Introduction
Psychological distress is common among palliative care patients and contributes to a heightened severity of physical symptoms and poor quality of life (Ann-Yi et al. Reference Ann-Yi, Bruera and Wu2018; O’Malley et al. Reference O’Malley, Blakley and Ramos2021). As a holistic and multidisciplinary specialty that addresses physical, psychological, and spiritual problems, palliative care ideally includes health professionals that can adequately address medical and psychological needs to improve quality of life for patients with terminal illness (Ann-Yi et al. Reference Ann-Yi, Bruera and Wu2018; Edlynn and Kaur Reference Edlynn and Kaur2016). Australia’s 2004 National Consensus Project’s Clinical Practice Guidelines for Quality Palliative Care states that a palliative care team must address psychological aspects of care and treat a patient and their family in a way that respects their spiritual beliefs (National Consensus Project for Quality Palliative Care 2018). Despite this, little is known about the availability of psychological services to support palliative care patients within Australia.
The aim of this project was to determine the level of psychological support services available within Palliative Care Services in Australia during 2021/22. We aimed to identify the types of psychological supports available, the health professionals involved in the delivery of psychological care, and their availability, skills, and roles within the palliative care service. An unpublished study by Crawford in 1999 examined adult psychological service provision in Palliative Care Services in Australia (Crawford Reference Crawford2007). Comparison with these data allows examination of differences over time.
Methods
A list of all Palliative Care Services in Australia was obtained online from the Australian Palliative Care Outcomes Collaboration (PCOC) website, a national government-funded initiative that collects data for quality improvement for more than 80% of Palliative Care Services in Australia (Palliative Care Outcomes Collaboration 2021). Only services providing hospice/inpatient care and/or community Palliative Care Services to adult patients were included. Services that involved children and/or only outpatient Palliative Care Services were excluded. Contact details for each service and their eligibility were ascertained using information available publicly on the internet.
Each service was initially contacted by email, using the generic email address listed for the service publicly online. If an email address was unavailable, the service was contacted by phone to obtain a generic email address. An email was sent that explained the study and requested that the email be forwarded to the most appropriate health professional to answer questions regarding psychological services available at the site. Reminder emails were sent at 3 and 5 weeks.
The 12-item online survey, based on a similar survey used by Crawford in 1999, was distributed using Qualtrics (Crawford Reference Crawford2007). The survey was anonymous, simply requesting the job title of the person completing the survey, before asking the type and size of their service and any screening tools utilized to assess psychological distress. The survey then explored access to professionals involved in delivering psychological care, including psychiatrists, social workers, psychologists, counselors, spiritual care workers, complementary therapists, and creative therapists (included art therapists, biographers, and music therapists). The availability of each professional, number of referrals they receive, and their roles within the service were explored. Questions were a combination of multiple choice and free text (Appendix 1).
Statistical analysis
Responses from both complete and partial respondents were used in the analysis. Partial respondents were defined as those who did not complete the survey but provided a response to at least 1 question. Continuous variables are presented as mean (standard deviation [SD]), median (interquartile range [IQR]), and range for completeness, and categorical variables are presented as count and percentages (%). Proportions obtained from the current survey were compared with data from the 1999 survey using 2-proportions z-test, and differences reported with their 95% confidence interval (CI). All analyses were performed using Stata/IC 15.1 (StataCorp 2017). Free text responses were analyzed using qualitative content analysis (Hsieh and Shannon Reference Hsieh and Shannon2005).
Results
Survey distribution and response
Email invitations were successfully sent to 79 out of the 90 Palliative Care Services listed on the PCOC website. Emails were not sent to the remaining 11 services as they were not contactable with no email or phone number (n = 7), declined to participate during the initial phone call (n = 2), or had invalid email addresses (n = 2). Responses were collected over a 2-month period from November 28, 2021 to January 27, 2022. Staff members of 47 out of the 79 services who received the email invitation attempted the online survey, a response rate of 59.5%. Six online surveys received were excluded from analysis as they provided no information about the service at all. Of the 41 services included in the analysis, 35 were complete respondents (i.e., progressed to the end of the survey) and 6 were partial respondents (i.e., stopped before reaching the end). Figure 1 summarizes the flow of the survey distribution and response.
Flow diagram of the survey distribution and response.

Sample characteristics
Respondents to the survey were primarily nurse consultants (36.6%) and social workers (36.6%). Tables 1 and 2 report general information about the Palliative Care Services. The mean number of new patient referrals per month was 42 (SD 60), the median was 20 (IQR 10–40), and the range was 3 to 265. Most services provided a community palliative care service (89.5%), which received an average of 17.4 referrals (SD 33.7) per week, with a median of 5 (IQR 4–10), and a range of 1 to 150. The mean number of patients known to a community palliative care team at any 1 time was 161.4 (SD 160.9), the median was 95 (IQR 60–200), and the range was 1 to 550. Access to hospice/dedicated palliative care inpatient beds was provided in 47.4% of services. The mean number of beds was 11.3 (SD 6.4), the median was 12 (IQR 8.0–15.5), and the range was 1 to 25. A hospital consultation service was provided in 52.6% of services, and 47.4% had an outpatient clinic.
Basic information of the Palliative Care Service (n = 41)

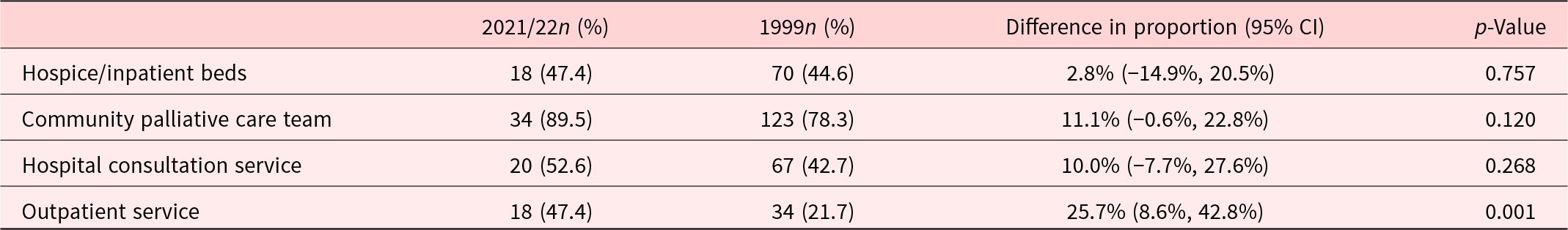
Comparison of the range of services offered by Palliative Care Services in Australia between 2021/22 (n = 38a) and 1999 (n = 157)

a Of the 41 respondents, 38 answered this question.
Except for more services providing a palliative care outpatient service in 2021/22 (p = 0.001), there was no significant difference in the proportion of services providing hospice, community or hospital consultation services in 2021/22 compared with 1999.
Screening for psychological distress
Just over half of services, 53.7%, reported using a screening instrument for psychological distress. For those services that nominated use of a screening instrument, the specific screening instrument used was highly variable. In total, 19 different tools were reported, with a majority (6 services) stating use of the Bereavement Risk Assessment Tool (Sealey et al. Reference Sealey, Breen and O’Connor2015).
Access to psychological support services
The majority (56.1%) of respondents rated access to psychological support services within their own organization as “fair/good/very good,” 29.3% rated access to psychological support services as “poor/very poor,” and 14.6% provided no response.
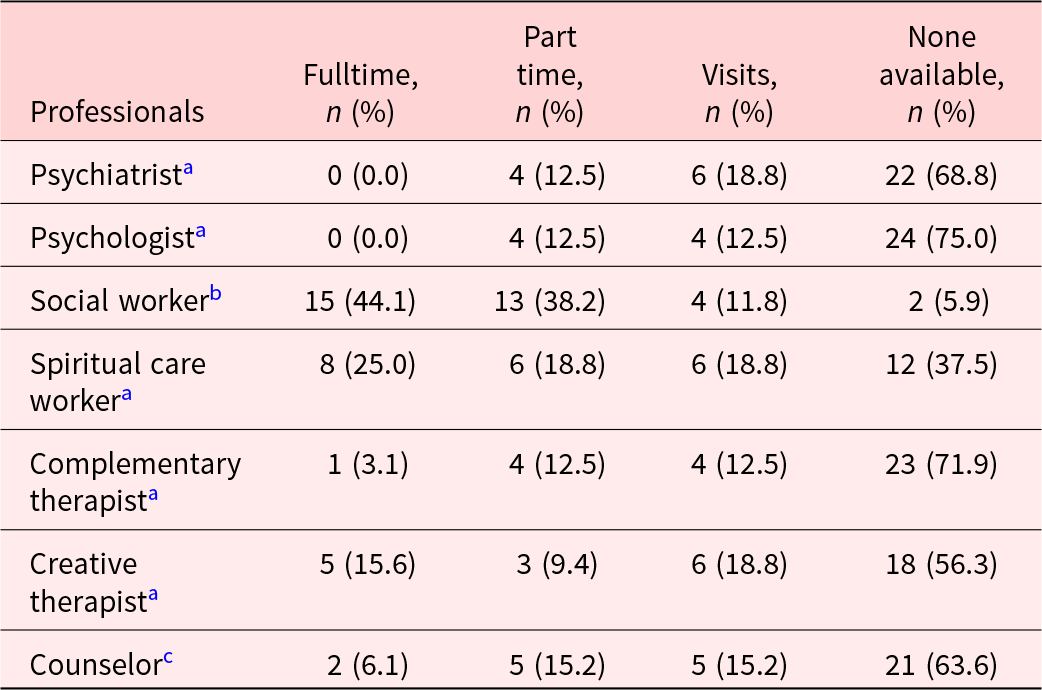
The availability of different health professionals providing psychological support in Palliative Care Services in Australia is reported in Table 3. Social workers were the most widely available, present in 94.1% of Palliative Care Services. Spiritual care workers were the next most prevalent (62.5%), followed by creative therapists (43.8%), counselors (36.4%), psychiatrists (31.3%), complementary therapists (28.1%), and psychologists (25.0%). Psychiatrists and psychologists were the least available psychological health professional. Nearly 60% of Palliative Care Services did not have access to either a psychiatrist or a psychologist. Only 25% of services had access to either a psychiatrist or psychologist, and only 15.6% of services had access to both a psychiatrist and psychologist.
Availability of psychological health professionals in Palliative Care Services in Australia (n = 32–34)

Missing data:
a Thirty-two services responded.
b Thirty-four services responded.
c Thirty-three services responded.
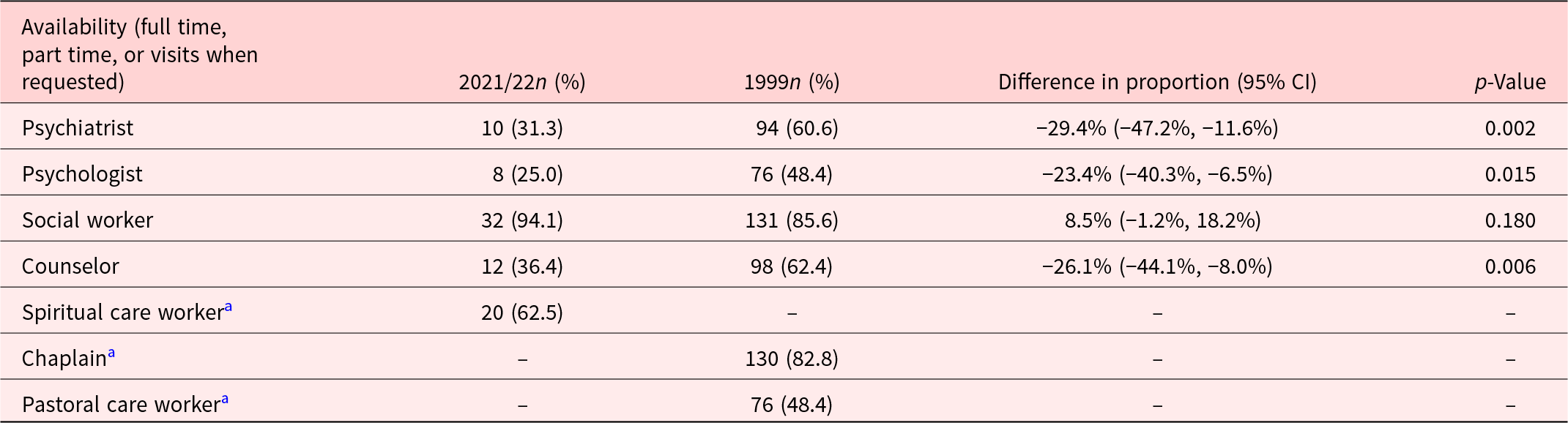
Comparison of the availability of psychological health professionals in 2021/22 and 1999 is shown in Table 4. The proportion of Palliative Care Services that had access to a psychiatrist, psychologist or counselor is significantly less in 2021/22 compared with 1999, with a difference of 29.4% (p = 0.002), 23.4% (p = 0.015), and 26.1% (p = 0.006), respectively. Presence of social work in Palliative Care Services has remained high and unchanged over time. Due to differences in data collection from Crawford in 1999, comparisons were unable to be made over time with regard to availability of spiritual care workers, complementary therapists, and creative therapists (Crawford Reference Crawford2007).
Availability of psychological health professionals in Palliative Care Services in Australia in 2021/22 (n = 32–34) and 1999 (n = 153–157)

a No comparison was made for these professionals due to different descriptions used in the surveys.
Very few services in the current study provided information about the number of referrals to each psychological health professional per month. The largest response was with social worker referrals. A total of 13 services answered this question with a range of 2 to 40 patients referred per month. Data about the number of referrals to other psychological health professionals were provided by fewer than 5 services for each discipline.
Respondents were asked to describe the role of different psychological health professionals in free text boxes and identify (by means of selecting “yes” or “no” boxes) whether the health professional had special skills or interest in palliative care. Respondents were able to describe the role of social workers in their service most readily (58.5% response rate). The response rate for defining the roles of spiritual care workers was next most common at 36.6%. The roles of other psychological health professionals were reported less frequently – response rate of 19.5% for creative therapists, 17.1% for both counselors and psychiatrists, 12.2% for complementary therapists, and 4.9% for psychologists.
The most frequently described roles of social workers were patient counseling (45.8% of responses), bereavement support (41.7% of responses), and family support (25% of responses). Other less frequently described roles included assistance in complex discharge planning, financial support, and legal documents. A total of 96.9% of social workers were considered to have skills or interest in palliative care. The role of spiritual care workers was defined simply as “spiritual care” in most responses (6 of the 15 responses), with only one response mentioning spiritual rituals and another mentioning assistance in resolving family conflict. The majority, 90%, of spiritual care workers were considered to have skills or interest in palliative care, 65% were paid employees, and 20% were volunteers. The role of creative therapists was divided equally between music therapy, art therapy, and legacy work/life review, with 28.6% being volunteers and 64.3% having skills or interest in palliative care. Counselors were reported to assist in bereavement and social support primarily, with 8.3% reported to be volunteers and 58.3% with skills or interest in palliative care. Psychiatrists were all reported to assist in mental health assessment and consultation and 70% were considered to have skills or interest in palliative care. Complementary therapists were primarily reported as massage therapists. The role of psychologists was the least frequently answered question. The 2 responses were emotional support and cognitive assessments. Only 50% of psychologists in Palliative Care Services were considered to have skills or interest in palliative care.
Qualitative content analysis of other comments
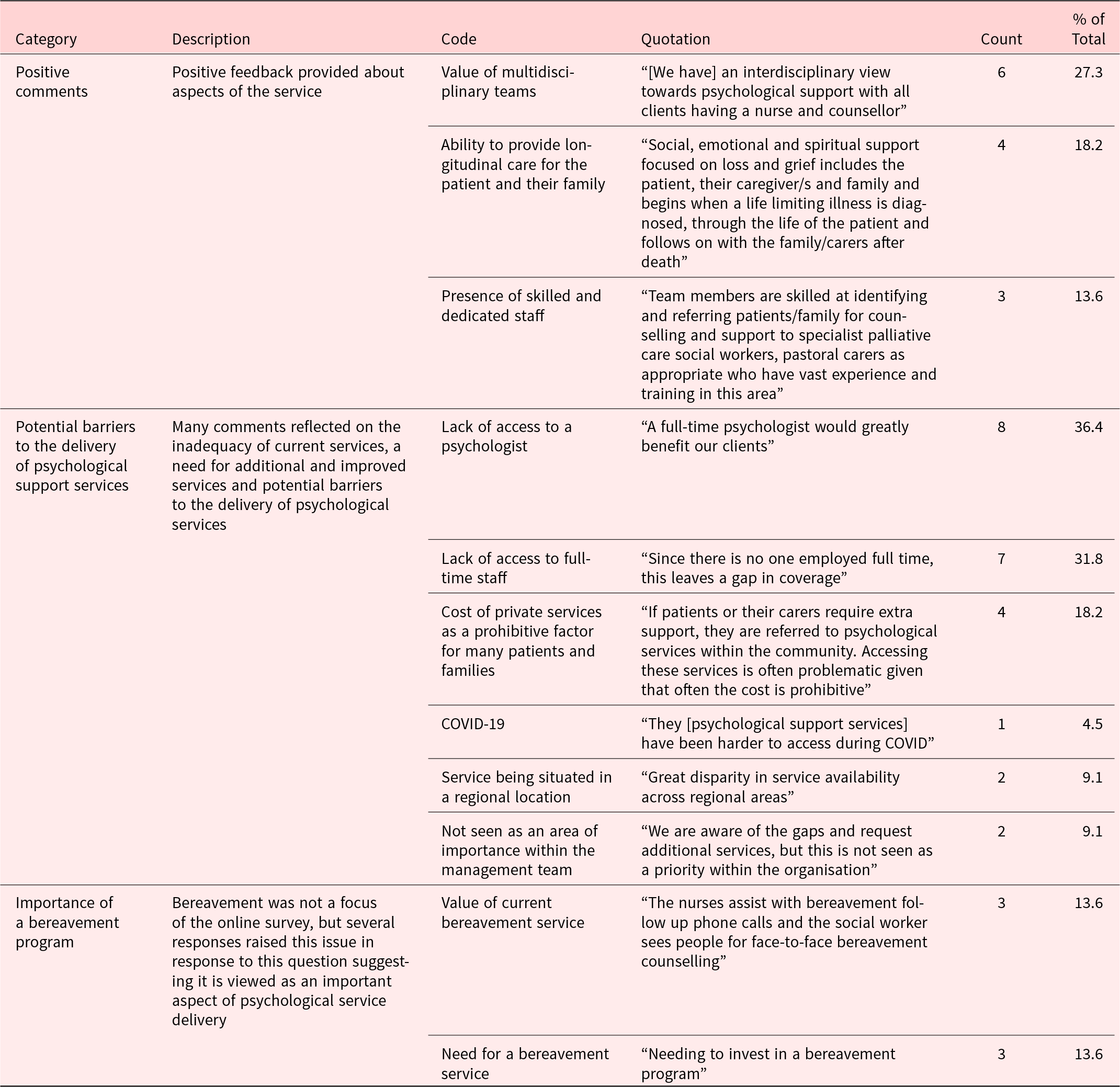
The survey included a free text section where respondents could provide further comments about psychological support services in their organization. A total of 22 out of the 41 services answered this question (response rate of 53.7%). A summary of these findings is reported in Table 5.
Qualitative analysis of further comments made about psychological service provision at each organization (n = 22)

Discussion
With the exception of a similar study by Crawford in 1999, to the best of our knowledge, there are no other studies examining the current delivery of psychological services in Australian Palliative Care Services (Crawford Reference Crawford2007). However, a similar study examining Palliative Care Services in the UK was conducted by McInnerney et al. in 2019, although notably this only included hospices and not community Palliative Care Services (McInnerney et al. Reference McInnerney, Candy and Stone2021). Similar to our study, McInnerney et al. found that psychiatrists and psychologists were the least available psychological health professional, with no access to a psychiatrist in 20% of hospices, no access to a clinical psychologist in 19% of hospices, and no access to a counseling psychologist in 39% of hospices (McInnerney et al. Reference McInnerney, Candy and Stone2021). However, creative therapists, social workers, complementary therapists, counselors, and spiritual advisers were all well represented and available in a much greater proportion of services than in Australia – all were available in over 85% of hospices (McInnerney et al. Reference McInnerney, Candy and Stone2021). Of significance, they showed improved access to psychological support over a 15-year period, particularly with regard to access to psychologists, counselors, and psychiatrists, the opposite trend to our study (McInnerney et al. Reference McInnerney, Candy and Stone2021). They proposed that improved access may reflect increased awareness of psychological well-being in end-of-life care situations (McInnerney et al. Reference McInnerney, Candy and Stone2021). Awareness of worsening access to some psychological health professionals is an important part of addressing the issue. This is reflected in our qualitative data, where several respondents stated that psychological services were not seen as an area of importance within the management team.
Our study identified that nearly 60% of Palliative Care Services had no access to either a psychiatrist or a psychologist and 36.4% of services highlighted that lack of access to a psychologist was a significant barrier to psychological service delivery. More specifically, 75% of services did not have access to a psychologist and 68.7% of services did not have access to a psychiatrist, both reflecting a greater than 20% reduction since 1999. Depression, anxiety, delirium, and adjustment disorders are common in palliative care patients and contribute to patient and family distress (Fairman and Irwin Reference Fairman and Irwin2013). While arguably other disciplines may assist in treating these disorders, psychologists and psychiatrists are both specifically trained in testing for and addressing complex mental health needs in different ways (Ann-Yi et al. Reference Ann-Yi, Bruera and Wu2018; Fairman and Irwin Reference Fairman and Irwin2013; O’Malley et al. Reference O’Malley, Blakley and Ramos2021). It has been suggested that palliative medicine specialists may under-recognize psychiatric illness, lack confidence in the off-label use of psychotropic medications, and have inadequate experience in providing psychotherapeutic interventions (Ann-Yi et al. Reference Ann-Yi, Bruera and Wu2018; Fairman and Irwin Reference Fairman and Irwin2013; O’Malley et al. Reference O’Malley, Blakley and Ramos2021). Early psychological interventions may assist in preventing normal adjustment from progressing to a mental health disorder (Ann-Yi et al. Reference Ann-Yi, Bruera and Wu2018). Few palliative care teams have access to these health professionals despite evidence that their presence improves patient well-being (Edlynn and Kaur Reference Edlynn and Kaur2016; Kasl-Godley et al. Reference Kasl-Godley, King and Quill2014; O’Malley et al. Reference O’Malley, Blakley and Ramos2021). A study by Ann-Yi et al. (Reference Ann-Yi, Bruera and Wu2018) showed how palliative care psychology services can successfully integrate into a palliative care department, with substantial growth in demand demonstrated in inpatient and outpatient settings.
Our study found that respondents cited lack of access to psychologists and cost of these services as barriers to psychological service delivery. There is a significant shortage of psychologists and psychiatrists in Australia, so it is not unexpected that this deficit is also apparent in Palliative Care Services. A survey from the Australian Psychological Society in 2022 found that 1 in 3 psychologists were not taking on new clients (Australian Psychological Society 2022). The Federal Government is only meeting 35% of its psychology workforce target listed in the National Mental Health Service Planning Framework (Australian Psychological Society 2022). Access to psychiatrists in health care is similarly limited due to long waiting lists, the majority working only in metropolitan areas, few private psychiatrists bulk-billing, and too few psychiatrists employed in the public sector (Parliament of Australia 2006). Addressing the shortage of these health professionals, improving waiting times and employing more in the public sector, will be vital to improving their accessibility in Palliative Care Services.
In our study, few respondents answered the question about the role of a psychologist in their Palliative Care Service, which may reflect a lack of understanding about how psychologists can assist patients and their families. Similarly, we found that only 70% of psychiatrists and 50% of psychologists in palliative care settings were reported to have special skills or interest in palliative care. A study by Nakajima et al. (Reference Nakajima, Iwamitsu and Matsubara2015) in Japan found that many psychologists in palliative care felt unable to meet workplace expectations and lacked adequate knowledge in palliative care to work effectively. A review by Fairman and Irwin (Reference Fairman and Irwin2013) suggested that an important way to improve the integration of psychiatrists into palliative care was to develop opportunities for psychiatric trainees to gain experience in a palliative care setting, given the unique skill set required for this work. Improving both palliative care skills in psychologists and psychiatrists and educating other disciplines about the role of these professionals may improve current Palliative Care Services.
Our study found that counselors were present in 36.4% of Palliative Care Services, a 26.1% reduction since 1999. Notably, the role of counselors was only described by 17.1% of respondents and descriptions of this role were broad. Studies examining the role of counselors in the palliative care setting demonstrate how they may assist in many areas including psychological assessment, counseling interventions, advocacy, education, and team support (Thompson et al. Reference Thompson, Rose and Wainwright2001). The education and training of counselors is varied, and as such their skill set may overlap with other health professionals including psychologists and social workers. Consequently, the prevalence and reduction in the presence of counselors over time may reflect different definitions of this professional and their role may be absorbed by others within the service. This would be important to explore in further studies.
Our study identified a strong presence of social workers throughout Palliative Care Services in Australia, and this has been consistent since 1999. Respondents to our survey also identified spiritual care workers, creative therapists, and complementary therapists as important providers of psychological support in some Palliative Care Services. However, our study was unable to identify information about the number of referrals these professionals receive, making it difficult to appreciate the number of patients who use these services. This would be important to know when evaluating feasibility of these professionals within a Palliative Care Service.
This study has identified areas of overlap in the role of different professionals providing some services, such as psychological interventions. There is evidence that psychological interventions such as guided imagery, mindfulness, and cognitive behavioral therapy can be led by specifically trained social workers and assist in reducing patient anxiety and depression (Farabelli et al. Reference Farabelli, Kimberly and Altilio2020). Similarly, there is evidence to suggest that biographical therapies can be effectively provided by volunteers (Hesse et al. Reference Hesse, Forstmeier and Cuhls2019). Given the lack of access to psychologists, psychiatrists, and counselors identified in our study, further exploration of using other professionals to provide these services may be of value.
Almost half of the Palliative Care Services in our study stated that they did not use any screening instruments for psychological distress, yet national and international guidelines recommend routine screening (Thekkumpurath et al. Reference Thekkumpurath, Venkateswaran and Kumar2008). A study by Kozlov et al. (Reference Kozlov, Eghan and Moran2018), investigating how inpatient Palliative Care Services screened for psychological distress in New York, found significant variability in the screening tools used, in addition to inconsistencies in responses to high detected scores. This suggests that although recommendations for use of a screening tool are clear, there is a role for clarification of the most useful instrument and optimal response to a high score.
Limitations
To improve the response rate, respondents to the survey could skip questions or leave answers blank if unknown, resulting in missing data. Inherent in this style of study is response bias – the results may reflect the views of palliative care staff who have an interest in psychological care. Compared with data collection in 1999 that included distribution of 247 surveys, our study identified and approached 90 Palliative Care Services. This may reflect differences in the method of identifying services and/or service amalgamation over time.
Conclusion
Lack of access to mental health professionals in Australian Palliative Care Services has become more prevalent over the last 2 decades. While the direct impact of this for palliative care patients is difficult to determine, there is clear evidence that these health professionals play a vital role in the palliative care setting. Ongoing advocacy and increased government funding to enable these professionals to be readily employed in Palliative Care Services is vital.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S1478951523000925.
Author contributions
E Brook: Conceptualization, Methodology, Investigation, Data Curation, Writing-Original Draft, Visualization. A Chur-Hansen: Conceptualization, Methodology, Writing-Review and Editing, Supervision. L Chan: Formal analysis, Data Curation, Writing-Review, and Editing. GB Crawford: Conceptualization, Methodology, Writing-Review, and Editing, Supervision.
Funding
This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
Competing interests
No conflicts of interest declared.
Ethical approval
This research project was approved by the Human Research Subcommittee in the School of Psychology at the University of Adelaide in 2021 (approval number: 21/73).