Suicide is a global public health problem. In 2000, according to the World Health Organization (WHO) approximately 1 million people worldwide died by suicide. Reference Krug, Dahlberg, Mercy, Zwi and Lozano1 Most of these suicides (86%) were in low- and middle-income countries (LMICs) and more than half were 15-44 years old. Reference Prince, Patel, Saxena, Maj, Maselko and Phillips2 These figures are likely to be an underestimate since suicide data from many LMICs are not reliable. In a verbal autopsy study from India, the suicide rates were found to be three times more than the official estimates. Reference Patel, Ramasundarahettige, Vijaykumar, Thakur, Gajalakshmi and Gururaj3 In Pakistan there are no reliable official data on suicide - it is an Islamic country where historically the rates of suicide have been low. Reference Bertolote and Fleischmann4,Reference Shah and Chandia5 The rates are not reliable because of the strong disapproval of suicide in Islam, social stigma, legal complications and police involvement, all of which encourage underreporting.
Both suicide and self-harm are illegal acts in Pakistan which are condemned religiously and socially; however, there is accumulating evidence that suicide rates have been gradually increasing over the past few years. Reference Khan and Prince6,Reference Syed and Khan7 The results reported by Syed & Khan Reference Syed and Khan7 indicate a strong association of suicide with depression and they conclude that absence of any effective healthcare system within the primary care setting is a huge challenge for prevention of suicide in Pakistan. Thus it is extremely important that effective treatments for patients who self-harm that can be widely utilised in clinical practice be identified. Reference Arensman, Townsend, Hawton, Bremner, Feldman and Goldney8
Prevention of suicide is included in health policy initiatives in several countries 9,Reference O'Connor, Gaynes, Burda, Soh and Whitlock10 and reduction in suicidal behaviour is part of the framework Public Health Action for the Prevention of Suicide. 11 It is recommended that suicide is recognised as a public health problem and national preventive programmes are developed. As recommended by the UK national strategy for suicide prevention, 9 one public health approach for the prevention of suicide includes identification of individuals who are at a high risk for suicide and providing them with appropriate treatment. Of the known risk factors for suicide, the most predictive of a future episode of self-harm or completed suicide is a history of self-harm. Reference Brown, Beck, Steer and Grisham12
In a report from Pakistan, self-harm was one of the most common causes of admission to a medical ward. Reference Memmon, Shafique, Afsar, Zuberi and Qadeer13 Of patients presenting to hospital with self-harm, up to 15% eventually kill themselves. Reference Nordentoft and Rubin14 It has been estimated that in the year following a self-harm episode, the risk of a repeat episode or completed suicide may be up to 100 times greater than that seen in people who have no history of self-harm. Reference Garland and Zigler15 Although there is a lack of conclusive findings among studies investigating the effects of interventions following self-harm, development of effective treatments is an important element in suicide prevention. In the West there are a number of different treatments being offered to patients after an episode of self-harm; as yet there are no guidelines for the management of self-harm in Pakistan.
Studies in many LMICs such as India, China and Pakistan suggest that risk factors associated with self-harm behaviour differ from those in high-income countries. A higher proportion of patients who self-harm (particularly women) have cited an interpersonal problem with family members as the main precipitant of the self-harm episode in studies in Karachi. Reference Syed and Khan7,Reference Zakiullah, Saleem, Sadiq, Sani, Shahpurwala and Shamim16 The psychosocial stressors, which precipitate self-harm, may be culturally and structurally influenced, but this should not exclude them from psychological help. Cognitive-behavioural therapy (CBT), Reference Brown, Thomas, Henriques, Xie, Hollander and Beck17 brief intervention and contact (BIC), Reference Vijayakumar, Umamaheswari, Shujaath Ali, Devaraj and Kesavan18 problem-solving therapies Reference Salkovskis, Atha and Storer19,Reference Hawton, Arensman, Townsend, Bremner, Feldman and Goldney20 and interpersonal psychotherapy Reference Guthrie, Kapur, Mackway-Jones, Chew-Graham, Moorey and Medel21 are of benefit to patients who self-harm, and could potentially be of help to this group. Problem-solving therapy has been identified in a recent National Institute for Health and Care Excellence (NICE) guideline as a promising intervention to prevent repeated self-harm. Reference Kendall, Taylor, Bhatti, Chan and Kapur22 Since most episodes of self-harm in Pakistan are precipitated by an interpersonal problem with family members, there is a strong rationale for investigating the efficacy of an intervention that addresses such issues. Where the interpersonal issues relate to unequal gender relations (e.g. domestic violence, controlling movement and/or aspirations of women), adaptations to therapeutic models will need to incorporate wider gender relations in their formulations. Consistent evidence has shown that people who self-harm have poor problem-solving skills. Reference Linehan, Camper, Chiles, Strosahl and Shearin23-Reference Pollock and Williams26 It is suggested that problem-solving deficits contribute to depression and hopelessness, which in turn increase both suicidal ideation and intent. Reference Schotte and Clum24,Reference D'Zurilla, Chang, Nottingham and Faccini27 Problem-solving therapy has been reported to be effective in reducing hopelessness and severity of depression in patients who self-harm. Reference Townsend, Hawton, Altman, Arensman, Gunnell and Hazell28 Thus a strong rationale exists for developing and testing a brief psychological intervention with problem-solving components following self-harm in a Pakistani population.
Our aim was to determine whether culturally adapted manual-assisted problem-solving therapy (C-MAP) results in decreased suicidal ideation, depression and hopelessness in patients with a history of self-harm compared with treatment as usual (TAU). Our primary hypothesis was that patients receiving C-MAP will show a greater reduction in suicidal ideation compared with the patients receiving TAU. The secondary hypotheses were that patients in the C-MAP group will show a greater reduction in measures of psychopathology, healthcare utilisation and an improvement in coping strategies used and in quality of life, compared with the TAU group.
Method
Setting
Karachi is one of the most populous cities in the world with a population of approximately 20 million. The city is divided into 18 towns.
Participants
Individuals invited for this study were all patients admitted after an episode of self-harm to the participating medical units of three university hospitals: Civil Hospital Karachi, Abbassi Shaheed Hospital, and Jinnah Hospital Karachi. The study period was from March 2010 to October 2012. Most of the patients belonged to the lower or lower-middle social class.
Inclusion criteria were:
-
(a) age 16-64 years
-
(b) living within the catchment area of the participating hospitals
-
(c) not requiring in-patient psychiatric treatment.
All consecutive patients meeting inclusion criteria were invited to take part in the study by the ward doctor, who assessed them at the time of admission. The research study was then explained in much more detail by one of the research assistants, who were not involved in their treatment. In the context of this study, self-harm was defined as:
‘an act with non-fatal outcome, in which an individual deliberately initiates a non-habitual behaviour that, without interventions from others, will cause self-harm, or deliberately ingests a substance in excess of the prescribed or generally recognised therapeutic dosage, and which is aimed at realizing changes which the subject desired via the actual or expected physical consequences’. Reference Schmidtke, Bille-Brahe, DeLeo, Kerkhof, Bjerke and Crepet29
Exclusion criteria were:
-
(a) temporary resident unlikely to be available for follow-up
-
(b) participants with a diagnosis of DSM-IV mental disorder due to general medical condition or substance misuse, dementia, delirium, alcohol and drug dependence, schizophrenia, bipolar disorder and intellectual disability.
Study design
The study was a randomised controlled assessor-masked clinical trial carried out in one centre over three sites (trial registration: ClinicalTrials.gov NCT01308151).
After the patient gave written informed consent having been offered oral and written information about the study, the research assistant referred to an allocation sequence which was provided by the off-site statistician (independent of the research team) and was based on a computer-generated list of random numbers, to allocate patients to the C-MAP plus TAU or TAU alone. Randomisation was performed using www.randomization.com. Participants meeting the entry criteria were randomly allocated to each condition in a 1:1 ratio using randomised permuted blocks of 6.
Patients were assessed at baseline and 3- and 6-month assessments were carried out for primary and secondary outcome measures and to establish timing of any self-harm. Baseline assessment included administration of a sociodemographic questionnaire. Research assistants, masked to treatment allocation, carried out a face-to-face interview with the participants at each time point. Participants were requested not to give any information about treatment. It was not possible to keep the clinicians at participating centres or the participants themselves masked to the group allocation.
Although it is essential that studies evaluating the efficacy of treatments for self-harm include repetition rates as the primary outcome measure, the low base rate of self-harm and completed suicide means that it is also critical that studies assess the effects of treatments on predictors of self-harm such as suicidal ideation, hopelessness and depression.
The study was approved by the ethics committees of Dow University of Health Sciences (ERB-86/DUHS-09) and the Pakistan Institute of Learning and Living (PILL-07-IRB/EC-05/09).
Trial interventions
Experimental treatment (C-MAP)
The intervention is a manual-assisted intervention which has been adapted from a self-help guide called Life After Self-Harm Reference Schmidt and Davidson30 based on the principles of CBT. Included in this intervention is an evaluation of the self-harm attempt, crisis skills, problem-solving and CBT techniques to manage emotions, negative thinking, interpersonal relationships and relapse prevention strategies. Reference Husain, Chaudhry, Durairaj, Chaudhry, Khan and Husain31 This was chosen as there is consistent evidence in the literature indicating that people who self-harm have poor problem-solving skills which can lead to hopelessness and depression. Reference Pollock and Williams26,Reference Townsend, Hawton, Altman, Arensman, Gunnell and Hazell28 A focus group of multidisciplinary mental health professionals initially translated the content of the manual into the Urdu language, giving special consideration to cultural adaptation of phrases and concepts to reflect Pakistani culture. Additionally, culturally appropriate case scenarios were incorporated and a consensual view to address cultural factors such as gender role, family conflicts and financial difficulties was taken. Issues related to substance misuse were replaced with more emphasis on family conflicts due to the low prevalence of substance misuse and the importance of family conflict.
C-MAP is a brief problem-focused therapy comprising six sessions within 3 months (Table 1). An engagement session was conducted prior to commencing the actual therapy. The aim is to help the participant in identifying and resolving interpersonal difficulties, which cause or exacerbate distress. The therapist delivered the intervention at the participant’s home/outpatient clinic depending on the participant’s choice. The first two sessions were offered weekly and then fortnightly, and lasted about 50 min each. The sessions were structured around the participant’s current problems, with the relevant sections of the manual helping the participant to deal with problems related to the self-harm episode. Participants were guided to use this structure and approach in future situations. Family involvement can be helpful and therefore family education and involvement was supported where appropriate and where participants were comfortable with this. As stated earlier, family conflicts are a common issue and therefore one session focused on the use of culturally sensitive training in assertiveness and conflict management. At each session the therapists assessed suicide risk and liaised with the treating doctor if concerned.
The intervention was delivered by qualified Masters-level psychologists, who had a minimum of 3 years’ post-qualification experience.
Training and fidelity. The therapists received training in fidelity to the model from F.N., N.C. and B.F. (who were involved in the adaptation of the intervention), who also offered subsequent regular supervision, and attendance often through internet video-conferencing at a weekly supervision group. The protocol adherence and treatment integrity was assessed using the revised Cognitive Therapy Scale (CTS-R). Reference Blackburn, James, Milne, Baker, Standart and Garland32
Cultural adaptation. Our group culturally adapted CBT for depression using mixed methods, in Pakistan, Reference Naeem, Ayub, Gobbi and Kingdon33 which was found to be effective in a preliminary study. Reference Naeem, Waheed, Gobbi, Ayub and Kingdon34 We used culturally acceptable idioms, local stories and images (e.g. to explain the concept of multiple perspectives) as well as examples from Islamic teachings. We incorporated simple strategies to improve engagement, which have worked in the past. These included speaking in simple language with a minimum number of English terms and establishing a good rapport and a trusting relationship during the session. We also involved the main carer, if the patient agreed to this. Patients often present with their families in Pakistan and family members like to be involved in therapy. One way to tackle this is to involve one of the family members and agree on boundaries.
Treatment as usual (TAU)
Local medical, psychiatric and primary care services provided standard routine care. Participants received an initial assessment along with TAU as ascertained by their treating doctor at the hospital or their primary care physician (general practitioner, GP). Patients are not routinely referred to psychiatric or psychology services. We obtained the details of any treatment received by each participant. Research psychologists delivering the intervention were not involved with the patients allocated to TAU.
C-MAP sessions details

| Description | Task | |
|---|---|---|
| Introduction | Introduction to therapy, information about self-harm, causes, examples of self-harm, understanding situation that caused self-harm, advantages and disadvantages of self-harm | Worksheets, understanding your self-harm attempt, people around you and advantages and disadvantages of self-harm |
| Dealing with crises | How to get help, keeping yourself safe, distraction techniques, relaxation, crisis plan | Worksheet, things to do, crisis plan |
| Problem-solving | Steps in problem-solving, religion and spirituality | Worksheets, making a list of problems, defining problems, choosing problems, dividing the solution in steps |
| Changing thoughts | Types of emotions, situations and mood, cognitive errors, thought records, challenging thoughts, changing thoughts | Worksheets, identifying the link between situations, thoughts and emotions, challenging thoughts, alternative thoughts |
| Family conflicts | Understanding and managing self-esteem, conflict resolution, assertiveness and confidence building | Worksheets, problem-solving, relaxation, ‘taking time out’, breaking social isolation and building social networks, managing negative thoughts |
| More thoughts | Review of what has been learned, crisis plan, long-term plans, accepting what cannot be changed, things to remember | Worksheet, learning from past experiences |
Sample size
We considered suicidal ideation as our primary outcome measure because it is a strong predictor of completed suicide. Reference Beck, Steer, Kovacs and Garisson35 We estimated a difference of 5 points on the Beck Scale for Suicide Ideation (BSI) to be clinically significant. Reference Beck, Kovacs and Weissman36 In the study by Guthrie et al, Reference Guthrie, Kapur, Mackway-Jones, Chew-Graham, Moorey and Medel21 the mean reduction in BSI from baseline to 6 months was 8.34 in the intervention group and 2.78 in the control group. The common standard deviation was 9.66. The difference between groups was significant (P<0.01) using baseline scores as covariate. A sample size of 49 in each group gave 80% power to detect a difference in means of 5.56 (the difference between intervention mean of 8.34 and control mean of 2.78), assuming that the common standard deviation is 9.66 and using a two-group t-test with a two-sided significance level of 0.05. Allowing for up to 50% drop-out rate, we calculated that we would need to recruit 100 participants in each group.
Primary outcome
Beck Scale for Suicide Ideation
The primary outcome was suicidal ideation as measured by the Beck Scale for Suicide Ideation (BSI). The BSI Reference Beck and Steer37,Reference Ayub38 is a 19-item self-report instrument for detecting and measuring the current intensity of the patient’s attitudes, behaviours and specificity of a patient’s thoughts to die by suicide during the past week. It is rated on a 3-point scale ranging from 0 to 2. Higher scores on the scale indicate greater suicidal intent and we considered a score of <6 to mean that a patient was no longer suicidal. The internal consistency coefficient for BSI is reported to be 0.96 and test-retest reliability 0.88. Reference Pinninti, Steer, Rissmiller, Nelson and Beck39 This scale has been previously used in Pakistan and the reported Cronbach’s alpha for the Urdu translation of the BSI is 0.75. Reference Ayub38 The Cronbach’s alpha in our study was 0.89.
Secondary outcomes
Beck Depression Inventory
Participants also completed the Beck Depression Inventory (BDI), Reference Beck, Ward, Mendelsohn, Mock and Erbaugh40 which is a 21-item scale measuring symptoms of depression. Higher scores on the scale indicate greater severity of depression. The average internal consistency estimates for the BDI are reported to be 0.86. Reference Beck, Ward, Mendelsohn, Mock and Erbaugh40 Wang et al Reference Wang, Andrade and Gorenstein41 reported good internal consistency (Cronbach’s alpha 0.82). There is also evidence for high 1-week test-retest reliability (r = 0.60) of the BDI. Reference Jo, Park, Jo, Ryu and Han42 The Cronbach alpha in our study was 0.96.
Beck Hopelessness Scale
The Beck Hopelessness Scale (BHS) Reference Beck and Steer43 is a self-report instrument designed to measure three aspects of hopelessness: feelings about the future, loss of motivation and expectations during the past week. Each of the 20 statements is scored 0 or 1. The scale also has good reliability (test-retest, r = 0.81). Reference Bouvard, Charles, Guérin, Aimard and Cottraux44 The BHS has been previously used in Pakistan and the reliability coefficient for the Urdu translation of this scale is reported as 0.81. Reference Ayub45 The Cronbach alpha in our study was 0.92.
Quality of Life
This was measured using EuroQoL (EQ-5D). Reference Brooks46 This is a standardised instrument to measure health-related quality of life. It consists of a self-report questionnaire covering five dimensions of health (mobility, self-care, usual activities, pain/discomfort and anxiety/depression).
Coping Resource Inventory
We used the Coping Resource Inventory (CRI) Reference Martin and Hammer47 to assess the coping resources available to the individual to manage stress.
Client Service Receipt Inventory
Participants were asked to give a detailed description of the use of health services (including the informal sector faith healers/Imams) at 3 months follow up. The Client Service Receipt Inventory (CSRI) Reference Beecham, Knapp, Thornicroft, Brewin and Wing48 has previously been used in Pakistan. Reference Chisholm, James, Sekar, Kumar, Murthy and Saeed49
Episodes of self-harm
Participants were interviewed to get a detailed description of further episodes of self-harm at 3- and 6-month follow-up. We used questions from the Suicide Attempt Self-Injury Interview (SASII), Reference Linehan, Comtois, Brown, Heard and Wagner50 which records self-harm events by severity and chronological order.
Translations
We selected all the above instruments carefully so as to avoid any problems in translation of difficult-to-translate concepts. The scales which were not available in the Urdu language were translated into Urdu based on our previous work. Reference Rahman, Iqbal, Waheed and Husain51
Statistical methods
Comparisons between the two groups were made on an intention-to-treat basis. Patients were included in the groups to which they were randomised regardless of how long or even whether they received the treatment allocated to them. All continuous variables (several on consulting use, and all the baseline questionnaire scores) were compared using t-tests, and categorical variables for consulting behaviour were compared using Fisher’s exact test. Questionnaire scores at 3- and 6-month follow-ups were compared using analysis of covariance to adjust for baseline scores and with multiple imputation of ten randomly generated imputed values per item of missing data, dependent on age, gender, group and baseline score of the same measure. The numbers of patients who were no longer suicidal, as defined by a BSI score <6, were compared using Fisher’s exact test.
Results
A total of 250 patients who had self-harmed were screened for inclusion into the study; 28 were excluded before baseline interviews were conducted, 1 refused immediately after baseline interview, and 221 were randomised (Fig. 1). Three patients in the C-MAP group dropped out of the study before receiving any intervention (two died and 1 had moved away), and one patient in the TAU group died before the 3-month follow-up (Fig. 1). A further three patients in the C-MAP group moved away and one patient in the TAU group died during the post-treatment period.
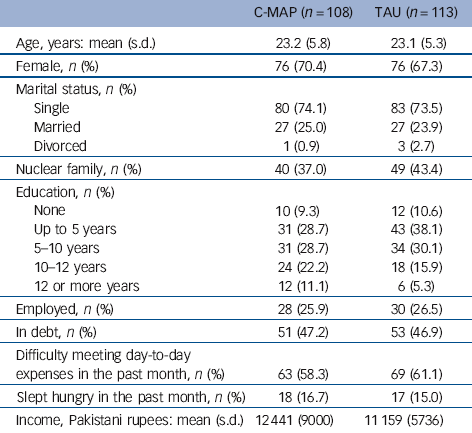
A total of 108 patients were randomised to the C-MAP group and 113 to the TAU group. Of the 221 participants, 152 (69%) were women, and the mean age was 23.1 years (s.d. = 5.5); 54 (24%) were married and 4 (2%) divorced; 89 (40%) were in a nuclear family and 132 (60%) in a joint family; 60 (27%) had received 10 years of schooling or more; and 58 (26%) were in employment (Table 2). Overall, 104 participants (47%) said they were in debt, 132 (60%) said they had difficulty meeting day-to-day expenses during the past month, and 35 (16%) said they had gone to sleep hungry at some point during the past month.
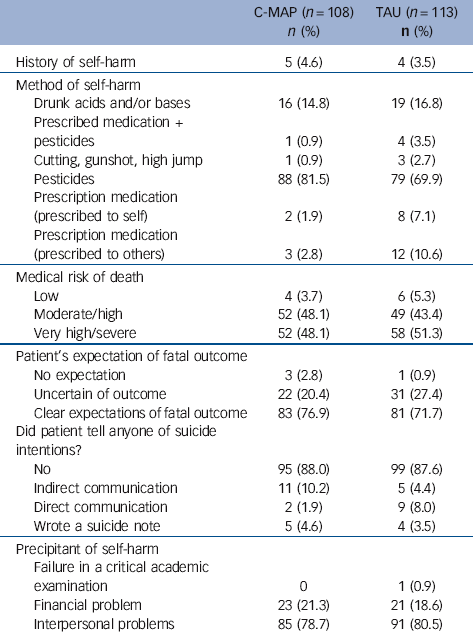
The most common method of self-harm was pesticides (n = 167, 76%), followed by drinking acids and/or bases (n = 35, 16%) and 15 participants (7%) had used prescription medication (prescribed either for self or others) (Table 3). The medical risk of death based on the method and other substances present at the time was classified as low for 10 participants (4%), moderate or high for 101 (46%) and very high or severe for 110 participants (50%). There was no expectation of a fatal outcome for 4 (2%), uncertain expectation for 53 (24%) and clear expectations of a fatal outcome for 164 (74%) participants. Sixteen participants (7%) made an indirect communication that they were thinking of suicide and 11 (5%) made a direct communication; 9 (4%) wrote a suicide note. Eighty per cent of participants cited interpersonal problems (n = 176), with 44 patients (20%) citing financial problems (Table 3).
Sociodemographic characteristics of patients by treatment group
| C-MAP (n = 108) | TAU (n = 113) | |
|---|---|---|
| Age, years: mean (s.d.) | 23.2 (5.8) | 23.1 (5.3) |
| Female, n (%) | 76 (70.4) | 76 (67.3) |
| Marital status, n (%) | ||
| Single | 80 (74.1) | 83 (73.5) |
| Married | 27 (25.0) | 27 (23.9) |
| Divorced | 1 (0.9) | 3 (2.7) |
| Nuclear family, n (%) | 40 (37.0) | 49 (43.4) |
| Education, n (%) | ||
| None | 10 (9.3) | 12 (10.6) |
| Up to 5 years | 31 (28.7) | 43 (38.1) |
| 5-10 years | 31 (28.7) | 34 (30.1) |
| 10-12 years | 24 (22.2) | 18 (15.9) |
| 12 or more years | 12 (11.1) | 6 (5.3) |
| Employed, n (%) | 28 (25.9) | 30 (26.5) |
| In debt, n (%) | 51 (47.2) | 53 (46.9) |
| Difficulty meeting day-to-day expenses in the past month, n (%) | 63 (58.3) | 69 (61.1) |
| Slept hungry in the past month, n (%) | 18 (16.7) | 17 (15.0) |
| Income, Pakistani rupees: mean (s.d.) | 12 441 (9000) | 11 159 (5736) |
C-MAP, culturally adapted manual-assisted problem-solving training; TAU, treatment as usual.
Flow diagram. C-MAP, culturally adapted manual-assisted problem-solving training.

Healthcare utilisation at 3-month follow-up
All participants had sought help for a physical problem and all had consulted a doctor, but very few patients had sought help for a mental health problem (Table 4). Significantly more of the TAU group had sought help from religious or spiritual healers such as an Immam, Molvi or Pir (35%) than the C-MAP group (21%), but there was no significant difference between the proportions who sought help from a homeopath (25% v. 18%). The TAU group had significantly more out-patient clinic attendances for physical illness and visits to a doctor other than the GP than the C-MAP group, but there were no significant differences between the groups on in-patient days (for physical or mental health), GP attendances (for physical or mental health) or for out-patient attendances for mental health (Table 4). A total of four participants in the C-MAP group and six participants in the TAU group were prescribed antidepressants during the 3 months after baseline assessment (end of intervention).
Symptom measures
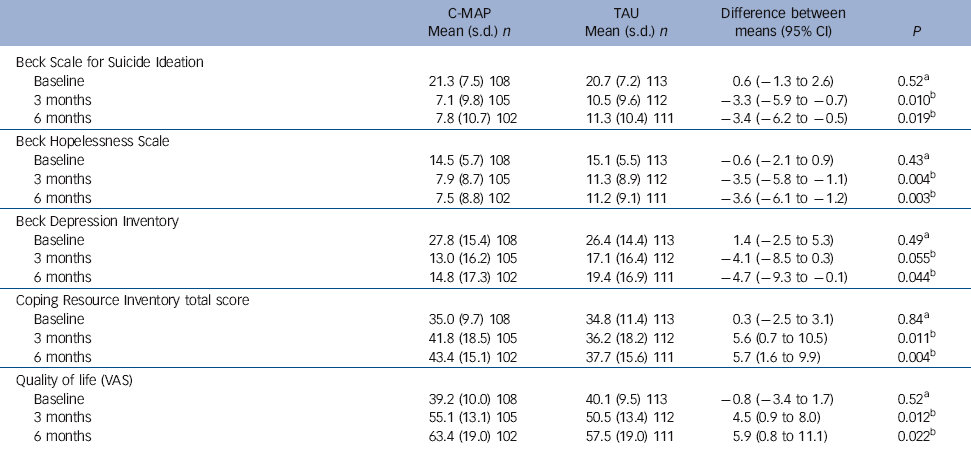
Participants in the C-MAP group showed significantly greater improvements from baseline than the TAU group on all measures at both 3 and 6 months, with the sole exception of the 3-month BDI scores, which just failed to reach statistical significance (P = 0.055) (Table 5). The effect sizes for the primary outcome measure, BSI, was 0.34 for the change from baseline to 3 months, and 0.32 for the change from baseline to 6 months.
There were a total of four completed suicides, two in each group. There were only two further episodes of self-harm, one in each group. Sixty-seven of the C-MAP group (62.0%) were no longer suicidal (BSI <6) at 3-month follow-up compared with 46 (40.7%) of the TAU group, Fisher’s exact P = 0.002. At 6 months, 66 patients (61.1%) in the C-MAP group and 49 patients (43.4%) in the TAU group were no longer suicidal (P = 0.010).
Number of sessions attended
More than half of the C-MAP group attended all 6 sessions (n = 56), 20 attended 5, 15 attended 4, 11 attended 3, and 3 attended 2 sessions. Improvements in all measures in Table 5 were positively correlated with the number of sessions attended. This was significant for hopelessness at 3 months (Spearman’s R = 0.22), suicidal ideation (R = 0.21), hopelessness (R = 0.26), CRI (R = 0.23) and quality of life (R = 0.35). A description of the sessions is given in Table 1.
Ancillary analyses
There were no significant differences between C-MAP and TAU for one of the three therapists in this study: one showed significant differences on all the measures (Table 5) and one showed significant differences for suicidal ideation and depression at 3 months only.
Self-harm characteristics of patients by treatment group
| C-MAP (n = 108) n (%) |
TAU (n = 113) n (%) |
|
|---|---|---|
| History of self-harm | 5 (4.6) | 4 (3.5) |
| Method of self-harm | ||
| Drunk acids and/or bases | 16 (14.8) | 19 (16.8) |
| Prescribed medication + pesticides | 1 (0.9) | 4 (3.5) |
| Cutting, gunshot, high jump | 1 (0.9) | 3 (2.7) |
| Pesticides | 88 (81.5) | 79 (69.9) |
| Prescription medication (prescribed to self) | 2 (1.9) | 8 (7.1) |
| Prescription medication (prescribed to others) | 3 (2.8) | 12 (10.6) |
| Medical risk of death | ||
| Low | 4 (3.7) | 6 (5.3) |
| Moderate/high | 52 (48.1) | 49 (43.4) |
| Very high/severe | 52 (48.1) | 58 (51.3) |
| Patient’s expectation of fatal outcome | ||
| No expectation | 3 (2.8) | 1 (0.9) |
| Uncertain of outcome | 22 (20.4) | 31 (27.4) |
| Clear expectations of fatal outcome | 83 (76.9) | 81 (71.7) |
| Did patient tell anyone of suicide intentions? | ||
| No | 95 (88.0) | 99 (87.6) |
| Indirect communication | 11 (10.2) | 5 (4.4) |
| Direct communication | 2 (1.9) | 9 (8.0) |
| Wrote a suicide note | 5 (4.6) | 4 (3.5) |
| Precipitant of self-harm | ||
| Failure in a critical academic examination | 0 | 1 (0.9) |
| Financial problem | 23 (21.3) | 21 (18.6) |
| Interpersonal problems | 85 (78.7) | 91 (80.5) |
C-MAP, culturally adapted manual-assisted problem-solving training; TAU, treatment as usual.
Discussion
The principal finding of this randomised controlled trial is that suicidal ideation was significantly reduced in patients randomised to C-MAP compared with patients receiving TAU. Patients receiving C-MAP also had a significant reduction in hopelessness and symptoms of depression.
Client Service Receipt Inventory: help-seeking behaviour in the previous 3 months, by treatment groupFootnote a

| C-MAP (n = 105) | TAU (n = 112) | ComparisonFootnote b | |
|---|---|---|---|
| Sought help for any physical health problem, n (%) | 105 (100) | 112 (100) | - |
| Sought help for any mental health problem, n (%) | 6 (5.7) | 8 (7.1) | Fisher’s P = 0.79 |
| In-patient days for physical health problem, mean (s.d.) | 4.9 (1.9) | 4.7 (1.8) | t = 0.8, P = 0.41 |
| In-patient days for mental health problem, mean (s.d.) | 0.05 (0.4) | 0.06 (0.4) | t = 0.3, P = 0.78 |
| Consulted any doctor, n (%) | 105 (100) | 112 (100) | - |
| Out-patient clinic attendances for physical illness, mean (s.d.) | 5.5 (4.9) | 6.9 (4.9) | t = 2.0, P = 0.045 |
| GP attendances for physical illness, mean (s.d.) | 2.1 (3.1) | 2.2 (3.6) | t = 0.1, P = 0.92 |
| Seen any other doctor for physical illness, mean (s.d.) | 0.17 (0.9) | 0.62 (1.6) | t = 2.5, P = 0.012 |
| Out-patient clinic attendances for psychological illness, mean (s.d.) | 0.07 (0.5) | 0.13 (1.0) | t = 0.6, P = 0.53 |
| GP attendances for psychological illness, mean (s.d.) | 0.05 (0.5) | 0.06 (0.4) | t = 0.2, P = 0.81 |
| Sought help from non-medical healers (Immam/Molvi/Pirs), n (%) | 22 (21.0) | 39 (34.8) | Fisher’s P = 0.024 |
| Sought help from non-medical healers (homeopathic), n (%) | 19 (18.1) | 28 (25.0) | Fisher’s P = 0.25 |
C-MAP, culturally adapted manual-assisted problem-solving training; GP, general practitioner; TAU, treatment as usual.
a. Measured at the end of the intervention (3 months).
b. Comparison made by t-test for continuous measures or Fisher’s exact test (FET) for dichotomous variables.
It is estimated that each year there may be up to 4000 cases of self-harm in the city of Karachi. Reference Shaid, Khan, Saleem Khan, Jamal, Badshah and Rehmani52 Because of sociocultural, legal and financial reasons, many patients after an episode of self-harm do not even make contact with health services, but patients who do present after an episode of self-harm are at an increased risk of repeating this behaviour. Reference Schmidtke, Bille-Brahe, DeLeo, Kerkhof, Bjerke and Crepet29,Reference Morgan and Hawton53 Our results suggest that 25% of patients had mild, 28% had moderate and 47% had severe depressive disorder as measured by the BDI. Patients with psychiatric disorders are at a higher risk of completed suicide, of which depressive disorder is the most common. Reference Khan, Mahmud, Karim, Zaman and Prince54-Reference Haw, Hawton, Houston and Townsend56 In a study from Karachi, Reference Khan, Mahmud, Karim, Zaman and Prince54 the majority of patients had a psychiatric disorder, predominantly depression, but only a very small number were receiving appropriate treatment. In our C-MAP group there was more than 50% reduction in moderate and severe depression at 3 and 6 months, an improvement rate similar to that observed in the depression trials. Reference Pilling, Anderson, Goldberg, Meader and Taylor57
The most common method of self-harm was poisoning by organophosphorous pesticides or corrosives (bases). This is similar to the report by Kinyanda et al. Reference Kinyanda, Hjelmeland and Musisi58 These substances have a high case-fatality ratio. In high-income countries the case-fatality ratio is 1-2%, whereas in LMICs it is 12-15%. Reference Vijaykumar and Rajkumar59 Khan et al, Reference Khan, Mahmud, Karim, Zaman and Prince54 in their study from Karachi, reported that for the majority of suicide victims it was their first attempt, showing the high case-fatality ratio. More than 90% of patients used poisonous/lethal substances which included organophosphate compounds, washing liquids and household bleach. Therefore a useful approach may be reducing access to such potentially lethal methods of self-harm. Among our sample there was only one person who had used alcohol on the day of self-harm. Only 24% of patients were married, which is quite different from earlier reports where most of the patients were married. Reference Shahid and Hyder60 The low number of patients with a history of self-harm in our study is similar to India, Reference Vijaykumar and Rajkumar59 China Reference Phillips, Yang, Zhang, Wang, Ji and Zhou61 and Sri Lanka. Reference Eddleston, Sheriff and Hawton62
More than 60% of patients in the C-MAP group reporting suicidal ideation were no longer suicidal at 3 and 6 months, compared with only 44% or less for the TAU group. This improvement rate is not very different to that observed in more intensive interventions in the West. Reference Szanto, Mulsant, Houck, Dew and Reynolds63 The C-MAP focused on interpersonal problems, which are an important precipitant of self-harm in Pakistan Reference Shahid and Hyder60 and on problem-solving skills, which are reported to be impaired in patients who present after self-harm. Reference Pollock and Williams26,Reference Townsend, Hawton, Altman, Arensman, Gunnell and Hazell28
Limitations
We did not control for the non-specific effects of the psychological intervention in this trial and the effects of C-MAP may have resulted from nonspecific factors, such as increased contact with psychologists. However, many studies in the West that have involved a similar intensity of clinical contact did not show a significant improvement on several of the outcomes, Reference Morthorst, Krogh, Erlangsen, Alberdi and Nordentoft64,Reference Morthorst, Krogh, Erlangsen, Alberdi and Nordentoft64 although some CBT-based interventions have been reported to be superior to routine care. Reference Brown, Thomas, Henriques, Xie, Hollander and Beck17 A further limitation concerns treatment integrity - there is a therapist effect in our findings which needs to be investigated further. In this trial we did not use audio/video tapes of therapy sessions and we think this could have helped us to better ensure the integrity of the treatment.
Mean scores for symptom measures at baseline, 3 and 6 months, by treatment group
| C-MAP Mean (s.d.) n |
TAU Mean (s.d.) n |
Difference between means (95% CI) |
P | |
|---|---|---|---|---|
| Beck Scale for Suicide Ideation | ||||
| Baseline | 21.3 (7.5) 108 | 20.7 (7.2) 113 | 0.6 (−1.3 to 2.6) | 0.52Footnote a |
| 3 months | 7.1 (9.8) 105 | 10.5 (9.6) 112 | −3.3 (−5.9 to −0.7) | 0.010Footnote b |
| 6 months | 7.8 (10.7) 102 | 11.3 (10.4) 111 | −3.4 (−6.2 to −0.5) | 0.019Footnote b |
| Beck Hopelessness Scale | ||||
| Baseline | 14.5 (5.7) 108 | 15.1 (5.5) 113 | −0.6 (−2.1 to 0.9) | 0.43Footnote a |
| 3 months | 7.9 (8.7) 105 | 11.3 (8.9) 112 | −3.5 (−5.8 to −1.1) | 0.004Footnote b |
| 6 months | 7.5 (8.8) 102 | 11.2 (9.1) 111 | −3.6 (−6.1 to −1.2) | 0.003Footnote b |
| Beck Depression Inventory | ||||
| Baseline | 27.8 (15.4) 108 | 26.4 (14.4) 113 | 1.4 (−2.5 to 5.3) | 0.49Footnote a |
| 3 months | 13.0 (16.2) 105 | 17.1 (16.4) 112 | −4.1 (−8.5 to 0.3) | 0.055Footnote b |
| 6 months | 14.8 (17.3) 102 | 19.4 (16.9) 111 | −4.7 (−9.3 to −0.1) | 0.044Footnote b |
| Coping Resource Inventory total score | ||||
| Baseline | 35.0 (9.7) 108 | 34.8 (11.4) 113 | 0.3 (−2.5 to 3.1) | 0.84Footnote a |
| 3 months | 41.8 (18.5) 105 | 36.2 (18.2) 112 | 5.6 (0.7 to 10.5) | 0.011Footnote b |
| 6 months | 43.4 (15.1) 102 | 37.7 (15.6) 111 | 5.7 (1.6 to 9.9) | 0.004Footnote b |
| Quality of life (VAS) | ||||
| Baseline | 39.2 (10.0) 108 | 40.1 (9.5) 113 | −0.8 (−3.4 to 1.7) | 0.52Footnote a |
| 3 months | 55.1 (13.1) 105 | 50.5 (13.4) 112 | 4.5 (0.9 to 8.0) | 0.012Footnote b |
| 6 months | 63.4 (19.0) 102 | 57.5 (19.0) 111 | 5.9 (0.8 to 11.1) | 0.022Footnote b |
C-MAP, culturally adapted manual-assisted problem-solving training; TAU, treatment as usual.
a. Comparison made by t-test at baseline.
b. Comparison made by analysis of covariance at 3 and 6-month follow-ups with baseline score as covariate, and with multiple imputation of 10 randomly generated imputed values per item of missing data, dependent on age, gender, group and baseline score of the same measure.
As part of the WHO Multisite Intervention Study on Suicidal Behaviours (SUPRE-MISS), Reference Fleischmann, Bertolote, Wasserman, De Leo, Bolhari and Botega66 Vijayakumar and colleagues Reference Vijayakumar, Umamaheswari, Shujaath Ali, Devaraj and Kesavan18 reported the effectiveness of BIC in a very large sample of individuals presenting to a general hospital after a suicide attempt in India. The results show that a low-cost intervention significantly reduced completed suicide and further suicide attempts compared with TAU. It is difficult to compare our findings with those of Vijayakumar et al, Reference Vijayakumar, Umamaheswari, Shujaath Ali, Devaraj and Kesavan18 considering that C-MAP is a brief psychological intervention based on the principles of CBT delivered over a period of 3 months, whereas BIC consists of an information session with regular follow-up contacts up to 18 months after discharge from the hospital. During our follow-up contact sessions, participants were asked whether they needed any support and appropriate referrals were made accordingly.
As we only recruited participants who were admitted to medical wards after an episode of self-harm, this may have resulted in the exclusion of individuals who may be at a higher risk of self-harm or completed suicide in the future who either did not present to hospital or who discharged themselves before any assessment or treatment. It has been suggested that the majority of patients in Pakistan leave the healthcare setting against medical advice and without psychiatric assessment because of stigma, fear of involvement of the police, confidentiality and sometimes financial reasons. Reference Khan, Mahmud, Karim, Zaman and Prince54 Up until recently the law in Pakistan required each case of self-harm to be taken to a government healthcare facility designated as medico-legal centres, where a case would be registered against the individual by the police. Harassment and extortion from the victim and the family is still common and as a result self-harm attracts sociocultural sanctions and involves a lot of secrecy. It can even affect the marriage prospects of a girl, and even other girls in her family. Reference Kebede and Alem67 There are also very strong religious sanctions against such behaviour. Despite all of these factors, there are reports of increasing rates of both self-harm and completed suicide. Reference Khan and Prince6
Most of the eligible participants agreed to participate. This finding is very different from previous reports Reference Guthrie, Kapur, Mackway-Jones, Chew-Graham, Moorey and Medel21,Reference Morthorst, Krogh, Erlangsen, Alberdi and Nordentoft64,Reference van der Sande, van Rooijen, Buskens, Allart, Hawton and van der Graaf65 and shows the potential of engaging patients in intervention studies in LMICSs where access to healthcare, particularly mental healthcare, is low. Participants in this trial had quite a high level of psychiatric morbidity compared with other patients who self-harm. Reference Morthorst, Krogh, Erlangsen, Alberdi and Nordentoft64,Reference Mann, Apter, Bertolote, Beautrais, Currier and Haas68 Our results may therefore not be generalisable to other patients who self-harm but may have less severe mental health difficulties. Similarly, caution is warranted in extrapolating these results to other LMICs and even other parts of Pakistan, especially rural areas. The patients were from public-sector teaching hospitals and the results may not be generalisable to other groups. Data regarding further episodes of self-harm are based on reports from the patients themselves and therefore should be interpreted with caution.
Clinical implications
Additional studies are required to examine the effectiveness and cost-effectiveness of C-MAP in both hospital and primary care settings. Individuals who present to health services after an episode of self-harm offer a unique opportunity for prevention, as individuals who have attempted suicide are often quite receptive to interventions. Reference Forster and Bilsker69 In patients with low income with a recent history of self-harm and who were admitted to a medical ward, we have shown that suicidal ideation, depression and hopelessness can be significantly reduced after a brief psychological intervention. The positive effects of C-MAP in a low-resourced healthcare system are promising.
There is a potential for only limited impact of the findings of this study on patients presenting after self-harm, their carers, allied health professionals, academics and health services in Pakistan. The primary objective of this study was to show in an exploratory trial that a brief psychological intervention can bring about a reduction in self-harm morbidity and an improvement in health-related quality of life. In LMICs there is a huge treatment gap and up to nine out of ten people with mental health difficulties do not receive appropriate treatment. The preliminary results from this study offer a foundation to build on and may aid the translation of the findings into action in the participating hospitals. The WHO’s Mental Health Gap Action Programme (mhGAP) 70 for LMICs advocates delivery of evidence-based interventions to manage a number of priority conditions including suicide and self-harm. The guidelines suggest to focus on the person’s positive strengths by getting them to talk of how earlier problems have been resolved, to offer and activate psychosocial support and consider problem-solving therapy for treating people with acts of self-harm in the past year. Our current work contributes to the WHO’s vision to deliver interventions for self-harm in LMICs.
Funding
This study was jointly funded by the University of Manchester and Pakistan Institute of Learning and Living. The sponsor of the study had no role in the study design, data collection, analysis of the data, data interpretation or writing of the manuscript.
Acknowledgements
We thank all the participants and all the clinicians of the participating medical units. We are thankful to authors Ulrike Schmidt and Kate Davidson for allowing us to translate and culturally adapt their manual Life after Self-Harm a Guide to the Future. We are grateful to Professor M.M. Khan for his comments on the earlier draft of the manuscript.








eLetters
No eLetters have been published for this article.