Introduction
Late-life depression (LLD) is a common illness characterized by increased disability, medical illness comorbidity, suicide risk, and higher mortality (Szymkowicz, Gerlach, Homiack, & Taylor, Reference Szymkowicz, Gerlach, Homiack and Taylor2023a). Beyond its affective symptoms, LLD is further characterized by poor or impaired cognitive function, particularly in executive functions, with an increased risk for dementia (Diniz, Butters, Albert, Dew, & Reynolds, Reference Diniz, Butters, Albert, Dew and Reynolds2013; Manning & Steffens, Reference Manning and Steffens2018; Szymkowicz et al., Reference Szymkowicz, Gerlach, Homiack and Taylor2023a). These negative outcomes may be related to adverse physiological responses occurring in depression, magnified by experiencing repeated episodes (Andreescu et al., Reference Andreescu, Ajilore, Aizenstein, Albert, Butters, Landman and Taylor2019). Despite maintenance treatment, older adults with LLD who experience remission remain at high relapse risk, with maintenance clinical trials and naturalistic cohort studies indicating a 35%–45% recurrence rate over two years (Andreescu et al., Reference Andreescu, Ajilore, Aizenstein, Albert, Butters, Landman and Taylor2019; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Reynolds et al., Reference Reynolds, Dew, Pollock, Mulsant, Frank, Miller and Kupfer2006). While a greater number of prior depressive episodes predicts relapse (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018), and maintenance antidepressant treatment is protective (Reynolds et al., Reference Reynolds, Frank, Perel, Imber, Cornes, Miller and Kupfer1999, Reference Reynolds, Dew, Pollock, Mulsant, Frank, Miller and Kupfer2006), little is known about other factors that predict or may protect against future depressive episodes, particularly in older adults with an established history of recurrent LLD (Andreescu et al., Reference Andreescu, Ajilore, Aizenstein, Albert, Butters, Landman and Taylor2019; Taylor et al., Reference Taylor, Ajilore, Karim, Butters, Krafty, Boyd and Andreescu2024).
Past research has reported discrepant findings relating clinical and demographic characteristics with risk of future depressive episodes (Hardeveld, Spijker, De Graaf, Nolen, & Beekman, Reference Hardeveld, Spijker, De Graaf, Nolen and Beekman2010). Recurrence risk is associated both with number of prior episodes and with residual depression symptoms in both adult and geriatric populations (Bulloch, Williams, Lavorato, & Patten, Reference Bulloch, Williams, Lavorato and Patten2014; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Judd et al., Reference Judd, Akiskal, Maser, Zeller, Endicott, Coryell and Keller1998; Nierenberg et al., Reference Nierenberg, Husain, Trivedi, Fava, Warden, Wisniewski and Rush2010). In LLD, depression severity during the index episode is not associated with relapse (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018), although greater severity of specific affective symptoms such as anxiety, sadness, suicidality, or sleep disturbance may be informative (Andreescu et al., Reference Andreescu, Lenze, Dew, Begley, Mulsant, Dombrovski and Reynolds2007; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Reynolds et al., Reference Reynolds, Dew, Pollock, Mulsant, Frank, Miller and Kupfer2006). In contrast, medical comorbidity in LLD may not influence recurrence risk (Alexopoulos et al., Reference Alexopoulos, Meyers, Young, Kalayam, Kakuma, Gabrielle and Hull2000; Alexopoulos, Young, Abrams, Meyers, & Shamoian, Reference Alexopoulos, Young, Abrams, Meyers and Shamoian1989; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Hinrichsen & Hernandez, Reference Hinrichsen and Hernandez1993). Although reports are inconsistent, some data in LLD suggest that female sex and earlier life onset of a first depressive episode may increase risk of relapse (Alexopoulos et al., Reference Alexopoulos, Meyers, Young, Kalayam, Kakuma, Gabrielle and Hull2000; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Hinrichsen & Hernandez, Reference Hinrichsen and Hernandez1993; Stoudemire, Reference Stoudemire1997).
Environmental and social factors substantially influence recurrence risk. We previously associated LLD recurrence with greater perceived stress, lower levels of instrumental social support, and greater difficulty performing instrumental activities of daily living (IADLs) (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018). Recurrence risk is further associated with fewer positive social supports and more negative stressful life events, both in older adults (Alexopoulos et al., Reference Alexopoulos, Young, Abrams, Meyers and Shamoian1989; Hinrichsen & Hernandez, Reference Hinrichsen and Hernandez1993) and broader adult populations (Patten et al., Reference Patten, Wang, Williams, Lavorato, Khaled and Bulloch2010; Solomon et al., Reference Solomon, Leon, Endicott, Mueller, Coryell, Shea and Keller2004; van Loo, Aggen, Gardner, & Kendler, Reference van Loo, Aggen, Gardner and Kendler2015).
It is unclear whether impaired cognitive performance influences relapse. While not all patients with LLD exhibit poorer cognitive performance (Szymkowicz, Ryan, Elson, Kang, & Taylor, Reference Szymkowicz, Ryan, Elson, Kang and Taylor2023b), poor performance across multiple cognitive domains is common, and associated with a worse acute antidepressant response (Butters et al., Reference Butters, Bhalla, Mulsant, Mazumdar, Houck, Begley and Reynolds2004; Manning & Steffens, Reference Manning and Steffens2018; Sheline et al., Reference Sheline, Disabato, Hranilovich, Morris, D'Angelo, Pieper and Doraiswamy2012). While some have associated LLD relapse with executive dysfunction (Alexopoulos et al., Reference Alexopoulos, Meyers, Young, Kalayam, Kakuma, Gabrielle and Hull2000), other work has not associated risk of relapse with poorer performance on neuropsychological measures (Butters et al., Reference Butters, Bhalla, Mulsant, Mazumdar, Houck, Begley and Reynolds2004; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018).
The REMBRANDT study (recurrence markers, cognitive burden, and neurobiological homeostasis in depression) examined potential risk factors and predictors of depression relapse following remission in recurrent LLD (Andreescu et al., Reference Andreescu, Ajilore, Aizenstein, Albert, Butters, Landman and Taylor2019; Taylor et al., Reference Taylor, Ajilore, Karim, Butters, Krafty, Boyd and Andreescu2024). We examined demographic, clinical, medical, environmental, social, and neuropsychological factors present in remission that may differ from healthy comparison participants and predict relapse over two years. While recurrence of depression can occur beyond this two-year window, even after many years of maintained remission (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Mueller et al., Reference Mueller, Leon, Keller, Solomon, Endicott, Coryell and Maser1999), we focus on a two-year window as this is the period where recurrence risk is the highest (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Mueller et al., Reference Mueller, Leon, Keller, Solomon, Endicott, Coryell and Maser1999). Based on past work (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018), we hypothesized that relapse risk would be associated with greater residual depressive symptom severity, greater stress exposure, lower levels of social support, and greater functional disability.
Methods
Overall study design
The full methods for the REMBRANDT study are published (Taylor et al., Reference Taylor, Ajilore, Karim, Butters, Krafty, Boyd and Andreescu2024). Participants were recruited using clinical referrals and community advertisements at three sites: the University of Illinois-Chicago, the University of Pittsburgh, and Vanderbilt University Medical Center. Briefly, participants were recruited into a longitudinal study including clinical assessments and phenotyping and were followed for two years. Two longitudinal cohorts were recruited: (1) remitted LLD participants recently recovered from a major depressive episode in the last four months; and (2) comparison participants without any psychiatric history. Some LLD participants were enrolled when acutely depressed and treated per an initial structured treatment algorithm (Taylor et al., Reference Taylor, Ajilore, Karim, Butters, Krafty, Boyd and Andreescu2024), but only those who achieved remission and entered the two-year longitudinal phase are included in these analyses.
As participants were followed prospectively, we categorized remitted LLD participants according to who did and did not experience depression recurrence over the longitudinal period. Relapse (including both relapse and recurrence) was defined as a MADRS score of 15 or greater, plus meeting DSM5 criteria for a new major depressive episode, including the two-week duration criterion. LLD participants with a relapse were included in the ‘Relapsing’ subgroup, while those who maintained remission without a relapse were classified in the ‘Sustained Remission’ subgroup.
Participant eligibility criteria
Common inclusion criteria included: (1) age 60 years or older; (2) Montreal Cognitive Assessment (MoCA) score of 24 or higher; (3) fluency in English. Common exclusion criteria included: (a) history of a substance use disorder other than nicotine in the last year; (b) other DSM5 disorders, aside from co-occurring anxiety disorders present during depressive episodes; (c) history of developmental disorder; (d) acute suicidal ideation; (e) acute grief; (f) current or past psychosis; (g) primary neurological disorders, including dementia; (h) unstable medical illnesses; (i) electroconvulsive therapy in the last 6 months, or current use of transcranial magnetic stimulation, ketamine, or esketamine. Individuals were not excluded for exhibiting cognitive difficulties concordant with mild cognitive impairment.
Additional criteria were specific to the participant groups. Remitted depressed participants required a DSM5 diagnosis of major depressive disorder, recurrent, in partial or full remission, with a Montgomery-Asberg Depression Rating Scale (MADRS) (Montgomery & Asberg, Reference Montgomery and Asberg1979) score of 10 or less for two consecutive assessments, at least a month apar. Remission from a documented depressive episode had to occur no more than four months prior to entry in the longitudinal phase. Comparison participants had to exhibit a MADRS score of 8 or less, could not endorse any lifetime psychiatric history, and could not have a history of psychotropic medication use. Importantly, the remitted depressed participants and comparison participants had a slightly different MADRS thresholds for eligibility. The lower MADRS in comparison participants was intended to assure that these participants exhibited an absence of potentially significant subthreshold depressive symptoms. The higher MADRS in the remitted participants was intended to allow for some modest residual symptoms that may affect recurrence risk.
The study was approved across all three sites through the Vanderbilt Institutional Review Board (IRB). All participants provided written, informed consent.
Clinical assessments
At enrollment, mental health diagnoses were confirmed using the MINI International Neuropsychiatric Interview for DSM5 (Sheehan et al., Reference Sheehan, Lecrubier, Sheehan, Amorim, Janavs, Weiller and Dunbar1998). Review of past psychiatric history included psychotropic medication use, age of initial depression onset, and duration of most recent depressive episode. To accurately quantify episode duration, clinical interview repeatedly returned to describing the core symptoms of depression, relied on personal and societal milestones, and assessed for periods of symptom improvement that may indicate a break between recurrent episodes. Current medical burden was quantified using the Cumulative Illness Rating Scale – Geriatric (CIRS-G) (Miller et al., Reference Miller, Paradis, Houck, Mazumdar, Stack, Rifai and Reynolds1992), pain severity and fatigue severity with visual-analog scales, and self-reported disability using the World Health Organization Disability Assessment Schedule 2.0 (WHODAS), examining both total and subdomain scores. Vital signs, including weight, blood pressure, and pulse rate were measured. Intensity of current antidepressant treatment was quantified using an updated version of the Antidepressant Treatment History Form (ATHF) that considers number of medications, dose, and duration (Sackeim et al., Reference Sackeim, Prudic, Devanand, Decina, Kerr and Malitz1990), with higher scores indicating more intense treatment regimens needed to achieve remission.
Symptom phenotyping
Clinical staff rated depression severity using the MADRS and anxiety severity using the Hamilton Anxiety Rating Scale (HARS) (Hamilton, Reference Hamilton1959). Participants completed a broad battery of self-report symptom scales probing specific affective symptoms. These assessed severity of apathy (Apathy Evaluation Scale [AES]) (Marin, Biedrzycki, & Firinciogullari, Reference Marin, Biedrzycki and Firinciogullari1991), fatigue (Fatigue Severity Scale [FSS]) (Krupp, LaRocca, Muir-Nash, & Steinberg, Reference Krupp, LaRocca, Muir-Nash and Steinberg1989), resilience (Connor-Davidson Resilience Scale-10 [CD-RISC10]) (Connor & Davidson, Reference Connor and Davidson2003), rumination (Ruminative Response Scale [RRS]) (Nolen-Hoeksema, Morrow, & Fredrickson, Reference Nolen-Hoeksema, Morrow and Fredrickson1993), and worry (Penn State Worry Questionnaire [PSWQ]) (Meyer, Miller, Metzger, & Borkovec, Reference Meyer, Miller, Metzger and Borkovec1990). Across these measures, higher scores indicate greater symptom severity, aside from the CD-RISC10 where higher scores indicate greater resilience. Personality characteristics were assessed using the Five Factor Inventory (Costa & McCrae, Reference Costa and McCrae1992).
Social support and environmental stress
Additional self-report questionnaires assessed participants' social support and stress exposures. Instrumental social support, or having social assistance to complete tasks, was assessed using the Duke Social Support Index (Hays et al., Reference Hays, Krishnan, George, Pieper, Flint and Blazer1997). Perceived social support and social conflict were assessed using the MIDUS II Perceived Social Support Conflict Scale (Elliot, Heffner, Mooney, Moynihan, & Chapman, Reference Elliot, Heffner, Mooney, Moynihan and Chapman2018). Social isolation was assessed using the 4-item PROMIS social isolation scale. Recent exposure to stressful life events was quantified using the Holmes-Rahe Life Stress Inventory (Holmes & Rahe, Reference Holmes and Rahe1967) and subjective stress was assessed using the Perceived Stress Scale (PSS) (Cohen, Kamarck, & Mermelstein, Reference Cohen, Kamarck and Mermelstein1983).
Neuropsychological measures
Full details of the neuropsychological testing battery are published (Taylor et al., Reference Taylor, Ajilore, Karim, Butters, Krafty, Boyd and Andreescu2024). All testing sessions were conducted via videoconference. The comprehensive battery assessed cognitive processes and domains affected in both aging and depression. Estimated premorbid cognitive function was assessed via the word reading subtest of the Wide Range Achievement Test, 5th edition (WRAT5) (Wilkinson & Robertson, Reference Wilkinson and Robertson2017). Administered tests included the Repeatable Battery for the Assessment of Neuropsychological Status (RBANS) (Randolph, Reference Randolph1998), Wechsler Adult Intelligence Scale, 4th edition (WAIS-4) Letter-Number Sequencing (Wechsler, Reference Wechsler2008), Trail Making Test (TMT), Controlled Oral Word Association Test (COWA; FAS letters and Animals) (Lezak, Howieson, Bigler, & Tranel, Reference Lezak, Howieson, Bigler and Tranel2012b), and the Golden Stroop Color and Word Test (SCWT) (Golden & Freshwater, Reference Golden and Freshwater2002). Assessed cognitive domains included: (a) learning (RBANS word list and story memory); (b) memory (delayed recall of the RBANS word lists, story, and complex figure); (c) Processing Speed (RBANS Coding, TMT part A, and SCWT word reading and color naming); and (d) executive function (COWA FAS, Letter-Number Sequencing, TMT part B, and SCWT color-word). Analyses of neuropsychological test data used converted z-scores created based on the study's comparison group performance measures.
Clinical monitoring and treatment during the longitudinal phase
Following completion of baseline assessments, regular contacts occurred every two months throughout the longitudinal study and included a mix of telephone, telemedicine, and clinic visits. After entering the longitudinal phase, participants generally continued the antidepressant regimen that led to remission. Treatment could be provided by study clinicians or existing clinical providers following standard practice. Changes to the treatment regimen were not restricted, allowing changes to antidepressant medication treatment, cessation of treatment, psychotherapy, or initiation of neuromodulation. Participants continued in the study following depressive episode relapse.
Statistical analyses
Analyses were conducted in R Statistical Software (version 4.3.2) using data from all available baseline assessments. Missing data were accounted for by either mean imputation for LASSO models or listwise deletion for general linear and logistic models.
Descriptive group differences in categorical variables were tested with Pearson's χ2 tests. The differences in continuous variables were tested with Welch two sample t test. Independent phenotypic group differences were assessed using massive univariate general linear models adjusting for age, gender, and education predicting baseline phenotypic measure scores from binary group assignment (a) comparison or LLD or (b) LLD sustained remission or relapsing. Statistical significance was assessed using both an unadjusted p value at α = 0.05 and a false discovery rate (FDR) (Benjamini & Hochberg, Reference Benjamini and Hochberg1995) corrected p value at α = 0.05.
Logistic regression with least absolute shrinkage and selection operator (LASSO) penalty was conducted to determine a reduced set of phenotypic predictors for group prediction (a) comparison or LLD, (b) LLD subgroups (sustained remission or relapsed). Models were specified using glmnet version 4.1-8 (Friedman, Hastie, & Tibshirani, Reference Friedman, Hastie and Tibshirani2010) and included standardized scores of all phenotypic variables except weight (due to collinearity with BMI), and psychiatric history measures in models including comparison participants. LASSO models were cross validated using 10 folds, and the lambda value yielding the lowest MSE was selected for the final LASSO model. A logistic regression model including the set of predictors from the LASSO and adjusting for age, gender, and education was specified to evaluate individual measure group prediction. Odds ratios were calculated with a 95% confidence interval to assess statistical significance of individual measures.
We repeated the massive univariate general linear model and LASSO logistic regression analyses using neuropsychological test performance scores as predictor variables. Initial general linear models predicted test scores from group assignment and adjusted for age, gender, and WRAT5 word reading subtest, as it is a stronger marker for estimated premorbid level of cognitive function than education (Boyle et al., Reference Boyle, Knight, De Looze, Carey, Scarlett, Stern and Whelan2021). After cross validation and lambda selection for LASSO models, a final logistic model including the set of remaining predictors from the LASSO and adjusting for age, gender, and estimated premorbid cognitive function was specified to evaluate individual test group prediction.
Finally, we tested two assumptions. First, we compared LASSO models with Ridge and Elastic Net models to determine whether LASSO models had the optimal fit (online Supplementary Table S1). Second, we tested the assumption that any missing data were missing completely at random (MCAR), we utilized Little's MCAR test. If we determined that data for any group comparison was not MCAR, we planned to rerun the final logistic model using single imputed data derived from predictive means matching and present any differences between the models.
Results
Analyses included 204 participants (135 with remitted LLD and 69 comparison participants). There were no differences between diagnostic groups in age or gender, although there was a predominance of women in both groups (Table 1). The comparison group was more highly educated and had a higher proportion of individuals from underrepresented backgrounds. Both groups had a comparable mean duration of time in the study (comparison: 574.4 days, s.d. = 374.2, range = 0–1277 days; LLD: 595.2 days, s.d. = 315.9, range = 54–1323 days; Welch's t = 0.40, 119df, p = 0.694).
Differences in clinical measures between remitted LLD and healthy comparison participants
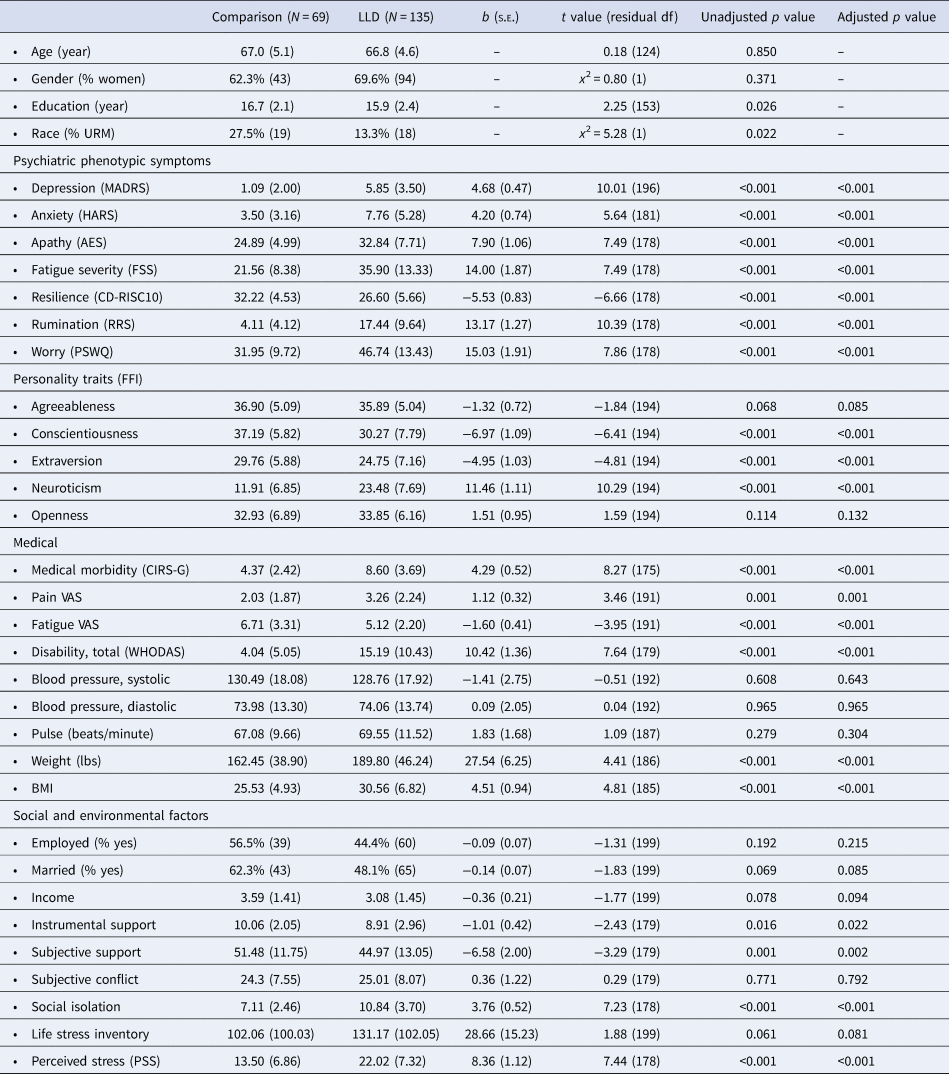
AES, Apathy Evaluation Scale; ATHF, antidepressant treatment history form; BMI, body mass index; CD-RISC10, Connor-Davidson Resilience Scale, 10 item; CIRS-G, cumulative illness rating scale, geriatric; FFI, Five Factor Inventory; FSS, fatigue severity scale; HARS, Hamilton Anxiety Rating Scale; MADRS, Montgomery-Asberg Depression Rating Scale; PSS, Perceived Stress Scale; PSWQ, Penn State worry questionnaire; RRS, ruminative response scale; s.e., standard error; URM, under-represented minority population; VAS, visual analogue 10-point scale; WHODAS, World Health Organization Disability Assessment Schedule.
Values presented as mean (standard deviation) for continuous measures and number (proportion) for categorical variables. Parameter estimates from binary group assignment presented. Models were controlling for age, gender, and education. Adjusted p values represent values after FDR (false discovery rate) correction.
In the remitted LLD group, 60 participants (44%) relapsed, while 75 (56%) sustained remission over the study. LLD participants exhibited a relatively young mean age of onset for their first depressive episode (29.51 years, s.d. = 15.28, range 4–67 years), with only 13% (18 of 135) reporting a late-life onset of depression occurring after age 50 years of age. They also reported a long mean duration for their most recent depressive episode of approximately 2.5 years (883.51 days, s.d. = 1866.72, range 14–11 095 days), with variability in the treatment intensity needed to achieve remission in the current episode (ATHF mean score = 4.38, s.d. = 2.61, range 1–12). There were no significant demographic differences between the LLD subgroups (Table 2). The relapsing subgroup exhibited a longer duration of study participation (relapsing = 686.2 days, s.d. = 271.4, range = 56–1316 days; sustained remission = 526.5 days, s.d. = 331.9, range = 54–1323 days; Welch's t = 3.09, 134df, p = 0.003).
Differences in clinical measures between LLD relapsing and sustained remission subgroups
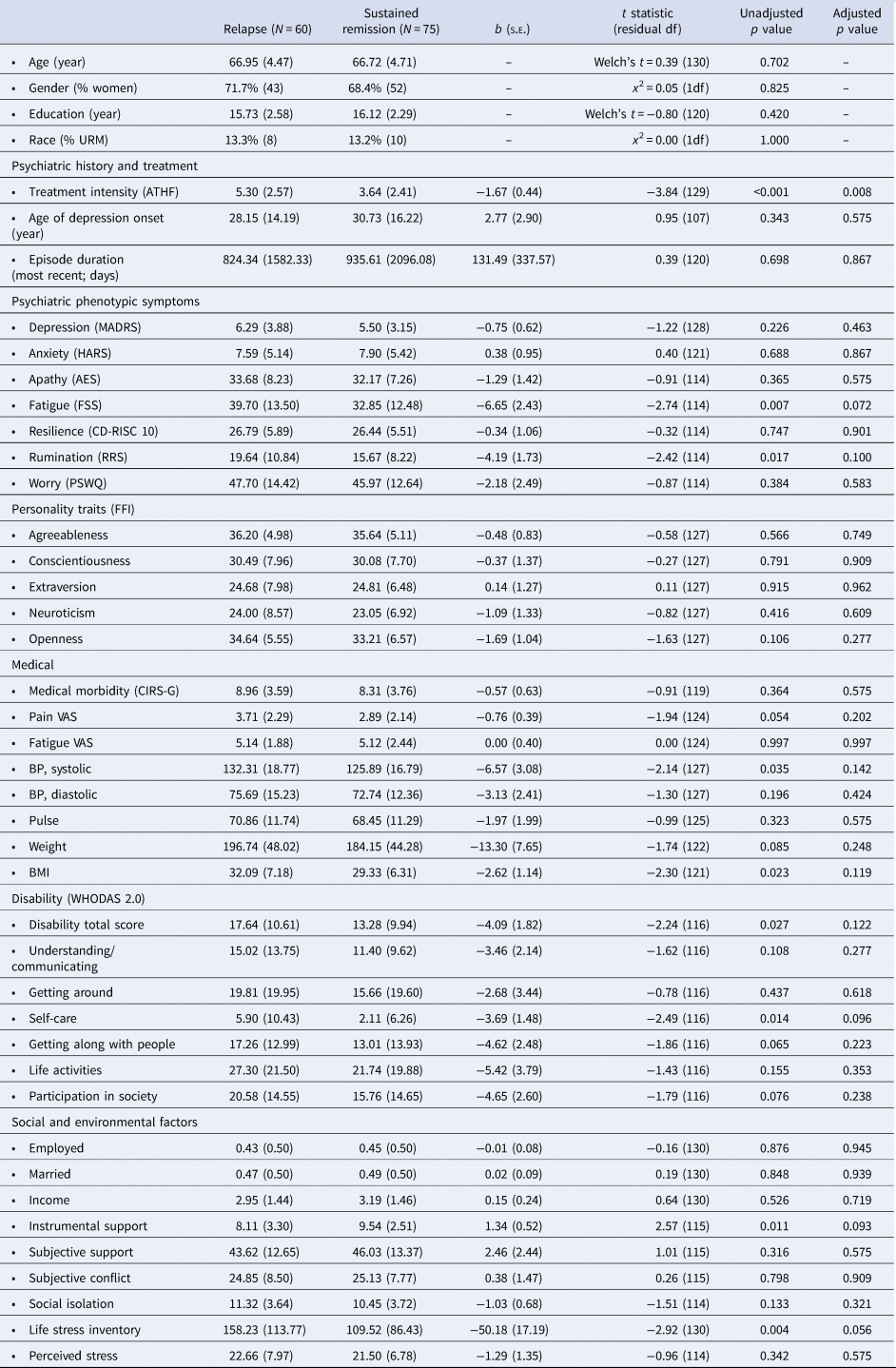
AES, Apathy Evaluation Scale; ATHF, antidepressant treatment history form; BMI, body mass index; CD-RISC10, Connor-Davidson Resilience Scale, 10 item; CIRS-G, cumulative illness rating scale, geriatric; FFI, Five Factor Inventory; FSS, fatigue severity scale; HARS, Hamilton Anxiety Rating Scale; MADRS, Montgomery-Asberg Depression Rating Scale; PSWQ, Penn State worry questionnaire; RRS, ruminative response scale; s.e., standard error; URM, under-represented minority population; VAS, visual analogue 10-point scale; WHODAS, World Health Organization Disability Assessment Schedule.
Values presented as mean (standard deviation) for continuous measures and number (proportion) for categorical variables. Parameter estimates from binary group assignment presented. Models were controlling for age, gender, and education. Adjusted p values represent values after FDR (false discovery rate) correction.
Group differences in phenotypic assessments
We observed multiple baseline differences between the LLD and comparison groups (Table 1). Despite clinical remission, the LLD group exhibited higher depressive and anxiety symptom severity, including higher self-reported apathy, fatigue, rumination, worry, and lower resilience. They also exhibited higher levels of neuroticism on the FFI and significantly lower levels of conscientiousness and extraversion. The LLD group exhibited greater medical morbidity and disability, higher pain and fatigue severity, and higher body mass index (BMI). Finally, the LLD group reported greater social isolation and lower levels of instrumental and subjective social support. They also reported higher perceived stress, despite reporting comparable severity of current life stressors.
Fewer measures significantly differed between LLD participants with sustained remission and those experiencing relapse (Table 2). At the FDR-adjusted 0.05 significance level, the only difference was that relapsing individuals required a higher intensity of treatment to achieve remission. At the unadjusted 0.05 significance level, relapsing LLD participants also exhibited greater self-reported severity of rumination and fatigue, higher systolic blood pressure, greater self-care disability, lower levels of instrumental social support, and greater severity of current life stressors.
Phenotypic predictors of diagnostic group assignment
Despite widespread individual differences between the LLD and comparison groups (Table 1), few phenotypic variables from the LASSO selection significantly predicted diagnostic group assignment in final models (N = 143; Table 3). Greater residual depression severity, greater medical morbidity, and higher self-reported rumination significantly predicted classification into the comparison and LLD groups (Table 3), as well as informing classification between the comparison group and both the sustained remission and relapse LLD subgroups (online Supplementary Table S2). Notably, in those supplemental analyses, higher systolic blood pressure differentiated the relapsing LLD subgroup from the comparison group (OR = 6.99, s.e. = 0.87; z = 1.65, 1df, p = 0.025) but did not differentiate between the sustained remission LLD subgroup and comparison group (OR = 4.34, s.e. = 0.85, z = 1.73, 1df, p = 0.083). Analyses supported that data were missing completely at random (χ2 (72) = 77.3, p = 0.310).
Clinical predictors retained in LASSO regression between study population groups and LLD subgroups
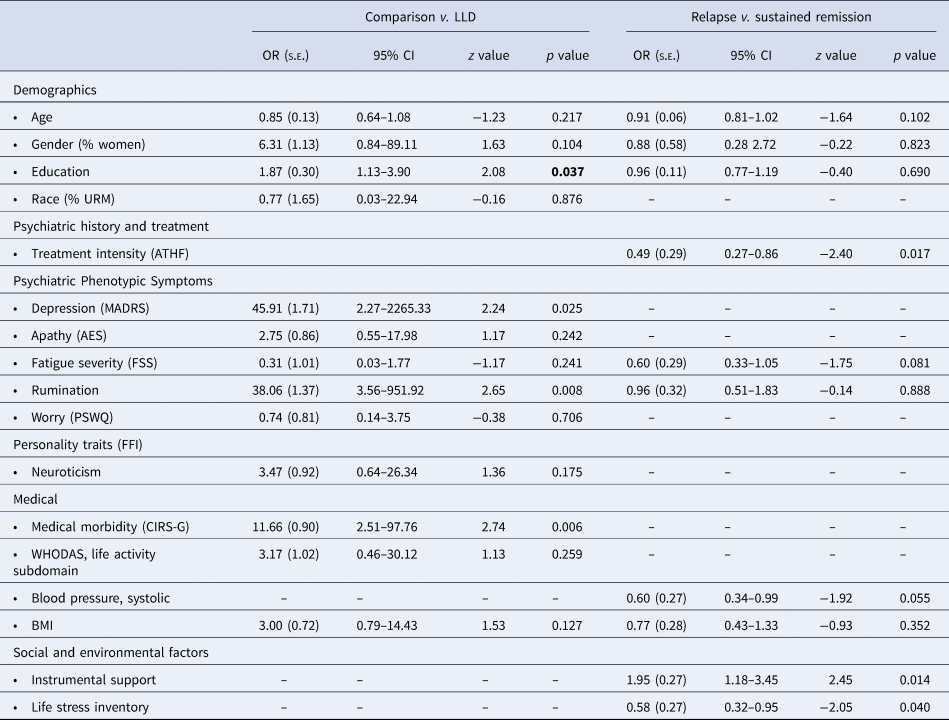
AES, Apathy Evaluation Scale; ATHF, antidepressant treatment history form; BMI, body mass index; CI, confidence interval; CIRS-G, cumulative illness rating scale = geriatric; FSS, fatigue severity scale; OR, odds ratio; PSWQ, Penn State worry questionnaire; s.e., standard error; WHODAS, World Health Organization Disability Assessment Schedule.
Estimates presented from final logistic regression model including all remaining LASSO predictors and demographic covariates. Psychiatric history variables not measured in comparison groups and excluded from LLD v. comparison models. Variables with a dash (–) were not retained in that specific model. Final models included n = 147 for LLD and comparison groups and n = 100 for relapsing and sustained remission groups.
LASSO regression models similarly identified few baseline measures predicting subsequent relapse v. sustained remission (Table 3). In the final logistic regression model (N = 100), relapsing LLD subgroup membership was primarily predicted by greater ATHF score (indicating greater intensity of antidepressant treatment needed to achieve remission), lower instrumental social support, and greater severity of life stressors. Analyses supported that data were not missing completely at random (χ2 (49) = 111, p < 0.001), so we reran the logistic regression model using single imputed data derived from predictive mean matching. The imputed model's significant predictor variables were identical to the original model, except that higher systolic blood pressure was now also significantly predictive of relapse (OR = 0.60, s.e. = 0.20, 95% CI 0.39–0.88, z value = −2.54, p = 0.011). In the original model, systolic blood pressure did not reach the a priori level of statistical significance.
Group differences in neuropsychological test performance
LLD and comparison groups exhibited comparable estimated premorbid cognitive function, assessed by the WRAT5 reading subtest standard score (comparison: 114.8 (s.d. = 10.7); LLD: 116.1 (s.d. = 11.7); Welch's t = 0.75, 133df, p = 0.453). They were also comparable on cognitive screening using the MoCA (Table 4). The LLD group exhibited lower performance only on information processing speed (RBANS Coding) and the executive function ability working memory (Letter-Number Sequencing). We did not observe any significant differences in test performance between relapsing or sustained remission LLD subgroups (online Supplementary Table S3). Analyses supported that data were missing completely at random (χ2 (6) = 7.68, p = 0.262).
Differences in neuropsychological test measures between remitted LLD and healthy comparison participants
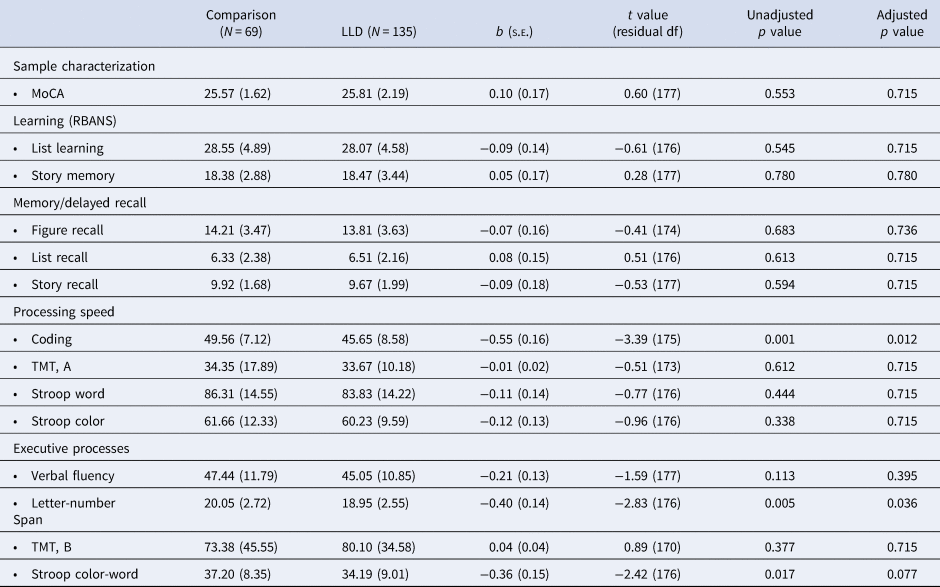
MoCA, Montreal Cognitive Assessment; RBANS, Repeatable Battery for the Assessment of Neuropsychological Status; s.e., standard error; TMT, Trails Making Test.
Values presented as mean (standard deviation). Parameter estimates from binary group assignment presented. Models were controlling for age, gender, and premorbid cognitive function measured with the WRAT5 (Wide Range Achievement Test, Version 5) word reading task score. Adjusted p values represent values after FDR (false discovery rate) correction.
Neuropsychological test performance predictors of diagnostic group assignment
Final logistic regression models examining the remaining set of neuropsychological performance tests included 178 participants (121 LLD and 57 comparison participants with full neuropsychological test data). In these models, performance on both RBANS Coding and Letter-Number Sequencing predicted assignment between LLD and comparison groups (Table 5). No neuropsychological test measures were selected in LASSO models predicting assignment into relapse or sustained remission LLD subgroups.
Neuropsychological test group predictors retained in LASSO regression between study population groups and LLD subgroups
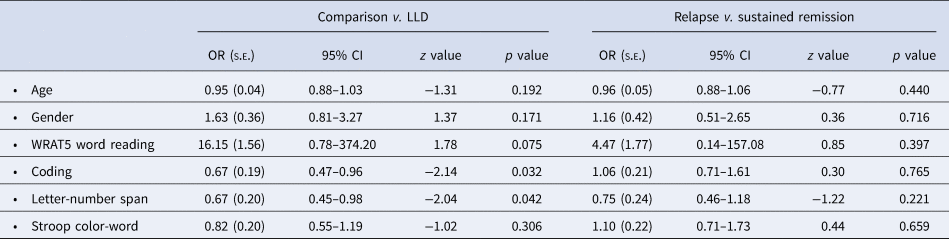
CI, confidence interval; OR, odds ratio; s.e., standard error; WRAT5, Wide Range Achievement Test, Version 5.
Estimates presented from final logistic regression model including all remaining LASSO predictors plus covariates of age, gender, and estimated premorbid function, measured by WRAT5 word reading score. Final models included n = 178 for LLD and comparison groups and n = 121 for relapsing and sustained remission groups.
Discussion
This multisite longitudinal study utilizing deep clinical phenotyping observed multiple measures exhibiting group differences between individuals with remitted, recurrent LLD and healthy comparison subjects. However, only lower education level, greater medical morbidity and more severe residual depressive and ruminative symptoms informed group classification. We observed relatively fewer phenotypic measures differing between LLD subgroups who subsequently relapsed or sustained remission over two years, while LLD subgroup classification was informed by treatment intensity and social factors. These classification variables may be particularly important as they may more accurately predict who will experience a relapse. While individuals with LLD exhibited lower performance than comparison participants on measures of processing speed and executive function, there were no LLD subgroup differences in neuropsychological test measures.
Despite being in remission, the LLD group exhibited greater residual psychiatric symptom severity across multiple clinician-rated and self-report psychiatric symptom domains, greater medical comorbidity and disability, higher BMI, personality trait differences, poorer social support, greater perceived stress, and lower cognitive function performance. The LLD group also exhibited lower levels of educational achievement, a finding consistent with past work and confounded by family background and socioeconomic factors (Bauldry, Reference Bauldry2015; Lorant et al., Reference Lorant, Deliege, Eaton, Robert, Philippot and Ansseau2003; Schaan, Reference Schaan2014). These findings replicate a broader literature describing vulnerability factors for LLD, including neuroticism, medical morbidity, stress, and poor social support (Hayward, Taylor, Smoski, Steffens, & Payne, Reference Hayward, Taylor, Smoski, Steffens and Payne2013; Szymkowicz et al., Reference Szymkowicz, Gerlach, Homiack and Taylor2023a; Taylor, McQuoid, & Krishnan, Reference Taylor, McQuoid and Krishnan2004a; Zannas, McQuoid, Steffens, Chrousos, & Taylor, Reference Zannas, McQuoid, Steffens, Chrousos and Taylor2012). It also highlights a constellation of affective symptoms that persist into ‘acute’ remission, including anxiety, apathy, fatigue, rumination, and worry. Regarding cognitive performance, while we classified RBANS Coding into the Processing Speed domain, this test measures a broad range of cognitive functions, including fine motor speed, complex attention, episodic memory, processing speed, and executive functioning (Lezak, Howieson, Bigler, & Tranel, Reference Lezak, Howieson, Bigler and Tranel2012a). In combination with the Letter-Number Sequencing test, the LLD participants demonstrated lower performance on measures tapping into executive processes. Persistent executive dysfunction is thus a core cognitive weakness that is associated with poorer response to acute antidepressant treatment, persists despite remission, contributes to disability, and increases risk of dementia (Alexopoulos, Reference Alexopoulos2019; Koenig et al., Reference Koenig, DeLozier, Zmuda, Marron, Begley, Anderson and Butters2015; Manning, Wu, McQuoid, Steffens, & Potter, Reference Manning, Wu, McQuoid, Steffens and Potter2023; Szymkowicz et al., Reference Szymkowicz, Gerlach, Homiack and Taylor2023a, Reference Szymkowicz, Ryan, Elson, Kang and Taylor2023b). However, as seen in our previous reports (Butters et al., Reference Butters, Bhalla, Mulsant, Mazumdar, Houck, Begley and Reynolds2004; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018), baseline cognitive performance measures did not inform relapse risk. However, it remains possible there is a bidirectional longitudinal relationship between decline in cognitive performance and depression relapse (Szymkowicz et al., Reference Szymkowicz, Gerlach, Homiack and Taylor2023a).
When combining all measures, LLD group classification was informed only by residual depressive symptom and rumination severity, education level, medical morbidity, and lower executive function performance. In this profile, subclinical depressive symptoms along with greater self-reflective ruminative thought processes may predispose to LLD. These influences may be worsened by greater overall medical burden, with some medical conditions contributing to executive dysfunction through injury to frontostriatal and cognitive control pathways (Taylor, Aizenstein, & Alexopoulos, Reference Taylor, Aizenstein and Alexopoulos2013). Executive function deficits may reciprocally hinder efforts to halt negative ruminative thought processes that worsen depressive symptoms (von Hippel, Vasey, Gonda, & Stern, Reference von Hippel, Vasey, Gonda and Stern2008).
Fewer factors distinguished individuals with remitted LLD who subsequently did or did not experience relapse. Unadjusted analyses associated relapse with greater residual severity of rumination and fatigue, higher systolic blood pressure, greater self-care disability, poorer instrumental social support, and greater severity of life stressors. The relationship with higher systolic blood pressure could be due to numerous factors, such as elevated sympathetic activity, differences in BMI, or effects of SNRI medications. It may be clinically meaningful, as systolic blood pressure interacts with depression to increase rates of cognitive decline (Tully, Debette, & Tzourio, Reference Tully, Debette and Tzourio2018). However, after applying the FDR adjustment, the only statistically significant difference was that individuals who relapsed were on a more intense treatment regimen as measured by ATHF. In other words, a greater intensity of treatment needed to achieve remission is a marker of vulnerability for future relapse. However, greater treatment intensity, lower instrumental social support, and greater life stress informed LLD subgroup classification. These variables are particularly important as may be more helpful in predicting relapse. While systolic blood pressure also informed subgroup classification in the imputed model, some missing data may have limited our ability to detect an effect without imputation and needs further study. Our findings replicate previous reports (Alexopoulos et al., Reference Alexopoulos, Young, Abrams, Meyers and Shamoian1989; Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018; Hinrichsen & Hernandez, Reference Hinrichsen and Hernandez1993) and point toward intervention targets that may help prevent future relapses, such as psychosocial interventions to improve social support and enhance coping with stress. It also supports our past findings that while greater residual depression severity is associated with relapse risk, this is not a particularly sensitive or specific approach (Taylor, McQuoid, Steffens, & Krishnan, Reference Taylor, McQuoid, Steffens and Krishnan2004b).
Unlike our prior report (Deng et al., Reference Deng, McQuoid, Potter, Steffens, Albert, Riddle and Taylor2018), we did not observe that age of initial depression onset differentiated relapsing and sustained remission subgroups. This may reflect that eligibility criteria specified recurrent depression, excluding individuals with a later life onset with only a single episode. Importantly, individuals with early-life onset depression can still exhibit impaired cognitive performance and remain at risk for cognitive decline (Riddle et al., Reference Riddle, Potter, McQuoid, Steffens, Beyer and Taylor2017). Relatedly, we did not quantify the total number of prior episodes beyond the two required for diagnosis. While it is straightforward to diagnose the presence of recurrent depression in older adults, our experience is that approaches to quantify the actual number of episodes are unreliable. This is due to multiple factors, including presence of cognitive impairment, recall bias, mental health stigma and lack of mental health awareness earlier in life, and chronicity of episodes for some participants.
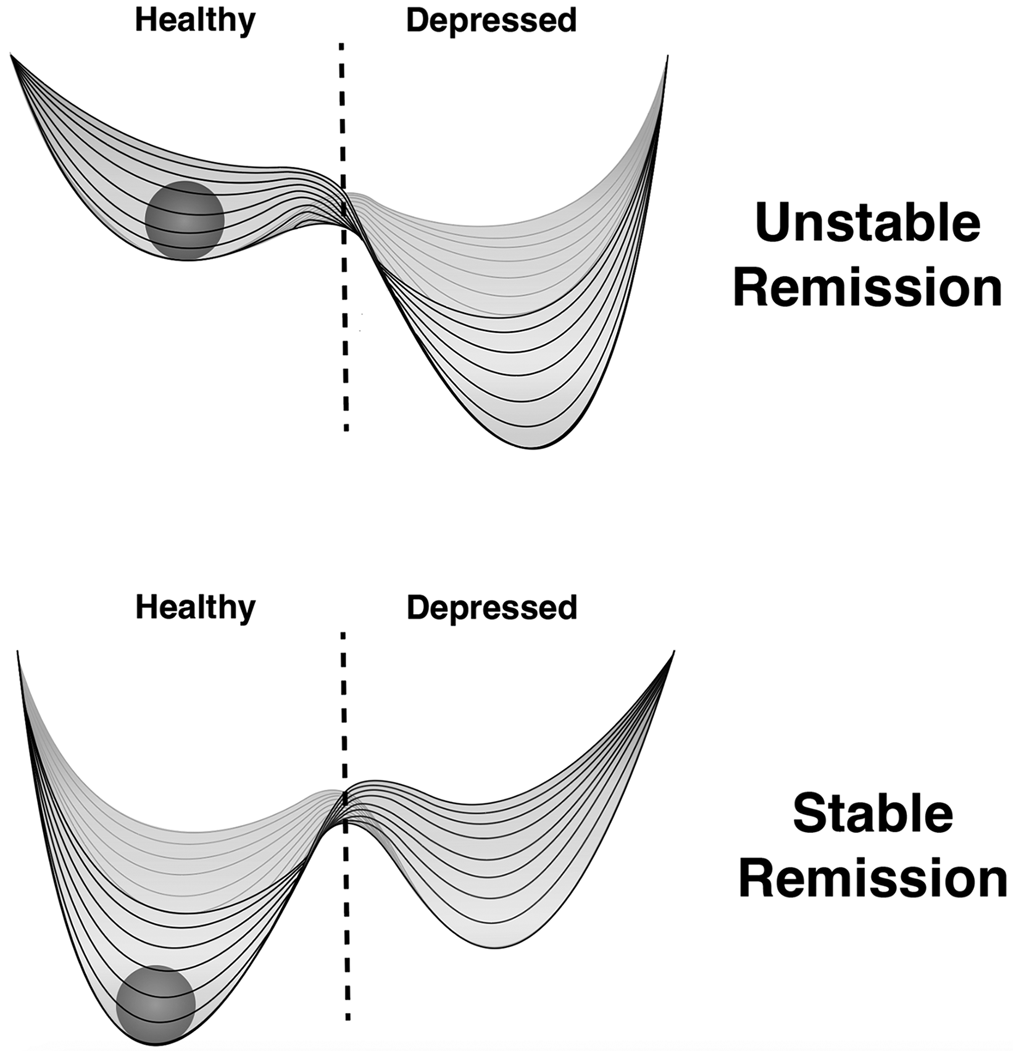
Given persistent symptoms and high risk of relapse, the conceptualization of remission in recurrent LLD may need reconsideration. As we have previously reported, this should move beyond using standard depression severity thresholds to define remission, which are neither sensitive nor specific for predicting relapse (Taylor et al., Reference Taylor, McQuoid, Steffens and Krishnan2004b). We propose our findings can be conceptualized using a dynamical systems model (Scheffer et al., Reference Scheffer, Bockting, Borsboom, Cools, Delecroix, Hartmann and Nelson2024a, Reference Scheffer, Bockting, Borsboom, Cools, Delecroix, Hartmann and Nelson2024b) where mood can be conceptualized as stability landscapes (Fig. 1), including ‘healthy’ or ‘depressed’ states. These mood states may exhibit varying levels of attractor strength and resilience, or the likelihood of that mood state persisting. Some of the characteristics identified, such as greater medical morbidity or tendency to engage in ruminative thought processes, may increase resilience of a depressed state. In contrast, greater social support may increase resilience of a healthy state. Inverse relationships are possible, as limited social support and a greater intensity of treatment required to achieve remission may indicate a more fragile remitted state, wherein exposure to stressors increases the risk of a return to the depressed state. Testing such a model and potentially establishing a new definition of remission requires quantifying the resilience of mood states (Scheffer et al., Reference Scheffer, Bockting, Borsboom, Cools, Delecroix, Hartmann and Nelson2024a) and would benefit from examining underlying neurobiological contributors (Andreescu et al., Reference Andreescu, Ajilore, Aizenstein, Albert, Butters, Landman and Taylor2019).
Variability in resilience of mood states influencing relapse vulnerability. In both figure examples, the participant in remission (illustrated by the ball) is in the healthy state. However, the ‘stable remission’ displays a more resilient topographic landscape where a greater impetus is needed to ‘push’ the individual back into a depressive episode. In contrast, the ‘unstable remission’ displays a more fragile topography, where a modest change could precipitate a new depressive episode. Our data suggest that a greater antidepressant intensity needed to achieve remission indicates a more fragile, unstable remission state. Greater life stress and lower social support may provide the impetus to re-enter a depressive episode, should the hurdle to entering a new state be overcome.
Accurately identifying individuals experiencing such a ‘fragile’ remission with elevated risk of relapse can inform sorely needed relapse prevention interventions (Cuijpers, Beekman, & Reynolds, Reference Cuijpers, Beekman and Reynolds2012). A variety of interventions for primary or secondary prevention have been studied in various populations, with evidence supporting potential benefits of psychotherapeutic interventions and physical activity (Hoare et al., Reference Hoare, Collins, Marx, Callaly, Moxham-Smith, Cuijpers and Berk2021). Secondary prevention, or preventing recurrent episodes for high-risk individuals with LLD, may be crucially important to reduce the effect of depression on a range of health outcomes, including dementia risk.
While study strengths include depth of participant characterization and length of followup, there are limitations. Despite following participants prospectively, these analyses examined only cross-sectional predictors. Thus, we cannot comment on whether relapse or sustained remission contribute to changes in residual affective symptoms or changes in cognitive performance over time. Additionally, while not demented on screening, some participants would be expected to decline over time. However, we did not assess Alzheimer's-related biomarkers, so cannot comment about any underlying neuropathology. Finally, as participant followup is ongoing, it is possible some individuals may experience a later relapse so are incorrectly classified as being in the sustained remission subgroup.
In conclusion, remitted LLD is characterized by residual depressive symptoms, rumination, lower education, greater medical morbidity, and executive dysfunction. In contrast, only a few key variables contributed to the classification of LLD subgroups and distinguished individuals who experienced a relapse, including greater antidepressant treatment intensity, lower instrumental support, and greater life stress. While the goal in clinical treatment should always be to achieve the lowest level of depression severity possible, this may not fully protect against relapse (Taylor et al., Reference Taylor, McQuoid, Steffens and Krishnan2004b). Future work is needed to examine neurobiological differences related to relapse risk, examine how phenotypic and neuroimaging measures change over time and are influenced by relapse, and examine how this work can guide risk stratification and inform preventive interventions.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291724003246.
Funding statement
This work was supported by National of Institute of Health grants R01 MH108506, R01 MH121619, R01 MH121620, and R01 MH121384, and the National Center for Advancing Translational Sciences grants UL1 TR000445 and UL1 TR002243.
Competing interests
All authors deny any competing interests or conflict of interest with this work.








