INTRODUCTION
There is nothing in the literature of medicine to compare with the phantasmagoria of disorder manifested in the course of this strange malady [Reference McKenzie1].
How did it come about that a novel form of encephalitis, encephalitis lethargica (EL) or ‘sleepy sickness’, appeared in central Europe about 1917, became epidemic in Europe simultaneously with the second, most virulent, wave of the influenza pandemic of 1918/1919, spread around the world with increasing severity up to the mid-1920s, and then petered out in its acute form after 1927? The question has never been satisfactorily answered. Some contemporary observers persisted in associating EL with pandemic influenza but most were sceptical, and neither the origin of EL, its spread, its seasonal recurrence, its decline in its acute form or, most importantly, its cause, have ever been satisfactorily explained. In spite, therefore, of the voluminous clinical literature [Reference Hall2, 3] and the extensive although technically very limited laboratory investigations that took place in the 1920s, it must now remain doubtful whether the cause of EL will ever definitely be established, at least until a possible recurrence of it in epidemic form.
On the other hand, the scope for laboratory investigation is now much greater, and with pandemic influenza now the focus of attention, a re-examination of the notions that EL was a sequela of influenza, or some other acute infection or affliction, is justified. While numerically the mortality due to EL was modest compared with that of influenza in 1918/1919, up to a half of the EL cases ultimately died of it or were left permanently brain damaged. In excess of 65 000 cases were reported worldwide, and EL institutionalized many of the survivors for the remainder of their lives [Reference Sacks4]. Sporadic cases, diagnosed on clinical grounds, are still thought to be occurring [Reference Greenough and Davis5] and these might possibly reveal the cause of the disease as it occurred in epidemic form in the decade following 1918. Like influenza, EL was at that time a global phenomenon, and its recurrence in that guise cannot be ruled out.
Some clinical descriptions of EL
Throughout its period of prevalence EL was a clinical diagnosis, not confirmable by laboratory tests. The first cases had been reported in Vienna by von Economo, in 1917. He described seven severe cases, two fatal, of an acute encephalitis of which the main features were fever, headache, intense lethargy, sleep disturbance and ocular pareses. On account of the First World War this was not at first known to the Frenchmen Cruchet, Moutier and Calmette who at much the same time reported 40 similar cases in soldiers in Northern France [Reference Von Economo6, Reference Cruchet, Moutier and Calmette7]; but thereafter reports of the disease, which von Economo named ‘encephalitis lethargica’; and others named after him or Cruchet, were legion, especially in the years immediately following the influenza pandemic of 1918/1919.
Ten years into the EL epidemic McKenzie gave a vivid description of its clinical range:
profound and prolonged torpor, protracted and resistive sleeplessness, paralysis, violent jactitation, chorea, athetosis and convulsing pains referable to the head, limbs and internal organs, every conceivable anomaly of movement of the external and intrinsic muscles of the eye, giddiness and rotatory displacement of the body, abnormal reactions of alimentation, circulation and respiration, delirium, maniacal excitement and fever comprise some of the outstanding features of this picture of chaos [Reference McKenzie1].
By the time McKenzie published this, EL had come to be regarded as a clinical presentation distinct from that of polioencephalomyelitis, Wernicke's syndrome or a toxigenic illness such as botulism. Some still referred its origin back to the influenza pandemic of 1918/1919 [Reference Greenwood8], but in McKenzie's and most others' opinion EL was not a post-infective complication of influenza but a separate infective entity.
A great many individual clinical descriptions of acute EL are available but perhaps the most arresting is an anonymous account by a young American physician of his own illness. This occurred early in 1919, 7 weeks after a coryza that may have been a mild bout of influenza [9]. The author apparently recovered from acute EL, but other professional witnesses of EL noted its persistent or recurrent, often downhill, course, with sudden death a feature both of the acute, the recurrent and the chronic phases. In McKenzie's series of mostly young patients ‘not more than 60 out of 300 were healthy two years after onset’, and chronic EL could linger for much longer.
Later The Lancet, reviewing the range of clinical signs and sequelae associated with EL, highlighted its psychotic residua. It even ventured to suggest that the ‘violent and aggressive behaviour and gesticulation of Hitler may have been due, at least partly, to EL’ [10]. Other twentieth-century figures whose instability or wayward behaviour has been anecdotally attributed to EL are Stalin, Kafka and Greta Garbo.
Analyses of the clinical presentations of EL were made by several contemporary neurologists, as recently reviewed [Reference Vilensky and Gilman11], and it was suggested that in certain epidemic years and regions EL took on a particular form. In 1943 Sir Arthur Hall, at the close of an entire career spent studying the disease, wrote that the frequent recurrences of EL, sometimes after only mild acute disease, led him to believe that its cause must be a latent virus which could at any time reactivate with consequent clinical relapse [Reference Hall12]. By then the acute diagnosis was very rarely being made, although each year still saw significant mortality in EL cases first diagnosed decades earlier. Relapses of EL were often as grave as the preceding acute illness, bearing out Hall's concept of an embedded infection capable of being reignited, as is the case with Herpes simplex.
The pathology of EL
In the acute stage the post-mortem histological appearances of the EL brain were usually normal, but more advanced cases showed varying degrees of vascular congestion and perivascular lymphocytic cuffing. In chronic EL there was less inflammation but degeneration in the midbrain, especially of the oculomotor nuclei and the substantia nigra [Reference Buzzard and Greenfield13]. During the epidemic phase the typical clinical picture reflected this, distinguishing EL from a range of other encephalitic conditions most of which were first characterized in the 1920s or 1930s (Table 1). Some of these were ascribable to specific viruses, but investigators were divided on whether to associate EL with a specific virus, with influenza itself, or with some non-infective cause. Some researchers claimed to have seen viral inclusion bodies in sections of EL brains, but Cowdry, who classified these bodies in 1928, rejected this [Reference Cowdry and Rivers14].
Features of influenza, encephalitis lethargica and other human encephalitides
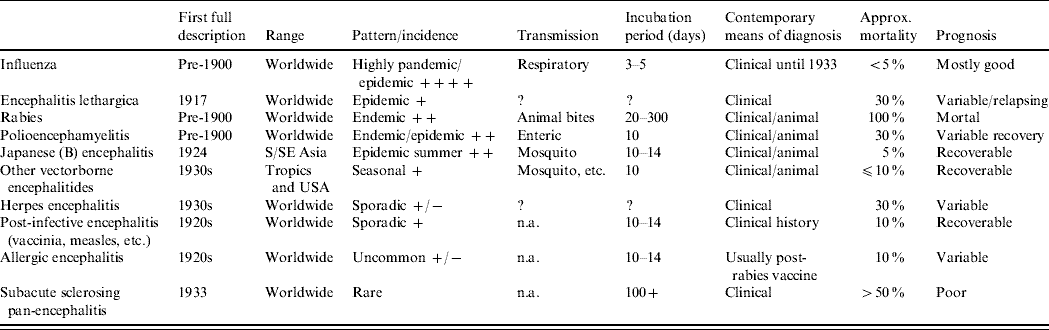
Contemporary attempts to transmit an EL virus and reproduce an EL-like illness by inoculating laboratory animals with post-mortem brain extracts were unrewarding in that no consistent clinical effect was noted and repeated passage was not achieved. Intra-cerebral inoculation of mice, rabbits and macaques all produced inconsistent results [Reference Greenfield15, Reference McIntosh16]. Virological techniques such as inoculation of embryonated eggs or tissue cultures were not available in the 1920s, so other attempts at virus isolation and passage could not be pursued. In so far as the animal experiments ruled out polioencephalomyelitis and some vector-borne encephalitides for which particular animal susceptibilities had already been established they were of value; but no reproducible effect in animals was identified that might point to a specific infection.
The epidemiology of EL
It is by re-evaluating the epidemiology of EL that there is perhaps the best chance of finding new clues to its cause. Though EL may never have been seen before von Economo's first case, some physicians did recall a form of sleepy sickness called ‘nona’ in Northern Italy and Austro-Hungary about the time that a previous pandemic of influenza had swept around the world between 1889 and 1893 [17]. However, any relationship between nona and EL is speculative and EL, unless very loosely clinically defined, only became epidemic in Europe and North America during the second wave of the pandemic of influenza in October and November 1918. By the beginning of 1919 EL had become sufficiently alarming in England and Wales for it to be made a notifiable disease, and it recurred there in successive years, as well as spreading from Europe to other parts of the world. In its acute form EL presented with annual, mostly winter, peaks of varying size and severity. In England and Wales its incidence was highest in 1924 when 5039 cases were notified, with 1704 deaths. The incidence of EL diminished everywhere in the late 1920s, and thereafter there were more deaths among chronic than acute cases.
EL showed no consistent gender, socio-economic or occupational biases. All ages were affected, including newborns apparently affected following EL late in pregnancy [18]. Clusters of EL cases were rare, but a few were described. In England they included an outbreak in a residential home in Derby in August 1919 where 12 out of 22 girls were affected with five deaths [Reference MacNalty19], and another in the school at an isolated village in Warwickshire in 1922 where there were four cases within 4 weeks in a small class [Reference Fyfe20]. Generally, though, observers remarked on the absence of familial or other groups of cases. EL may, therefore, either have been due to an unusual pathogen or, in its epidemic form, been an uncommon complication of a common infection. One paper, referring to cases of EL in the Wilhelmina Province of Sweden, described mild febrile attacks, formes frustes, in family contacts [Reference Kling and Liljenquist21]. This would suggest that, like poliomyelitis, EL was the occasionally severe clinical expression of a much more prevalent, usually trivial, infection.
Causal theories
The decade-long epidemic of EL was ascribed to several causes and, 80 years on, these theories can be summarized in an updated form:
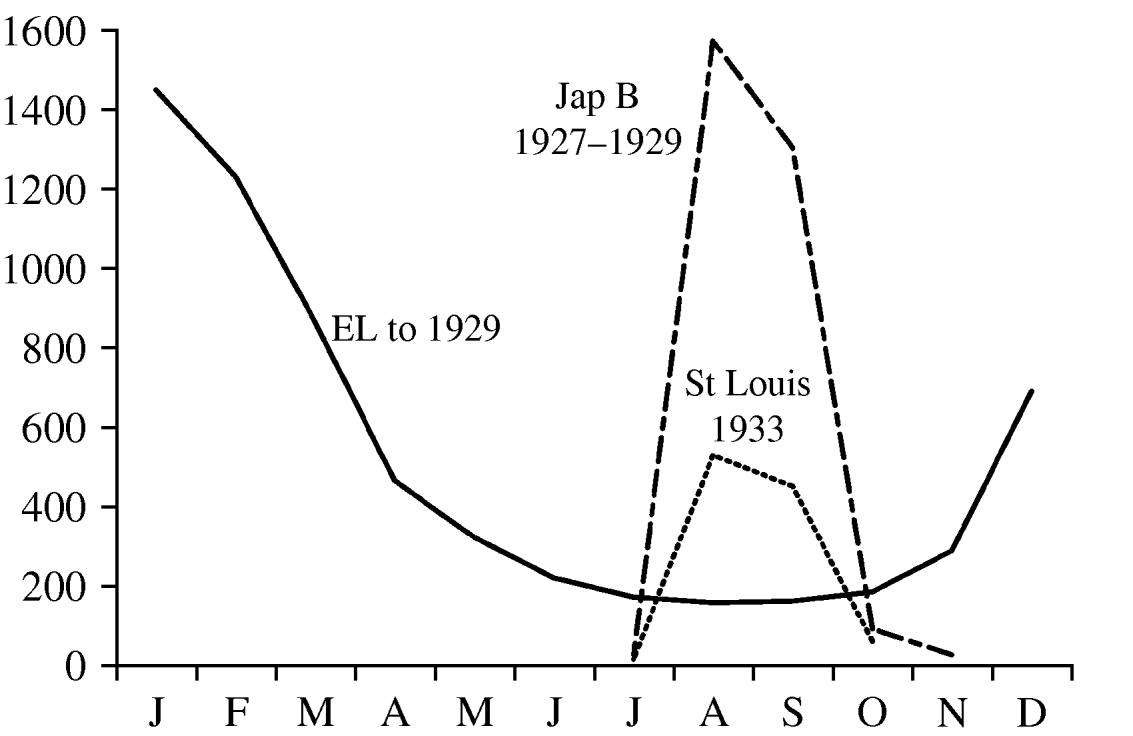
(1) Most plausibly, perhaps, it was suggested that EL was an acute focal encephalitis caused by a neurotropic virus epidemiologically comparable to polioencephalomyelitis as experienced, e.g. in the devastating summer 1916 epidemic in New York. The frequently described EL prodrome of fever and pharyngitis and the seemingly random occurrence of cases of EL were similar to polio; but polio had a different seasonality (Fig. 1) and a different central nervous system target. Although transmission of the putative EL virus was probably by the respiratory or enteric route no such virus was ever found. However, it should be borne in mind that up to the early 1950s formidable technical constraints surrounded virus tissue culture, and that the belief that poliovirus was exclusively neurotropic delayed the in vitro isolation even of that virus until 1949. By that time the EL epidemic was long over.
(2) EL was due to the activation of a latent human virus by an attack of influenza or some other acute insult, as suggested by some researchers, particularly after animal inoculations of brain material had revealed a latent neural herpes virus of rabbits [Reference Greenfield15]. The often recurrent nature of EL is consistent with this latency, but hard evidence in the shape of a persistent virus is still lacking.
(3) EL was exclusively a post-influenzal disease, as a diminishing band of clinicians and epidemiologists went on believing. The emergence of EL was roughly coincident with that of the influenza virus strain that became pandemic in 1918, and the idea drew further support from the recognition in the 1920s of post-vaccinial and post-measles encephalitis. However, both these latter had incubation periods of less than 2 weeks whereas the interval between the onset of EL and a preceding influenzal illness was usually longer and more variable so that any connection was more tenuous. Nevertheless, some post-infective neurological conditions first clearly described during the EL era, such as canine distemper and human subacute sclerosing panencephalitis, did have longer and more variable incubation periods and were also, like EL, chronic or recurrent. This may have encouraged some contemporaries to continue to relate EL to the 1918/1919 pandemic of influenza.
(4) It has sometimes been suggested that EL was a post-streptococcal illness, partly by clinical analogy with Sydenham's (i.e. rheumatic fever-associated) chorea. Sydenham's chorea typically presents 1–4 weeks after acute rheumatic fever with involuntary movements comparable to those of EL. It may recur several times, although usually this is over not more than 2 years, and on average 4 months [Reference Aron, Freeman and Carter22]. Between 1918 and 1921 several authors isolated ‘Wiesner's diplostreptococcus’ from EL patients. Wiesner had first isolated it from one of von Economo's patients, but this was before either grouping or M-typing of β-haemolytic streptococci had been described, and in his later writing von Economo remained sceptical about the aetiological role of a particular streptococcus. Recently, Dale and colleagues have again implicated Streptococcus pyogenes, postulating that EL-like disease initiates an autoimmune neural process. They have reported 20 cases with ‘EL phenotype’ [Reference Dale23], 60% of whom had a preceding pharyngitis, 65% raised ASO titres and 95% auto-antibodies to basal ganglia antigens. The authors write: ‘we believe an EL like syndrome is still prevalent and propose … [it] may be secondary to autoimmunity against deep grey matter antigens’.
(5) EL was a non-infectious condition due to a toxin or a dietary lack such as of thiamine, as was at first often suggested. At most, though, it seems that a non-infective process might have predisposed to EL. Due to war, economic deprivation was rife in Europe by 1917, yet EL did not spare the privileged classes and it can therefore scarcely have been wholly related to a vitamin or other dietary deficiency. Its spread across Europe and then other continents had the hallmarks of an infectious process even if any contagiousness was far from obvious, and the rapidity of spread after 1918 was perhaps referable to post-war demobilization.
(6) Finally, it has been suggested that EL was a ‘ragbag’ diagnosis, its true incidence inflated by other conditions even if there had at first been a nosological entity. There never having been any diagnostic serological, animal, or electrographical test for EL, the label given by von Economo in 1917 could easily attach itself to other clinical presentations. Conditions such as ‘epidemic hiccough’ were soon included, and illnesses comparable with Royal Free disease or chronic fatigue syndrome might have been notified as EL. The abnormal movements and behavioural abnormalities typical of acute and recurrent EL could have been interpreted as hysterical states lacking a histopathological basis.
Seasonal incidence of three forms of encephalitis: 7876 cases of encephalitis lethargica (EL) (up to 1929); 3118 cases of Japanese B encephalitis (Jap B) (1927–1929); and 1097 cases of St Louis encephalitis (1933). Acute EL was predominantly a winter illness (source: Matheson Commission, 3rd Report [3]).
DISCUSSION
With the current lively appreciation of pandemic influenza as a global health threat the question arises whether there is any evidence, or new interpretation, that points to a relationship between the notorious pandemic influenza virus strain of 1918/1919 and the concurrently emergent disease, EL. In 1982 Ravenholt & Foege published data suggesting that the apparently successful quarantining of American Samoa from influenza in 1919 spared those islands from EL in subsequent years [Reference Ravenholt and Foege24]. They also sought to show that the epidemic influenza years in Seattle after 1919 were followed by peaks of cases of EL. They judged these two sets of data ‘compelling’ evidence of a link between EL and the 1918/1919 strain of the influenza virus. However, few others have claimed as much and most researchers have argued to the contrary.
It might nevertheless be assumed that, epidemiologically, the behaviour of the 1918/1919 influenza virus was similar to that of other historical pandemic strains, i.e. it arose locally, perhaps before 1918, and spread globally over several seasons. Note that the previous, 1889, pandemic strain of influenza was still active 4 years later in the winter of 1893/1894 [Reference Parsons and Franklin25], and that the 1957 and 1968 strains of influenza A only became fully pandemic in 1958 and 1969, respectively. Influenza A H3N2 has remained seasonally epidemic ever since 1969. The 1918 strain may have been in circulation for a decade or more, consistent with EL being an acute disease related to influenza during the 1920s. A connection between the influenza pandemic of 1918/1919 and acute EL cannot be dismissed merely on the grounds that the latter slightly preceded the former and then persisted for more than a decade.
Recently RNA extracts from preserved brain tissue of some acute and chronic EL cases have been analysed for putative influenza A sequences, although with negative results [Reference McCall26]. These investigators [Reference Reid27] and another authoritative group [Reference Casals, Elizan and Yahr28] have also reviewed in depth the available information about EL and influenza. Both have concluded that influenza was not associated with the emergence of EL; but negative findings cannot be definitive and it remains the case that roughly coincident cases of influenza and EL were common. Even the belated discovery of an ‘EL virus’ would not entirely exclude a causative role for the influenza virus of 1918/1919, at least in the early cases of EL. As one author has argued, the ‘naysayers’ who deny a link between influenza virus and EL are obliged to identify a more plausible candidate virus [Reference Manriz29], and the only tenable argument to explain its absence would seem to be that the putative EL agent became extinct in humans around 1930, perhaps because the supply of susceptibles was by then exhausted. The EL virus might have remained latent, but there can now scarcely be any surviving chronic cases from whom it might be retrievable.
The contrary position is that the search for an EL virus should go on, and that any sporadic cases that are clinically diagnosed as EL should attract close virological analysis using molecular tools such as generic PCR primers. This is not just a matter of historical curiosity as EL might again become epidemic, perhaps in conjunction with influenza. Unfortunately, few if any of the more recently described clinical cases of EL have been comprehensively investigated by modern open-ended virological methods; there may even in future be difficulties in doing so should access to CNS specimens after death become constrained [Reference Furness30].
EL is a topic burdened with a high ratio of observational evidence to objective data. However, the considered contemporary clinical view was [Reference Flexner31], and most modern virological opinion is [Reference Reid27, Reference McCall32] against it having been a post-influenzal condition even though its secular spread in acute form matched that of a particularly virulent pandemic strain of influenza. It would nevertheless be prudent to include basic surveillance for EL in contingency plans for future influenza pandemics. The frequent recurrence and subsequent chronicity of EL warrant efforts to investigate its cause whenever sporadic cases now seem to occur. This is justified both because of the poor prognosis of EL itself and because its elucidation might contribute to a better understanding of various chronic neurological conditions, especially Parkinsonism. Apart from the threat of re-emergence of EL in an acute form it is as an infectious form of Parkinson's disease that it should perhaps now attract particular clinical [33] and pathological interest and investigation.
DECLARATION OF INTEREST
None.



