Isolated right-sided infective endocarditis is uncommon, especially in neonates. Candida species is the underlying micro-organism in 10% of infants with infective endocarditis. In neonates, this results in a right-sided endocarditis in 90% of the Candida endocarditis cases.Reference Anil Kumar, Francis, Sreehari and Raj 1
First choice treatment is anti-microbial medication. Surgery should be considered when large tricuspid valve vegetation is present, when antibiotic medical treatment fails, when the infection is caused by micro-organisms difficult to eradicate, or when refractive right heart failure is present.Reference Habib, Lancellotti and Iung 2 The preferred surgical treatment is valve repair. Because of the long-term risk of developing severe right heart failure, tricuspid valvectomy is considered only in exceptional cases.Reference Yong, Coffey and Prendergast 3
Data on prognosis of living without tricuspid valve are scarce.Reference Yong, Coffey and Prendergast 3 , Reference Rodes-Cabau, Taramasso and O’Gara 4 Aim of this report is to share a history of over 10-year survival after tricuspid valvectomy in infancy.
Case report
We describe the case of a female infant born at 29 weeks and 3 days of gestational age with birth weight of 1310 kg. Details of her medical history in the first months of life have been reported previously.Reference du Plessis, Helbing and Bogers 5
At the age of 5 months, she was diagnosed with a thrombus obstructing the tricuspid orifice. Cardiac surgery was performed within 24 hours after admission. The tricuspid valve could not be repaired and valvectomy was performed. Blood cultures and thrombus examination showed a Candida albicans, so fluconazole was initiated. The post-operative course was prolonged, requiring maximal support with inotropic medication, diuretics, nitric oxide, and sildenafil. Eventually she was discharged 5 weeks post-operatively using diuretics, sildenafil 8 mg/kg/day, and fluconazole. Ultrasonography at discharge showed a dilated right heart, with normal cardiac output and moderate reversed flow in the hepatic veins.Reference du Plessis, Helbing and Bogers 5
The following years the girl did surprisingly well. Mild pulmonic regurgitation was noted. Based on the measurements of pulmonic regurgitation flow velocity and the shape of the right ventricle, there were no signs of increased pulmonary artery pressure. Because of the combined clinical and echo findings, we did not perform invasive measurements. Sildenafil dosage was gradually reduced and sildenafil was stopped 1 year after surgery. With the diuretics as only medication, she had a normal growth pattern and exercise capacity during the subsequent years. There was no progressive dilatation of the right atrium or ventricle. Until the age of 11 years old, she stayed clinically stable without cardiac arrhythmias or signs of right heart failure.
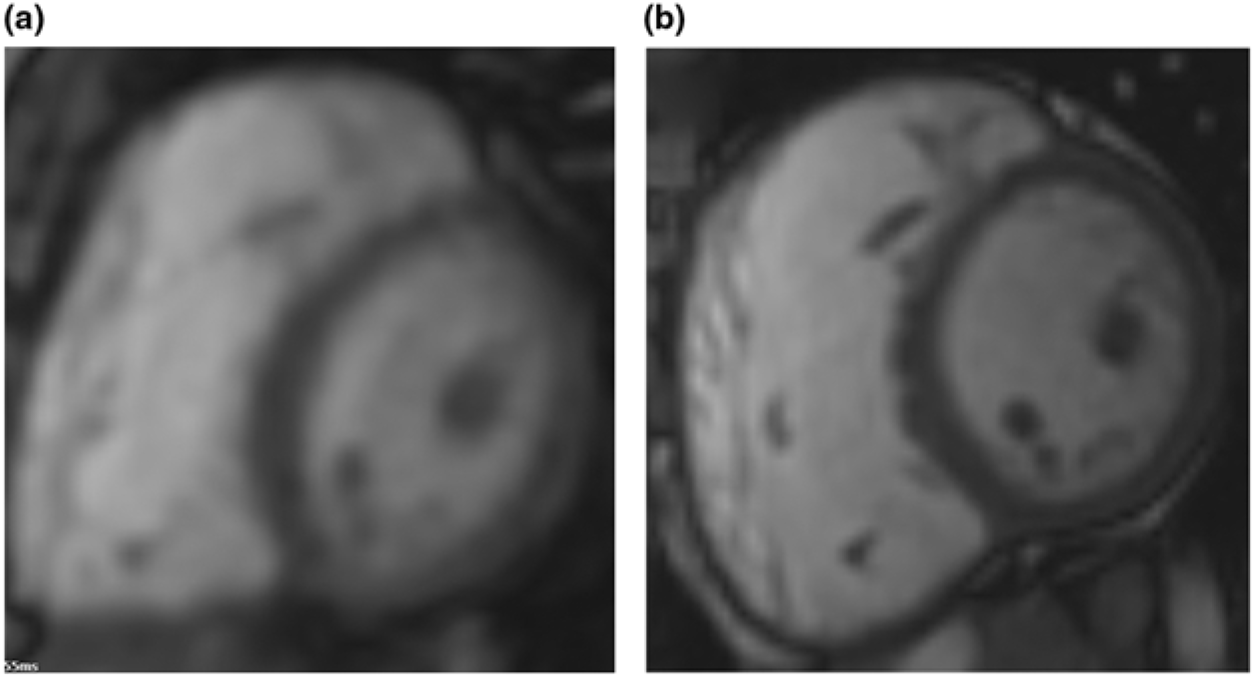
Since the age of 11 years, exercise intolerance is present. Cardiopulmonary exercise test showed exercise intolerance with a peak workload of 100 W (predicted 140 W, 71%) and a decrease of peak oxygen uptake from 37 to 28 ml/kg/minute over the last 3 years (Table 1). There were no signs of ventricular arrhythmias (as confirmed on 24-hour Holter monitoring). Cardiac MRI showed non-progressive dilatation of the right ventricle and a normal ventricular ejection fraction (Fig 1). Because of sub-optimal exercise performance and dilatation of the right heart (Table 1), the question for surgical intervention arises. Based on criteria including those used in more common situations of right ventricular dilatation, such as pulmonary regurgitation, for now a conservative strategy is implemented, guided by the clinical state of the patient.
Still frames of end-diastolic images of short axis orientation steady-state free-precession cine cardiac magnetic resonance imaging performed in 2014 ( a ) and 2017 ( b ). Left ventricle is on the right-hand side of panels (a) and (b).
Evolution of cardiopulmonary measurements
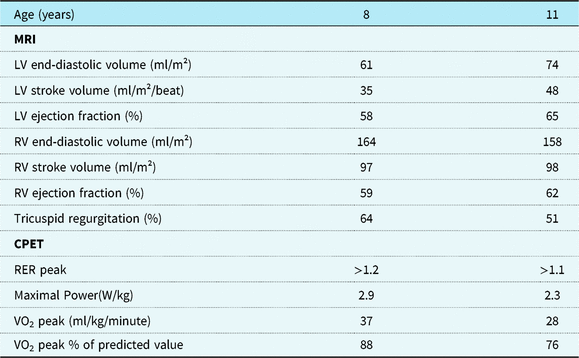
CPET = cardiopulmonary exercise testing; LV = left ventricle; RER peak = respiratory exchange ratio at peak exercise; RV = right ventricle.
Discussion
Information on long-term outcome after tricuspid valvectomy is scarce. Isolated tricuspid regurgitation is commonly well tolerated in adults.Reference Rodes-Cabau, Taramasso and O’Gara 4 However, chronic severe tricuspid regurgitation may lead to volume overload of the right ventricle, which may cause ventricular dilatation and loss of cardiac function. Symptoms may appear only when the disease is already advanced.Reference Rodes-Cabau, Taramasso and O’Gara 4 Chronic medical treatment for severe isolated tricuspid regurgitation in adults consists of diuretics, and is used when clinical symptoms of right heart failure are present. There is no evidence that the use of diuretics improves the survival rate in these patients.Reference Rodes-Cabau, Taramasso and O’Gara 4 , Reference Nishimura, Otto and Bonow 6 Furthermore, diuretics might reduce clinical symptoms and be successful in reducing heart failure symptoms, which might result in delay of surgical intervention and poorer outcome.Reference Baumgartner, Falk and Bax 7
In our case, pulmonary hypertension, following tricuspid valvectomy, initially persisted despite maximum support with diuretics, inotropics, high oxygen ventilation, and inhaled NO. Eventually, weaning from respiratory support was successful after introduction of sildenafil 8 mg/kg/day. In the following year, the girl was treated with diuretics and sildenafil to provide optimal preload and afterload of the right ventricle. There were no side effects reported.
Sildenafil is well studied and approved for pulmonary hypertension in adults. Currently, large trials in term and pre-term neonates are lacking.Reference Perez and Laughon 8 A Cochrane 2017 systematic review evaluated the efficacy of sildenafil monotherapy in lowering mortality in neonates compared to placebo. Sildenafil as adjuvant therapy with other pulmonary vasodilating products did not change mortality rates.Reference Kelly, Ohlsson and Shah 9
Tricuspid valvectomy has never been the first choice treatment option for endocarditis.Reference Yong, Coffey and Prendergast 3 In our case, clinical state and heart function remained normal for 10 years after tricuspid valvectomy. This favourable outcome can be explained by the positive response on medical treatment and absence of complications such as pulmonary embolism in the acute phase. Furthermore, chronic medical treatment with diuretics and new drugs such as sildenafil may have improved the outcome.Reference Perez and Laughon 8 , Reference Kelly, Ohlsson and Shah 9
There is no guideline concerning timing of surgical re-intervention after tricuspid valvectomy.Reference Rodes-Cabau, Taramasso and O’Gara 4 Our case shows a long-term survival with possibility to postpone surgery, in a young child.
The AHA/ACC and ESC/EACTS guidelines for adults recommend surgical intervention for primary, isolated tricuspid regurgitation when patients are symptomatic or, if they are asymptomatic, when there is progressive right ventricular dilatation and/or dysfunction (class IIa recommendation, level of evidence C). Surgery needs to be performed as soon as the indication is set, to avoid irreversible right ventricular dysfunction.Reference Nishimura, Otto and Bonow 6 , Reference Baumgartner, Falk and Bax 7
Follow-up includes imaging with echocardiography and MRI. The 2017 ESC/EACTS guideline describes cut-off values of echocardiographic measurements defining severe valve regurgitation in adults.Reference Nishimura, Otto and Bonow 6 , Reference Baumgartner, Falk and Bax 7 The lack of cut-off values for children is striking. This bears resemblance to the setting of chronic right ventricle volume overload following chronic pulmonary regurgitation, in which size criteria of the right ventricle as indication for intervention are subject of continued debate.Reference Tretter, Friedberg, Wald and McElhinney 10 This hampers decision-making in a case like this. In analogy to the situation in valve replacement in pulmonary regurgitation, we will opt for tricuspid valve replacement if symptoms, exercise test results, right ventricular size, and function and/or ECG changes all point towards progressive decline of right ventricular function.
Conclusion
This case illustrates the ability for survival in good clinical condition for more than 10 years after tricuspid valvectomy performed in infancy. Growth, exercise capacity, and right ventricular size and function remained within acceptable limits. Consensus criteria for timing of re-intervention are lacking.
Financial Support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Conflicts of Interest
None.
Ethical Standards
Written informed consent was obtained.



