Introduction
The study was set in a community-based otolaryngology practice in Malta. Retrospective records of 7476 patients presenting at a rhinology clinic showed that 25 per cent had significant facial pain. A cohort of 240 patients who satisfied the criteria for chronic facial pain was followed for 3 years in an attempt to classify the types of facial pain according to International Headache Society criteria1 and to report on long-term patient outcome. The study aimed to identify clinical patterns in these patients that could help the otolaryngologist distinguish between the main categories of chronic facial pain. The body mass index (BMI), occupation and educational level of this cohort were compared to those in the general population.
A recent study of 305 Maltese patients who satisfied the 1997 American Academy Taskforce clinical criteria for chronic rhinosinusitis identified facial pain as the commonest principal presenting symptom. However, 60 per cent of these patients had normal sinus computed tomography (CT) scans.Reference Agius2 ‘Sinusitis’ may therefore not have been an appropriate diagnosis in spite of chronic facial pain.Reference Kieff and Busaba3 The European Position Paper of 2007 published revised diagnostic criteria for rhinosinusitis that included correlation of CT with nasal endoscopic findings.Reference Fokkens, Lund, Mullol, Bachert, Cohen and Cobo4 The 2012 update contained a section on facial pain as this may present under the guise of chronic rhinosinusitis.Reference Fokkens, Lund, Mullol, Bachert, Alobid and Baroody5
Patients presenting with symptoms of rhinosinusitis, but with normal sinus CT and nasal endoscopy, have responded to medical treatment for neurological diagnoses.Reference West and Jones6 Jones described mid-facial segmental pain as a tension-type pain of neurological origin, pressing or aching in quality, with a bilateral distribution involving the nasion, peri-orbital regions, cheeks or paranasal areas.Reference Jones7 Mid-facial segmental pain involves the frontal, parietal and occipital regions and is associated with tension-type headaches.Reference Jones8
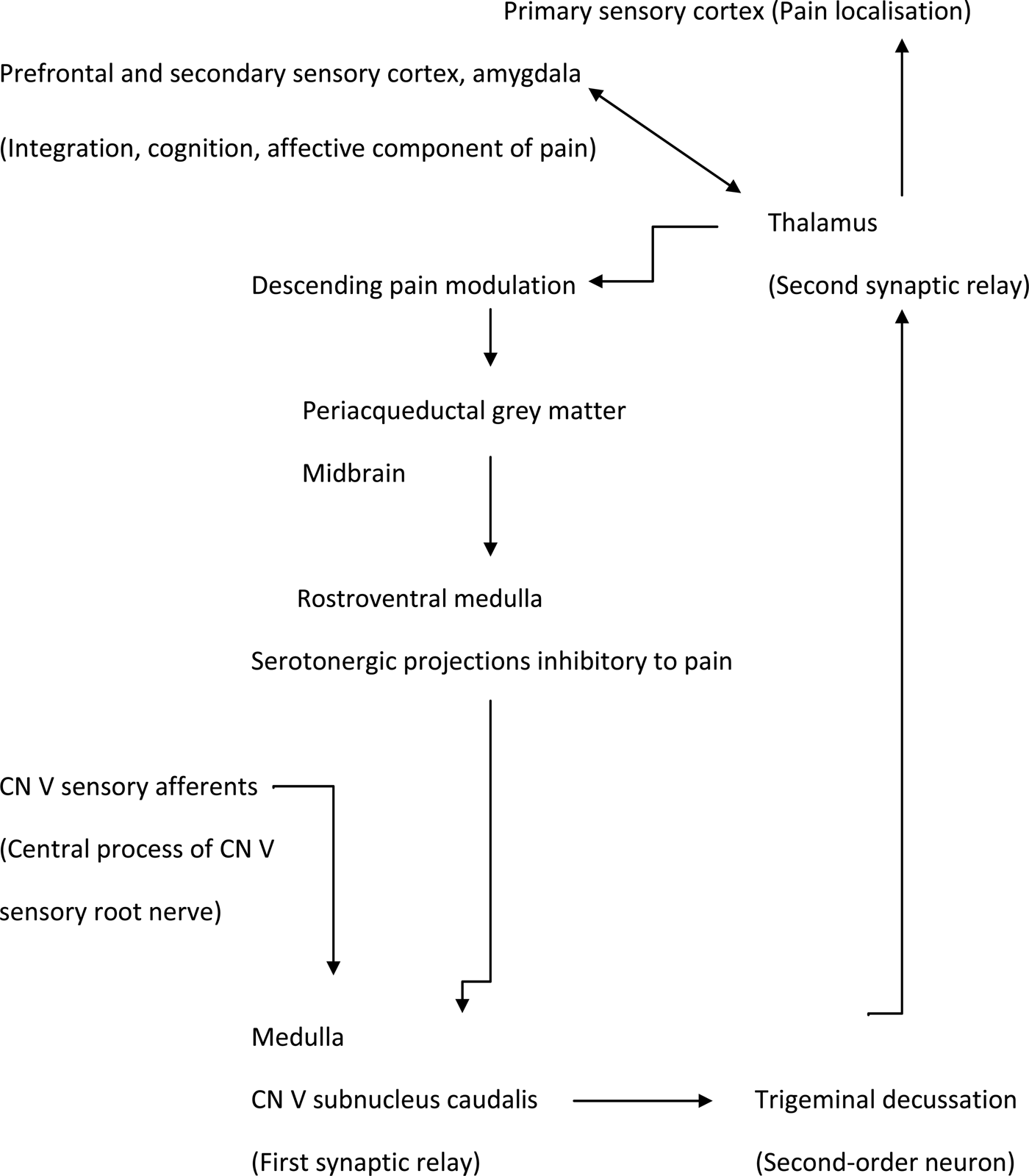
Tension-type pain is thought to be due to sensitisation of second order neurons at the trigeminal nucleus subcaudalis, which is the facial equivalent of the dorsal horn of the spinal cord (Figure 1).Reference Bendtsen9 Face, head and neck afferents converge onto the subnucleus caudalis. This convergence explains why headache and neck ache frequently accompany tension-type facial pain.Reference Sessle, Hu, Amano and Zhong10, Reference Bartsch and Goadsby11 Convergence may also explain why autonomic nasal symptoms frequently accompany chronic facial pain.
Schematic diagram of the facial nociceptive pathway. CN = cranial nerve

Jones suggested low-dose amitriptyline as an effective treatment for mid-facial pain.Reference Jones7 Tricyclic antidepressants are known to be effective in the prophylaxis of tension-type headache and are thought to reduce the sensitivity of second order neurons at the level of the spinal cord.Reference Bendtsen, Jensen and Olesen12
In chronic tension-type headache, as defined by the International Headache Society classification 2.3, patients have at least 15 days per month with headache along with the characteristics detailed in Table I.1 The criteria for chronic mid-facial pain were extrapolated from these criteria.
Diagnostic criteria for chronic tension-type headache1

Migraine is a common episodic disorder of the central nervous system, affecting 10 to 15 per cent of the population. It is more prevalent in women, with a female-to-male ratio of 3:1, and peaks at the fourth to fifth decade of life.Reference O'Brien, Goeree and Steiner13–Reference Lyngberg, Rasmussen, Jorgensen and Jensen15 Migraine causes a unilateral throbbing-type headache with photophobia, phonophobia, nausea and vomiting. The headache sometimes spreads to the face. In migraine with aura, the pain is preceded by neurological symptoms such as visual disturbances or numbness. Of 100 patients who referred themselves for ‘sinus headache’, up to 52 per cent were classified as having migraine without aura.Reference Eross, Dodick and Eross16 Facial migraine without aura may be easily misdiagnosed as ‘sinusitis’ because autonomic nasal symptoms may be present.Reference Obermann, Mueller, Yoon, Pageler, Diener and Katsarava17
The International Headache Society defines chronic migraine as over 15 days per month with headache with the characteristics described in Table II.
Diagnostic criteria for migraine without aura1

Materials and methods
A total of 240 patients who had experienced chronic mid-facial pain for at least 4 hours daily, for a minimum of 15 days per month, over a period of at least 3 months (as per the international classification of headache disorders1) were eligible for entry into the study. These patients were prospectively followed up for 36 months to determine their long-term outcomes.
The processes of prospective recruitment and follow up were conducted in accordance with the Consolidated Standards of Reporting Trials (‘CONSORT’) guidelines.Reference Moher, Hopewell, Schulz, Montori, Gøtzsche and Devereaux18 Patients were selected by applying the International Headache Society criteria; these were used to define and differentiate tension-type pain from facial migraine without aura (Tables I and II) and from other less common types of facial neuralgia. Tension-type facial pain and facial migraine become more difficult to distinguish from each other when pain frequency increases.Reference Silberstein, Lipton, Solomon and Mathew19 Some patients with severe exacerbation of tension-type facial pain experience a migrainous attack, suggesting an overlap between the two conditions.Reference Solomon, Lipton and Newman20 Migraine with aura was much easier to distinguish from tension-type pain than migraine without aura.
The recruitment inclusion and exclusion criteria for entry into the cohort are listed in Table III. Only patients aged between 16 and 65 years were recruited. A standard patient history was taken, as shown in Table IV.
Cohort inclusion and exclusion criteria

CT = computed tomography; CNS = central nervous system
Facial pain patients: structured clinical interview and follow up

BMI = body mass index; CT = computed tomography
Basic patient data were collected from patients, including their state identity number (the unique identifier number provided by the Maltese government for every individual), age, sex, address, contact number, date seen and length of follow up in months. The main site of facial pain (unilateral, bilateral, alternating, right or left, frontal, peri-orbital, temporal, occipital or cheeks), its quality, duration and frequency was recorded. Exacerbating factors such as light, noise or exercise were noted, as was a personal history or family history of migraine.
Pregnant women, and patients with facial trauma or with pain caused by changes in ambient pressure (such as flying or diving), were excluded. Patients with temporomandibular dysfunction with clicking, tenderness of the temporomandibular joint or dental pain related to thermal sensitivity or percussion of the teeth were excluded.
Any symptoms that have been implicated in the diagnosis of rhinosinusitis, such as nasal obstruction, postnasal drip, rhinorrhoea, hyposmia, cough, fever, halitosis, toothache, fatigue or ear pressure, were recorded. Nasal atopy, whether intermittent or persistent, and whether supported by positive skin tests or not, was also recorded. The presence of rhinitis, or other significant respiratory or systemic disease, was recorded; this is because an association of headaches with asthma, rhinitis or chronic bronchitis has been described.Reference Aamodt, Stovner, Langammer, Hagen and Zwart21 The presence of atopy, especially if the patient had positive skin tests, was also recorded.
Exposure to tobacco smoke, whether active or passive, was recorded. A history of systemic illness such as hepatic, renal or pulmonary disease was noted.
Any prior surgical treatment was documented, and only patients whose sinus surgery pre-dated the study by two years were allowed to participate. Patients whose facial pain was accompanied by a tension headache were allowed to participate in the study. Patients with mixed tension-type pain with migraine were included in the study as long as they did not have more than one episode of migraine per month, in accordance with criteria established by previous studies on tension headache.Reference Jensen and Hindberg22–Reference Bendtsen and Mellerup24 Patients with more frequent migraine were excluded because they have been shown to have variations in blood serotonin levels.Reference Ribeiro, Cotrim, Morgadinho, Ramos, Santos and de Macedo Tdos25 Such variations could affect the outcome of serotonin estimation carried out as part of this study on a selected group of patients with mid-facial pain; however, these results will not be reported in this paper.
Patients with a history of psychiatric illness or those on any antidepressant, antipsychotic or hypnotic treatment were excluded as such individuals are suspected to have dysfunctional serotonergic pathways. Indeed, headaches have been associated with depression.Reference Delgado26, Reference Yucel, Kora, Ozyalcin, Alçalar, Ozdemir and Yücel27
Individuals with medication overuse headaches were excluded because they could constitute a particular group that is difficult to treat and whose medication may have altered serotonin reuptake activity. Patients with a history of substance or alcohol abuse were excluded for the same reasons.
Treatment regimes
As all patients had chronic pain (more than 15 pain days per month), prophylactic treatment was indicated. For mid-facial pain, 10 mg amitriptyline at night was prescribed for eight weeks. A second eight-week course was prescribed if the patient did not respond to the initial course of treatment. Patients who relapsed were continued on this medication for up to one year. Further relapses were treated with carbamazepine. Subsequent to this study, we now use pregabalin.
Prophylaxis for patients with facial migraine consisted of 10 mg amitriptyline or 20 mg propranolol daily for eight weeks. Triptans, being more expensive, were prescribed for breakthrough episodes or for more severe pain. Non-steroidal anti-inflammatory drugs were given as an alternative to triptans to patients not wishing to have prophylactic treatment. Cost was an important consideration because patients had to fund their own treatment.
Treatment success was defined as a greater than 50 per cent reduction in pain frequency, intensity or both, as laid out in the Cochrane guidelines.Reference Saarto and Wiffen28
Follow up
Patients recruited into the cohort were followed up for three years, from June 2010 to May 2013.
Details of facial pain frequency and severity, medical treatment, any changes to treatment, and the results of follow up were recorded. The type and dose of any medication prescribed, together with outcome and addition to or change in medication, were noted. If facial pain recurred after treatment, the elapsed time between the course of treatment and recurrence was recorded. Clinical success was defined as a greater than 50 per cent decrease in pain frequency, pain intensity or both. Outcome in the cohort follow up at 36 months was broadly classified according to International Headache Society guidelines as remaining chronic, becoming episodic (1–14 days of pain per month) or having resolved.
Following the initial interview, all patients were reviewed after four weeks. Patients were then contacted for telephone interview at least once per year during follow up to ascertain the progression of facial pain. Symptomatic patients could obtain a same-day appointment at the out-patient clinic if required. Another two attempts were made to contact those who did not respond to the telephone call. Failing this, a letter was sent to their last known address in an attempt to elicit a response.
Statistics
Statistical analyses were conducted using SPSS Statistics software version 16.0 (Chicago, Illinois, USA). Results are presented as mean ± standard deviation. Comparisons between patients with mid-facial tension-type pain and those with facial migraine were made using a chi-square test. When calculating treatment efficacy, the cut-off point between success and failure was a greater than 50 per cent improvement in pain scores. The dichotomous analysis was performed using the chi-square test. Statistical significance was set at p < 0.05.
Results
The mean age of 240 patients with chronic facial pain was 37.7 ± 12.4 years. Most were women (172, or 72 per cent).
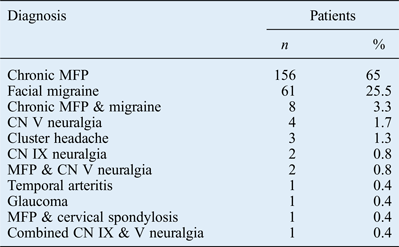
The great majority (156) of these patients were found to have chronic mid-facial segmental tension-type pain. Sixty-one patients had facial migraine, of which 16 had migraine with aura. Eight individuals had a combination of mid-facial pain and migraine. The remaining 15 had cranial nerve neuralgias, cluster headaches and temporal arteritis (Table V). Most of the results relate to the two main patient groups.
Chronic facial pain causes

MFP = mid-facial pain; CN = cranial nerve
The BMI, level of education and occupation of these patients were compared to national statistics. The national census of 2005 recorded the Maltese population as 404 962.29 Between the ages of 16 and 65 years, 49.5 per cent of the Maltese population were women, while 72 per cent of the facial pain cohort were women.
Body mass index
National statistical data collected by the Health Department National Survey of 2008 recorded the mean BMI for the Maltese adult population as 26.5 kg/m2,30 while the mean BMI for 240 patients with chronic facial pain was 25.4 ± 4.2 kg/m2.
Education level
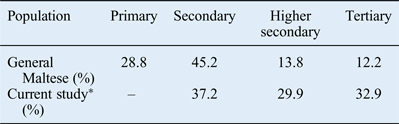
Table VI shows the proportion of the population with a primary, secondary, higher secondary and tertiary level of education. In general, facial pain patients had a higher level of education than the general population. The fact that these patients attended a private clinic may be relevant to these findings.
Education level in general maltese and study populations

*n = 240
Occupation
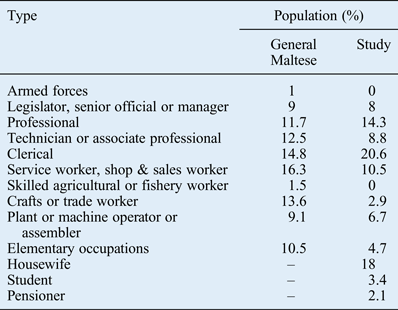
The national census of 2005 classified occupations into categories 1 to 10. Housewives, students and pensioners were missing from the national classification as they were not considered to be gainfully employed. In this study, these groups were given the code numbers 11, 12 and 13 respectively. Table VII gives the relative percentages of the different occupations in the chronic facial pain patient group, together with the national percentage for each category.
Occupation type in general maltese and study populations

Patients with chronic facial pain consulting a private specialist were likely to be better educated and have a better job than the general population, with a slightly lower BMI than the national average.
Chronic mid-facial pain
Of the 156 patients with chronic mid-facial tension-type pain, 111 (71 per cent) were women, with a mean age of 37 ± 11.6 years (Table VIII). The 45 men were slightly older, with a mean age of 40 ± 14 years. The mean age of all mid-facial pain patients was 37.8 ± 12.4 years. Dizziness was a common accompanying symptom to facial pain, occurring in 37 out of 156 (23.7 per cent) patients and usually resolving within a week of commencing treatment.
Demographic data for mid-facial pain and facial migraine patients

*n = 156; †n = 61. SD = standard deviation; MFP = mid-facial pain
Patients with mid-facial pain were treated with an 8-week course of 10 mg amitriptyline per day and followed up for 36 months. If there was no response after two weeks, the dose was increased to 20 mg, but this was unusual. In 24 out of 156 patients (15.3 per cent), pain recurred within 3 months. Even when the pain was not as severe as it had previously been, these individuals were offered a second course of amitriptyline.
Patients who retained their pre-treatment pattern of pain were classified as having ‘chronic’ pain. In patients whose pain decreased in frequency and severity so that they recorded less than one pain day a month, the pain was considered to be ‘resolved’. Patients with 1–14 pain days per month at 36 months were labelled as having ‘episodic’ pain.
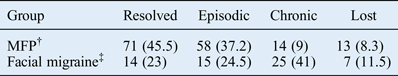
Facial pain resolved in almost half of the mid-facial pain patients (45.5 per cent), while in a third it changed to an episodic pattern (37.2 per cent) with infrequent bouts of pain (Table IX). In 14 patients (9 per cent), chronic pain was retained, that is, they had more than 15 pain days per month. The remaining 8.3 per cent were lost to follow up.
Outcome in mid-facial pain and facial migraine patients*

Data represent patient numbers and percentages.
* At 36-month follow up. †n = 156; ‡n = 61. MFP = mid-facial pain
For those patients in the episodic and chronic groups whose pain returned, it did so after 10.5 ± 10 months following their course of amitriptyline.
Facial migraine
A total of 61 patients had facial migraine: 41 (67.2 per cent) were women (mean age 35 ± 10.9 years) and 20 were men (mean age 38.5 ± 10.9 years) (Table VIII). The mean age of all facial migraine patients was 36.1 ± 10.9 years. Dizziness was described in only four (6.5 per cent) facial migraine patients.
Patients were treated prophylactically with 10 mg amitriptyline daily for eight weeks (n = 16) or propranolol 20 mg daily for eight weeks (n = 21). One patient was treated with both. Patients who did not accept prophylactic treatment received triptans (sumatriptan or zolmitriptan, n = 8) or non-steroidal anti-inflammatory drugs (n = 13) on an ‘as required’ basis. One took paracetamol with codeine and one did not receive any treatment. The choice of treatment was influenced by patient preference and cost.
Patients were followed up for 36 months. On evaluation at 36 months, the largest proportion of facial migraine patients (41 per cent) had unchanged chronic symptoms. In 23 per cent, their pain had ‘resolved’ to less than one episode per month. In one-third, the pain frequency was reduced to ‘episodic’, i.e. occurring between 1 and 14 days per month (Table IX). Overall, in patients whose facial migraine did not resolve (‘chronic’ and ‘episodic’ groups together), the original pain pattern took a mean of 8.7 ± 10 months to return after treatment. In 18 patients (30 per cent), pain returned within 3 months of stopping treatment.
In the subgroup of patients receiving prophylactic propranolol (n = 21), the previous pain pattern returned after 13.3 ± 12.3 months; in those receiving prophylactic amitriptyline (n = 16), pain returned after 18.4 ± 16.1 months; and in patients receiving triptans (n = 8), the previous pain pattern returned after 19.3 ± 17.9 months. The shortest interval before return to the previous pain pattern was seen in patients receiving non-steroidal anti-inflammatory drugs ‘as required’ (n = 13): their pain returned after 9.7 ± 13.3 months.
Mid-facial pain versus facial migraine
A comparison of outcomes revealed that patients with mid-facial pain and facial migraine had similar dropout rates on follow up (chi-square test, p = 0.69 (not significant)), and similar rates of progression from chronic to episodic pain (chi-square test, p = 0.27 (not significant)). However, mid-facial pain patients were much more likely to experience resolution of their pain compared to patients with migraine (p = 0.05), and facial migraine was significantly more likely to remain chronic (p = 0.00001).
The most common sites of pain described by patients with mid-facial pain were the nasion and frontal regions; most had a combination of sites, with 384 sites described by 156 patients. In facial migraine, 141 sites were described by 61 patients, with the peri-orbital and frontal regions being most commonly involved (Table X). In mid-facial pain, the pain was typically bilateral; in migraine, it was bilateral in half of patients (26, or 48 per cent), and unilateral or alternating in the other half.
Sites of chronic facial pain*

Data represent patient numbers and percentages.
* Patients generally had more than one site involved at the same time. †n = 156; ‡n = 61. MFP = mid-facial pain
In mid-facial pain, the pain was characteristically pressing in 122 patients (78 per cent) and aching in 30 patients (19 per cent). In facial migraine, the pain was described as throbbing in 34 patients (56 per cent), as pressing in 17 (28 per cent), and as aching, stabbing, boring, pinching or sharp in the rest. Thus, the description of pain in mid-facial pain was more uniform.
Photophobia and nausea were much more common in facial migraine (Table XI). Most facial migraine patients had never been properly diagnosed and had a low awareness of this condition. As a consequence, they typically denied a history of migraine and attributed their previous symptoms to sinusitis. However, when asked about migraine in their families, the rates turned out to be high.
Additional medical history and symptoms for mid-facial pain and facial migraine patients

Data represent patient numbers and percentages. *n = 156; †n = 61. MFP = mid-facial pain
The incidence of rhinitis, and rates of positive skin tests, exposure to cigarette smoke or systemic illness such as asthma were similar in the mid-facial pain and facial migraine groups (Table XII).
Rhinitis, positive skin tests, smoke exposure and systemic illness in mid-facial pain and facial migraine patients

Data represent patient numbers and percentages. *For example, asthma. †n = 156; ‡n = 61. Exp = exposure; syst = systemic; MFP = mid-facial pain
Mid-facial pain and facial migraine
In 8 patients with a combination of mid-facial pain and migraine, the pain pattern reappeared after a mean of 12.6 ± 4.5 months after treatment with amitriptyline.
Neuralgia and cluster headache
Most patients with trigeminal or glossopharyngeal neuralgia responded well to carbamazepine, while those with cluster headaches responded to triptans or prophylactic low-dose propranolol.
Discussion
This cohort represents a sample of patients who either self-referred or were referred by their general practitioner to a community-based otolaryngologist, and may therefore not be representative of patients in the whole population with chronic facial pain. It is also likely that a broader spectrum of pain types would be encountered in an otolaryngological practice than in a tertiary referral neurological centre. The age and gender distribution in patients with facial pain in Malta was very similar to that in a group of 409 patients with facial pain presenting to a rhinology clinic in the UK, where the mean age was 37.6 years and 68.6 per cent were female.Reference Daudia and Jones31
The patients in this cohort had a similar mean BMI to that of the general population, but were better educated. The fact that the patients attended a private practice may be relevant to these findings. In previous studies, patients with chronic tension headache were low academic achieversReference Boardman, Thomas, Croft and Millson32 and had lower incomesReference Schwartz, Stewart, Simon and Lipton33 than the general population. In men, tension-type headaches were associated with sedentary occupations.Reference Rasmussen34
Patient dropout rates varied between 8 and 11 per cent. Most tension-type pain was described as of mild-to-moderate intensity; therefore, not all patients may have thought it worth the time and effort to attend follow up. Most individuals were already taking analgesics on an ‘as required’ basis and there was some resistance to changing to prophylactic treatment. Therefore, patient education was important to explain the aetiology of their condition. It was encouraging that in patients with mid-facial pain, pain frequency or severity significantly dropped within two weeks of starting low-dose amitriptyline.Reference Agius, Jones and Muscat35
A 10-year follow-up study of 62 Danish patients with chronic tension-type headache showed that 45 per cent went into remission. A reduction in headache frequency led to the development of an episodic pattern from a chronic pattern of headaches.Reference Lyngberg, Rasmussen, Jorgensen and Jensen36
The same findings were reported in another Danish study of 740 individuals with headache followed up for 2 years.Reference Lyngberg, Rasmussen, Jorgensen and Jensen37 Similar data were also recorded in the USA.Reference Spierings and Mutsaerts38 However, patients with coexisting chronic tension-type headache and migraine were more likely to continue having frequent headaches. Similar observations for facial pain were recorded in this study (Table IX). Clinical improvement (‘resolved’ and ‘episodic’ outcomes taken together) was much higher in mid-facial pain patients (82.7 per cent) than in facial migraine patients (51 per cent).
The treatment of mid-facial pain patients was uniform and the outcome more favourable. Facial migraine patients treated with non-steroidal anti-inflammatory drugs ‘as required’ were quick to return to their previous pain pattern, while prophylactic low-dose amitriptyline or triptans seemed to break the pain cycle and give longer-lasting relief.
Because time to recurrence of the original pain pattern was, in general, similar in both mid-facial pain and facial migraine patients, a common underlying cause of these conditions is hypothesised. Medication may simply reduce the sensitivity of the nociceptive pathway for a variable period of time, probably at the level of the synaptic relay in the trigeminal subnucleus caudalis.
• In a cohort of chronic facial pain patients, 72 per cent were women in their fourth decade
• Patients had a slightly lower mean body mass index, and better educations and jobs, than the general population
• Commonest causes of pain were tension-type mid-facial pain and facial migraine
• Patients with tension-type mid-facial pain responded to low-dose amitriptyline
• Patients with facial migraine responded to low-dose amitriptyline and triptans
The pain resolved in nearly half of the individuals with mid-facial pain, and in a third it became episodic. We do not know whether the medication altered the natural course of the condition as no long-term study of untreated patients with this condition has been performed. However, these findings are similar to those obtained for tension-type headache patients.Reference Lance and Anthony39
Photophobia has been reported in 49–95 per cent of patients with migraine.Reference Rasmussen and Olesen40, Reference Olesen41 In this series, the incidence was 74 per cent in facial migraine patients, which is consistent with the other studies (Table XI).
Nausea has been reported as present in 90 per cent of patients with migraine, with vomiting present in 50 per cent.Reference Rasmussen and Olesen40, Reference Olesen41 The rates of these symptoms in facial migraine patients in this study were similar (Table XI).
The rates of rhinitis, positive skin test results, cigarette smoke exposure or systemic illness such as asthma were similar in the mid-facial pain and facial migraine groups, and did not differ from those in the general Maltese population.Reference Agius, Cordina and Calleja42 This contrasts with findings from a Norwegian study, which showed an association of asthma, rhinitis and chronic bronchitis with migrainous and non-migrainous headaches.Reference Aamodt, Stovner, Langammer, Hagen and Zwart21
Education is important to encourage patients to keep analgesic doses as low as possible. This will help to prevent the development of medication overuse headaches, especially those resulting from migraine medication overuse.Reference Bendtsen, Birk, Kasch, Aegidius, Sørensen and Thomsen43
During the three years follow up, two of the patients became pregnant; their facial pain significantly improved during pregnancy. In one female patient with facial migraine, thyroid nodules were incidentally discovered and she was eventually diagnosed with medullary carcinoma of the thyroid.
Conclusion
In this cohort of patients with chronic facial pain, 72 per cent were women in their fourth decade of life. As a group, the cohort had a slightly lower than average BMI, better educational attainment and better jobs compared with the general population.
The commonest causes of pain were tension-type mid-facial pain and facial migraine. Patients in the first group frequently responded to an 8-week course of low-dose amitriptyline, with nearly half of the patients being pain free at 36 months and one-third suffering less severe and less frequent episodes of pain. For patients with facial migraine, the most effective long-term treatment was low-dose amitriptyline and triptans.
Acknowledgements
This work was partly funded by the Malta Government Scholarship Scheme and the dean's fund from the Faculty of Medicine and Surgery, University of Malta. Dr Neville Calleja, the Head of Department of Medical Statistics, Department of Health, Malta, kindly assisted with the clinical analyses. The authors are especially grateful to all patients who kindly consented to taking part in this study.