Compulsory treatment is integral to mental healthcare and originally restricted to in-patient settings. Reference Kjellin, Hoyer, Engberg, Kaltiala-Heino and Sigurjonsdottir1 Several legislations now permit coerced treatment in the community. Reference Dawson2 Many ‘voluntary’ patients experience their cooperation with mental healthcare as coerced. Reference Hoge, Lidz, Eisenberg, Gardner, Monahan and Mulvey3 A study of public mental health service patients in five US cities found that half the sample reported experiencing specific pressures to promote treatment adherence. Reference Monahan, Redlich, Swanson, Robbins, Appelbaum and Petrila4 These pressures are referred to as ‘informal coercion’ or more commonly ‘leverages’. Leverages included access to accommodation, financial assistance and reduction or waiving of judicial sanctions. It is not clear if these high levels of leverage are restricted to the USA. The US mental healthcare system has a relatively fragmented community provision, limited availability of adequate benefits Reference Clark Robbins, Petrila, LeMelle and Monahan5 and some availability of ‘mental health courts’. Reference Redlich, Steadman, Clark Robbins and Swanson6 Leverage may be less common in a European setting where accommodation and welfare payments are basic entitlements and cannot be easily linked to treatment. We measured the prevalence and patterns of leverage across four differing clinical samples and tested for patient and treatment characteristics associated with them.
Method
Ethical approval was given by Oxfordshire Research Ethics Committee A (22 February 2006, Ref. No. 05/Q1604/180). An independent researcher explained the study and obtained written informed consent for an interview and examination of case notes. Participants were paid £10 (US$15) for the 50 min interview. This comprised demographic and historical data plus a series of structured questions (Appendix) on four forms of leverage adapted from Monahan and colleagues’ US study. Reference Monahan, Redlich, Swanson, Robbins, Appelbaum and Petrila4
Sample
Participants were recruited from the Oxford and Buckinghamshire Mental Health Trust that serves a mixed urban and rural population of 1 million. Recruitment procedures varied between the different teams. We aimed to recruit 100 assertive outreach team (AOT) patients with a diagnosis of psychosis, 100 community mental health team (CMHT) patients with a diagnosis of psychosis, 100 CMHT patients with a diagnosis of non-psychosis and lastly 100 people with heroin-dependent substance misuse currently treated with substitution medication (methadone or subutex). There were no exclusion criteria apart from a duration of care of less than 6 months.
Assertive outreach teams target hard to engage people with psychosis and have small case-loads (1:12), whereas CMHTs have higher, diagnostically mixed case-loads (usually 1:25). The participants with substance misuse either attended dispersed local clinics run by the mental health services or attended their general practitioner as ‘shared-care’ patients for prescribing and follow-up.
All patients on the case-loads of the Trust’s four AOTs were approached and CMHT participants were recruited in randomly selected blocks of 25 with either psychosis or non-psychosis diagnoses from the case-loads of eight teams. Oversampling was undertaken in all four samples because the duration of contact (required to confirm eligibility) could not always be identified reliably from the case notes. Comprehensive case-loads were not available in the substance misuse services. A consecutive convenience sample was obtained from the four methadone clinics in the Oxfordshire County and the Oxford City shared-care methadone services.
A series of established, validated questionnaires and rating instruments were conducted by the researcher at the interview between January 2008 and April 2009. Training was provided by an experienced psychiatrist for the clinical rating scales. The first 20 participants were jointly rated by both researchers. Interrater reliability for Global Assessment of Functioning (GAF) Reference Endicott, Spitzer, Fleiss and Cohen7 was fair (intraclass correlation coefficient (ICC) = 0.489) and for Brief Psychiatric Rating Scale (BPRS) Reference Overall and Gorham8 was moderate (ICC = 0.789). Refresher sessions were conducted every 6 months.
Instruments
-
(a) The GAF rates impairment in functioning ranging from 0 to 100, with given anchors at 10-point levels.
-
(b) BPRS Reference Overall and Gorham8 rates 18 symptoms each for severity from one to seven.
-
(c) The Insight and Treatment Attitudes Questionnaire (ITAQ) Reference McEvoy, Freter, Everett, Geller, Appelbaum and Apperson9 is a self-reported, semi-structured 11-item questionnaire assessing awareness of illness and need for treatment.
-
(d) The Conjoint CAGE Reference Erwing10 is an 8-item questionnaire for screening both alcohol (four items) and drug misuse (four items). Two or more positive responses on either scale indicate pathology.
-
(e) Leverage questions are detailed in the Appendix and are taken from the Monahan study. Reference Monahan, Redlich, Swanson, Robbins, Appelbaum and Petrila4 Questions test for both access to and potential withdrawal of benefits. Questions are repeated for each stage of the criminal justice system. Any positive response within a specific leverage area counts as ‘reported’.
Statistical analysis
Comparisons across three or more sample groups were carried out using Kruskall–Wallis non-parametric tests. A variety of tests were used when only two groups were compared. These were: the Mann–Whitney test for non-normally distributed continuous variables; chi-squared test for binary variables; and ANOVA for categorical variables. To compare our outcomes with the US sample, overall percentages and pooled means and standard deviations were calculated for the latter. A t-test was used when comparing means and a two-proportion Z-test when comparing percentages. Analyses were run in SPSS 15.0 for Windows.
Univariate and multivariate multilevel logistic regressions were used to investigate the association of sociodemographic and clinical characteristics with types of leverage in the whole sample. As the sample comprised participants from four different groups, it was treated as a stratified sample with two levels or strata. The four subgroups occupy the upper level and the participants form the lower level. It is expected that participants in the same sample group are more similar to each other, thus breaking the independence assumption needed for standard statistical methods. Multilevel models were used to analyse variables measured at different levels simultaneously, employing a statistical model that includes the various dependencies. Reference Hox11 Stata 9.0 command xtlogit on Windows was used for this analysis.
Results
We recruited 417 participants: 101 in the CMHT psychosis group, 101 in the substance misuse group, 102 in the AOT (with psychosis) group and 113 in the CMHT non-psychosis group. Of 912 identified patients, 308 were uncontactable, discharged or ineligible. Of the 604 approached 188 refused involvement.
Baseline characteristics
Table 1 outlines the sociodemographic and main historical and clinical features of the four samples using the same presentation format and variables as Monahan and colleagues Reference Monahan, Redlich, Swanson, Robbins, Appelbaum and Petrila4 for ease of comparison. The group was predominantly male (60%), White (89%) and born in the UK (89%). Most patients were single (60%) and most (83%) lived in independent accommodation. Service contact ranged from a mean of 17 years for the AOT group to 11.5 years for the substance misuse group with repeated hospitalisations in the mental illness sample (AOT and CMHT groups combined). The BPRS mean total score of 33.0 and GAF of 56.9 indicate a relatively poorly functioning group.
Differences in baseline characteristics between the clinical samples
There were statistically significant differences between the four clinical samples on a number of variables not included in Table 1. General education was shorter in the substance misuse group; employment was lowest in the AOT group who also were much more likely to be single. The proportion of those with children under 18 who were living with them was lowest in the AOT group at 15% in contrast to 65% of those in the CMHT non-psychosis group and 54% of those in the CMHT psychosis group. The number of past hospitalisations ranged from a mean of 6.5 in the AOT group to 0.2 in the substance misuse group.
Differences between the mental illness and substance misuse samples
The substance misuse sample appears to have contributed most to the variation in baseline characteristics and so it was compared individually with the mental illness group. The substance misuse sample was significantly younger than the mental illness sample (mean 34.7 v. 42.0 years) with more men (76% v. 55%) and fewer participants from ethnic minorities (3% v. 13%). Significant differences were found for all psychiatric history variables. Age at first contact with psychiatric services was significantly lower for the substance misuse group (mean 23.3 v. 25.9), number of psychiatric hospitalisations was lower (mean 0.2 v. 4.0) and number of previous involuntary hospitalisations lower (4% v. 52%). The substance misuse sample had more criminal convictions (82% v. 26%) and previous imprisonments (48% v. 14%).
Differences within the mental illness groups
The three mental illness groups (AOT and CMHTs) demonstrated greater homogeneity. There were no significant differences in years of general education, proportion of those with children younger than 18 years and proportion with criminal convictions. All other differences identified across the four samples retained their significance.
Lifetime experience of leverage
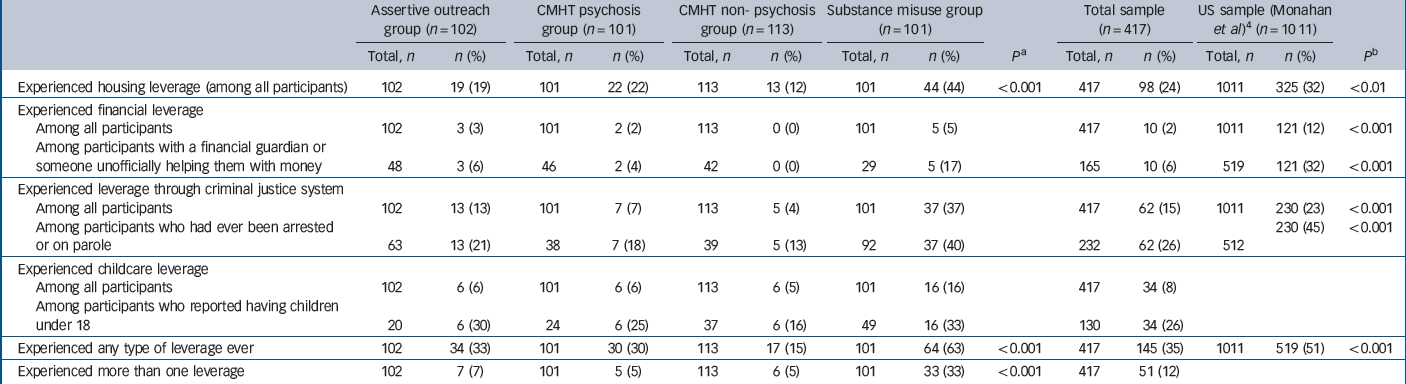
Table 2 displays the rates of lifetime experience of reported leverage types across the four groups. Overall, 145 (35%) participants reported any leverage, of whom 51 (12%) reported more than one type and seven more than two. Multiple leverages are predominantly reported in the substance misuse group (33%). Housing leverage is by far the most common (24%). The criminal justice system leverage of 15% overall is accounted for almost entirely by the substance misuse and AOT groups. Financial leverage was only reported by ten participants (2%) but childcare access leverage was reported for 34 (8%) participants; reflecting 26% of the 130 with children under 18 years of age.
Table 3 shows the univariate associations of individual leverages and Table 4 the univariate and multivariate associations of overall experience of leverages and of the experience of more than one type of leverage. In multivariate analysis all the significances are lost apart from ethnicity. Reporting more than one type of leverage (Table 4) remains significantly associated in
Sociodemographic characteristics across the four samplesa

| Assertive outreach group (n = 102) | CMHT psychosis group (n = 101) | CMHT non-psychosis group (n = 113) | Substance misuse group (n = 101) | Total sample (n = 417) | P b | US sample (Monahan et al)4 (n = 1011) | P c | |
|---|---|---|---|---|---|---|---|---|
| Age, years: mean (s.d.) | 40.1 (10.37) | 42.2 (10.67) | 43.7 (10.69) | 34.7 (8.56) | 40.3 (10.65) | <0.001 | 43.4 (10) | <0.001 |
| Ethnicity, n (%) | ||||||||
| White d | 80 (78) | 86 (85) | 108 (95) | 98 (97) | 372 (89) | <0.001 | 341 (34) | |
| Other e | 22 (22) | 15 (15) | 5 (5) | 3 (3) | 45 (11) | 662 (65) | ||
| Male, n (%) | 77 (76) | 55 (55) | 43 (38) | 77 (76) | 252 (60) | 509 (50) | <0.001 | |
| Diagnosis (ICD-10),12 n (%) | <0.001 | |||||||
| Schizophrenia | 93 (91) | 75 (74) | 0 (0) | 0 (0) | 168 (40) | 457 (45) | ||
| Bipolar disorder | 3 (3) | 26 (26) | 0 (0) | 0 (0) | 29 (7) | 166 (16) | <0.001 | |
| Major depression | 6 (6) | 0 (0) | 82 (73) | 0 (0) | 88 (21) | 299 (30) | <0.001 | |
| Substance misuse | 0 (0) | 0 (0) | 1 (1) | 101 (100) | 102 (25) | 250 (25) | ||
| Anxiety | 34 (3) | |||||||
| Other diagnosis | 0 (0) | 0 (0) | 30 (26) | 0 (0) | 30 (7) | 40 (4) | ||
| More than two hospitalisations, n (%) | 84 (82) | 50 (50) | 38 (34) | 2 (2) | 174 (42) | <0.001 | 624 (62) | <0.001 |
| Duration of psychiatric history, years: mean (s.d.) | 17.0 (9.26) | 16.7 (10.78) | 14.6 (11.86) | 11.5 (8.63) | 15.0 (10.45) | <0.001 | 21 (11.6) | <0.001 |
| Number of out-patient visits in the past month, mean (s.d.) | 6.3 (7.85) | 1.3 (1.73) | 1.1 (1.66) | 2.2 (1.34) | 2.7 (4.58) | <0.001 | 4.4 (4.8) | <0.001 |
| CAGE Positive for drug or alcohol, n (%) | 18 (18) | 20 | 17 (15) | 76 (75) | 131 (31) | <0.001 | 214 (21) | <0.001 |
| ITAQ total score, mean (s.d.) | 15.5 (5.61) | 17.7 (3.70) | 17.6 (3.38) | 16.5 (2.98) | 16.9 (4.11) | <0.001 | 18.4 (3.8) | <0.001 |
| BPRS, mean (s.d.) | 34.2 (7.50) | 32.9 (9.74) | 35.8 (8.29) | 29.1 (7.04) | 33.0 (8.45) | <0.001 | 32.4 (8.4) | <0.05 |
| GAF, mean (s.d.) | 56.0 (11.69) | 57.1 (14.54) | 55.2 (14.53) | 59.6 (11.13) | 56.9 (13.18) | 47.8 (9.4) | <0.001 | |
CMHT, community mental health team; ITAQ, Insight and Treatment Attitudes Questionnaire; BPRS, Brief Psychiatric Rating Scale; GAF, Global Assessment of Functioning.
a All percentages do not always add up, because of missing data.
b Comparison of baseline characteristic across four samples; Kruskall–Wallis test.
c Comparison of baseline characteristic between English and US samples; two-proportion Z-test.
d For US sample this category is ‘White or other’.
e For US sample this category is ‘Black’.
Types of leverage received by patients in community mental healthcare across the four samples
| Assertive outreach group (n = 102) | CMHT psychosis group (n = 101) | CMHT non- psychosis group (n = 113) | Substance misuse group (n = 101) | Total sample (n = 417) | US sample (Monahan et al)4 (n = 1011) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total, n | n (%) | Total, n | n (%) | Total, n | n (%) | Total, n | n (%) | P a | Total, n | n (%) | Total, n | n (%) | P b | |
| Experienced housing leverage (among all participants) | 102 | 19 (19) | 101 | 22 (22) | 113 | 13 (12) | 101 | 44 (44) | <0.001 | 417 | 98 (24) | 1011 | 325 (32) | <0.01 |
| Experienced financial leverage | ||||||||||||||
| Among all participants | 102 | 3 (3) | 101 | 2 (2) | 113 | 0 (0) | 101 | 5 (5) | 417 | 10 (2) | 1011 | 121 (12) | <0.001 | |
| Among participants with a financial guardian or someone unofficially helping them with money | 48 | 3 (6) | 46 | 2 (4) | 42 | 0 (0) | 29 | 5 (17) | 165 | 10 (6) | 519 | 121 (32) | <0.001 | |
| Experienced leverage through criminal justice system | ||||||||||||||
| Among all participants | 102 | 13 (13) | 101 | 7 (7) | 113 | 5 (4) | 101 | 37 (37) | 417 | 62 (15) | 1011 | 230 (23) | <0.001 | |
| Among participants who had ever been arrested or on parole | 63 | 13 (21) | 38 | 7 (18) | 39 | 5 (13) | 92 | 37 (40) | 232 | 62 (26) | 512 | 230 (45) | <0.001 | |
| Experienced childcare leverage | ||||||||||||||
| Among all participants | 102 | 6 (6) | 101 | 6 (6) | 113 | 6 (5) | 101 | 16 (16) | 417 | 34 (8) | ||||
| Among participants who reported having children under 18 | 20 | 6 (30) | 24 | 6 (25) | 37 | 6 (16) | 49 | 16 (33) | 130 | 34 (26) | ||||
| Experienced any type of leverage ever | 102 | 34 (33) | 101 | 30 (30) | 113 | 17 (15) | 101 | 64 (63) | <0.001 | 417 | 145 (35) | 1011 | 519 (51) | <0.001 |
| Experienced more than one leverage | 102 | 7 (7) | 101 | 5 (5) | 113 | 6 (5) | 101 | 33 (33) | <0.001 | 417 | 51 (12) | |||
CMHT, community mental health team.
a Comparison of experienced leverage across four samples; Kruskall—Wallis test.
b Comparison of experienced leverage in English and US samples; two-proportion Z-test.
multivariate analysis for independent accommodation, substance misuse diagnosis and a history of imprisonment.
Discussion
England–USA differences
This is the first study of leverage in England and demonstrates that it is common in public mental health services for severely ill patients. A third reported feeling coerced to adhere to treatment at some time in their lives. These levels are substantially lower than those from the USA (35% compared with 51%). This difference is more pronounced when childcare and access leverage is removed (overall leverage 31% of English participants, 9% with more than one form) as this was not reported in the US reference paper, although it has been reported subsequently from the same sample. Reference Busch and Redlich13 Formal coercion in the community was available in the USA but not in the English context at the time of the study. It was experienced by 12–20% of the US sample Reference Monahan, Redlich, Swanson, Robbins, Appelbaum and Petrila4,Reference Swartz, Swanson, Kim and Petrila14 but, as it is formal coercion, is not included in our comparison with the US study.
Univariate associations of leverages and baseline characteristicsa

| Housing leverage OR (95% CI) | Financial leverage OR (95% CI) | Leverage through criminal justice, OR (95% CI) | Childcare leverage OR (95% CI) | |
|---|---|---|---|---|
| Ethnicity, White | 0.8 (0.3–1.8) | – | 0.1 ** (0.03–0.5) | 0.3 (0.1–1.2) |
| Marital status, single v. others | 1.8 * (1.1–3.1) | 5.7 (0.3–114.8) | 0.8 (0.2–2.5) | 1.6 (0.7–3.5) |
| If children under 18 years, they live: with a separated partner | 2.6 * (1.04–6.4) | – | 0.2 (0.02–2.0) | 1.9 (0.8–4.6) |
| Accommodation, independent v. other | 0.3 *** (0.2–0.6) | 1.2 (0.2–8.7) | 1.4 (0.5–4.2) | 0.9 (0.3–2.3) |
| If independent, live with: alone v. other | 1.2 (0.7–2.1) | 3.1 (0.1–125.3) | 0.1 * (0.03–0.7) | 1.3 (0.5–3.4) |
| Diagnosis (ICD-10) (compared with those with schizophrenia) | ||||
| Bipolar disorder | 0.4 (0.1–1.4) | 4.9 × 10–13 (0–∞) | 1.1 (0.1–13.8) | 1.9 (0.4–10.3) |
| Major depression | 0.5 (0.2–1.1) | 4.3 × 10–13 (0–∞) | 2.1 × 1012 (0–∞) | 0.6 (0.2–1.9) |
| Substance misuse | 2.7 *** (1.5–4.6) | 9.0 (0.8–100.2) | 2.3 (0.8–6.6) | 1.2 (0.5–3.3) |
| Other diagnosis | 0.4 (0.1–1.4) | 4.3 × 10–13 (0–∞) | 2.1 × 1012 (0–∞) | 2.4 × 10–13 (0–∞) |
| Age at first contact with psychiatric services | 0.5 * (0.3–0.9) | 0.6 (0.1–3.5) | 0.8 (0.3–2.2) | 0.5 (0.2–1.1) |
| Number of out-patient visits in the past month | 1.1 (0.7–2.0) | 1.2 (0.2–10.0) | 0.2 * (0.04–0.9) | 1.3 (0.6–2.9) |
| CAGE: positive for drug or alcohol | 1.80 * (1.0–3.2) | 2.50 (0.46–13.65) | 1.03 (0.27–3.91) | 1.52 (0.69–3.37) |
a Table 3 contains information only for variables that were significant for any type of leverage.
* P < 0.05
** P < 0.01
*** P < 0.001.
Multivariate and univariate associations with receiving any type of leverage and more than one leveragea

| Univariate | Multivariate | |||
|---|---|---|---|---|
| Any leverage OR (95% CI) | More than one type of leverage, OR (95% CI) | Any leverage OR (95% CI) | More than one type of leverage, OR (95% CI) | |
| Children under 18 years old, yes | 1.4 (0.9–2.2) | 1.9 * (1.0–3.5) | - | 1.5 (0.7–2.8) |
| Accommodation, independent v. other | 0.4 ** (0.2–0.7) | 0.4 ** (0.2–0.8) | 0.53 (0.3–1.0) | 0.5 * (0.2–0.9) |
| Diagnosis (ICD-10) (compared with those with schizophrenia) | ||||
| Bipolar disorder | 0.5 (0.2–1.2) | 1.0 (0.2–4.5) | 0.82 (0.3–2.5) | 1.4 (0.3–6.8) |
| Major depression | 0.4 ** (0.2–0.7) | 1.0 (0.3–2.6) | 0.6 (0.3–1.3) | 1.2 (0.4–3.5) |
| Substance misuse | 3.0 *** (1.8–5.1) | 6.2 *** (3.0–12.8) | 5.7 *** (2.2–15.1) | 3.0 * (1.3–7.2) |
| Other diagnosis | 0.5 (0.2–1.4) | 0.4 (0.1–3.6) | 0.7 (0.2–2.3) | 0.5 (0.1–4.3) |
| Age at first contact with psychiatric services | 0.5 ** (0.3–0.8) | 0.5 (0.3–1.0) | 0.6 (0.4–1.0) | – |
| More than two hospitalisations | 3.3 *** (1.8–6.0) | 2.6 (0.9–6.9) | 2.8 ** (1.4–5.6) | – |
| Hospitalisations ever | 1.8 * (1.1–3.0) | 1.5 (0.6–3.5) | 1.1 (0.6–2.3) | – |
| Duration of psychiatric history, years | 1.9 ** (1.2–2.9) | 1.9 (0.98–3.5) | 1.3 (0.8–2.2) | – |
| Criminal convictions ever, yes/no | 2.5 *** (1.6–4.1) | 3.2 ** (1.5–6.8) | 1.4 (0.7–2.6) | 1.4 (0.6–3.4) |
| Imprisonment ever, yes/no | 2.7 *** (1.6–4.6) | 3.4 *** (1.7–6.7) | 1.8 (0.9–3.7) | 2.4 * (1.1–5.2) |
| ITAQ total score | 2.0 ** (1.2–3.1) | 0.9 (0.5–1.8) | 2.0 * (1.1–3.4) | – |
| CAGE: positive for drugs or alcohol | 1.6 (0.96–2.7) | 2.6 * (1.2–5.4) | – | 1.6 (0.8–3.4) |
ITAQ, Insight and Treatment Attitudes Questionnaire.
a Table 4 contains information only for variables that were significant in univariate analysis.
* P < 0.05
** P < 0.01
*** P < 0.001.
Clinical group differences
Leverage varied considerably across the clinical groups in the manner anticipated. The younger, substance misuse group reported the highest level of leverage; higher than the US group (63% compared with 51%). Levels fell according to the general severity of the groups through the psychosis groups to the non-psychosis CMHT group.
Types of leverage
The highest rate of leverage was related to accommodation. A quarter of the sample reported this (32% in the USA). It was substantially higher in the substance misuse group (44%), presumably reflecting the practice of many landlords (both private and public sector) of demanding attendance at drug programmes as a condition of tenancy. This is much less common in mental illness services, particularly in private accommodation. The 20% rate found in participants with psychosis is restricted to hostel and supervised accommodation. We found evidence of leverage by private landlords in the mental illness samples.
The USA has a highly developed system of ‘drug courts’ and, more recently, ‘mental health courts’ Reference Redlich, Steadman, Monahan, Robbins and Petrila15 exclusively trying and sentencing individuals with behavioural and mental health problems. England utilises a range of ‘court diversion’ schemes where individuals are identified pre-trial and diverted into the healthcare system. In the USA the coercion is explicit in the sentencing procedure –‘choose treatment or punishment’. The less formal English approach may mean that potential coercion is not registered.
The most striking difference between the two national samples is in the use of money as leverage. Over half of the US sample (n = 519) had a financial guardian or someone unofficially managing their money. Of these, 121 (32%) participants reported that receiving it had depended on their accepting treatment. In the English sample, 165 (40%) reported that they had someone managing their money but only 10 (6%) experienced it as leverage. Money management remains a controversial issue in England and few teams use it or feel comfortable with it. Half (n = 5) of those reporting it were in the substance misuse group and presumably this was family pressure as the clinical teams did not use it. Some AOTs in England are now experimenting with its use. Reference Burns and Firn16
Baseline characteristics associated with leverage
We failed to find the strong association between leverage and patient characteristics as in the USA, probably because of their larger sample and greater clinical variation. Our only significant associations were with a substance misuse diagnosis, more than two hospitalisations and a lower score on the insight and treatment attitudes measure (ITAQ).
Limitations
Our study has several limitations. It reports ‘experience’ of leverage without third-party corroboration. Some of the leverages reported would probably have been disputed by the clinicians. Leverage may also have been applied but not recognised as such. Szmukler & Appelbaum have outlined a gradation of informal coercion and many staff may strive to recast leverage as persuasion. Reference Szmukler and Appelbaum17 We were also obliged to use differing sampling strategies for the different teams but it is unclear what effects this would exert. Our refusal rate is also more than twice that in the US sample (31% compared with 2–15%). The reasons for this are unclear and it cannot be discounted that participants perceiving higher levels of coercion might be more likely to refuse, thereby reducing the reported English levels. Higher levels of leverage were demonstrated to be associated with committed acts of violence (18–21% in the preceding 6 months) in the US sample. Reference Swanson, Van Dorn, Monahan and Swartz18 In the absence of comparable violence data in the English sample we cannot estimate if it might account for the reported leverage differences. We are unable to draw any conclusions as to the efficacy of leverage in this cross-sectional study.
Implications
Despite these limitations we believe our results convey a broadly accurate picture of the experience of leverage in these patient groups. In the mental illness groups leverage rates are associated with increasing severity of illness. The high levels in substance misusers reflect a tougher negotiating approach to individuals generally perceived to have more control over their behaviour. English staff assume that severely ill individuals are ‘entitled’ to a wide range of social benefits (housing, financial support, etc). In the USA, benefits are rarely viewed as automatic entitlements, but are targeted where most likely to achieve effect. The participants in the US study were, however, generally in receipt of these benefits and it is possible that higher reported perceived coercion may reflect the more widespread sense of entitlement in the English sample rather than any higher actual leverage in the US sample.
Overall, the pattern is more similar than different between the USA and England. A substantial proportion of individuals in public mental healthcare do not feel entirely free in their interactions with services. Although some pressure comes from family and friends, many experience healthcare staff as coercing them. Informal coercion is as widespread, if not more so, than formal coercion. There is a pressing need for research to understand it both to inform policy and to train staff who are clearly using it routinely.
Appendix
Questions used to identify experienced leverage
Finance
Did anyone (financial manager/guardian) ever make giving you your money, or giving you spending money, depend on whether you did what he or she wanted in terms of getting mental health, alcohol or drug treatment (or taking medication)?
Housing
Have you ever lived somewhere where you were required to stay in mental health or substance use treatment (or required to continue taking your medication) to keep living there (including family home)?
Have you ever been told that obtaining new accommodation is dependent on you taking treatment?
Criminal justice
Has anyone in the legal system ever told you or your lawyer that the charges will be dropped or reduced if you get treatment in the community for your mental health, alcohol or drug problems?
Has a mental health professional, or anyone in the legal system, or their report, suggested that you take treatment for a mental health problem as a condition of not going to prison?
Child custody
Have you ever been told that your children might be taken into care if you did not participate in mental health, alcohol or drug treatment (or taking your medication)?
Have you ever been told that your access to see your children would be reduced if you did not participate in mental health, alcohol or drug treatment (or taking your medication)?






eLetters
No eLetters have been published for this article.