Stalking is a prevalent social problem, affecting an estimated 10% of adults at some time (Reference Tjaden and ThoennesTjaden & Thoennes, 1998; Reference Budd and MattinsonBudd & Mattinson, 2000; Reference Purcell, Pathé and MullenPurcell et al, 2002). Stalking occurs when one person repeatedly intrudes on another to such an extent that the recipient fears for their safety. Clinical studies report high rates of post-traumatic stress, anxiety, depression and suicidality among victims presenting to specialist services for assistance (Reference Pathé and MullenPathé & Mullen, 1997; Reference Kamphuis and EmmelkampKamphuis & Emmelkamp, 2001; Reference Blaauw, Winkel and ArensmanBlaauw et al, 2002). However, the experiences of support-seeking victims probably represent the extreme end of the spectrum of stalking. This study examines psychiatric symptomatology in a representative community sample of stalking victims and compares the rates of psychopathology with a control group of respondents that had never experienced harassment. The results will afford greater understanding of the psychological sequelae of stalking and the mental health needs of victims.
METHOD
The data derive from an epidemiological survey that examined the prevalence and nature of stalking victimisation in an Australian community sample (see Reference Purcell, Pathé and MullenPurcell et al, 2002). A survey was mailed to a randomly selected sample of 3700 men and women whose names and addresses were taken from the electoral roll in the Australian State of Victoria (population 4.7 million). Entry age to the electoral rolls is 18 years and the rolls cover over 96% of the population, as both registration and voting are compulsory. Of 88 electoral districts in Victoria, one was randomly selected for the purpose of obtaining a sample. In Australia, electoral districts correspond to ‘statistical local areas’ compiled from census data. Each statistical local area records the demographic characteristics of citizens residing in that electoral district. Obtaining a sample from one electoral district therefore allows for comparison of the representativeness of the sample with the total district population. The selected electoral district (comprising 36 766 adults) was located approximately 15 km from the central business district of Melbourne.
Of the 3700 surveys distributed, 74% could be accounted for, including completed surveys (n=1844), known refusals and surveys not received (e.g. person no longer at that address, deceased, or overseas). Adjusting for the 697 surveys not received, the valid response rate was 61%. The response rate did not differ according to gender. Survey respondents were representative of the base electoral population in relation to gender, marital status, highest level of education, employment and occupational status. However, the sample contained fewer people aged 18–25 years (10 v. 19%) and more individuals aged 56 years and over (39 v. 31%).
Each respondent completed questions regarding their demographic characteristics, the experience of harassment and aspects of their current general health. The study was conducted with the approval of the Human Ethics Committee at Monash University.
Definition of harassment and stalking
Consistent with previous research (e.g. Reference Tjaden and ThoennesTjaden & Thoennes, 1998) the survey employed a behavioural definition of harassment. Respondents were asked whether any person, male or female, had ever: followed them; kept them under surveillance; loitered around their home, workplace or other places they frequent; made unwanted approaches; made unwanted telephone calls; sent unwanted letters, faxes or e-mails; sent offensive materials; ordered things on their behalf that they did not want; or interfered with their property. Respondents who recorded any of these behaviours were asked to indicate the frequency with which they occurred (once, twice, 3–9 times, 10 or more times) and whether they were fearful as a result of the behaviour. Those who had been harassed on more than one occasion by different individuals were asked to refer only to the experience with the one person they best remembered. This was to ensure that the index event referred only to one discrete episode of harassment, rather than an aggregation of the respondent's experiences of harassment.
In keeping with legal definitions of stalking (see Reference Purcell, Pathé and MullenPurcell et al, 2004a ), respondents who acknowledged two or more intrusions that induced fear were broadly classed as victims. However, analysis indicates that there is heuristic value in distinguishing between two types of repeated intrusiveness: short-lived harassment and protracted stalking (Reference Purcell, Pathé and MullenPurcell et al, 2004b ). Short-lived harassment involves an intense burst of intrusiveness that usually abates within days but may continue for up to 2 weeks. This form of harassment is usually perpetrated by strangers and largely confined to unwanted telephone calls and intrusive approaches. Intrusions that persist beyond the threshold of 2 weeks are likely to continue for months, be perpetrated by someone known to the victim and involve numerous methods of pursuit. This study distinguished between victims of short-lived harassment and protracted stalking, with 2 weeks being the threshold (for empirical validation of the 2-week threshold see Reference Purcell, Pathé and MullenPurcell et al, 2004b ).
Nature of the victimisation
Respondents who reported experiencing repeated intrusions completed items examining the nature of the behaviour, including whether the conduct had occurred in the 12 months prior to the survey, the duration of the harassment (number of days) and the nature of the prior relationship with the perpetrator (ex-intimate, acquaintance, estranged relative or friend, work-related contact, or stranger). Respondents were also asked to indicate whether there had been associated violence during the course of the pursuit, including threats and/or physical or sexual assault.
Indices of current mental health
All respondents completed the 28-item General Health Questionnaire (GHQ–28; Reference Goldberg and HillierGoldberg & Hillier, 1979), which provides an indication of current psychological health. Respondents are asked to rate the recent (past month) intensity of certain symptoms in comparison with their usual experience. Questions are rated on a four-point scale (e.g. from ‘better than usual’ to ‘much worse than usual’). The 28-item version of the GHQ provides scaled scores in four domains: somatic complaints, anxiety and insomnia, social dysfunction and severe depression. These sub-scales do not reflect psychiatric diagnoses and are not independent. The GHQ–28 has been validated in community samples (Reference BanksBanks, 1983; Reference Romans-Clarkson, Walton and HerbisonRomans-Clarkson et al, 1989) as well as in studies examining chronic forms of victimisation, including domestic violence (Reference Mullen, Romans-Clarkson and WaltonMullen et al, 1988; Reference Scott-Gliba, Minne and MezeyScott-Gliba et al, 1995) and stalking (Reference Blaauw, Winkel and ArensmanBlaauw et al, 2002).
The Impact of Event Scale (IES; Reference Horowitz, Wilner and AlvarezHorowitz et al, 1979) was used to assess post-traumatic stress symptomatology. In relation to a specific index event (in this study, the experience of harassment), respondents are asked to rate the applicability of each of 15 items over the preceding 7 days (never, rarely, sometimes, often). The IES comprises two sub-scales measuring the common post-trauma reactions of avoidance and re-experiencing phenomena. Seven items enquire about intrusive thoughts and images related to the event and eight items assess attempts to avoid thoughts or reminders of the incident. The IES has been extensively used in trauma-related research, including studies examining the impact of domestic violence (Reference Scott-Gliba, Minne and MezeyScott-Gliba et al, 1995) and stalking (Reference Blaauw, Winkel and ArensmanBlaauw et al, 2002).
Data analyses
The rates of psychiatric symptomatology were compared between victims of brief harassment (n=196; median duration 2 days), victims of protracted stalking (n=236; median duration 6 months) and a control group of respondents that had never experienced harassment (n=432). We have previously reported the demographic characteristics of the victim group (Reference Purcell, Pathé and MullenPurcell et al, 2002), which were highly skewed (e.g. 75% female, 43% aged 16–30 years, 76% in paid employment). Non-harassed individuals were therefore selected to match the victim group according to gender, age, highest level of education and employment status. Marital status could not be controlled between the groups, as the rates of separation and divorce were significantly higher among victims of stalking (16.1%) than among both the victims of brief harassment (5.1%) and the controls (7.1%; χ2=19.8, d.f.=2, P=0.003).
Data scoring
The GHQ–28 was analysed both as a continuous score and categorically, the latter indicating probable ‘caseness’. The term ‘case’ refers to the existence of significant psychological symptoms that are likely not only to adversely effect the respondent's quality of life, but are of a level frequently found among individuals seeking help from mental health professionals. The categorical scoring method involves the application of weights to the four response alternatives (0–0–1–1). Binary scoring (range 0–28) was then applied in the evaluation of threshold caseness morbidity levels using the conservative cut-off 5/6, in which those scoring a total of six or more are considered a probable case (Reference Goldberg, Gater and SartoriusGoldberg et al, 1997). For each of the four seven-item sub-scales, the Likert method of scoring was applied (0–1–2–3; range 0–21). The IES was also analysed as a continuous score and categorically. Measured as a continuous variable, the scale yields three scores: a total score (0–1–3–5; range 0–75) and sub-scale scores for symptoms of avoidance (range 0–40) and intrusion (range 0–35). As the avoidance and intrusion sub-scales were highly correlated (r=0.80, P=0.001), only the IES total score was analysed. A total score of 35 or more on the IES has previously been taken to indicate probable caseness reflecting significant post-traumatic reactions (Reference Scott-Gliba, Minne and MezeyScott-Gliba et al, 1995).
Statistical analyses
Discrete variables were analysed using χ2-tests. Odds ratios (ORs) and 95% CIs were calculated where appropriate. Continuous variables were compared between groups using independent groups t-tests or analysis of variance, with post hoc analyses of group main effects conducted using Tukey's honest significant difference. Pearson's product-moment correlation coefficients were calculated to examine the association between psychiatric morbidity and the nature of the intrusions. In order to minimise type I error associated with multiple comparisons, the error rate required to demonstrate significance was set at 0.01.
RESULTS
General psychiatric morbidity (GHQ–28)
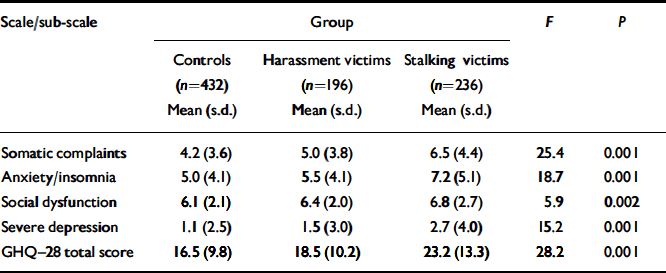
The proportion meeting the threshold for caseness on the GHQ–28 differed according to group (χ2=25.1, d.f.=2, P=0.001), the rates being significantly higher among victims of stalking (36.4%) than among those experiencing short-lived harassment (21.9%) and controls (19.3%). Sub-scale scores on the GHQ–28 also differed according to group, with victims of stalking scoring higher than both victims of short-lived harassment and controls on most measures (Table 1). The scores for victims of short-lived harassment did not differ significantly from those of controls on any measure.
Table 1 Total and sub-scale scores on the 28-item General Health Questionnaire (GHQ–28) for victims of stalking, victims of harassment and matched controls
| Scale/sub-scale | Group | F | P | ||
|---|---|---|---|---|---|
| Controls (n=432) Mean (s.d.) | Harassment victims (n=196) Mean (s.d.) | Stalking victims (n=236) Mean (s.d.) | |||
| Somatic complaints | 4.2 (3.6) | 5.0 (3.8) | 6.5 (4.4) | 25.4 | 0.001 |
| Anxiety/insomnia | 5.0 (4.1) | 5.5 (4.1) | 7.2 (5.1) | 18.7 | 0.001 |
| Social dysfunction | 6.1 (2.1) | 6.4 (2.0) | 6.8 (2.7) | 5.9 | 0.002 |
| Severe depression | 1.1 (2.5) | 1.5 (3.0) | 2.7 (4.0) | 15.2 | 0.001 |
| GHQ—28 total score | 16.5 (9.8) | 18.5 (10.2) | 23.2 (13.3) | 28.2 | 0.001 |
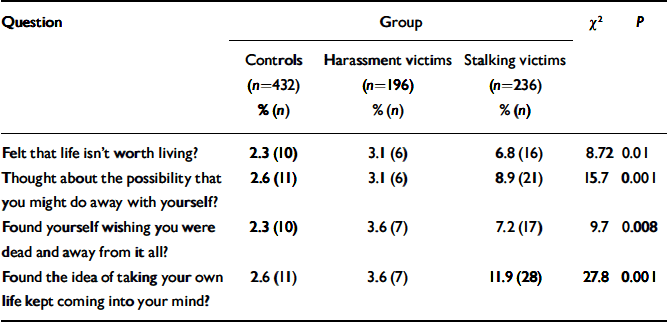
Victims of stalking notably had elevated scores on the index of severe depression. As high rates of suicidal ideation have previously been identified among stalking victims (Reference Pathé and MullenPathé & Mullen, 1997), the four GHQ–28 items assessing suicidality were examined (items 24, 25, 27 and 28). Victims of stalking were more likely than victims of short-lived harassment and controls to endorse recent suicidal ideation (Table 2).
Table 2 Respondents’ endorsement of suicidal ideation items on the 28-item General Health Questionnaire
| Question | Group | χ2 | P | ||
|---|---|---|---|---|---|
| Controls (n=432) % (n) | Harassment victims (n=196) % (n) | Stalking victims (n=236) % (n) | |||
| Felt that life isn't worth living? | 2.3 (10) | 3.1 (6) | 6.8 (16) | 8.72 | 0.01 |
| Thought about the possibility that you might do away with yourself? | 2.6 (11) | 3.1 (6) | 8.9 (21) | 15.7 | 0.001 |
| Found yourself wishing you were dead and away from it all? | 2.3 (10) | 3.6 (7) | 7.2 (17) | 9.7 | 0.008 |
| Found the idea of taking your own life kept coming into your mind? | 2.6 (11) | 3.6 (7) | 11.9 (28) | 27.8 | 0.001 |
Post-traumatic psychopathology
Only those who reported harassment completed the IES. Victims of stalking were three times more likely to meet the threshold for caseness on the IES (16.3%) than victims of short-lived harassment (5.1%; OR=3.6, 95% CI 1.7–7.4; P=0.001). Total IES scores were also higher among victims of stalking (mean (s.d.)=12.9 (17.7)) compared with victims of short-lived harassment (5.2 (10.6); t=5.5, d.f.=426, P=0.001).
Relationship between psychiatric morbidity and recency of victimisation
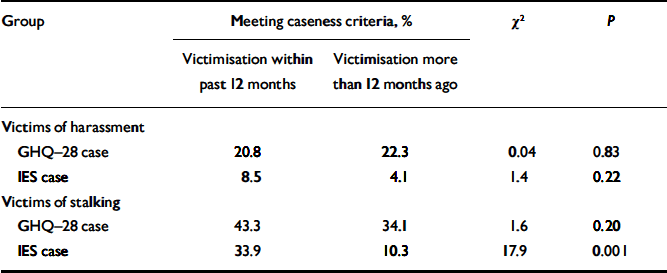
To examine whether victimisation is associated with acute or chronic disturbance, the proportion of victims meeting the criteria for caseness on the GHQ–28 and IES was compared between those victimised in the 12 months prior to the survey and those whose victimisation occurred before that time (Table 3). The rates of psychiatric morbidity among victims of harassment did not differ according to the recency of the victimisation. Among the victims of stalking, post-traumatic symptoms were higher among those victimised in the 12 months prior to the survey, although the rates of general psychopathology did not differ.
Table 3 Relationship between psychiatric morbidity and the recency of victimisation
| Group | Meeting caseness criteria, % | χ2 | P | |
|---|---|---|---|---|
| Victimisation within past 12 months | Victimisation more than 12 months ago | |||
| Victims of harassment | ||||
| GHQ—28 case | 20.8 | 22.3 | 0.04 | 0.83 |
| IES case | 8.5 | 4.1 | 1.4 | 0.22 |
| Victims of stalking | ||||
| GHQ—28 case | 43.3 | 34.1 | 1.6 | 0.20 |
| IES case | 33.9 | 10.3 | 17.9 | 0.001 |
Relationship between psychiatric morbidity and nature of the harassment
The number of harassment methods experienced (range 1–9) did not correlate with total scores on the GHQ–28 or IES among victims of either brief harassment or stalking (in all cases r < 0.15, P > 0.01). Among victims of harassment, the proportion meeting the criteria for caseness on the GHQ–28 and IES did not differ according to whether they were exposed to explicit threats or physical assault. For victims of protracted stalking, those subjected to explicit threats were significantly more likely than non-threatened victims to be classified as a case on the IES (27.2 v. 9.0%; OR=3.6, 95% CI 1.7–7.6, P=0.001). Post-traumatic symptoms were also elevated among victims of stalking who were assaulted in comparison with their non-assaulted counterparts (25.0 v. 13.6%), although this failed to reach statistical significance (χ2=4.07, P=0.04). The proportion of victims of stalking meeting the criteria for caseness on the GHQ–28 did not differ according to exposure to threats or assault.
The nature of the prior relationship between victim and perpetrator
Associations between the nature of the prior relationship with the perpetrator and rates of caseness morbidity on the GHQ–28 and IES were examined for the victims of stalking. For these victims, the perpetrator was a stranger in 17.5% of cases, an ex-intimate partner in 21.4%, a casual acquaintance in 30.3%, an estranged relative or friend in 8.5%, or a work contact in 22.2% of cases. There was no association between the nature of the prior relationship to the stalker and morbidity on either the GHQ–28 (χ=2.6, d.f.=4, P=0.62) or IES (χ2=6.4, d.f.=4, P 0.16), suggesting that psychopathology in victims of stalking is largely independent of who engages in the pursuit.
DISCUSSION
Unlike many crimes that involve relatively discrete or circumscribed events (e.g. rape, robbery), stalking is characterised by repeated and often prolonged victimisation. The stalkers’ ongoing intrusions represent a loss of control for the victims, many of whom feel that they live in a state of constant threat or siege (Reference Hall and MeloyHall, 1998). The results of this study demonstrate a significant association between reported victimisation and current psychiatric disturbance. Over a third of those exposed to protracted stalking reported elevated levels of psychiatric morbidity and almost one in five reported significant post-traumatic symptomatology. Importantly, the levels of psychopathology observed in this study were among a randomly selected community sample, as opposed to victims seeking assistance to manage the stalking or associated psychiatric difficulties.
The impact of persistent stalking: general psychiatric morbidity
Those who reported being victims of stalking had high levels of anxiety and depression, as evidenced by their scores on the GHQ–28. Approximately 10% of victims acknowledged recent suicidal ideation, with one in eight having strongly considered the possibility of taking their own life in the month prior to the survey. This finding alone is disquieting and underscores the need for greater clinical recognition of the desperation that may accompany such persistent forms of pursuit and victimisation.
The rates of general psychiatric morbidity among the victims of stalking were not associated with the methods of pursuit, the prior relationship with the perpetrator or the experience of threats and violence. The nature of the victimisation therefore contributed little to the rates of anxiety and depressive symptomatology. Interestingly, the recency of the stalking also failed to moderate the levels of general psychiatric distress, with an equivalent proportion of victims stalked in the 12 months prior to the study meeting the threshold for caseness on the GHQ–28 as those stalked more than a year earlier (43 and 34%, respectively).
Reports of high levels of anxiety and depression by a third of victims long after the stalking had ended emphasise the chronic course of impairment that can accompany such victimisation. Persistent anxiety appears the most common legacy of stalking (Reference Pathé and MullenPathé & Mullen, 1997; Reference Kamphuis and EmmelkampKamphuis & Emmelkamp, 2001). Faced with repeated intrusions over which they have little control, victims often come to perceive the world as inherently dangerous and their safety and well-being wholly compromised. In this context, hypervigilance, panic and insomnia are not unexpected. Pervasive symptoms of depression may also emerge among those whose sense of autonomy has been eroded by the stalking and who perceive their quality of life as having been irreversibly altered. It is critical that victims of stalking receive appropriate assistance both to end the intrusions and to relieve potentially enduring symptoms of anxiety and depression.
Post-traumatic morbidity
Some 16% of victims of stalking reported elevated scores on the IES, indicating significant avoidance and re-experiencing phenomena associated with their victimisation. Unlike the rates of general psychiatric morbidity, the levels of post-traumatic psychopathology differed according to the recency of victimisation, with a higher proportion of victims stalked in the year prior to the survey meeting the threshold for caseness than those whose stalking ended more than a year earlier. These findings suggest that although symptoms of anxiety and depression often persist, the severity of intrusive reminders and restrictive avoidance behaviours are for most victims likely to diminish over time.
The rates of post-traumatic symptomatology varied according to the nature of the stalking, with those exposed to associated violence more likely to meet the criteria for caseness on the IES. Specifically, victims who had been threatened by the perpetrator were three times more likely than their non-threatened counterparts to report significant post-trauma symptoms. However, actual physical assaults failed to moderate the levels of post-traumatic symptomatology. This suggests that threats may be more emotionally damaging to victims than the reality of physical harm. Although perhaps counter to expectations, this is in accordance with Pathé & Mullen's (Reference Pathé and Mullen1997) earlier observation that several victims in their clinical study felt they may have coped better with ‘the more tangible damage of physical assault’ (p. 15) than the sense of looming vulnerability that accompanies threats.
It should be noted that the rates of post-traumatic symptomatology in this community sample are considerably lower than those observed in clinical settings. Pathé & Mullen (Reference Pathé and Mullen1997) reported that over 30% of the victims in their sample met the full diagnostic criteria for post-traumatic stress disorder, with an additional 20% meeting all the conditions except criterion A (i.e. an actual threat to one's physical integrity). Kamphuis & Emmelkamp (Reference Kamphuis and Emmelkamp2001) similarly reported high levels of post-traumatic psychopathology in their Dutch sample of female victims of stalking seeking assistance from an anti-stalking foundation. Although the average total IES score in the Dutch study was three times higher than that reported here (mean=39.7, s.d.=17.0), victims in that study were predominantly stalked by ex-intimates (73%) and subjected to high levels of threats (74%) and violence (55%) (Reference Kamphuis and EmmelkampKamphuis & Emmelkamp, 2001). These factors likely contributed to the substantial levels of reported distress. None the less, the results from this community sample suggest that significant post-traumatic reactions affect a minority of victims, particularly in the immediate period post-victimisation and in the context of threats of violence.
The effects of short-lived harassment
The behaviours associated with stalking overlap with other experiences which, however unwelcome and unsettling, are relatively common (e.g. repeated ‘prank’ telephone calls or being followed in the street). In this study, the proportion of participants meeting the criteria for caseness on the GHQ–28 was equivalent between those exposed to such brief bursts of harassment and controls not experiencing harassment. This is not to say that those experiencing short-lived harassment have no ill-effects. Such conduct creates fear and apprehension and may precipitate in some cases a sense of vulnerability or a preoccupation with safety. None the less, this form of harassment is not associated with the longer-term emotional disturbance that can accompany protracted stalking, which highlights the importance of early intervention to avert persistent psychiatric morbidity.
Limitations
There are several limitations of the current study which may limit the generalisability of the results. We utilised a single questionnaire in which enquiries regarding the experience of harassment were included alongside questions about current general health. It cannot be discounted that this approach influenced the levels of psychiatric morbidity observed. This is unlikely, however, as the results demonstrated a dissociation in the rates of psychopathology. Only those victims who disclosed a protracted episode of pursuit reported elevated rates of psychiatric morbidity. Victims who reported a brief burst of intrusiveness did not differ from matched controls in their levels of psychopathology. This dissociation would not be expected if victims of harassment perceived an imperative to report a decline in their current general health in conjunction with their victimisation.
In addition, although a significant proportion of stalking victims reported psychological difficulties, the majority did not. Even among those stalked in the year prior to the survey, more than half did not report elevated levels of psychopathology. It is likely that other factors unrelated to stalking contribute to resilience or vulnerability to psychological impairment in this group, for example the availability of social support, the adequacy of coping resources or the experience of other forms of violence, such as childhood abuse or domestic violence. This study did not consider the extent to which variance in psychopathology is accounted for by factors unrelated to stalking, an issue that remains pertinent to future research.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Stalking that extends beyond a threshold of 2 weeks is associated with higher rates of persistent anxiety, depression and post-traumatic symptoms.
-
▪ A significant minority of victims of stalking consider suicide as a means of relieving their ongoing harassment and distress.
-
▪ Early intervention is critical to bringing stalking to an end and circumventing the development of serious and persistent psychiatric morbidity.
LIMITATIONS
-
▪ Additional variables that may mediate psychopathology among victims of stalking were not considered.
-
▪ As marital status could not be controlled between groups, the possibility remains that increased rates of psychopathology among victims of stalking may be associated with higher rates of separation and divorce.
-
▪ The study used brief screening measures to assess rates of psychopathology.
Acknowledgements
R.P. is the recipient of an Australian Postgraduate Award from the Australian Federal Government.





eLetters
No eLetters have been published for this article.