This is the final paper in a series addressing the practical application of cognitive–behavioural therapy (CBT) in clinical settings. The first two papers (Reference Williams and GarlandWilliams & Garland, 2002a; Reference Wright, Williams and GarlandWright et al, 2002) describe the Five Areas Assessment model and its application. The third (Reference Williams and GarlandWilliams & Garland, 2002b) discusses how to identify and challenge extreme thinking, and the fourth (Reference Garland, Fox and WilliamsGarland et al, 2002) discusses overcoming problems of altered behaviour (reduced activity and avoidance) using CBT.
This article gives an overview of issues involved in the delivery of psychotherapeutic interventions, not just within specialist services but also in busy everyday clinical practice. It examines some key papers on clinical effectiveness. Because of the very large range of topics that could be covered, only depression is discussed in detail here. The purpose is not to provide a systematic review of all outcome data but rather to point to sources where such information is available and to examine areas such as service delivery and training needs that have been largely overlooked in existing reviews.
The history of psychological therapies has been marked by a lack of well-designed outcome studies accompanied by the reluctance of many psychotherapists to adopt ideas such as diagnosis and disagreements about the nature or importance of outcome measures and, sometimes, of the benefits of evidence-based approaches. This situation has altered radically with the increased use of cognitive–behavioural therapy (CBT) treatments, which are based on the scientist–practitioner model and routinely gather outcome data. CBT and other psychotherapeutic approaches committed to the importance of evidence-based practice are better placed than most psychotherapies to point to a range of studies that evaluate their approach.
Evidence for the effectiveness of CBT in depression
A recent key document in this area is the Department of Health's review Treatment Choice in Psychological Therapies and Counselling (Department of Health, 2001). These guidelines summarise evidence-based information that can aid decisions about which psychological therapies are most appropriate for which patients. This is the most comprehensive review and appraisal of psychological treatments since the review by Reference Roth and FonagyRoth & Fonagy (1996).
The review group concentrated on the following common mental health disorders: depression, including suicidal behaviour; anxiety, panic disorder, social anxiety, phobias; post-traumatic disorders, eating disorders; obsessive–compulsive disorder; personality disorders, including repetitive self-harm; chronic pain, chronic fatigue, gastrointestinal disorders (irritable bowel syndrome) and gynaecological presentations (premenstrual syndrome).
All the established psychotherapeutic modalities were included in the review: cognitive and behavioural treatments; psychoanalytic therapies (focal and long-term); systemic therapy (family therapy); eclectic therapies (pragmatic treatments tailored to the individual); integrative therapy (formal theoretical and methodological integration of, for example, behavioural, cognitive and humanistic approaches, e.g. in cognitive–analytic therapy); other psychotherapies (e.g. existential, humanistic, feminist, personal construct, art therapy, drama therapy).
The aim of the Department of Health's review was to provide a clear summary of the evidence for the effectiveness of psychotherapy and counselling for people with particular diagnoses. It also reviewed the evidence of the impact of other factors on therapy outcome, including comorbidity, chronicity, severity, demographics, family situation, attitude to therapy, therapeutic alliance, and the setting and process of treatment. The review addressed treatments for adults only and specifically excluded children, those who misuse substances and those with schizophrenia. We identify below a number of complementary papers addressing these issues.
Identifying the evidence
The Department of Health group found papers by searching the Cochrane database for reviews, and identifying published reviews that satisfied criteria for high-quality evidence (Box 1).
Box 1 Criteria for assessing the quality of reviews (after Reference Oxman and GuyattOxman & Guyatt, 1988)
Were questions and methods clearly stated?
Were comprehensive search methods used?
Were explicit methods used to determine articles to include in the review?
Was the validity of primary studies assessed?
Was assessment of the primary studies reproducible and free from bias?
Was variation in the findings of the relevant studies analysed?
Were the findings of the primary studies combined appropriately?
Were reviewers’ conclusions supported by the data cited?
In total, 217 published reviews were identified for the years 1990–1998. Because the review papers alone could not answer some of the group's questions, further papers were collected on a non-systematic basis. Finally, expert consensus meetings were held to discuss the findings.
Key review papers in depression
Five reviews with high-quality evidence were identified for the guidelines’ estimation of the effectiveness of psychological therapies for depression (Table 1). The between-group effect sizes (treatment v. control) varied between 0.49 (Reference Robinson, Berman and NeimeyerRobinson et al, 1990) and 1.56 (Reference Gaffan, Tsaousis and Kemp-WheelerGaffan et al, 1995).
Linking evidence to recommendations
The guidelines used the classification and rating system shown in Box 2 to grade the strength of recommendations on the basis of established categories of evidence.
The main recommendations
Which therapies have evidence that they work?
The Department of Health group concluded that there is good evidence supporting the effectiveness of psychological therapies in the treatment of depression in general adult and older adult populations, including in-patient care. Cognitive therapy and interpersonal therapy proved to be effective treatments for depression, and a number of other brief structured therapies such as psychodynamic therapy showed some possible benefit, as did other forms of psychological therapy, including focal psychodynamic therapy, psychodynamic interpersonal therapy and counselling.
Contrary to recent commentaries on the review which suggest that there is an overwhelming endorsement for the use of CBT approaches alone (Reference HolmesHolmes, 2002), the guidelines actually point out that there is some evidence for the efficacy of other modalities such as behavioural therapy, problem-solving therapy, group therapy and marital and family interventions in the treatment of depression (Table 2). They also suggest that CBT approaches might be of superior efficacy compared with other brief therapies. However, it should be noted that most direct comparison studies between the types of therapy fail to show significant differences. The review also found that very little of the research considered the cost-effectiveness of the services provided.
Box 2 Evidence classification and rating system
Category of evidence
Ia From meta-analyses of RCTs
Ib From at least one RCT
IIa From at least one controlled study without randomisation
IIb From at least one other type of quasi-experimental study
III From descriptive studies (e.g. comparative, correlation and case–control studies)
IV From expert committee reports or opinions, or clinical experience of repeated authority or both
Ratings for strength of supporting evidence
A Directly based on Category I evidence
B Directly based on Category II evidence or extrapolated from Category I evidence
C Directly based on Category III evidence or extrapolated from Category II evidence
D Directly based on Category IV evidence or extrapolated from Category III evidence
The Department of Health group also reviewed the evidence for other factors that influence the psychotherapeutic process. It reports that, in general, gender and age have not been shown to affect outcome in depression; neither was any outcome effect observed for differences in length of treatment. It concludes that the evidence pertaining to the effect of the severity of depression on outcome is, in the main, descriptive rather than experimental and that the results have been equivocal.
Which therapies have no evidence that they work?
The guidelines report that eclectic, counselling and psychodynamic therapies are not presently supported by high-quality research evidence, even though they are commonly offered in National Health Service (NHS) practice (Department of Health, 2001: p. 40). When referring specifically to the treatment of depression, the guidelines do conclude that there is some evidence of effectiveness for psychodynamic interpersonal therapy and non-directive counselling in primary care. Research into eclectic therapy is difficult because of the practice of standardising treatment approaches in trials. The absence of high-quality evidence raises the challenge of how to complete well-designed outcome studies in these areas.
What makes a psychosocial intervention effective?
Effective psychosocial interventions tend to share certain characteristics by providing:
-
(a) a clear underlying model/structure/plan for the treatment being offered;
-
(b) a focus on current problems of relevance to the patient;
-
(c) delivery that is based on an effective relationship with the practitioner.
These are factors shared by the psychotherapies identified as having a strong evidence base, including CBT, problem-solving, interpersonal psychotherapy, group therapy, and marital and family interventions.
Filling the gaps
Additional useful reviews
Table 3 lists some recent reviews of the research evidence on the effectiveness of psychotherapeutic interventions that are not included in the Department of Health's (2001) guidelines. Some of these address areas that, for the sake of brevity, were not addressed by the Department of Health group. Others give a detailed description of the research carried out for a particular form of affective disorder. Finally, there are reviews of areas discussed in the guidelines but covered here in much more detail and including recent work not available to the group.
Reference PaykelPaykel (2001) concentrates on the evidence for psychological therapies, including CBT, in the treatment of patients with chronic and recurrent depressive disorder – the type of patient seen by psychiatrists. Although there is some evidence for a preventive effect of CBT after the acute treatment of depression (Reference Evans, Hollon and De RubeisEvans et al, 1992), this has not always been observed.
More recently, studies have begun to address the specific treatment of residual depressive symptoms using CBT. The largest such study to date is a controlled trial of 158 patients with residual symptoms after an episode of major depressive disorder (Reference Paykel, Scott and TeasdalePaykel et al, 1999; Reference Scott, Teasdale and PaykelScott et al, 2000). All participants continued on antidepressant medication but some also received cognitive therapy. The latter group had a relapse rate of 29%, compared with 47% in the group that was not given cognitive therapy. Significant differences were also observed in the proportion in each group that achieved full remission, although the effect was not as dramatic as that seen in the reduction in the rate of relapse. Reference PaykelPaykel (2001) concludes that cognitive therapy therefore appears to have a specific indication as a continuation or maintenance therapy for relapsing and recurring depression, particularly in the presence of residual symptoms and in conjunction with medication. He finds that other psychological therapies have less evidence to support them in this role.
In a study of 650 patients with chronic depressive disorder Reference Keller, McCullough and KleinKeller et al(2000) also found a greater remission rate in the patients who received both an antidepressant medication and a modified form of CBT (42%) compared with either treatment on its own (22–24%). It should be noted, however, that over 20% of these patients had not received treatment for their depression before inclusion in the study.
By following up a cohort of patients seeing a psychiatrist over 2 years, Reference Cornwall and ScottCornwall & Scott (1999) examined the factors that predict whether an individual with major depression will have a full or only a partial response to medication and hospitalisation. They noted that residual symptoms of depression remained in significant numbers of those who had received adequate doses of antidepressant medication for a sufficient period of time. Thus, some patients do not fully recover with medication alone. This group tended to have significantly lower levels of self-esteem. Over the 2-year period, they also tended to judge their levels of depression as worse than the ratings made by the professionals. This divergence of self-ratings and professional ratings suggested to Cornwall & Scott that the persistence of depressive symptoms might be evidence of Reference TeasdaleTeasdale's (1988) hypothesis that some individuals ‘get depressed about being depressed’. This causes a feedback loop in which the depressive symptoms and the secondary beliefs maintain each other. Cornwall & Scott suggest, therefore, that CBT might have a special role in partial responders by both helping to alleviate the biological symptoms of depression through behavioural interventions such as increased activities and also addressing the maintaining beliefs.
Barkham & Hardy's review (2001) suggests that considerable headway has been made in securing the evidence base for counselling and interpersonal therapies. Nevertheless, the research evidence for counselling does appear to be more equivocal than the findings for CBT. However, the counselling approach is very important in UK health care, as it is the most common form of psychological therapy delivered in primary care, with one-third of general practices in England and Wales employing a full-time counsellor for mental health problems (Reference Sibbald, Addington-Hall and BrennemanSibbald et al, 1993). It therefore represents the most commonly prescribed psychological treatment for depression in Britain. Despite this, its use has been criticised because of the paucity of research supporting its effectiveness in this role. A recent illustration of this was the study in Derbyshire, UK, by Reference Simpson, Corney and FitzgeraldSimpson et al(2000), which compared counselling and GP care for chronic depression with GP care alone. They found no benefit from adding the counselling to the usual GP interventions. This situation raises significant questions about how best to deliver services within the NHS.
What is not covered in the Department of Health review
How best to deliver services
The Department of Health guidelines provide a useful synthesis of the current evidence for different psychological therapies. What they do not aim to address, however, is how to deliver these services, merely stating that ‘nowhere is the gap between research and practice wider than in this field’ (Department of Health, 2001). This is clearly true of the way that CBT services are offered.
In their key paper concerning effective service delivery models, Reference Lovell and RichardsLovell & Richards (2000) present Multiple Access Points and Levels of Entry (MAPLE). They ask us to question why we do what we do within mental health services. They argue that because CBT treatments are short term and evidence based they are greatly in demand, yet there are currently fewer than 800 practitioners in the UK accredited by the lead body for CBT – the British Association for Behavioural and Cognitive Psychotherapies (BABCP; http://www.babcp.com).
Traditionally, most services that deliver CBT do so within secondary or tertiary care situations that offer specialist CBT to a number of highly selected patients. The qualifying criteria for receipt of this treatment are therefore high, resulting in long waiting lists and limited access to treatment. Thus, these services appear to offer a high-quality and specialist service – but only to a few. Consequently, there is a huge unmet need in primary and secondary care and a mismatch of demand and supply that results in frustrations for patients and their referring practitioners. Lovell & Richards argue that ‘services characterised by 9–5 working, hourly appointments and face-to-face therapy disenfranchise the majority of people who would benefit from CBT’. Not only do such services fail to provide access to treatment; they also fail to offer CBT in line with the available evidence. In short, although CBT is an evidence-based form of psychotherapy, we tend to deliver it in services that are themselves not evidence based.
Failure to provide evidence-based delivery
By tradition, CBT is offered for 12–16 1-hour sessions within specialist units. Lovell & Richards argue that services have adopted this model on weak grounds: there is no convincing evidence base supporting the need for 1-hour sessions or for 12–16 weeks of treatment. They claim that this format is traditional and convenient rather than evidence based. In contrast, there is an evidence base for offering shorter, more focused treatments and self-help. For example, a significant number of meta-analyses support the effectiveness of structured CBT self-help materials. Four such reports gave overall treatment effect sizes for self-help approaches of: 0.76 immediately after treatment and 0.53 at follow-up (Reference Gould and ClumGould & Clum, 1993); 0.82 post-treatment (Reference CuijpersCuijpers, 1997); 0.57 immediately after treatment and at follow-up (Reference MarrsMarrs, 1995); 0.96 for self-administered treatments over controls and 1.19 for bibliotherapy with minimal therapy contact (Reference Scogin, Bynum and StephensScogin et al, 1990). Despite this, such treatments are rarely delivered by services in a formalised way.
Obsessive–compulsive problems and phobic disorders may be treated relatively quickly using simpler, focused ‘single-strand’ treatments such as progressive exposure (facing up to a fear in a planned, step-by-step way). Such treatments are as effective as traditional CBT (Reference Chambless and GillisChambless & Gillis, 1993). Reference Lovell and RichardsLovell & Richards (2000) suggest that multi-strand treatments such as ‘full’ CBT do not confer any benefit over single-strand treatments for these disorders. Reference Jacobson, Dobson and TrauxJacobson et al(1996) found a similar picture in depression, where many patients improve with behavioural activation alone. In their study, 150 out-patients with major depressive disorder were offered behavioural activation only, or behavioural activation plus work identifying and challenging negative thinking; a third cohort received ‘full’ cognitive therapy, including both behavioural activation and identifying and challenging extreme and unhelpful cognitions, as well as other CBT techniques. All three groups improved and the ‘full’ CBT treatment was not superior to the other two interventions either immediately after treatment or at 6 months.
Most improvement in CBT treatment occurs during the first eight treatment sessions, and further gains are relatively lower when treatment continues for more sessions (Reference Barkham, Rees and StilesBarkham et al, 1996). If this is the case, why does traditional CBT routinely often offer 12–16 sessions?
Lovell & Richards suggest that traditional services often fail to involve users and fail to provide the choice, accessibility and continuity of care that a flexible service should. The challenge is to consider alternative treatment delivery models and, especially, briefer treatments.
A related issue is the concept of maximum gains for minimum expenditure of limited clinical resources. The evidence base for the effectiveness of CBT is at its strongest in disorders such as anxiety, panic, phobias, obsessive–compulsive disorder and depression. However, these are disorders that, if present singly, frequently do not meet the qualifying criteria for CBT within a service that (often by choice) focuses on complex and chronic cases.
Providing evidence-based CBT in the NHS
Lovell & Richards (2000) argue for three broad levels of entry to CBT in the routine delivery of services. These levels should be flexible and accessible to a far more inclusive range of people than at present, addressing a wide range of mental health problems.
Level 1
Less-intensive treatments should be the first choice for the majority of patients. Treatments should routinely be initiated by the provision of brief therapies such as self-help delivered via structured computerised or written materials or telephone advice lines. Service-user groups such as Triumph over Phobia (http://www.triumphoverphobia.com), which base their support on the use of structured CBT self-help materials, also deliver this level of treatment.
Level 2
If patients have more severe or complex disorders or are at risk, more intensive therapist-guided care packages should be provided. Unless robust evidence shows that multi-strand or complex therapies are more effective, these second-level packages should be offered first. Typically, such a package would offer focused single-strand treatments, for example exposure treatments and planned increases in activity as a treatment for depression (behavioural activation).
Level 3
For more complex or treatment-resistant cases and those at risk, multi-strand specialist CBT could be offered by experts. Level 3 input is indicated when there is clear evidence that patients have not benefited from simpler focused single-strand packages or when such simpler approaches are inappropriate.
This approach fits with the ‘stepped care’ model, which suggests that patients respond differently to psychosocial interventions of varying type and intensity and that it is therefore sensible to provide a variety of interventions ranging from self-help to long-term individual treatment (Reference HaagaHaaga, 2000). This has the advantage of using health care resources wisely. However, a criticism of this approach is that many patients will not respond to simple interventions alone and, as a result, may be held back from receiving evidence-based treatment of the type they truly need. It is also possible that the shorter failed interventions adversely affect patients’ ability to benefit from more specialist interventions at a later date. These suggestions have important implications for service structure and delivery. Critical factors in this approach include a service's ability to offer a range of effective evidence-based treatments and adequate training of practitioners in these treatments. At present, CBT training is accredited by the Royal College of Psychiatrists for very small numbers of consultant medical psychotherapists, yet far more psychiatrists have received CBT training. Such training varies, from individual workshops to 1-year specialist postgraduate courses that lead to expert status and the possibility of BABCP accreditation. However, there is no structure currently available that specifically addresses the separate training needs of the three levels. The specialist 1-year courses such as those at Newcastle, South of Scotland, Oxford, Dundee and the Institute of Psychiatry in London address specialist Level 3 training needs (details available at http://www.babcp.com). To date, no courses aim to train practitioners to be competent and effective at Levels 1 or 2.
The relative lack of training in the use of Level 1 self-help materials is highlighted in the results of a recent national survey of the use of self-help by expert CBT practitioners (Reference Keeley, Williams and ShapiroKeeley et al, 2002). This found that, although almost 90% used self-help materials with their patients, only 36.2% of BABCP-accredited therapists had been trained in their use. Compared with those that had not received training, therapists that had been trained recommended self-help treatments to more patients per week and were significantly more likely to rate self-help as effective.
The three-level model of service delivery also involves other aspects of training: practitioners must be able to identify which patients will benefit from which approach and to make appropriate referrals. This will, perhaps, be as great a challenge as developing the services in the first place.
The SPIRIT course
The SPIRIT (Structured Psychosocial InteRventions In Teams) course has been designed to address the need to train practitioners to work effectively at Level 1 of CBT delivery. It aims to keep the strengths of the CBT model (its structure and focus on current clinical problems) in ways that build on the relationship with the practitioner and to support this delivery with structured CBT self-help materials that are used with the support of the health care practitioner.
Training needs vary depending on which level of CBT delivery is provided. The SPIRIT course (further details available from the authors on request) offers jargon-free training in cognitive–behavioural treatments to staff working within the health service. The aim of the training is to teach the CBT model in a pragmatic, user-friendly style (the Five Areas Assessment model has been described in previous APT articles: Reference Garland, Fox and WilliamsGarland et al, 2002; Reference Williams and GarlandWilliams & Garland, 2002a ,Reference Williams and Garland b ; Reference Wright, Williams and GarlandWright et al, 2002). Training is skills-based in certain focused areas of CBT (Level 1 working) and it builds on multi-disciplinary and multi-agency team-based working. It does not aim to make staff experts in CBT at Levels 2 or 3.
The SPIRIT course consists of ten 3½-hour training sessions for groups of up to 20 practitioners from any part of a single clinical service. The main goal of the course is to provide training in:
-
(a) focused clinical assessment and management using a CBT model to identify areas for change (Reference Williams and GarlandWilliams & Garland, 2002a ; Reference Wright, Williams and GarlandWright et al, 2002);
-
(b) helping the patient to identify and overcome extreme and unhelpful thinking (Reference Williams and GarlandWilliams & Garland, 2002b );
-
(c) helping the patient to identify and overcome reduced activity and unhelpful behaviours (Reference Garland, Fox and WilliamsGarland et al, 2002);
-
(d) helping the patient to use structured self-help materials effectively and safely (Reference WilliamsWilliams, 2001); for the materials used, which were developed as part of an NHS commission, see Reference WilliamsWilliams (2002);
-
(e) teaching patients practical problem-solving and assertiveness skills;
-
(f) teaching patients to overcome physical problems such as low energy and insomnia;
-
(g) addressing the effective use of antidepressants and relapse prevention techniques.
The course develops clinical skills for use in busy everyday clinical practice and uses a range of proven educational techniques:
-
(a) team-based small-group training
-
(b) supervised role-play
-
(c) a clinical supervision session at the beginning and end of each session
-
(d) an interactive skills-based CD–ROM produced by the Computer-Aided Learning in Psychiatry (Calipso) unit at the University of Leeds (http:// www.calipso.co.uk).
Delivering SPIRIT
The project has three steps.
Step 1
Selecting the trainers. These are the skilled practitioners who deliver the training to the clinical teams. They are chosen for their clinical credibility, experience in psychosocial interventions (not always CBT) and, importantly, skills in small-group skills-based training and clinical supervision.
Step 2
Training the trainers.
Step 3
Training delivery by the trainers.
The SPIRIT training course is currently being offered to all adult and old age psychiatry teams throughout Glasgow, UK. The training is multi-disciplinary and multi-agency and is offered to teams including both community and in-patient staff. Team training rather than individual training is used because of the observation that individuals often find it difficult on their own to make changes in their clinical work setting. A related difficulty is that clinical staff often work only within specific parts of the clinical service such as in-patient care, a community team or a day hospital (the consultant psychiatrist is one of the few exceptions to this rule). The problem is that staff sometimes fail to make the links between their own work setting and other aspects of the same sector service. The multi-disciplinary and multi-agency nature of the trainers and the trained breaks down barriers, enhancing the team-based approach, developing a common language of assessment and encouraging collaborative team working.
How many staff can benefit?
There are currently eight trainers in Glasgow and they work in multi-disciplinary pairs to deliver the training. They offer the ten training sessions over a period of about 3 months and, at the end of the formal course, ongoing supervision sessions are offered for a further 3 months to support changes introduced by the individuals and the team. With up to 20 staff attending each course (as a closed group including up to four in-patient staff, for whom agency cover is provided, and 16 community team members) and running the course three times a year, a total of 208 staff (48 in-patient and 160 community staff) per year can receive training and ongoing supervision. A certificate of completion is offered to staff who achieve over 70% attendance.
Is the teaching effective?
The aim in Glasgow is to train over 200 staff by June 2003. During evaluation, the trainers examine subjective and objective knowledge, skills and team functioning, together with adherence to the training content of the course and measures of its acceptability and content. Analysis of the results for the first 78 attendees confirms statistically and clinically significant increases in overall subjective and objective knowledge and skills, with high ratings for the acceptability and content of training (Glasgow Institute for Psychosocial Interventions, 2002).
The challenge of achieving sustainable and relevant change should not be underestimated. Previous research has confirmed the great difficulties both of bringing about change in staff knowledge, attitudes and skills, and of maintaining change and confirming its effect on patient care (Reference King, Davidson and TaylorKing et al, 2002). The next stage of the SPIRIT project includes an analysis of the impact of change on staff care delivery and on patient outcomes.
Conclusions
The Department of Health's (2001) review brings together much of the best available evidence for the effectiveness of psychological therapies and counselling. The publication highlights the extensive evidence for the effectiveness of CBT for depression, both in a range of settings and compared with a number of other treatments. There is also strong evidence to support the effectiveness of other therapies, for example interpersonal psychotherapy, problem-solving, group therapy, and marital and family interventions. The psychosocial treatments such as counselling that are frequently offered within the NHS have far weaker evidence of effectiveness. In making service changes, health care planners should address the method of service delivery as well as deciding on the range of psychological therapies offered.
The implications for services and referring practitioners are that we need to consider how we can best deliver CBT and other evidence-based treatments in ways that are also evidence based and that allow the greatest access to the most people who may benefit. The MAPLE model of different levels of CBT treatment provides a useful structure that can inform such service delivery. However, this model creates new training needs and few practitioners are currently trained in Level 1 service delivery (self-help approaches). The aim of the SPIRIT course is to provide training in the appropriate use of selfhelp materials within an audited evidence-based training course.
Multiple choice questions
-
1 The following psychotherapy has a strong Category IA evidence base in the treatment of depression:
-
a cognitive–behavioural therapy
-
b interpersonal psychotherapy
-
c eclectic treatments
-
d integrative psychotherapy
-
e brief psychodynamic approaches.
-
-
2 The disorders/clinical problems covered by the Department of Health's (2001) guidelines include:
-
a depression
-
b schizophrenia
-
c generalised anxiety disorder
-
d post-traumatic stress disorder
-
e eating disorders.
-
-
3 Characteristics of evidence-based psychosocial interventions are:
-
a longer individual sessions
-
b the use of a clear therapeutic model
-
c a focus on current clinical problems
-
d the delivery of individual rather than group treatments
-
e the relationship between the practitioner and the patient.
-
-
4 A strong evidence base exists supporting the delivery of CBT:
-
a to waiting-list patients
-
b using structured self-help materials
-
c only as hourly sessions
-
d with 12–16 sessions providing the optimal response
-
e using different levels of treatment that can be delivered as appropriate.
-
-
5 The stepped-care model of treatment suggests that:
-
a no patients should be offered more complex care until they have been offered a simpler, more-focused treatment
-
b simpler, more-focused interventions may be as effective as more complex interventions
-
c most benefits in treatment are obtained in the first eight sessions
-
d patient selection is required to avoid demoralisation that can result from being offered inappropriate treatment
-
e all psychosocial care should be offered by trained experts in psychosocial intervention.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | T | a | T | a | F | a | T | a | F |
| b | T | b | F | b | T | b | T | b | T |
| c | F | c | T | c | T | c | F | c | T |
| d | F | d | T | d | F | d | F | d | T |
| e | T | e | T | e | T | e | T | e | F |
The studies addressing depression included in the Department of Health's (2001) review

| Reference | Focus of the review | Principal findings |
|---|---|---|
| Reference Gaffan, Tsaousis and Kemp-WheelerGaffan et al(1995) | Cognitive–behavioural therapy (CBT) v. other therapies; outcome measure: Beck Depression Inventory | CBT was superior to other psychotherapies, pharmacotherapy or control groups. The allegiance of the researcher to a model of therapy must be taken into account |
| Reference Gorey and CrynsGorey & Cryns (1991) | Group therapies for patients aged 65 and above. The majority had a cognitive, behavioural or psychodynamic focus | Group therapy gave significant improvement (between group effect size of 0.62), but 87% of the improvement was accounted for by non-specific factors. The types of therapy (CBT v. psychodynamic) were not operationalised, hindering comparisons between them |
| Reference Robinson, Berman and NeimeyerRobinson et al(1990) | Psychotherapies for depression, classifed as cognitive and/or behavioural, and ‘general verbal’ (which included psychodynamic) | The psychotherapies had superior results to waiting-list control, equivalent results to each other and to pharmacotherapy. Treatment v. control effect sizes varied between 0.49 (general verbal) and 1.02 (behavioural). The investigator's allegiance to a therapy had a substantial influence on results |
| Reference Scogin and McElreathScogin & McElreath (1994) | Psychological treatments for geriatric depression, classified as behavioural, cognitive, psychodynamic, reminiscence and eclectic. Delivered in group, self-help and individualised formats | Psychosocial treatments were shown to be effective. Between-group effect sizes (0.78–1.05) were comparable with those obtained by Reference Robinson, Berman and NeimeyerRobinson et al(1990) for younger populations. Psychosocial interventions each had similar effects, independent of whether the elderly patient had major depressive disorder or subclinical variety |
| Reference Stuart and BowersStuart & Bowers (1995) | CBT for depression in in-patients | Generally, the studies included showed CBT to be effective, both as a primary treatment and as an adjunct to anti-depressant medication. It is suggested that in-patient CBT can reduce symptoms, improve medication compliance and ease the transition to out-patient care |
Supplementary evidence identified in the Department of Health's (2001) review

| Reference | Focus of the review | Principal findings |
|---|---|---|
| Reference Shapiro, Barkham and ReesShapiro et al1994 | Compared psychodynamic interpersonal therapy and CBT | The treatments gave broadly similar and beneficial outcomes |
| Reference King, Sibbald and WardKing et al (2000) | Compared short-term effectiveness of CBT, non-directive counselling and general practitioner (GP) ‘treatment as usual’ (TAU) in a controlled trial of 464 patients in primary care. Participants could choose their form of treatment or consent to randomisation | At 4 months, the Beck Depression Inventory showed significantly superior clinical outcomes for CBT and counselling over GP TAU. Effect size for CBT = 1.73, that for counselling = 1.62. But at 12 months, there was no significant difference between the three treatments. Comprehensive costing data showed a consistent trend for higher costs with non-directive counselling, although cost differences between groups were not significant at either 4 months or 1 year |
| Reference Schulberg, Katon and SimonSchulberg et al(1998) | Studied efficacy of psychological treatments for depression in primary care from RCT data. Compared psychological treatments with pharmacotherapy | Time-limited depression-targeted psychotherapies are efficacious when transferred from psychiatric to primary care settings. There is a lack of evidence regarding the potential cost-offset of psychological treatments on medical costs and work productivity |
Review papers complementary to the findings of the Department of Health's (2001) guidelines on depression
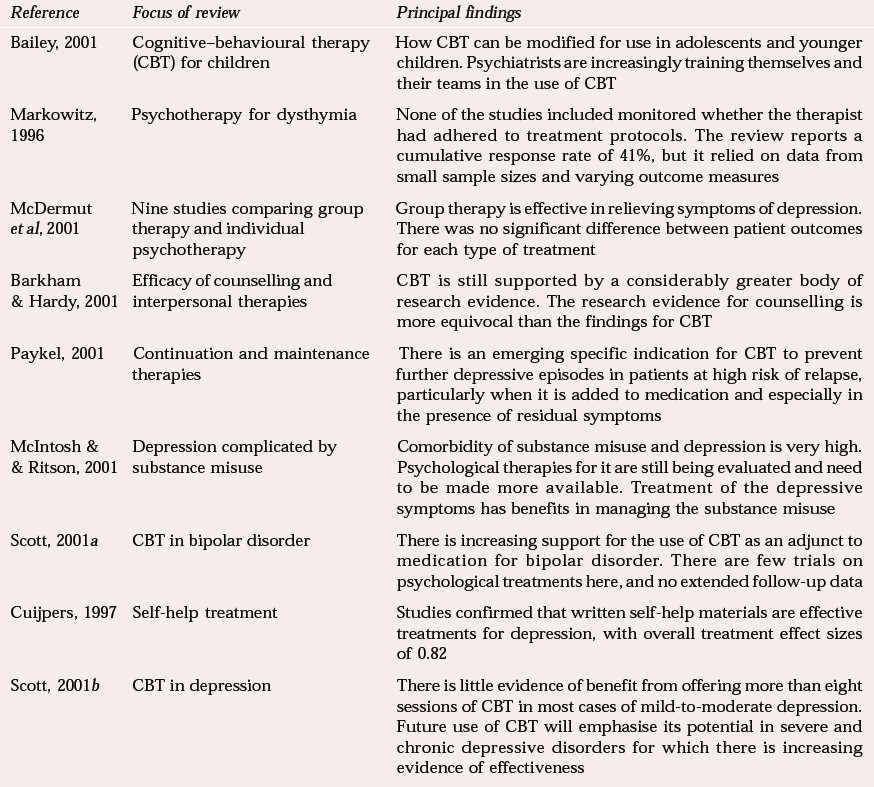
| Reference | Focus of review | Principal findings |
|---|---|---|
| Reference BaileyBailey, 2001 | Cognitive–behavioural therapy (CBT) for children | How CBT can be modified for use in adolescents and younger children. Psychiatrists are increasingly training themselves and their teams in the use of CBT |
| Reference MarkowitzMarkowitz, 1996 | Psychotherapy for dysthymia | None of the studies included monitored whether the therapist had adhered to treatment protocols. The review reports a cumulative response rate of 41%, but it relied on data from small sample sizes and varying outcome measures |
| Reference McDermut, Miller and BrownMcDermut et al, 2001 | Nine studies comparing group therapy and individual psychotherapy | Group therapy is effective in relieving symptoms of depression. There was no significant difference between patient outcomes for each type of treatment |
| Reference Barkham and HardyBarkham & Hardy, 2001 | Efficacy of counselling and interpersonal therapies | CBT is still supported by a considerably greater body of research evidence. The research evidence for counselling is more equivocal than the findings for CBT |
| Reference PaykelPaykel, 2001 | Continuation and maintenance therapies | There is an emerging specific indication for CBT to prevent further depressive episodes in patients at high risk of relapse, particularly when it is added to medication and especially in the presence of residual symptoms |
| McIntosh & & Ritson, 2001 | Depression complicated by substance misuse | Comorbidity of substance misuse and depression is very high. Psychological therapies for it are still being evaluated and need to be made more available. Treatment of the depressive symptoms has benefits in managing the substance misuse |
| Reference ScottScott, 2001a | CBT in bipolar disorder | There is increasing support for the use of CBT as an adjunct to medication for bipolar disorder. There are few trials on psychological treatments here, and no extended follow-up data |
| Reference CuijpersCuijpers, 1997 | Self-help treatment | Studies confirmed that written self-help materials are effective treatments for depression, with overall treatment effect sizes of 0.82 |
| Reference ScottScott, 2001b | CBT in depression | There is little evidence of benefit from offering more than eight sessions of CBT in most cases of mild-to-moderate depression. Future use of CBT will emphasise its potential in severe and chronic depressive disorders for which there is increasing evidence of effectiveness |





eLetters
No eLetters have been published for this article.