Introduction
Musculoskeletal (MSK) problems are extremely common, affecting more than 21% of the adult population (Helmick et al., Reference Helmick, Felson, Lawrence, Gabriel, Hirsch, Kwoh, Liang, Kremers, Mayes, Merkel, Pillemer, Reveille and Stone2008). They represent a substantial economic burden (Le Pen et al., Reference Le Pen, Reygrobellet and Gerentes2005; Bitton, Reference Bitton2009) and are now the second most significant cause of disability worldwide [years lived with disability (YLD)] (Vos et al., Reference Vos, Flaxman, Naghavi, Lozano, Michaud and Ezzati2012). In primary care, up to 20% of adults consult their general practitioner (GP) with a MSK problem (Jordan et al., Reference Jordan, Kadam, Hayward, Porcheret, Young and Croft2010).
Large epidemiological studies have reported that chronic multiple-site joint pain (MSJP) is more common than single joint problems (Urwin et al., Reference Urwin, Symmons, Allison, Brammah, Busby, Roxby, Simmons and Williams1998; Croft et al., Reference Croft, Jordan and Jinks2005; Keenan et al., Reference Keenan, Tennant, Fear, Emery and Conaghan2006; Peat et al., Reference Peat, Thomas, Wilkie and Croft2006; Carnes et al., Reference Carnes, Parsons, Ashby, Breen, Foster, Pincus, Vogel and Underwood2007) with the median number of painful joints for people over the age of 55 being 4 (Keenan et al., Reference Keenan, Tennant, Fear, Emery and Conaghan2006). At least 75% of people in such community-based cohorts have multiple joint involvement (Carnes et al., Reference Carnes, Parsons, Ashby, Breen, Foster, Pincus, Vogel and Underwood2007) compared with single joint involvement, whose incidence is as low as 12.5% (Keenan et al., Reference Keenan, Tennant, Fear, Emery and Conaghan2006). Increased numbers of painful joints are associated with increased anxiety and depression (Croft et al., Reference Croft, Jordan and Jinks2005), reduced overall health (Kamaleri et al., Reference Kamaleri, Natvig, Ihlebaek, Benth and Bruusgaard2008), poor physical function (Croft et al., Reference Croft, Jordan and Jinks2005; Peat et al., Reference Peat, Thomas, Wilkie and Croft2006) and increased site-specific pain severity (Peat et al., Reference Peat, Thomas, Wilkie and Croft2006). With respect to impact on the workforce, MSJP is associated with increased work disability (Miranda et al., Reference Miranda, Kaila-Kangas, Heliovaara, Leino-Arjas, Haukka, Liira and Viikari-Juntura2010), lost productive time in the workforce (Stewart et al., Reference Stewart, Ricci, Chee, Morganstein and Lipton2003), increased disability pensioning (Kamaleri et al., Reference Kamaleri, Natvig, Ihlebaek and Bruusgaard2009) and also predicts future reduced work ability (Neupane et al., Reference Neupane, Miranda, Virtanen, Siukola and Nygard2011).
MSJP can be conceptualised as different combinations of mechanical back pain, peripheral joint osteoarthritis (OA) and soft tissue disorders. However the characteristics of MSJP have not been well described or researched. Importantly, despite the frequent prevalence of MSJP and poor outcomes, there are extremely few therapeutic trials in this area. The vast majority of MSK pain trials involve selection for a predominantly single painful joint, such as knee OA or shoulder pain. It is therefore not known if currently available therapies are effective or how to employ them in people with MSJP.
As primary care is the first point of contact for most people with these common MSJP problems, the aim of this study was to examine current GP understanding and approach to management of MSJP in the primary care setting. Such information would provide a crucial first step in developing therapeutic strategies for MSJP management.
Methods
Questionnaire development
Following a review of the published literature on MSJP management (manuscript in progress), consultation with researchers experienced in health professional surveys and a GP representative, an 11-question multiple choice questionnaire was developed to obtain information on GPs’ approach to pharmacological management of MSJP, understanding of oral analgesia use for different MSK conditions and strategies used for optimisation of MSJP therapy.
Sample
The attendees at a UK national GP educational seminar participated in an electronic survey. Attendees were made up of GPs, GPs with a special interest in MSK conditions (GPwSI) and GP specialty trainees. In order to maximise response rates (given the traditional low response rates from mailed or electronic surveys), the multiple-choice questionnaire was presented in a power point slide format with the response recorded upon entering a choice on a remote controlled device. The GP presenting the slides was then able to check the degree of completion for each question (ie, extent of audience participation per question). The attendees were briefed before the survey to ensure a clear understanding that MSJP referred to multiple mechanical (non-inflammatory) joint pains and did not include patients with inflammatory arthritis and fibromyalgia. All respondents remained anonymous.
Ethical review
According to the National Research Ethics Service definitions of research, this project was classified as a service evaluation and was therefore exempt from the need for ethical review.
Data analysis
Descriptive statistics were used to present the data according to the questionnaire categories.
Results
Profile of respondents
A total of 150 attendees participated in the survey of which the majority were GPs (86%), with smaller numbers of GP specialty trainees and GPwSIs (Table 1). Almost two-thirds of attendees were under the age of 45 and most participants were working in group GP practices. The mean response rate across the 11-question multi-choice questionnaire was 96%.
Characteristics of attendees participating in survey
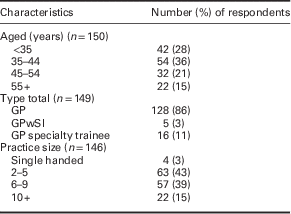
GP=general practitioner; GPwSI=general practitioner with a special interest in musculoskeletal conditions.
Approach to treatment strategy for multiple joint pain
When consulting with a patient with MSJP, most participants reported treating all joints concurrently (n=112/144, 78%) as a usual treatment strategy. Twenty-one per cent (n=30/144) of the participants preferred to focus on treating one joint and only a minority (n=2/144, 1%) reported referring the patient to a specialist in the first instance.
Factors deciding the ‘focus on a single joint’ approach to treatment
Among participants who reported focusing on treating a single joint, the majority (n=16/30, 53%) chose that approach for the reason that different treatment options are required for the different joints. Forty per cent (n=12/30) focused on a single joint due to time limitations and 7% (n=2/30) believed that there was lack of effective treatment options for multiple mechanical joint pains. When deciding which single joint to treat, 77% (n=23/30) would treat the joint that the patient prioritises compared with treating the most painful joint (n=7/30, 23%).
Approach to using oral analgesia in OA versus chronic soft tissue disorder
The survey asked participants whether the prescription of oral analgesia differed depending on whether the joint pain was due to OA or chronic soft tissue disorder. A majority of the participants believed that there was no difference in the choice of analgesia between the two conditions when selecting paracetamol (n=123/146, 84%), non-steroidal anti-inflammatory drug (NSAID)/COX-2 inhibitor (n=73/128, 57%) or opioid (n=97/139, 70%) treatment.
Optimisation of oral MSJP analgesia therapy
When consulting a MSJP patient experiencing inadequate pain relief when using paracetamol and non-maximal daily dose of NSAID, 41% (n=59/145) of the participants would increase the dose of NSAID, 30% (n=43/145) would change to another NSAID or COX-2 inhibitor therapy, 23% (n=34/145) preferred the addition of an opioid, and 6% (n=9/145) would change the NSAID to an opioid medication.
If a patient were to experience some gastrointestinal (GI) intolerance (dyspepsia not suspicious of GI bleed or peptic ulcer) while using a non-selective NSAID for MSJP, the majority of participants (n=106/144, 74%) would add a gastro-protective agent whereas 8% (n=11/144) would change to another non-selective NSAID while adding a gastro-protective agent. One per cent (n=2/144) would change to a COX-2 inhibitor and 17% (n=25/144) preferred to change the NSAID to an opioid therapy.
Discussion
This is the first study to examine the GP approach to pharmacological management of the common problem of MSJP. Participants were mostly non-special interest GPs working in small to medium sized practices. Most GPs reported treating all painful joints simultaneously and felt that there was no difference in the choice of analgesia regardless of the diagnosis of back pain, OA or soft tissue pathology. This strategy suggests that GPs utilise a systemic pharmacotherapeutic approach. It also suggests a belief in equal efficacy of the different classes of analgesia across the range of MSK pathologies that comprise MSJP.
There is a marked paucity of studies reporting interventional strategies for MSJP. Observational studies have thus far mainly examined treatment modalities used in primary care for knee pain but not MSJP (Jordan et al., Reference Jordan, Sawyer, Coakley, Smith, Cooper and Arden2004; Porcheret et al., Reference Porcheret, Jordan and Croft2007). While pharmacological interventional studies have occasionally included ‘multiple joint’ area involvement, the inclusion criteria often only required single joint involvement (eg, either hip or knee pain) and therefore are not representative of a true MSJP cohort (Boureau et al., Reference Boureau, Schneid, Zeghari, Wall and Bourgeois2004; Lin et al., Reference Lin, Cheng, Wang, Lee, Chen, Lei, Lac, Gammaitoni, Smugar and Chen2010).
There is also a scarcity of research into the efficacy of currently available analgesics in the setting of MSJP. It is not known whether there is a difference in efficacy across the classes of oral analgesia for different MSK pathologies. There are studies showing that NSAIDs are beneficial for some soft tissue disorders (such as rotator cuff tendinitis and lateral epicondylitis), however studies are lacking for other conditions and types of analgesia, especially for opioids (Green et al., Reference Green, Buchbinder, Glazier and Forbes2000; Reference Green, Buchbinder, Barnsley, Hall, White, Smidt and Assendelft2002).
With respect to pharmacotherapy optimisation, when consulting a MSJP patient with inadequate pain relief on non-maximal dose of NSAID, the majority of GPs preferred to optimise NSAID therapy in the first instance either by increasing dosage or switching to another NSAID. This indicates preference for intra-class optimisation before an inter-class drug change. The response was similar when faced with NSAID-related GI intolerance, whereby most GPs would persist with NSAID therapy by introducing a gastro-protective agent. It is not known what the most effective optimisation approach is in MSJP and thus far there are no trials for pharmacotherapy optimisation in this field. Recommendations are available for a stepped model of care involving single joint pain (Porcheret et al., Reference Porcheret, Jordan and Croft2007; Smink et al., Reference Smink, van den Ende, Vliet Vlieland, Swierstra, Kortland, Bijlsma, Voorn, Schers, Bierma-Zeinstra and Dekker2011) along with the National Institute for Health and Clinical Excellence guidelines on pharmacotherapy for OA in general (Conaghan et al., Reference Conaghan, Dickson and Grant2008). These recommendations focus on inter-class and lack intra-class oral analgesia optimisation strategies, and this probably reflects the lack of research in this area. There is one randomised clinical trial for pharmacotherapy optimisation in primary care for knee OA (Hay et al., Reference Hay, Foster, Thomas, Peat, Phelan, Yates, Blenkinsopp and Sim2006). Hay et al. showed that an enhanced pharmacy review by an experienced community pharmacist using a pre-defined algorithm resulted in short-term improvements in pain scores, reduced use of NSAIDs and produced high patient satisfaction when compared with the control group (GP led analgesia advice plus information and advice leaflet reinforced by telephone call). The pre-defined algorithm from that study considered both inter-class step-up therapy and intra-class (NSAID) optimisation strategies.
An electronic touch pad method of survey was deliberately chosen to obtain a high response rate from the GP study population and this is reflected by the high mean response rate (96%) across all the questions in this study. Physician online surveys on the other hand achieve response rates of 23–43% (Bleich et al., Reference Bleich, Bennett, Gudzune and Cooper2012; Kingsbury and Conaghan Reference Kingsbury and Conaghan2012; Masupe and Parker Reference Masupe and Parker2013). In MSJP cross-sectional studies, the rate of response for postal questionnaires was 57–70% (Croft et al., Reference Croft, Jordan and Jinks2005; Carnes et al., Reference Carnes, Parsons, Ashby, Breen, Foster, Pincus, Vogel and Underwood2007; Grotle et al., Reference Grotle, Hagen, Natvig, Dahl and Kvien2008).
There were limitations to this study. The study population chosen for the survey may have introduced bias given they were seminar attendees, although the number of GPs with special interest was low. Attendees at such educational seminars may have a tendency to give a more normative response rather than reflecting usual practice which would cause a significant bias in the result. On the other hand, such bias is likely to have been minimised in this study by using an electronic touch pad method. Giving an anonymised response in a quick and discrete manner using a touch pad may have resulted in a response more reflective of actual practice. Owing to the method of the electronic survey, some participants may have had limited time to respond in time and also were unable to return to previous questions to contemplate and confirm their response. Technical problems preventing a response from being registered may have occurred although all of the handsets had been checked prior to the survey taking place. These factors may explain the small numbers of non-responders in our study. The satisfaction rate for the method of survey was not measured.
Although clinicians have been seeing MSJP for a long time, the lack of understanding and characterisation of this condition, the lack of recommendations and management strategies, and the associated poor outcomes, make MSJP a hugely important area for further research, especially in the context of a rapidly ageing and increasingly obese society where such degenerative and mechanical joint problems are massively increasing.
Conclusion
A survey of GPs at an educational seminar suggests that in MSJP, the majority of GPs aim to treat all painful joints concurrently, with systemic pharmacotherapy regardless of underlying pathology. Intra-class optimisation was preferred to inter-class step up therapy in the first instance. There is need for further research to help better characterise MSJP and examine optimal pharmacotherapy regimens.
Acknowledgement
R.R. is funded by the Rose Hellaby Scholarship (Guardian Trust) New Zealand and The Royal Australasian College of Physicians (RACP)/Australian Rheumatology Association & Starr Fellowship (Australia).
S.R.K. and P.G.C. are funded in part by Arthritis Research UK and the NIHR Leeds Musculoskeletal Biomedical Research Unit.
Conflicts of Interest
R.R.: no disclosures. S.R.K.: no disclosures. E.W.: speaker or advisory boards for Napp, Pfizer, Servier. P.G.C.: speaker or advisory boards for Janssen, Merck, Napp, Pfizer, Servier.



