Introduction
Healthcare professionals (HCPs) are among the most vulnerable groups at high risk of exposure to infectious agents due to occupational exposures, making them a priority population for both infection prevention and control (IPC) and immunization programs. Reference Ndongo, Eteki and Siedner1–Reference Cheuyem, Lyonga, Kamga, Mbopi-Keou and Takougang3 A systematic review conducted across 21 African countries found that two-thirds of HCPs had at least one occupational exposure during their career, with both public and private health facilities being equally affected. Reference Cheuyem, Lyonga, Kamga, Mbopi-Keou and Takougang3,Reference Mengistu and Tolera4 Effective IPC and vaccination are essential for protecting HCPs, maintaining resilient health systems, and preventing healthcare-associated infections. 5
Systemic challenges, such as limited IPC infrastructure, irregular supply of personal protective equipment (PPE), and inadequate training on standard precautions, magnify the risk in low- and middle-income countries (LMICs) like Cameroon. Reference Nteungue, Tandi and Campbell6–Reference Sastry, Masroor and Bearman9 Behavioral factors such as high workload and low-risk perception, which reduce adherence to basic precautions, are additional factors to these systemic challenges. Reference Cheuyem, Lyonga, Kamga, Mbopi-Keou and Takougang3,8,Reference Sastry, Masroor and Bearman9 Along the same line, the burden of vaccine-preventable diseases like hepatitis B and COVID-19 remains significant amongst HCPs, with low vaccination coverage attributed to limited access, vaccine hesitancy, and the absence of institutional policies. Reference Ndongo, Eteki and Siedner1,Reference Nteungue, Tandi and Bilounga Ndongo7,Reference Mueller, Stoetter and Kalluvya10
Although most studies in Cameroon have separately investigated IPC and vaccination regarding healthcare workers’ safety, a significant gap remains in integrated assessments of both IPC knowledge and vaccination status within the same group of HCPs. Understanding the common link between the two domains is essential for designing holistic interventions that address behavioral, structural, and systemic barriers to HCP protection.
This study aimed to assess the uptake of occupational vaccinations (hepatitis B and COVID-19) and IPC knowledge among HCPs in four selected health facilities in the Fako division of Cameroon. The goal was to assist in developing integrated strategies to improve occupational safety and health outcomes among HCPs.
Materials and method
Study design: This cross-sectional study was conducted among HCPs at four selected health facilities in the Fako Division, Cameroon.
Study period and Populations: The study was conducted over five months (January to May 2024) among HCPs at four health facilities.
Study area and setting: The study was conducted across all units of Buea Regional Hospital (BRH), Limbe Regional Hospital (LRH), Mount Mary Hospital (MMH), and Solidarity Health Foundation (SHF).
Buea Regional Hospital (BRH) is a secondary-level health facility in the South West Region. The hospital has pediatrics, internal medicine, Surgery, Obstetrics, Gynecology, and a laboratory. The HCPs are made up of doctors (30, nurses and midwives (180), laboratory technicians (lab.technician) (30), and pharmacy attendants (06).
The LRH is a secondary health facility and a referral hospital in the SW region. The hospital has a pediatric department, an obstetrics and gynecology department, an internal medicine department, a surgical department, and a laboratory. The HCPs are made up of doctors (39), nurses and midwives (181), lab. technician (36), and pharmacy attendants (06).
Mount Mary Hospital (MMH) is situated in Buea at the foot of Mount Cameroon, and covers. a total catchment area is about 50,000. It has internal medicine, pediatric, maternity, laboratory, and outpatient departments. The HCPs are made up of doctors (05), nurses (26), midwives (13), lab.technicians (09), and pharmacy attendants (02).
Solidarity Health Foundation (SHF) is a private clinic located in Buea. The clinic is made up of medical, surgical, maternity, pediatric, and laboratory. The HCPs are made up of doctors (9), nurses (27), midwives (09), lab. technician (08), pharmacy (05).
Sampling and sample size determination
After selecting four health facilities via convenience sampling, a minimum sample of 242 was calculated from 607 HCPs using Yamane’s formula. This was increased to 267 to account for a 10% nonresponse rate. A total of 276 HCPs were recruited via simple random sampling across the four previously mentioned health facilities, using a proportionate-to-size sampling approach.
Proportionate to size sampling from each of the four facilities:
![]() ${n\times Nf \over N}$
${n\times Nf \over N}$
n: minimum sample size of the study population
Nf: total number of healthcare workers in the health facility
N: the total number of healthcare workers in all the hospitals
BRH:
![]() ${267\times 240 \over 607}$
=105.56 ∼ 106
${267\times 240 \over 607}$
=105.56 ∼ 106
LRH:
![]() ${267\times 256 \over 607}$
= 112.60 ∼ 113
${267\times 256 \over 607}$
= 112.60 ∼ 113
MMH:
![]() ${267\times 53 \over 607}$
= 23.31 ∼ 24
${267\times 53 \over 607}$
= 23.31 ∼ 24
SHF:
![]() ${267\times 58 \over 607}$
= 25.51 ∼ 26
${267\times 58 \over 607}$
= 25.51 ∼ 26
Data collection
A pretested, self-administered, structured questionnaire, designed for this study, was used to collect data on the participants’ sociodemographic characteristics, Vaccination status (hepatitis B and COVID-19), and knowledge of IPC. The assessment of knowledge questionnaire was adapted from a 10-item questionnaire in a study by Mutaru et al., 2022 in Ghana, a similar LMIC context, with a Cronbach’s alpha of .691. Reference Mutaru, Balegha, Kunsu and Gbeti11
Study variables
Dependent variables
-
• Proportion of occupational vaccine uptake.
-
• Knowledge of IPC measures (good, poor).
Independent variables
Age, gender (male, female), Cadre (doctor, nurse/midwife, lab.technician), PPE availability (yes, no), previous occupational hazard exposure (yes, no), work experience (<3 yr, 3–7 yr, > 7 yr), training on IPC (yes, no), IPC committee (yes, no), IPC guideline in the facility (yes, no), employment status ( volunteer, contract worker, public worker)
Study procedure
Two research team members pretested the structured questionnaire among 10 HCPs in a different facility. After obtaining written consent, the structured questionnaire was self-administered to assess participants’ knowledge of IPC practices and occupational vaccination status (hepatitis B and COVID-19).
Data analysis
Data was cleaned in Excel and exported into StataSE 18.5 for analysis. Categorical variables were presented as frequencies and percentages, and quantitative variables as means with standard deviations or medians with interquartile ranges. A good knowledge was set at or above the mean knowledge score (≥7). Multivariable logistic regression analysis was used to identify factors independently associated with good knowledge and with combined occupational vaccine uptake. Covariates from the univariable model included in the multivariable model for good knowledge had a cut-off P < .20. In contrast, combined occupational vaccine uptake was based solely on theoretical relevance to the study. Multicollinearity was assessed using the mean-variance inflation factor: 1.22 for the occupational vaccine uptake model and 1.14 for the good knowledge model. Backward elimination was done to obtain the final full models. The model fitness with Hosmer-Lemeshow goodness of fit for the occupational vaccine uptake model, P = .644, and for the good knowledge model, P = .246. The level of significance was set at P value <.05
Definition of terms
-
1. Occupational vaccine. These are vaccines required to protect workers, such as HCPs, against diseases related to their jobs. for example hepatitis B, COVID-19, influenza virus. However, this study assessed the uptake of COVID-19 and hepatitis B, which are required in this study setting.
-
2. Combined occupational vaccine uptake. Participants who have received both the COVID-19 and hepatitis B vaccines.
-
3. Good IPC knowledge. Participants with IPC knowledge score of seven or more (based on the mean knowledge score of ≈ 7 in the study).
Results
In this study, the 18 to 25-year age group was slightly higher at 56.5%. Most participants were female (72.8%), and most workers were volunteers, with 65.6% having worked for 3 to 7 years. Nurses represented 53.3% of the participants, doctors 25.0%, laboratory technicians 13.0%, and midwives 8.7%. In this study, 87.3% of participants had appropriate PPE in their health facilities, 87% had IPC guidelines in their departments, 67.7% had received IPC training, and 69.9% had IPC committees in place. See Table 1.
Table 1. General characteristics of participants and facility in Fako division (N = 276)

Occupational vaccine uptake among healthcare professionals
In this study, the uptake of the COVID-19 vaccine was 32.6% (95% CI: 27.1–38.5), while the uptake of the hepatitis B vaccine was 67.4% (95% CI: 61.5–72.9). The percentage of HCPs who received at least one vaccine was 78.6% (95% CI: 73.3–83.3). Meanwhile, the proportion of HCPs who received both vaccines was 21.4% (95% CI: 16.7–26.7).
For COVID-19 vaccine uptake, midwives had the lowest proportion (25.0%), followed by doctors (30.4%), with no difference in professional cadre (P = .774). More males (36.0%) took the vaccine than females (31.3%) (P = .463), and more participants with previous exposure to COVID-19 (41.0%) took the vaccine than those without (29.0%) (P = .052). More HCPs with IPC training (34.8%) received the vaccine than those without IPC training (28.1%) (P = .269), and participants with more than 7 years of work experience (48.0%) had higher vaccine uptake than their counterparts (P = .190). See Table 2.
Table 2. Occupational vaccine uptake among healthcare professionals in Fako division

%, percentage; IPC, infection prevention and control.
For hepatitis B vaccine uptake, laboratory technicians (77.8%) had the highest proportion, whereas doctors (50.7%) had the lowest (P = .007). A higher percentage of participants with IPC training (74.3%) received the vaccine than those without IPC training (52.8%) (P < .001). More HCPs with more than seven years of work experience (84.0%) received the vaccine than those with less than three years (72.6%) and those with three to seven years (62.3%) (P = .046). See Table 2.
For HCPs who had received at least one vaccine, doctors (62.3%) exhibited the lowest uptake, while midwives (87.5%) showed the highest (P = .002). A higher percentage of participants with IPC training (85.0%) received the vaccine than those without IPC training (65.2%) (P < .001). More HCPs with previous occupational exposure (31.3%) received both vaccines than those without reported exposure (17.1%) (P = .008). See Table 2.
Factors associated with complete occupational vaccine uptake of healthcare professionals in Cameroon
After controlling for other factors, age greater than 25 years (aOR: 2.41 [95% CI: 1.33–4.39], P = .004) and previous accidental exposure (aOR: 2.14 [95% CI: 1.17–3.93], P = .014) were independently associated with HCP uptake of complete vaccination (both hepatitis B and COVID-19 vaccine). Good knowledge of IPC (aOR: 0.91 [95% CI: 0.47–1.78], P = .789), having trained in IPC (aOR: 1.19 [95% CI: 0.55–2.60], P = .657), and working in a facility with an IPC committee (aOR: 1.25 [95% CI: 0.60–2.62], P = .548) where not associated with complete occupational vaccination of HCPs. See Table 3.
Table 3. Factors associated with complete occupational vaccine uptake of healthcare professionals

IPC, infection prevention and control; aOR, adjusted odds ratio; %, percentage; N, sample; CI, confidence interval.
Knowledge of infection prevention and control among healthcare professionals
In this study, the mean IPC knowledge score was 7.05 (SD ±1.12). HCPs with a good knowledge of IPC constituted 34.8% (95% CI: 29.2–40.7).
Laboratory technicians (47.2%) had the highest proportion of good knowledge of IPC, followed by midwives (41.7%). Doctors (27.5%) demonstrated the least knowledge of IPC (P = .204). Contract workers were more knowledgeable about IPC (50.0%), whereas state workers were the least knowledgeable about IPC (24.1%) (P = .009). Participants with prior occupational hazard exposure were less knowledgeable about IPC (28.9%) than those without previous exposure (37.3%) (P = .180). Healthcare professionals (HCPs) in facilities with PPE were more knowledgeable about IPC (37.3%) than those without PPE (17.1%) (P = .019). Additionally, HCPs who received IPC training (36.4%) had better IPC knowledge than those without IPC training (31.5%) (P = .424). The proportion of participants with IPC guidelines who had good knowledge of IPC was 35.4%, whereas those without IPC guidelines was 30.6% (P = .568). See Table 4.
Table 4. Proportions of good knowledge of infection prevention and control among healthcare professionals (n = 276)

X2, Chi square; n, number of participants; %, percentage; IPC, infection prevention and control; PPE, personal protective equipment.
Assessment of knowledge of infection prevention and control practice
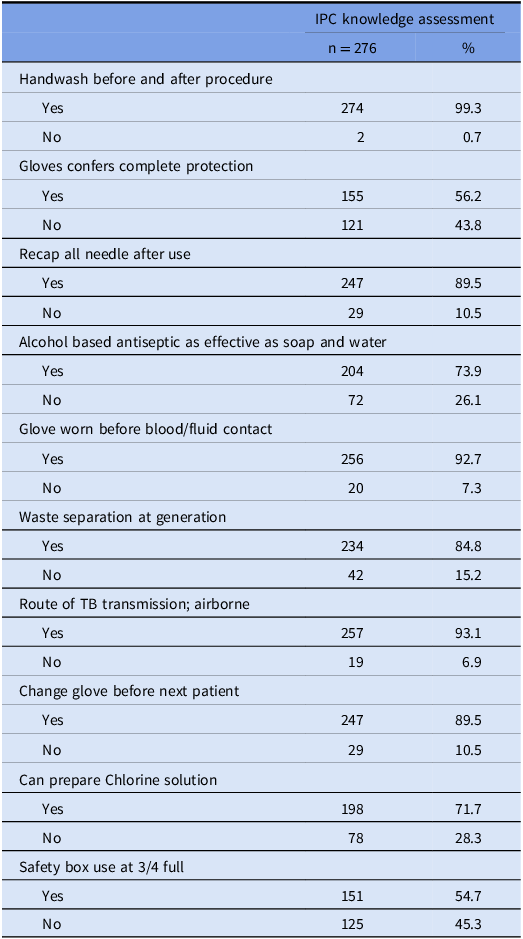
In this study, 56.2% of participants answered that gloves confer complete protection, 89.5% answered that all needles should be recapped after use, and 54.7% answered that the safety box should still be used when three-quarters full. See Table 5.
Table 5. Knowledge assessment on IPC components among healthcare professionals (n = 276)

Factors associated with good knowledge of infection prevention and control among healthcare professionals
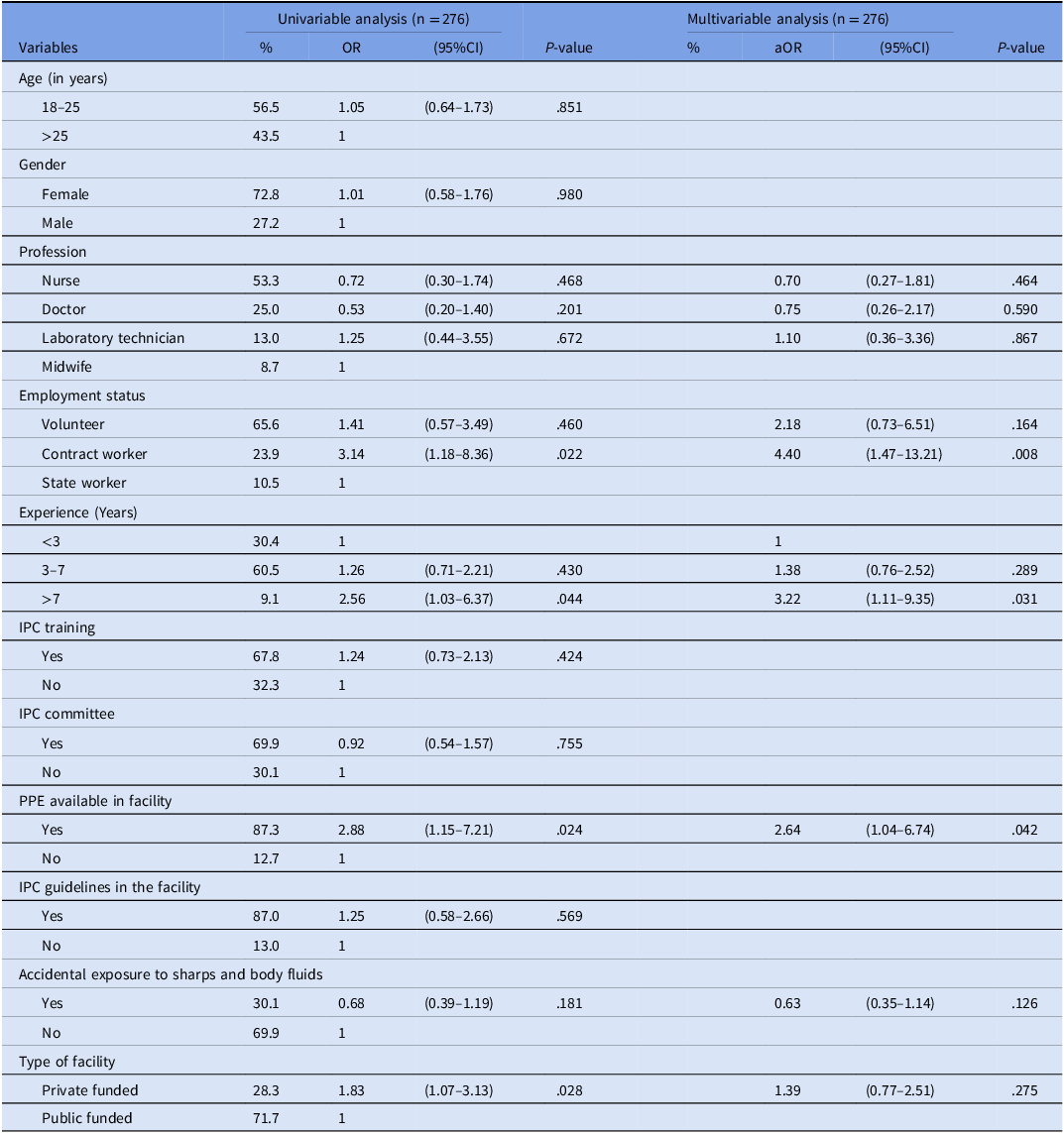
In the multivariable regression analysis, HCPs working in a department with PPE (aOR: 2.64 [95% CI: 1.04–6.74], P = .042), having more than 7 years of work experience (aOR: 3.22 [95% CI: 1.11–9.35], P = .031) and being a contract worker (aOR: 4.40 [95% CI: 1.47–13.21], P = .008) were independently associated with good knowledge of IPC. It is worth noting that having complete occupational vaccination was not associated with good knowledge of IPC. Previous occupational hazard exposure was not associated with good knowledge of IPC (aOR: 0.63 [95% CI: 0.35–1.14], P = .126). See Table 6.
Table 6. Factors associated with good knowledge of infection prevention and control among healthcare professionals in Fako division

PPE, personal protective equipment; IPC, infection prevention and control; TBP, transmission-based precautions; OR, odds ratio; aOR, adjusted odds ratio; n, sample; %, percentage; CI, confidence interval.
Discussion
This study assessed vaccination status for hepatitis B and COVID-19, and knowledge of IPC HCPs in the Fako division of Cameroon. The findings revealed a disparity in vaccine uptake, with significantly lower uptake for the COVID-19 vaccine compared to the hepatitis B vaccine, and identified a knowledge gap in IPC among HCPs in the study area.
Hepatitis B vaccination uptake was higher (67.4%) compared to COVID-19 vaccine uptake (32.6%) among HCPs. In 2018, Ndongo et al reported that fewer than 25% of HCPs received hepatitis B virus (HBV) vaccination, Reference Ndongo, Eteki and Siedner1 which contrasts with our findings and may indicate a marked improvement in HBV prevention among HCPs in Cameroon over the years. However, the higher HBV vaccine uptake in this study may be due to HBV vaccination being considered for at least the first dose. In contrast, in the study by Ndongo et al., three complete doses were considered vaccination. This is similar to the findings by Ogoina et al.,2014 in Nigeria, where they reported that 64.5% of HCPs had received at least a dose of HBV vaccine, and 36.2% had three full doses. Reference Ogoina, Pondei, Adetunji, Chima, Isichei and Gidado12 Despite this coverage, up to 31.3% to 48.9% of HCPs are susceptible to HBV, necessitating ongoing efforts to improve coverage. Reference Ziraba, Bwogi, Namale, Wainaina and Mayanja-Kizza2,Reference Mueller, Stoetter and Kalluvya10
The COVID-19 vaccine uptake in this study was lower than the 42.12% reported among HCPs in a systematic review and meta-analysis in Cameroon by Cheuyem et al., 2025. Reference Cheuyem, Amani and Achangwa13 It is worth noting that both levels of coverage are below the 70% target set by Cameroon and international partners in 2022. 14 This low uptake is attributed to vaccine hesitancy. A study in Cameroon by Aseneh et al., 2023 reported factors associated with COVID-19 vaccine hesitancy among HCPs, which were a lower perception of the importance of the vaccine on their personal health, little or no trust in the COVID-19 vaccines, greater concerns about vaccine-related adverse effects, and uncertainty about colleagues’ acceptability of the vaccine. Reference Aseneh, Agbor and Kadia15 The low COVID-19 vaccine uptake among HCPs necessitates ongoing efforts to educate them on the importance of vaccination to protect themselves and their patients in high-risk settings, such as healthcare settings.
There were disparities in vaccine uptake among different professional groups. Laboratory technicians had the highest hepatitis B vaccine uptake at 77.8%, while doctors had the lowest, at 50.7%. This may be because laboratory technicians work more frequently with sharps, blood samples, and bodily fluids, making them more aware of the health risks. This contrasts with a systematic review and meta-analysis in Africa, which reports that doctors are more likely to be fully vaccinated against HBV than nurses at 52.4%. Reference Auta, Adewuyi, Kureh, Onoviran and Adeloye16 This implies that 1 in 2 doctors in this study setting is susceptible to HBV, indicating the need for more stringent measures to increase vaccine uptake.
The factors identified as significant predictors of combined occupational vaccination uptake (HBV and COVID-19) were age over 25 years and previous accidental occupational exposure. These findings align with other authors who demonstrate that age and past exposures serve as strong motivators for vaccine uptake due to heightened risk awareness. Reference Nteungue, Tandi and Campbell6 Contrary to expectations, IPC training, presence of IPC committee, and good IPC knowledge were not significantly associated with combined occupational vaccine uptake. This disconnect between knowledge and practice could be due to systemic barriers, inconsistent training quality, or inadequate reinforcement of IPC principles during clinical activities.
This study found that only 34.8% of HCPs had a good knowledge of IPC measures despite IPC training (67.7%), the availability of PPE (87.3%), and IPC guidelines (87%). These findings are similar to a study in Ghana by Mutaru et al., 2022 where IPC knowledge was low despite adequate training opportunities. Reference Mutaru, Balegha, Kunsu and Gbeti11 This suggests that it is not enough to train providers and provide IPC materials; ongoing follow-up and knowledge retention over time are also necessary.
Certain misconceptions about IPC knowledge were reported, where 52.2% of HCPs believed that disposable gloves provided complete protection, and 89.5% reported that needles should be recapped after use. In addition, only 45.3% correctly identified that safety boxes should not be used when three-quarters full, which is lower than the 85.2% reported by Mutaru et al., 2022 in Ghana. Reference Mutaru, Balegha, Kunsu and Gbeti11 These misconceptions are also noted in other studies in Africa, and are linked to higher occupational risks. Reference Sastry, Masroor and Bearman9
PPE availability and having more than 7 years of work experience were predictors of good IPC knowledge. This demonstrates that hands-on experience and resource availability play a significant role in reinforcing IPC principles. In addition, being a contract worker was associated with good IPC knowledge. This is because contract workers often undergo more frequent orientation or refresher training as part of short-term or project-based employment, and may have concerns about job security and contract renewal, which may motivate greater adherence to institutional IPC protocols. However, IPC training was not a predictor of good knowledge. This is in line with findings from the WHO Global Report on IPC, which emphasized the importance of practical, experience-based training over theoretical instructions 8 as IPC training in this setting is often a one-off session, with insufficient emphasis on practical application and continuous reinforcement.
Recommendations
-
1. Stakeholders should enhance IPC training by emphasizing practical application over theoretical knowledge and by conducting regular workshops with hands-on simulations to address misconceptions about PPE use and sharps handling.
-
2. Focused risk communication strategies to address vaccine hesitancy, most especially among doctors, to improve occupational vaccine uptake.
Study strength and limitation
The study offers a comprehensive perspective on occupational health readiness by evaluating vaccine uptake (hepatitis B and COVID-19) alongside IPC knowledge.
Study limitations include relying on individuals’ self-reported vaccination status and infection prevention control (IPC) practices, which can introduce social desirability or recall bias and compromise the accuracy of the results. The study was conducted in four conveniently selected health facilities, which limits the generalizability of the findings to all healthcare workers in Fako Division. In addition, the cross-sectional nature of the study precludes establishing causal relationships between the identified factors and IPC knowledge or vaccination uptake.
Data availability statement
The data that supports the findings of this study are available on reasonable request from the corresponding author.
Acknowledgements
The authors sincerely thank each participant for their valuable contributions. The research team expresses gratitude to Buea and LRHs, MMH, SHF, and Triad Research Foundation for their essential support in bringing this project to fruition.
Authors contribution
Conceptualization: SMT, LTM, DGT, Methodology: SMT, LTM, DGT, Data curation: MMT, TFT, AMZS, Data analysis: LTM, Writing- Original draft preparation: SMT, LTM, LAK, MTN, STE, FEJ, and MMT, Visualization: LTM and BCMP, Supervision: DGT, Writing- Reviewing and Editing: All authors.
Financial support
None reported.
Competing interests
All authors report no conflict of interest relevant to this article.
Ethical standard
Ethical clearance was obtained from the Institutional Review Board of the Faculty of Health Sciences at the University of Buea (Reference;2024/2364–01/UB/SG/IRB/FHS) and administrative approval from the four health facilities. After clearly explaining the research and its goal, informed consent was obtained from the participants.