Background
Suicide is a major public health issue and the second leading cause of death for young people worldwide (WHO, 2014). In the United Kingdom, 3156 young people aged 15–29 died by suicide between 2011 and 2013 (Samaritans, Reference Sudak, Roy, Sudak, Lipschitz, Maltsberger and Hendin2015). As well as the obvious emotional impact on families and others affected, the economic impact is profound with the average cost per completed suicide in England reaching £1.67 m (Knapp et al., Reference Knapp, MCDaid and Parsonage2011). Youth suicide holds the highest economic burden due to the longest years of lost earnings (Kennelly, Reference Kennelly2007).
Youth suicide prevention is a global public health target (WHO, 2014). Improved management through early identification and assessment of those at risk has been highlighted in the national strategy for the prevention of suicide in England [Department of Health (DoH), 2014]. Competence in assessing and managing young suicidal people, knowledge about youth suicide, and attitudes towards vulnerable young people are likely to influence clinical practice (Saunders et al., Reference Taylor, Hawton, Fortune and Kapur2012) as well as patients’ experience of service provision (Taylor et al., Reference O’Connor, Gaynes, Burda, Soh and Whitlock2009) and therapeutic engagement (Thompson et al., Reference Pit, Vo and Pyakurel2008). A systematic review (Taylor et al., Reference O’Connor, Gaynes, Burda, Soh and Whitlock2009) of attitudes towards clinical services among people who self-harm, including adolescents, showed that staff knowledge, communication, attitudes and better after-care arrangements could increase service user satisfaction and treatment adherence.
There is extensive research investigating the attitudes, knowledge, and competence of clinical staff, including those in emergency departments, paediatric wards and Child and Adolescent Mental Health Services (CAMHS) towards young people who self-harm and/or are at risk of suicide (Crawford et al., Reference Cleaver2003; Anderson and Standen, Reference Appleby, Morriss, Gask, Roland, Perry, Lewis, Battersby, Colbert, Green, Amos, Davies and Faragher2007; Cleaver, Reference Crawford, Geraghtyb, Streetb and Simonoffa2014). However, we know very little about the competence, knowledge, and attitudes of primary care health staff, and particularly general practitioners (GPs), towards suicidal young people with the exception of one study (Fox et al., Reference Fox, Stallard and Cooney2015). This is surprising considering that GPs are often the first point of contact for people in distress (Goldberg and Huxley, Reference Goldberg and Huxley1992) and young people are more likely to seek professional help from a GP when it comes to mental health problems (Rickwood et al., Reference Roberts, Crosland and Fulton2007). Evidence also shows increased contact with GPs by those completing suicide, including young adults, one to three months before their death (Appleby et al., 1996; Luoma et al., Reference Luoma, Martin and Pearson2002). A qualitative study we conducted recently, exploring GPs’ experiences of assessing, communicating with and managing suicidal young people (Michail and Tait, Reference Michail and Tait2016), revealed significant gaps in GPs’ specific knowledge and clinical skills required for the assessment and management of suicide risk in young people. In addition, GPs’ reported perceptions of young people as impulsive, unpredictable and difficult to communicate with, confirmed the findings of previous studies (Illiffe et al., Reference Illiffe, Williams, Fernandez, Vila, Kramer, Gledhill and Miller2008; Roberts et al., Reference Saini, Windfuhr, Pearson, Da Cruz, Miles, Cordingley, While, Swinson, Williams, Shaw, Appleby and Kapur2013) and raise questions about the potential influence of these views on GPs’ diagnostic skills relevant to the care of vulnerable young people.
The aim of this study was to conduct a cross-sectional survey to assess GPs’ level of confidence on aspects of care and management of young people at risk of suicide; knowledge of risk factors and warning signs of suicide in young people; attitudes towards young people at risk of suicide and preferences towards different modes of receiving further training on managing young people at risk of suicide. We were particularly interested in determining whether length of experience as a GP or recent mental health update training was associated with perceived confidence in the assessment and management of suicide risk in young people; levels of knowledge of suicide risk factors and warning signs; and attitudes towards young people at risk of suicide.
This study is part of a larger study examining GPs’ clinical expertise in assessing, communicating with, and managing suicidal young people aged 14–25 that would inform the development of an educational intervention for GPs on youth suicide prevention (Michail and Tait, Reference Michail and Tait2016).
Method
Study design
A survey was designed by the authors and conducted with GPs in Nottingham City as part of a larger study on youth suicide prevention in primary care (Michail and Tait, Reference Michail and Tait2016). The study received ethical approval by NRES Committee West Midlands – Coventry & Warwickshire (14/WM/1100).
Development and piloting of survey
A structured, self-administered survey comprising four sections (confidence about skills; knowledge of published guidelines in suicide prevention, risk factors of suicide in young people, and warning signs of suicide in young people; attitudes towards young people at risk of suicide; and preferred training method) was developed following the principles of questionnaire development (Fink and Kosecoff, Reference Fink and Kosecoff1985). These included a literature review, conceptual refinement, item generation, content and face validation. Following an extensive literature review, an initial pool of items was generated: 7 for the confidence section; 1 for knowledge of published guidelines; 13 for knowledge of risk factors; 10 for knowledge of warning signs; 7 for attitudes; and 7 for preferred training method. A further question about GPs’ level of interest in learning more about caring for young people at risk of suicide was included. An expert panel led by D.C. (academic GP with expertise in youth mental health) reviewed the survey questions to assess how well each item measured the construct in question. Feedback was provided as to which questions should be excluded; which should be added, and which questions should be re-phrased and clarified. Following an iterative process of revision and review, the survey was amended to include the following sections (Supplementary material):
-
1. Confidence about skills (7 items)
-
2. Knowledge: (a) published guidelines (1 item), (b) risk factors of suicide in young people (15 items), (c) warning signs of suicide in young people (15 items)
-
3. Attitudes towards young people at risk of suicide (7 items)
-
4. Preferred training method (7 different types of training)
The question about GPs’ level of interest in learning more about caring for young people at risk of suicide remained and space for free text was added where respondents could include comments or feedback. Sections 1 (confidence) and 3 (attitudes) were rated using a Likert scale ranging from 1 (strongly disagree) to 5 (strongly agree). Items in section 2 (knowledge) were rated as true (=1) or false (=0). In section 4 (preferred training method), respondents were asked to rank on a scale of 1 (most preferred) to 7 (least preferred) which of seven different training methods on youth mental health and suicide they were likely to access.
The survey was subsequently piloted with a convenience sample of 10 GPs to assess face validity. D.C. led this exercise and selected the pilot group taking into consideration age group, gender, and years of professional experience. Verbal consent was obtained for participation in the pilot. As a result of the pilot exercise, further feedback was obtained and revisions were made to the survey as appropriate.
Sample and data collection
All GPs (~300) from 62 general practices in Nottingham City were invited to participate in the survey. The survey took 10 min to complete and was anonymous. It was available both online (Survey Monkey) and in hard copy format for completion during lunchtime practice meetings or Clinical Commissioning Group (CCG)Footnote 1 Board meetings. The study team initially approached the four GP cluster leads in Nottingham City CCG to facilitate recruitment. An email including a link to the online survey was sent by the GP cluster leadsFootnote 2 to all GPs in Nottingham City practices informing them about the study and encouraging them to complete the survey. Recruitment was also facilitated by the Clinical Research Network (CRN): East Midlands.
Data analysis
The Statistical Package for the Social Sciences (SPSS) version 22 was used to perform all statistical analyses. Due to the ordinal nature of the data, non-parametric analyses were carried out. Descriptive statistics were reported including frequencies and mean ranks. Differences in levels of confidence, knowledge and attitudes between (i) experienced (>10 years of professional experience) versus less experienced GPs (<10 years of professional experience) and (ii) GPs who had recently (past five years) received update mental health training versus those who had not, were analysed using Mann–Whitney U test; χ2 tests were used to analyse categorical data. A 5% statistical significance level was used.
The total number of correct (eg, rated as True when the statement was True) and incorrect (eg, rated as True when the statement was False) item responses in the knowledge scale were calculated for each participant by summing individual item responses. Similarly, in the attitudes scale individual scores were summed to obtain a total score for each participant, with higher scores indicating more negative attitudes.
Results
The sample
The demographic characteristics of the sample are presented in Table 1. A total of 70 (23.3%) GPs completed the survey, 30 of whom were males. The median number of years of professional experience was 25.5 years. The majority of GPs (82.9%) reported that they had not attended or undertaken any specific mental health training in the past five years.
Demographic characteristics of sample

a Median.
Perceived confidence about skills
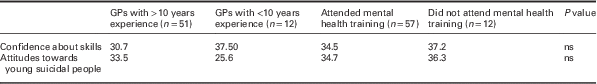
GPs were asked to rate their perceived confidence in the assessment and management of suicide risk in young people. The majority of GPs reported feeling confident in diagnosing depression in young people (70.4%) and in asking young patients about suicidal thoughts (62%). In all, 44% of GPs felt confident in clinically managing young people at risk of suicide. With regards to discussing strategies with young patients for coping with future suicidal thoughts, 39.5% of GPs compared with 17% reported feeling confident to do so; 35% of GPs replied by neither agreeing nor disagreeing with the statement. A similar response pattern was noted when GPs were asked to rate their confidence in screening for suicide risk factors; 44% of GPs, compared with 13%, felt confident doing so; however, a relatively high number of GPs (37%) responded to the statement by neither agreeing nor disagreeing. The majority of GPs (59%) were also ambivalent (ie, neither agreed nor disagreed with the statement) about their confidence in effectively preventing youth suicide. With regards to GPs’ confidence in using suicide risk screening tools with at risk young people, 35% disagreed and 41% neither agreed nor disagreed with the statement. Mann–Whitney U test was used to examine differences in levels of perceived confidence between (i) experienced versus less experienced GPs and (ii) GPs who had attended or undertaken mental health training in the past five years versus those who had not. The test revealed no significant differences between those groups (Table 2). GPs with more than 10 years of experience did not report higher levels of confidence in assessing and managing suicide risk in young people compared with those with <10 years of experience (U=240, P=0.24). Similarly, GPs who had received mental health training in the past five years did not report higher levels of confidence in their skills compared to those who had not received mental health training recently (U=316, P=0.67).
Mean rank of GPs’ confidence about skills and attitudes towards at-risk young people
Knowledge
-
(1) Published guidelines on suicide prevention
Of the 69 GPs who responded to this question, 59.4% were not aware of any published guidelines (local, national, or international) on suicide prevention. There was no association between knowledge of published guidelines on suicide prevention and experience. Experienced GPs were not more aware of published guidelines on suicide prevention compared with less experienced GPs (x 2 =0.05, df=1, P=0.81). There was also no association between knowledge of published guidelines on suicide prevention and mental health training status. GPs who had attended or undertaken mental health training in the past five years were not more aware of published guidelines on suicide prevention compared with those who had not (x 2=3.23, df=1, P=0.07).
-
(2) Suicide risk factors in young people
Out of a total of 1035 item responses, GPs correctly identified either as true or false statements 733 items (70.8%), compared with 302 (29.2%), which were incorrectly identified. The data for correct and incorrect responses for (a) experienced versus less experienced GPs and (b) GPs who had attended or undertaken mental health training in the past five years versus those who had not are presented in Table 3. There was an association between level of knowledge and experience, with experienced GPs identifying a significantly higher number of correct responses and a significantly lower number of incorrect responses compared with less experienced GPs (x 2=3.99, df=1, P<0.05). There was no association between level of knowledge and mental health training status. GPs who had attended or undertaken mental health training in the past five years did not identify a higher number of correct responses compared to those who had not (x 2=0.41, df=1, P=0.52).
-
(3) Warning signs of suicide in young people
GP correct and incorrect response on knowledge section

Of the 70 GPs, 69 completed this section, giving a total of 1035 item responses. In all, 524 (n=524) items (50.6%), compared with 511 (49.4%), were correctly identified by GPs either as true or false statements. The data for correct and incorrect responses for (a) experienced versus less experienced GPs and (b) GPs who had attended or undertaken mental health training in the past five years versus those who had not are presented in Table 3. There was no association between level of knowledge and experience. Experienced GPs did not identify a significantly higher number of correct responses compared to less experienced GPs (x 2=0.85, df=1, P=0.35). There was also no association between level of knowledge and mental health training status. GPs who had attended or undertaken mental health training in the past five years did not identify a higher number of correct responses compared with those who had not attended or undertaken mental health training in the past five years (x 2=0.03, df=1, P=0.85).
Attitudes towards young people at risk of suicide
GPs’ views about whether patients who self-harm are a tremendous burden to a GP were split, with 38% reporting being unsure about the statement; 29% disagreeing and 18% agreeing. GPs’ views on whether patients at risk of suicide are frustrating to manage were also split, with 35% disagreeing; 31% agreeing and 22.5% reporting being unsure; 42% of GPs, compared with 24%, agreed that young patients are harder to communicate with than adult patients; 48% compared with 17%, disagreed that maintaining compassionate care is difficult with patients who deliberately self-harm. Views about whether young people who deliberately self-harm are at high risk of suicide were split, with 35% of GPs disagreeing with the statement; 30% agreeing and 28% being unsure. Opinions about whether routine screening for suicide risk factors or suicidality can be effective in preventing suicide behaviour in young people were also split, with 42% reporting being unsure and 41% agreeing. Totally, 81% of GPs, compared with 1.4%, disagreed with the statement that asking about suicide might increase the likelihood of a young patient attempting suicide. Mann–Whitney U test revealed no significant differences in relation to GP length of experience and recent mental health training (Table 2). GPs with more than 10 years of experience did not differ in their attitudes towards young people at risk of suicide from those with <10 years of experience (U=229.5, P=0.17). Similarly, GPs who had received mental health training in the past five years did not differ in their attitudes towards young people at risk of suicide from to those who had not received mental health training recently (U=326, P=0.79).
Preferred training method
GPs were asked to identify their preferred method of training delivery: short courses; shadowing/learning from others; workshops; online/e-learning and web-based resources; on-site training; user guide/written workbook; video. A total of 56 GPs (80%) responded to this question. The three most preferred options were short courses (28.6%); workshops and online/e-learning (26.8%); and on-site training (16%).
Discussion
This is the first study to assess GPs’ level of confidence on aspects of care and management of young people at risk of suicide; knowledge of suicide risk factors and warning signs in young people as well as attitudes towards young people at risk of suicide. It sampled from 62 inner-city general practices and compared experienced and less experienced GPs.
The majority of GPs reported feeling confident in their abilities and skills in assessing and managing suicidality in young people, including diagnosing depression, asking about suicidal thoughts and discussing strategies for coping with those thoughts. Years of experience and previous mental health training did not seem to play a role in GPs’ levels of perceived confidence. There was, however, uncertainty among GPs whether their diagnostic skills did or could effectively help in preventing suicide in young people. This finding of uncertainty is in line with the findings of a recent qualitative study by Michail and Tait (Reference Michail and Tait2016) where GPs reported confidence in dealing with general mental health problems but felt ill-equipped to effectively manage and potentially prevent suicide attempts and suicides in vulnerable young people. It is worth highlighting that 62% of GPs reported feeling confident in asking young patients about suicidal thoughts and 81% did not believe that asking about suicide might inadvertently increase suicidal ideation. Evidence in the literature about GPs’ confidence in screening for suicidal ideation and concerns about the possibility of this inducing suicidal ideation is mixed. In some studies (Bajaj et al., Reference Bajaj, Borreani, Ghosh, Methuen, Patel and Joseph2008; Fox et al., Reference Fox, Stallard and Cooney2015), GPs’ confidence in asking sensitive questions is confirmed whereas in other studies (Michail and Tait, Reference Michail and Tait2016) GPs’ narratives revealed difficulties in discussing suicidal thoughts and self-harm with young people highlighting significant communication difficulties during consultations. Similar communication issues in GP consultations with young people have been reported previously (Roberts et al., Reference Saini, Windfuhr, Pearson, Da Cruz, Miles, Cordingley, While, Swinson, Williams, Shaw, Appleby and Kapur2013).
In terms of knowledge, GPs, and specifically those more experienced, demonstrated high levels of knowledge and awareness of those factors associated with suicide risk in young people. This is confirmed by previous studies (Ritter et al., Reference Rudd2008; Michail and Tait, Reference Michail and Tait2016) where GPs’ knowledge on suicidality, risk and its management was also supported. In Michail and Tait (Reference Michail and Tait2016), GPs highlighted that although they are well informed about those factors associated with suicidality in young people, they are less confident about how risk factors can be applied to accurately identify risk during consultations. Regarding knowledge of suicide warning signs in young people, the survey confirmed previous findings that GPs find challenging the accurate recognition of those signs that might indicate heightened risk in young people in the near future. Indeed, in Michail and Tait (Reference Michail and Tait2016), GPs reported significant challenges in distinguishing between signs indicating imminent suicide risk from behavioural and affective changes that form part of ‘normal adolescence’. Rudd (2008) has highlighted the theoretical and clinical challenges in differentiating between warning signs and risk factors for suicide as well as effectively identifying warning signs in day-to-day clinical practice. Although there is considerable confusion about the definition, nature and manifestation of suicide warning signs, Rudd (2008) emphasises some key distinctions (eg, proximal relationship to suicidal behaviour; observable and subjective; should be seen as a collection of signs and symptoms rather than individually) between these and risk factors that should be helpful in guiding clinical judgements. Most importantly, Rudd (2008) highlights the episodic and variable nature of warning signs, which justifies why the involvement of family members and significant others in clinical consultations is so important, especially so when these consultations involve vulnerable young people.
An important part of the survey was to investigate GPs’ personal attitudes towards young people at risk of suicide. We know that attitudes can influence clinical behaviour and practice (Saunders et al., Reference Taylor, Hawton, Fortune and Kapur2012), with evidence showing that negative attitudes on behalf of clinicians towards people who deliberately self-harm affect therapeutic engagement and management (Taylor, 2009). In line with previous findings (Illiffe et al., Reference Illiffe, Williams, Fernandez, Vila, Kramer, Gledhill and Miller2008; Roberts et al., Reference Saini, Windfuhr, Pearson, Da Cruz, Miles, Cordingley, While, Swinson, Williams, Shaw, Appleby and Kapur2013; Michail and Tait, Reference Michail and Tait2016), GPs perceived young people to be difficult to communicate with (more so than adult patients), with one-third of GPs reporting that those at risk of suicide are frustrating to manage. There was also uncertainty amongst the majority of GPs’ views about whether patients who self-harm are viewed as a burden to a GP. A sense of frustration could be associated with organisational barriers, heavy workload and/or limited management options, all barriers consistently identified by GPs in previous studies (Saini et al., Reference Saunders, Hawton and Fortune2010; Michail and Tait, Reference Michail and Tait2016). However, we have previously argued that signs such as impulsivity, distress, lack of communication and unpredictability are all key emotional, psychological and social mechanisms inherently linked with suicidality and self-harm (Hawton et al., Reference Hawton, Saunders and O’Connor2012; O’Connor et al., 2012) and do not simply reflect traits of adolescence or being a ‘difficult youth’. In fact, all aforementioned signs could indicate imminent risk (ie, warning signs) and should therefore be explored not dismissed in clinical consultations (Rudd, 2008).
The survey also sought to explore GPs’ views regarding the effectiveness of routine screening (ie, enquiring patients about suicidal ideas and intent using screening tools or scales) in preventing suicides in young people. GPs were split in their views with 42% feeling unsure and 41% supporting the effectiveness of routine screening. Although the importance of early identification and assessment of those at risk has been consistently highlighted in national and international suicide prevention strategies (DoH, 2014; WHO, 2014), the evidence base for the effectiveness of routine screening is limited. A recent systematic review (O’Connor et al., Reference Rickwood, Deane and Wilson2013) concluded that evidence was insufficient to determine the benefits of screening in primary care populations, which is in line with findings from previous reviews (Gaynes et al., Reference Gaynes, West, Ford, Frame, Klein and Lohr2004). Most importantly, O’Connor et al. (Reference Rickwood, Deane and Wilson2013) demonstrated the limited evidence base supporting the accuracy of screening tools in identifying at-risk individuals, especially adolescents, and have, therefore, called for the need for further research on how to effectively identify and treat youth at increased risk for suicide. The predictive validity of screening tools and checklists has also been questioned by clinical guidelines (NICE guidelines, 2012), which argue against their use in isolation, but as part of a holistic, needs-based assessment to facilitate clinical decision making.
Clinical implications
The study has important implications for the provision of specialist training to support GPs (especially those less experienced) in the assessment and management of youth suicide risk. Despite the reported high levels of confidence, and to some extent knowledge, only 38% of young people with mental health problems are identified by their GP (Gledhill et al., Reference Gledhill and Garralda2003) usually those at the severe end of the spectrum (Martinez, Reference Martinez2006); whereas, those with less severe depressive disorders are not systematically detected (Gledhill and Garralda, Reference Gledhill, Kramer, Iliffe and Garrald2011). It is not surprising, therefore, that 75% of GPs in our study said they would be very interested in receiving further training on assessing and managing young people at risk of suicide.
We also draw attention to the findings of this survey that existing mental health training for GPs did not seem to improve levels of knowledge of suicide warning signs. Almost 60% of GPs were not aware of any published suicide prevention guidelines, regardless of their mental health training status. The importance of continued education in this field has been highlighted previously (Sudak et al., Reference Thompson, Powis and Carradice2007; Saini et al., Reference Saunders, Hawton and Fortune2010; Grimholt et al., Reference Grimholt, Haave, Jacobsen, Sandvik and Ekeberg2014), although existing training has primarily focussed on the provision and promotion of micro-skills (Appleby et al., Reference Appleby, Amos, Doyle, Tomenson and Woodman2000; Gould et al., Reference Gould, Greenberg, Velting and Shaffer2003). We argue instead for the importance of enhancing, through specific training and education, GPs’ competencies and capabilities in conducting a holistic, psychosocial needs-based assessment in line with NICE Recommendations (2012) to facilitate therapeutic engagement and communication with young people (Michail and Tait, Reference Michail and Tait2016). Taking into consideration the wider psychosocial context of the individual (Morriss et al., Reference Morriss, Kapur and Byng2013), adopting a compassionate approach in the assessment and mitigation of risk (Cole-King and Lepping, Reference Cole-King and Lepping2010a) as well as addressing how GPs understand and conceptualise the notion of risk (Michail and Tait, Reference Michail and Tait2016) should be pivotal aspects of any educational programme for GPs on youth suicide.
At the same time, for any training to be effective and feasible, it would need to be accompanied by changes in primary care organisation. International initiatives such as the WHO framework for the development of youth friendly health services (Tylee et al., Reference Tylee, Haller, Graham, Churchill and Sandi2007) offers a valuable resource for the provision of an innovative, equitable and collaborative model of care where young people are at the centre of the decisions made about their care. Promoting such a model of care in our primary care services could improve the communication between GPs and young people to facilitate a trusting doctor–patient relationship and, thus, help address some of the attitudinal issues identified by the present study and others before (Illiffe et al., Reference Illiffe, Williams, Fernandez, Vila, Kramer, Gledhill and Miller2008; Roberts et al., Reference Saini, Windfuhr, Pearson, Da Cruz, Miles, Cordingley, While, Swinson, Williams, Shaw, Appleby and Kapur2013; Michail and Tait, Reference Michail and Tait2016).
Limitations
The generalisability of the findings is limited by the relatively low response rate, which reflects well documented challenges in engaging busy clinicians in research (Pit et al., Reference Ritter, Stompe, Voracek and Etzersdorfer2014). The possibility of a response bias is also likely as GPs responding to the survey might be those more interested in the topic. In addition, self-reported confidence and attitudes may not necessarily accord with actual behaviour. The survey was developed specifically for this study and therefore might not have adequate construct validity. We intend to assess the construct validity of the survey in a future study.
Conclusion
Despite the high levels of confidence reported by GPs, the study revealed significant gaps in GPs’ knowledge required for the assessment and management of suicide risk in young people. GPs’ views towards suicidal young people also varied significantly with a great number of GPs expressing some negativity towards suicidal young patients and aspects of their care. We highlight the importance of continued education in suicide risk assessment and management in youth through the provision of specialist training to facilitate therapeutic engagement and communication with young people.
Acknowledgements
The authors would like to thank the members of Project Steering Group who served as scientific advisors and the GPs who participating in the study.
Financial Support
This work was supported by a NIHR Research Capability grant from Nottingham City Clinical Commissioning Group awarded to the corresponding author.
Conflicts of Interest
None.
Funding
This work was supported by a NIHR Research Capability grant from Nottingham City Clinical Commissioning Group awarded to the corresponding author.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional guidelines on human experimentation (University of Nottingham) and with the Helsinki Declaration of 1975, as revised in 2008.
Supplementary Material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1463423617000299





