Recent systematic reviews (Reference Gowers and Bryant-WaughGowers & Bryant-Waugh, 2004; National Collaborating Centre for Mental Health, 2004; Reference Treasure and SchmidtTreasure & Schmidt, 2004) have drawn attention to the shortage of high-quality, adequately-powered treatment trials for anorexia nervosa. Indeed, the National Institute for Clinical Excellence (NICE) evidence-based guideline (National Collaborating Centre for Mental Health, 2004) was unable to make a single Grade A treatment recommendation across the age range. The choice of treatment setting has tended to be based on clinical judgement and the availability of different models of service rather than research evidence (National Collaborating Centre for Mental Health, 2004). Debate about the merits of inpatient management frequently fails to distinguish between (often brief) medical admission and longer psychiatric admission aimed at a combination of weight restoration, normal eating and psychological change. We report here a large population-based randomised controlled trial (RCT) of the three main treatments available for adolescents in the UK in order to clarify the relative merits of in-patient psychiatric treatment and two forms of out-patient management.
METHOD
The Treatment Outcome for Child and adolescent Anorexia Nervosa (TOuCAN) trial aimed to compare the clinical effectiveness of in-patient against specialist out-patient and treatment as usual in the community. The study also examined the cost-effectiveness of each approach (Reference Byford, Barrett and RobertsByford et al, 2007, this issue) and user satisfaction with each treatment (not reported here).
Our hypotheses were that: (a) the more intensive in-patient treatment would be more effective than out-patient treatment; and (b) specialist out-patient treatment would be more effective than general child and adolescent mental health service (CAMHS) treatment.
Participants
The trial took place in the north-west of England. The population (total 7.2 million) is served by 38 community CAMHS and four in-patient psychiatric units. The study aimed to recruit as complete a series as possible of consecutive cases referred to community CAMHS. In total 35 out of 38 CAMHS services agreed to refer to the trial.
Inclusion criteria were male or female adolescents aged 12–18 years with a diagnosis of anorexia nervosa according to DSM–IV criteria (American Psychiatric Association, 1994) modified for this age group as follows: food restriction with or without compensatory behaviours; weight below 85% of that expected within 1 month of assessment, based on age and current height or previous height centile; intense fear of gaining weight or undue influence of weight or shape on self-evaluation; primary or secondary amenorrhoea of at least 3 months, or menstruation only while on the contraceptive pill. No exclusions were made on grounds of clinical severity, but the responsible clinician reserved the right to refer for acute medical management if required. Those with severe intellectual disability and severe, chronic comorbid physical conditions affecting digestion or metabolism were excluded.
Recruitment strategy
Child and adolescent mental health services identified patients with probable anorexia nervosa and invited them to meet the researchers. The research team supported by a clinician then interviewed the young person (generally with a parental informant), confirmed the diagnosis and obtained informed consent for them to take part in the randomisation, along with baseline measures. Those agreeing were sent an appointment at the allocated treatment facility closest to their home. The recruitment and consent strategy was approved by the North-West Multi-Centre Research Ethics Committee. Treatment allocation was carried out by an independent randomisation service using stochastic minimisation controlling for gender, age above and below 16 years and body mass index (BMI) above and below 15.5.
Treatments
In-patient psychiatric treatment (4 services)
This was provided within generic children's or adolescent psychiatric in-patient units. All four services had substantial experience in treating eating disorders, although they were not exclusively eating disorder services. In keeping with the national census findings (Reference O'Herlihy, Worrall and LelliottO'Herlihy et al, 2003), anorexia nervosa often comprised the most prevalent diagnosis within the units. Treatment lasted 6 weeks in the first instance, extended as clinically indicated and determined by the treating service. The treatment was not manualised, but services met at the outset to identify core elements in treatment. They all used a multidisciplinary psychiatric approach with the aim of normalising eating, restoring healthy weight and facilitating psychological (cognitive) change. Each participant received both individual supportive or cognitive therapies and family therapy. There was a high expectation of early behavioural change and services employed a weight restoration programme with an expected weight increase of 800–1000 g per week. Participants were ambulant and attended the unit school subject to medical stability. Nasogastric feeding was rarely employed and the services avoided coercive treatment practices.
Specialised out-patient treatment (2 services)
This programme was manualised and devised for the trial. It comprised an initial motivational interview, individual cognitive–behavioural therapy (CBT) plus parental feedback (12 sessions), parental counselling with the patient (minimum 4 sessions, increasing to 8 for younger patients), dietary therapy (4 sessions, with parental involvement as required), multi-modal feedback (weight, self-report and clinician-rated questionnaire) monitoring (4 sessions). The treatment was designed to last 6 months. The CBT programme and parental counselling were provided by a trained member of the eating disorder team who had pilot experience of the manualised treatment. The same therapist provided feedback to the patient every 6 weeks, covering physical and self-report questionnaire data. The aim was to demonstrate an association between weight gain and reduced self-reported psychopathology, to motivate the patient to take the next steps to recovery. Dietetic therapy was provided by a trained dietician working as a fully integrated member of the team. This treatment has been described in detail (Reference Gowers and SmythGowers & Smyth, 2004) along with the rationale behind it (Reference GowersGowers, 2006). Checks of treatment fidelity were made at weekly joint meetings between the clinical and research teams. Travel times to the specialist services were generally under 90 min.
Treatment as usual in general community CAMHS
This was not a manualised treatment, but comprised the usual first-line treatment approach that young people in the UK receive. The 35 services provided (generally) a multidisciplinary, family-based approach, with variable dietetic, individual supportive therapy and paediatric (medical) liaison. As the study aimed to compare the specialised treatment with treatment as usual, the latter was not prescriptive and the out-patient arms were not matched for intensity, however the duration of therapy was set at 6 months.
Measures
Interviewer-based measures
Clinical diagnosis was based on modified DSM–IV (American Psychiatric Association, 1994).
Morgan–Russell Average Outcome Scale (MRAOS; Reference Morgan and HaywardMorgan & Hayward, 1988) was adjusted for adolescents and used as a severity measure. It provides a quantitative score from 0 to 12 based on the mean of five sub-scales A–E covering nutritional status, menstruation, mental state, psychosexual adjustment and socio-economic status. It also provides a categorical measure (good, intermediate and poor). It has been widely used in anorexia nervosa research (Reference Russell, Szmukler and DareRussell et al, 1987; Reference Crisp, Norton and GowersCrisp et al, 1991; Reference Eisler, Dare and RussellEisler et al, 1997; Reference North and GowersNorth & Gowers, 1999; Reference Eisler, Dare and HodesEisler et al, 2000).
Health of the Nation Outcome Scale for Children and Adolescents (HoNOSCA; Reference Gowers, Harrington and WhittonGowers et al, 1999) is a 13-item clinician-rated measure yielding a total severity and outcome score which has been shown to be reliable, valid and sensitive to change (Reference Yates, Garralda and HigginsonYates et al, 1999; Reference Garralda, Yates and HigginsonGarralda et al, 2000).
Participant ratings
Eating Disorder Inventory 2 (EDI; Reference GarnerGarner, 1991) is a self-rated questionnaire covering 12 domains of eating cognitions, behaviours and social functioning. Total and sub-scale scores can be generated, with satisfactory validity and sensitivity to change.
HoNOSCA–SR (Reference Gowers, Levine and Bailey-RogersGowers et al, 2002) is the adolescent self-rated version of HoNOSCA.
Family Assessment Device (FAD; Reference Epstein, Bishop and LevinEpstein et al, 1983) is a self-report questionnaire designed to evaluate family functioning based on the seven sub-scales of the McMaster model.
Mood and Feelings Questionnaire (MFQ; Reference Angold, Costello and MesserAngold et al, 1995) is a 42-item questionnaire to rate depression, which has good properties in clinical adolescent samples (Reference Wood, Kroll and MooreWood et al, 1995).
All measures were carried out at baseline and follow-up. Follow-up took place 1 and 2 years after baseline, either at a local CAMHS or the participant's home according to their preference. Interviews were carried out masked to treatment allocation by a research worker who had not been involved in recruitment and did not have access to the baseline database or recruitment file. Where the participant declined an interview, information was provided (with consent) by a relative (usually parent), a health service professional involved in their care or (rarely) by telephone interview.
Sample size
The sample size was calculated a priori using the main outcome measure, the MRAOS. Based on previous findings (Reference North and GowersNorth & Gowers, 1999), an effect size of 1.5 units on this primary outcome was considered to be a clinically important difference. Assuming a similar standard deviation of 2.3 units, the study would have a power of 80% to detect a difference of this magnitude with 46 participants followed-up in each arm using a 2.5% two-sided significance level to adjust for two treatment comparisons. Assuming an 85% follow-up rate, this would require 55 participants randomised to each of the three groups.
Statistical analysis
Analysis comparing the three treatment arms was based on intention to treat. Outcome measures at 1 and 2 years were analysed using analysis of covariance with covariates for baseline value for the main outcome measure (MRAOS), treatment group, gender, research site (Liverpool/Manchester), age and baseline MFQ score. Models were checked for robustness using standard regression diagnostics. Where there was evidence of non-normality, the non-parametric bootstrap was used to check the robustness of the analysis (Reference Efron and TibshiraniEfron & Tibshirani 1993). Diagnostic outcome category was modelled using ordinal logistic regression with the same covariates (Reference McCullaghMcCullagh, 1980).
RESULTS
Participants
The 35 CAMHS identified 347 young people between 2000 and 2003; 100 were excluded because they did not fulfil the diagnosis (n=98, chiefly eating disorder not otherwise specified; EDNOS), and because of physical comorbidity (cystic fibrosis n=1, epilepsy n=1); 31 young people refused all consent, and 46 agreed to follow-up but not randomisation; 170 were randomised to treatment, but 3 were excluded post-randomisation because information subsequently came to light that questioned the diagnosis (2 reclassified EDNOS, 1 chronic fatigue syndrome). The final sample comprised 216 young people, of whom 167 were randomised and are reported here (see Fig. 1 for CONSORT details).
TOuCAN Trial CONSORT diagram.

Annual CAMHS audits were carried out to identify young people known to them but not referred to the trial. This identified a further 25 young people, chiefly where the diagnosis had emerged after some time of CAMHS treatment. Overall the study recruited 79% of young people with anorexia nervosa known to community CAMHS in this period (215 out of 271).
Demographic characteristics
Participants were aged between 11 years 11 months and 17 years 11 months (mean 14 years 11 months); 153 (92%) were female; 127 (76%) experienced the restricting subtype and 40 (24%) the binge purging subtype of anorexia nervosa. Mean length of history was 13 months; 104 (62.3%) lived with both biological parents, 32 with mother (19.2%) and 6 (3.6%) with father; 11 (6.6%) lived with mother and stepfather and 13 (7.8%) in other arrangements (1 case not known). There were no significant differences between the samples recruited from the Manchester site (n=80) and the Liverpool site (n=87).
Clinical features
Tables 1 and 2 show the presenting features according to allocated treatment. The treatment groups were generally moderately to severely ill (mean weight for height 78.0%, lowest 57.9%). Eight had a weight for height above the anorexic threshold. Of these, 4 were included because they lost significant weight in the 4 weeks following assessment, or they had previously attained a greater height percentile, suggesting stunting of growth, whereas 4 others with borderline weights were included because they fulfilled the other criteria plus significant (>15% and generally >20%) weight loss with amenorrhoea. Five females were sporadically menstruating, but at lower than 85% weight for height. There were no significant differences between groups on any variable; including length of history. For the EDI, MFQ, FAD and HoNOSCA a higher score indicates greater difficulty, whereas the Morgan–Russell scales indicate greater clinical severity by a lower score.
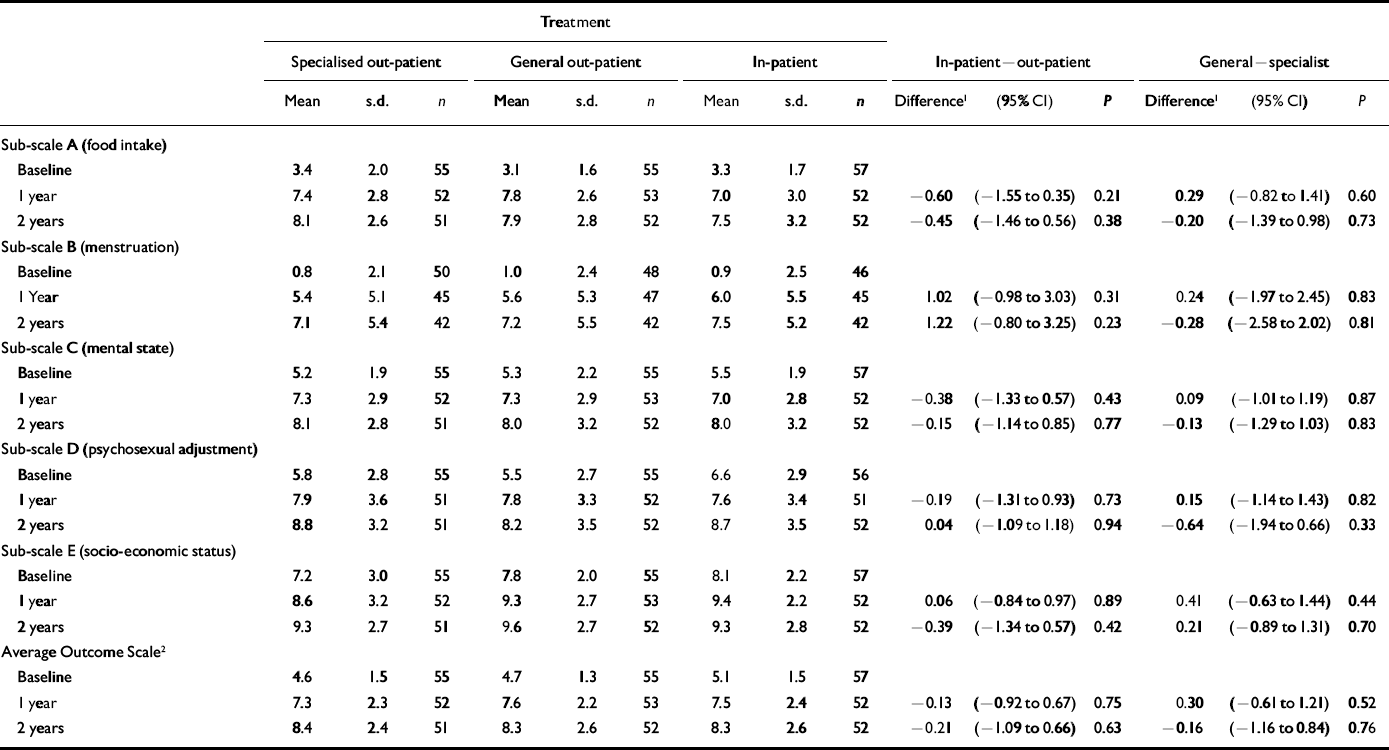
Intention-to-treat analysis of 1- and 2-year outcomes for Morgan–Russell Average Outcome Scale
| Treatment | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Specialised out-patient | General out-patient | In-patient | In-patient — out-patient | General — specialist | |||||||||||
| Mean | s.d. | n | Mean | s.d. | n | Mean | s.d. | n | Difference1 | (95% Cl) | P | Difference1 | (95% Cl) | P | |
| Sub-scale A (food intake) | |||||||||||||||
| Baseline | 3.4 | 2.0 | 55 | 3.1 | 1.6 | 55 | 3.3 | 1.7 | 57 | ||||||
| 1 year | 7.4 | 2.8 | 52 | 7.8 | 2.6 | 53 | 7.0 | 3.0 | 52 | -0.60 | (-1.55 to 0.35) | 0.21 | 0.29 | (-0.82 to 1.41) | 0.60 |
| 2 years | 8.1 | 2.6 | 51 | 7.9 | 2.8 | 52 | 7.5 | 3.2 | 52 | -0.45 | (-1.46 to 0.56) | 0.38 | -0.20 | (-1.39 to 0.98) | 0.73 |
| Sub-scale B (menstruation) | |||||||||||||||
| Baseline | 0.8 | 2.1 | 50 | 1.0 | 2.4 | 48 | 0.9 | 2.5 | 46 | ||||||
| 1 Year | 5.4 | 5.1 | 45 | 5.6 | 5.3 | 47 | 6.0 | 5.5 | 45 | 1.02 | (-0.98 to 3.03) | 0.31 | 0.24 | (-1.97 to 2.45) | 0.83 |
| 2 years | 7.1 | 5.4 | 42 | 7.2 | 5.5 | 42 | 7.5 | 5.2 | 42 | 1.22 | (-0.80 to 3.25) | 0.23 | -0.28 | (-2.58 to 2.02) | 0.81 |
| Sub-scale C (mental state) | |||||||||||||||
| Baseline | 5.2 | 1.9 | 55 | 5.3 | 2.2 | 55 | 5.5 | 1.9 | 57 | ||||||
| 1 year | 7.3 | 2.9 | 52 | 7.3 | 2.9 | 53 | 7.0 | 2.8 | 52 | -0.38 | (-1.33 to 0.57) | 0.43 | 0.09 | (-1.01 to 1.19) | 0.87 |
| 2 years | 8.1 | 2.8 | 51 | 8.0 | 3.2 | 52 | 8.0 | 3.2 | 52 | -0.15 | (-1.14 to 0.85) | 0.77 | -0.13 | (-1.29 to 1.03) | 0.83 |
| Sub-scale D (psychosexual adjustment) | |||||||||||||||
| Baseline | 5.8 | 2.8 | 55 | 5.5 | 2.7 | 55 | 6.6 | 2.9 | 56 | ||||||
| 1 year | 7.9 | 3.6 | 51 | 7.8 | 3.3 | 52 | 7.6 | 3.4 | 51 | -0.19 | (-1.31 to 0.93) | 0.73 | 0.15 | (-1.14 to 1.43) | 0.82 |
| 2 years | 8.8 | 3.2 | 51 | 8.2 | 3.5 | 52 | 8.7 | 3.5 | 52 | 0.04 | (-1.09 to 1.18) | 0.94 | -0.64 | (-1.94 to 0.66) | 0.33 |
| Sub-scale E (socio-economic status) | |||||||||||||||
| Baseline | 7.2 | 3.0 | 55 | 7.8 | 2.0 | 55 | 8.1 | 2.2 | 57 | ||||||
| 1 year | 8.6 | 3.2 | 52 | 9.3 | 2.7 | 53 | 9.4 | 2.2 | 52 | 0.06 | (-0.84 to 0.97) | 0.89 | 0.41 | (-0.63 to 1.44) | 0.44 |
| 2 years | 9.3 | 2.7 | 51 | 9.6 | 2.7 | 52 | 9.3 | 2.8 | 52 | -0.39 | (-1.34 to 0.57) | 0.42 | 0.21 | (-0.89 to 1.31) | 0.70 |
| Average Outcome Scale2 | |||||||||||||||
| Baseline | 4.6 | 1.5 | 55 | 4.7 | 1.3 | 55 | 5.1 | 1.5 | 57 | ||||||
| 1 year | 7.3 | 2.3 | 52 | 7.6 | 2.2 | 53 | 7.5 | 2.4 | 52 | -0.13 | (-0.92 to 0.67) | 0.75 | 0.30 | (-0.61 to 1.21) | 0.52 |
| 2 years | 8.4 | 2.4 | 51 | 8.3 | 2.6 | 52 | 8.3 | 2.6 | 52 | -0.21 | (-1.09 to 0.66) | 0.63 | -0.16 | (-1.16 to 0.84) | 0.76 |
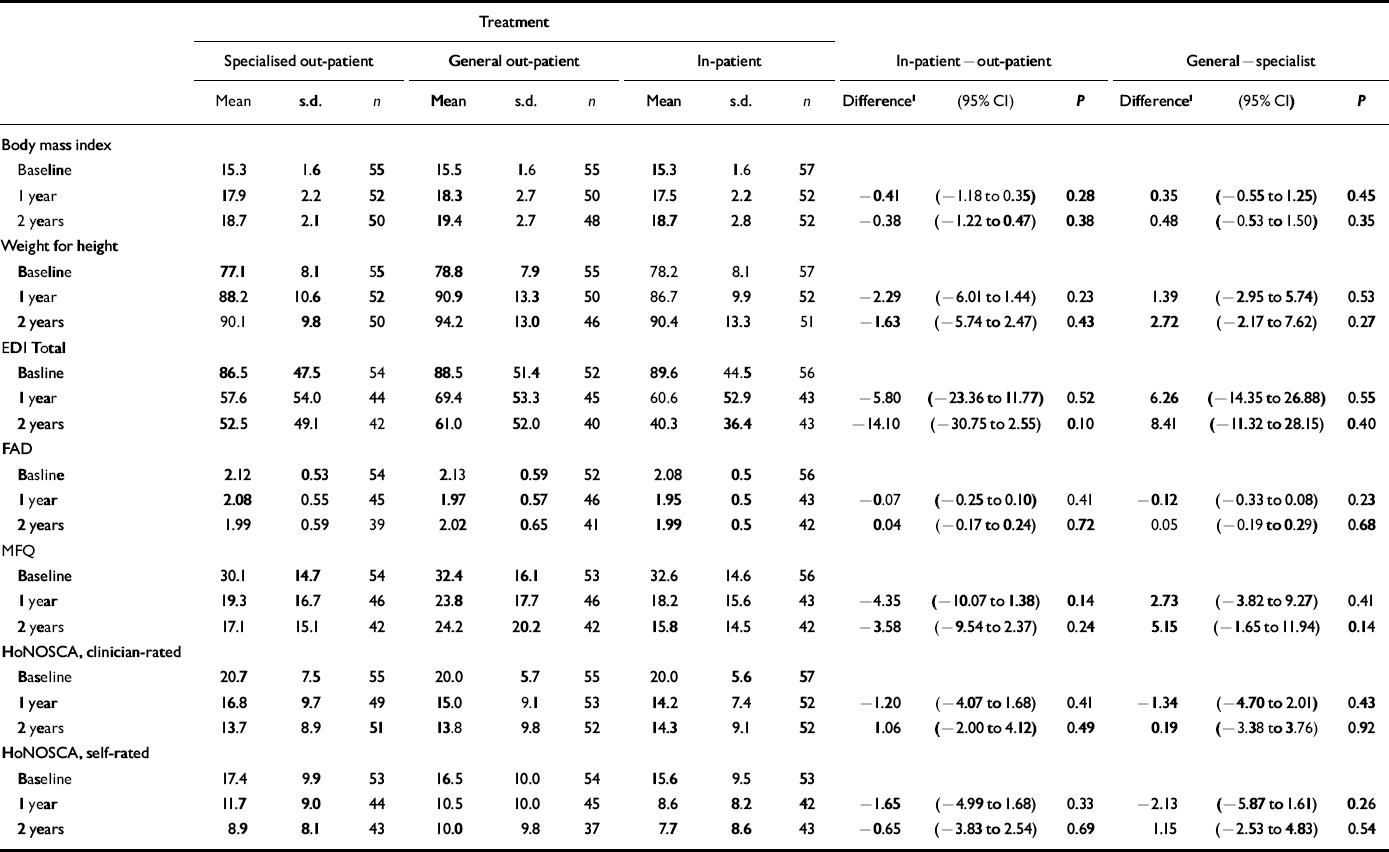
Intention-to-treat analysis for secondary outcomes at 1 and 2 years
| Treatment | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Specialised out-patient | General out-patient | In-patient | In-patient — out-patient | General — specialist | |||||||||||
| Mean | s.d. | n | Mean | s.d. | n | Mean | s.d. | n | Difference1 | (95% CI) | P | Difference1 | (95% CI) | P | |
| Body mass index | |||||||||||||||
| Baseline | 15.3 | 1.6 | 55 | 15.5 | 1.6 | 55 | 15.3 | 1.6 | 57 | ||||||
| 1 year | 17.9 | 2.2 | 52 | 18.3 | 2.7 | 50 | 17.5 | 2.2 | 52 | -0.41 | (-1.18 to 0.35) | 0.28 | 0.35 | (-0.55 to 1.25) | 0.45 |
| 2 years | 18.7 | 2.1 | 50 | 19.4 | 2.7 | 48 | 18.7 | 2.8 | 52 | -0.38 | (-1.22 to 0.47) | 0.38 | 0.48 | (-0.53 to 1.50) | 0.35 |
| Weight for height | |||||||||||||||
| Baseline | 77.1 | 8.1 | 55 | 78.8 | 7.9 | 55 | 78.2 | 8.1 | 57 | ||||||
| 1 year | 88.2 | 10.6 | 52 | 90.9 | 13.3 | 50 | 86.7 | 9.9 | 52 | -2.29 | (-6.01 to 1.44) | 0.23 | 1.39 | (-2.95 to 5.74) | 0.53 |
| 2 years | 90.1 | 9.8 | 50 | 94.2 | 13.0 | 46 | 90.4 | 13.3 | 51 | -1.63 | (-5.74 to 2.47) | 0.43 | 2.72 | (-2.17 to 7.62) | 0.27 |
| EDI Total | |||||||||||||||
| Basline | 86.5 | 47.5 | 54 | 88.5 | 51.4 | 52 | 89.6 | 44.5 | 56 | ||||||
| 1 year | 57.6 | 54.0 | 44 | 69.4 | 53.3 | 45 | 60.6 | 52.9 | 43 | -5.80 | (-23.36 to 11.77) | 0.52 | 6.26 | (-14.35 to 26.88) | 0.55 |
| 2 years | 52.5 | 49.1 | 42 | 61.0 | 52.0 | 40 | 40.3 | 36.4 | 43 | -14.10 | (-30.75 to 2.55) | 0.10 | 8.41 | (-11.32 to 28.15) | 0.40 |
| FAD | |||||||||||||||
| Basline | 2.12 | 0.53 | 54 | 2.13 | 0.59 | 52 | 2.08 | 0.5 | 56 | ||||||
| 1 year | 2.08 | 0.55 | 45 | 1.97 | 0.57 | 46 | 1.95 | 0.5 | 43 | -0.07 | (-0.25 to 0.10) | 0.41 | -0.12 | (-0.33 to 0.08) | 0.23 |
| 2 years | 1.99 | 0.59 | 39 | 2.02 | 0.65 | 41 | 1.99 | 0.5 | 42 | 0.04 | (-0.17 to 0.24) | 0.72 | 0.05 | (-0.19 to 0.29) | 0.68 |
| MFQ | |||||||||||||||
| Baseline | 30.1 | 14.7 | 54 | 32.4 | 16.1 | 53 | 32.6 | 14.6 | 56 | ||||||
| 1 year | 19.3 | 16.7 | 46 | 23.8 | 17.7 | 46 | 18.2 | 15.6 | 43 | -4.35 | (-10.07 to 1.38) | 0.14 | 2.73 | (-3.82 to 9.27) | 0.41 |
| 2 years | 17.1 | 15.1 | 42 | 24.2 | 20.2 | 42 | 15.8 | 14.5 | 42 | -3.58 | (-9.54 to 2.37) | 0.24 | 5.15 | (-1.65 to 11.94) | 0.14 |
| HoNOSCA, clinician-rated | |||||||||||||||
| Baseline | 20.7 | 7.5 | 55 | 20.0 | 5.7 | 55 | 20.0 | 5.6 | 57 | ||||||
| 1 year | 16.8 | 9.7 | 49 | 15.0 | 9.1 | 53 | 14.2 | 7.4 | 52 | -1.20 | (-4.07 to 1.68) | 0.41 | -1.34 | (-4.70 to 2.01) | 0.43 |
| 2 years | 13.7 | 8.9 | 51 | 13.8 | 9.8 | 52 | 14.3 | 9.1 | 52 | 1.06 | (-2.00 to 4.12) | 0.49 | 0.19 | (-3.38 to 3.76) | 0.92 |
| HoNOSCA, self-rated | |||||||||||||||
| Baseline | 17.4 | 9.9 | 53 | 16.5 | 10.0 | 54 | 15.6 | 9.5 | 53 | ||||||
| 1 year | 11.7 | 9.0 | 44 | 10.5 | 10.0 | 45 | 8.6 | 8.2 | 42 | -1.65 | (-4.99 to 1.68) | 0.33 | -2.13 | (-5.87 to 1.61) | 0.26 |
| 2 years | 8.9 | 8.1 | 43 | 10.0 | 9.8 | 37 | 7.7 | 8.6 | 43 | -0.65 | (-3.83 to 2.54) | 0.69 | 1.15 | (-2.53 to 4.83) | 0.54 |
Adherence to treatment allocation
Adherence to allocated treatment was 65% but varied between groups. For in-patient treatment, defined as a 4-week in-patient stay, 28 out of 57 adhered (49.1%). In most cases, those failing to adhere agreed initially to admission and then bargained their way out by achieving a small weight gain in the short time between randomisation and admission. Mean length of stay for those admitted was 15.2 weeks. For specialist out-patient treatment, defined as a minimum of 6 attendances, 41 out of 55 adhered (74.5%). Of the remainder, 10 changed their mind and opted for general CAMHS treatment (generally because of travelling distance), 3 were admitted before treatment could start and 1 dropped out of all treatment. For general CAMHS treatment, defined as attending general CAMHS and no other treatment in the initial phase, 38 out of 55 adhered (69.1%). Two of the remainder had no treatment, 4 opted for specialist out-patient treatment and 11 were referred to an alternative by clinician preference (10 in-patient, 1 specialist out-patient).
Clinical outcomes
Every participant was traced, with the main outcome measures completed as follows: diagnostic outcome and outcome category, 164 participants (98%) at 1 year, 160 (96%) at 2 years; MRAOS, 157 (94%) at 1 year, 155 (93%) at 2 years; BMI/weight for height, 154 (92%) at 1 year, 150 (90%) at 2 years; HoNOSCA 154 (92%) at 1 year, 155 (93%) at 2 years. These were achieved by face-to-face interview in 129 participants (77%) at 1 year and 121 (73%) at 2 years. Outcome data were obtained by telephone interview or interview with a health professional informant in 34 (20%) at 1 year and 40 (24%) at 2 years. The remaining 4 at 1 year and 6 at 2 years were all traced (alive) but little or no information was obtained on their health status.
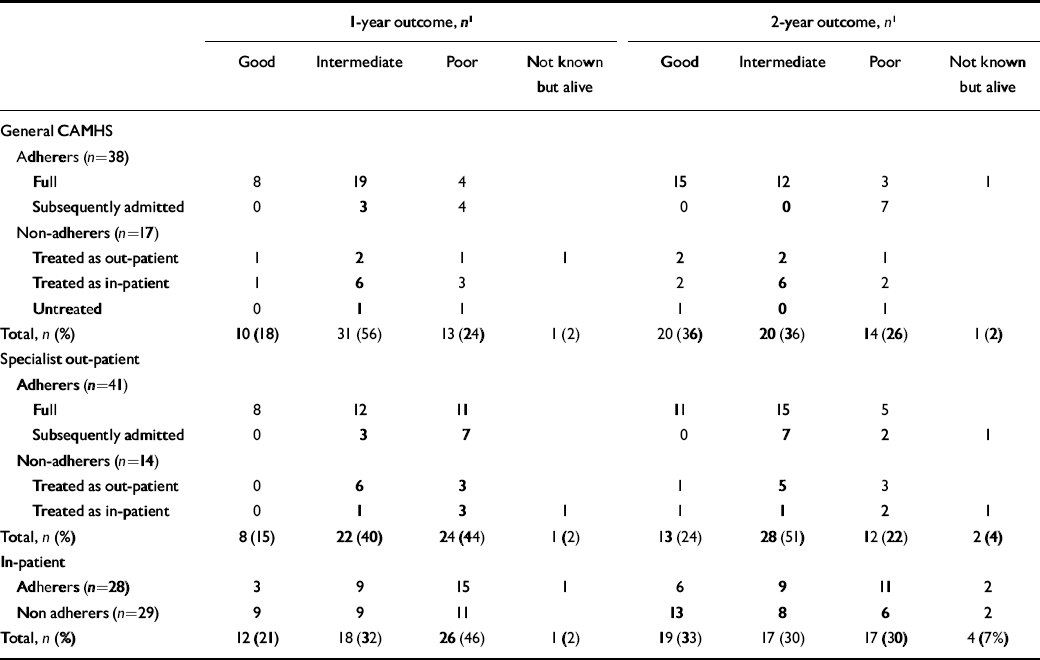
Table 3 shows the categorical outcomes based on those employed in the Maudsley studies (Reference Russell, Szmukler and DareRussell et al, 1987) and we employed a high threshold for assigning recovery. A good outcome indicates a full recovery from anorexia nervosa (weight above 85% of expected, return of menstruation, bingeing/purging no greater than once per month). A poor outcome was indicated if weight was not above 85% or the young person was still being treated as an in-patient for anorexia nervosa. The intermediate category comprises those whose weight had risen to within the normal range, but without return of menstruation, with bingeing/purging at a frequency greater than monthly or considerable residual concerns about weight and shape according to Morgan–Russell scale A scores for food intake.
Categorical outcomes at 1 and 2 years by intention to treat
| 1-year outcome, n 1 | 2-year outcome, n 1 | |||||||
|---|---|---|---|---|---|---|---|---|
| Good | Intermediate | Poor | Not known but alive | Good | Intermediate | Poor | Not known but alive | |
| General CAMHS | ||||||||
| Adherers (n=38) | ||||||||
| Full | 8 | 19 | 4 | 15 | 12 | 3 | 1 | |
| Subsequently admitted | 0 | 3 | 4 | 0 | 0 | 7 | ||
| Non-adherers (n=17) | ||||||||
| Treated as out-patient | 1 | 2 | 1 | 1 | 2 | 2 | 1 | |
| Treated as in-patient | 1 | 6 | 3 | 2 | 6 | 2 | ||
| Untreated | 0 | 1 | 1 | 1 | 0 | 1 | ||
| Total, n (%) | 10 (18) | 31 (56) | 13 (24) | 1 (2) | 20 (36) | 20 (36) | 14 (26) | 1 (2) |
| Specialist out-patient | ||||||||
| Adherers (n=41) | ||||||||
| Full | 8 | 12 | 11 | 11 | 15 | 5 | ||
| Subsequently admitted | 0 | 3 | 7 | 0 | 7 | 2 | 1 | |
| Non-adherers (n=14) | ||||||||
| Treated as out-patient | 0 | 6 | 3 | 1 | 5 | 3 | ||
| Treated as in-patient | 0 | 1 | 3 | 1 | 1 | 1 | 2 | 1 |
| Total, n (%) | 8 (15) | 22 (40) | 24 (44) | 1 (2) | 13 (24) | 28 (51) | 12 (22) | 2 (4) |
| In-patient | ||||||||
| Adherers (n=28) | 3 | 9 | 15 | 1 | 6 | 9 | 11 | 2 |
| Non adherers (n=29) | 9 | 9 | 11 | 13 | 8 | 6 | 2 | |
| Total, n (%) | 12 (21) | 18 (32) | 26 (46) | 1 (2) | 19 (33) | 17 (30) | 17 (30) | 4 (7%) |
Reliability of assessment measures
Interrater reliability (IRR) series were carried out within research site and between sites at baseline; intraclass correlation (ICC) coefficients were as follows: MRAOS, Manchester 0.93, Liverpool 0.97, intersite 0.96, IRR at 1 year 0.93, 2 years 0.90; HONOSCA, Manchester 0.83, Liverpool 0.98, intersite 0.87, IRR at 1 year 0.89, 2 years 0.89.
1 year outcome
All groups made substantial mean improvements in terms of weight, global measures and self-reported psychopathology (Tables 1 and 2). In an intention-to-treat analysis there are no statistically significant differences between the three groups. In particular, the mean values on the MRAOS are remarkably similar across the treatments. Those allocated to general CAMHS treatment were less likely to still have anorexia nervosa at 1 year (Table 3), but by intention to treat there were no significant differences between the three groups (ordinal logistic regression P=0.22). For the two out-patient treatment arms there was a much better outcome for those who fully adhered to treatment compared with those failing to adhere or later transferring away from allocated treatment. Specifically, for general CAMHS treatment, only 1 out of 17 admitted for in-patient treatment had a good outcome at 1 year, whereas for the specialist out-patient programme, none of the 14 who initially failed to adhere to the allocated programme had a good outcome, nor any of 14 subsequently admitted to in-patient treatment.
Sub-analysis of those allocated to in-patient treatment
The relatively poor outcomes at 1 year of those allocated to in-patient treatment merits further exploration. Adherence to treatment was poor (49%, 28 out of 57) for this option, therefore in theory this might have compromised the effectiveness of this treatment. To explore this further, we carried out a comparison between those randomised to in-patient treatment who were admitted and those who subsequently refused admission and continued with out-patient treatment. At baseline there was little difference between the two subgroups although those who were admitted were on average 6 months younger and showed a reduced food intake (MRAOS sub-scale A; see Table DS1 in the data supplement to the online version of this paper). At 1-year follow-up, those refusing admission were doing significantly better on the MRAOS (mean difference 2.0, 95% CI 0.8–3.2, P=0.001) and virtually all self-report measures of psychopathology, including mood (all change scores controlled for baseline values). Intriguingly in-patient admission appears to have little or no impact on core cognitions such as body dissatisfaction or drive for thinness, whereas those who declined admission made improvements in these areas.
2-year outcome
At 2 years there was further improvement in outcomes for all groups, with an overall good outcome for 33%, but 27% still had anorexia nervosa. Again there are no significant differences between the groups by intention to treat on either the MRAOS, the other main outcome measures or the categorical outcomes (ordinal logistic regression P=0.89; Table 3). There were 47 (28.1%) still in treatment at 2 years (9 as in-patients) with no clear differences between groups. Although differences between treatment groups are minimal, the impact of adherence to treatment and hospitalisation remain or indeed are more marked at 2 years (Table 3). For those allocated in-patient treatment, there is a general improvement between 1 and 2 years, but this is more marked for those who declined admission. Of those allocated to the two out-patient treatments, 31 were admitted to hospital in year 1, of whom only 3 had a good outcome at 2 years, and none out of 17 who fully adhered to the out-patient programmes but were subsequently admitted, presumably owing to their failure to respond to out-patient management. For those allocated to in-patient treatment, there remains a better outcome on the main outcome measure for those declining admission compared with those who were admitted, even controlling for baseline values (see Table DS1 in online data supplement).
DISCUSSION
This trial reports the outcome of a large, population-based RCT of adolescents with anorexia nervosa. Although frequently a chronic condition, treatment in a range of services brought about significant improvement by 1 year after presentation, with further progress by 2 years. Fewer than 1 in 5 fully recovered within 1 year, but one-third had recovered by 2 years, with only a quarter still having anorexia nervosa at this time point.
Contrary to our hypotheses, there was no advantage for specialist over general CAMHS treatment or in-patient over out-patient management. It could be argued that the in-patient services in the study were not truly specialised, as they were not exclusive eating disorder facilities. However, all four units had extensive experience and tradition of treating such patients. Indeed 17 adolescents entered other (often exclusive) specialist in-patient services in the follow-up period of the study and still had poor outcomes at 2 years. Most of those who found their way into in-patient management had failed to improve with out-patient treatment. Nevertheless, their poor outcomes challenge the intuitive clinical belief that a step up progression from out-patient to in-patient psychiatric care is indicated for those who fail to make progress. The outcomes of those allocated to and receiving in-patient management were also rather poor. It may be that the decision to accept randomised admission is based on a number of negative prognostic variables, rather than it reflecting on the in-patient treatment itself. Our analysis suggests that those agreeing to admission were marginally thinner and had a lower MRAOS sub-scale A (food intake) score. However, given that the presenting values on these variables did not account for the differences in outcome, some unmeasured variables such as motivation or family resources may have accounted for the difference in response. This finding does not deny the necessity of emergency medical management of physical complications in an in-patient setting, which may on occasions be life-saving, but our results do suggest that in-patient management rarely leads to comprehensive recovery, as opposed to improvement or stability within the condition. The health economic implications of this finding are presented elsewhere, (Reference Byford, Barrett and RobertsByford et al, 2007, this issue), but this finding has significant cost implications.
Comparison with previous research
The NICE eating disorder guideline (National Collaborating Centre for Mental Health, 2004) highlighted the shortage of quality treatment trials for anorexia nervosa. A number of relatively small RCTs (Reference Russell, Szmukler and DareRussell et al, 1987; Reference Le Grange, Eisler and DareLe Grange et al, 1992; Reference Eisler, Dare and RussellEisler et al, 1997; Reference Robin, Siegel and MoyeRobin et al, 1999; Reference Eisler, Dare and HodesEisler et al, 2000; Reference Lock, Agras and BrysonLock et al, 2005) have suggested promising outcomes of family interventions for adolescents and few would contest the necessity of involving parents in their treatment. Most of this research has followed the Maudsley model, but differences in research design (for example inclusion in some studies of participants who have had their weight restored) makes for uncertainties in interpretation, particularly as this treatment has not been fully tested against other approaches. The present study was devised before the more recent positive outcomes of family-based treatment were published and it is of note that our findings suggest poorer outcomes. We had been impressed by the preliminary outcomes of extended CBT (Reference Fairburn, Cooper and ShafranFairburn et al, 2003) in addressing the core psychopathology of eating and weight concerns and questioned the power of family-based treatment to address these as opposed to behavioural aspects of the condition. Recent research from the Maudsley group (Reference Eisler, Dare and HodesEisler et al, 2000) has cast some doubt on the value of conjoint family therapy in a trial that found it less effective than separated family therapy, based on the Morgan–Russell outcome categories. Strikingly no young people had a good outcome where there was high expressed emotion in the family. Clearly further adequately powered studies are required of family-based treatment against CBT, either as described here or the transdiagnostic form devised by the Oxford group (Reference Fairburn, Cooper and ShafranFairburn et al, 2003).
Treatment setting has been investigated far less. The relatively underpowered St George's trial failed to find an advantage for in-patient over specialist out-patient treatment in a mixed age sample (Reference Crisp, Norton and GowersCrisp et al, 1991, Reference Gowers, Norton and HalekGowers et al, 1994). This led Meads et al (Reference Meads, Gold and Burls2001) to conclude in their systematic review that out-patient treatment in a specialist eating disorder service was as effective as in-patient treatment in those not so severely ill as to warrant emergency admission. Furthermore, these reviewers estimated the costs of out-patient treatment to be approximately one-tenth the cost of in-patient treatment.
The facility to offer long-term psychiatric (as opposed to medical) treatment in the UK has often been highly valued, clinical intuition suggesting that more intensive treatments should be more effective than briefer, non-specialist treatment for a condition that is often chronic and has a high morbidity and mortality (Reference Herzog, Herzog, Deter and VandereyckenHerzog, 1992). However, there is little research evidence to demonstrate the benefits of lengthy in-patient psychiatric treatment and a recent survey (Reference Roots, Hawker and GowersRoots et al, 2006) of adolescent services in the UK and Europe revealed great variation in typical length of stay, target weight and treatment philosophy. The St George's (Reference Crisp, Norton and GowersCrisp et al, 1991) and Maudsley studies (Reference Russell, Szmukler and DareRussell et al, 1987) showed that although the majority of those receiving lengthy in-patient treatment gained weight to normal levels, many had lost a significant amount of weight by 1 year follow-up. Furthermore, there has been little or no research into potential unwanted effects of different treatment settings. The poor outcomes of in-patient treatment in a naturalistic cohort of young people have led to speculation that certain features of anorexia nervosa, for example ineffectiveness, low self-esteem, interpersonal distrust, might be exacerbated by lengthy admission (Reference Gowers, Weetman and ShoreGowers et al, 2000).
Research into the length and content of out-patient treatment has also provided mixed findings. Clinical intuition would suggest that intensive, longer-term treatment is required for this condition. However, one study (Reference McIntosh, Jordan and CarterMcIntosh et al, 2005) recently reported that supportive clinical management was more effective (in adults) than two specialised and intensive forms of psychotherapy, although these authors now describe this as a specialist treatment (Reference McIntosh, Jordan and LutyMcIntosh et al, 2006). A further trial (Reference Lock, Agras and BrysonLock et al, 2005) found that a short course of family therapy appeared to be as effective as a long course for adolescents with short-duration anorexia nervosa. There was a suggestion, however, that those with more severe obsessive–compulsive thinking and non-intact families benefited from longer treatment. It is clear that emerging research findings are challenging established beliefs about the treatment of this condition and further clarification is required. There has been much recent interest in the importance of patient motivation and interventions aimed at improving it (Reference Vitousek, Watson and WilsonVitousek et al, 1998; Reference Geller, Cockell and DrabGeller et al, 2001), in order to overcome resistance or passive acceptance of treatment.
Together, these findings and the lack of evidence from systematic reviews suggest much uncertainty remains about effective treatment for this condition, although there is a growing literature challenging approaches delivered without the patient's active cooperation.
Strengths and limitations
This study is much larger than those reported in the literature to date and includes around four-fifths of incident cases known to child and adolescent mental health services in the north-west of England over a 3-year period. We achieved a high follow-up rate with demonstrably reliable outcome measures. The outcome of our individual CBT was poorer than reported for family-based treatment – a direct comparison is required on a similar population to clarify this further. Not all participants fully adhered to randomised treatment. It is, on the one hand a problem for long-term follow-up of RCTs of chronic conditions that some will subsequently engage in other treatments on clinical grounds. On the other hand, this provides an insight into use of services and enables evaluation of the outcome of step-up treatments.
Acknowledgements
This project is funded by the NHS (E) HTA programme, grant no. 97/42/02, and supported by the North West MHRN. Trial registry: ISRCTN39345394. They are responsible for approving the design and supervising the conduct of the study.
We thank the child and adolescent mental health services in the north-west of England who contributed to the project and especially the Young People's Centre Chester and the Adolescent Psychiatry Service, Prestwich. The following also made significant contributions: Dr Asha Bhatt Clinical Lead, Specialist Out-Patient Programme, Manchester; Sheeba Ehsan, Irene Cohen, Laura Rowlands, Dr Tania Stanway, Kandy Giles, Rachel Charlesworth, Matilda Moffatt and Sarah Bailey-Rogers.






eLetters
No eLetters have been published for this article.