Health professionals give information to carers to support them in their caring role (Department of Health, 2002), but the carer's need for information must be balanced with the service user's rights to privacy (Reference Szmukler and BlochSzmukler & Bloch, 1997). When carer involvement seems justified but the service user is withholding consent, professionals face an ethical dilemma between non-malificence (i.e. not doing harm, through failing to disclose) and beneficence (doing good, by respecting patient confidentiality) (Reference Furlong and LeggattFurlong & Leggatt, 1996; Reference Beauchamp and ChildressBeauchamp & Childress, 2001). This dilemma is especially complex in psychiatry (Reference Arksey, O'Mal ley and BaldwinArksey et al, 2002), where capacity to give informed consent may not be present, and where the relationship with the carer can in itself influence the course of the disorder (Reference Raune, Kuipers and BebbingtonRaune et al, 2004). Where consent is withheld, professionals may still need information from the carer for a full assessment, and carers retain the right to have their own needs assessed (Department of Health, 2000).
There is a lack of research-based evidence in this area. We therefore completed a national study with the aim of developing a framework for best clinical practice where service user consent for sharing information with their carer is withheld.
METHOD
Data presented here were collected as part of a UK study assessing mental health information-sharing practices across the life course, including children and adolescents, adults of working age and older people. The final report containing a more detailed methodological description is available at http://www.sdo.lshtm.ac.uk/sdo542003.html. The data presented here are focused on adults of working age with psychosis.
Study design
Data were synthesised from a consecutive policy review, a national survey of current practice and individual qualitative interviews. Each stage informed the next. The larger study also included facilitated stakeholder groups holding informal discussions and large group workshops, but these components did not address the subject of non-consent by people with psychosis, and so are not included in the analyses here. Multiple methods of data collection were used to allow triangulation – the use of different data sources to reach the results. Synthesising quantitative and qualitative methods is the right approach in an area characterised by a complex and often conflicting set of polarised beliefs from different groups: service users, carers and staff.
Three groups informed the design: a core research group (n=10), an expert panel who met three times (n=19) and a virtual panel who communicated electronically (n=14). Both panels comprised service users, carers, multidisciplinary professionals, carer support workers and academics. All groups contributed to the sequential stages of data collection, the analysis of the data and the development of emergent frameworks.
Setting and participants
Policy review
We collated policy documentation by surveying professional, service user and carer organisations, including the Mental Health Alliance (comprising 60 organisations) and the Care Programme Approach Association; directors of mental health trusts and social services in England; websites of professional and voluntary organisations; and international contacts.
Current practice survey
Electronic and paper surveys were developed in three different versions (service user, carer, and professional) and were piloted with relevant stakeholders (n=14). Each version comprised similar core questions (demographic details, experiences of information sharing, examples of good practice) and stakeholder-specific questions. The surveys were advertised through research partner organisations’ websites (n=13), group e-mails (n=7), promotion at conferences (n=5), targeted mailings (n=53), magazine advertisements (n=3), targeted promotion to Black and minority ethnic groups (n=5) and individual contacts from existing databases (n=290).
Individual qualitative interviews
Quota sampling was used to maximise representativeness, by balancing location, gender, ethnicity of participants and experience. Two researchers piloted and used an in-depth interview schedule for professionals, carers and service users to assess involvement in mental health; how confidentiality and information-sharing practices have affected roles; where information-sharing has worked well; issues in information-sharing; and how information sharing could be improved. Interviews were conducted by telephone (except for five, which were conducted face-to-face on request), and lasted 25–90 min. Detailed manual notes were made during interviews and these were typed immediately afterwards to provide an accurate record of the discussion.
Analysis
Policies were categorised using an existing framework (Surrey-Wide Operational Partnership Group in Mental Health, 1999) by one researcher, with a subsample categorised by a second researcher to check the coding accuracy. Quantitative differences between survey groups were assessed using the Statistical Package for the Social Sciences Version 12 for Windows. Qualitative survey responses were analysed using content analysis (Reference WeberWeber, 1990). Qualitative interview data were stored and managed using NVivo version 2 (http://www.qsrinternational.com). The transcripts were analysed manually, following good practice principles to identify emergent themes (Reference SilvermanSilverman, 2001). Four researchers generated a preliminary coding framework, which was then applied to the full data in NVivo by one researcher, with reliability checks carried out by two other researchers. The data presented in this paper are extracted from two interview analysis themes: information-sharing principles and information-sharing strategies.
Data from the three sources were used to produce an emergent framework for information-sharing when consent is withheld by people with psychosis. It was developed by clustering recommendations to remove duplicates, prioritising those generated from more than one source and/or those more strongly present (either numerically in the quantitative data, or as strength-of-theme data in either qualitative source), separating them into different points in the information-sharing pathway (e.g. obtaining consent, exploring decisions with the service user), developing a draft emergent framework, and then refining through feedback from the core research group, expert panel and virtual panel.
RESULTS
Policy
The review identified 56 policies and 35 supporting documents, although many included conflicting statements. Only 5 policies provided practical guidance on how to appropriately share information. Eleven policies (20%) specifically addressed information-sharing with carers: 5 from National Health Service trusts, 5 from carer bodies and 1 from the National Institute of Mental Health in England. Statutory sector policies emphasised professional responsibilities: to assess mental capacity and where present to seek the service user's consent to disclose personal information to the carer on a need-to-know basis; to review consent regularly; and to ensure accurate recording of information. Policies co-authored with carer groups also highlighted the use of advance statements to record preferences for crisis management (Reference Henderson, Flood and LeeseHenderson et al, 2004) and the promotion of inclusive approaches in respect of carers.
National survey
Survey participants comprised mental health service users (n=91), carers (n=329) and professionals (n=175). In the service user group 44 (48%) were male, 85 (93%) were White, 39 (42%) lived with their carer and 21 (23%) had been compulsorily detained in the previous year. In the carer group 64 (20%) were male, 309 (94%) were White, and 161 (49%) lived with the service user. Professionals included 66 (38%) psychiatric nurses, 29 (17%) social workers, 23 (13%) psychiatrists and 16 (9%) psychologists. Work settings comprised community teams (n=92; 53%), in-patient units (n=47; 27%), day care (n=26; 15%) and primary care (n=10; 6%). The combined sample provided 595 responses.
In the carer sample (n=329) the majority reported they were well supported in terms of access to ‘general information’. Ninety-two per cent understood the service user's diagnosis and 69% had access to sufficient ‘general information’ which they gained from voluntary sector organisations (49%), carer support groups (47%), other carers (35%), the internet (32%) and community psychiatric nurses (CPNs) (30%). A total of 186 carers (60%) had been given the opportunity to discuss the information they came across from a variety of sources with mental health professionals; these carers were significantly more likely to live separately from the service user (77% v. 87%, P=0.023) to be aged less than 61 years (74% v. 85%, P=0.023) and not be providing 24 h care, 7 days per week (86% v. 72%, P=0.002). Considering personal information, 261 (82%) stated they needed access to personal information in order to care both effectively and safely. The types of personal information required included details of whom to contact in a crisis (79%), possible future treatment options (68%), likely progress of the service user's mental health problems (65%), what the care plan says (59%), early signs of relapse (52%) and what treatments the service user is currently receiving (50%). In the previous year, 145 carers (46%) had received personal information to support their role and 171 (54%) had not. Table 1 shows that carers identified both professional practice and service user-based explanations for professionals not sharing personal information with them.
Carer perspectives on reasons why professionals did not share personal information (n=171)

| Number (%) of carers | |
|---|---|
| Personal information not shared with carer because: | |
| I have not asked for any | 59 (35) |
| Service user did not provide consent | 35 (21) |
| Service user was unable to give consent | 9 (5) |
| Service user was not asked to provide consent | 32 (19) |
| Patient confidentiality was given as the reason but without a supportive explanation | 47 (28) |
| Patient confidentiality was given as the reason but with a supportive explanation | 20 (12) |
| Don't know | 18 (11) |
| Specific comments: | 21 (12) |
| For example, ‘service user provides consent and then changes mind’; ‘out of respect for service user would like to know but respect their wishes so don't persist’; ‘carer is not next of kin’; ‘language barriers’ |
In the service user sample (n=91), more than half (59%; n=51 stated that their carers should have access to some personal information, with 47 (55%) reporting feeling ‘comfortable’ with their carer being involved and 47 (55%) believing carers should be offered separate time with professionals as a source of support. Service users and carers highlighted the absence of regular collection of consent to disclose authorisation – 51 (67%) of 76 service users with a named carer had not been asked to sign a disclosure consent form. Updating of consent authorisation was variable: 13 service users (14%) reported always being asked before information was disclosed, 19 (21%) sometimes, 20 (22%) rarely, 15 (16%) never and 24 (27%) did not know.
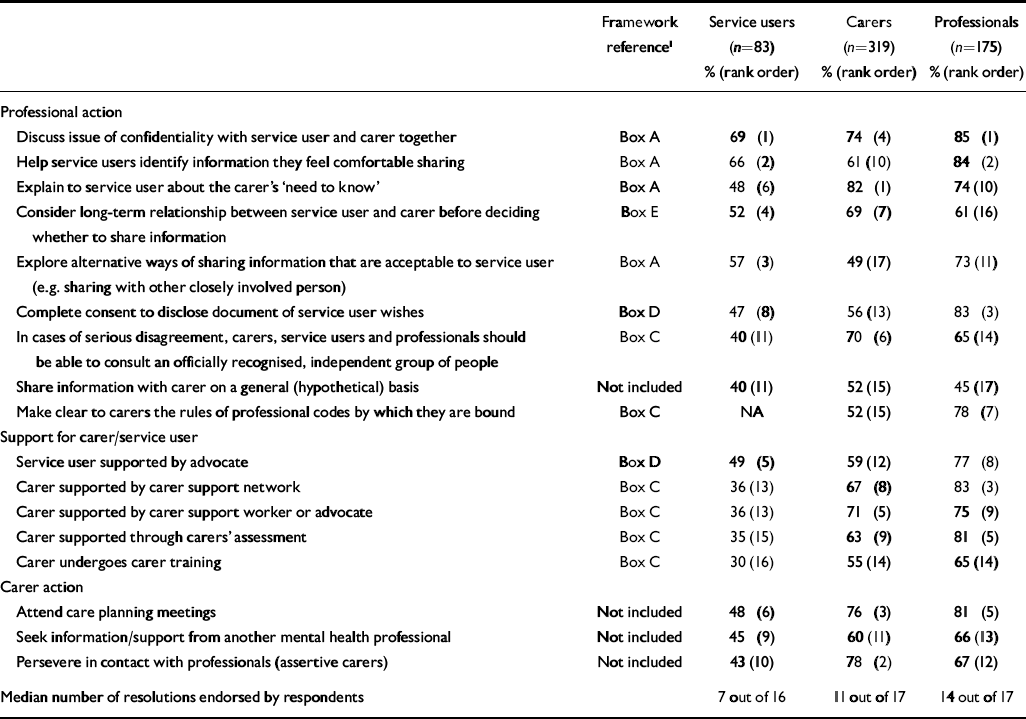
In the professional sample (n=175), half (50%) identified that their employer had a policy regarding sharing confidential information with carers. Among those with policies (n=88), 23% found these very helpful and 63% quite helpful. Professionals also identified why information is not shared with carers: 79% service user withheld consent; 55% carers not accessible; 48% they had insufficient time; 42% not asked service user for consent; 29% service user unable to provide consent; 23% service user lacked capacity to provide consent. Table 2 presents the perspectives of each stakeholder group on whether and when information should be disclosed without consent. Views on potential problem resolution strategies are shown in Table 3.
Stakeholder views of appropriate contexts for breaking patient confidentiality

| Service users (n=91) | Carers (n=326) | Professionals (n=175) | |
|---|---|---|---|
| Are there any occasions when information should be shared without service user consent? | |||
| Respondents (number stating there are occasions), n (%) | 59 (65) | 312 (96) | 170 (97) |
| Reason for breaking patient confidentiality and sharing information without consent, n (%) | |||
| When the service user is very unwell | 35 (59) | 274 (88) | 74 (44) |
| When the service user has agreed in advance | 40 (67) | 185 (59) | 114 (67) |
| If people are worried about the service user's safety | 37 (63) | 237 (76) | 132 (78) |
| If there are concerns about the service user harming other people | 35 (59) | 209 (67) | 152 (90) |
| If carer lives with service user | 14 (24) | 180 (58) | 40 (24) |
Endorsement of possible resolutions to information sharing problems
| Framework reference1 | Service users (n=83) % (rank order) | Carers (n=319) % (rank order) | Professionals (n=175) % (rank order) | |
|---|---|---|---|---|
| Professional action | ||||
| Discuss issue of confidentiality with service user and carer together | Box A | 69 (1) | 74 (4) | 85 (1) |
| Help service users identify information they feel comfortable sharing | Box A | 66 (2) | 61 (10) | 84 (2) |
| Explain to service user about the carer's ‘need to know’ | Box A | 48 (6) | 82 (1) | 74 (10) |
| Consider long-term relationship between service user and carer before deciding whether to share information | Box E | 52 (4) | 69 (7) | 61 (16) |
| Explore alternative ways of sharing information that are acceptable to service user (e.g. sharing with other closely involved person) | Box A | 57 (3) | 49 (17) | 73 (11) |
| Complete consent to disclose document of service user wishes | Box D | 47 (8) | 56 (13) | 83 (3) |
| In cases of serious disagreement, carers, service users and professionals should be able to consult an officially recognised, independent group of people | Box C | 40 (11) | 70 (6) | 65 (14) |
| Share information with carer on a general (hypothetical) basis | Not included | 40 (11) | 52 (15) | 45 (17) |
| Make clear to carers the rules of professional codes by which they are bound | Box C | NA | 52 (15) | 78 (7) |
| Support for carer/service user | ||||
| Service user supported by advocate | Box D | 49 (5) | 59 (12) | 77 (8) |
| Carer supported by carer support network | Box C | 36 (13) | 67 (8) | 83 (3) |
| Carer supported by carer support worker or advocate | Box C | 36 (13) | 71 (5) | 75 (9) |
| Carer supported through carers’ assessment | Box C | 35 (15) | 63 (9) | 81 (5) |
| Carer undergoes carer training | Box C | 30 (16) | 55 (14) | 65 (14) |
| Carer action | ||||
| Attend care planning meetings | Not included | 48 (6) | 76 (3) | 81 (5) |
| Seek information/support from another mental health professional | Not included | 45 (9) | 60 (11) | 66 (13) |
| Persevere in contact with professionals (assertive carers) | Not included | 43 (10) | 78 (2) | 67 (12) |
| Median number of resolutions endorsed by respondents | 7 out of 16 | 11 out of 17 | 14 out of 17 |
Content analysis of qualitative data provided in the surveys identified principles to underpin good information sharing practices. For service users (n=37) the key principles were establishing and maintaining better dialogue between all parties; routine collection of informed consent; positive attitude of professionals towards service users and carers; and flexible and creative approaches to information-sharing.
‘Don't talk without my permission. Don't talk without me being there. Advance directives – decide who can know what when we are well so that everyone knows what the boundaries are when we are in distress.’ (service user 21)
‘I find that where I have been explicitly asked what information it is okay to share and to agree that in a care plan, it has improved communications all round.’ (service user 67)
‘More consultation with carer who may be unaware of some of the problems experienced by mental health professionals with regard to confidentiality rules.’ (service user 122)
For carers (n=107), good practice principles were identified as carer proactivity; recognition of carers’ needs and rights; improved communication between all parties; improved professional attitudes towards carers; and collection of informed consent.
‘By the carer physically seeking appointments to get over the point that they need to be included all the time – this really works and the user learns to trust both carer and professional.’ (carer 307)
‘Generally, any resolution has come about because of reminding, pushing, and demanding on our parts. This should not be.’ (carer 100)
‘My son has frequently withdrawn consent for me to have information about him. His care team have gone to great lengths to explain to him exactly what they would tell me and why they feel I need to know it. Usually this works. When it doesn't (i.e. when he refuses) they revisit his decision regularly with him.’ (carer 99)
‘A lot is down to individuals.I cannot tell you what a difference it has made since a new CPN has taken over care for my son. I can phone her at any time and she follows this up with appropriate action.’ (carer 115)
Good practice principles identified by professionals (n=100) were maintaining dialogue and establishing effective communication; collecting consent; recognition of carers’ rights and ‘need to know’; and recognition of the carer role.
‘I have found joint policies between agencies very useful. Once explained, most carers appreciate that we have to work within a remit of respecting our client's right to confidentiality.’ (CPN 60)
‘Gaining consent in difficult and sensitive contexts is best practice.’ (social worker 36)
‘If you have received information from each side it is usually possible to raise relevant questions in a diplomatic way, at a joint meeting, to get issues out on the table in a positive fashion.’ (psychiatrist 41)
Individual qualitative interviews
The 24 interview participants comprised mental health service users (n=5), carers for people with severe mental illness (n=7), professionals (n=9) and carer support workers (n=3). Interviewees identified both governing principles and specific strategies to guide information-sharing. They emphasised the core role of individual judgement, relationships built upon openness, knowledge and trust, and the process of collecting informed consent. The importance and complexity of information-sharing decisions were highlighted by each stakeholder group.
‘Possibly the most important thing about [information] sharing is once you have, you can't change things. You only get one chance so it has to be right.’ (service user 1)
‘I think the information that carers need varies from one case to another. Professionals need to talk to carers about confidentiality. I have never come across a carer who knows their rights and the procedures involved in confidentiality. Carers need to be given sufficient information to do their job well.’ (carer 12)
‘[Black and minority ethnic] families are very distrusting of services. Having been in mental health for so long I can understand why. There's something about stigma. They are frightened to share information in case they are pre-judged. My approach has been about acknowledging their anger and distrust, and not being defensive about the services we offer.’ (carer support worker 2)
‘Every party wants to have their voice heard.’ (psychiatrist 1)
The service user interviews were dominated by one issue: the importance of patient confidentiality. All stressed how consent to disclose should be obtained before information is shared with carers. The requirement for consent was strongly linked to self-esteem, privacy, personal choice, independence, autonomy, general wellbeing and empowerment.
Carers accepted the service user's right to withhold consent, but (like service users) acknowledged this might have an impact on the standard of care they can provide. They emphasised the importance of information relevant to their support role, but did not need or want to know everything about the person supported. Carers viewed professionals as often lacking the confidence, empathy, skills, time and organisational backing to fulfil a carer support role alongside provision of health and social care treatment for the service user.
The perspectives of professionals on information-sharing were largely consistent with carers and service users in emphasising confidentiality; context of care (length of relationship, type of illness, stage of recovery, living arrangements, past history); mental capacity and consent; and establishing service user and carer confidence in professionals. In addition, professionals identified that they had a duty to assess risk, to avoid harm and to use professional discernment for decision-making. Appendix 1 provides illustrative quotations from each stakeholder group about patient confidentiality and stakeholder responsibilities.
Suggestions for good practice in information-sharing were made. Service user recommendations included effective communication, whereby all parties are kept informed of decisions; professional assessment of appropriate level of information-sharing; use of advance agreements; service improvements for both service users and carers, improving quality of care in mental health; and service user involvement in the local development of information-sharing guidelines and procedures. Carer recommendations included open and honest communication between stakeholders; improved recognition of the role of carers and their relevant knowledge; and a reduction in the perceived lack of engagement with or respect for those providing informal support. Professionals considered that an assessment of the carer's and service user's personal circumstances was a vital part of information-sharing with carers. Most professionals highlighted the benefits of bringing together parties to discuss care and treatment plans when an identified carer was involved. Community-based professionals were particularly aware of the importance of spending time separately with service users and carers.
Framework for best clinical practice when consent is not given to share information with carers

Framework for best clinical practice
Based on the above results, a framework for best practice was developed for information-sharing with carers where professionals are dealing with service user non-consent. A key distinction to emerge was between two types of information: general and personal. General information is defined as information that supports carers in their role, without providing new details specific to the service user. In contrast, personal information is new and specific to the service user. Whether information is general or personal is case-specific: providing information about schizophrenia would be general information if the diagnosis were known by the carer but personal information if it were not known. By distinguishing between general and personal information the framework emphasises that support and some information can be provided to carers without patient confidentiality being broken. For example, carers might need support to deal with being excluded from an information-sharing dialogue, usually as a consequence of the service user developing increased independence. Equally, service users may need support to involve carers within prescribed boundaries, while revisiting their non-consenting decision regularly.
Two levels of action were identified: organisational and clinical. Organisational actions are recommendations that require organisational planning and implementation, (see Appendix 2). Clinical responsibilities are actions that individuals working in mental health can take to support service users and carers through information-sharing. An emergent framework for best practice by clinicians is shown in Fig. 1. Contrasting opinions were found on questions such as whether information can ever be shared without consent, and whether carers should meet professionals without the service users being present. Therefore the best practice framework emphasises the central role of clinical judgement in decision-making.
DISCUSSION
This study found that there is not yet consensus in the UK as to best practice when service users refuse or give only partial consent to information-sharing with carers. However, it was possible to synthesise the identified good practice points into a clinically applicable framework for best practice. A central distinction to emerge was between general information and personal information.
Strengths and weaknesses of the study
Limitations include the self-selection of respondents, who may therefore not be representative. In particular, the sample included few people from Black and minority ethnic backgrounds. This means that any differences in perspective will not have been captured, which compromises the generalisability of the emergent framework. There were also difficulties in accessing policy documents. The identification of policy about carers was problematic given the lack of an agreed definition of a ‘carer’ – the term sometimes was used to include paid staff. The main strength of this study was the use of multiple sources of data. This was facilitated by active collaboration between researchers and relevant voluntary sector groups, with the intention of making participation in the study simple so as to minimise access barriers. Our multiple methods allowed for validation of themes, and the large set of respondents overall is also a positive feature.
The importance of support for carers
We heard from professionals, service users and carers about the importance of providing carers with timely and appropriate information. However, carers reported that in practice they experienced a lack of confidence, skills and organisational backing for staff to engage with them. This finding is consistent with other studies. For example, a qualitative study of 27 Australian primary carers found that lack of engagement by professional staff led to increased levels of distress among the carers, and left them feeling resentful and frustrated (Reference Wynaden and OrbWynaden & Orb, 2005).
Carers are likely to benefit from good information-sharing practices. Research by the mental health charity Rethink found that carers with access to information and support were likely to rate fewer adverse affects from caring, including mental or physical health problems, financial pressures, and impact on family relationships (Reference Pinfold and CorryPinfold & Corry, 2003). Furthermore, there are adverse clinical consequences for the service user where the carer is inadequately supported, since high expressed emotion in carers can predict relapse in psychosis (Reference Raune, Kuipers and BebbingtonRaune et al, 2004).
Implications for health and social care organisations
Policy documents on information-sharing practices in mental health must be translated into practice on the ground with the support of local organisational structures. Professionals reported that when policies on information-sharing were well published in the workplace they were useful documents. In particular such documents were helpful when they provided practical guidance on how to resolve information-sharing dilemmas, and when they outlined the legal and ethical boundaries of professional responsibility. The best practice framework (see Fig. 1) is recommended as an evidence-based and multiprofessional approach suitable for incorporation into local policy. Dissemination of collaboratively authored local protocols based on this framework to staff and through carer groups might improve practice in this area.
Other factors to consider include organisational barriers, such as insufficient time to work with carers and a professional tendency to avoid working with carers. Carers’ rights to a needs assessment provided one route to support the carer. All these considerations informed the development of the organisational checklist (see Appendix 2). The checklist is intended to be used as an audit tool for mental health services to monitor and improve their organisational approaches to supporting information-sharing with carers.
Implications for healthcare professionals
Dealing with situations in which service users do not consent to information-sharing poses clinical and ethical dilemmas. On the one hand, the training of health professionals is oriented towards patient confidentiality rather than information-sharing, and they are concerned to keep the trust of the service user (British Medical Association, 1999). On the other hand, legal rights to confidentiality are not absolute (Department of Health, 1995; House of Commons, 1998a , b ). Such complexity is not amenable to simple deterministic solutions, and clinical judgement must remain at the heart of decision-making in this area. This is particularly true when working with people with psychosis, whose capacity to provide informed consent can fluctuate, and the process – as opposed to the event – of providing consent requires continuity of care and strong therapeutic relationships.
The development of an empirically justified best practice framework is important for several reasons: first, to ensure that there is a shared understanding between service users, their carers and professionals about the centrality of service user consent, and the situations in which it can be justified to share information without consent; second, to highlight that carers can be supported even when consent is not given for sharing of personal information; and third, to support professional accountability in clinical practice.
For healthcare professionals, several strategies emerged. A change in attitude towards carers is indicated, to value more fully the carer's role. Ongoing communication with both patient and carer is vital, covering the aspects in Boxes A–D in Fig. 1. Fluctuating mental capacity – a problem not restricted to psychiatry (Reference Raymont, Bingley and BuchananRaymont et al, 2004) – means that advance statements and regular review of consent should be routine practice.
General information that builds on the carer's existing knowledge can always be shared without consent, so the distinction between general and personal information needs to be understood by service users, carers and professionals. Clinical skills are also needed to identify what the carer already knows before any information is disclosed: what would be general information (which can be shared without considering consent issues) and what would be personal information (where consent needs to be considered) for this carer? Supportive communication with carers is desirable, even when consent for personal information-sharing has not been given. Clinical strategies might include viewing non consent as a positive indicator of recovery and increased autonomy; emphasising that the refusal of consent is the current stance of the service user which will be regularly reviewed by the clinician; and providing as much general information as possible.
Future research
The benefits and difficulties for both carers and service users of dealing actively with situations in which information-sharing consent is withheld could be investigated. There is evidence that when the need of carers for timely and appropriate information to fulfil their role is met, they experience lower carer burden (Reference Pinfold and CorryPinfold & Corry, 2003). Interventions targeted at reducing expressed emotion have been developed to support families, including carer education and psychosocial services (Reference Barrowclough, Tarrier and LewisBarrowclough et al, 1999; Reference Szmukler, Kuipers and JoyceSzmukler et al, 2003). In part, these interventions involve the provision of information to help the carer interpret the service user's behaviour in ways that do not lead to criticism or emotional overinvolvement. It is plausible that better information-sharing is one of the active ingredients of the intervention. Future research should investigate whether the best clinical practice framework leads to a more positive impact of caring on the carer and reduces relapse rates by lowering expressed emotion.
Sharing information with carers is a complex process which is increasingly an international focus of policy (Department of Family and Community Services, 1999) and research (Reference Marshall and SolomonMarshall & Solomon, 2000). The joint interests of service users and their carers are best balanced when clinical judgement about the individual context remains central to balancing the implications of sharing or of not sharing information.
APPENDIX 1
Stakeholder views on patient confidentiality in practice
Service user perspective
‘I can see it [patient confidentiality] is a difficult issue for carers, but there is also the problem of involvement of the carer if the service user finds it unhelpful or distressing. I know there is a lot of talk about abuse but it doesn't have to be that extreme. Whether the relationship is happy, healthy, harmonious at a particular traumatic time or not, if carer involvement is not welcomed this needs to be addressed.’ (service user 4)
‘I definitely think that the service user should be the one to have the final say on how much information to share if they have the capability.’ (service user 1)
‘I am fond of advance directives, I think they are a very good idea. Everyone should have a statement for for when or if they are ill again. This would mop up all the issues, and should help a carers involvement as well.’ (service user 5)
Carer perspective
‘I have a reasonable relationship with my son, I always seek his permission first before I look at his care plan or medical notes. I agree with patient consent as I would not be happy for my son to know information about me without my consent.’ (carer 12)
‘When the service user doesn't want the carer involved they need to know that when they leave hospital and expect care, the carer can't provide the best service without the relevant information.’ (carer 13)
‘If the carers don't have the full knowledge this is very dangerous. You cannot care fully unless you have full knowledge, mistakes will be made and this could be harmful.’ (carer 14)
Professional perspective
‘I think there are times when you really want to tell relatives about the patient's behaviour. Sometimes you have to say, “I can't let you go home [from hospital] unless I tell them this.”’ (consultant psychiatrist 26)
‘The capacity of the patient to make decisions is the key factor in determining what information is shared with others.’ (psychiatrist 39)
‘Risk drives information sharing in mental health.’ (social work manager 33)
‘Often my role in hospital would be explaining rights to people, giving a factual explanation about legal aspects rather than sensitive information. But if they were asking me to confirm something I would still be guarded and not to be seen to be confirming to avoid breaches of confidentiality and the patient coming back to me. A lot of health staff have this attitude.’ (approved social worker 28)
APPENDIX 2
Organisational actions to support information-sharing with carers
-
▪ Positive approach towards working with carers, including a programme of support, e.g. carers’ assessments, information resource packs, carer involvement opportunities.
-
▪ Easy access to information sharing policy document and implementation guidelines which have been developed in partnership by mental health professionals, service users and carers.
-
▪ ‘Know your rights’ resources available for carers in a language of their choice
-
▪ Training for mental health professionals on how to work effectively with carers, including guidance on information-sharing.
-
▪ Specific training for dealing with situations where the service user withholds full or partial consent to share information, e.g. using the best clinical practice framework (Fig. 1).
-
▪ Acknowledgement of the complexity of information-sharing decisions and support structures to assist staff in applying professional discernment.
-
▪ Awareness of the culturally sensitive approaches required to support carers from diverse communities.
-
▪ Organisational validation of information-sharing, with carers being part of the clinical role.
-
▪ Develop and audit use of a system for collecting and reviewing ‘patient consent to disclose’ documentation and advance statements.
-
Develop and audit use of a system for recording what information has already been shared with carers, so that the distinction between general and personal information can be maintained.
-
Continuity of care for service users (and carers) which supports information-sharing practices through development of a strong therapeutic relationship and in-depth in-depth knowledge of caring context.
-
Promotion of effective, open and honest communication between professionals, carers and service users.
-
Carer's needs assessment process includes consideration of information needs.
Acknowledgements
This research was a collaboration between the Institute of Psychiatry (King's College London) and Rethink. We thank the research participants, panel members, and all the organisations who supported the study. The study was funded by the NHS Service Delivery and Organisation Research and Development Programme. The views expressed are those of the authors.






eLetters
No eLetters have been published for this article.