Introduction
The presence of recent stressful life events (SLEs) has been associated with the etiology of psychosis (Brown & Birley, Reference Brown and Birley1968). Meta-analytic evidence suggests that individuals with psychosis are three times more likely to have experienced SLEs prior to onset as compared to healthy controls (HC) (Beards et al., Reference Beards, Gayer-Anderson, Borges, Dewey, Fisher and Morgan2013), and that SLEs are associated with psychotic relapse (Martland, Martland, Cullen, & Bhattacharyya, Reference Martland, Martland, Cullen and Bhattacharyya2020). However, it is unclear whether SLEs contribute toward an individual becoming vulnerable to psychosis or is associated with transition to psychosis. This question could be addressed by studying recent SLEs in individuals at clinical high risk (CHR) for psychosis over time, to determine whether there are any associations between SLEs and their clinical outcomes. CHR individuals are identified as experiencing subclinical or intermittent psychotic symptoms, or as having a familial vulnerability to psychosis, defined as a recent deterioration in functioning and family history of psychosis or schizotypal personality disorder (Yung et al., Reference Yung, Yuen, McGorry, Phillips, Kelly, Dell'Olio and Buckby2005). To date, a small number of studies have examined recent SLEs in CHR samples and results have been inconsistent. Some studies found CHR individuals reported more recent SLEs than HC (Huang et al., Reference Huang, Hou, Huang, He, Wang, Chen and Jia2019; Munoz-Samons et al., Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021), while other studies did not (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013; Mason et al., Reference Mason, Startup, Halpin, Schall, Conrad and Carr2004; Phillips, Edwards, McMurray, & Francey, Reference Phillips, Edwards, McMurray and Francey2012). Findings are also inconclusive as to whether recent SLEs exacerbate symptoms or result in poorer psychosocial function in CHR individuals. Two studies reported a higher incidence of recent SLEs was associated with higher symptom severity and lower functioning (Huang et al., Reference Huang, Hou, Huang, He, Wang, Chen and Jia2019; Munoz-Samons et al., Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021), while one study found no association (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013). Most of these studies were cross-sectional and could not examine the temporal relationship between SLEs and clinical outcomes (Huang et al., Reference Huang, Hou, Huang, He, Wang, Chen and Jia2019; Munoz-Samons et al., Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021; Phillips et al., Reference Phillips, Edwards, McMurray and Francey2012; Thompson et al., Reference Thompson, Phillips, Komesaroff, Yuen, Wood, Pantelis and McGorry2007), and studies that analyzed longitudinal data employed smaller sample sizes which may have reduced their statistical power (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013; Mason et al., Reference Mason, Startup, Halpin, Schall, Conrad and Carr2004). As noted by Mayo et al. (Reference Mayo, Corey, Kelly, Yohannes, Youngquist, Stuart and Loewy2017), these inconsistencies in findings encourage further research efforts to understand the relationship between recent SLEs and the CHR state.
An important consideration is that CHR individuals may experience more SLEs due to their subthreshold symptoms. For example, the break-up of a relationship could be due to increasing social withdrawal. To clarify this, studies have examined independent events, which are events unlikely to be brought about by an individual's mental state (e.g. death of a loved one), and found evidence of patients reporting more independent SLEs prior to psychosis onset (Beards et al., Reference Beards, Fisher, Gayer-Anderson, Hubbard, Reininghaus, Craig and Morgan2020; Raune, Kuipers, & Bebbington, Reference Raune, Kuipers and Bebbington2011). Previous work has also found that interpersonal events involving conflict with someone else were more prevalent in patients with psychosis as compared to controls (Mansueto & Faravelli, Reference Mansueto and Faravelli2017). By considering independent and interpersonal events, we can explore whether the increased prevalence of SLEs in CHR individuals is solely attributable to their mental state.
The current study sought to address these questions by investigating the associations between recent SLEs and clinical outcomes within a CHR sample using a large longitudinal dataset from the European Network of National Schizophrenia Networks Studying Gene-Environment Interactions (EU-GEI) High-Risk study (van Os et al., Reference van Os, Rutten, Myin-Germeys, Delespaul, Viechtbauer, van Zelst and Mirjanic2014). Participants were recruited across Europe, Australia, and South America, ensuring geographical diversity capturing cultural and environmental contexts. We adopted two approaches: (1) group comparisons of recent SLEs at baseline between CHR and HC, and between CHR individuals who subsequently transitioned to psychosis (CHR-T) and those who did not (CHR-NT); and (2) a longitudinal analysis to investigate the impact of recent SLEs on the trajectory of changes in functioning and symptom severity within the CHR group. We hypothesized CHR individuals would report more SLEs than HC, and CHR-T would report more SLEs than CHR-NT at baseline. We also predicted that SLEs would negatively affect the trajectory of functioning, positive symptoms, and negative symptoms within the CHR group. We expected these associations would remain evident when considering independent SLEs, but not with interpersonal events, demonstrating that SLEs contribute to the CHR state independent of an individual's mental state.
Exploratory analyses considered the effects of childhood trauma and cannabis use as potential confounders. Childhood adversity is a risk factor for mental health disorders (Haidl et al., Reference Haidl, Hedderich, Rosen, Kaiser, Seves, Lichtenstein and Koutsouleris2023), and may compound the effects of SLEs experienced in adulthood as a pathway to psychosis (Betz et al., Reference Betz, Penzel, Kambeitz-Ilankovic, Rosen, Chisholm and Stainton2020; Mansueto & Faravelli, Reference Mansueto and Faravelli2017; Morgan et al., Reference Morgan, Reininghaus, Fearon, Hutchinson, Morgan, Dazzan and Craig2014). Cannabis use is associated with a higher risk of psychosis onset (Marconi, Di Forti, Lewis, Murray, & Vassos, Reference Marconi, Di Forti, Lewis, Murray and Vassos2016), and it has been suggested cannabis may amplify the stress response (Arranz et al., Reference Arranz, Monferrer, Jose Algora, Cabezas, Sole, Vilella and Sanchez-Gistau2018). Previous work is limited in this regard, where none of the previously mentioned CHR studies adjusted for childhood trauma or cannabis use in their analyses.
Methods
Participants
The EU-GEI High Risk study is a multicenter, naturalistic prospective study (van Os et al., Reference van Os, Rutten, Myin-Germeys, Delespaul, Viechtbauer, van Zelst and Mirjanic2014). In the current study, we used a subset of participants of 331 CHR and 67 HC for which recent SLE data were available. CHR participants were recruited from early detection centers across 11 sites: London, Amsterdam, The Hague, Basel, Cologne, Melbourne, Vienna, Copenhagen, Paris, Barcelona, and São Paolo. HC participants were recruited from four sites: London, Melbourne, Amsterdam, and The Hague. The age range of participants was 14–45 years. Ethical approval was obtained locally at each site, and participants who agreed to take part in the study provided informed, written consent.
CHR participants were eligible if they met at least one of the high-risk criteria as defined by the Comprehensive Assessment of At-Risk Mental States (CAARMS) (Yung et al., Reference Yung, Yuen, McGorry, Phillips, Kelly, Dell'Olio and Buckby2005): Vulnerability Group, Attenuated Psychotic Symptoms, or Brief Limited Psychotic Symptoms. The exclusion criteria for all participants were: (1) current or previous diagnosis of a psychotic disorder as determined by CAARMS or the Structured Clinical Interview for DSM-IV Disorders (SCID-IV) (First & Gibbon, Reference First, Gibbon, Hilsesnroth and Segal2004); (2) current or previous neurological disorder; (3) symptoms explained by substance use or dependency; (4) estimated IQ < 60; or (5) unwillingness to provide blood or saliva samples. HC participants were excluded if they met any of the CHR criteria.
Design
The EU-GEI High Risk study followed participants over a 2-year period and conducted structured in-person assessments at three timepoints: baseline, 12-months, and 24-months (Hedges et al., Reference Hedges, Dickson, Tognin, Modinos, Antoniades, van der Gaag and Kempton2022). During the study, five sites (London, Amsterdam, The Hague, Paris, and São Paulo) were able to expand data collection to include an additional 6-month follow-up. While every effort was made to assess participants at regular time intervals, there were instances where the follow-up assessments did not align with the targeted follow-up date. In total, 98% of observations were completed within 2.5 years from baseline, but to collect as much data as possible, several assessments were administered beyond 2.5 years, but no more than 4 years, after baseline. The statistical model (linear mixed model [LMM]) used in the present study accounted for different follow-up times, enabling us to retain as much participant data as possible.
At each follow-up, CHR participants were re-assessed using CAARMS to determine if they had transitioned to psychosis and subsequently categorized into CHR-T or CHR-NT. When participants did not return for their follow-up assessments, clinical records were used, where available, to determine their transition status. For the present study, we focused on CHR participants prior to transition and the small number of post-transition assessments have not been included. Assessments were performed by trained raters, as previously reported in Hedges et al. (Reference Hedges, Dickson, Tognin, Modinos, Antoniades, van der Gaag and Kempton2022).
Measures
At each visit, participants were assessed on a suite of social, clinical, neuroimaging, and blood measures (van Os et al., Reference van Os, Rutten, Myin-Germeys, Delespaul, Viechtbauer, van Zelst and Mirjanic2014). The instruments and measures described below are relevant to the current study, with additional information included in the online Supplementary material.
Sociodemographic and clinical data
The Medical Research Council Sociodemographic Schedule (Mallett, Reference Mallett1997) was used to collect baseline demographic information. Socioeconomic status (SES) was defined by a participant's father's socioeconomic class at the time of their birth and categorized into three classes: salariat, intermediate, and working-class (Hedges et al., Reference Hedges, Dickson, Tognin, Modinos, Antoniades, van der Gaag and Kempton2022). Current cannabis use was assessed using the modified Cannabis Experiences Questionnaire (Di Forti et al., Reference Di Forti, Quattrone, Freeman, Tripoli, Gayer-Anderson, Quigley and van der Ven2019) and baseline data were dichotomized into current users and non-users. The Childhood Trauma Questionnaire (CTQ) (Bernstein et al., Reference Bernstein, Stein, Newcomb, Walker, Pogge, Ahluvalia and Zule2003) was used to assess childhood adversity before the age of 17, and measured using the total CTQ score. Participants' antipsychotic and antidepressant medication use, dosage and length of use were also recorded at baseline in a structured interview. Further details on the treatment of these variables are reported in the online Supplementary material.
Recent stressful life events
Recent SLEs were counted as an event that occurred over a period of 12 months prior to the day of the assessment. The List of Threatening Experiences (LTE) questionnaire (Brugha, Bebbington, Tennant, & Hurry, Reference Brugha, Bebbington, Tennant and Hurry1985) was used to gather recent SLE data and was administered at baseline and at each subsequent follow-up. The 12-item questionnaire covers major categories of life events such as serious illness and injury or significant loss, and has demonstrated a high test-retest reliability (Brugha & Cragg, Reference Brugha and Cragg1990). A total LTE score for each assessment was calculated by summing the number of events experienced within the prior 12-month period. We calculated independent and interpersonal LTE scores using a subset of items from the LTE questionnaire (denoted in online Supplementary Table S1), as seen in previous studies (Park et al., Reference Park, Hatim, Si, Jeon, Srisurapanont, Bautista and Hong2015; Powers, Gleason, & Oltmanns, Reference Powers, Gleason and Oltmanns2013).
Outcome measures
Global functioning was assessed using Global Assessment of Functioning (GAF) (Hall, Reference Hall1995) split into disability and symptoms subscales (Hedges et al., Reference Hedges, Dickson, Tognin, Modinos, Antoniades, van der Gaag and Kempton2022). The GAF disability subscale is similar to the established Social and Occupational Functioning Assessment Scale (Goldman, Skodol, & Lave, Reference Goldman, Skodol and Lave1992). For the present study, GAF disability was used to measure functioning where scores ranged from 0 to 100, with higher scores indicating superior functioning.
Positive prodromal symptoms were measured using the CAARMS positive symptoms subscale by summing severity ratings for a maximum total score of 24. Negative symptoms were measured using the Scale for the Assessment of Negative Symptoms (SANS) (Andreasen, Reference Andreasen1982; Reference Andreasen1983) by summing ratings for a maximum total score of 125.
Complete observations were used in the analyses, except for childhood trauma and SANS scores, where missing items were imputed as described in the online Supplementary material.
Statistical analysis
All analyses were performed in R version 4.3.1. The statistical significance level was set at p < 0.05 (two-tailed).
Baseline analysis
The baseline characteristics of CHR and HC participants, and CHR-T and CHR-NT participants were compared using independent sample t tests, χ2 tests, or Fisher's exact tests as appropriate. Recent SLEs were compared across groups (CHR v. HC and CHR-T v. CHR-NT) using separate bootstrapped multiple linear regression models where LTE score was set as the dependent variable and group as the main independent variable. The comparison between CHR and HC groups was restricted to participants from sites that recruited both CHR and HC individuals. We also fit separate models including childhood trauma and cannabis use as covariates to test for any changes to the significance of our results. As the proportions across ethnicity were found to be significantly different between CHR and HC groups (Table 1), an additional sensitivity analysis was conducted to include ethnicity as a covariate of no interest. In comparing CHR-T and CHR-NT, we performed separate sensitivity analyses to control for antipsychotic and antidepressant medication use, dosage, and length of use, as psychotropic medication has been found to have some anti-stress properties (Sanson & Riva, Reference Sanson and Riva2020; Subramaniam, LoPilato, & Walker, Reference Subramaniam, LoPilato and Walker2019).
Baseline characteristics for the subset of participants from sites that recruited both CHR and HC individuals, used in the CHR v. HC comparison
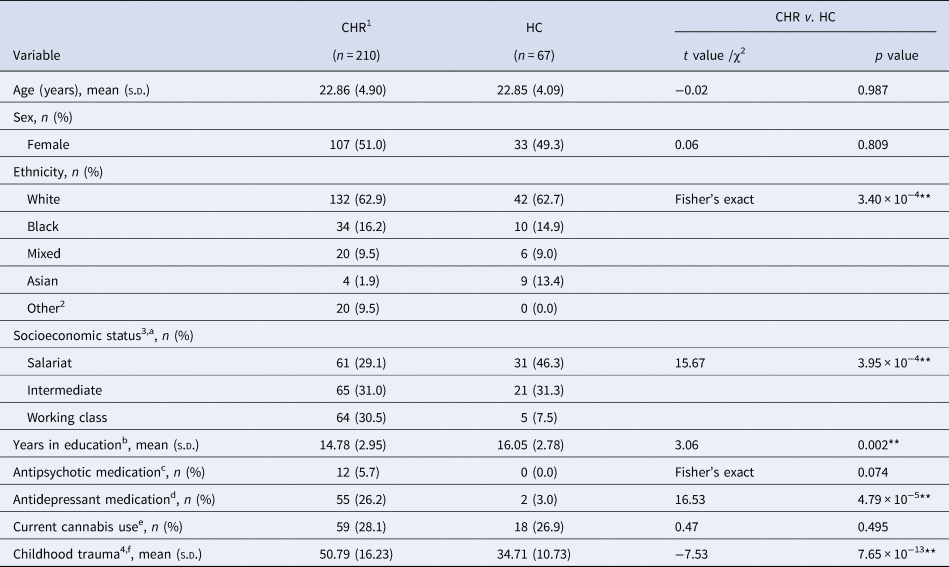
*p < 0.05; **p < 0.01.
Participants included in the present study have LTE data recorded for at least one timepoint.
1Only participants from sites that recruited both CHR and HC individuals were included. These sites were London, The Hague, Amsterdam, and Melbourne; 2other includes those of North African and other ethnic backgrounds; 3socioeconomic status is based on the father's socioeconomic class at participant's birth; 4Childhood Trauma Questionnaire total score.
CHR, clinical high risk; HC, healthy controls.
Data missing for: a20 CHR and 10 HC; b7CHR and 1 HC; c11 CHR and 8 HC; d55 CHR and 8 HC; e47 CHR and 24 HC; f4 CHR and 1 HC.
Longitudinal analysis
The association between recent SLEs and functioning, positive symptoms, and negative symptoms were analyzed using LMMs, using the R package lme4 (Bates, Mächler, Bolker, & Walker, Reference Bates, Mächler, Bolker and Walker2015). LMMs include fixed and random effects, accounting for repeated measurements within each participant. LMMs do not require data to be measured at consistent time intervals, and can accommodate missing data (Detry & Ma, Reference Detry and Ma2016). In the present study, we modeled a multi-level structure with participants nested in site as a random intercept. There were 11 sites, and the number of participants were dependent on the available data for each model, as observations with missing data were excluded. The longitudinal analyses were conducted only within the CHR group as the HC group was expected to exhibit little change in functioning and symptom scores over the 2-year follow-up.
Separate LMMs were fitted for each outcome measure with GAF disability, CAARMS positive symptom score, and SANS negative symptom score as the dependent variables. First, base models were fitted with LTE score and time (measured in years from baseline) as fixed effects to test for associations with the outcome measures. A second model (the ‘interaction model’) included the interaction term of LTE score × time to examine the effect of LTE score on the trajectory of the outcome measure over time. The analysis was repeated with independent and interpersonal LTE scores. LTE data from baseline and all follow-up assessments were used in each model. All models were fitted using restricted maximum likelihood estimation and adjusted for sex, age at baseline, and SES.
We also explored for the potential effects of childhood trauma and cannabis use on our longitudinal results by refitting the base models separately with total CTQ score and current cannabis use as additional covariates. Sensitivity analyses were conducted to include baseline antipsychotic and antidepressant medication use as dichotomous covariates of no interest, as well as antipsychotic and antidepressant medication dose equivalents and length of use (as detailed in the online Supplementary material).
To adjust for multiple comparisons, we used a 5% false discovery rate correction (Benjamini & Hochberg, Reference Benjamini and Hochberg1995) inclusive of all models (59 p values). The p values reported in the results section for the baseline and longitudinal models are uncorrected, with a superscript indicating whether significant p values had passed correction.
There is some concern that the loss of participants over a longitudinal study can introduce a form of attrition bias as participants who continue with a study may be associated with particular characteristics (Fewtrell et al., Reference Fewtrell, Kennedy, Singhal, Martin, Ness, Hadders-Algra and Lucas2008). To investigate this, we grouped CHR participants by the number of completed assessments and compared baseline characteristics across groups using one-way ANOVA, χ2, and Fisher's exact tests as appropriate. To clarify, participants who completed one assessment were compared against participants who completed two, three, or four assessments in total.
Results
Sample characteristics
The current study used 331 CHR and 67 HC participants who had recent SLE data recorded for at least one timepoint. Baseline characteristics for the subset of participants (from four sites that recruited both CHR and HC individuals) used in the CHR v. HC comparison are reported in Table 1. There were significant differences in ethnicity, with the HC group comprising of more participants from Asian and Other (inclusive of North African) ethnic backgrounds, and SES, where the HC group had a higher proportion of individuals from salariat class backgrounds and the CHR group had more individuals from working class backgrounds. In comparison to HC, CHR participants also spent fewer years in education, had experienced more childhood trauma, and a higher proportion were taking antidepressant medication at baseline. The study accepted HC participants who had non-psychotic morbidities and in the current study 11 (16.4%) participants reported having a previous or current major depressive disorder, four (6.0%) an anxiety disorder, and one (1.5%) an eating disorder at baseline, as identified using the SCID-IV (First & Gibbon, Reference First, Gibbon, Hilsesnroth and Segal2004).
The baseline characteristics for the CHR group, further split into CHR-T and CHR-NT are reported in Table 2. There was only a significant difference in baseline antipsychotic medication where the CHR-T group reported higher use than the CHR-NT group.
Baseline characteristics of CHR participants, further split into CHR-T and CHR-NT
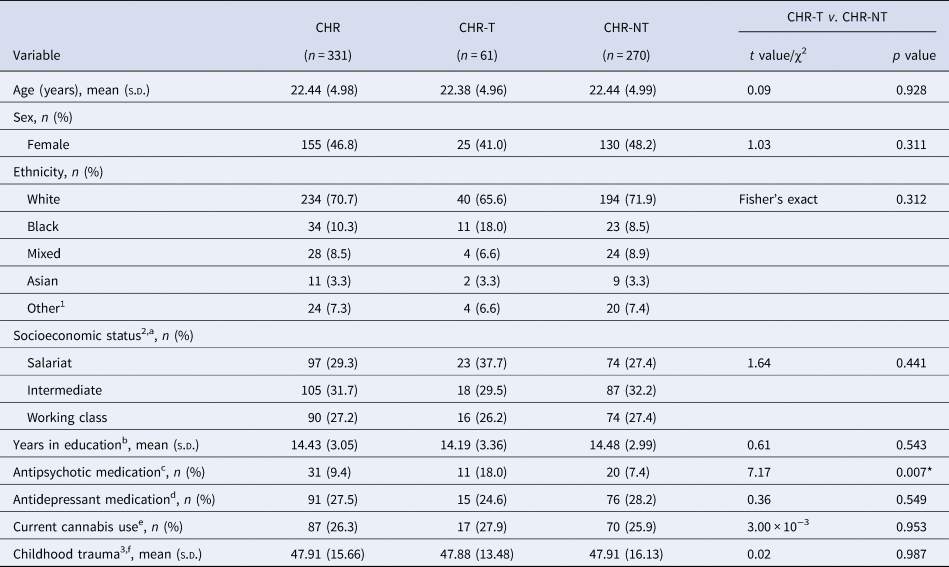
*p < 0.05.
Participants included in the present study have LTE data recorded for at least one timepoint.
1Other includes those of North African and other ethnic backgrounds; 2socioeconomic status is based on the father's socioeconomic class at participant's birth; 3Childhood Trauma Questionnaire total score.
CHR, clinical high risk; CHR-T, CHR who transitioned to psychosis; CHR-NT, CHR who did not transition to psychosis.
Data missing for: a39 CHR; b31 CHR; c25 CHR; d34 CHR; e88 CHR; f19 CHR.
At baseline, CHR individuals had mean scores of 55.39 (s.d. = 12.32) for GAF disability, 10.16 (3.97) for CAARMS positive symptoms subscale, and 20.99 (14.93) for SANS. Raw data scores for GAF disability, CAARMS, SANS, and total LTE plotted against time are presented in online Supplementary Figs S1–S4. The frequencies of the reported LTE items can be found in online Supplementary Table S1.
In total, 331 CHR individuals completed a total of 618 assessments in the study. Out of a maximum of four assessments, 152 (45.9%) participants completed one assessment, 82 (24.8%) completed two assessments, 86 (26.0%) completed three assessments, and 11 (3.3%) completed four assessments.
Group differences in recent SLEs at baseline
The results from the linear regression models comparing groups at baseline are reported in Table 3 with LTE score as the dependent variable and group status as the main independent variable. CHR participants reported significantly more total recent SLEs (M = 2.10, s.d. = 1.74) than HC (M = 1.15, s.d. = 1.06), and more interpersonal events (M = 0.63, s.d. = 0.72) than HC (M = 0.25, s.d. = 0.44). There was no significant difference between the number of independent events reported by CHR (M = 0.81, s.d. = 0.99) and HC (M = 0.70, s.d. = 0.82). The significance of the results did not change when we included ethnicity as a covariate of no interest.
Group differences in LTE score at baseline using multiple linear regression1 comparing CHR and HC individuals, and CHR individuals who transitioned to psychosis to those who did not
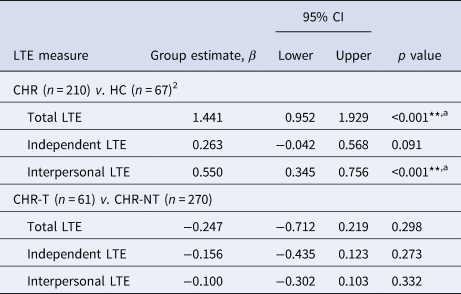
**p < 0.01; p values reported are uncorrected values. afindings survived false discovery rate correction for multiple comparisons.
LTE, list of threatening experiences; CHR, clinical high risk; HC, healthy controls; CHR-T, CHR who transitioned to psychosis; CHR-NT, CHR who did not transition to psychosis.
1All models were controlled for age at baseline, sex, socioeconomic status, and site; 2the analysis only included a subset of participants from four sites that recruited both CHR and HC individuals. Full results in online Supplementary Tables S2 and S3.
There were no significant differences in total SLEs between CHR-T (M = 1.93, s.d. = 1.47) and CHR-NT (M = 2.14, s.d. = 1.79), in independent events (CHR-T: M = 0.66, s.d. = 0.87; CHR-NT: M = 0.84, s.d. = 1.01), nor in interpersonal events (CHR-T: M = 0.59, s.d. = 0.62; CHR-NT: M = 0.63, s.d. = 0.74). When we included antipsychotic medication and antidepressant medication in sensitivity analyses as covariates of no interest, the significance of the results did not change.
The significance of the results from the group comparison did not change when we controlled for childhood trauma and current cannabis use. There was a significant association between CTQ score and total LTE in the model for CHR v. HC (β = 0.018, p = 0.012), and in the model for CHR-T v. CHR-NT (β = 0.019, p = 0.004), indicating participants who experienced more childhood trauma reported more recent SLEs regardless of group membership. Cannabis use was only significantly associated with total LTE score in the model comparing CHR-T v. CHR-NT (β = 0.528, p = 0.023), suggesting CHR participants who were cannabis users experienced more recent SLEs. The full results are reported in online Supplementary Tables S2 and S3.
The longitudinal association between recent SLEs and functioning, positive symptoms, and negative symptoms
The interaction term LTE score × time was not statistically significant across all models and therefore we report only the results from the base model for interpretation in Table 4. This includes the main effects of LTE score and time (measured in years from baseline) for each of the LMMs fitted with functioning, positive symptoms, and negative symptoms, as dependent variables. All models adjusted for sex, age at baseline, and SES. The predicted marginal effects of LTE score and time on functioning and symptom severity from the base model are presented in Fig. 1. The fixed-effects estimates for all models are reported in online Supplementary Tables S4–S6.
Estimates from the base model of the main fixed effects examining the association between recent stressful life events and functioning and symptom outcomes over the 2-year follow-up period within the CHR group1
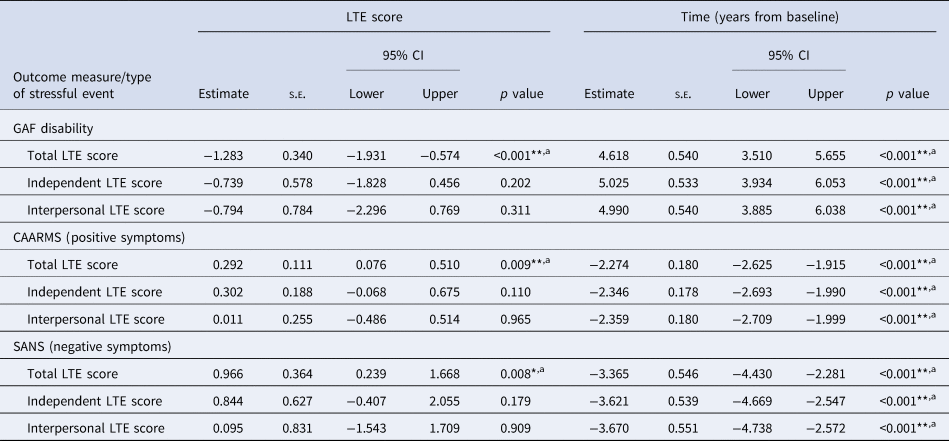
*p < 0.05; **p < 0.01; p values are uncorrected values. afindings survived false discovery rate correction for multiple comparisons.
LTE, List of Threatening Experiences; GAF, Global Assessment of Functioning; CAARMS, Assessment of At-Risk Mental State; SANS, Scale for the Assessment of Negative Symptoms.
1Models included participants nested in site (n = 11) as random intercepts. Number of participants used in each model varied due to missing data: GAF disability, n = 287; CAARMS, n = 290; SANS, n = 288. All models were controlled for sex, age at baseline, and socioeconomic status; Full results in online Supplementary Tables S5 and S6.
The predicted marginal effects of (i) time (measured in years from baseline) and (ii) Total List of Threatening Experiences (LTE) score on: (a) functioning as measured by the Global Assessment of Functioning (GAF) disability subscale; (b) positive symptom score measured by the Comprehensive Assessment of At-Risk Mental States (CAARMS) positive symptom severity subscale; and (c) negative symptom scores measured by the Scale for the Assessment of Negative Symptoms (SANS), using the linear mixed model estimates from the base model. The graphs show overall poorer functioning and more severe symptoms associated with a higher LTE score controlling for time, and an improvement in functioning and symptom scores over the course of the study. The grey band represents the 95% confidence interval. All models control for sex, age at baseline, and socioeconomic status, with participants nested in site modeled as random intercepts.
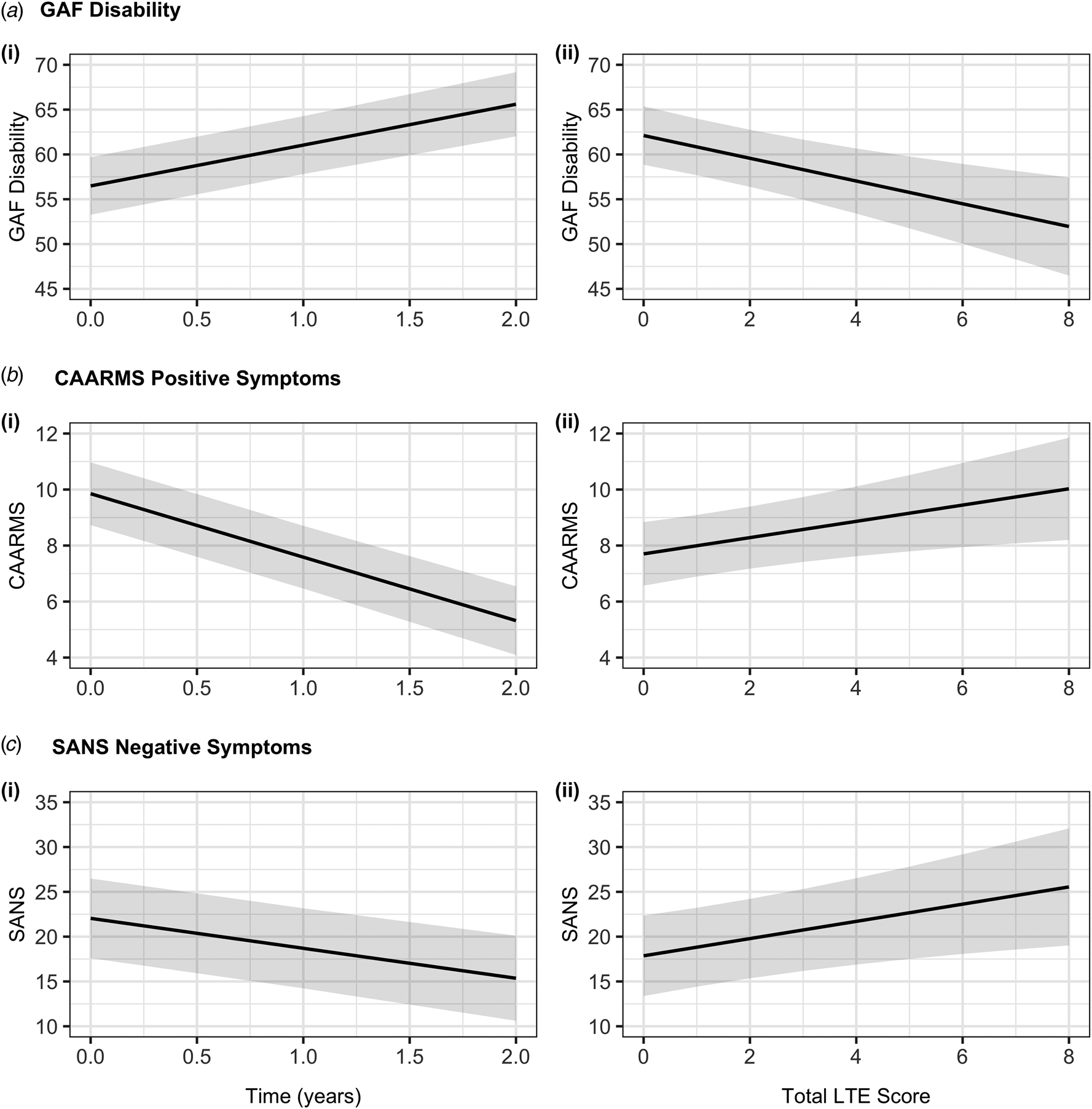
Total LTE score had a significant negative effect on GAF disability, where a higher occurrence of recent SLEs was associated with lower functioning when controlling for time. There was a significant effect of time, where functioning was found to improve over the study period (Table 4, Fig. 1a). The interaction term LTE score × time in the interaction model was not significant suggesting that recent SLEs did not impact the rate of improvement in functioning over the follow-up period (online Supplementary Table S4).
There was a significant positive association between total LTE score and both the CAARMS positive symptoms and SANS scores, meaning a higher occurrence of recent SLEs was associated with more severe positive and negative symptoms when controlling for time. There was a significant effect of time on both CAARMS and SANS scores, indicating symptom severity decreased over the course of the study (Table 4, Fig. 1b and 1c). There was no significant effect of the interaction term LTE score × time in the interaction model, suggesting recent SLEs did not affect the rate of change in symptom severity over the 2-year follow-up (online Supplementary Table S5 and S6).
There were no significant associations between independent or interpersonal events and functioning, positive symptoms, or negative symptoms.
Sensitivity analysis for the longitudinal data
There were no changes to the significance of the results for functioning, positive symptoms, or negative symptoms when we adjusted for baseline antipsychotic and antidepressant medication use, dosage and length of use, nor when we included childhood trauma as a covariate in each model. There were no significant associations between childhood trauma and functioning, positive symptoms, or negative symptoms (online Supplementary Tables S4b, S5b, and S6b).
When the base model was adjusted for current cannabis use, the significance of the results did not change for GAF disability (online Supplementary Table S4b), nor was there a significant main effect of cannabis use on functioning. However, the main effects of LTE score on positive symptoms and negative symptoms were no longer significant when controlling for cannabis use, and there was no significant main effect of cannabis use on either positive or negative symptoms (online Supplementary Tables S5b and S6b).
Participants were grouped by the number of completed assessments and baseline characteristics were compared to test for attrition bias, in line with recommended reporting requirements (Fewtrell et al., Reference Fewtrell, Kennedy, Singhal, Martin, Ness, Hadders-Algra and Lucas2008). There were significant differences across groups in the years spent in education (F (3,296) = 8.30, p < 0.001), CAARMS positive symptom scores (F (3,324) = 6.78, p < 0.001), ethnicity (Fisher's exact p = 0.020), and in baseline antipsychotic medication use (Fisher's exact p = 0.011) (online Supplementary Table S7).
Discussion
This is the largest longitudinal study to date investigating the effects of recent SLEs on functioning and symptom severity in individuals at CHR for psychosis. As hypothesized, we found CHR individuals reported more total recent SLEs and interpersonal SLEs than HCs at baseline. Contrary to our prediction, there was no significant difference in the number of SLEs reported by CHR-T individuals as compared to CHR-NT individuals, nor were there any differences in the number of independent and interpersonal SLEs between CHR-T and CHR-NT at baseline. Our final hypothesis was partially confirmed in our longitudinal analyses: recent SLEs were associated with lower functioning, and more severe positive and negative symptoms when controlling for time. However, while we observed an improvement in functioning and symptoms over the course of the study, recent SLEs did not affect the longitudinal trajectories of either of these outcome measures. The significance of our results did not change when we adjusted for childhood trauma, although when adjusting for cannabis use, we found SLEs were no longer significantly associated with positive or negative symptoms.
Our finding that CHR individuals reported more recent SLEs than HCs is consistent in previous studies that measured recent SLEs across 12 months (Huang et al., Reference Huang, Hou, Huang, He, Wang, Chen and Jia2019; Munoz-Samons et al., Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021), as has been done in the current study. Where our findings conflict with previous work, recent SLEs were measured over a shorter period of 1 (Phillips et al., Reference Phillips, Edwards, McMurray and Francey2012) and 3 months (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013). We found that CHR individuals did not report significantly more independent events than HC, suggesting that the higher prevalence of SLEs reported by CHR individuals could be a consequence of their subclinical symptoms. This is further supported by our findings that CHR individuals reported more interpersonal events than HCs, possibly driven by a heightened sensitivity to interpersonal issues (Georgiades et al., Reference Georgiades, Almuqrin, Rubinic, Mouhitzadeh, Tognin and Mechelli2023). It is also possible that interpersonal events themselves contribute to the CHR state as proposed in cognitive models, where the appraisal of interpersonal events results in negative schemas, leading to the development of psychosis (Lovatt, Mason, Brett, & Peters, Reference Lovatt, Mason, Brett and Peters2010).
Contrary to our hypothesis but similar to previous work (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013; Mason et al., Reference Mason, Startup, Halpin, Schall, Conrad and Carr2004), the number of SLEs did not differ between CHR-T and CHR-NT groups. However, given that CHR-T individuals transitioned at varying timepoints during study, there may not have been any discernible differences at baseline due to variation in the staging of psychosis progression within the CHR-T group. There were insufficient data in the current study to examine recent SLEs in the CHR-T group precipitating their transition date, which would be an important consideration in future studies. The CHR group is also highly variable and heterogeneous in terms of clinical presentation and is highly comorbid with other mental disorders (Solmi et al., Reference Solmi, Soardo, Kaur, Azis, Cabras, Censori and Fusar-Poli2023). It is estimated only approximately 20% of CHR individuals transition to psychosis after 2 years (Salazar de Pablo et al., Reference Salazar de Pablo, Davies, de Diego, Solmi, Shin, Carvalho and Fusar-Poli2021a, Reference Salazar de Pablo, Radua, Pereira, Bonoldi, Arienti, Besana and Fusar-Poli2021b). It is possible that recent SLEs are not directly associated with transition to psychosis, and instead may have a broader effect on the general psychopathology of CHR individuals. A network analysis by Betz et al. (Reference Betz, Penzel, Kambeitz-Ilankovic, Rosen, Chisholm and Stainton2020) found that recent SLEs were not directly linked to psychotic symptoms but were mediated by other symptoms such as depression and anxiety.
Poorer functioning and more severe positive and negative symptoms were associated with a higher incidence of recent SLEs overall, which supports findings by Munoz-Samons et al. (Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021), but differs from other CHR studies (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013; Thompson et al., Reference Thompson, Phillips, Komesaroff, Yuen, Wood, Pantelis and McGorry2007). This could be due to methodological differences in study design and analyses. For instance, Thompson et al. (Reference Thompson, Phillips, Komesaroff, Yuen, Wood, Pantelis and McGorry2007) was a cross-sectional study using correlational analysis, while the current study analyzed a larger, longitudinal dataset which would have increased statistical power.
The significance of results from the baseline comparison between CHR and HC individuals and the longitudinal findings did not change when we adjusted for childhood adversity, which suggests recent SLEs may have their own distinct contribution to the psychopathology of psychosis. We found that individuals who had experienced more childhood adversity reported more recent SLEs at baseline, irrespective of their group membership (CHR v. HC or CHR-T v. CHR-NT). As has been suggested by Morgan et al. (Reference Morgan, Reininghaus, Fearon, Hutchinson, Morgan, Dazzan and Craig2014), early adversity is more likely to lead to adult disadvantage, resulting in a higher incidence of SLEs. Our results further suggest SLEs may impact symptom outcomes via cannabis use, which has been previously proposed (Arranz et al., Reference Arranz, Monferrer, Jose Algora, Cabezas, Sole, Vilella and Sanchez-Gistau2018). There is evidence of a bi-directional effect between cannabis and stress, where stress is associated with higher cannabis use, and long-term cannabis use is associated with a blunted stress response, therefore affecting stress-related outcomes (al'Absi & Allen, Reference al'Absi and Allen2021; Glodosky, Cuttler, & McLaughlin, Reference Glodosky, Cuttler and McLaughlin2021). However, 88 participants were missing data on cannabis use and so the results should be interpreted with caution.
The CHR group exhibited an overall improvement in functioning and symptoms over time although their outcomes were still poorer than the HC group. This has previously been observed in studies examining outcomes in help-seeking CHR samples (Addington et al., Reference Addington, Cornblatt, Cadenhead, Cannon, McGlashan, Perkins and Heinssen2011; Brandizzi et al., Reference Brandizzi, Valmaggia, Byrne, Jones, Iwegbu, Badger and Fusar-Poli2015). However, contrary to our hypothesis, the trajectory of outcomes appeared to be unaffected by the occurrence of recent SLEs. We may posit that recent SLEs is a risk factor for an individual becoming CHR for psychosis, rather than having a significant influence over the progression of their clinical outcomes while in the CHR state. Previous work has found that individuals who were referred to early intervention psychosis services but did not meet the CHR criteria exhibited many overlapping risk factors (Reference Naughton, Brady, Geary, Counihan and Clarke2024). In addition, given that our sample comprised of individuals who contacted clinical services, treatment received during the study could have countered any deleterious effects of SLEs, although we found there were no changes to the significance of our results when controlling for antipsychotic and antidepressant medication.
It is possible that results were obscured by the heterogeneity of the CHR group, where previous studies have not only identified distinct subgroups of CHR individuals with differing trajectories of clinical outcomes (Allswede et al., Reference Allswede, Addington, Bearden, Cadenhead, Cornblatt, Mathalon and Cannon2020; Healey et al., Reference Healey, Penn, Perkins, Woods, Keefe and Addington2018), but also found different risk factors associated with the clinical staging of CHR individuals (Wigman, van der Tuin, van den Berg, Muller, & Booij, Reference Wigman, van der Tuin, van den Berg, Muller and Booij2023). Recent SLEs may therefore have a significant effect on the trajectory of clinical outcomes for a particular CHR subgroup but not another, and further work is required to clarify this.
We must also consider that stress is subjective to an individual, and that it may be the perceived experience that affects the trajectory of outcomes within the CHR state rather than the prevalence of events (Haidl et al., Reference Haidl, Rosen, Schultze-Lutter, Nieman, Eggers and Heinimaa2018). CHR individuals have been found to exhibit an impaired tolerance to stress associated with poorer outcomes (DeVylder et al., Reference DeVylder, Ben-David, Schobel, Kimhy, Malaspina and Corcoran2013; Munoz-Samons et al., Reference Munoz-Samons, Tor, Rodriguez-Pascual, Alvarez-Subiela, Sugranyes, de la Serna and Baeza2021), and they have reported higher levels of distress despite reporting fewer recent SLEs compared to HC (Kraan, Velthorst, Smit, de Haan, & van der Gaag, Reference Kraan, Velthorst, Smit, de Haan and van der Gaag2015). Future studies should consider incorporating subjective stress measures.
Limitations and strengths
As is commonly faced in retrospective studies, recent SLE and childhood adversity data are subject to recall bias, although previous work has demonstrated that memory biases appear to have minimal effect on the relationship between self-reported adversity and psychopathology, with retrospective data potentially being a more useful risk indicator (Fergusson, Horwood, & Boden, Reference Fergusson, Horwood and Boden2011; Newbury et al., Reference Newbury, Arseneault, Moffitt, Caspi, Danese, Baldwin and Fisher2018). The items in the LTE questionnaire may not have been appropriate for the age range of our study, where younger participants may not have had the same exposure to the type of life events included in the questionnaire such as the loss of a job, while experiences such as difficulties at school were not captured. The current study also did not record psychological treatment which could have meant changes in behavior or adaptive coping to improve resilience could have obscured results. This could be of interest in future work, given the associations with functioning and symptom severity, and potential protective factors (Mian, Lattanzi, & Tognin, Reference Mian, Lattanzi and Tognin2018; Stainton et al., Reference Stainton, Chisholm, Kaiser, Rosen, Upthegrove, Ruhrmann and Wood2019). Longitudinal data pertaining to antipsychotic and antidepressant medication use were unfortunately unavailable, which is a significant limitation of the study. We found there were some differences between participants based on how many assessments they had completed indicating potential attrition bias, which is a broader challenge in longitudinal studies (Fewtrell et al., Reference Fewtrell, Kennedy, Singhal, Martin, Ness, Hadders-Algra and Lucas2008; Homman, Smart, O'Neill, & MacCabe, Reference Homman, Smart, O'Neill and MacCabe2021). This may also affect our statistical analysis as LMMs assume data are missing at random.
The main strength of our study is in the use of a large dataset to examine the effect of recent SLEs on the trajectory of outcomes in CHR individuals over time. Using LMMs meant greater statistical power as the models took into account the variation between participants and site, used all observed datapoints, and adjusted for covariates of no interest. The EU-GEI High Risk study collected a wide range of social and environmental variables, which subsequently meant we could adjust for childhood trauma and cannabis use, which had not been done in previous CHR studies of recent SLEs. Further work is still required to understand recent SLEs as a risk factor for psychosis to determine when early intervention strategies seeking to mitigate against the effects of stress can be most effective.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291724003039
Funding statement
The European Network of National Schizophrenia Networks Studying Gene-Environment Interactions (EU-GEI) Project is funded by grant agreement HEALTH-F2-2010-241909 (Project EU-GEI) from the European Community's Seventh Framework Programme. C. See is supported by the UK Medical Research Council (MR/N013700/1) and King's College London member of the MRC Doctoral Training Partnership in Biomedical Sciences. Additional support was provided by a Medical Research Council Fellowship to M. Kempton (grant MR/J008915/1), and by the Ministerio de Ciencia, Innovación e Universidades (PSI2017-87512-C2-1-R) and the Generalitat de Catalunya (2017SGR1612) to N. Barrantes-Vidal. M. Kempton receives funding support from the National Institute for Health and Care Research (NIHR) Maudsley Biomedical Research Centre at South London and Maudsley NHS Foundation Trust and King's College London. E. Velthorst receives funding support from the National Institute for Mental Health (1R01MH128971-01A1). The views expressed are those of the authors and not necessarily those of the NIHR, or the Department of Health and Social Care. For the purposes of open access, the author has applied a Creative Commons Attribution (CC BY) license to any Accepted Author Manuscript version arising from this submission.
Competing interests
None.
EU-GEI High Risk Study group authors
Philip McGuire1,2, Sara Pisani1, Mathilde Antoniades3, Maria Calem1, Stefania Tognin1, Gemma Modinos4, Lieuwe de Haan5,6, Mark van der Gaag7,8, Eva Velthorst9, Tamar C. Kraan5, Daniella S. van Dam5, Nadine Burger8, Barnaby Nelson10, Patrick McGorry10, G. Paul Amminger10, Christos Pantelis11, Athena Politis10, Joanne Goodall10, Anita Riecher-Rössler12, Stefan Borgwardt12, Erich Studerus12, Rodrigo Bressan13, Ary Gadelha13, Elisa Brietzke14, Graccielle Asevedo13, Elson Asevedo13, Andre Zugman13, Neus Barrantes-Vidal15, Tecelli Domínguez-Martínez16, Anna Racioppi17, Thomas R. Kwapil18, Manel Monsonet17, Lídia Hinojosa17, Mathilde Kazes19, Claire Daban19, Julie Bourgin19, Olivier Gay19, Célia Mam-Lam-Fook19, Marie-Odile Krebs19, Dorte Nordholm20, Lasse Randers20, Kristine Krakauer20, Louise Glenthøj20, Birte Glenthøj21, Merete Nordentoft20, Stephan Ruhrmann22, Dominika Gebhard22, Julia Arnhold23, Joachim Klosterkötter22, Gabriele Sachs24, Iris Lasser24, Bernadette Winklbaur24, Philippe A. Delespaul25,26, Bart P. Rutten25, Jim van Os1,25
Affiliations:
1. Department of Psychosis Studies, Institute of Psychiatry, Psychology & Neuroscience, King's College London, De Crespigny Park, Denmark 458 Hill, London, United Kingdom SE5 8AF
2. Department of Psychiatry, University of Oxford, Oxford, United Kingdom
3. Department of Psychiatry, Icahn School of Medicine at Mount Sinai, 1425 Madison Ave, New York, NY 10029, United States
4. Department of Psychological Medicine, Institute of Psychiatry, Psychology & Neuroscience, King's College London, De Crespigny Park, Denmark 458 Hill, London, United Kingdom SE5 8AF
5. AMC, Academic Psychiatric Centre, Department Early Psychosis, Meibergdreef 5, 1105 AZ Amsterdam, The Netherlands
6. Arkin Amsterdam, The Netherlands
7. VU University, Faculty of Behavioural and Movement Sciences, Department of Clinical Psychology, van der Boechorststraat 7, 1081 BT Amsterdam, The Netherlands
8. Parnassia Psychiatric Institute, Department of Psychosis Research, Zoutkeetsingel 40, 2512 HN The Hague, The Netherlands
9. Department of Research, GGZ Noord-Holland-Noord, Heerhugowaard, The Netherlands
10. Centre for Youth Mental Health, University of Melbourne, 35 Poplar Road (Locked Bag 10), Parkville, Victoria 485 3052, Australia
11. Melbourne Neuropsychiatry Centre, University of Melbourne & Melbourne Health, Carlton South, VIC, Australia
12. University of Basel, Switzerland
13. LiNC – Lab Interdisciplinar Neurociências Clínicas, Depto Psiquiatria, Escola Paulista de Medicina, Universidade Federal de São Paulo – UNIFESP, Brazil
14. Depto Psiquiatria, Escola Paulista de Medicina, Universidade Federal de São Paulo – UNIFESP, Brazil
15. Departament de Psicologia Clínica i de la Salut (Universitat Autònoma de Barcelona), Spanish Mental Health Research Network (CIBERSAM), Spain
16. CONACYT-Dirección de Investigaciones Epidemiológicas y Psicosociales, Instituto Nacional de Psiquiatría Ramón de la Fuente Muñiz, México.
17. Departament de Psicologia Clínica i de la Salut (Universitat Autònoma de Barcelona), Spain
18. Department of Psychology, University of Illinois at Urbana-Champaign, USA
19. University Paris Descartes, Hôpital Sainte-Anne, C'JAAD, Service Hospitalo-Universitaire, Inserm U894, Institut de Psychiatrie (CNRS 3557) Paris, France
20. Mental Health Center Copenhagen and Center for Clinical Intervention and Neuropsychiatric Schizophrenia Research, CINS, Mental Health Center Glostrup, Mental Health Services in the Capital Region of Copenhagen, University of Copenhagen, Denmark
21. Centre for Neuropsychiatric Schizophrenia Research (CNSR) & Centre for Clinical Intervention and Neuropsychiatric Schizophrenia Research (CINS), Mental Health Centre Glostrup, University of Copenhagen, Glostrup, Denmark
22. Department of Psychiatry and Psychotherapy, Faculty of Medicine and University Hospital, University of Cologne, Cologne, Germany
23. Psyberlin, Berlin, Germany
24. Medical University of Vienna, Department of Psychiatry and Psychotherapy, Austria
25. Department of Psychiatry and Neuropsychology, School for Mental Health and Neuroscience, Maastricht University Medical Centre, P.O. Box 616, 6200 MD 464 Maastricht, The Netherlands
26. Mondriaan Mental health Trust, P.O. Box 4436 CX Heerlen, The Netherlands







