Dementia is a significant complication of late-life affective disorders (LLADs), and its association has been most extensively studied in late-life depression.Reference Stafford, Chung, Sommerlad, Kirkbride and Howard1 Depression is also the most common mental disorder in late life, affecting 2% of those over the age of 60,Reference Nichols, Szoeke, Vollset, Abbasi, Abd-Allah and Abdela2 and is projected to increase significantly by 2050.Reference Patterson3 Depression, especially in late life, has been associated with up to a two-fold increased risk for dementia.Reference Cherbuin, Kim and Anstey4–Reference Ly, Karim, Becker, Lopez, Anderson and Aizenstein6 The development of a LLAD, or the repeated relapse of a pre-existing illness, might accelerate biological ageing and promote earlier neurodegeneration, therefore increasing the risk of dementia. Alternatively, affective symptoms may herald the development of dementia as a psychological symptom that develops during a progressive and protracted period of cognitive decline.
The link between dementia and LLADs other than depression, including anxiety and bipolar affective disorder, is less well understood. Regarding anxiety disorders, a prior meta-analysis has suggested that anxiety disorders increase the risk of dementia, and a stronger association is evident for anxiety symptoms developing in later life. A second meta-analysis replicated the finding of an increased risk of dementia being associated with anxiety disorders in patients aged ∼60–80 years old.Reference Santabárbara, Lipnicki, Olaya, Villagrasa, Bueno-Notivol and Nuez7 However, there is heterogeneity across individual studies, with some not demonstrating a linkReference de Bruijn, Direk, Mirza, Hofman, Koudstaal and Tiemeier8 or highlighting that the increased risk is mediated by concurrent depressive symptoms.Reference Mortamais, Abdennour, Bergua, Tzourio, Berr and Gabelle9
A link between bipolar affective disorder and dementia dates as far back as 1913, when KraepelinReference Kraepelin10 wrote on the autopsy of a patient with bipolar disorder, noting widespread arteriosclerosis of blood vessels. However, there is marked variability in recent studies. A recent meta-analysis suggested psychotic disorders (including bipolar affective disorder) were associated with subsequent dementia, although evidence was ‘sparse’.Reference Stafford, Chung, Sommerlad, Kirkbride and Howard1 Some studies have found evidence of cognitive impairments that are worse with later onset of bipolar affective disorder,Reference Samamé, Martino and Strejilevich11 whereas others have suggested age and illness duration are negatively correlated with the degree of cognitive impairment.Reference Mann-Wrobel, Carreno and Dickinson12 Other studies still have emphasised that there is marked intra-individual short-term variability in cognitive impairmentsReference Depp, Savla, Moore, Palmer, Stricker and Lebowitz13 whereas some have identified similar age-related patterns of cognitive decline to healthy controls,Reference Delaloye, Moy, de Bilbao, Weber, Baudois and Haller14 suggesting that the disorder ‘does not have a significant adverse impact on cognitive and brain aging’.Reference Delaloye, Moy, de Bilbao, Weber, Baudois and Haller14
Previous work has tried to identify biomarkers and risk factors for LLADs (particularly depression) progressing to dementia. Poor antidepressant response,Reference Chang, Hayes, Perera, Broadbent, Fernandes and Lee15 disease phenotype, higher symptom burden,Reference Peakman, Karunatilake, Seynaeve, Perera, Aarsland and Stewart16 physical health measures such as hand-grip strengthReference Singh-Manoux, Dugravot, Fournier, Abell, Ebmeier and Kivimäki17 and genetic markersReference Huang, Wang, Tseng, Hung and Lin18 have all provided some insight but not enough to be clinically actionable. Furthermore, it remains unclear as to whether the biomarkers and risk factors differ across different LLADs.
No study to date has directly compared the risk of dementia progression across LLADs, nor determined the demographic and clinical features that might mediate differences in risk. This study aims to address this gap by leveraging electronic health records using a retrospective cohort design. Using late-life depression as a reference group with a well-established risk of dementia progression, we explore whether anxiety disorders and bipolar affective disorder similarly increase dementia risk. In addition, we aim to identify demographic- and illness-related characteristics that may modulate the risk of dementia progression in these disorders. By addressing these questions, this research seeks to refine our understanding of the relationship between LLADs and dementia, inform clinical risk stratification and guide interventions to mitigate the cognitive and functional decline associated with LLADs.
Method
Data source
The study cohort was generated using the Clinical Records Interactive Search (CRIS) resource.Reference Stewart, Soremekun, Perera, Broadbent, Callard and Denis19 CRIS was developed in 2008 to provide access to de-identified structured and open-text data extracted from the electronic health records system of the South London and Maudsley National Health Service Foundation Trust (SLaM). SLaM is one of Europe’s largest mental health and dementia care providers, serving the 1.4 million residents of four south London boroughs (Croydon, Lambeth, Lewisham and Southwark). CRIS records reflect the total secondary care mental health usage of this population, with the anonymised records of over 500 000 mental health and dementia patients. Records from primary care are not included.
CRIS has research ethical approval as an anonymised database for secondary analysis (Oxford Research Ethics Committee C, reference 23/SC/0257). Data are extracted from structured fields or free text (events, clinical correspondence), for which a wide range of natural language processing (NLP; ‘text-mining’) applications are used.Reference Cunningham, Tablan, Roberts and Bontcheva20 All NLP algorithms and their performance data are listed in an open-source online catalogue.21
Sample
To be included patients needed to have a diagnosis of one of the following affective disorders according to ICD-1022 criteria: bipolar affective disorder (F30 or F31), depressive disorder (F32 or F33) or anxiety disorder (F41). The diagnosis needed to be made between 1 January 2008 and 31 December 2022 and patients needed to be at least 60 years old at the time of diagnosis. The date of first recording of a LLAD served as index date for longitudinal analyses. If a patient had several LLAD diagnoses recorded at the time of diagnosis we prioritised bipolar affective disorder over anxiety disorder, and anxiety disorder over depressive disorder. Patients were excluded if a diagnosis of dementia was made before the LLAD diagnosis or within 3 months of the diagnosis, as this is the usual time frame in which memory services establish dementia diagnoses. Patients were considered to have a previous diagnosis of bipolar affective disorder, depression or anxiety disorder if such a diagnosis could be identified before the index date. Further, a patient was considered to have a previous diagnosis of depression if their diagnosis at index date was recurrent depressive disorder (ICD-10: F33).
Outcome
We ascertained whether a diagnosis of dementia according to ICD-10 criteria (F00–F03) was made in the follow-up period. Patients were followed up from the first affective disorder diagnosis (index date) to the first recording of a dementia diagnosis, their last attended appointment with a SLaM clinician or a census date on 17 March 2023. Patients were excluded if less than 3 months of follow-up was available.
Covariates and potential predictors of dementia development
Data were extracted on age at affective disorder diagnosis, gender, ethnicity (classified as White, Black, Asian, other) and a neighbourhood-level deprivation score (Index of Multiple Deprivation).Reference Noble, McLennan, Wilkinson, Whitworth, Exley and Barnes23 We also extracted the score of Health of the Nation Outcome Scales (HoNOS),Reference Burns, Beevor, Lelliott, Wing, Blakey and Orrell24 which are routinely used in UK mental health services. We used the following subscales as recorded closest to first affective disorder diagnosis: agitated behaviour, non-accidental self-injury (which includes suicidal ideation), drug/alcohol problems, hallucinations or delusions, depressed mood, physical illness or disability, cognitive problems, difficulties with activities of daily living (ADLs) and problems with social relationships. HoNOS items are rated from 0 (least severe status) to 4 (most severe status). For this analysis, we dichotomised the subscales and considered scores of 0–1 as the patient not experiencing problems in the domain, while scores of 2–4 indicated that problems were present. To measure physical health more accurately, the HoNOS physical illness or disability scale was divided in three categories: ‘no or minor’ (score 0–1), ‘mild’ (score 2) and ‘moderate to severe’ (score 3–4). HoNOS have been shown to be related to dementia risk in other CRIS cohorts.Reference Willmott, Martin West, Yung, Giri Shankar, Perera and Tsamakis25
Statistical analysis
Data were analysed using STATA software version 15 (Stata Corp LP, College Station, TX, USA, 2017; see https://www.stata.com/stata15/). First, we generated descriptive statistics comparing those with bipolar affective disorder in later life to those with depression in later life and comparing those with anxiety disorder in later life to those with depression in later life. Then we used adjusted and unadjusted Cox proportional hazard models to determine differences in dementia risk between bipolar affective disorder or anxiety disorder and depression. As a sensitivity analysis, we further compared those with bipolar affective disorder or anxiety disorder to those with late-onset depressive disorder (i.e. those without a prior history of depression). We then used the adjusted Cox proportional hazard model to determine predictors of dementia development in each of the three affective disorder groups. The adjusted models were adjusted for age at affective disorder diagnosis, age-squared, gender, ethnicity, marital status, deprivation, baseline cognition and time*cognition interaction. Adjusting for baseline cognition accounted for pre-existing cognitive differences that may confound the relationship between LLADs and dementia risk.
Using the test of Schoefield residuals we tested whether the proportional hazards assumption was met. This assumption was violated for the HoNOS cognitive problems and the HoNOS physical disabilities scales. Therefore, a time*cognition interaction and/or a time*physical illness interaction was included in the relevant analyses.
In the whole data-set 25% of patients had data on at least one covariate missing. Variables with missing data were deprivation, ethnicity, HoNOS scores and marital status. Therefore, we used the mi package in STATA to create 25 imputed data-sets, which were generated by replacing missing values with simulated values assembled from covariates and outcome values without missing data, as well as any additional prescribing information available.Reference Oudshoorn, van Buuren and van Rijckevorsel26 Rubin’s rulesReference Rubin27 were applied to combine coefficients in final analyses.
Results
We identified 11 192 patients with an affective disorder diagnosis after the age of 60 years. After removing 5947 patients as they developed dementia within 3 months (or before affective disorder diagnosis) or had less than 3 months of follow-up time available, the final sample consisted of 5695 patients. Of these 388 (6.8%) had a diagnosis of bipolar affective disorder, 1365 (24.0%) an anxiety disorder and 3942 (69.2%) a depressive disorder. In total 29.1% of patients with bipolar affective disorder had a prior history of the condition, 5.3% of patients with anxiety disorder had a prior history of an anxiety disorder and 30.3% of patients with depression had a prior history of depression.
Baseline characteristics
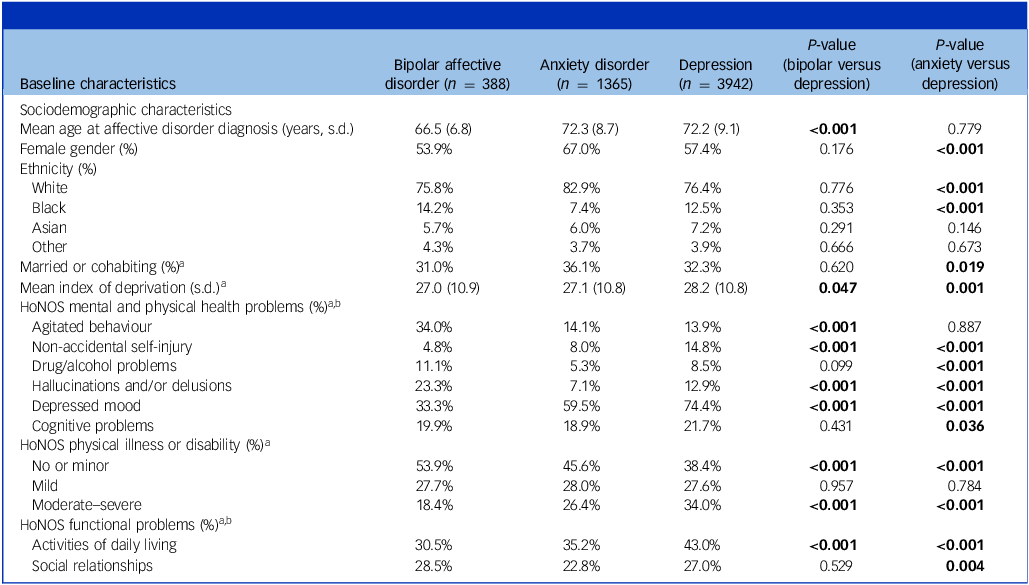
Characteristics at the time of first affective disorder diagnosis recording after the age of 60 years are presented in Table 1.
Baseline characteristics

HoNOS, Health of the Nation Outcome Scales. Bold indicates a significant P value at P = 0.05.
a. At the time of affective disorder diagnosis (±6 months).
b. Health of the Nation Outcome Scale 65+ (HoNOS65+) subscale scores 0–4 (0 = least severe, 4 = most severe status) were categorised into scores of 0–1, representing that the patient was not experiencing problems in that domain, and scores of 2–4, representing that the patient was experiencing problems. Values represent frequencies of patients scored as experiencing problems in that domain.
Bipolar affective disorder versus depression
Compared to those with depression, patients diagnosed with bipolar affective disorder were younger at the point of affective disorder diagnosis, from less deprived areas and a higher proportion presented with agitated behaviour or hallucinations and/or delusions. There were no significant differences in cognitive difficulties at bipolar/depression diagnosis. Patients with bipolar affective disorder less frequently presented with non-accidental self-injury (which includes suicidal ideation), depressed mood, moderate-to-severe physical health problems and problems with ADLs.
Anxiety versus depression
When compared to patients with depression, patients with anxiety disorders were at a similar age at the time of the affective disorder diagnosis, but were more frequently female, of White ethnicity, married and from less deprived areas. A lower proportion of patients with anxiety disorders were from a Black background, and fewer patients presented with agitated behaviour, drug/alcohol problems, hallucinations and/or delusions, depressed mood or cognitive problems. Patients with anxiety disorders less frequently had moderate–severe physical health problems or problems with ADLs or social relationships.
Risk of dementia
Of 388 patients with bipolar affective disorder, 29 (7.5%) developed dementia; of 1365 patients with anxiety disorder, 232 (17.0%) developed dementia; and of 3942 patients with depression, 701 (17.8%) developed dementia. Mean follow-up time (until dementia diagnosis/death/census) was 4.0 (s.d. ± 3.3) years for bipolar affective disorder, 2.8 (±2.7) years for anxiety disorders and 2.9 (±3.0) years for depression. The available follow-up time for bipolar affective disorder was significantly longer than for anxiety or depression.
Compared to depression, patients with bipolar affective disorder had a lower risk of developing dementia in the unadjusted analysis (hazard ratio: 0.30; 95% CI: 0.21–0.44) and in the adjusted analysis (hazard ratio: 0.60; 95% CI: 0.41–0.87).
Compared to depression, patients with anxiety had a similar dementia risk in the unadjusted analysis (hazard ratio: 1.01; 95% CI: 0.87–1.17) and in the adjusted analysis (hazard ratio: 1.05; 95% CI: 0.90–1.22).
In a sensitivity analysis, we excluded recurrent depressive disorder to ascertain whether the onset of a new depressive disorder in later life confers particular risk. In the unadjusted analysis, both bipolar affective disorder (hazard ratio: 0.25; 95% CI: 0.17–0.37) and anxiety disorders (hazard ratio: 0.81; 95% CI: 0.69–0.94) had a lower risk of dementia, suggesting the development of new depression in late life might confer greater risk. However, while the effect survived adjustment for bipolar affective disorder (hazard ratio: 0.52; 95% CI: 0.35–0.76), it did not for anxiety disorders (hazard ratio: 0.94; 95% CI: 0.81–1.10).
Factors associated with dementia development in the three sub-cohorts
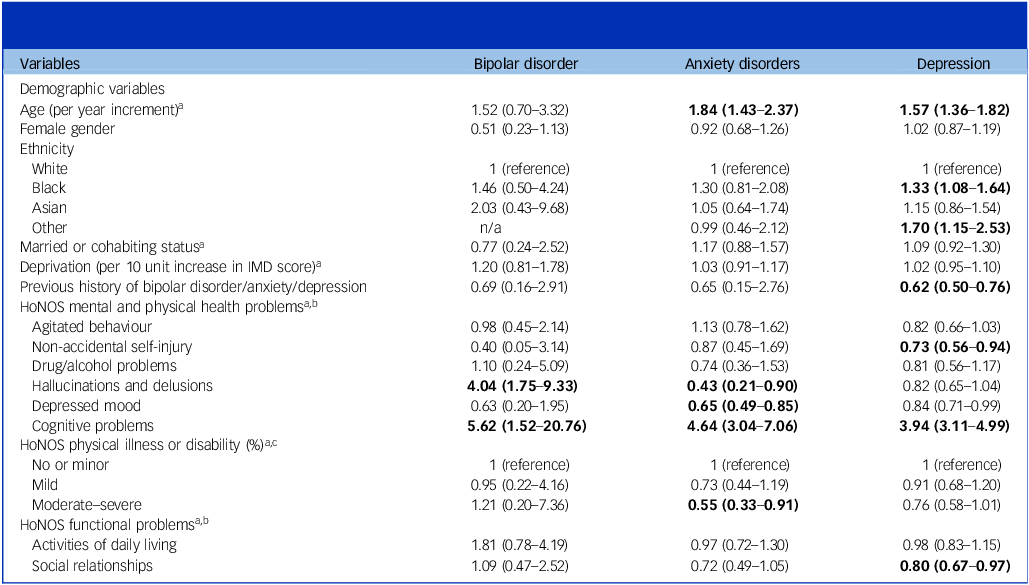
Using the multivariate Cox proportional hazards model, we determined the factors associated with subsequent dementia development in each group. The results are shown in Table 2.
Factors associated with dementia development in the three cohorts of patients with affective disorders using multivariate Cox proportional hazard model adjusted for age, age-squared, gender, ethnicity, marital status, deprivation, baseline cognition and time*cognition interaction

HoNOS, Health of the Nation Outcome Scales; IMD, Index of Multiple Deprivation. Bold indicates a significant increase or decrease in hazard ratio at P = 0.05.
a. At the time of affective disorder diagnosis (±6 months)
b. Health of the Nation Outcome Scale 65+ (HoNOS65+) subscale scores 0–4 (0 = least severe, 4 = most severe status) were categorised into scores of 0–1, representing that the patient was not experiencing problems in that domain, and scores of 2–4, representing that the patient was experiencing problems. Values represent frequencies of patients scored as experiencing problems in that domain.
c. Analysis incorporates a time*physical illness or disability interaction.
In patients with bipolar affective disorder, hallucinations and/or delusions and cognitive problems measured close to the time of affective disorder diagnosis were associated with a higher risk of dementia development. Neither age at diagnosis nor a prior history of bipolar affective disorder were associated with dementia development.
In patients with anxiety disorder, age at anxiety disorder diagnosis and cognitive problems were associated with a higher risk of dementia development, while depressed mood, hallucinations and delusions and moderate–severe physical health problems yielded a lower risk. A previous history of an anxiety disorder did not affect dementia risk.
In patients with depression, age at depression diagnosis, Black and ‘other’ (compared to White) ethnicity and cognitive problems yielded a higher risk of developing dementia. The presence of non-accidental self-injury, difficulties with social relationships and a previous history of depression were associated with a lower risk of developing dementia.
Discussion
In a large cohort of patients diagnosed with an affective disorder in later life in routine mental health services, we evaluated how the risk of progressing to a dementia diagnosis differed among bipolar affective disorder, anxiety disorders and depression. While patients with late-life anxiety disorders had a similar dementia risk as patients with late-life depression, patients with late-life bipolar affective disorder had a 40% lower dementia risk than those with depression after confounder adjustment. These findings advance our understanding of how distinct affective disorder subtypes influence dementia risk and, by identifying specific variables associated with increased risk, our work could help refine risk prediction models for dementia among patients with affective disorders, enabling early identification of high-risk individuals. It provides a basis for targeted interventions that address modifiable factors, potentially mitigating the progression to dementia.
Dementia development
The reduced rate of dementia diagnosis in those with late-life bipolar affective disorder compared to those with late-life depression (hazard ratio: 0.60; 95% CI: 0.41–0.87) occurred despite the longer follow-up time available for these patients. One explanation might relate to the substantially younger age at the time of affective disorder diagnosis for bipolar affective disorder patients, compared to those with depression. However, age and age-squared were adjusted for in our multivariate model, and the risk remained lower. Furthermore, age did not seem to predict dementia development in people diagnosed with bipolar affective disorder. A second possibility is that patients with bipolar affective disorder who survive to dementia-risk ages are relatively healthier than those with depression, owing to the survival pressure associated with a severe mental illness (‘survivor effect’). Therefore, the cohort reaching this age range may carry a relatively lower baseline dementia risk. A third reason may be that bipolar affective disorder is more distinguishable from dementia compared to depression, which can present with marked cognitive impairment.Reference Austin, Mitchell and Goodwin28
The distinguishability of bipolar affective disorder relates to a fourth reason – access to treatment. Many older people with depression do not access treatment, and the risk of progression to dementia is higher in untreated depression.Reference Yang, Deng, Leng, Ou, Li and Chen29 As bipolar affective disorder is arguably more distinguishable and apparent, patients may be more likely to access appropriate treatment. Cognitive decline in bipolar affective disorder seems to stabilise over time, especially in people who are receiving treatmentReference Flaaten, Melle, Bjella, Engen, Åsbø and Wold30; by contrast, cognitive decline continues to progress in patients with unipolar depression.Reference Yin, John and Cadar31 Lithium may be important – previous work has suggested that bipolar affective disorder is associated with an increased risk of dementia, but that the risk is reduced when patients are treated with lithium.Reference Velosa, Delgado, Finger, Berk, Kapczinski and de Azevedo Cardoso32 Because of low numbers, we were unable to determine if there were different patterns for patients on or off lithium. Retrospective cohort studies suggest that lithium exposure (across both unipolar and bipolar depression) reduces the risk of developing dementia subsequently.Reference Chen, Underwood, Jones, Lewis and Cardinal33 A randomised clinical trial investigating the utility of lithium in protecting against the progressive cognitive decline associated with mild cognitive impairment has shown that lithium improves long-term global cognitive outcomes.Reference Damiano, Loureiro, Pais, Pereira, Corradi and Di Santi34 The presence of some patients on lithium in the cohort we examined might therefore result in an overall lower risk of dementia in patients with late-life bipolar affective disorder compared to those with late-life depression, although this cannot be disentangled from the potential survivor effect, or baseline health differences.
The presence of a late-life anxiety disorder was associated with a similar risk of dementia to the presence of a late-life depressive disorder (hazard ratio: 1.02; 95% CI: 0.88–1.19). In some studies, anxiety disorders have been shown to increase the risk of all-cause dementiaReference Santabárbara, Lipnicki, Olaya, Villagrasa, Bueno-Notivol and Nuez7; however, other studies have not supported a link.Reference de Bruijn, Direk, Mirza, Hofman, Koudstaal and Tiemeier8 The emotional dysregulation characteristic of anxiety disorders may be caused by neurobiological changes in vulnerable brain regions associated with dementia, such as the hippocampus, which precede the onset of cognitive decline.Reference Singh-Manoux, Dugravot, Fournier, Abell, Ebmeier and Kivimäki17 Anxiety disorders are associated with a higher risk of cardiovascular disease,Reference Emdin, Odutayo, Wong, Tran, Hsiao and Hunn35 raised levels of glucocorticoidsReference Raglan, Schmidt and Schulkin36 and avoidant behaviour and social isolation, all of which may also act to increase the risk of dementia. It is also important to consider diagnostic clarity; there is overlap between anxiety and depression and the disorders are highly comorbid, especially in later life.Reference Lenze37,Reference Post38 This might contribute to the similar dementia risk.
Factors associated with the development of dementia
In those with a depressive disorder, a prior history seemed to reduce the risk of a subsequent diagnosis of dementia. This might seem counterintuitive; previous studies have suggested that no matter when a depressive episode occurs, it increases the risk of dementia,Reference Elser, Horváth-Puhó, Gradus, Smith, Lash and Glymour39 and furthermore that repeated depressive episodes increase the risk of subsequently developing dementiaReference Kessing and Andersen40 through the cumulative effects of sustained stress and a failure of improvement in cognition between episodes. One interpretation might be that the new onset of a depressive disorder later in life is more likely to reflect a dementia prodrome rather than a primary affective illness, compared to the relapse of a pre-existing depressive disorder.Reference Peakman, Karunatilake, Seynaeve, Perera, Aarsland and Stewart16 Therefore, a prior history of the disorder would be protective. This is corroborated by our finding that in an unadjusted sensitivity analysis, excluding recurrent depression, both bipolar affective disorder and anxiety disorders were associated with a lower risk of dementia compared to late-life depression. This further adds evidence that the new onset of a depressive disorder in late life is particularly associated with the development of subsequent dementia.Reference Singh-Manoux, Dugravot, Fournier, Abell, Ebmeier and Kivimäki17
Interestingly, problems with social relationships in those with late-life depression were associated with a lower risk of dementia. The HoNOS subscale however refers to relationship problems – which are risk factors for depression (as lack of intimacy or poor social support) – rather than social isolation in the context of cognitive decline.Reference Burns, Beevor, Lelliott, Wing, Blakey and Orrell24 Problematic relationships on this scale may therefore be better predictors of a depressive illness rather than an underlying dementia.
In late-life depression, Black (and other) ethnicity was associated with an increased risk of dementia progression. Dementia incidence is higher in people of Black ethnicity, likely contributed to by socioeconomic and physical health factors (in particular, vascular risk factorsReference Mukadam, Marston, Lewis, Mathur, Rait and Livingston41). The increased burden of psychiatric symptoms, greater degree of functional impairment and poorer access to timely mental health treatment associated with late-life depressiveReference Vyas, Donneyong, Mischoulon, Chang, Gibson and Cook42 and anxietyReference Jones, Rafferty, Cochran, Abelson and Mays43 disorders in people of Black ethnicity may contribute to the increased risk of subsequent progression to dementia, through the effects of chronic stress and/or incomplete cognitive recovery between episodes. There may also be an increased burden of physical illness and comorbidity in people of Black ethnicity, which additionally increase the risk of dementia.Reference Johnson-Lawrence, Griffith and Watkins44
In those with anxiety disorders, the presence of comorbid depressed mood was protective against dementia. Similarly, the presence of hallucinations and/or delusions was associated with a lower risk. In older people, isolated anxiety, especially if severe, can suggest an organic process such as dementia. By contrast, anxiety in the context of other symptoms may be occurring in conjunction with another psychiatric disorder; anxiety in older people is often noted in the context of a depressive illnessReference Lenze37 and generalised anxiety in particular is frequently considered to be a manifestation of the same underlying depressive illness. Moderate–severe physical health issues yielded a lower dementia risk too; this may be a mortality effect.
In those with late-life bipolar affective disorder, hallucinations, delusions and cognitive problems were strong predictors of the subsequent development of dementia. The presence of hallucinations and delusions indicates a worse disease severity, resulting in admission to hospital and poor concordance with medications for both mental and physical illness,Reference Jawad, Watson, Haddad, Talbot and McAllister-Williams45 all of which could contribute to an increased dementia risk. It is also possible that psychotic symptoms might herald the development of dementia, not occurring infrequently in, for example, Alzheimer’s diseaseReference Murray, Kumar, DeMichele-Sweet and Sweet46 and Lewy body dementias.Reference Mueller, Ballard, Corbett and Aarsland47 Hallucinations and delusions have been linked to a ‘mild behavioural impairment’ that has been described as a transitional state towards dementia, analogous to mild cognitive impairment.Reference Taragano, Allegri, Krupitzki, Sarasola, Serrano and Loñ48 It is also possible that a misdiagnosed delirium accounts for the increased risk associated with these symptoms.Reference FitzGerald, Perera, Chang-Tave, Price, Rajkumar and Bhattarai49
Strengths and limitations
Our findings are derived from data collected using CRIS, which leverages the largest and most detailed electronic health record system for secondary mental health care globally. This enhances the generalisability of our results, particularly to urban populations engaged in secondary care mental health services, given the ethnic and socioeconomic diversity of the catchment area. The depth of CRIS data allows for diagnostic ascertainment, follow-up and exploration of confounding factors, bolstering the credibility of our findings.
However, limitations must be acknowledged. As our cohort is drawn exclusively from secondary care, it may not fully capture individuals with milder affective disorders or those managed entirely in primary care or community settings. In addition, while the diversity of the population is a strength, findings may not directly generalise to rural or less diverse populations, or to healthcare systems differing substantially from the National Health Service (NHS).
Selection bias arises as our patients are selected from a predominantly secondary care cohort. Many late-life depressive and anxiety disorders may be managed at a primary care level, while our cohort is in specialist mental health care. Cases of depression and anxiety in secondary care are typically more severe than those seen in primary care; bipolar affective disorder is almost always managed in secondary care. In our cohort, the risk of dementia in secondary care depression and anxiety may therefore be higher than that seen in primary care settings.
Information bias may arise from inaccuracies in the clinical records. Misclassification errors related to diagnosis are possible, although we believe this is a relatively small threat; in CRIS, diagnoses are made by specialised psychiatrists who are applying ICD-10 criteria (compared to primary care or national registries). The misclassification of bipolar affective disorder is lower in later life, given the more extensive past psychiatric history and reduced challenge of disentangling bipolar affective disorder and a personality disorder. The risk of misclassification with anxiety disorders versus unipolar depression may be higher, given that anxiety in later life often occurs in the context of a depressive illness.Reference Lenze37,Reference Post38 The comparison between anxiety disorders versus unipolar depression may, therefore, in part be a comparison between depression with anxiety versus depression without anxiety.
Patients with comorbid late-life depression and late-life anxiety were classified in the anxiety disorders group; it was not possible to disentangle the primary diagnosis in these patients and this may affect the comparative rates of dementia in the groups. There may be ascertainment bias as we may have missed some patients’ previous histories of bipolar affective disorder and are therefore underestimating their occurrence; indeed, the sample size of patients with late-life bipolar affective disorder was small. Finally, the HoNOS illness confounders might also be inaccurately recorded.
Inherent in the retrospective cohort design is the issue of confounders. We tried to control for demographic confounders in our multivariate modelling. However, factors such as different ages of the cohorts, lifestyle factors and physical health comorbidities may not be completely controlled for using multivariate modelling. The HoNOS subscales do not include diagnostic information about specific physical health conditions, such as diabetes and cardiovascular disease; including such information could more comprehensively account for physical health as a potential confounder.
Causality cannot be established in a study of this design. It is also challenging to establish a clear temporal relationship between the exposures (LLADs) and the outcome (dementia), as cognitive impairments and neuropathological changes may have predated the onset of LLADs but may not have been detected.
In summary, in this large cohort of over 5000 patients with a LLAD, late-life anxiety disorders were associated with a similar risk of progression to dementia as late-life depressive disorders, whereas late-life bipolar affective disorder was associated with a lower risk. We were able to determine predisposing and protective factors, within LLAD cohorts, associated with the risk of dementia. Prospective cohort studies are needed to further explore the link between LLADs and the subsequent risk of developing dementia, including whether these populations are particularly at risk of certain dementia subtypes.
Data availability
All relevant aggregate data are found within the paper. The data used in this work have been obtained from CRIS, a system that has been developed for use within the National Institute for Health Research (NIHR) Mental Health Biomedical Research Centre (BRC) at South London and Maudsley NHS Foundation Trust (SLaM). It provides authorised researchers with regulated access to anonymised information extracted from SLaM’s electronic clinical records system. Individual-level data are restricted in accordance to the strict patient-led governance established at SLaM, and by NHS Digital for the case of linked data. Data are available for researchers who meet the criteria for access to this restricted data: (a) SLaM employees or (b) those having an honorary contract or letter of access from the trust. For further details, and to obtain an honorary research contract or letter of access, contact the corresponding author, L.A.
Author contributions
R.C. and C.M. conceived the study. C.M. acquired and analysed the data. L.A., K.B., M.B., A.H.Y., R.S. and C.M. interpreted the data. L.A., K.B., R.C. and C.M. drafted the manuscript. M.B., A.H.Y. and R.S. reviewed the manuscript for important intellectual content. All authors read and approved the final manuscript.
Funding
L.A. is funded through a NIHR Academic Clinical Fellowship award (ACF-2022-17-016). K.B. is funded through the Rosetrees Trust, Stoneygate Trust and a NIHR Academic Clinical Lectureship award. A.H.Y., R.S. and C.M. are part-funded by the NIHR Maudsley BRC at SLaM and King’s College London. R.S. and C.M. are also part-funded by the NIHR HealthTech Research Centre in Brain Health. R.S. is additionally part-funded by (a) the NIHR Applied Research Collaboration South London (NIHR ARC South London) at King’s College Hospital NHS Foundation Trust, (b) the UK Research and Innovation (UKRI) – Medical Research Council (MRC) through the DATAMIND HDR UK Mental Health Data Hub (MRC reference: MR/W014386) and (c) the UK Prevention Research Partnership (Violence, Health and Society; MR-VO49879/1), an initiative funded by UKRI Councils, the Department of Health and Social Care (England), the UK devolved administrations and leading health research charities. The views expressed are those of the authors and not necessarily those of the NIHR or the Department of Health and Social Care.
Declaration of interest
L.A. is an editor at BJPsych Open. R.S. declares research support received in the last 3 years from Janssen, GSK and Takeda. A.H.Y. is an editor at BJPsych and The Journal of Psychopharmacology and is a deputy editor at BJPsych Open. He did not take part in the review or decision-making process of this paper. He has carried out paid lectures and/or sat on advisory boards for the following companies with drugs used in affective and related disorders: Flow Neuroscience, Novartis, Roche, Janssen, Takeda, Noema pharma, Compass, AstraZeneca, Boehringer Ingelheim, Eli Lilly, LivaNova, Lundbeck, Sunovion, Servier, Livanova, Janssen, Allegan, Bionomics, Sumitomo Dainippon Pharma, Sage and Neurocentrx. K.B., M.B., R.C. and C.M. declare no conflict of interest.



eLetters
No eLetters have been published for this article.