Introduction
Nasal obstruction can be caused by structural nasal deformities or be due to inflammatory processes affecting the nasal mucosa.Reference Teitelbaum and Barrett1 Structural causes of nasal obstruction include deviation of septal cartilage and/or the nasal bones, turbinate enlargement or deformities of the alar cartilage.Reference Teitelbaum and Barrett1 Septal deviation is a common cause of chronic upper airway nasal obstruction and septoplasty is commonly performed to relieve symptomatic nasal obstruction secondary to septal deviation.Reference Balai, Jolly, Bhamra, Osborne and Barraclough2 In the National Health Service (NHS) in England, approximately 17,000 septoplasties are performed annually,Reference Balai, Jolly, Bhamra, Osborne and Barraclough2 while in the United States, approximately 250,000 septoplasties are performed annually.Reference Bhattacharyya3
Septoplasty provides functional and objective benefits for patients with chronic nasal obstruction secondary to structural deformities by improving nasal airflow.Reference Moore and Eccles4–Reference Pedersen, Schiöler, Finjan, Davidsson, Sunnergren and Holmberg6 However, patient selection for septoplasty remains undefined. The diagnosis of nasal obstruction is predominantly based on clinical history from patients and clinical examination of the nasal valve, lateral nasal wall, septum and inferior turbinate.Reference Clark, Del Signore, Raithatha and Senior7 Subjective patient-reported symptom scoring tools such as the Nasal Obstruction Symptom Evaluation (NOSE)Reference Stewart, Witsell, Smith, Weaver, Yueh and Hannley8 and Sino-Nasal Outcome Test (SNOT-20) scoresReference Hopkins, Gillett, Slack, Lund and Browne9 are available but used infrequently in clinical settings to assess the severity of nasal obstruction.
Objective nasal patency measuring tools such as acoustic rhinometry, rhinomanometry, rhinospirometry and peak nasal inspiratory flow (PNIF) are also available to assess the degree of nasal obstruction. Acoustic rhinometry measures the cross-sectional areas and nasal volumes using reflected sound waves from the nasal cavities to establish the degree of nasal patency.Reference Roithmann, Cole, Chapnik, Shpirer, Hoffstein and Zamel10 Valleys in acoustic rhinometry graphs represent reductions in cross-sectional area at specific distances from the interface and these valleys represent a defined anatomic structure.Reference Corey, Nalbone and Ng11 Cross-sectional areas (CSAs) are dips on acoustic rhinometry. CSA1 corresponds to the area of the nasal valve, CSA 2 to the inferior and/or medial nasal concha and CSA3 corresponds to the medial-posterior end of the medial nasal concha. Rhinomanometry measures trans-nasal airflow and pressure to establish nasal airway resistance during inspiration.Reference Spataro and Most12 Rhinospirometry measures the difference in volume, average flow, peak flow and partitioning of airflow between the nasal passages.13 The reference pressures of 75 and 150 Pascal (Pa) are often used to calculate the expiratory and inspiratory nasal airway resistances. In rhinospirometry, the nasal partitioning ratio is a measure of asymmetry of airflow through the nasal cavities that ranges from -1 (complete left nostril obstruction) to +1 (complete right nostril obstruction), with 0 indicating symmetrical airflow.Reference Roblin and Eccles14 PNIF measures maximal airflow during forced nasal inspiration through both nostrils.Reference Spataro and Most12
Despite evidence demonstrating objective improvement in measures of nasal patency and airflow following septoplasty,Reference Moore and Eccles4 the clinical applicability of objective nasal patency measures using acoustic rhinometry, PNIF, rhinomanometry and rhinospirometry for selecting patients with structural nasal obstruction for septoplasty remains undefined.
This systematic review aims to explore the currently available evidence on the relationship between clinical nasal examination findings in structural nasal obstructions and objective nasal patency measures using acoustic rhinometry, PNIF, rhinomanometry and rhinospirometry. This will allow clinicians to decide if objective nasal patency measures can be used alongside clinical examination findings to aid patient selection for septoplasty.
Methods
Ethical consideration
No patient-identifiable data are included. This study is a systematic review of previously published articles. No ethical approval was required.
Data search strategy
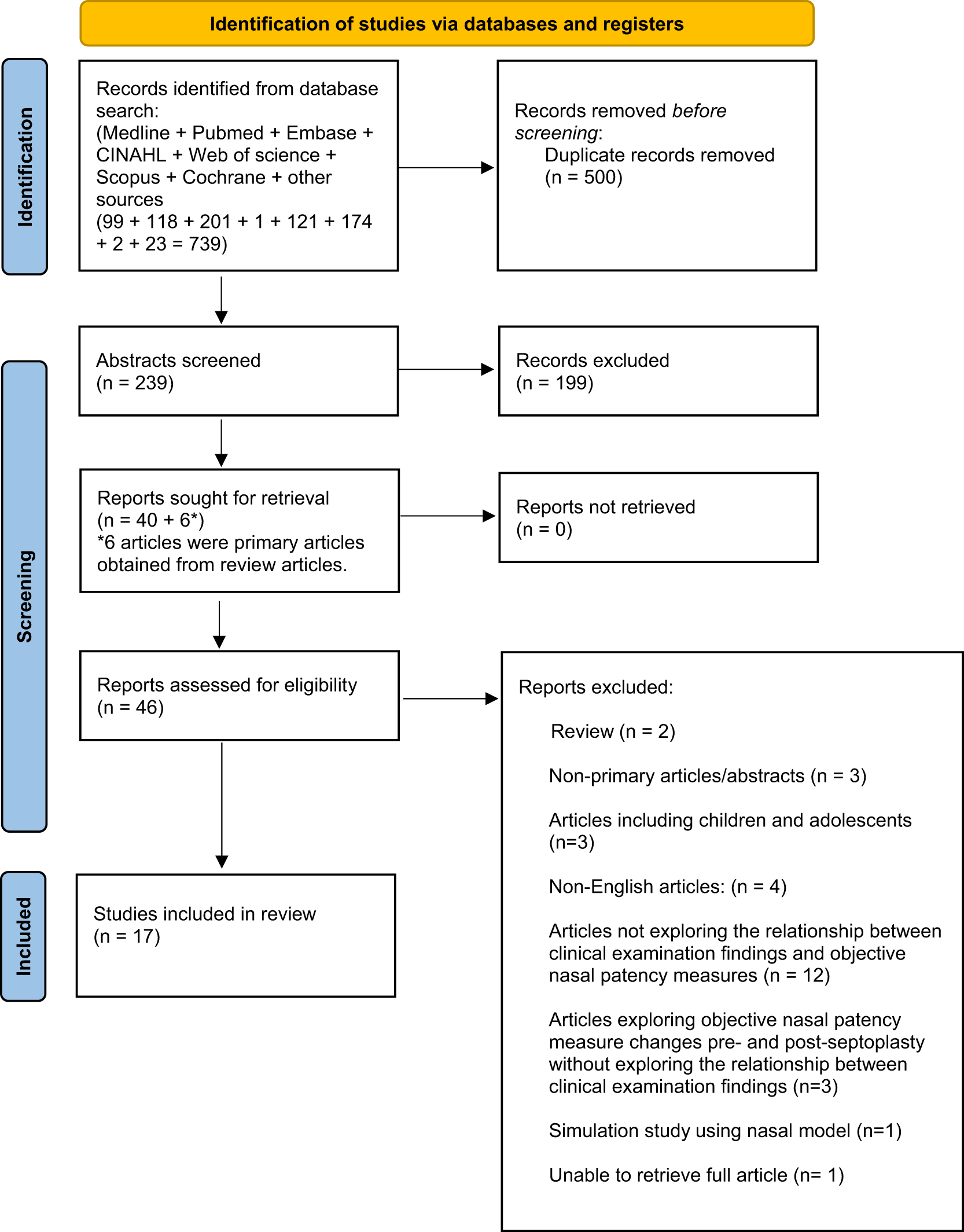
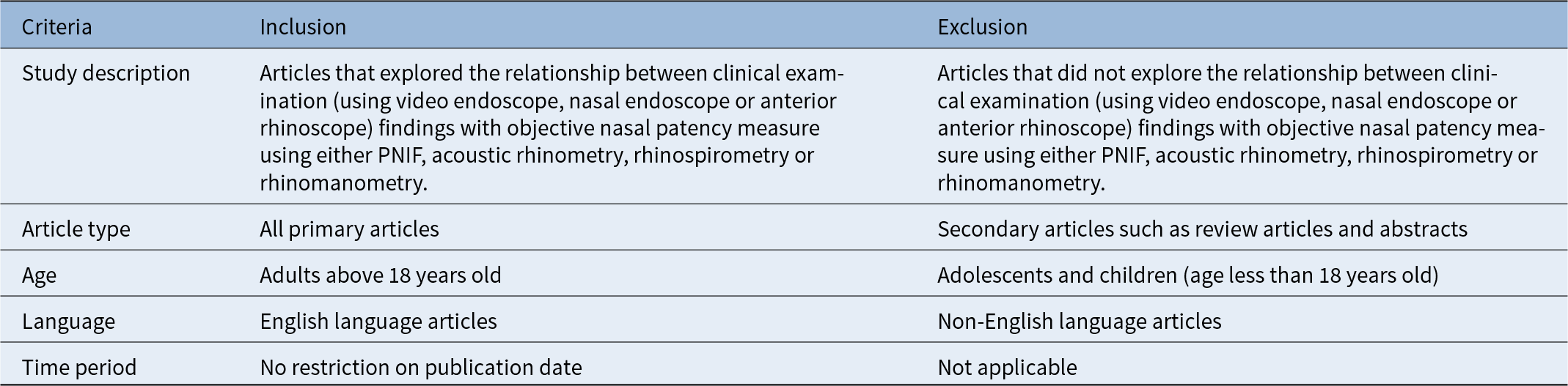
This systematic review was registered with the International Prospective Register of Systematic Reviews (PROSPERO) (Registration number: CRD 42023417330).15 A systematic literature search was performed using Medical Subject Heading (MeSH) terms and other keywords as outlined by the Preferred Reporting Items for Systematic Reviews and Meta‐Analyses (PRISMA) 2020 statement.16 Pubmed (US National Library of Medicine), Medline, Embase, SCOPUS, Web of Science, Cumulated Index to Nursing and Allied Health Literature (CINAHL), Cochrane Library and Google Scholar databases were used. The final literature search was performed on 17/05/2024. The MeSH terms and search strategy for this systematic review are provided in Appendix 1. The inclusion and exclusion criteria are outlined in Table 1. The Oxford Centre for Evidence-Based Medicine guidelines were used to establish the level of evidence of scientific articles.Reference Howick, Chalmers, Glasziou, Greenhalgh, Heneghan and Liberati17 The workflow for the systematic review is outlined in Figure 1.
Workflow of article screening for final narrative synthesis.
Inclusion and exclusion criteria for systematic review
Following data synthesis, findings from the literature are summarised according to the type of objective nasal patency measures. This allows comparison of evidence from the literature based on the type of objective nasal patency measure and to establish how individual objective measures correlate with clinical examination findings. The strength of correlation reported in each study is classified as described by Hensch and EvansReference Hensch and Evans18 as “very weak correlation” (correlation coefficient of 0.00–0.19), “weak correlation” (0.20–0.39), “moderate correlation” (0.40–0.59), “strong correlation” (0.60–0.79) and “very strong correlation” (0.80–1.0). Cohen k statistics were also used to describe the agreement between the different outcome measures. A kappa score of less than 0 indicates no agreement, 0.01–0.20 slight agreement, 0.21–0.40 fair agreement, 0.41–0.60 moderate agreement, 0.61–0.80 substantial agreement and 0.81–0.99 almost perfect agreement.Reference Fyrmpas, Kyrmizakis, Vital and Constantinidis19
Results
A total of 17 articles met the inclusion criteria (Table 1) and were included in the review (Tables 2–5).
Studies investigating the correlation between clinical examination findings and acoustic rhinometry
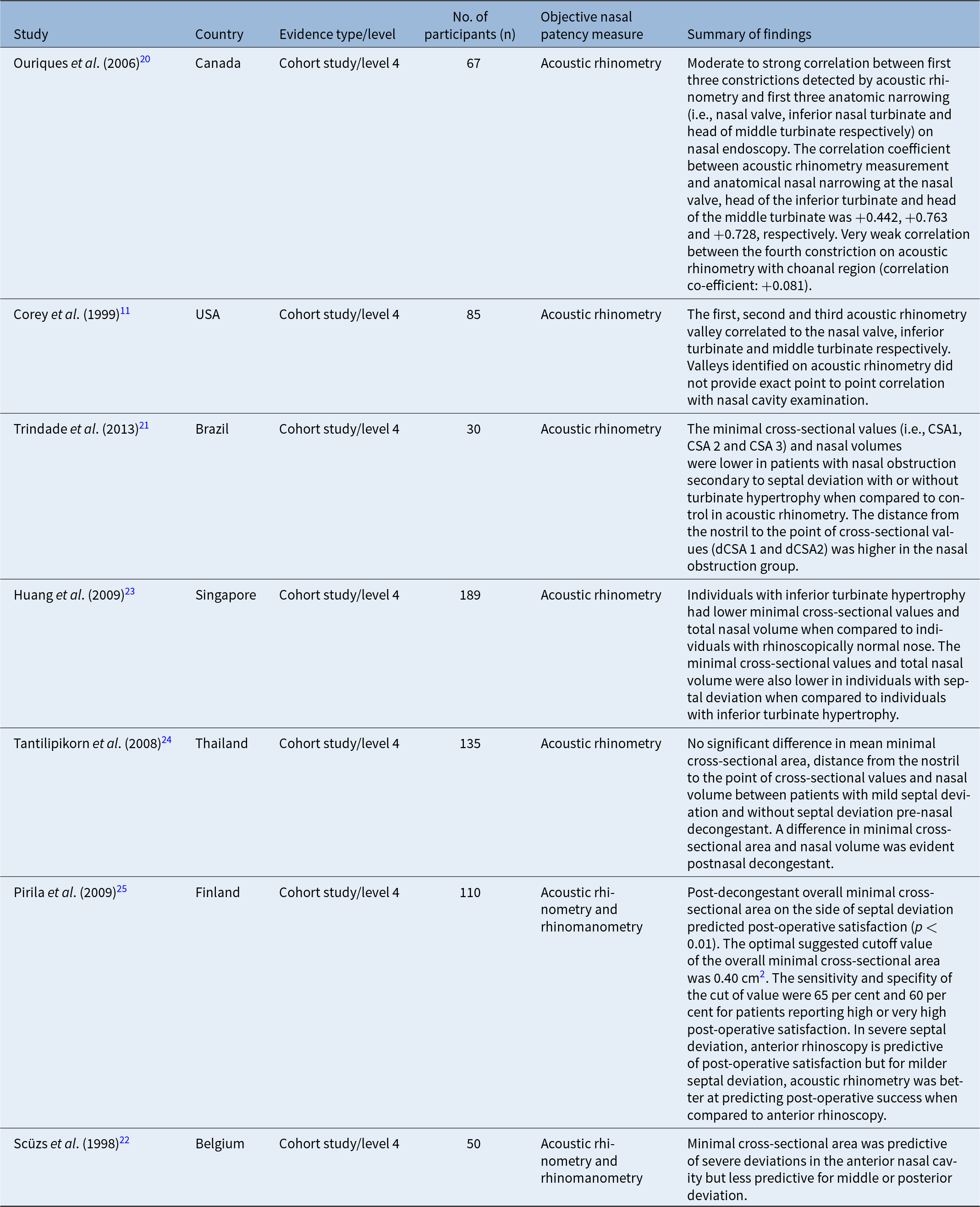
Relationship between clinical examination findings and acoustic rhinometry
Studies exploring the relationship between clinical examination findings and acoustic rhinometry were level 4 cohort studies/case series (Table 2). Positive relationships between clinical examination findings and acoustic rhinometry assessment were observed in some studiesReference Corey, Nalbone and Ng11, Reference Ouriques, Carlini, Fujita, Pignatari and Weckx20–Reference Huang, Wang, Zhang, Dong and Yeoh23 (Table 2). Ouriques et al. compared and correlated areas of anatomical nasal narrowing on fibreoptic nasal endoscopy with acoustic rhinometry measurements in individuals without nasal complaints. A moderate to strong correlation was identified among the first three constrictions detected on acoustic rhinomanometry and the first three parts of anatomic narrowing (i.e., nasal valve, head of the inferior turbinate and head of the middle turbinate) on nasal endoscopy. A very weak correlation was evident between the fourth constriction measurement on acoustic rhinometry and the fourth anatomic constriction which is the posterior choanal regionReference Ouriques, Carlini, Fujita, Pignatari and Weckx20 (Table 2). Similarly, Corey et al. highlighted that the first valley on acoustic rhinometry correlated with the nasal valve anatomy, the second valley corresponded to the anterior aspect of the inferior turbinate and the third valley correlated to the anterior aspect of the middle turbinate. However, these valley measurements on acoustic rhinometry failed to provide an exact point-to-point correlation with the nasal cavity on clinical examination (Table 2).Reference Corey, Nalbone and Ng11
Studies investigating the correlation between clinical examination findings and rhinomanometry
Other studies also reported findings whereby the minimal cross-sectional area values and nasal volumes were lower in patients with nasal obstruction when compared to healthy controls suggesting that most patients with structural nasal obstruction had impairment in acoustic rhinometry assessment due to anatomical differencesReference Trindade, Conegliam, Trindade, Dias and Sampaio-Teixeira21–Reference Huang, Wang, Zhang, Dong and Yeoh23 (Table 2). Trindade et al. highlighted that the minimal cross-sectional values were lower in patients with septal deviation when compared to healthy control whereas the distance from the nostril to the point of cross-sectional values was higher.Reference Trindade, Conegliam, Trindade, Dias and Sampaio-Teixeira21 Scüzs et al. also reported that the minimal cross-sectional area is lower in patients with septal deviation when compared to the control cohort although the minimal cross-sectional area was more sensitive in identifying severe deviations in the anterior nasal cavity when compared to the middle or posterior septal deviation.Reference Szücs and Clement22
A study by Tantilipikorn et al. explored the relationship between acoustic rhinometry measurements and clinical examination findings using anterior rhinoscopy in asymptomatic adults with mild septal deviation or without septal deviation. In this study, no difference in pre-decongestant minimal cross-sectional area, nasal volume and distance from nostril to the point of cross-sectional values were observed between patients with mild septal deviation and patients without septal deviation. However, a difference in post-decongestant minimal cross-sectional area and nasal volume was observed in these groups of patientsReference Tantilipikorn, Jareoncharsri, Voraprayoon, Bunnag and Clement24 (Table 2).
Pirila et al. assessed the degree of septal deviation using anterior rhinoscopy and classified deviations as “very severe” if total or sub-total obstruction was noted, “severe” if more than 50 per cent obstruction was noted and “moderate” or “mild” if less than 50 per cent of the airway was obstructed by the deviation. Post-operative satisfaction was expressed by patients as “very high”, “high”, “moderate”, or “low” one year after septoplasty. Post-decongestion overall minimal cross-sectional area of the deviated septum on acoustic rhinometry performed pre-operatively had the highest impact in identifying patients with high or very high post-operative satisfaction. With anterior rhinoscopy, the optimum cutoff value to achieve high post-operative satisfaction is between “severe” and “moderate” septal deviation. Pirila et al. concluded that, for patients with very severe septal deviation, anterior rhinoscopy alone was sufficient to screen for post-operative satisfaction but for patients with milder septal deviation, acoustic rhinometry was a better screening tool to assess post-operative satisfaction when compared to anterior rhinoscopyReference Pirilä and Tikanto25 (Table 2).
Relationship between clinical examination findings and rhinomanometry
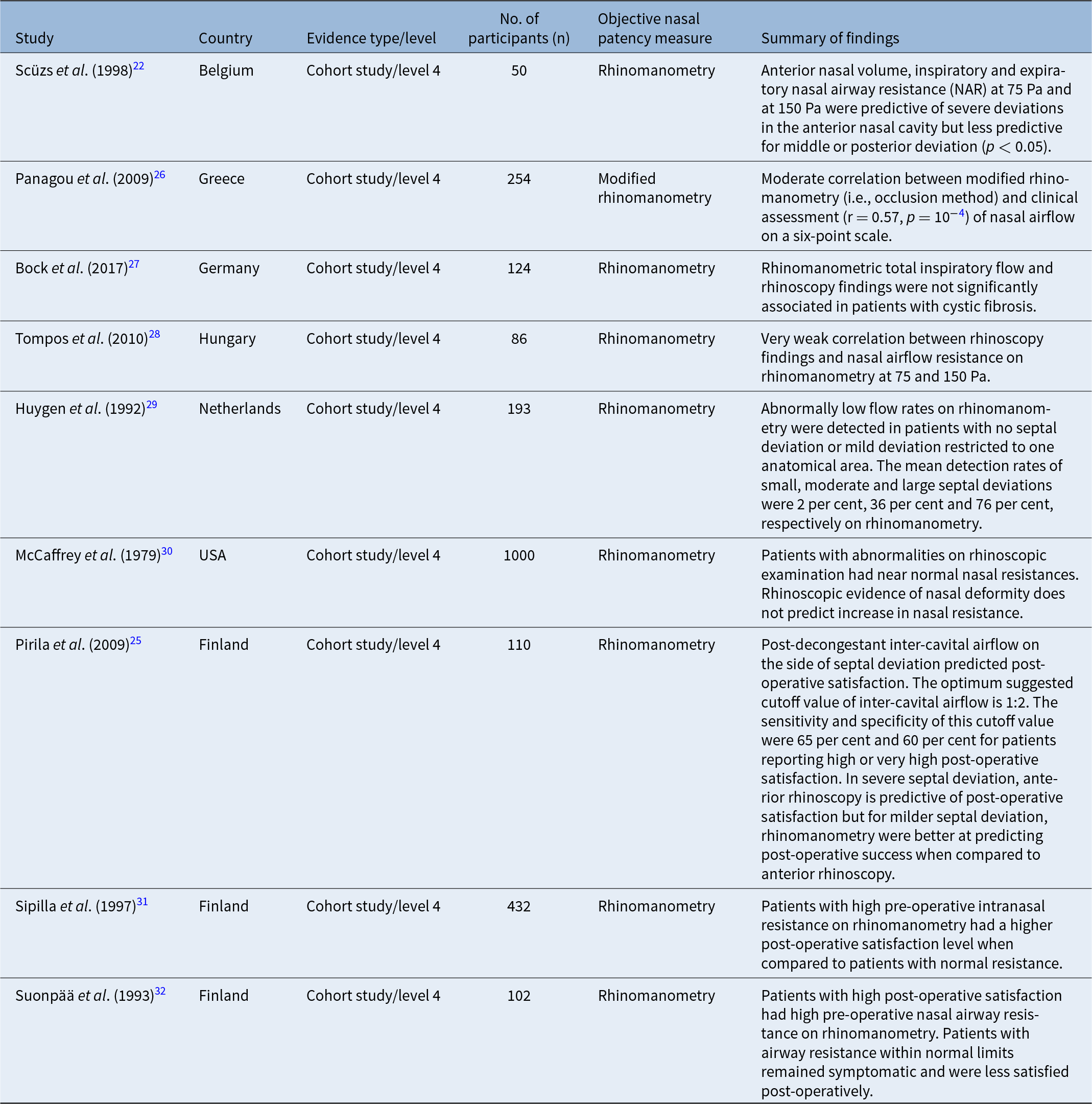
Studies exploring the relationship between clinical examination findings and rhinomanometry are shown in Table 3. Scüzs et al. highlighted that anterior nasal volume, inspiratory and expiratory nasal airway resistance (NAR) on rhinomanometry assessment were sensitive measurements to assess for severe deviation in the anterior nasal cavity. However, these measurements were less sensitive for middle and posterior septal deviation, limiting their role in assessing patients with middle or posterior septal deviation.Reference Szücs and Clement22 In this study, anterior deviation was defined as septal deviation less than 2.5 cm from the middle of columella, middle septal deviation between 2.5 cm and 4.5 cm from the middle of columella and posterior deviation between 4.5 cm and 8 cm from the middle columella. Septal deviation was classified as severe if the deviation occluded more than 50 per cent of the nasal cavity and moderate if it occluded less than 50 per cent of the nasal cavity on clinical examination.
Other evidence in the literature suggests a limited role for rhinomanometry in assessing nasal airway patencyReference Panagou, Loukides, Tsipra, Syrigou, Anastasakis and Kalogeropoulos26–Reference McCaffrey and Kern30 (Table 3). Panagou et al. reported a moderate correlation between modified rhinomanometry (i.e., occlusion method) and subjective clinician assessment of nasal airflow on a six-point scale.Reference Panagou, Loukides, Tsipra, Syrigou, Anastasakis and Kalogeropoulos26 In this study, each nostril was rated on a three-point scale (0 = no obstruction, 1= significant reduction of airflow compared to the contralateral side and 2 = nearly complete or complete obstruction of nasal airflow). The sum of score of each nostril provided the subjective clinical assessment score for nasal obstruction. Tompos et al. highlighted a very weak correlation between rhinoscopy findings and nasal airflow resistance on rhinomanometry.Reference Tompos, Garai, Zemplén and Gerlinger28 Huygen et al. reported abnormally low flow rates on rhinospirometry assessment for patients with no septal deviation or mild septal deviation restricted to one anatomical area, limiting the role of rhinomanometric evaluation in selecting patients for septoplasty. The mean detection rates of clinically diagnosed small, moderate and large septal deviations using rhinomanometry were 22 per cent, 36 per cent and 76 per cent, respectively.Reference Huygen, Klaassen, de Leeuw TJ and Wentges29
Pirila et al. highlighted that the pre-operative post-decongestant inter-cavital air flow ratio (i.e., the ratio between the flow on the deviated side and the wide side of the nasal cavity) is a strong predictor for post-operative satisfaction. With anterior rhinoscopy, the optimal cutoff value to predict post-operative satisfaction was between severe and moderate septal deviation. Pirila et al. concluded that, for patients with very severe septal deviation, anterior rhinoscopy was predictive of post-operative satisfaction but for patients with milder septal deviation, rhinomanometry was a useful tool for predicting post-operative satisfaction when compared to anterior rhinoscopy.Reference Pirilä and Tikanto25 Similarly, Sipilä et al. and Suonpää et al. also highlighted those patients with a deviated septum had a higher pre-operative nasal airway resistance on rhinomanometry when compared to the control cohort and pre-operative rhinomanometry assessment was predictive of post-operative satisfactionReference Sipilä and Suonpää31, Reference Suonpää, Sipilä and Laippala32 (Table 3).
Relationship between clinical examination findings and PNIF
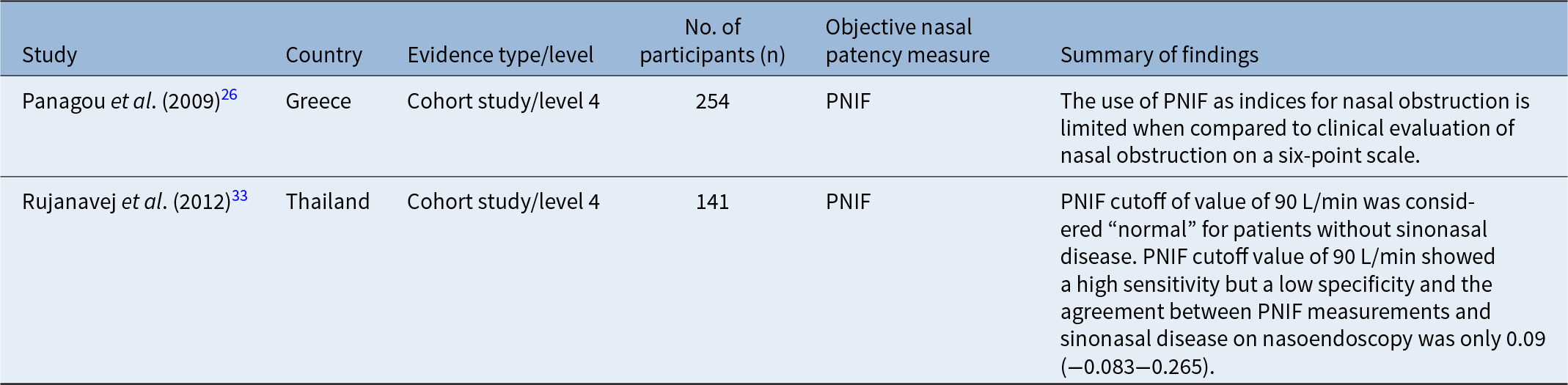
Evidence in the literature evaluating the relationship between clinical examination findings and PNIF is limited and is all level 4 cohort studies/case series (Table 4). Panagou et al. highlighted that the use of PNIF as an index of nasal patency measure is limited when compared to clinical evaluation of nasal obstruction.Reference Panagou, Loukides, Tsipra, Syrigou, Anastasakis and Kalogeropoulos26 In this study, the severity of nasal obstruction was evaluated subjectively by clinicians estimating nasal flow airflow using a six-point scale. Similarly, Rujanavej et al. highlighted that the correlation between PNIF measurements and sinonasal disease identified on nasal endoscopy was very weak (Table 4). In this study, PNIF at a cutoff value of 90 L/min showed high sensitivity but a low specificity when compared to anterior rhinomanometry. The high sensitivity of PNIF at a cutoff value of 90 L/min may aid clinicians in identifying patients with sinonasal disease but its low specificity may result in difficulty in interpreting PNIF values in healthy asymptomatic individuals without sinonasal disease.Reference Rujanavej, Snidvongs, Chusakul and Aeumjaturapat33
Studies investigating the correlation between clinical examination findings and PNIF
Relationship between clinical examination findings and rhinospirometry
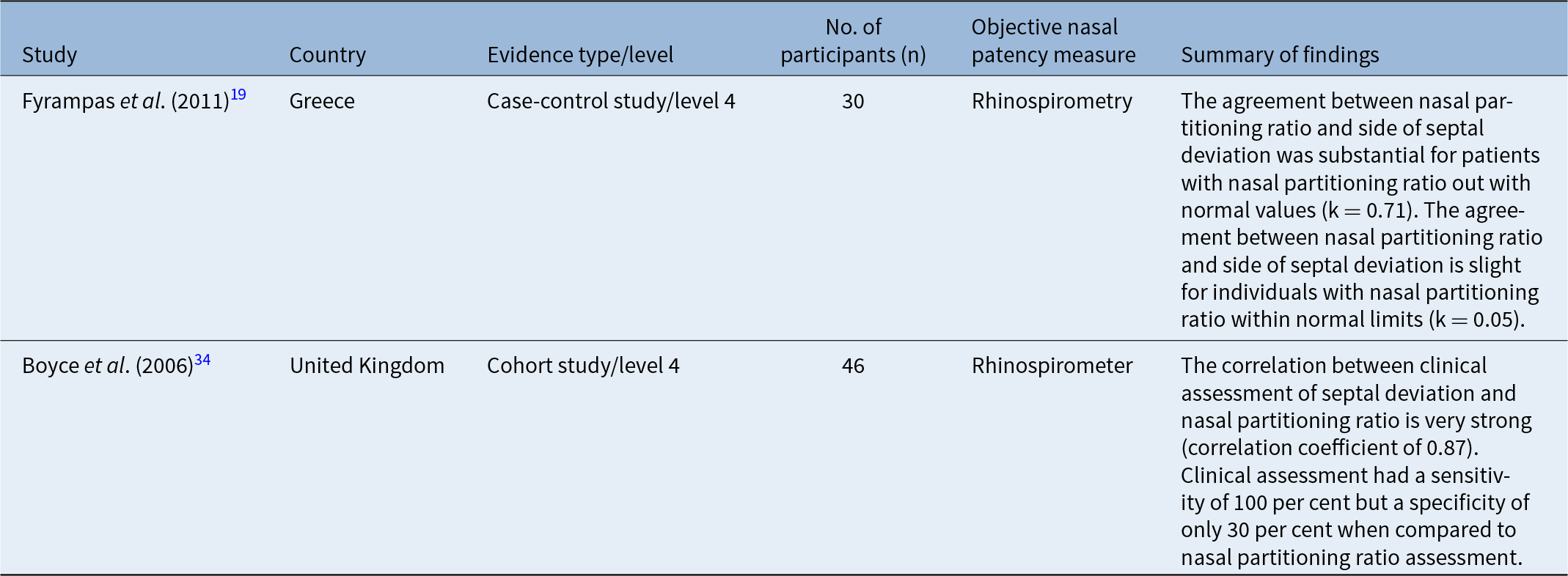
Studies exploring the relationship between clinical examination findings and rhinospirometry are shown in Table 5. Fyrmpas et al. reported that in patients with nasal partitioning ratio within normal limits (NPR value between +0.30 to -0.34 is the 95% reference range in the normal population), the agreement between nasal partitioning ratio and side of septal deviation using anterior rhinoscopy and nasal endoscopy is slight.Reference Fyrmpas, Kyrmizakis, Vital and Constantinidis19 However, in patients with a nasal partitioning ratio outside the normal range, the agreement between nasal partitioning ratio and side of septal deviation on clinical examination is substantial.Reference Fyrmpas, Kyrmizakis, Vital and Constantinidis19 Boyce et al. highlighted that the correlation between clinical assessment of septal deviation and nasal partitioning ratio is very strong.Reference Boyce and Eccles34 Clinicians are able to identify severe deviation more accurately with high sensitivity, but for patients with less severe septal deviation, the specificity of clinical examination is lowReference Boyce and Eccles34 and clinical examination alone may not be an alternative to rhinomanometry (Table 5).
Studies investigating the correlation between clinical examination findings and rhinospirometry
Discussion
Summary of key findings
This review aimed to explore the role of objective nasal patency measures using acoustic rhinomanometry, PNIF and rhinomanometry in supporting clinical nasal examination findings in structural nasal deformities. The body of evidence evaluating the relationship between objective nasal patency measures and clinical nasal examination in the literature is small and limited to cohort studies. Several studies have suggested that nasal constrictions measured on acoustic rhinomanometry correlated well with anatomical nasal narrowing identified on nasal endoscopy and individuals with nasal obstruction generally had a lower minimal cross-sectional area on acoustic rhinomanometry when compared to healthy individuals.Reference Corey, Nalbone and Ng11, Reference Trindade, Conegliam, Trindade, Dias and Sampaio-Teixeira21–Reference Huang, Wang, Zhang, Dong and Yeoh23 Acoustic rhinometry is a useful screening assessment prior to septoplasty, and this may guide clinicians to select patients who may achieve high post-operative satisfaction.Reference Pirilä and Tikanto25 However, other studies suggested that acoustic rhinometry failed to provide an exact point-to-point correlation with the nasal cavity and minimal cross-sectional areas and nasal volumes are not related to nasal obstruction secondary to septal deviation.Reference Tantilipikorn, Jareoncharsri, Voraprayoon, Bunnag and Clement24, Reference Isaac, Major, Witmans, Alrajhi, Flores-Mir and Major35 Although acoustic rhinometry is useful in predicting the major sites of anatomical nasal narrowing and confirming clinical examination findings, external factors such as nasal cycle, age, posture, temperature and inter-rater variability affect objective airway testing when using acoustic rhinometry. Therefore, acoustic rhinometry may be a useful tool when used in conjunction with clinical examination findings to facilitate pre-operative planning and predicting post-operative outcomes in septoplasty. However, the use of acoustic rhinometry assessment in isolation without clinical examination may be limited by its failure to provide exact point-to-point correlation with the nasal cavity.
There is limited evidence in the literature to assess the relationship between PNIF and clinical examination findings. Current evidence suggests that the relationship between PNIF assessment and clinical examination findings is very weak.Reference Panagou, Loukides, Tsipra, Syrigou, Anastasakis and Kalogeropoulos26, Reference Rujanavej, Snidvongs, Chusakul and Aeumjaturapat33 A cutoff value of 90 L/min on PNIF was considered “normal” for patients without sinonasal disease.Reference Panagou, Loukides, Tsipra, Syrigou, Anastasakis and Kalogeropoulos26 However, this cutoff value has a high sensitivity but a low specificity when compared to anterior rhinomanometry, making clinical interpretation of PNIF values difficult in patients with nasal obstruction. The high sensitivity of PNIF may aid clinicians in identifying patients with sinonasal disease but its low specificity may result in difficulty in interpreting low PNIF values in healthy asymptomatic individuals without sinonasal disease. The bilateral nature of PNIF assessment and the fact that the nasal valve and alar collapse during rapid inspiration causing some degree of airway block make PNIF less reliable when assessing nasal blockage. The use of PNIF as a screening tool for nasal obstruction has not been widely explored and further research focusing on unilateral PNIF may be useful in the future to assess patients with varying degrees of nasal obstruction.
Rhinomanometry assessment correlates well with clinical examination findings in severe anterior septal deviation.Reference Szücs and Clement22 However, the role of rhinospirometry in assessing middle/posterior and mild/moderate septal deviation remains uncertain. Rhinomanometry assessment should be interpreted with caution as abnormally low flow rates on rhinomanometry have been previously detected in patients in patients with no septal deviation or mild deviation restricted to one anatomical area.Reference Huygen, Klaassen, de Leeuw TJ and Wentges29 Rhinomanometry is also a useful screening assessment tool prior to septoplasty to guide clinicians in selecting patients who may achieve high post-operative satisfaction.Reference Pirilä and Tikanto25, Reference Sipilä and Suonpää31, Reference Suonpää, Sipilä and Laippala32 Pirila et al. suggested that the pre-operative post-decongestant inter-cavital airflow ratio is a strong predictor for post-operative satisfaction and the optimum suggested cut of value is 1:2.Reference Pirilä and Tikanto25 The sensitivity and specificity of this cutoff value were 65 per cent and 60 per cent respectively for patients reporting high and very high post-operative satisfaction when compared to the sensitivity/specificity of anterior rhinoscopy (55%/55%). Although the sensitivity/specificity of this measurement is higher when compared to anterior rhinoscopy, the results should be interpreted with caution given the difference in sensitivity and specificity between rhinomanometry measurement and anterior rhinoscopy in assessing post-operative satisfaction is marginal.
The relationship between clinical examination findings and rhinospirometry also remains inconclusive. Nasal partitioning ratio measured from rhinospirometry is highly predictive of severe septal deviation. Although clinicians were able to differentiate severe septal deviation from moderate/mild deviation on clinical examination easily, differentiating less severe deviation from severe remains a challenge for clinicians. The sensitivity of clinical assessment of septal deviation is high but its specificity is low when compared to nasal partitioning ratio assessment in rhinospirometry. Although clinicians are able to identify severe septal deviations with NPR outside the normal range, the ability of clinicians to confidently differentiate less severe septal deviation from normal and abnormal NPR remains poor. Hence, nasal partitioning ratio assessment in rhinospirometry may be useful in assessing less severe septal deviation when used in conjunction with clinical examination findings.Reference Fyrmpas, Kyrmizakis, Vital and Constantinidis19, Reference Boyce and Eccles34
• The role of objective nasal patency measures (ONPM) in assessing structural nasal obstruction remains uncertain.
• Studies exploring the relationship between ONPM and clinical nasal examination findings are limited and confined to cohort studies in the literature.
• Acoustic rhinometry, rhinomanometry and rhinospirometry assessment correlate positively in severe anterior septal deviation but their role in assessing middle/posterior and mild/moderate septal deviation in isolation remains uncertain.
• ONPM supports clinical examination findings in severe structural nasal obstruction. Using ONPM alongside clinical examination findings may aid patient selection for septoplasty and predict post-operative satisfaction.
Risk of bias and limitations
Most of the evidence described in this review was derived from low-level findings from cohort studies and case series. The participants from these cohort studies were heterogeneous and subjected to selection, publication and ascertainment bias. A meta-analysis was also not possible due to limited and heterogeneous evidence in the literature. The focus of the published literature has mainly been on septal deviation and other causes of nasal obstruction secondary to structural sinonasal disease such as nasal polyps and trauma remain unclear. Non-English primary articles and studies involving children were also excluded in this review.
Implication for research and clinical practice
Evidence from this review highlights that objective nasal patency measuring tools have a limited role in supporting clinical examination findings. Although objective nasal patency measures are useful in identifying patients with severe nasal obstruction, their utility in investigating mild or moderate nasal obstruction remains poor. Objective nasal patency measures can be used in conjunction with clinical examination findings to aid patient selection for septoplasty and predict post-operative satisfaction. Further research in this field is necessary to investigate how objective nasal patency measures can be used as an objective diagnostic tool when assessing severe, moderate and mild nasal obstruction.
Data availability statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Competing interest
None to declare
Authors contributions
Pavithran Maniam is an Academic Clinical Fellow at North East England and is the lead author and was involved in conceptualisation of research question, analysis of data and writing of this manuscript. Ian Wei Lim is a final year medical student based at the University of Sheffield Medical School, Sheffield, UK, and was involved in data collection and data analysis. Kim Hui Lim is a core surgical trainee based at Northwest Anglia NHS Foundation Trust and was involved in data analysis and writing of manuscript. Sean Carrie is a Consultant Otolaryngologist at Newcastle Hospital NHS Foundation Trust and was the project supervisor and was involved in writing of this manuscript. James O’Hara is a Consultant Otolaryngologist at Newcastle Hospital NHS Foundation Trust and was the project supervisor and was involved in writing of this manuscript.
Acknowledgement
We are grateful to the University of Newcastle librarian for assistance with the identification and sourcing of our cited literature.
Appendix 1
The literature search was performed and reviewed by two independent assessors (PM and IL) using the following databases: Pubmed (US National Library of Medicine), Medline, Embase, SCOPUS, Web of Science, Cumulated Index to Nursing and Allied Health Literature (CINAHL), Cochrane Library and Google Scholar.
Search terms used
Medline/Web of science
((Video endoscop* or nasal endoscop* or clinical examination* or anterior rhinoscope*) and (rhinometry, acoustic or acoustic rhinometry or PNIF or peak nasal inspiratory flow or rhinospirometer or rhinomanometer or nasal patency or nasal partitioning ratio))
Pubmed/Embase/CINAHL/SCOPUS/COCHRANE
((“Video endoscop*” or “nasal endoscop*” or “clinical examination*” or “anterior rhinoscope*”) and (“rhinometry, acoustic” or “acoustic rhinometry” or “PNIF” or “peak nasal inspiratory flow” or “rhinospirometer” or “rhinomanometer” or “nasal patency” or “nasal partitioning ratio”))
A random search was also performed on Google scholar and Google using the search terms above. Additional articles identified from citation lists of articles searched from the databases mentioned above were also supplemented during the review stage. Articles exploring the relationship between clinical examination and objective nasal patency measures were included in the synthesis of results. The titles and abstracts were screened independently by reviewers (PM and IL) as per the inclusion and exclusion criteria outlined in Table 1. In the event of uncertainties in including or excluding an article following the assessment of the inclusion criteria, a discussion was held between the reviewers (PM and IL) to reach a consensus. All articles included following title and abstract screening were reviewed in full for further inclusion/exclusion. A narrative synthesis of the articles included was provided to explore the relationship between clinical examination findings and objective nasal patency measures.







