Durable powers of attorney for healthcare have been used by other countries, for example the USA, for an appreciable time. In the UK, the advent in 2007 of lasting powers of attorney (LPAs) under the auspices of the Mental Capacity Act 2005 has brought with it an epoch-making legal change. For the first time in English and Welsh law, substituted decision-making is allowed for medical treatment – the LPA being a vehicle that aims to enhance prospective autonomous decision-making in the event of future incapacity (Reference SamantaSamanta 2009). This article reviews the history of powers of attorney; describes the introduction and initial use of LPAs; reviews pertinent LPA case law emanating from the Court of Protection; and considers implications of LPAs, particularly the health and welfare LPA, for clinicians.
The power of attorney
The power of attorney has been used in Britain for hundreds of years. One of the earliest recorded dates is 1378 when Geoffrey Chaucer (author of The Canterbury Tales) named two friends as appointees during a diplomatic trip to Italy.
Ordinary powers of attorney
Today an ‘ordinary power of attorney’ (OPA), which is governed in England and Wales by the Powers of Attorney Act 1971, remains a commonly used document, allowing donors to nominate an attorney to deal with financial matters on their behalf – this can be general and cover every aspect of their affairs or can specify which matters the attorney can handle. This arrangement can be ended at any time by the donor and the document automatically becomes invalid if the donor loses mental capacity. An OPA might be considered when someone is going abroad for a period of time, going into hospital or is physically unable to manage their finances owing to illness or disability.
Enduring powers of attorney
An OPA is automatically revoked by the mental incapacity of the donor and so the Enduring Powers of Attorney Act 1985 was introduced to enable an attorney to continue to deal with the donor’s financial affairs after they became mentally incapacitated, subject to registering the enduring power of attorney (EPA) with the Court of Protection. This Act was repealed by the Mental Capacity Act 2005 with effect from 1 October 2007, but EPAs created before this remain valid, subject to being registered with the Office of the Public Guardian.
Lasting powers of attorney
In replacing the Enduring Powers of Attorney Act 1985, the Mental Capacity Act introduced the lasting power of attorney. An LPA is a legal document that enables a person who has capacity and is over 18 (the donor) to choose another person or people (the attorney(s)) to make decisions on their behalf. There are two types of LPA: a property and financial affairs LPA and a health and welfare LPA.
The property and financial affairs LPA is similar to an EPA, although it must be registered with the Office of the Public Guardian before it can be used. In Engand and Wales, the health and welfare LPA allows donors to nominate an attorney to make decisions about their personal health and welfare once they become incapacitated for the first time. Only adults aged 18 or over can make an LPA. There are separate LPA forms for health and welfare, and property and financial affairs. The forms comprise three sections: Part A should be filled in by the donor; Part B by the certificate provider; and Part C by the attorney(s). A certificate provider must be chosen by the donor and can be either someone who has known the donor personally for at least 2 years or, if the donor has borderline capacity, a professional who is qualified to make the judgements required to be able to sign the certificate. Patients may ask a doctor to be the certificate provider and it is prudent to get any such requests in writing from either the solicitor involved or the donor (if the donor is completing and submitting the LPA forms without involving a solicitor). The Mental Capacity Act sets out a number of requirements that the donor, attorney(s) and certificate provider must satisfy before a valid LPA is created (Box 1).
Mental Capacity Act 2005 requirements in creating a valid LPA
-
1 The donor must sign a statement indicating that they understand the purpose of the lasting power of attorney (LPA), that the attorney(s) can only act when the donor has lost the relevant mental capacity and that the attorneys are governed to act by the principles set out in the Act.
-
2 The form allows for replacement attorney(s) to be made available but a replacement attorney may only act on the occurrence of an event mentioned in s. 13(6)(a)–(d) of the Act, for example, where an original attorney disclaims, dies, loses mental capacity or becomes bankrupt, or on the dissolution or annulment of a marriage or civil partnership between the donor and attorney.
-
3 The donor should name people (other than their attorney/replacement attorney(s)) who should be informed about their application to register an LPA. If they do not have a named person, there should be two people acting as certificate providers.
-
4 For a health and welfare LPA, the donor is asked to choose one of two options on whether they would give their attorney(s) the authority to consent or refuse life-sustaining treatment on their behalf.
-
5 The form allows the donor to appoint two or more attorneys and specify whether they should act:
-
jointly (always act together);
-
jointly and severally (either together or independently); or
-
jointly in respect of some matters and jointly and severally in respect of others.
The form allows the donor to write down any restrictions, conditions and guidance for their attorney(s).
-
-
6 The attorney(s) must sign a statement saying that they have read the prescribed information and that they understand their duties (in particular the duty to act in the donor’s best interests).
-
7 The witness chosen by the donor cannot be an attorney or replacement attorney or the employee of any trust corporation named as an attorney or replacement attorney. A certificate provider or a ‘named person’ can act as a witness.
-
8 The document must include a certificate provided by an independent third party (the certificate provider), confirming that:
-
the donor understood the purpose of the LPA and the scope of authority conferred under it; no fraud or undue pressure was used to induce the donor to create the LPA; and there is nothing to stop the LPA from being created.
-
In response to criticisms of the two original forms, a statutory instrument came into force on 1 October 2009 (Sectretary of State 2009), which introduced two new prescribed LPA forms (the original LPA forms could still be used until 1 April 2011). The changes included: the renaming of personal welfare LPAs as health and welfare LPAs; a reduction in length of both documents from 25 pages to 11 pages for property and financial affairs and 12 for health and welfare; a new colour-coordinated design; clearer instructions within the document; a reduction in the number of tick boxes; and, most importantly, a reduction in registration fee from £150 to £120 for each LPA, with potential exemption or remission if the donor’s gross annual income was £16 500 or under (the situation since changed again: the registration fee is currently £130 and there is a new fee remission of £65 for gross income up to £12 000; partial remissions have been abolished). However, because an LPA is more complicated than an EPA many people use a solicitor to create it, which carries substantial additional expense: it can cost £400–500 to register an LPA (such costs may, of course, be so prohibitive as to ostracise a large group for whom the LPA is particularly useful – older people).
The health and welfare LPA
Detailed guidance on making a health and welfare LPA has been published by the Office of the Public Guardian (2011). It includes specific sections on ‘life-sustaining treatments’ and ‘restrictions and conditions’. A health and welfare LPA can only be used after the donor lacks capacity to make the decisions themselves and only after registering it with the Office of the Public Guardian.
Unless the health and welfare LPA contains conditions, once it is registered and the donor loses capacity, the attorney will be able to do anything in relation to the personal welfare of the donor that the donor could have done before losing capacity. The Mental Capacity Act 2005 Code of Practice (Department for Constitutional Affairs 2007) explains salient health and welfare decisions for attorneys (Box 2).
Examples of health and welfare decisions in which the attorney may participate
-
• Where and with whom the donor should live – if this involves the potential sale of their house/property, then discussion will need to be had with the property and finances attorney(s)
-
• Consenting to or refusing medical examinations and treatment
-
• Arranging medical, dental or optical treatment
-
• Assessments for, and provision of, community care services
-
• Deciding, alone or with others, what care would be most suitable
-
• Day-to-day care of the donor, including diet and dress
-
• Who the donor may have contact with
-
• Whether the donor should participate in social or leisure activities, education or training
-
• Rights of access to personal information about the donor, including personal correspondence
-
• Complaints about the donor’s care and treatment
However, attorneys cannot do whatever they like. Guidance from the Office of the Public Guardian (2011) makes it clear that they must follow the core principles of the 2005 Act, based on acting in the best interests of the donor. In addition, the donor may be unable to make some decisions, but retain capacity to make others. As such, the attorney has a duty to have regard to the Code of Practice, establishing that the donor lacks capacity for each decision to be made before acting on their behalf. An attorney should also permit the donor to make decisions perceived as being unwise, providing that the donor retains capacity to make such a decision (in reality such a scenario may be problematic and difficult for attorneys who are not familiar with the Code of Practice).
The Office of the Public Guardian guidance specifically notes that attorneys can only make decisions about life-sustaining treatment if the donor has indicated that they want them to do so by signing a specific option in the LPA document. It importantly states that, in making such health and welfare decisions, the attorney must not be motivated by a desire to bring about the person’s death. It goes on to say that an attorney cannot make decisions about:
-
• consenting to marriage or a civil partnership;
-
• consenting to a decree of divorce (or civil partnership dissolution) based on 2 years’ separation; or
-
• consenting to sex.
A donor has an opportunity in the document to specify conditions and procedures that an attorney(s) must follow (e.g. not consenting to medical treatment involving blood products on religious grounds) and advice they must seek (e.g. consulting a doctor’s opinion over decisions about moving into residential care). The Office of the Public Guardian guidance suggests an example of a typical and useful restriction would be one that states that the attorney(s) must not consent to any life-sustaining treatment if the donor were in a persistent vegetative state. It also states the important fact that any restrictions or conditions made by the donor in the LPA are binding and the attorney(s) must follow them. However, there are circumstances described in the 2005 Act Code of Practice in which health and welfare attorneys do not have the right to consent to or refuse treatment:
-
• the donor has capacity to make the particular healthcare decision (s. 11(7)(a));
-
• the donor has made an advanced decision to refuse the proposed treatment (s. 11(7)(b));
-
• a decision relates to life-sustaining treatment (s. 11(7)(c) – an attorney has no power to consent to or refuse life-sustaining treatment, unless the LPA document expressly authorises it); or
-
• the donor is detained under the Mental Health Act (Mental Capacity Act 2005, s. 28).
The initial use of LPAs
From the inception of LPAs on 1 October 2007 until 11 June 2008, 17 806 applications were made to the Office of the Public Guardian to register LPAs. Of these, 81.8% were for property and financial affairs and 18.2% were for health and welfare. Of all of the LPA applications, 23% were made by people in their 70s, 47% by people in their 80s, 15% by people in their 90s and 1.3% made by people over 100 years of age. Only 3% of LPAs were made by people aged under 50 (Reference LushLush 2009). The numbers of LPA applications in the first year were far more than predicted and resulted in a long backlog, delays and a large number of complaints. Such administrative inadequacies led to an early review and prompt action by the Office of the Public Guardian and the Ministry of Justice thereafter, resulting in more people completing an LPA without incurring the cost of legal advice and a concomitant reduction in the number of errors and rejected forms (Public Guardian Board 2010). Since then, the number of applications for LPAs to be registered has increased dramatically – between October 2008 and December 2009 just under 104 000 applications were made to the Office of the Public Guardian (Ministry of Justice 2010).
LPAs and the courts
During the first 12 months from October 2007, all 24 LPA cases that came before the Court of Protection involved LPAs for property and financial affairs (although two cases involved a donor who had made both types of LPA; Reference LushLush 2009).
As with any new statute, there is unsurprisingly an increase in court cases as the statute is tested, clarified and refined. Between January 2009 and December 2009 just over 300 LPA cases came before the Court of Protection (Ministry of Justice 2010). Cases being brought to the court were mainly due to LPA objections by interested parties and LPA validity applications made by the Public Guardian (where there are questions about the validity of an LPA, the Public Guardian is prevented from registering the document and must apply to the Court of Protection to determine whether or not the document is valid).
LPA case law
The following cases from the Court of Protection highlight pertinent issues for clinicians.
Assessment of capacity to revoke a registered EPA
In the case of Re Cloutt (2008), the 87-year-old donor revoked a registered EPA, replacing it a few days later with an LPA. A solicitor and consultant psychiatrist witnessed both the deed of revocation for the EPA and the relevant parts of the LPA. The LPA attorney applied to court for an order confirming the revocation of the EPA (as required by the Mental Capacity Act 2005). The court, in upholding the central tenet of the Act (that assessment of capacity is decision-specific), required separate evidence from the solicitor and the psychiatrist relating to both the capacity of the donor to revoke the EPA and the capacity to create the LPA, which the donor did indeed satisfy (the capacity to create an LPA is not the same as capacity to revoke an EPA).
The certificate provider discussing the LPA with the donor in the presence of the attorney
The Office of the Public Guardian guidance is that a certificate provider at first instance should discuss the contents of an LPA with the donor while not in the presence of the chosen attorney(s) ‘if at all possible’ to form an opinion and ensuring that the donor can communicate freely (it does, however, say that there may be ‘exceptional circumstances’ when this may not be possible). The 2005 Act empowers the Public Guardian to reject an application to register an LPA on the grounds that there is either a defect in completing the form or where there has been a procedural defect in the execution and completion of the form(s).
In the case of Re Gibbs (2008), the 86-year-old donor, who had a diagnosis of dementia, made out two LPAs. The donor’s general practitioner (GP) incorrectly completed Part B of both forms (inappropriately ticking boxes to say that he had discussed the LPA with the donor alone but also that the attorneys had been present). The GP needed to confirm in writing that he had indeed interviewed the donor alone and in the presence of the attorneys to correct this error, as the Public Guardian refused to register the LPA (causing a delay of 6 months). A similar mistake occurred in the case of Re Bullock (2009) where the certificate provider did not tick the box to confirm that they had discussed the LPA with the donor and that the attorney was not present. Whereas the Public Guardian refused registration on the grounds that the LPA document was incorrectly completed, the Court, in exercising its discretion under the 2005 Act, declared that the form, with this minor aberration, should be treated as if it had been made out appropriately and the LPA was subsequently registered.
Capacity to make an LPA
In the case of Re Collis (2010), there was a dispute as to whether the donor had the requisite capacity when making a property and financial affairs LPA. The judge analysed opposing views from a solicitor and doctor involved and ruled that it was more than likely that Mr Collis was incapable of managing his property and affairs in a ‘general sense’, but this did not automatically mean that he was incapable of executing an LPA. In doing so, he reinforced that mental capacity was both issue- and time-specific. He explained that mental capacity being issue-specific meant ‘that the capacity required to create an LPA is not the same as the capacity to manage one’s property and financial affairs generally, or the capacity to make a will or a gift or a loan, or the capacity to decide on a certain course of medical treatment, or the capacity to decide whether to live in a residential care home’. On capacity being time-specific, he said that this focused on the ‘particular time when a decision is made or has to be made’ and ‘[t]he fact that, after just a few minutes, or on the following day, a person cannot recall having made a particular decision doesn’t automatically mean that he or she lacked the capacity to make that decision, or that the decision is invalid’. The judge preferred the evidence from the solicitor, which was both issue- and time-specific, and held the donor did have the requisite capacity and hence had made a valid LPA. (The judgment in Collis and the Mental Capacity Act Code of Practice demonstrate the differences between an LPA and an EPA – Table 1.)
Differences between an LPA and an EPA
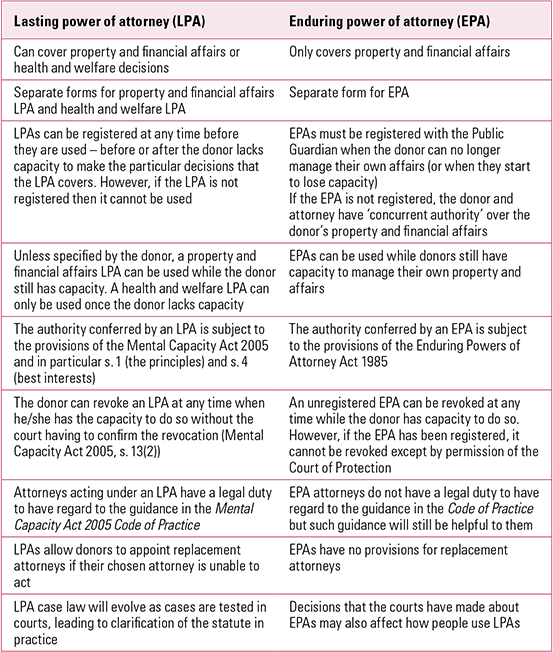
Clarity needed when devising restrictions and provisions
The following cases provide guidance when setting out restrictions and provisions in LPA documents. In the case of Re Azancot (2009), the donor of a health and welfare LPA inserted a restriction that her attorneys could only act in the event that she was ‘physically or mentally incapacitated and there is written medical evidence to that effect’. The words ‘physically or’ were removed by the Public Guardian because under s. 11(7) of the Mental Capacity Act a health and welfare attorney can only make decisions if the donor lacks mental capacity and not physical capacity. In the case of Re Thrussell (2010), the court removed a provision whereby the donor directed her attorneys to consult with X ‘in respect of any major decision’ because this was ‘so uncertain as to be unworkable’.
Defective execution of LPAs
As noted above, the defective execution of an LPA may affect its registration by the Public Guardian. In the case of Re Murdoch (2009), there were several mistakes in completing the document. The court upheld the Public Guardian’s refusal to register the document because the multiple errors in its execution were ‘too fundamental’. However, courts do have discretion under the Mental Capacity Act 2005 to declare an LPA that has not been submitted in the appropriate form to be treated as if it were, if it is satisfied that the person executing the document intended to create an LPA. This discretion was applied in the cases of Re M Crook (2010) and Re Helmsley (2009), whereby documents with minor defects were treated as if they had been appropriately completed.
The role of the clinician
An attorney or donor may request a doctor to act as the ‘certificate provider’. The role of the certificate provider is to confirm that the donor has the capacity to understand the significance of the LPA. The certificate provider also needs to certify that no undue pressure or fraud is involved. As noted above, it is important that the clinician assesses the donor on their own. In addition, the certificate provider can also be an ‘independent witness’, required to witness the attorney(s) signing the document. A solicitor may request a doctor to assess and confirm that a patient has the capacity to arrange an LPA if they feel unable to do this themselves (for example, in more difficult cases). A doctor may also be requested to assess and confirm that a patient has lost capacity, particularly for health and welfare LPAs where the attorney has no power to act until the donor loses capacity. A study by Reference Gregory, Roked and JonesGregory and colleagues (2007) found that clinicians were often asked to retrospectively assess a patient’s capacity to create an EPA. The study comprised 80 patients with Alzheimer’s disease and found that a Mini-Mental State Examination (MMSE; Reference Folstein, Folstein and McHughFolstein 1975) cut-off score of 18 gave the optimal sensitivity and specificity to aid clinicians in deciding whether or not a patient has capacity to create an EPA. Furthermore, they commented that the results of the study were relevant to patients creating LPAs but that it was possible that an even higher level of capacity would be required to create this more complex and extensive power. Therefore, a higher MMSE cut-off score might be required to discriminate capacity status (of course, deciding capacity solely on a single MMSE score is inappropriate but it can be helpful as part of the overall capacity assessment). Other aides for clinicians that were acceptable to both users and providers were easy-to-follow care pathways for powers of attorney and advance decisions (Reference Bisson, Hampton and RosserBisson 2009). This pilot study by Bisson et al was in relation to people with Huntingdon’s disease, many of whom will, at some stage, lose capacity to determine their ongoing care. There were three pathways devised for three stages of the assessment:
-
1 introduction of advance decisions and powers of attorney
-
2 education and capacity assessment process
-
3 post-assessment administrative pathway.
Although optimal delivery of this model required significant clinical and administrative commitment and resources, Bisson and colleagues believe that such a pathway process could be incorporated into a variety of chronic disease management services and clinical care pathways.
No formal test has yet evolved for assessing capacity for making an LPA, but previous jurisprudence pertaining to EPAs has produced a test (Reference MacFarlaneMacFarlane 1988) that could be utilised when assessing capacity for an LPA. To create a valid EPA, the donor should understand all three limbs of a test:
-
1 (if such be the terms of the power) that the attorney will be able to assume complete authority over the donor’s affairs; and
-
2 (if such be the terms of the power) that the attorney will, in general, be able to do anything with the donor’s property that the donor could have done; and
-
3 that the authority will continue if the donor should be or becomes mentally incapable but that, in that event, the power will be irrevocable without the confirmation of the Court of Protection.
Potential problems with LPAs
New statute law will inevitably evolve as it is tested, clarified and refined by courts and this is already the case for LPAs. Potential problematic areas have already emerged from case law, as noted above (Box 3).
Lasting power of attorney (LPA) guidance for clinicians
Clinicians should ensure that:
-
• they possess sufficient knowledge (of the donor and Mental Capacity Act principles) and have the experience to provide a formal report of capacity for an LPA
-
• they are familiar with the LPA forms (http://www.justice.gov.uk/global/forms/opg/lasting-power-of-attorney/index.htm)
-
• they meet and interview the donor, on more than one occasion if needs be, to clarify any assessment of capacity issues
-
• where relevant, solicitors have expressed (it is advisable to get such requests in writing):
-
for what purpose a capacity assessment is being sought (e.g. creating an LPA, making a will)
-
why a medical opinion is sought
-
whether there is a dispute or disagreement in the matter
-
During the assessment of capacity the clinician should:
-
• act in accordance with the Mental Capacity Act and guidance in the Code of Practice, paying attention to the fact that capacity is both issue- and time-specific
-
• perform and document a thorough assessment of the donor’s mental state and include, where relevant, an assessment of their cognitive function, for example, Mini-Mental State Examination score (Reference Folstein, Folstein and McHughFolstein 1975)
-
• ensure that the attorney(s) are not present during the assessment
-
• where relevant, ensure that the donor understands the differences between and limitations pertinent to each restriction and guidance made in the LPA
-
• ensure that the donor understands the nature of the health and welfare decisions that the attorney can make on their behalf (Box 2)
-
• be mindful that a health and welfare LPA includes an option for allowing the attorney(s) to make decisions about life-sustaining treatment; the donor’s capacity to make such decisions should be made clear
-
• be aware that, if the donor is detained under the Mental Health Act, the attorney no longer has the right to consent or refuse treatment on behalf of the donor
When providing a report to a solicitor, the clinician should:
-
• be specific to the pertaining issue, explaining and justifying their reasoning in detail
-
• be aware that they could be called to court to provide evidence based on the report
Where there is disagreement with an attorney:
-
• for example, regarding treatment of a donor, first try to resolve the issue through discussion (which may involve explanation and education regarding the Mental Capacity Act and/or treatment principles; direct referral to the Code of Practice can be of help here), but be prepared to consider referral for further mediation or referral to the Court of Protection to review and decide should agreement not be forthcoming
Where exploitation or abuse of a donor is suspected:
-
• the Mental Capacity Act Code of Practice advises contacting and seeking advice from the Office of the Public Guardian, which can direct a Court of Protection visitor to meet the attorney to investigate
-
• in serious cases the Court of Protection can revoke or prevent the registration of an LPA where: somebody has used fraud or undue pressure to get the donor to make the LPA; the attorney has done something that they are not authorised to do; or the attorney has behaved or is planning to behave in a way that is not in the donor’s best interests
Differing decisions regarding healthcare
Some clinicians have reservations regarding the introduction of LPAs that cover healthcare in the UK. In a survey of geriatricians, only 47% supported the idea of such an LPA and, although it was thought to encourage advance discussion on end-of-life care, there was little evidence that the decisions made by a patient and their proxy concurred (Reference Schiff, Sacares and SnookSchiff 2006). A study by Reference Seckler, Meier and MulvihillSeckler and colleagues (1991) found that even close relatives were not good at making judgements on behalf of others. This suggests that, as a practical means of extending the wishes of an incapacitated patient, health and welfare LPAs may not result in the treatment that the patient would have wanted. For example, the study found that few patients had discussed their resuscitation preferences with either a family member (16%) or their physician (7%) and this cast doubt on the usefulness of a strict substituted judgement standard as an approach to medical decision-making for patients with diminished mental capacity. (There is also wider concern regarding the public’s overall lack of awareness of available options for advance healthcare decision-making (Reference SamantaSamanta 2009).) The use of additional statements clarifying the intent of the donor has been advocated to improve the acceptance by doctors of an attorney’s decision to decline life-prolonging treatment for that person (Reference Corke and MannCorke 2009).
Assessing loss of capacity
The issue of capacity is obviously core to the implementation of an LPA. A review by Reference JonesJones (2005) suggests that although the Mental Capacity Act stresses that LPAs can only make decisions that the donors are incapable of making themselves, there is a clear potential for their misuse in terms of being inaccurately perceived as an ‘all-or-nothing’ phenomenon. Jones further suggests that loss of capacity in one area could lead to the view that an LPA was now ‘active’, giving the attorney wide-ranging powers over finance, health and welfare. Despite the improved LPA forms and guidance, many attorneys will have limited knowledge of the Mental Capacity Act and the Code of Practice and may have difficulty knowing exactly when the donor loses capacity. After an LPA has been registered, there is no further legal requirement to have the donor’s capacity assessed before acting on their behalf and as such an attorney may act too soon or too late.
Determining best interests
The introduction of the health and welfare LPA represents some advancement in being able to promote self-determined prospective choice. An LPA could offer a more flexible solution than an advance directive, which is constrained by requirements of applicability and validity (Reference SamantaSamanta 2009). However, a criticism of attorney powers is that the decision-making standard is essentially objective and that such powers do not extend to a substituted judgement approach (Reference SamantaSamanta 2009). Another potential issue would be to what extent a healthcare team is satisfied that the attorney is acting in the donor’s best interests in circumstances where the proxy decision does not align with medical wisdom (conversely, a potential weakness is the failure of the Mental Capacity Act 2005 to define sanctions for non-compliance by attorneys). Similarly, there may be issues where the donor’s priority of choices is unknown or cannot be ascertained, when in such circumstances it would seem appropriate to invoke best interests as the basis for decision-making (Reference SamantaSamanta 2009).
Reference SamantaSamanta (2009), in an in-depth review of LPAs for healthcare, considers it ‘somewhat incongruous’ that the 2005 Act has chosen to impose the best-interests benchmark for attorney decision-making (a ‘subjectively modified’ best-interests standard), as this is the weakest standard for respecting previous self-determined choice. Samanta also astutely point out the paradox of a person appointing a healthcare attorney but not informing that attorney of their wishes regarding treatment preferences in the event of subsequent incapacity.
Disagreements
Where there are disagreements arising between a doctor and an attorney as to what is in the best interests of the patient that cannot be resolved through discussion at first instance (which may revolve around Mental Capacity Act aspects with which the attorney may be unfamiliar), the Court of Protection should be consulted and requested to arbitrate. While a decision is awaited, the 2005 Act allows for the continuation of life-sustaining treatment or treatment to prevent serious deterioration of a condition, even if this conflicts with the decision of the attorney. Healthcare professionals should be mindful that in the same way as a competent adult has the right to refuse treatment, a valid documented refusal of treatment as part of an LPA should, in principle, give the attorney the power to enforce that refusal. Failure of the professional to respect that refusal may amount to assault and battery. There may also be occasions where the attorney and the donor disagree on a decision. In this situation, a clinician may be requested to confirm that the donor does or does not lack capacity to make a specific decision.
Some consider that the LPA offers little more than a ‘taster’ for prospective self-determination and that the new statute, in the form of the Mental Capacity Act, is unlikely to bring ‘major change’ (Reference SamantaSamanta 2009). Nevertheless, it will be interesting to see how the use of LPAs, especially that of the novel health and welfare LPA, evolves in everyday practice.
MCQs
Select the single best option for each question stem
-
1 A lasting power of attorney:
-
a can be used before its registration with the Office of the Public Guardian
-
b health and welfare decision can be made by the attorney when the donor has capacity
-
c can be registered at any time before or after the donor lacks capacity
-
d cannot be used following the implementation of the Mental Capacity Act in 2007
-
e means that attorneys are exempt from following the guidelines in the Mental Capacity Act Code of Practice.
-
-
2 With regard to powers of attorney:
-
a an ordinary power of attorney can be used when the donor loses capacity
-
b ordinary powers of attorney can be used in situations where capacity is likely to fluctuate
-
c attorneys should complete Part A of the new LPA form
-
d the Ordinary Powers of Attorney Act replaced the Enduring Powers of Attorney Act in 1985
-
e clinicians should complete Part B of the new LPA form.
-
-
3 With regard to powers of attorney:
-
a an EPA can cover health and welfare decisions
-
b an EPA can only be used when the donor loses capacity
-
c EPAs have provisions for replacement attorneys
-
d an LPA can be revoked by the donor at any time before its registration, provided the donor retains the relevant capacity
-
e the Court of Protection need not be involved following revocation of power of an LPA when the donor lacks capacity.
-
-
4 With regard to health and welfare LPAs:
-
a an attorney can consent on the donor’s behalf to a decree of divorce or dissolution of a civil partnership
-
b an attorney or replacement attorney can act as a witness
-
c attorneys cannot consent to or refuse medical examinations and treatment when the donor has allowed them to do so in the LPA form
-
d an attorney can decide who the donor may have contact with
-
e a donor can choose an attorney to be the certificate provider.
-
-
5 With regard to health and welfare LPAs:
-
a when the donor is detained under the Mental Health Act, the attorney, as specified in the LPA, can make decisions about treatment of the donor’s mental disorder
-
b the donor cannot specify any restrictions on the attorney’s authority
-
c a certificate provider or a ‘named person’ cannot act as a witness
-
d if the donor has a named person, two people should act as certificate providers
-
e an attorney has no power to consent to or refuse life-sustaining treatment, unless the LPA document expressly authorises this.
-
MCQ answers

| 1 | c | 2 | e | 3 | d | 4 | d | 5 | e |



eLetters
No eLetters have been published for this article.