Introduction
Posttraumatic stress disorder (PTSD) is characterized by excessive fear responses to cues associated with a traumatic event. It is hypothesized that this is due to dysfunction in fear extinction, the process whereby fear response is gradually reduced after multiple exposures to a conditioned stimulus (CS) without reinforcement (Milad & Quirk, Reference Milad and Quirk2012; Zuj, Palmer, Lommen, & Felmingham, Reference Zuj, Palmer, Lommen and Felmingham2016). After a traumatic event, fear extinction is achieved by repeated exposure to reminders of the traumatic event without the feared outcome. This mechanism is suggested to be the basis of exposure therapy for PTSD and other anxiety-related disorders (Craske, Treanor, Conway, Zbozinek, & Vervliet, Reference Craske, Treanor, Conway, Zbozinek and Vervliet2014).
Fear extinction is not simply an erasure of fear but relies on new learning and memory. While the preponderance of studies does not show impaired extinction learning in PTSD (reviewed in Bottary, Straus, & Pace-Schott, Reference Bottary, Straus and Pace-Schott2023; Pace-Schott, Seo, & Bottary, Reference Pace-Schott, Seo and Bottary2023), accumulating evidence suggests that impaired retention of extinction memory, acquired after trauma exposure (Milad et al., Reference Milad, Orr, Lasko, Chang, Rauch and Pitman2008), may be a critical mechanism that leads to PTSD (Helpman et al., Reference Helpman, Marin, Papini, Zhu, Sullivan, Schneier and Neria2016; Milad et al., Reference Milad, Orr, Lasko, Chang, Rauch and Pitman2008, Reference Milad, Pitman, Ellis, Gold, Shin, Lasko and Rauch2009; Milad & Quirk, Reference Milad and Quirk2012; Shvil et al., Reference Shvil, Sullivan, Schafer, Markowitz, Campeas, Wager and Neria2014; Suarez-Jimenez et al., Reference Suarez-Jimenez, Albajes-Eizagirre, Lazarov, Zhu, Harrison, Radua and Fullana2020; Wicking et al., Reference Wicking, Steiger, Nees, Diener, Grimm, Ruttorf and Flor2016). Sleep supports the consolidation of different types of memories, which stabilizes and integrates them, and enhances their retrieval (Klinzing, Niethard, & Born, Reference Klinzing, Niethard and Born2019). Recent evidence suggests that this extends to extinction memory, with rapid eye movement sleep (REM) implicated as an important sleep stage involved in its consolidation (Davidson & Pace-Schott, Reference Davidson and Pace-Schott2020). In healthy people, more REM has been shown to be associated with better extinction recall (Bottary et al., Reference Bottary, Seo, Daffre, Gazecki, Moore, Kopotiyenko and Pace-Schott2020; Menz, Rihm, & Buchel, Reference Menz, Rihm and Buchel2016; Pace-Schott et al., Reference Pace-Schott, Tracy, Rubin, Mollica, Ellenbogen, Bianchi and Orr2014; Spoormaker et al., Reference Spoormaker, Sturm, Andrade, Schroter, Goya-Maldonado, Holsboer and Czisch2010), and REM deprivation leads to impaired extinction memory (Spoormaker et al., Reference Spoormaker, Schroter, Andrade, Dresler, Kiem, Goya-Maldonado and Czisch2012), suggesting the possibility of a causal role for this sleep stage. Several studies and meta-analyses find REM abnormalities in PTSD (Kobayashi, Boarts, & Delahanty, Reference Kobayashi, Boarts and Delahanty2007; Richards, Kanady, & Neylan, Reference Richards, Kanady and Neylan2020; Zhang et al., Reference Zhang, Ren, Sanford, Yang, Zhou, Zhang and Tang2019), which also have been shown to be associated with the risk of developing PTSD after trauma (Mellman, Bustamante, Fins, Pigeon, & Nolan, Reference Mellman, Bustamante, Fins, Pigeon and Nolan2002; Mellman, Knorr, Pigeon, Leiter, & Akay, Reference Mellman, Knorr, Pigeon, Leiter and Akay2004; Mellman, Pigeon, Nowell, & Nolan, Reference Mellman, Pigeon, Nowell and Nolan2007). Therefore, it is postulated that sleep disruption, specifically of REM, may predispose traumatized individuals to develop PTSD symptoms by interfering with extinction memory (Colvonen, Straus, Acheson, & Gehrman, Reference Colvonen, Straus, Acheson and Gehrman2019; Pace-Schott et al., Reference Pace-Schott, Seo and Bottary2023). Supporting this hypothesis, in a sample overlapping that of the current report, we showed that prefrontal activations during extinction recall were associated with REM density during the night before extinction recall (Seo et al., Reference Seo, Oliver, Daffre, Moore, Gazecki, Lasko and Pace-Schott2022). However, much remains to be learned regarding the association between REM and extinction memory in trauma-exposed individuals. One preliminary study (Straus, Norman, Risbrough, Acheson, & Drummond, Reference Straus, Norman, Risbrough, Acheson and Drummond2018) did not find any association of REM with extinction recall in PTSD; however, the small sample size (n = 13) may explain this negative finding. This study's sample was also limited to those with PTSD diagnoses and, therefore, did not provide insight into this association in individuals with subthreshold PTSD symptoms. To address this gap in knowledge, we examine here the association of REM measures on the night following extinction learning with extinction recall the following day, in a large sample of trauma-exposed individuals. We hypothesized that disruptions in REM sleep would be associated with impaired extinction recall (Hypothesis 1).
PTSD is characterized by abnormal autonomic nervous system function, including reduced parasympathetic nervous system (PNS) activity (Seligowski, Webber, Marvar, Ressler, & Philip, Reference Seligowski, Webber, Marvar, Ressler and Philip2022). PNS activity can be estimated by measuring heart rate variability (HRV), the variation in the interval between successive heartbeats. Specific HRV measures in the frequency (high frequency; HF-HRV) and time (root mean square of successive differences in the R–R interval; RMSSD) domains reflect control of heart rate by the vagus nerve, the main component of PNS outflow from the CNS (Laborde, Mosley, & Thayer, Reference Laborde, Mosley and Thayer2017; Shaffer & Ginsberg, Reference Shaffer and Ginsberg2017). Meta-analyses show that patients with PTSD display reduced vagal activity, as indexed by HF-HRV and RMSSD, during wakefulness (Chalmers, Quintana, Abbott, & Kemp, Reference Chalmers, Quintana, Abbott and Kemp2014; Ge, Yuan, Li, & Zhang, Reference Ge, Yuan, Li and Zhang2020; Schneider & Schwerdtfeger, Reference Schneider and Schwerdtfeger2020), and in one study, lower baseline HF-HRV predicted the severity of later post-traumatic stress symptoms (Pyne et al., Reference Pyne, Constans, Wiederhold, Gibson, Kimbrell, Kramer and McCune2016). Similar to wakefulness, a small number of recent studies in sleep find reduced vagal activity in PTSD (Kobayashi, Lavela, & Mellman, Reference Kobayashi, Lavela and Mellman2014), including in specific sleep stages (Daffre et al., Reference Daffre, Oliver, Nazareno, Mader, Seo, Dominguez and Pace-Schott2023; Ulmer, Hall, Dennis, Beckham, & Germain, Reference Ulmer, Hall, Dennis, Beckham and Germain2018). Additionally, in one study, HF-HRV across actigraphically measured sleep was associated with PTSD symptom severity (Rissling et al., Reference Rissling, Dennis, Watkins, Calhoun, Dennis, Beckham and Ulmer2016).
Vagally mediated HRV is considered to reflect the efficiency of the medial prefrontal cortex (mPFC) in inhibiting limbic subcortical structures (Thayer, Hansen, Saus-Rose, & Johnsen, Reference Thayer, Hansen, Saus-Rose and Johnsen2009), a process also critical for fear extinction (Giustino & Maren, Reference Giustino and Maren2015). Furthermore, converging evidence indicates that the vagus nerve contributes to emotional regulation and memory via its afferents to the brainstem nuclei, which in turn modulate the activity of multiple neurotransmitter systems and relevant brain regions within the central autonomic network, including the hippocampus, amygdala, and mPFC (Broncel, Bocian, Klos-Wojtczak, Kulbat-Warycha, & Konopacki, Reference Broncel, Bocian, Klos-Wojtczak, Kulbat-Warycha and Konopacki2020; McGaugh, Reference McGaugh2013). Consistent with these, high vagal tone is associated with better extinction learning in humans (Jenness, Miller, Rosen, & McLaughlin, Reference Jenness, Miller, Rosen and McLaughlin2019; Pappens et al., Reference Pappens, Schroijen, Sutterlin, Smets, Van den Bergh, Thayer and Van Diest2014; Wendt, Neubert, Koenig, Thayer, & Hamm, Reference Wendt, Neubert, Koenig, Thayer and Hamm2015), and enhancing vagal activity improves extinction learning and retention of extinction memory in both rodents (Noble et al., Reference Noble, Gonzalez, Meruva, Callahan, Belfort, Ramanathan and McIntyre2017, Reference Noble, Meruva, Hays, Rennaker, Kilgard and McIntyre2019b; Pena et al., Reference Pena, Childs, Willett, Vital, McIntyre and Kroener2014; Pena, Engineer, & McIntyre, Reference Pena, Engineer and McIntyre2013; Souza et al., Reference Souza, Powers, Rennaker, McIntyre, Hays and Kilgard2022) and humans (Burger et al., Reference Burger, Verkuil, Van Diest, Van der Does, Thayer and Brosschot2016, Reference Burger, Van Diest, Van der Does, Korbee, Waziri, Brosschot and Verkuil2019; Szeska, Richter, Wendt, Weymar, & Hamm, Reference Szeska, Richter, Wendt, Weymar and Hamm2020). In addition, a separate line of recent studies shows that vagal activity during sleep, as indexed by HF-HRV, independently contributes to memory consolidation over and above contributions by sleep architecture and sleep-related neural oscillations (Whitehurst, Cellini, McDevitt, Duggan, & Mednick, Reference Whitehurst, Cellini, McDevitt, Duggan and Mednick2016; Whitehurst, Subramoniam, Krystal, & Prather, Reference Whitehurst, Subramoniam, Krystal and Prather2022). However, to date, no study has examined the role of vagal activity in the sleep-dependent consolidation of extinction memory in any population. REM is characterized by activation in the aforementioned regions that regulate both vagal activity and fear extinction (Pace-Schott et al., Reference Pace-Schott, Seo and Bottary2023). We thus hypothesized that lower HF-HRV in REM during the night following extinction learning would independently predict lower extinction recall (i.e. consolidation of extinction memory) in trauma-exposed individuals (Hypothesis 2). If this hypothesis is supported, it would further underscore vagal activity as a promising target for enhancing extinction memory through readily accessible interventions (Jung, Yang, & Lee, Reference Jung, Yang and Lee2024; Siepmann, Weidner, Petrowski, & Siepmann, Reference Siepmann, Weidner, Petrowski and Siepmann2022) in the aftermath of trauma exposure.
Methods
Participants
A total of 139 participants, aged between 18 and 40, were recruited from the greater Boston metropolitan area using online and posted advertisements. All participants reported experiencing a DSM-5 criterion-A traumatic event (‘index trauma’) in the past two years, except within the last one month. Participants were allowed with a concurrent anxiety disorder, dysthymia, major depressive disorder (remitted or on a case-by-case basis), or if on a stable dose of an antidepressant (⩾8 weeks). Exclusion criteria included: history of chronic childhood abuse or neglect; PTSD diagnosis preceding traumatic event indexed at study interview; neurological disorder or injury; major medical disorders; psychotic, bipolar, autism spectrum, or other neurodevelopmental disorders; current drug or alcohol abuse or dependence; history of sleep disorder other than insomnia or nightmare disorder; current use of hypnotic or recently adjusted psychiatric medications; shift work; and any contraindication to MRI scans.
Twenty-six participants were excluded from all analyses because of missing or unusable EEG or ECG data (final n = 113). Psychiatric history was ascertained using the Structured Clinical Interview for DSM-IV-TR for Non-Patients (SCID-I/NP) (First, Gibbon, Spitzer, & Williams, Reference First, Gibbon, Spitzer and Williams2007). The Clinician-Administered PTSD Scale for DSM-5 (CAPS-5; [Weathers et al., Reference Weathers, Bovin, Lee, Sloan, Schnurr, Kaloupek and Marx2018]) was used to assess post-traumatic stress symptom severity (see online Supplementary Fig. S1 for its distribution in the sample). This study followed a Research Domain Criteria (RDoC) (Insel et al., Reference Insel, Cuthbert, Garvey, Heinssen, Pine, Quinn and Wang2010) design in which dimensional rather than categorical measures were targeted, and PTSD diagnoses were established post-hoc from diagnostic evaluations rather than by assigning subjects to PTSD and non-PTSD groups. 49.6% (n = 56) of participants met diagnostic criteria for PTSD. The Quick Inventory of Depressive Symptomatology, Self-Report (QIDS-SR) (Rush et al., Reference Rush, Trivedi, Ibrahim, Carmody, Arnow, Klein and Keller2003), and the Pittsburg Structured Clinical Interview for Sleep Disorders (SCID-SLD) (Stocker, Khan, Henry, & Germain, Reference Stocker, Khan, Henry and Germain2017) were administered to evaluate depressive and sleep disorder symptoms, respectively. Demographic and clinical characteristics of the final sample are displayed in Table 1. All participants provided written consent to participate in the study and were paid for their participation. All procedures were approved by the Partners Healthcare Institutional Review Board.
Demographic and clinical characteristics of the participants

CAPS-5, Clinician-Administered PTSD Scale for DSM-5; PTSS, Post-traumatic stress symptom; QIDS, Quick Inventory of Depressive Symptomatology.
Some of the data is displayed as mean ± standard deviation (minimum–maximum).
Procedures
Timeline of the study procedures are included in online Supplementary Methods (Fig. S2). Participants completed an approximately 2-week sleep assessment period during which they wore an actigraph (Actiwatch-2, Philips Respironics) and filled out a daily sleep and nightmare diary. Approximately midway through the 14-day period, they underwent a combined sleep-disorders-screening and acclimation night of ambulatory polysomnography (PSG) recording. This was followed by a ‘baseline’ overnight PSG recording. Starting in the evening immediately after the baseline night, participants completed a 2-day fear conditioning and extinction protocol with simultaneous fMRI recordings (Milad et al., Reference Milad, Furtak, Greenberg, Keshaviah, Im, Falkenstein and Wilhelm2013). Between fMRI sessions, participants completed a third (‘consolidation’) night of ambulatory PSG.
Ambulatory PSG
Ambulatory PSG was recorded on three nights using the Somte-PSG ambulatory sleep monitor (Compumedics USA, Charlotte, NC, USA). Sampling rate was 256 Hz. EEG data were acquired using six EEG channels (F3, F4, C3, C4, O1, O2; positioned according to the 10–20 system). Additional electrodes were placed on bilateral mastoids, above the right and below the left eye (EOG), under the chin (EMG), and below the right clavicle and in the left fifth intercostal space (ECG). Participants returned home to sleep after being instrumented. During the acclimation/screening (first) PSG night, additional channels for pulse-oximeter, respiration transducer belts, nasal cannula, and tibialis movement sensors were added to screen for obstructive sleep apnea (OSA) and periodic limb movement disorder (PLMD). No participant met criteria for clinically significant OSA or PLMD. All sleep records were scored by an experienced, registered polysomnographic technologist according to American Academy of Sleep Medicine criteria (Berry, Gamaldo, Harding, & Brooks, Reference Berry, Gamaldo, Harding and Brooks2015).
Fear conditioning, extinction learning, and extinction recall
A validated 2-day paradigm (Milad et al., Reference Milad, Wright, Orr, Pitman, Quirk and Rauch2007, Reference Milad, Furtak, Greenberg, Keshaviah, Im, Falkenstein and Wilhelm2013) was used to probe fear conditioning and extinction during ongoing fMRI recording. This protocol consisted of four phases, with habituation, fear conditioning, and extinction learning phases taking place on the first day and extinction recall 24 h later. During each phase, images of a colored desk lamp (red, yellow, or blue) appearing in a contextual background (office for conditioning context and conference room for extinction context) served as conditioned stimuli (CS). Context images were presented for nine seconds, with three seconds with the lamp off and six seconds with the lamp on (red, yellow, or blue). The unconditioned stimulus (US) was a mild (0.8–4.0 mA), 500 msec electric shock delivered to the index and middle fingers of participants' right hand using a Coulbourn Transcutaneous Aversive Finger Stimulator (Coulbourn Instruments, Allentown, PA). Prior to entering the scanner, participants were administered increasing intensities of shock and they each selected a level that they perceived as ‘highly annoying but not painful’. Prior to entering the scanner, MRI-safe 11-mm, Ag/AgCl skin conductance monitoring electrodes were attached to the participant's left palm. Skin conductance level (SCL) was continuously monitored at 37.5 Hz using the MP150 system with Acqknowledge 4.3 (BIOPAC Systems, Inc., Goleta, CA) software.
During habituation, all six possible combinations of lamp colors and contexts were presented across six trials. During the following fear conditioning phase, two of the three colored lamps (CS+) were each presented eight times paired with the US at stimulus offset, on a partial reinforcement schedule (five out of eight presentations were paired with US). The third lamp color, which was never paired with US (CS-), was interspersed among the CS + s for a total of 16 presentations. Fear conditioning was followed by extinction learning, during which one CS + (CS + E) was presented in the extinction context 16 times without the US along with 16 interspersed presentations of the CS−. The other CS+ remained conditioned but unextinguished (CS + U). During extinction recall, which took place 24 h later, each CS+ was presented eight times in the extinction context, with no US, along with 16 interspersed CS−.
During each phase, physiologic reactivity for each trial was indexed using skin conductance response (SCR), a measure of sympathetic activity (Dawson, Schell, & Filion, Reference Dawson, Schell, Filion, Cacioppo, Tassinary and Berntson2007), calculated as the mean SCL in microSiemens (μS) during the last 2 s of context presentation subtracted from the maximum SCL during the 6 s of CS presentation. Negative SCRs were coded as zero (Lonsdorf et al., Reference Lonsdorf, Menz, Andreatta, Fullana, Golkar, Haaker and Merz2017), and then all values were square root transformed. ‘non-conditioners’ were defined as those who exhibited less than two non-square-root transformed SCR responses to either of the two CS + s that were equal to or exceeding 0.05 μS during the Fear Conditioning phase (Orr et al., Reference Orr, Metzger, Lasko, Macklin, Peri and Pitman2000). Thirty-one non-conditioners were further excluded from SCR analyses based on these criteria. In addition, SCR data for three participants were lost.
Immediately following each phase except habituation, participants verbally reported shock expectancy for the first and last presentations of each CS (i.e. colored light) appearing in that phase on a scale from 1 (‘not expecting a shock at all’) to 5 (‘expecting a shock very much’). Ratings were obtained at this frequency with the goal of capturing the shift in expectancy from baseline to the end of the corresponding session. Expectancy ratings for seven participants were not included in the analyses, because they did not complete the experiment or because of missing data.
Extinction recall variables
To examine the association of physiologically expressed and subjective extinction recall with sleep and HRV measures, we used an extinction retention index (ERI) (Lonsdorf, Merz, & Fullana, Reference Lonsdorf, Merz and Fullana2019) and a subjective extinction retention index (sERI) (Bottary et al., Reference Bottary, Seo, Daffre, Gazecki, Moore, Kopotiyenko and Pace-Schott2020), respectively. ERI was calculated as: ([Average of the SCRs of the first 4 CS + E presentations at extinction recall phase/maximum SCR to the ‘to-be’ CS + E during the fear conditioning phase] × 100), which is one of the most commonly used formulae in the literature (Lonsdorf et al., Reference Lonsdorf, Merz and Fullana2019). Only the first four CS + E trials from the extinction recall phase were included in this calculation in order to avoid confounding recalled extinction with new extinction learning. Higher ERI reflected lower extinction memory. sERI was calculated as: Expectancy to the first CS + E in Extinction Recall/mean expectancy for the last of each CS + during Fear conditioning × 100. Larger sERI indicated lower extinction memory. Both ERI and sERI were formulated to quantify the degree of dominance for the putatively competing memories of extinction and fear (Lonsdorf et al., Reference Lonsdorf, Merz and Fullana2019).
Sleep measures
The PSG data analyzed in the present study were recorded during the consolidation night (the night between the extinction learning and extinction recall phases). For regression analyses, we selected the REM measures that have been associated with PTSD, including %REM (Zhang et al., Reference Zhang, Ren, Sanford, Yang, Zhou, Zhang and Tang2019), REM density (REMD) (Kobayashi et al., Reference Kobayashi, Boarts and Delahanty2007), REM latency (REML) (Mellman, Kobayashi, Lavela, Wilson, & Hall Brown, Reference Mellman, Kobayashi, Lavela, Wilson and Hall Brown2014), and REM fragmentation (REMF) (Breslau et al., Reference Breslau, Roth, Burduvali, Kapke, Schultz and Roehrs2004; Habukawa et al., Reference Habukawa, Uchimura, Maeda, Ogi, Hiejima and Kakuma2018; Insana, Kolko, & Germain, Reference Insana, Kolko and Germain2012; Lipinska & Thomas, Reference Lipinska and Thomas2019; Mellman et al., Reference Mellman, Bustamante, Fins, Pigeon and Nolan2002; Saguin, Gomez-Merino, Sauvet, Leger, & Chennaoui, Reference Saguin, Gomez-Merino, Sauvet, Leger and Chennaoui2021). Percent time spent in each sleep stage (%N1–N3, %REM) was computed as a percentage of total sleep time (TST). REMD is the number of rapid eye movements per minute of REM sleep and was calculated using an automatic algorithm (Yetton et al., Reference Yetton, Niknazar, Duggan, McDevitt, Whitehurst, Sattari and Mednick2016). REML was calculated as the number of minutes occurring after sleep onset before the first REM epoch. REMF was calculated as the average duration of REM segments (Mellman et al., Reference Mellman, Bustamante, Fins, Pigeon and Nolan2002). REM segments were defined as continuous REM from the start of at least 1 min of REM to the onset of at least 1 min of non-REM or wake (Mellman et al., Reference Mellman, Bustamante, Fins, Pigeon and Nolan2002).
Heart rate variability
HRV was calculated using Kubios HRV Premium software (Kubios Oy, Kuopio, Finland) in continuous REM ECG segments lasting at least 5 min during the entire night's sleep. Prior to analysis, ECG traces were visually inspected for physiological and technical artifacts (Laborde et al., Reference Laborde, Mosley and Thayer2017). Misplaced or ectopic beats were manually corrected if possible. Very low to low, or occasionally medium, filter was applied, if necessary, after correction (https://www.kubios.com/hrv-preprocessing/). Segments that did not provide reliable estimates due to excessive artifacts were removed. Twenty-three participants were excluded because of artifacts, not having ⩾5 min REM segments, or because their records were missing. High frequency (HF; 0.15–0.4 Hz) absolute power (HF[ms2]) was used as a predictor variable in the primary analyses because it was shown to be associated with sleep-dependent memory processing (Whitehurst et al., Reference Whitehurst, Cellini, McDevitt, Duggan and Mednick2016). We also carried out the same analyses with root mean square of the successive differences in the R–R interval (RMSSD), another measure of vagal activity (Shaffer & Ginsberg, Reference Shaffer and Ginsberg2017). For frequency domain analyses, an autoregressive method was used, with model order set at 16 (Laborde et al., Reference Laborde, Mosley and Thayer2017). Data were transformed by their natural logarithm (Laborde et al., Reference Laborde, Mosley and Thayer2017).
Statistical analyses
Associations were explored between extinction recall indices (ERI and sERI), and age, sex, months since index trauma, scores of symptom scales (CAPS-5 and QIDS), and medication use as a binary variable. For correlations, Pearson and Spearman's correlations were used depending on the distribution of variables. Student's t tests were used for comparisons between sexes and between medication users and non-users.
We used linear regression models to test whether REM sleep variables predicted extinction recall (ERI and sERI; Hypothesis 1). The models included %REM, REMD, REML, and REMF as predictor variables. Sex and medication use were also included as predictors as these factors have been shown to modulate fear extinction and its retention (Bouton, Kenney, & Rosengard, Reference Bouton, Kenney and Rosengard1990; Gunduz-Cinar et al., Reference Gunduz-Cinar, Flynn, Brockway, Kaugars, Baldi, Ramikie and Holmes2016; Milad et al., Reference Milad, Goldstein, Orr, Wedig, Klibanski, Pitman and Rauch2006).
Next, hierarchical regression analyses were used to test the hypothesis that vagal activity would improve the predictions of ERI and sERI above and beyond REM sleep measures alone (Hypothesis 2). For this purpose, two models were built. Model 1 included sex, medication use, and REM measures. HF[ms2] was added as an additional predictor in Model 2. Visual inspection of the data suggested that sex may be moderating the effect of HF[ms2] on ERI. Therefore, sex × HF[ms2] interaction was also added to the model for ERI. Because missing HF[ms2] data further limited the number of participants that could be included in the analysis, only REM variables that were significant predictors in the regression analysis that tested Hypothesis 1 were included. Results for the models that included all REM variables and RMSSD instead of HF[ms2] were also reported for completeness.
In all regression analyses, partial regression plots and a plot of studentized residuals against the predicted values indicated that assumptions of linear relationship were met. Variance inflation factors were within acceptable ranges (1.1–1.4), indicating that there was no confounding multicollinearity. Little's Missing Completely At Random (MCAR) test indicated that data was missing at random in our sample (χ2 = 84.253, DF = 71, Sig. = 0.135). For ERI, the distribution histogram and P–P plot of standardized residuals showed a non-normal distribution. In addition, plotting standardized residuals and predictors revealed heteroscedasticity. Therefore, ERI was log-transformed. After transformation, normal distributions of residuals and homoscedasticity were confirmed.
For all variables, outliers ± 3 standard deviations from the mean were removed. All analyses were two-tailed. The significance level for hypothesis testing (α) was set at 0.05.
Results
Association of extinction recall indexes with demographic and clinical measures
Age was inversely correlated with sERI (r s = −0.27, p = 0.006), while it was not significantly correlated with ERI (r s = 0.12, p = 0.305). There were no differences between sexes in ERI or sERI (t(76) = 0.233, p = 0.817 and t(104) = 0.116, p = 0.250, respectively). There were no significant correlations between either extinction recall index and the number of months since index trauma (ERI: r s = −0.03, p = 0.796; sERI: r s = −0.04, p = 0.659), or CAPS-5 (ERI: r s = 0.11, p = 0.333; sERI: r s = −0.02, p = 0.831) or QIDS (ERI: r s = 0.13, p = 0.350; sERI: r s = −0.04, p = 0.692) scores.
Regression analyses predicting ERI and sERI
Measures of REM characteristics and sleep architecture are displayed in Table 2. The multiple regression model with ERI as the dependent variable included sex, medication use, %REM, REMD, REML, and REMF as predictor variables (N = 67). The overall model explained a significant proportion of the variance (Adj. R 2 = 0.14, p = 0.021), with sex, %REM, REMD, and REML emerging as significant predictors (Table 3; online Supplementary Fig. S3). Poorer physiological extinction recall was associated with the male sex (B[s.e.] = −0.71[0.34], p = 0.041), less time in REM sleep (%REM; B[s.e.] = −0.06[0.03], p = 0.018), increased REMD (B[s.e.] = 0.14[0.05], p = 0.009), and shorter REML (B[s.e.] = −0.01[0.003], p = 0.002).
Sleep and HRV measures
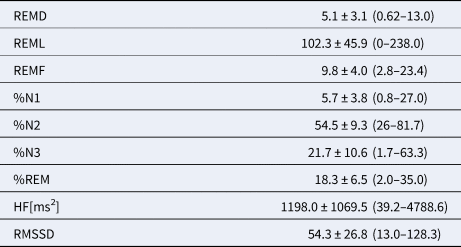

HF [ms2], absolute power of high frequency heart rate variability; %N1-REM, proportion of the sleep stage to the total sleep time; REMD, REM density; REMF, REM fragmentation; REML, REM latency; RMSSD, root mean square of the successive differences in the R–R interval.
Data is displayed as mean ± standard deviation (minimum–maximum).
Linear regression analysis for physiological extinction recall (ERI; N = 67)
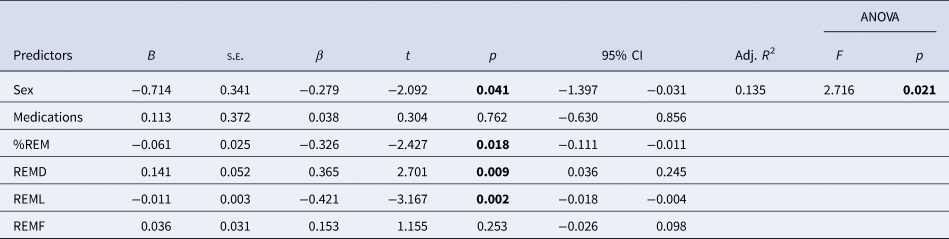
%REM, proportion of REM sleep to the total sleep time; REMD, REM density; REMF, REM fragmentation; REML, REM latency.
Sex, %REM, REMD and REML were significant predictors. Note that smaller ERI denotes better extinction recall.
A similar multiple regression model for sERI was carried out (N = 94). In our sample, age was associated with sERI (see above), therefore it was also included in the model. This model also explained a significant proportion of the variance (Adj. R 2 = 0.09, p = 0.031). In this model, REMD was the only significant predictor (Table 4; online Supplementary Fig. S4), and as with ERI, increased REMD was associated with poorer subjective extinction recall (B[s.e.] = 2.80[0.94], p = 0.004).
Linear regression analysis for subjective extinction recall (sERI; N = 94)
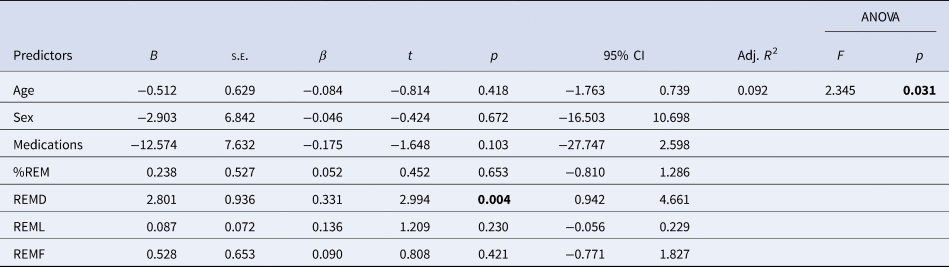
%REM, Proportion of REM sleep to the total sleep time; REMD, REM density; REMF, REM fragmentation; REML, REM latency.
REMD was the only significant predictor. Note that smaller sERI denotes better extinction recall.
Hierarchical regressions with HF HRV predicting ERI and sERI
Average HRV values are displayed in Table 2. For the hierarchical regression analyses with ERI as the dependent variable (N = 61), sex, medication use, and REM sleep measures (%REM, REMD, and REML) were included in the first model. HF [ms2] and sex × HF [ms2] interaction were included as additional predictors in the second model. The final model was significant (Adj. R 2 = 0.17, p = 0.018; Table 5). There was a trend for an increase in the variance accounted for by the second model (ΔR 2 = 0.08, p = 0.074). HF [ms2] and the sex × HF [ms2] interaction were significant predictors (B[s.e.] = −0.42[0.20], p = 0.042 and B[s.e.] = 0.65[0.29], p = 0.030), respectively. We therefore probed this interaction by examining the simple slopes, which showed that the effect of HF[ms2] on ERI was significant for males (B[s.e.] = −0.42[0.20], p = 0.042) but not for females (B[s.e.] = 0.23[0.21], p = 0.263), and the effects were different between sexes (p = 0.031).
Hierarchical regression analysis for physiological extinction recall (ERI; N = 61)
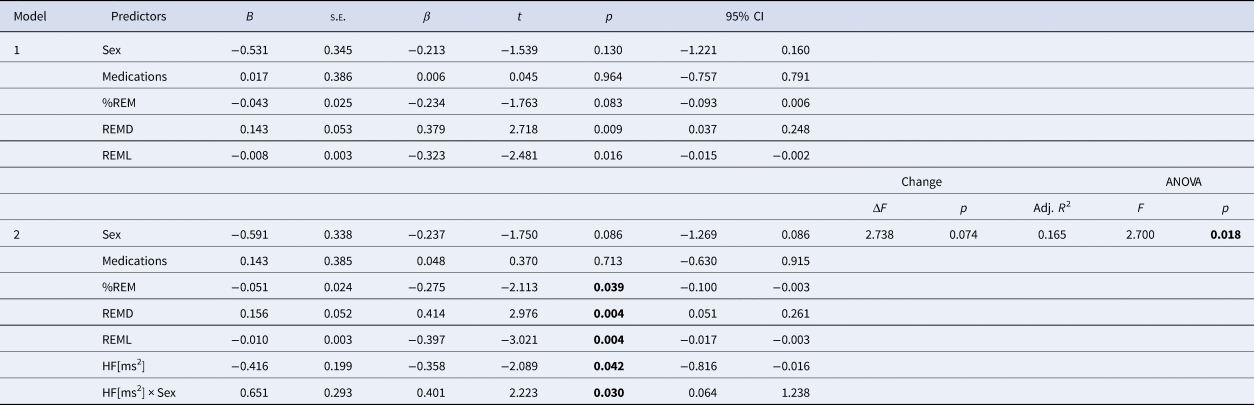
HF [ms2], absolute power of high frequency heart rate variability; %REM, proportion of REM sleep to the total sleep time; REMD, REM density; REML, REM latency.
HF [ms2] and HF [ms2] × sex interaction were significant predictors. Note that smaller ERI denotes better extinction recall.
A similar hierarchical regression analysis was carried out for sERI (N = 85). The first model included age, sex, medication use, and REMD. HF[ms2] was added to the predictors in the second model. The addition of HF [ms2] led to a significant increase in the variance accounted for by the model (ΔR 2 = 0.06, p = 0.018), indicating that vagal activity contributed to the prediction of subjective extinction recall above and beyond REM sleep measures. The final model was significant (Adj. R 2 = 0.13, p = 0.006), and medication use, REMD, and HF[ms2] emerged as significant predictors. Poorer subjective extinction recall was associated with not using medications (B[s.e.] = −18.81[8.19], p = 0.024), higher REMD (B[s.e.] = 2.64[0.95], p = 0.007), and lower HF [ms2] (B[s.e.] = −7.05[2.92], p = 0.018) (Table 6, online Supplementary Fig. S4).
Hierarchical regression analysis for subjective extinction recall (sERI; N = 85)
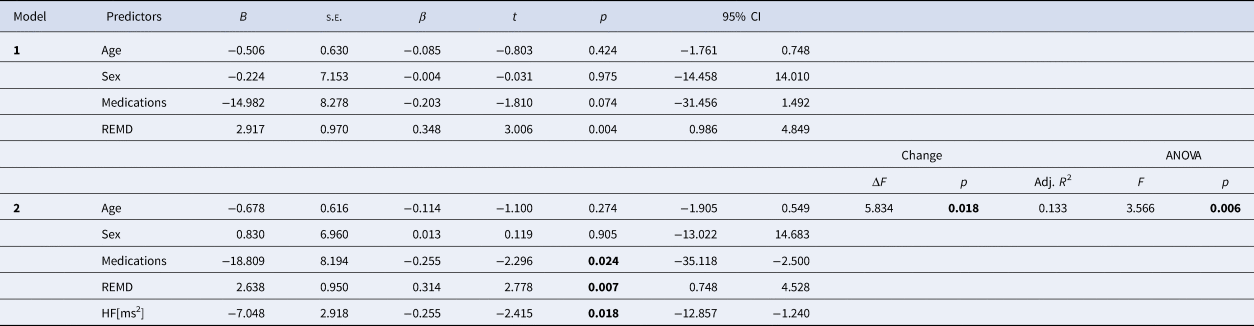
HF [ms2], absolute power of high frequency heart rate variability; REMD, REM density.
Addition of HF [ms2] significantly increased the proportion of variance explained by the model. Note that smaller sERI denotes better extinction recall.
For completeness, we repeated the same hierarchical regression analyses by adding all REM variables. The results were similar (online Supplementary Tables S1 and S2). Using RMSSD instead of HF [ms2] also did not change the results (online Supplementary Tables S3 and S4).
Results of regression analyses after the removal of non-contributory predictors are included in the Supplementary Methods (online Supplementary Tables S5–S8).
Discussion
We investigated the association of REM measures with the consolidation of physiological and subjective extinction memory in a large sample of trauma-exposed individuals. Confirming our first hypothesis, we found that less time spent in REM sleep, shorter REML, and higher REMD independently predicted poorer physiological extinction recall. Similarly, poorer subjective extinction recall was predicted by higher REMD. Furthermore, our second hypothesis, that higher HF HRV during REM would predict greater extinction recall above and beyond REM measures, was supported for subjective extinction recall and partially supported for physiological extinction recall. To the best of our knowledge, this is the first study to show that features of REM are associated with the consolidation of extinction memory in trauma-exposed individuals. In addition, we show here for the first time that vagal activity during a specific sleep stage contributes to the consolidation of an emotional memory.
REM measures predicting extinction recall is in agreement with previous research in healthy individuals (Davidson & Pace-Schott, Reference Davidson and Pace-Schott2020; Pace-Schott, Germain, & Milad, Reference Pace-Schott, Germain and Milad2015a) and in insomnia disorder (Bottary et al., Reference Bottary, Seo, Daffre, Gazecki, Moore, Kopotiyenko and Pace-Schott2020). In healthy individuals, better extinction recall was associated with the presence of REM during a nap (Spoormaker et al., Reference Spoormaker, Sturm, Andrade, Schroter, Goya-Maldonado, Holsboer and Czisch2010), higher overnight %REM (Pace-Schott et al., Reference Pace-Schott, Tracy, Rubin, Mollica, Ellenbogen, Bianchi and Orr2014), less fragmented REM, and increased REM theta power (Bottary et al., Reference Bottary, Seo, Daffre, Gazecki, Moore, Kopotiyenko and Pace-Schott2020). In addition, late-night (REM-rich) sleep but not early-night, NREM stage 3-rich sleep benefited extinction memory (Menz et al., Reference Menz, Rihm and Buchel2016), and selective REM, but not NREM, deprivation impaired extinction recall (Spoormaker et al., Reference Spoormaker, Schroter, Andrade, Dresler, Kiem, Goya-Maldonado and Czisch2012). In contrast, among individuals with insomnia disorder (Bottary et al., Reference Bottary, Seo, Daffre, Gazecki, Moore, Kopotiyenko and Pace-Schott2020), better extinction recall was associated with less %REM, shorter REM bouts, and longer REML. Findings are also in agreement with the general notion that REM is involved in processing emotional memories (Goldstein & Walker, Reference Goldstein and Walker2014), although this assertion is not consistently supported by experimental evidence (Davidson, Jonsson, Carlsson, & Pace-Schott, Reference Davidson, Jonsson, Carlsson and Pace-Schott2021).
We further showed that specific REM features were independently associated with extinction recall. There is a sizable literature that implicates both REML and REMD in a variety of psychiatric disorders, including PTSD (Baglioni et al., Reference Baglioni, Nanovska, Regen, Spiegelhalder, Feige, Nissen and Riemann2016). However, in PTSD, alterations in these variables are not consistently found, and the direction of change showed variability across studies, possibly due to the heterogeneity in samples and the settings in which data were collected (Baglioni et al., Reference Baglioni, Nanovska, Regen, Spiegelhalder, Feige, Nissen and Riemann2016; Kobayashi et al., Reference Kobayashi, Boarts and Delahanty2007; Zhang et al., Reference Zhang, Ren, Sanford, Yang, Zhou, Zhang and Tang2019). It was also proposed that two competing processes may be at play simultaneously, REM dysregulation and the resulting pressure to achieve REM (Mellman, Reference Mellman1997), which would explain the contradictory findings across studies (e.g. shorter or longer REML, depending on which of these processes predominate). Nonetheless, shortened REML and increased REMD have emerged as characteristics of PTSD in meta-analyses (Baglioni et al., Reference Baglioni, Nanovska, Regen, Spiegelhalder, Feige, Nissen and Riemann2016; Kobayashi et al., Reference Kobayashi, Boarts and Delahanty2007; Zhang et al., Reference Zhang, Ren, Sanford, Yang, Zhou, Zhang and Tang2019). Our findings advance insight into the significance of these REM alterations and indicate that they are associated with impaired extinction memory, a mechanism that is considered central to the development of PTSD (Bottary et al., Reference Bottary, Straus and Pace-Schott2023).
The mechanisms underlying REM alterations in PTSD and, by extension, how they might be associated with impaired extinction recall are not clear. However, it was proposed that hyperarousal, characterized by impairment in the inhibitory control of amygdala activity by the medial PFC (mPFC) with a concomitant increase in noradrenergic activity, contributes to REM dysregulation (Cabrera et al., Reference Cabrera, Koymans, Poe, Kessels, Van Someren and Wassing2024; Germain, Buysse, & Nofzinger, Reference Germain, Buysse and Nofzinger2008; Pace-Schott et al., Reference Pace-Schott, Seo and Bottary2023; Pace-Schott, Germain, & Milad, Reference Pace-Schott, Germain and Milad2015b). Indeed, increased REMD may be a direct manifestation of hyperarousal in PTSD (Barbato, Reference Barbato2023). Rapid eye movements are associated with activation in the limbic and paralimbic structures (Andrillon, Nir, Cirelli, Tononi, & Fried, Reference Andrillon, Nir, Cirelli, Tononi and Fried2015; Calvo & Fernandez-Guardiola, Reference Calvo and Fernandez-Guardiola1984; Corsi-Cabrera et al., Reference Corsi-Cabrera, Velasco, Del Rio-Portilla, Armony, Trejo-Martinez, Guevara and Velasco2016; Ioannides et al., Reference Ioannides, Corsi-Cabrera, Fenwick, del Rio Portilla, Laskaris, Khurshudyan and Kostopoulos2004; Miyauchi, Misaki, Kan, Fukunaga, & Koike, Reference Miyauchi, Misaki, Kan, Fukunaga and Koike2009; Wehrle et al., Reference Wehrle, Kaufmann, Wetter, Holsboer, Auer, Pollmacher and Czisch2007), as well as heart rate surges (Rowe et al., Reference Rowe, Moreno, Lau, Wallooppillai, Nearing, Kocsis and Verrier1999) and nightmares concurrent with autonomic arousal (Paul, Alpers, Reinhard, & Schredl, Reference Paul, Alpers, Reinhard and Schredl2019). Furthermore, in an overlapping sample, we recently showed that REMD was one of the predictors of self-reported hyperarousal symptoms in trauma-exposed individuals (Daffre et al., Reference Daffre, Oliver, Nazareno, Mader, Seo, Dominguez and Pace-Schott2023). Therefore, our results suggest that hyperarousal during REM interferes with the consolidation of extinction memory. REML has been considered an indicator of REM pressure, and the shortening of REML in PTSD has been attributed to an ‘unmet need’ (Mellman, Reference Mellman1997). This interpretation would suggest that a history of insufficient REM or a latent factor associated with a REM deficit may impair the consolidation of extinction memory. Alternatively, this association may be due to an adaptive REM enhancement to facilitate emotional processing (Mellman, Reference Mellman1997). Yet another possibility is that shortened REML may reflect depression (Palagini, Baglioni, Ciapparelli, Gemignani, & Riemann, Reference Palagini, Baglioni, Ciapparelli, Gemignani and Riemann2013). However, self-reported depressive symptoms were not correlated with REML (r s = 0.05, p = 0.65) or ERI (r s = 0.02, p = 0.86).
Vagal activity during REM, indexed as HF HRV, was a significant predictor of subjective extinction recall. This novel finding is consistent with the role of the vagal nerve in supporting memory formation (McGaugh, Reference McGaugh2013) and emotional regulation (Thayer & Lane, Reference Thayer and Lane2000), as well as the growing body of evidence indicating that vagal activity is causally involved in fear processing (Alvarez-Dieppa, Griffin, Cavalier, & McIntyre, Reference Alvarez-Dieppa, Griffin, Cavalier and McIntyre2016; Pena et al., Reference Pena, Engineer and McIntyre2013, Reference Pena, Childs, Willett, Vital, McIntyre and Kroener2014). Vagal activity in response to cognitive and emotional demands and vagally mediated HRV are considered to reflect the tonic inhibitory control of the amygdala by the mPFC (Thayer & Lane, Reference Thayer and Lane2009; Thayer, Ahs, Fredrikson, Sollers, & Wager, Reference Thayer, Ahs, Fredrikson, Sollers and Wager2012), circuitry that is also critical for fear extinction (Milad & Quirk, Reference Milad and Quirk2012). Consistent with this, high vagal activity during wake was repeatedly shown to be associated with better fear extinction in humans (Jenness et al., Reference Jenness, Miller, Rosen and McLaughlin2019; Pappens et al., Reference Pappens, Schroijen, Sutterlin, Smets, Van den Bergh, Thayer and Van Diest2014; Wendt et al., Reference Wendt, Neubert, Koenig, Thayer and Hamm2015, Reference Wendt, Konig, Hufenbach, Koenig, Thayer and Hamm2019). Furthermore, vagal nerve stimulation (VNS) facilitated plasticity in ventromedial PFC-amygdala connectivity in rodents (Pena et al., Reference Pena, Childs, Willett, Vital, McIntyre and Kroener2014), and improved extinction learning and recall in both rodents (Alvarez-Dieppa et al., Reference Alvarez-Dieppa, Griffin, Cavalier and McIntyre2016; Noble et al., Reference Noble, Gonzalez, Meruva, Callahan, Belfort, Ramanathan and McIntyre2017; Noble, Chuah, Callahan, Souza, & McIntyre, Reference Noble, Chuah, Callahan, Souza and McIntyre2019a; Pena et al., Reference Pena, Engineer and McIntyre2013, Reference Pena, Childs, Willett, Vital, McIntyre and Kroener2014; Souza et al., Reference Souza, Robertson, Pruitt, Gonzales, Hays, Rennaker and McIntyre2019, Reference Souza, Robertson, Mathew, Tabet, Bucksot, Pruitt and Kilgard2020, Reference Souza, Oleksiak, Tabet, Rennaker, Hays, Kilgard and McIntyre2021a, Reference Souza, Robertson, McIntyre, Rennaker, Hays and Kilgard2021b, Reference Souza, Powers, Rennaker, McIntyre, Hays and Kilgard2022) and humans (Burger et al., Reference Burger, Verkuil, Van Diest, Van der Does, Thayer and Brosschot2016, Reference Burger, Verkuil, Fenlon, Thijs, Cools, Miller and Van Diest2017, Reference Burger, Van Diest, Van der Does, Korbee, Waziri, Brosschot and Verkuil2019; Szeska et al., Reference Szeska, Richter, Wendt, Weymar and Hamm2020). Our results suggest that the contribution of vagal activity continues beyond extinction learning to its consolidation during sleep and supports the potential utility of interventions that can enhance sleep vagal activity in the prevention and treatment of fear-related disorders (Noble, Souza, & McIntyre, Reference Noble, Souza and McIntyre2019c). The association of HRV with physiological extinction recall in males should be treated as a preliminary finding, because of the small number of male participants in our sample (N = 34). Previous studies reported that sex and sex hormones were associated with differential activations in PFC and amygdala during extinction learning and recall (Benson et al., Reference Benson, Kattoor, Kullmann, Hofmann, Engler, Forsting and Elsenbruch2014; Merz et al., Reference Merz, Tabbert, Schweckendiek, Klucken, Vaitl, Stark and Wolf2012; Zeidan et al., Reference Zeidan, Igoe, Linnman, Vitalo, Levine, Klibanski and Milad2011). Therefore, the moderating effect of sex for the association of HRV with physiological extinction recall in our study may be due to the sex differences in the engagement of overlapping circuitry that processes fear extinction and regulates vagal activity.
Our study had several limitations. First, we had to exclude a substantial number of participants because of lost or unusable sleep data. Lack of oversight during ambulatory recordings can lead to more artifacts than in laboratory studies. Second, there is significant variability across studies in fear conditioning/extinction protocols and methods in analyzing generated data (Lonsdorf et al., Reference Lonsdorf, Menz, Andreatta, Fullana, Golkar, Haaker and Merz2017). Nonetheless, we used the widely employed Milad et al., Reference Milad, Wright, Orr, Pitman, Quirk and Rauch2007 fear conditioning and extinction protocol (Milad & Quirk, Reference Milad and Quirk2012), and we attempted to be consistent with our own and others' previously used metrics to index extinction recall. Third, a portion of our sample did not achieve physiological fear conditioning and was therefore excluded from the analysis. Nonetheless, the proportion of ‘non-conditioners’ in our sample (49/139, 35%) was smaller than in many previous studies (Alexandra Kredlow, Orr, & Otto, Reference Alexandra Kredlow, Orr and Otto2018). Lastly, the models for ERI and sERI revealed distinct predictors. A substantial body of research suggests that explicit and implicit fear conditioning, as well as extinction, are separate processes that engage overlapping but distinct neural circuits (Grillon, Reference Grillon2009; Knight, Nguyen, & Bandettini, Reference Knight, Nguyen and Bandettini2003; Knight, Waters, & Bandettini, Reference Knight, Waters and Bandettini2009; Siegel & Weinberger, Reference Siegel and Weinberger2012). This dissociation is also evident in our sample, where physiological and subjective extinction recall indexes (ERI and sERI) are not correlated (spearman's rho = 0.07, p = 0.52). Therefore, it is not surprising that different predictors emerged for ERI and sERI.
Conclusions
Abnormalities in REM have repeatedly been reported in individuals diagnosed with PTSD and have been shown to be associated with an increased risk of developing PTSD after a traumatic event. Results of this study further our insight into the role of REM disruptions and indicate that they are associated with impaired consolidation of extinction memory, a mechanism proposed to be critical in the pathogenesis of PTSD.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291724002757
Acknowledgments
The authors would like to thank Karen Gannon, RPSGT for scoring sleep recordings and Catherine Bostian for adapting the Yetton et al. REM density program.
Author contributions
Cagri Yuksel and Edward F. Pace-Schott conceptualized the study. Lauren Watford, Monami Muranaka, Emma McCoy, Augustus Kram Mendelsohn, Katelyn I. Oliver, Carolina Daffre, Hannah Lax, and Uriel Martinez, collected and reduced data. Cagri Yuksel, Lauren Watford, Monami Muranaka, Hannah Lax, Alexis Acosta, and Abegail Vidrin analyzed the data. Natasha B. Lasko interviewed participants. Carolina Daffre and Scott Orr provided consultation on statistical analyses. Cagri Yuksel and Edward F. Pace-Schott authored the manuscript draft. Carolina Daffre and Scott Orr provided feedback on the manuscript draft.
Funding statement
This project was primarily supported by the National Institute of Mental Health R01MH109638 and R21MH121832 to E.P.-S, and K23MH119322 to C.Y. Praxis Precision Medicines also provided partial salary support to E.P.-S. Funding bodies did not have any role in the design of the study, collection, and analysis of data, and decision to publish.
Competing interests
The authors declare no competing interests.








