and Krasner2013; Schroeder et al., Reference Schroeder, Stephens, Colgan, Hunsinger, Rubin and Christopher2016; Colgan et al., Reference Colgan, Klee, Memmott and Oken2018; West et al., Reference West, Dyrbye and Shanafelt2018). Following MBWR, participants reported increased awareness and non-reactivity of inner thoughts, emotions, and bodily sensations. Further, this increased awareness may have afforded an expanded behavioral repertoire and influenced participants’ reported increase in adaptive coping to stress or adverse conditions, permission and time devoted to personal growth.
The participants also described enhanced team cohesion and a greater sense of community, following the training. Three elements of team cohesion were revealed as improved communication, increased social support, and a greater sense of shared common humanity among teammates. This is a noteworthy finding because previous research has shown that members of highly cohesive teams are more likely to contribute equally to problem solving, are not as likely to be adversely affected by the power and status structures within the groups (Secord and Backman, Reference Secord and Backman1964), and contribute to increased provider satisfaction, which effectively predicts turnover (Lucas et al., Reference Lucas, Atwood and Hagaman1993; Tumulty et al., Reference Tumulty, Jernigan and Kohut1994; Leveck and Jones, Reference Leveck and Jones1996; Wells et al., Reference Wells, Roberts and Medlin2002) and reduces burnout among healthcare providers (Lasalvia et al., Reference Lasalvia, Bonetto, Bertani, Bissoli, Cristofalo, Marrella, Ceccato, Cremonese, de Rossi and Lazzarotto2009). Implementing MBWR in primary care teams may be an effective mechanism to facilitate enhanced community.
Additionally, MBWR participants emphasized the importance of integrating informal mindfulness practices into the workday. Fundamental to these efforts is the creation of a “container” of deliberate and consistent practice within which the culture of mindfulness can be cultivated and sustained. Humans become skilled at what they habitually do (Epstein, Reference Epstein2017); therefore, providing opportunities for IPCTs to train together and create tailored, authentic workflows that incorporate informal mindfulness practices may reduce sympathetic nervous system activation, improve emotion regulation, and enhance coping with psychological challenges (Hölzel et al., Reference Hölzel, Hoge, Greve, Gard, Creswell, Brown, Barrett, Schwartz, Vaitl and Lazar2013; Duchemin et al., Reference Duchemin, Steinberg, Marks, Vanover and Klatt2015; Westphal et al., Reference Westphal, Bingisser, Feng, Wall, Blakley, Bingisser and Kleim2015). Brief, yet frequent, informal mindfulness practices within this population may bolster individual mental immunity, as well as develop and sustain a culture of mindfulness-based resilience within the primary care work environment. The strong emphasis on informal practices may also reflect a greater sense of collectivism, congruent with the Latinx culture (García-Campayo et al., Reference García-Campayo, Demarzo, Shonin and van Gordon2017).
Focus groups and the online survey inquired about negative reactions or concerns regarding the training. The most frequent concern was the length: Participants requested that the training be longer (duration of training) and more frequent (more than one day a week). No other concerns or negative reactions were noted.
The results from this study must be interpreted with caution. Limited funding and the nature of the study design afforded several limitations. The small sample size reduced generalizability of the findings. Individual interviews were not conducted and the interventionist conducted the focus groups. As a result, social desirability bias may have influenced participants’ responses during the focus groups. Additionally, the interventionist was one of the researchers who analyzed the qualitative data. Further, group composition may have biased the findings. Future larger clinical trials are needed to explore the effects of MBWR on providers’ health, perceived burnout, patient–provider communication and relationship, while also exploring potential mechanisms of MBWR.
It is in healthcare institutions’ best interest to support the effort of all members of the workforce to enhance their capacity for resilience (Krasner et al., Reference Krasner, Epstein, Beckman, Suchman, Chapman, Mooney and Quill2009; Linzer et al., Reference Linzer, Levine, Meltzer, Poplau, Warde and West2014). The unique delivery model of MBWR, provided in the medical setting during paid-protected time and delivered to intact primary care teams, reflects the healthcare institution’s intention to support the workforce. The results of this study suggest that MBWR may assist in the cultivation and sustainability a thriving and flourishing primary care community and illustrate the potential benefits of an institutional commitment to provider well-being, that may offer at least a partial solution to the current crisis of physician burnout.
Author ORCIDs
Dana Dharmakaya Colgan 0000-0002-6806-1542
Acknowledgments
The authors would like to acknowledge all the medical providers for their time and dedication to this project and to their continued commitment to the communities they serve.
Financial Support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Conflicts of Interest
None.






