Introduction
Palliative care is “an approach that improves the quality of life of patients (adults and children) and their families who are facing the problems associated with life-threatening illness, through the prevention and relief of suffering by means of early identification and correct assessment and treatment of pain and other problems, whether physical, psychosocial or spiritual” (WHPCA 2020, 13). Palliative care and pain relief are the core components of Universal Health Coverage (UHC) (Knaul et al. Reference Knaul, Farmer and Krakauer2018). A study conducted in Ethiopia reported that the UHC in Ethiopia is very low (34%) (Eregata et al. Reference Eregata, Hailu and Memirie2019).
Ethiopia is one of the few African countries which recognizes palliative care in its national health plan. Ethiopia has developed the national palliative care guideline, and the role and responsibility of all 3-tier health-care system are described in this guideline (Federal Ministry of Health 2016). In addition, palliative care is incorporated as a fifth pillar in different national health-care plans and guidelines such as Health Sector Transformation Plan (Ministry of Health 2020-2020-2024), National Cancer Control Plan (Federal Ministry of Health 2015), Ethiopian primary health care clinical guidelines (Federal Ministry of Health 2017), National Strategic Action Plan for prevention and control of noncommunicable diseases (MOH 2014-2014-2016), and Ethiopia hospital transformation guidelines (MOH 2016).
In 2016, a national palliative care guideline was developed with an expanded focus, to articulate the role and responsibility of key players in palliative care practice at each level of the health system (Federal Ministry of Health 2015). However, to provide quality palliative care, nurses must be well-informed and have the training and skillset to provide needed services (Rosa et al. Reference Rosa, Buck and Squires2022a, Reference Rosa, Parekh de Campos and Abedini2022b; WHO 2020). In the National Cancer Control Plan, the government also planned to provide palliative care services in at least 50% of public health facilities by 2020 (Federal Ministry of Health 2015). Despite this, palliative care service is limited in a few nongovernmental organizations (NGOs) with the help of “iddir,” a self-help neighborhood association traditionally limited to assisting families during funerals, which started providing basic home-based care and support to patients with HIV and families (Kaba et al. Reference Kaba, de Fouw and Deribe2021; Reid et al. Reference Reid, Gudina and Ayers2018). Hence, Ethiopia is 1 of the 20 African countries categorized in isolated palliative care provision, because palliative care service in Ethiopia is limited in relation to size of the population and the services are donor dependant (Category 3a) (Clark et al. Reference Clark, Baur and Clelland2020; WHPCA 2020).
In addition, palliative care remains poorly understood and practiced, especially in regional Ethiopia (Zeru et al. Reference Zeru, Gerensea and Berihu2020b). There is inconsistent practice with limited knowledge evident in public and private hospitals (Kassa et al. Reference Kassa, Murugan and Zewdu2014), although a study in regional health settings found that nurses had a good level of palliative care knowledge (Zeru et al. Reference Zeru, Berihu and Gerensea2020a). These few Ethiopian studies examining the knowledge and practice of palliative care among nurses, only used quantitative data from those working in a few health-care settings, with none aimed to describe the barriers to poor practice (Kassa et al. Reference Kassa, Murugan and Zewdu2014; Zeru et al. Reference Zeru, Berihu and Gerensea2020a, Reference Zeru, Gerensea and Berihu2020b). Thus, there has been little work to highlight the underlying causes for low palliative care practice.
Our study used a mixed-method approach to measure and explore the barriers that prevent nurses from translating their theoretical knowledge into clinical practice, with participants drawn from various settings and professional backgrounds. In addition to nurses and health facilities, we sought the views of policymakers, educators in higher institutions of learning, and other professionals such as pharmacists and doctors involved in palliative care practice. As such, this study provides a more comprehensive picture of the barriers to translating theoretical knowledge of palliative care into clinical practice in Ethiopia, than previous studies (Kassa et al. Reference Kassa, Murugan and Zewdu2014; Zeru et al. Reference Zeru, Berihu and Gerensea2020a, Reference Zeru, Gerensea and Berihu2020b). The results are expected to inform policy and improve palliative care practice.
Methods
Design
A mixed-method study was undertaken as part of a larger case study on palliative care in regional Ethiopia. Interviews were conducted with 2 regional health bureau representatives, 7 pharmacists, 5 doctors, 4 health officers (clinical officers), and 17 nurses in leadership roles, including chief nursing officers.
Inclusion criteria
Nurses with experience caring for patients with chronic and terminal illnesses and those who held a diploma or above training were eligible to participate. For the cross-sectional survey, nurses working in medical and surgical wards, oncology and Tuberculosis units, and antiretroviral therapy (ART) clinics were targeted. Purposive sampling was used to recruit nurses caring for patients with chronic and terminal illnesses.
Participants and settings
This study was conducted in 1 of the 11 administrative regions in Ethiopia (Tesema et al. Reference Tesema, Peiris and Abimbola2022), with a population of 5.7 million (Central Statistics Agency 2022). Ethiopia follows a 3-tier health-care system, namely primary health-care units, secondary care (general hospital), and tertiary care (comprehensive specialized hospital) (Ministry of Health 2020-2020-2024). Each health-care level has their own responsibilities and are networked to each other by a referral system. The primary health-care units includes 1 primary hospital, which can serve a population of about 100,000; 4 health centers (each serving a population of 25,000), and 5 health posts are attached to each health center (each health post serving for about 5,000 people). The second level includes general hospitals, and each hospital provides service for an average of 1 million people, while the third level comprises specialized hospitals for about 5 million people (Eregata et al. Reference Eregata, Hailu and Memirie2019; Ministry of Health 2020-2024).
The study region comprises 2 comprehensive specialized hospitals administered by the federal government, 16 general hospitals, 29 primary hospitals, 233 health centers, and 712 satellite health posts (Gesesew et al. Reference Gesesew, Berhane and Siraj2021). At the time of the study, there were 19,324 health workers in the region, of whom 4,402 were nurses with at least a diploma qualification (Gesesew et al. Reference Gesesew, Berhane and Siraj2021). Nursing education occurs at 4 universities and in 2 regional health colleges. The Federal government manages 4 universities, while the regional government administers 2 health science colleges (Nyssen et al. Reference Nyssen, Negash and Deckers2021; Zeru et al. Reference Zeru, Berihu and Gerensea2020a).
Data collection and measurements
Data collection was undertaken between October 2018 and January 2019. A self-administered 4-part anonymous survey comprised sociodemographic variables; the Palliative Care Quiz for Nursing (PCQN) (Ross et al. Reference Ross, McDonald and McGuinness1996) modified by Kassa et al. (Reference Kassa, Murugan and Zewdu2014) for the Ethiopian context; nurses’ attitudes using the Frommelt Attitudes Toward Care of the Dying Scale (FATCOD) Form B (Mastroianni et al. Reference Mastroianni, Piredda and Taboga2015) modified by Kassa et al. (Reference Kassa, Murugan and Zewdu2014) for the Ethiopian context; and 23 questions about palliative care practice adapted from related works of literature (Callaway et al. Reference Callaway, Connor and Foley2018). Qualitative interviews were conducted with 42 participants from all levels of health-care institutions, the regional health bureau and 2 educational institutes. Thirty-eight of the 42 respondents were analyzed because the interviewees were duplicate informants, and we randomly excluded them. Of these, 15 nurses in leadership roles at all health-care institutions were interviewed. For the qualitative data, purposive sampling strategy was used to recruit the study participants who are engaged in leadership roles in the selected study settings. The interview guide was translated from English to the local language. The topics of interview questions were based on 1 of the 4 components of public health strategy (education) (Callaway et al. Reference Callaway, Connor and Foley2018).
Data analysis
Quantitative survey results were entered into the Statistical Package for the Social Science software (version 25). Audio files of the qualitative findings were transcribed verbatim by the author (AA) in the language of the interview. The author (AA) imported all the transcripts into NVivo 12 software and used the software for coding in addition to manual coding and analyzing the qualitative data. A thematic analysis technique was used for analyzing qualitative data. The thematic analysis utilized the following 6 steps: becoming familiar with the data set by transcribing; reading and re-reading and taking notes from the data; coding core features from the data; searching and gathering the relevant data and generating initial themes; developing potential themes and review; checking themes for relevance with the codes defining themes and writing the scholarly report of the final analysis (Braun and Clark Reference Braun and Clark2022).
The research team undertook several strategies to increase reflexivity and limit the researcher’s views being imposed on the data and impacted the study’s outcome. From the beginning of the research process, the first author identifies any personal beliefs that may have incidentally affected the research through regularly taking notes on the data. The research team also discussed and interpreted the data in their 40-night meeting.
Rigor of qualitative research operationalized using 4 criteria including credibility, dependability, confirmability, and transferability (Cypress Reference Cypress2017). To enhance credibility of this study, 5 months was allocated for data collection that helped the first author to be fully engaged in the data collection and the author is very familiar with the country context. To ensure dependability, the first author documented the raw data, transcripts, and all steps of data analysis, and the discussion and decision made for the analysis were described to be accurately judged by external experts. To enhance confirmability, the interviews and transcripts, along with the coding, were checked by other researcher who was specialized with qualitative research and confirmed the accuracy of coding. To ensure transferability, the author provided the detail description of each study process that is sufficiently rich for other researchers, to enables them to make informed decision about the generalization of the findings. Finally, the qualitative data (interviews) and quantitative results were triangulated and used to describe the barriers to palliative care practice (O’Cathain et al. Reference O’Cathain, Murphy and Nicholl2010).
Results
Sociodemographic characteristics of study participants
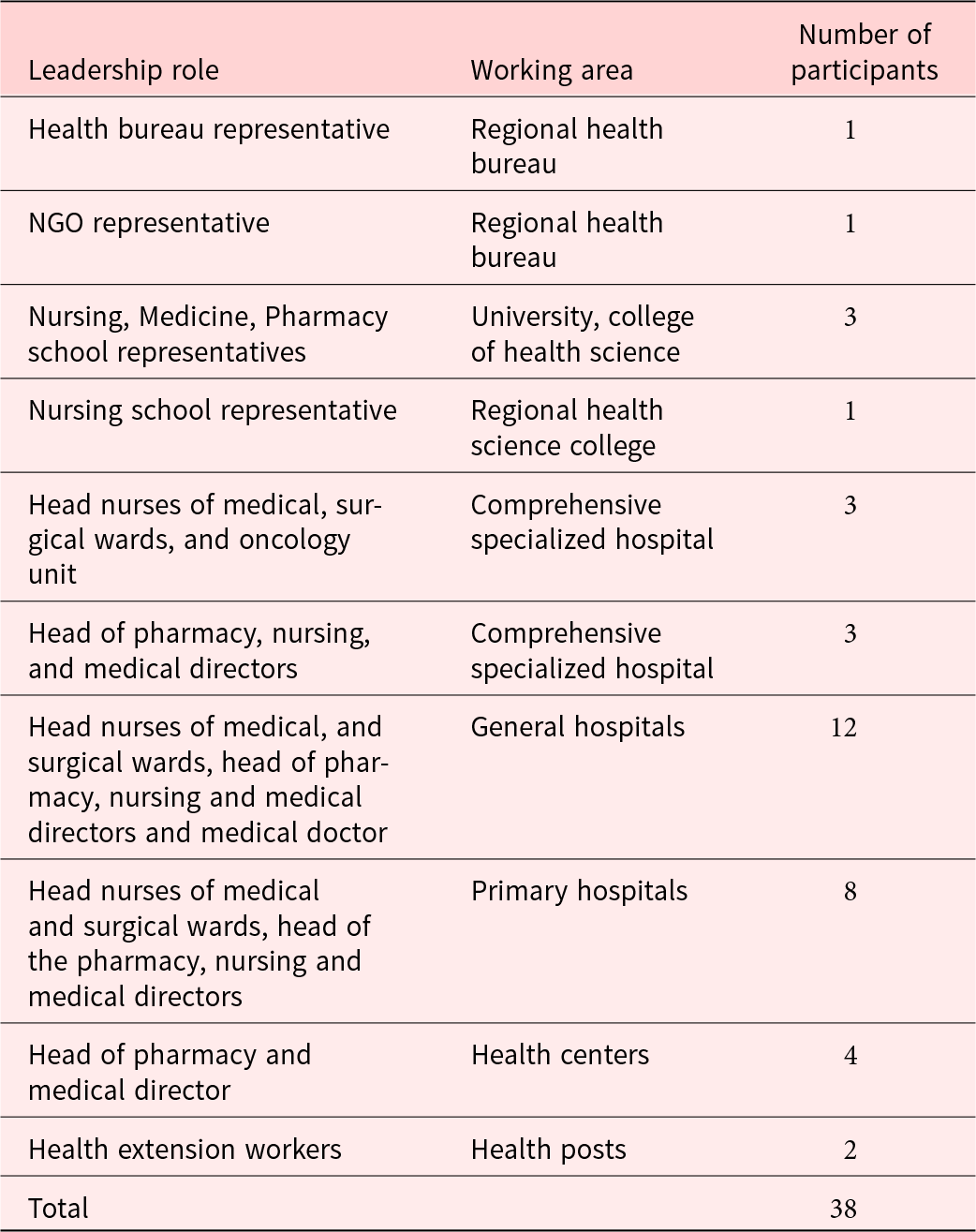
Of the 79% (173) nurses who responded to the quantitative survey, 51.4% (89) were from a tertiary hospital; 37.6% (65) worked in general hospitals; and 11% (19) were from primary health-care units. About 78% (135) of nurses held a bachelor’s degree, while 64.7% (112) had no in-service palliative care training. The mean age (standard deviation [SD]) of nurses was 32.6 (7.4) years, with the range of 22–57 years, and the overwhelming majority, 70% (123), were females (Table 1). The roles of the 38 interview participants are summarized in Table 2.
Number of interview participants and their leadership role

Attitudes toward palliative care
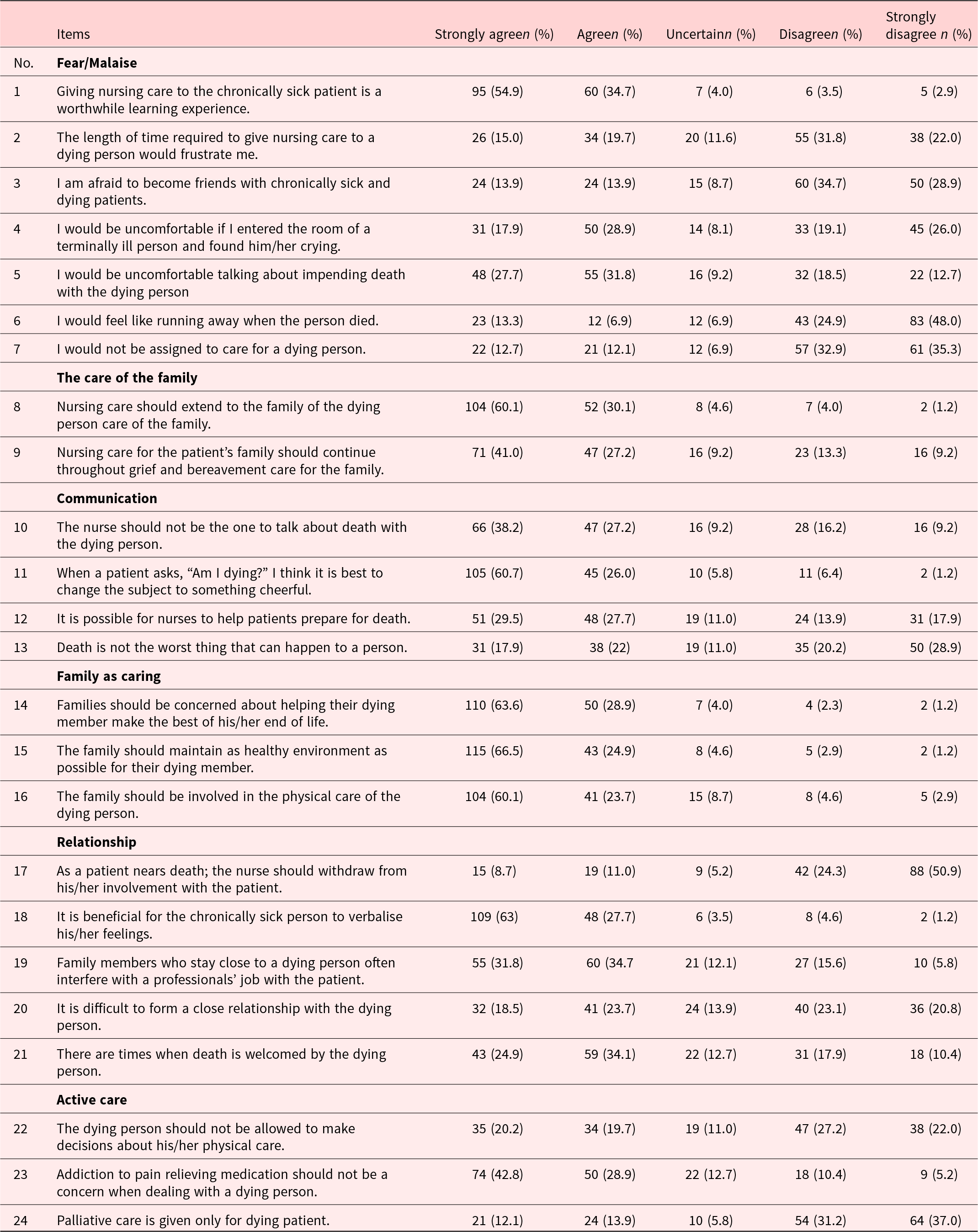
About 32.6% (7.4) of nurses scored 50% or greater, indicating a positive attitude toward palliative care. The total mean score of the modified version of FACTOD was 83.9 (SD, 8.6; range, 63–105) out of a possible score of 120. About 63% (109) of nurses believed palliative care benefits the chronically sick person, which shaped their attitudes toward palliative care practice. Nearly 60% (104) also thought family should be involved in physical care of the dying person (Table 3).
Nurses attitude according to their degree of agreement with FATCOD items (n = 173)

However, despite positive attitudes, health professionals reported limitations to implementing palliative care for patients in the current setting: “We know that it [palliative care] starts from diagnosis … until the end of life. However, hospital directives do not motivate professionals to deliver palliative care because we send patients to their homes as their conditions deteriorate” (Participant 1GHD).
Self-reported palliative care practices among nurses
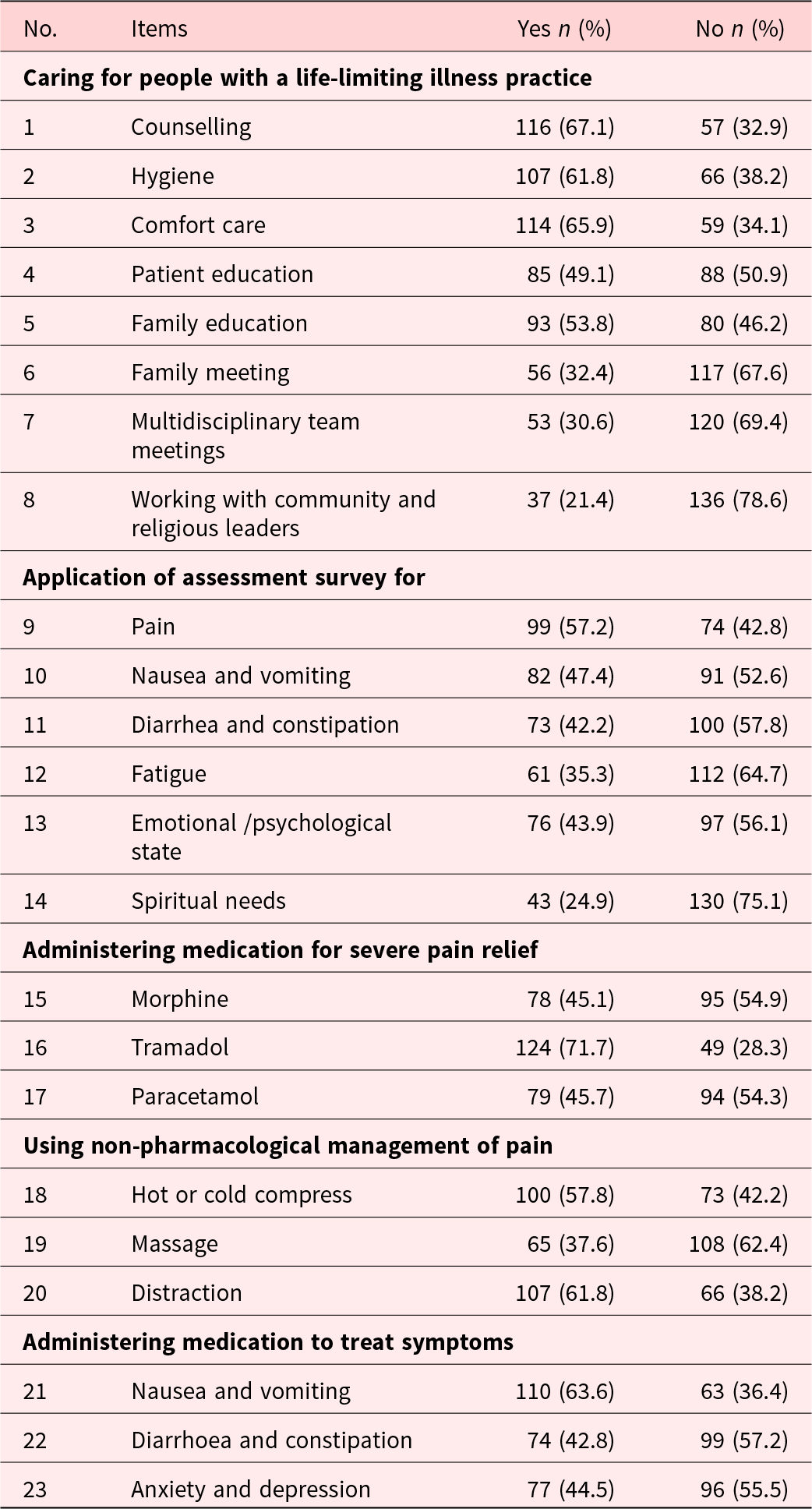
The mean score (SD) of self-reported palliative care practice was 11.0 (6.2), out of the possible score of 23 (Table 4). Regarding self-reported palliative care practice, only 18.5% (32) scored greater than 75%. Although 57% spontaneously reporting assessment of pain, most nurses did not address other symptoms; for example, over 50% of nurses did not assess other physical symptoms, psychological state, or spiritual needs. Similarly, although more than 70% (124) of nurses administered some pain relief (tramadol), other medications were provided by less than 50% of nurses. Medications to treat diarrhoea, constipation, anxiety, and depression were also used by less than 50% of nurses.
Self-reported practice of nurses toward palliative care (n = 173)

The quantitative survey’s self-reported palliative care results aligned with the qualitative findings. When participants discussed palliative care, they indicated that it was only available for those with HIV. A participant said, “Even as a term, palliative care, is linked with HIV. [It] is offered to relieve the severe pain of those who have HIV and … given as an independent service” (Participant CRHBR).
Others added that a comprehensive palliative care program is lacking. Participant 2PHND noted, “…it is difficult to say [if palliative care] is available. I prefer to say it is not applicable. We are yet to start palliative care, and this is not just here [primary hospital]. Even in our country, we don’t have comprehensive palliative care.”
This inability to practice palliative care distressed participants. Participant 1GHD suggested that professionals felt guilty for sending patients home when their condition became terminal. A clinical nurse leader at a comprehensive specialized hospital suggested, “When we see severe pain patients and unable to do anything, we feel distressed and psychologically affected: it creates a psychological problem” (Participant CTHWNH1).
Barriers to palliative care practice
There were 6 clear barriers to the practice of palliative care developed from the data.
Nurses’ lack of knowledge about palliative care
Although about 81% (183) of nurses indicated they knew about palliative care, 56.7% (97) responded that it is only appropriate where there is evidence of patient deterioration. Further, 77.2% (132) of nurses indicated that drug addiction is the major problem when morphine is used long-term. Of the participants, only 40% (69) scored 75% or greater for the modified version of the PCQN test. The highest number of incorrect responses was for the ‘pain and symptom management’ category of the PCQN item (156, 91%), followed by the “psychological and spiritual care” item (142, 83%) (Table 5).
Nurses’ knowledge about palliative care (an = 171)

a There were 2 missing values in knowledge items, so the total participants for the knowledge test was 171.
These quantitative results align with the qualitative findings. Participants from primary health-care units acknowledged that they lacked awareness about palliative care: “we do not have detailed information on how to provide care for chronically ill patients. We need guidance on providing palliative care” (Participant 1PHND).
Access to palliative care guidelines
When participants were asked about the availability of palliative care-related documents in their workplace, some mentioned the national palliative care guideline, confirming they knew about access. However, other participants were unaware of these guidelines. “we do not know about the documents [palliative care] … we do not have updated documents in this institute. And, as we don’t have them here, the alternative we have is, searching on the internet … if there is a national guideline, we must know that, but this is the problem” (Participant CRCR).
Additionlly, participants from general hospitals and primary health-care units indicated that no national palliative care guidelines existed in their sub-region and no palliative care documents were available in either the health center or the health post. However, they pointed out other materials, such as a pain management guideline; the Ethiopian hospital service transformation guideline; and a printed PowerPoint of the World Health Organization Module on palliative care, available for the leadership of the general and primary hospitals.
Gaps in preservice palliative care training
University participants said, “There is no dedicated chapter or topic on palliative care in the undergraduate program.” They continued, “we have not included them in our undergraduate Nursing curricula because it was designed nationally and standardised across Ethiopia” (Participant CSH1). However, it was noted that palliative care is incorporated in some postgraduate specialties, such as the master of adult health nursing and the diploma program in regional colleges for primary health providers. “Palliative care is included in our [regional health college] curriculum. We teach our nursing and midwifery students how to provide care for chronic disease patients from hospital admission to post-mortem care” (Participant CRCR).
The low awareness of palliative care among nurses was attributed to poor teaching methods, despite being part of some curricula in some institutions and settings. A doctor working in the comprehensive specialized hospital (Participant CTHD) noted, “I would say the way we train nurses needs to change. The traditional lecture-based system, bringing all the trainees together like in a meeting, does not work. We have to follow a different system. A new approach, such as training with clinical placement, is required.”
Other participants indicated that registered nurses who support students in implementing their classroom knowledge during placements, have limited knowledge about palliative care. “When students had a clinical placement in the hospital … the nurses did not know about it. Even they [some nurses] do not accept palliative care as part of their profession … nothing is applicable in the hospitals” (Participant CRCR).
Gaps in in-service palliative care training
It was noted that: “… there was palliative care in-service training for health care workers … I used to provide the training … but not to all [professionals] … It [the in-service training] is not only [for] nurses and GPs … but [also] … for other professionals working in health centre” (Participant 2GHD1).
However, nurse leaders working in the general hospital clarified that this was only ART-focused, organized, and funded by NGOs: “When we receive palliative care training, most of the time, it is provided by the CDC [Centres for Disease Control] and is to support our ART projects. We do not have professionals trained in palliative care other than ART nurses …” (Participant 2GHND).
Even with HIV training, participants said it was mostly about pain management rather than the full spectrum of palliative care, explaining that nurses were “trained in pain management, not palliative care training” (Participant 1GHWNH1). The need for regular, consistent training for all new staff was also highlighted: “There is a lot of turnover of health care workers. So, we have to give training whenever you have recruited health care workers” (Participant 2GHD1). Others also noted that those working in primary hospitals and health centres had not received training in either palliative care or pain management (Participant 1PHND).
Lack of political commitment and leadership toward palliative care
Participants working in general gospitals and primary health-care units argued that the country’s health system is skewed in favor of preventable and curable diseases, resulting in palliative care being a low priority among policymakers, health professionals, and the community. It was noted that: “In general, the top leaders did not prioritise palliative care and non-communicable conditions. The government’s focus is on communicable diseases. [As] the professionals are motivated to follow the tone set by the government directions, palliative care remains a neglected area” (Participant 2PHND).
The importance of governance was also highlighted: “Clinical commitment without political commitment is meaningless. If there is a [political] commitment [on palliative care] [in our hospital] the rest is very simple… So, these should happen first” (Participant 1GHD).
Supply and flow of resources for palliative care
In addition to inadequate political attention, participants thought that being a developing country created additional burden on translating palliative care knowledge and attitudes into care for patients with chronic diseases: “The core challenge is poverty. The government has no money for the sector as a whole, let alone for palliative care” (Participant 2GHD1). An educational leader further described the financial challenges: “To train individuals on palliative care … [to] establish, department [and] provide the service… we need money. However, we are a very resource-constrained country, and, in addition, we have so many priorities as a country” (Participant CSH2).
A participant from a comprehensive specialized hospital added that “we [the hospital] have a limited budget for our programs. So, we need to have a separate budget to implement [palliative care] initiatives, and without this, it could not be sustainable” (Participant CTHD).
Funding shortages affected priorities in the comprehensive specialized hospital. “There is a budget problem [to buy] the medications as we want … we have some lifesaving medications we need to take care. We prioritise these medications; then we jump to the next if we have remaining money” (Participant CTHP).
In addition to medications and operational guidelines, comprehensive palliative care requires dedicated facilities and skilled health workers. A regional health bureau participant noted, “Palliative care needs skilled health professionals, appropriate medicine and an adequate supply of medication for palliative care. It also requires equipment, and these are not yet available” (Participant CRHBR).
A separate and visible palliative care clinic to develop palliative care was described as being needed in the comprehensive specialized hospital. “There is no separate room to start palliative care up to now … they [palliative care trained staff] did not implement it practically …” (Participant CTHWNH2).
Discussion
The study findings describe the barriers to translating nurses’ palliative care knowledge into practice. Although nurses had favorable attitudes toward palliative care, both the quantitative and qualitative findings indicate inconsistent practice and knowledge gaps. The results showed slightly lower self-reported practice compared to the studies conducted in Addis Ababa and a regional health setting (Kassa et al. Reference Kassa, Murugan and Zewdu2014; Zeru et al. Reference Zeru, Gerensea and Berihu2020b). The qualitative findings also indicated that palliative care was mainly restricted to patients diagnosed with HIV/AIDs, similar to studies in Ethiopia (Mamo et al. Reference Mamo, Habte and Abreha2020; Onyeka et al. Reference Onyeka, Velijanashvili and Abdissa2013; Wube et al. Reference Wube, Horne and Stuer2010) and other African countries (Simms et al. Reference Simms, Higginson and Harding2012). This may be due to the financial support (Aregay et al. Reference Aregay, O’Connor and Stow2020; Callaway et al. Reference Callaway, Foley and De Lima2007) from different NGOs, including the Centre for Disease Control (CDC), emphasizing HIV care more than other illnesses.
Inadequate palliative care knowledge
The survey results indicate that nurses working directly with patients had low levels of palliative care knowledge, with less than 50% of nurses working at all levels of the health-care system scoring 75% or greater in the knowledge test. This study reported slightly higher knowledge scores compared with nurses’ knowledge in an earlier Ethiopian study (Kassa et al. Reference Kassa, Murugan and Zewdu2014), where fewer than 40% of nurses scored 75% or greater. The difference between these findings may be due to differences in the study period, the design and settings. Another study, (2018), found no government programs for palliative care, with only a few non-government hospice care centers providing home palliative care for patients with chronic illness. The improvements in knowledge scores over that time may indicate that palliative care initiatives in the northern region have had wider effect.
However, the nurses’ level of palliative care knowledge in our study is lower than in Tigray secondary and tertiary hospitals, where more than 60% of nurses scored 75% or greater for palliative care knowledge (Zeru et al. Reference Zeru, Berihu and Gerensea2020a). The differences in knowledge is likely a result of hospital staff having access to palliative care and pain management training, whereas primary health-care staff did not (Abdi and Dmitrovsky Reference Abdi and Dmitrovsky2020; O’Brien et al. Reference O'Brien, Schwartz and Plattner2018).
Nurses considered as a primary palliative care providers through dignity and compassion (WHO 2020). “Universal access to high-quality palliative care will not be possible without strategically optimizing the nursing workforce and integrating palliative care into nursing priorities at the local, national, and international levels” (Rosa et al. Reference Rosa, Buck and Squires2022a, e226). Earlier studies recommended the integration of palliative care into the nursing curricula to ensure equitable access to palliative care worldwide (American Nurses Association and Hospice & Palliative Nurses Association 2017; Rosa et al. Reference Rosa, Buck and Squires2022a). Additional studies also recommended palliative care education in 3 levels: basic education for all nursing professionals, intermediary education for nursing professionals who frequently care for patients who require palliative care, and specialized education for nursing professionals working in specialized palliative care areas (Callaway et al. Reference Callaway, Connor and Foley2018; Rosa et al. Reference Rosa, Buck and Squires2022a).
Despite including palliative care in nursing education being important for the implementation of palliative care programs, nurses are still primarly clinically focused on other aspects of care, like treating communicable diseases and mother and child care services (van der Plas et al. Reference van der Plas, Benjamens and Kruijff2020). This is consistent with the current study, in that although participants reported that palliative care was integrated into diploma and some postgraduate courses, nurses working in health-care settings prioirtized curable and preventable diseases rather than palliative care. So, despite a significant number of nurses possessing theoretical knowledge, there are few opportunities for practicing this knowledge, or for mentoring from other nurses. Similarly, the previous studies in Ethiopia indicated that theoretical and practical palliative care education in nursing is limited or not integrated into the nursing curricula (Onyeka et al. Reference Onyeka, Velijanashvili and Abdissa2013; Reid et al. Reference Reid, Gudina and Ayers2018). In comparison, the nursing education standards used differnt models of teaching to facilitate access to undergraduate and graduate education in palliative nursing in low- and middle-income countries such as Romania, Serbia, Kenya, Rwanda, Uganda, and Zambia (Rosa et al. Reference Rosa, Buck and Squires2022a). Similarly, studies in Kenya and Uganda where palliative care is integrated into undergraduate and postgraduate nursing curricula (Grant et al. Reference Grant, Downing and Luyirika2017; Kamonyo Reference Kamonyo2018; Luyirika et al. Reference Luyirika, Lohman and Ali2022), clinical placement sites and centers of excellence are ways to model best practice. There are numerous opportunities to learn from the experiences of other countries, in seeking ways to integrate palliative care practice beyond the theoretical learning.
The low priority of palliative care
Participants of this study perceived that the political commitment toward palliative care is poor as the government’s focus is still on curable and preventable diseases rather than incurable diseases. Tesema et al. (Reference Tesema, Abimbola and Mulugeta2021) described that noncommunicable conditions did not receive similar commitment, structural support, and funding in areas like HIV, malaria, and maternal and child health. This is despite Ethiopia being ranked the second highest among African countries in palliative care policy development and palliative care being a fifth pillar in the national health policies and guidelines (Ministry of Health 2020-2020-2024).
The qualitative findings also revealed that despite palliative care being included in the national health policies and guidelines, participants indicated that there was no dedicated budget for palliative care in the federal budget. Palliative care was most evident in NGOs, where funding was able to support palliative care for groups like patients with HIV (Mamo et al. Reference Mamo, Habte and Abreha2020; Onyeka et al. Reference Onyeka, Velijanashvili and Abdissa2013; Wube et al. Reference Wube, Horne and Stuer2010). Similarly, an African scoping review and an integrative review conducted in rural low- and middle-income countries indicated that where financial constraints are the major challenge, palliative care is dependent on external donors or funds (Aregay et al. Reference Aregay, O’Connor and Stow2020; Rhee et al. Reference Rhee, Garralda and Torrado2017).
Other countries may have solutions to this problem, as seen in studies reporting on palliative care budgets being tied to the national health policies in Uganda and Kenya (Fraser et al. Reference Fraser, Powell and Mwangi-Powell2017; Kamonyo Reference Kamonyo2018). The consequences of limited budgets and a low government focus toward palliative care included a lack of palliative care skilled nurses; limited infrastructure; and the unavailability of equipment and pain medications, particularly morphine (Fraser et al. Reference Fraser, Powell and Mwangi-Powell2017; Kamonyo Reference Kamonyo2018; Luyirika et al. Reference Luyirika, Lohman and Ali2022) The result is that trained professionals are not practicing their theoretical knowledge where needed.
Callaway et al. (Reference Callaway, Connor and Foley2018) suggest that national health policies and including palliative care and pain relief are priority areas for all health policies. As the goal in Ethiopia was to expand palliative care to 50% of health-care facilities by the end of 2020 (Federal Ministry of Health 2015), there is a need for a renewed focus and commitment to palliative care at a political level so that this national target is fully implemented.
Conclusion
This study explored the barriers to translating theoretical knowledge of palliative care into clinical practice in rural and regional resource-poor settings in Ethiopia. Insufficient attention to palliative care at government level has exacerbated financial constraints, and limited the availability of equipment and medications. A consequent lack of clinical placement-based training meant that while most nurses had positive views about palliative care, they had limited ability to put theoretical knowledge into practice.
Significance of results
While the results showed that the majority of nurses held positive views toward palliative care, improving palliative care practices requires, first and foremost, enhancing nurses’ knowledge of palliative care. This requires changing teaching methods and engaging higher-level policymakers to address resource constraints to enable clinical practice to occur.
Implications of the study
These findings have several implications for palliative care education, policy, and practice in Ethiopia. From a policy perspective, health-care managers may need to allocate a dedicated budget for palliative care, consider standardizing palliative care training and cultivate government support for palliative care. Concerning palliative care practice, the limited experience reported by nurses in this study suggests that opportunities like in-service training and placement could assist with improved knowledge and aspects of practice in patients’ homes. There is much to learn from some neighboring countries in Africa.
Limitations of the study
In this study, nurses were recruited from adult clinical settings of the 3 levels of the health-care system in only 1 of the 11 regions of the country. While drawing on other published Ethiopian studies for comparison, the results may not represent all nurses working in the country.
Afterword
This study was undertaken before the recent civil war in Ethiopia, when health-care systems were functional. The war caused major disruption to all aspects of life, with most health systems in the conflict region unable to function normally. Others have been either deliberately attacked or looted, resulting in limited services and care staff (Gebregziabher et al. Reference Gebregziabher, Amdeselassie and Esayas2022). It is hoped that recent cease-fire efforts will facilitate a return to normal life.
Acknowledgments
The authors acknowledge nurses working in all levels of the health-care system in Ethiopia, for their willing and committed response to the study survey. The authors also acknowledge Dr. Ensieh Fooladi for her advice in the statistical analysis and Professor Mariann Fossum for her time in reviewing the manuscript.
Funding
This research received no specific grant from any funding agency, commercial or not-for-profit sectors. Author AA is supported by an Australian Government Research Training Program stipend.
Competing interests
The author(s) declare none.
Ethical approval
Ethical approval was obtained from the Ethiopian University, Ethical Review Committee (1494) and Health Research-Ethical Review Committee, Monash University, Australia (13402). Survey participants were provided with an explanatory statement, and the return of the surveys implied consent. Responses were coded by service and region to ensure anonymity. Interviewees provided written consent prior to their interview. All transcripts were de-identified prior to analysis, and allocated identifiers by role and employer type.